6.2 The blood system
1/88
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
89 Terms
components of the blood
1. plasma
2. erythrocytes
3. leucocytes
4. platelets
plasma (d)
liquid portion of blood; contains water, proteins, salts, nutrients, lipids, hormones, and vitamins
Erythrocytes (d)
red blood cells
transport oxygen
3 main types of blood vessels
1. arteries
2. veins
3. capillaries
tissue layers of the walls of blood vessels (3)
1. tunica externa- outer layer
2. tunica media - muscle/elastin layer
3. tunica intima-endothelium
structure of the tunica media(2)
1. a layer of circumferential smooth muscle and variable amounts of connective tissue
2. as second layer of elastic fibers(the external elastic lamina) is located beneath the smooth muscle.
Function of arteries (2)
1. carry blood away from the heart.
2. transports blood at high pressure away from the ventricles to the body tissues.
function of veins (2)
1. carry blood toward the heart
2. transports blood at low pressure
Capillaries (d) (2)
1. very small vessels that can penetrate into body tissues
2. blood moves slowly through them under low pressure providing opportunities for the exchange of substances.
structure of arteries with respect to function (3)
1. relatively small lumen to maintain high blood pressure
2. thick muscular wall and fibrous outer layer of collagen helps it to withstand high bp
3. arterial wall contains an inner layer of muscle and elastic fibers to help maintain pulse flow
3 main types of arteries
1. elastic arteries
2. muscular arteries
3. arterioles
elastic arteries (d)
1. arteries that receive blood directly from the heart
2. need to be elastic because: They are relatively thin compared to their diameter.
3. When the heart contracts, and ejects blood into these arteries, the walls need to stretch to accommodate the blood surge, storing energy.
4. Between heart contractions, the elastic walls recoil, to maintain blood pressure, continuing to move blood even when ventricles are relaxed.
tunica media of elastic arteries
broad and elastic with concentric fenestrated sheets of elastin, and collagen and only relatively few smooth muscle fibers
muscular arteries (d) (2)
1. distribute blood to various parts of the body
2. The walls of these arteries have lots of smooth muscle, which means that they are able to contract or relax (dilate) to change the amount of blood delivered, as needed.
tunica media of muscular arteries (2)
1. well defined layer of smooth muscle
2. elastin sheet is reduced
Arterioles (3)
1 small arteries that deliver blood to the capillaries
2. controls blood flow by contracting and dilating the size of its lumen
3. tunica media contains concentric rings of circular muscle to do this.
elastic recoil (d) (2)
1. refers to the inherent resistance of a tissue to changes in shape, and the tendency of the tissue to revert to its original shape once deformed.
2. With each heartbeat, blood is forced into the arteries causing them to dilate (expand). Then the arteries contract (recoil) as the blood moves further along in the circulatory system.
pulse (d)
alternate expansion and recoil of an artery
how do smooth and elastin fibres maintain blood pressure between pump cycles? (2)
1. systolic pressure
>store potential energy in elastin due to high pressure
2.diastolic pressure
>elastin fibers squeezes the blood in the lumen when the pressure in lumen fall at the end of a heart beat.
blood pressure (d)
The force that blood exerts on the walls of vessels through which it flows
vasoconstriction (d)
decreases blood flow as the smooth muscle in the walls of the tunica media contracts, making the lumen narrower and increasing blood pressure.
Vasolidation (d)
increases blood flow as the smooth muscle relaxes, allowing the lumen to widen and blood pressure to drop
what are the vascular nerves that control vasoconstriction and vasodilation?
nervi vasorum
what are the 2 tissues that capillaries do not supply blood to?
cornea and lens
how does the structure of the veins correspond to its function 3
(3)
1. relatively thinner tunica media with fewer smooth/elastin fibres
2. much larger lumen
3. has valves to prevent backflow of blood
describe the flow of blood in arteries in comparison to veins (2)
1. blood flow in arteries is
pulsatile
2. blood flow in veins is non-pulsatile
what mechanism is used to increase the pressure within the veins?
skeletal muscle pump mechanism
skeletal muscle pump mechanism
(D)
contraction of the surrounding skeletal muscle increases the pressure of the blood flowing within veins
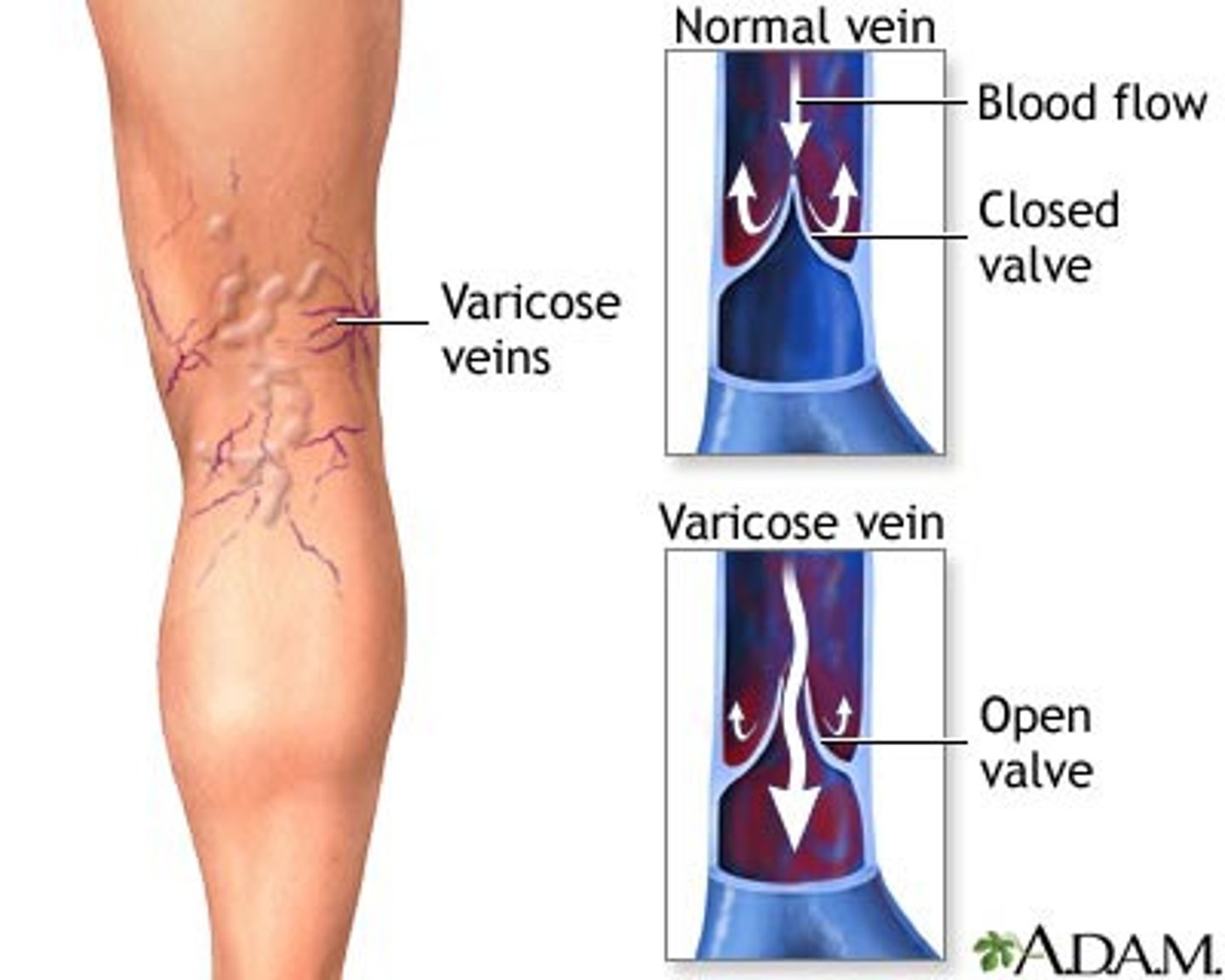
what is the function of valves in veins?
ensuring unidirectional blood flow
how do venous valves and skeletal muscles regulate blood flow in the veins (4)
1. valves in veins are bicuspid, have 2 flap like structures that regulate blood flow. these are called pocket valves as they can catch blood
2. when the skeletal muscles contract blood is pushed toward the heart
3. the valves are open so blood can circulate
4. when the skeletal muscle is at rest the valves close.
specialized structure of capillaries to conduct material exchange
1. very small diameter which allows the passage of only a single RBC at a time to ensure optimal exchange.
2. wall is made of a single layer of cells to minimize the path of diffusion.
3. surrounded by a basement membrane permeable to necessary materials
4. may contain pores
types of capillaries based on structure and function(3)
1. Continuous
2. Fenestrated
3. Sinusoidal
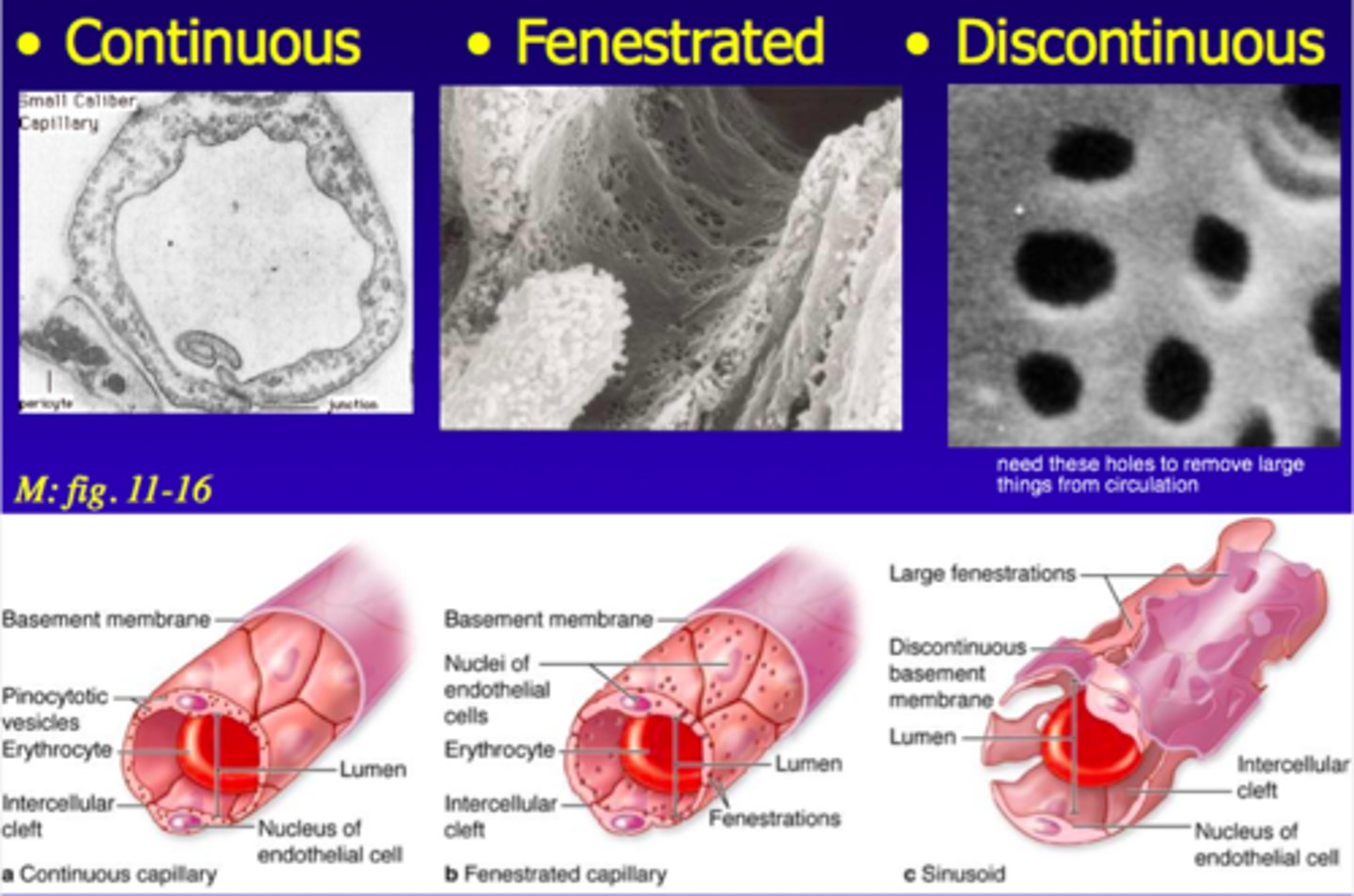
continuous capillaries
Capillary wall is continuous and endothelium is held together by tight junctions
fenestrated capillaries
Capillary wall contains pores
sinusoidal capillaries
have large gaps between adjacent endothelial cells
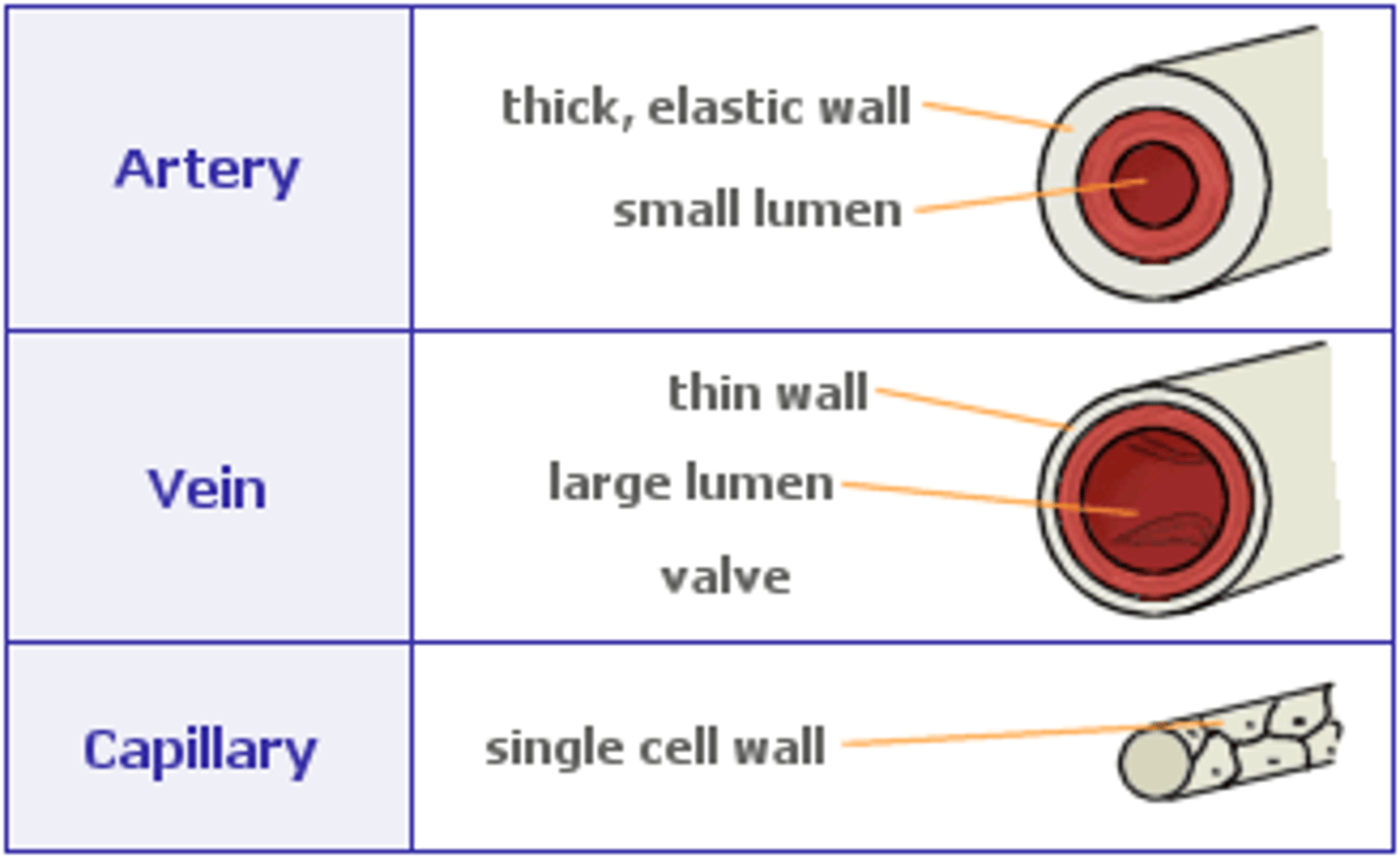
comparison of the structure of veins, capillaries and arteries (diagram)
double circulation
A type of blood circulation system in which the blood flows through the heart twice. In this type of circulation, the pulmonary circulation is separate from the systemic circulation.
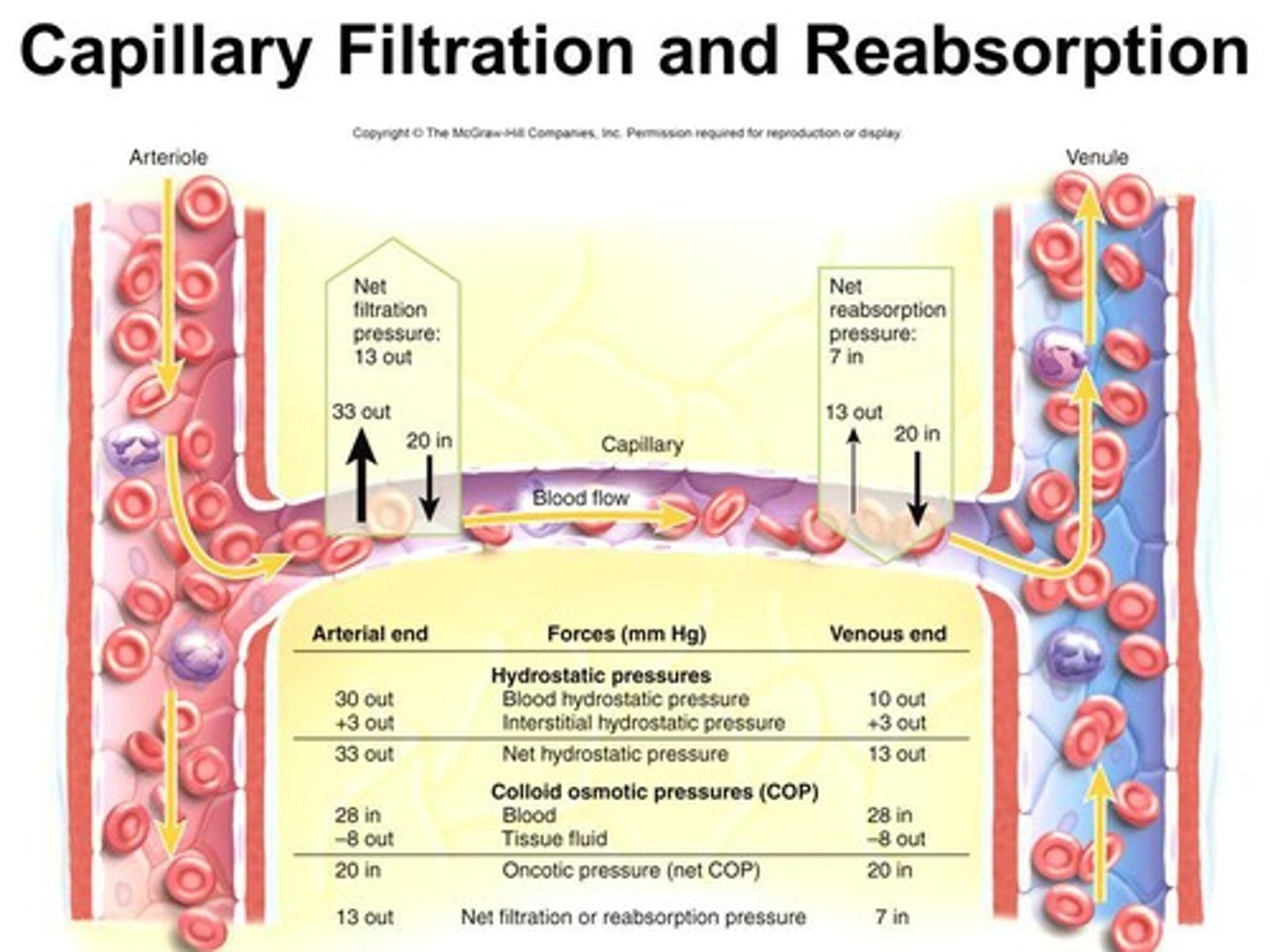
how are materials exchanged in capillaries, explain with reference to blood pressure. (5)
1. blood flows through capillaries at very low pressure to maximize material exchange
2. high blood pressure in arteries is dissipated by extensive branching of vessels and narrowing of lumen
3.atreriole end has higher hydrostatic pressure
4.forces material from the blood stream into the tissue fluid
5. venule end has lower hydrostatic pressure, allows materials from the tissues to enter the bloodstream.
anatomy of the heart
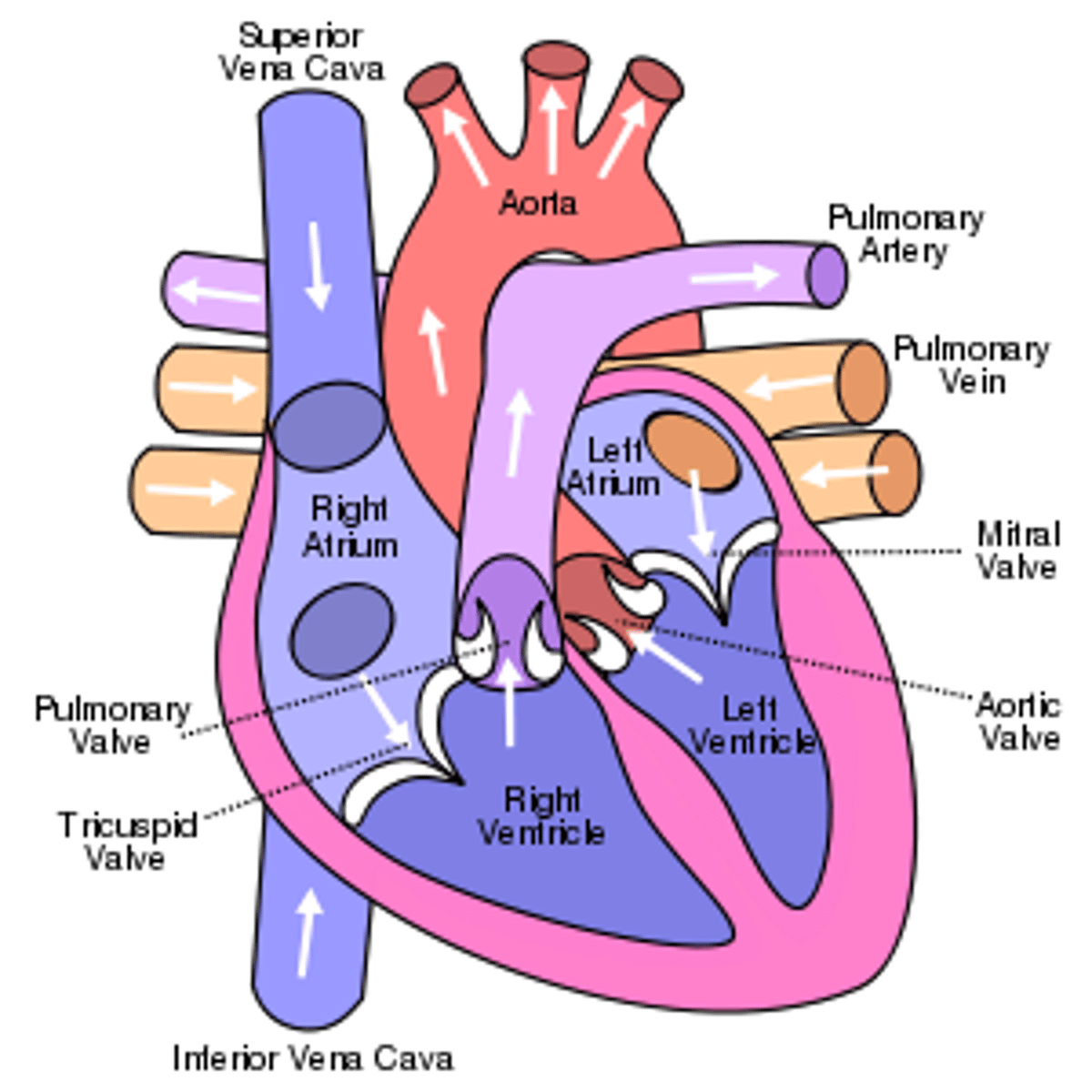
why is the contraction of the heart myogenic?
the signal for a cardiac compression is initiated by cardiomyocytes rather than from brain signals
name for heart muscle cells
cardiomyocytes
sinoatrial node (3)
1. cluster of specialized cardiomyocytes in the wall of the right atrium
2. directs the contraction of the heart muscle tissue
3. acts as the primary pacemaker
Secondary pacemaker of the heart
atrioventricular (AV) node
tertiary pacemaker of the heart
bundle of his
fibrillation
uncontrolled quivering or twitching of the heart muscle caused by the interference of pacemakers
sinus rhythm
the normal (optimal) heart rhythm arising from the sinoatrial node
Role of the pacemaker
Sends electrical signals to keep the pattern of the contraction and relaxation.
what are the steps of the electrical conduction of a heart beat? (6)
1. SA node sends out electrical impulse
2. impulse causes atria to contract
3. impulse stimulates the AV node
4. AV node sends a signal down the septum via a nerve bundle(bundle of his)
5. bundle of His innervates nerve fibres (purkinjie fibers) in the ventricular wall
6. innervation of purkinjie fibres causes ventricular contraction
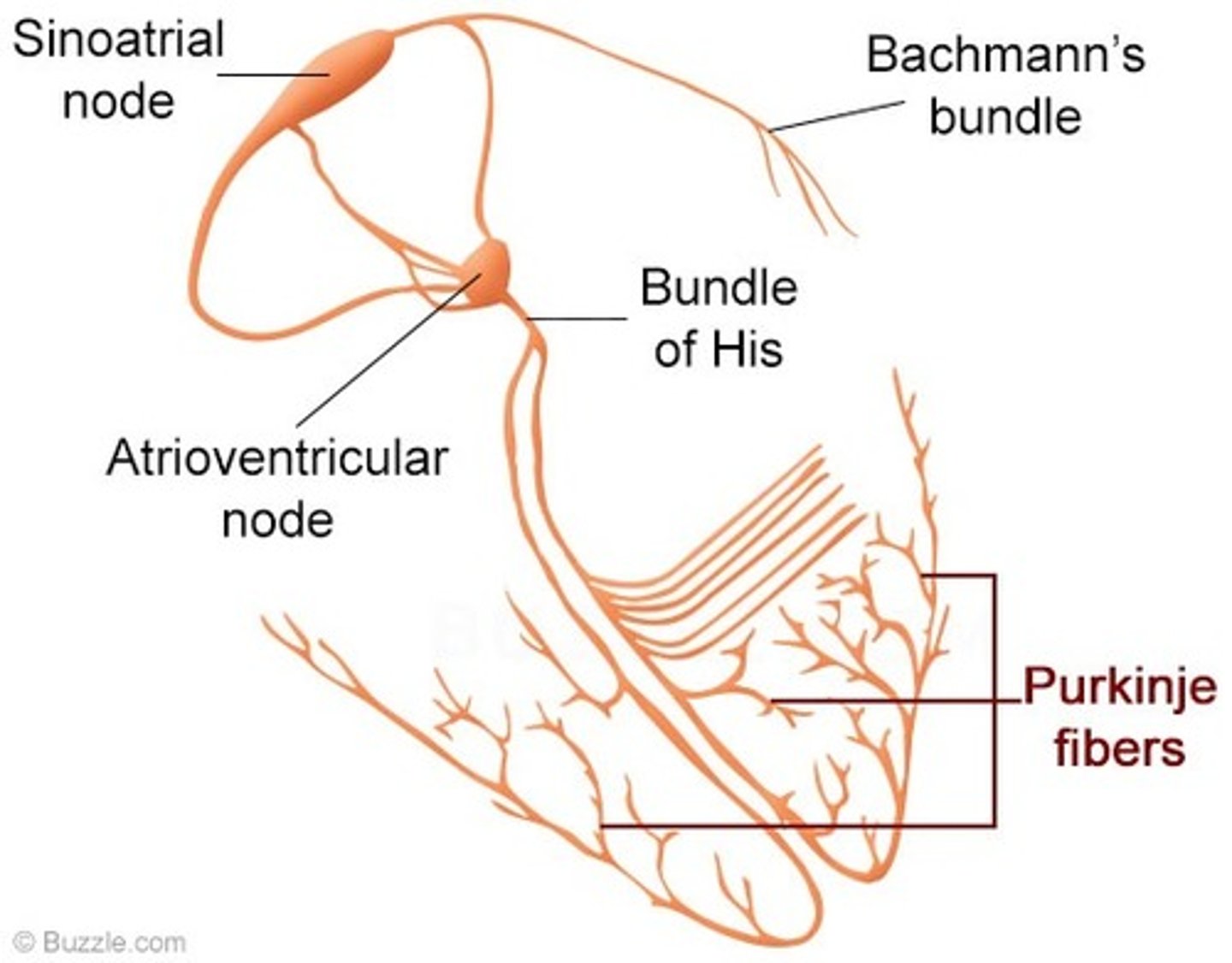
external signals that can regulate the heart rate?(4)
1. nerve signals, trigger rapid changes
2. endocrine signals, trigger more sustained changes
3. changes to blood pressure levels
4. changes to blood pH
which part of the brain is the pacemaker connected to?
medulla oblongata
how does an impulse from the sympathetic nerve affect the heart rate?
1. releases the neurotransmitter noradrenaline
2. increases heart rate
another name for noradrenaline
norepiphrine
how does an impulse from the parasympathetic nerve affect the heart rate?
1. releases the neurotransmitter acetylcholine
2. decreases heart rate
Hormones
chemical messengers that are manufactured by the endocrine glands, travel through the bloodstream, and affect other tissues
another name for adrenaline
epinephrine
what affect does adrenaline have on the heart rate?
1. increases heart rate
2. activates the same chemical pathways as noradrenaline
Where is adrenaline produced?
adrenal glands above kidneys
cardiac cycle
the series of events that take place in the heart over the duration of a single heart beat
Systole
contraction
Diastole
Relaxation /dilation
what are the 3 main events of the cardiac cycle?
atrial systole
ventricular systole
diastole
what happens during atrial systole?
1. atria contract
2. blood flows from atria to ventricles
3.AV valve is open, semiluna valves closed
what happens during ventricular systole?
1.ventricle contracts
2. blood flows from ventricle to aorta
3. semiluna valves open, AV valves closed
what happen during caridac diastole?
1. atria and ventricles relax
2. blood flows into atrium and ventricle
3.AV valve open, semi luna valves close
lub sound
AV valves closing
dub sound
semilunar valves closing
systolic pressure
Blood pressure in the arteries during contraction of the ventricles.
diastolic pressure
Blood pressure that remains between heart contractions.
blood pressure is measured in which blood vessel?
arteries
normal blood pressure of a healthy adult?
120/80 mmHg
electrocardiogram
record of the electrical activity of the heart
what are the different regions of an electrocardiograph and what do they represent?
P wave
>atrial contraction
>depolarization of the atria in respince to the signalling from the SA node
QRS complex
>ventricular contraction
>depolarization of ventricles due to signal from AV node
T wave
>repolarization of ventricles
>ventricular relaxation
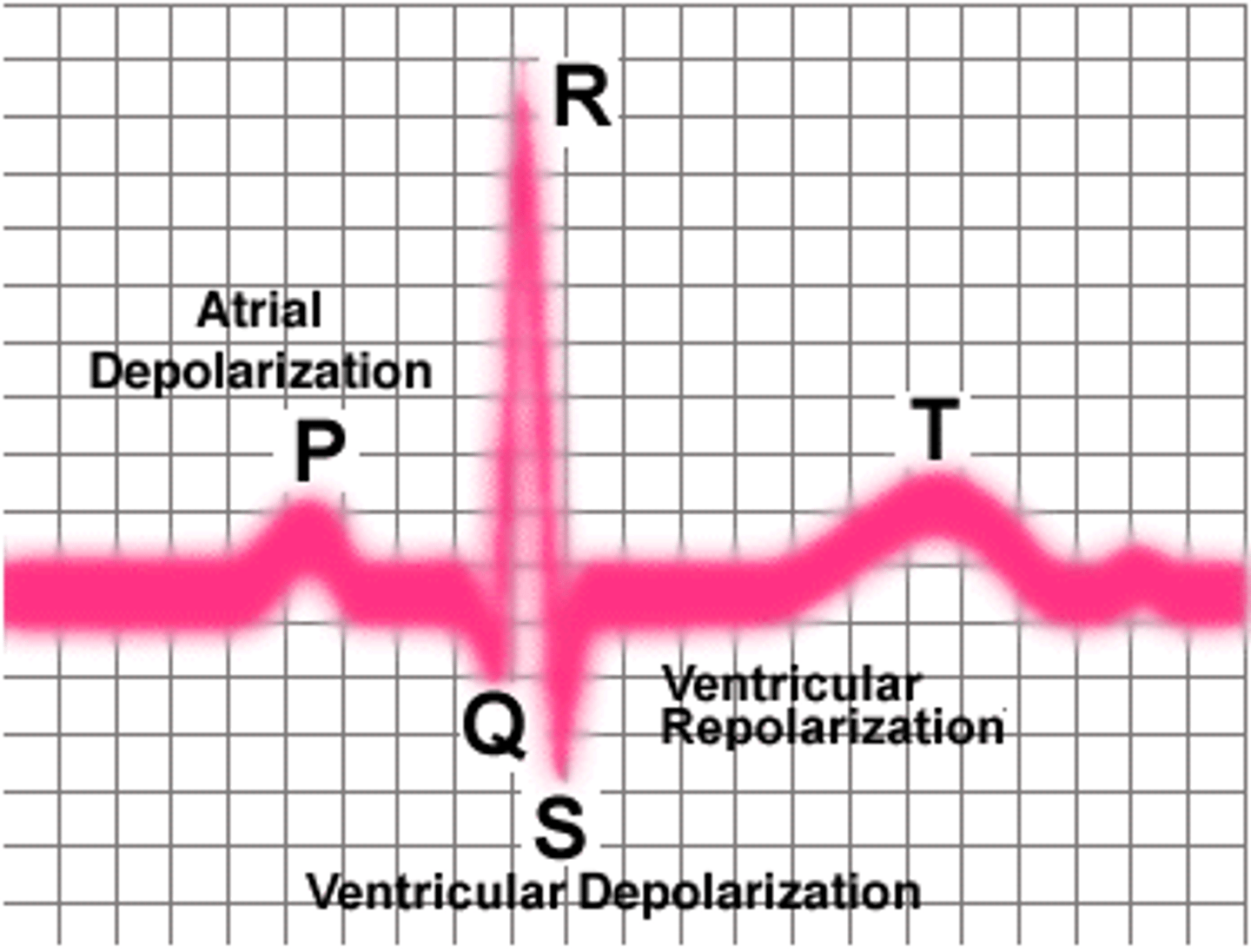
arrhythmia
Abnormal heart rhythm
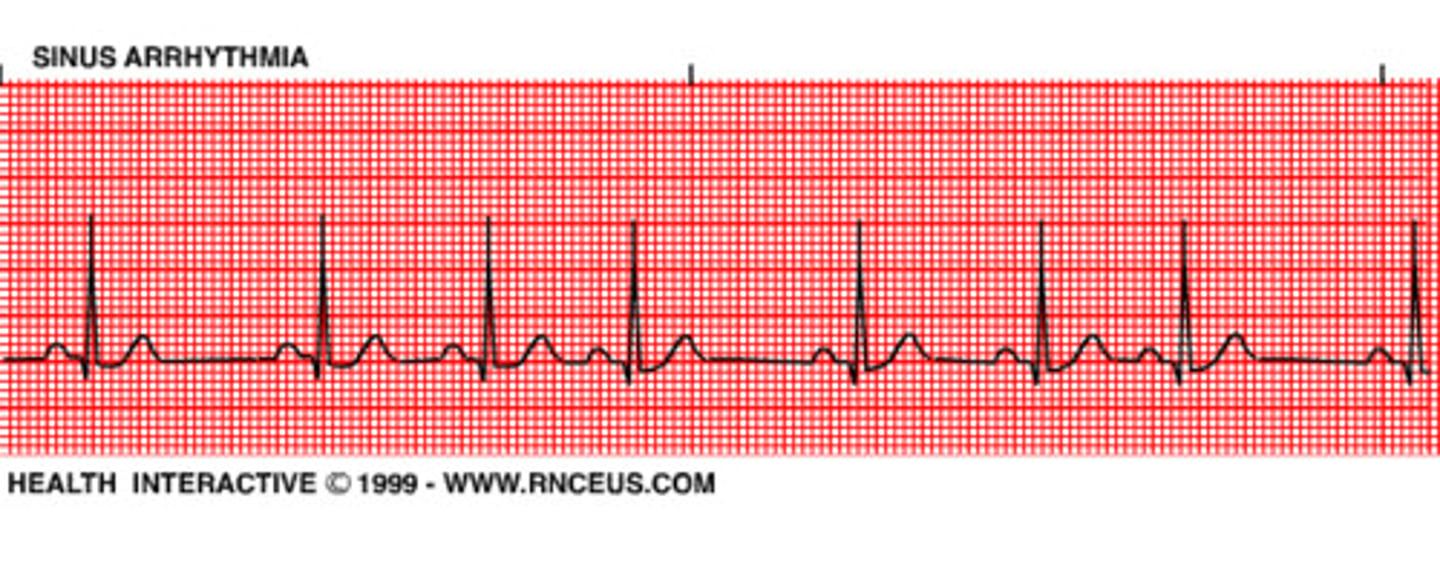
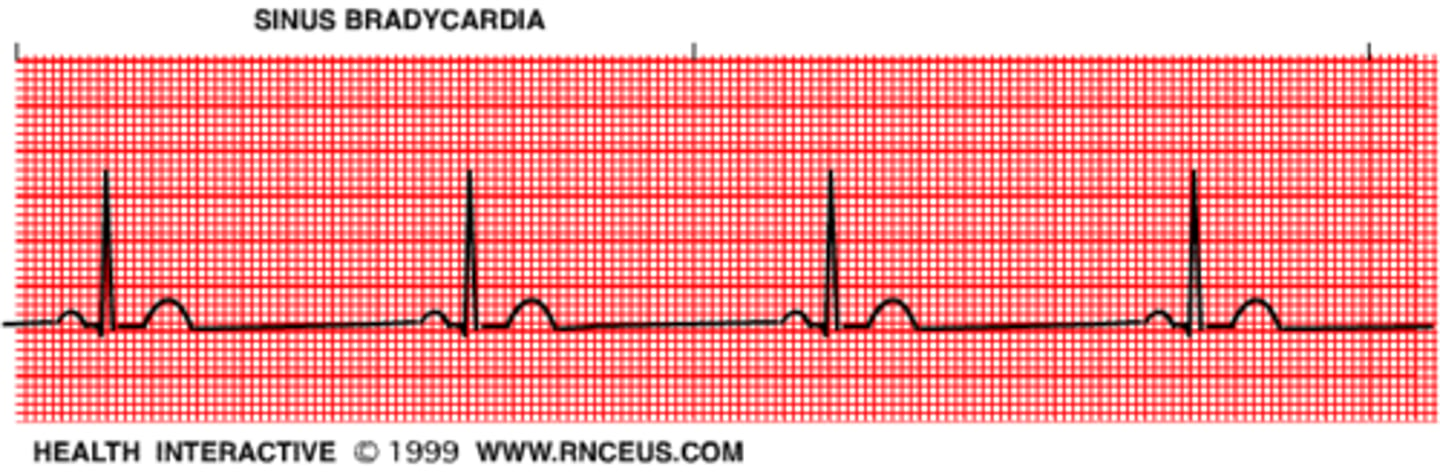
Bradycardia
slow heart rate
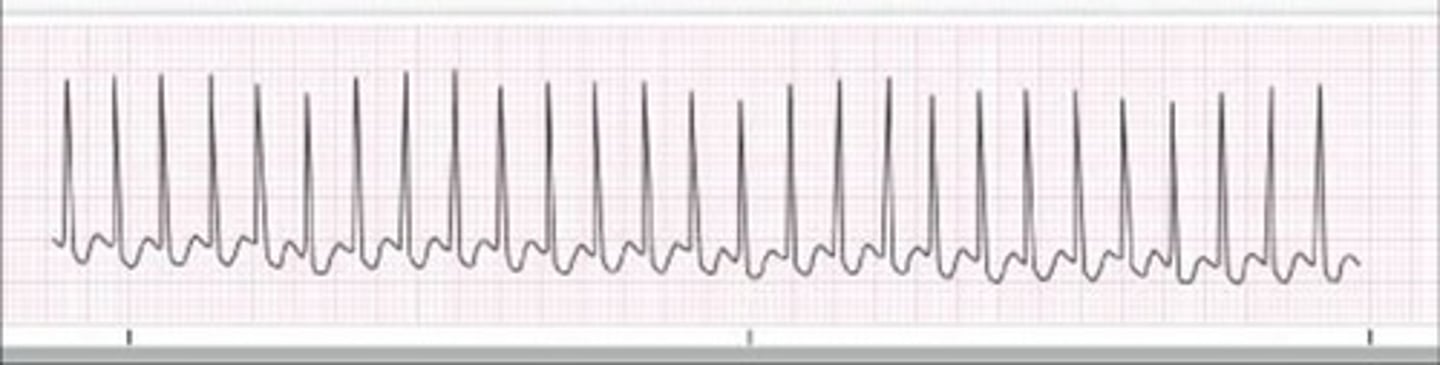
tachcardia
fast heart rate
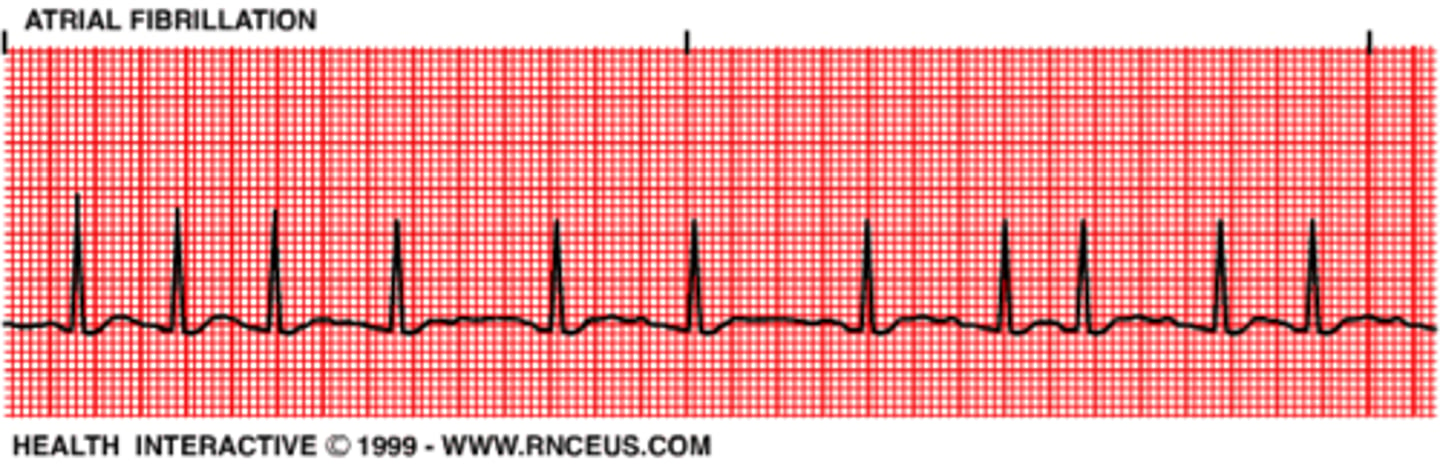
atrial fibrillation
rapid, random, ineffective contractions of the atrium
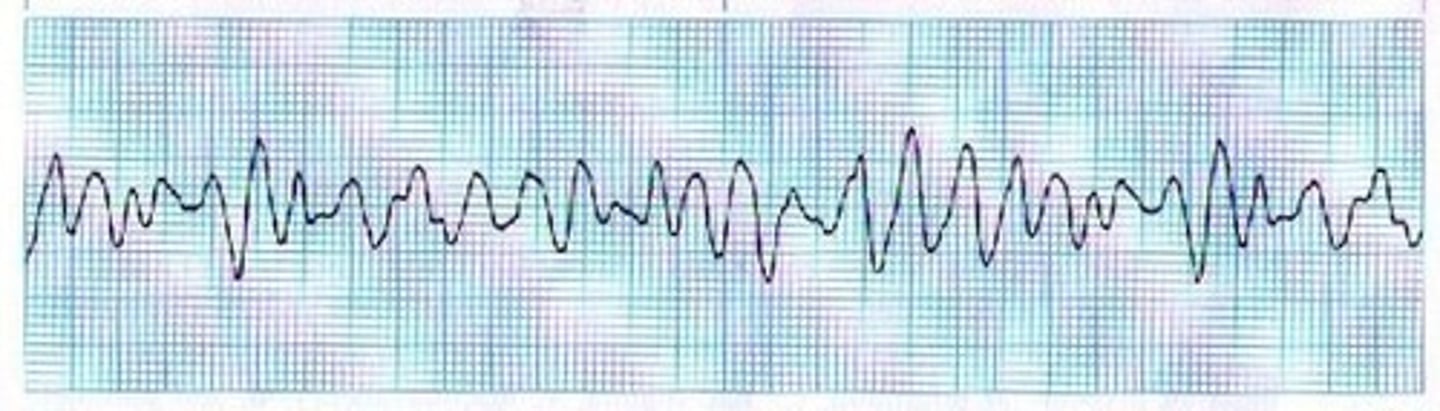
ventricular fibrillation
the rapid, irregular, and useless contractions of the ventricles
occlusion
blockage
coronary arteries
supply oxygen-rich blood to the myocardium
Artherosclerosis
Hardening and narrowing of the arteries due to buildup of cholesterol plaques
atherosclerotic plaque
The cholesterol-rich material that is deposited in the arteries of individuals with atherosclerosis.
How does coronary occlusion occur via atherosclerosis?(steps)
1. atheromas develop in the artery
2. reduce the diameter of the lumen
3. restricted blood flow increases pressure in the artery
4. damage to the internal wall due to stress
5.damaged region is repaired with fibrous tissue
6.reduces elasticity of the wall
7. lesions form as the smooth lining of the artery degrades
8.if the lesions rupture blood clotting is triggered forming a thrombus that restricts blood flow
9.if thrombus dislodges it can cause blockage in a smaller arteriole
artheroma
fatty deposit within the wall of an artery
embolus
A clot that breaks lose and travels through the bloodstream.
consequences of coronary occlusion?
- can lead to blood clots that cause heart attack or stroke
risk factors for coronary heart disease
age, genetics, obesity, diseases(eh.diabetes), diet, exercise, sex, smoking
why are males more susceptible to coronary heart disease
as they have lower oestrogen levels
why does smoking a risk facto for heart disease?
Nicotine causes vasoconstriction, raising blood pressure
What does the cardiovascular centre in the medulla oblongata of the brain monitor?
blood pressure, blood pH and carbon dioxide concentration