6.2 The blood system
1/44
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
45 Terms
William harvey
English physician, modern understanding of circulatory system
beliefs before harveys findings: Galens view
Arteries and veins were separate blood networks (except where they connected via invisible pores)
Veins were thought to pump natural blood (which was believed to be produced by the liver)
Arteries were thought to pump heat (produced by the heart) via the lungs (for cooling – like bellows)
harveys proposal
Arteries and veins were part of a single connected blood network (he did not predict the existence of capillaries however)
Arteries pumped blood from the heart (to the lungs and body tissues)
Veins returned blood to the heart (from the lungs and body tissues)
systemic circulation
The left side of the heart pumps oxygenated blood around the body
pulmonary circulation
the right side of the heart pumps de-oxygenated blood to the lungs
the heart has what type of circulatory system
a double
arteries
transport blood at high pressure from the from the ventircles to body tissues and the lungs(deoxygenated here, usually oxygenated)
arteries specialised structure
They have a narrow lumen (relative to wall thickness) to maintain a high blood pressure (~ 80 – 120 mmHg)
They have a thick wall containing an outer layer of collagen to prevent the artery from rupturing under the high pressure
The arterial wall also contains an inner layer of muscle and elastic fibres to help maintain pulse flow (it can contract and stretch)
labelled a diagram of the artery
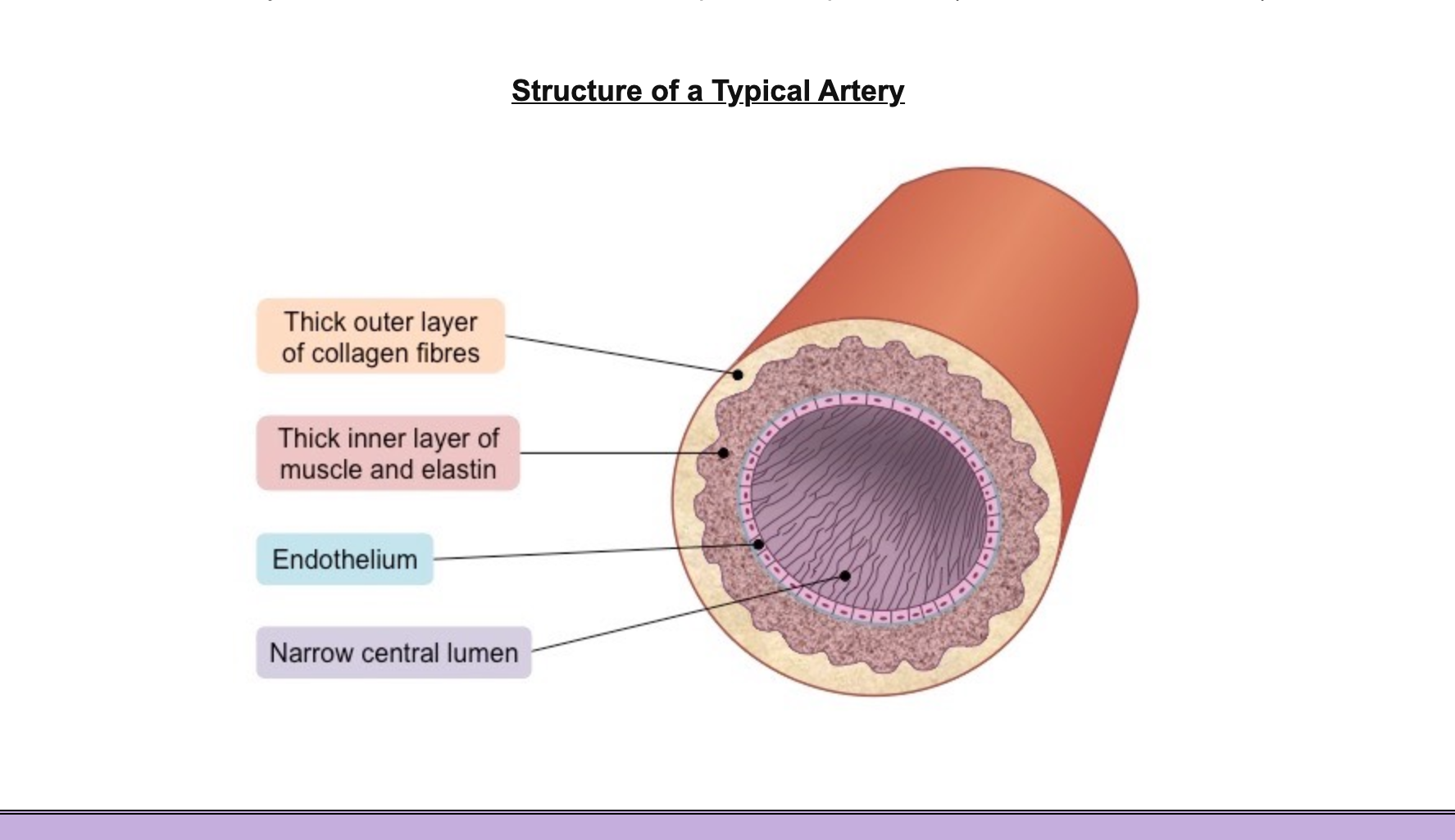
how does the blood flow through the arteries
in repeated surges called pulse
muscle fibre function
form a rigid arterial wall that is capable of withstanding the high blood pressure without rupturing
Muscle fibres can also contract to narrow the lumen, which increases the pressure between pumps and helps to maintain blood pressure throughout the cardiac cycle
elastic fibre function
allow arterial wall to stretch and expand upon the flow of a pulse through the lumen
capillaries
exchange materials between cells in tissues and blood travelling at a low pressure, has permeable walls
capillary adaptations
one cell thick/wide
-1 wall layer: Tunica Intima
aorta>
arteries>arterioles > capillaries decreasing arterial pressure as total vessel volume is increased
3 types of capillary structure
continous
fenestrated
sinusoid
continuos capillary structure
continuos with endothelial cells held together by tight junctions to limit permeability of large molecules
fenestrated capillary structure
contain pores, aids absorbtion eg. in the kidney
sinusoid capillary structure
open spaces between cells + permeable to large molecules eg.liver
how does blood flow through the capillaries
very slowly and at a very low pressure in order to allow for maximal material exchange
high blood pressure is dissipated by extensive branching of vessels and narrowing of the lumen eg.o2
where are high and low hydrostatic pressure found at a capillary
high at arteriole end forcing materials into tissue
low at venuos end allowing materials from tiisue to enter bloodstream eg.co2
veins
transports bloodt at low pressure to the atria of the heart
veins specialised structure
They have a very wide lumen (relative to wall thickness) to maximise blood flow for more effective return
They have a thin wall containing less muscle and elastic fibres as blood is flowing at a very low pressure (~ 5 – 10 mmHg)
Because the pressure is low, veins possess valves to prevent backflow and stop the blood from pooling at the lowest extremities
label the structure of a vein
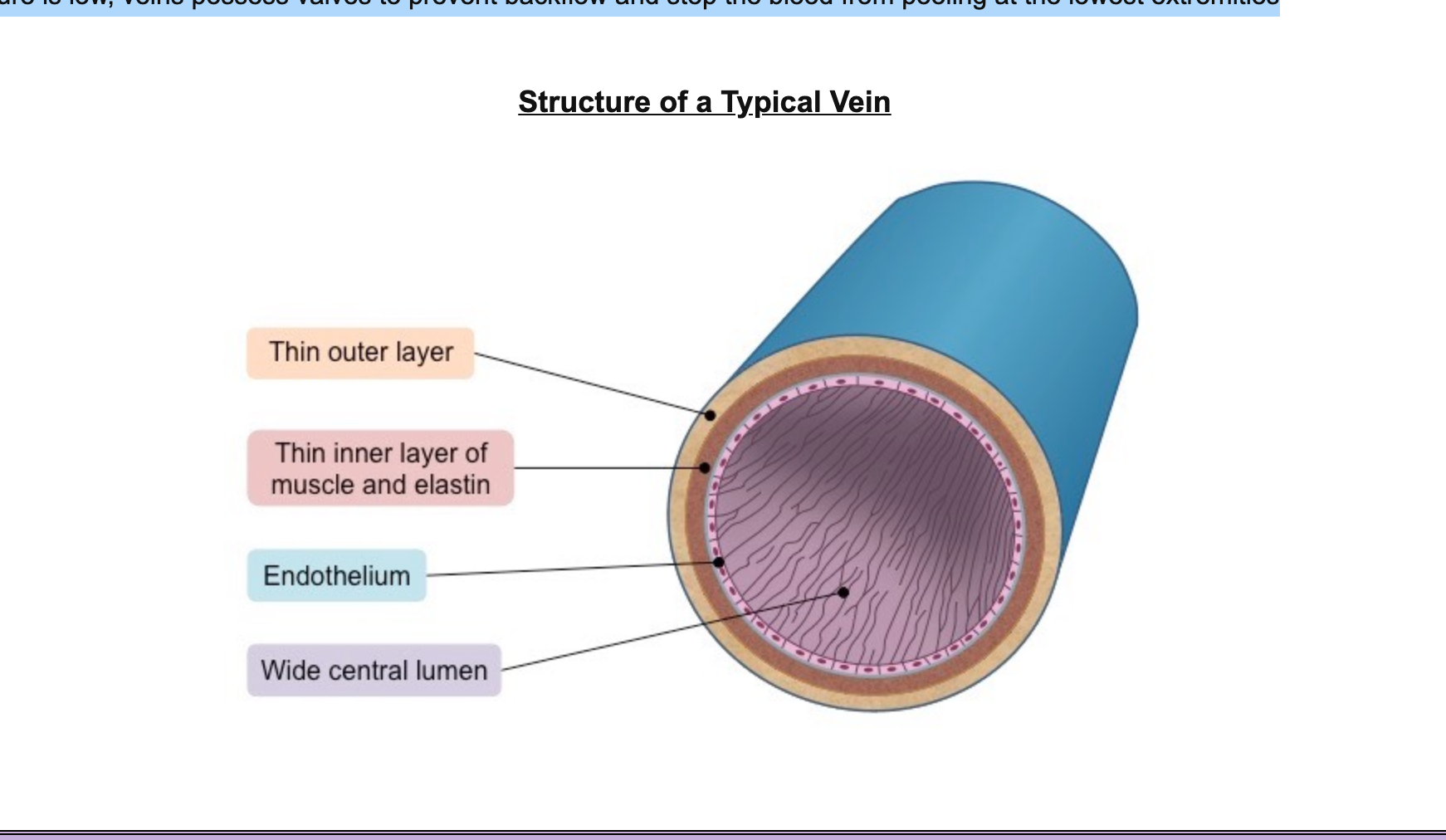
how does muscle contraction affect veins
when they contract the squeeze the vein + cause blood to flow from the site of compression increasing the rate of return of deoxygenated blood
the wall layers in arteries and veins
Tunica Adventitia
Tunica Media
Tunica Intima
identification of blood vessels
They have a very wide lumen (relative to wall thickness) to maximise blood flow for more effective return
They have a thin wall containing less muscle and elastic fibres as blood is flowing at a very low pressure (~ 5 – 10 mmHg)
Because the pressure is low, veins possess valves to prevent backflow and stop the blood from pooling at the lowest extremities
flow of blood through the heart
vena cava>right atrium>tricuspid valve>right ventricle> pulmonary valve>pulmonary artery>lungs>pulmonary vein>Left atrium> bicuspid valve>left ventricle> aortic valve> aorta
what is the heart contraction
myogenic(the signal for cardiac compression arises within the heart tissue itself)
where is the heart beat initiated
the SA node, the ‘pace maker’
what happens if the SA node fails
the AV node can maintain cardiac contractions but slower
if both fail, a final tertiary pacemaker (Bundle of His) may coordinate contractions at a constant rate of roughly 30 – 40 bpm
what happens if there is no pacemaker
cardiac cells act independently, irregular and uncordianted beats which requires defibrillation
conduction of a heart beat
an impulse is initiated in the Sa node which triggers a depolarisation that spreads across the atria causing it to contract.
it reaches the AV node where the impulse is delayed for 12s to allow filling of the ventricle.
the AV budnles carries the impluse down through the septum where they meet the purkinje fibres which carry the impulse up the wall of the ventricles causing them too contract
external signals which increase HR
nerve signals from the brain(rapid changes)
endocrine signals(more sustained changes)
blood pH or changes to blood pressure
how nerve signals affects hr
involuntary from the medulla oblongata
The sympathetic nerve releases the neurotransmitter noradrenaline to increase heart rate
The parasympathetic nerve releases the neurotransmitter acetylcholine to decrease heart rate
how hormones affect the heart
The hormone adrenaline (a.k.a. epinephrine) is released from the adrenal glands (located above the kidneys)
Adrenaline increases heart rate by activating the same chemical pathways as the neurotransmitter noradrenaline
systole
the contraction of the heart
diastole
the relaxation of the heart
atrial systole
the period when the atria are contracting
The atrioventricular valves are open as the pressure in the atria exceeds the pressure in the ventricles
The semilunar valves are closed as the pressure in the ventricles is less than the pressure in the aorta and pulmonary artery
Atrial systole happens around 0.13 seconds after ventricular systole
Atrial systole forces blood from the atria into the ventricles
ventricular systole
the period where the ventricles are contracting
The atrioventricular valves are closed as the pressure in the ventricles exceeds the pressure in the atria
The semilunar valves are open as the pressure in the ventricles exceeds the pressure in the aorta and pulmonary artery
diastole
both chamblers are relaxed
blood flows into av valves open, semilunar closed
coronary arteries
blood vessels that surround the heart and nourish the cardiac tissue to keep the heart working
if blocked will cause a heart attack
coronary occlusion(Atherosclerosis)
hardening and narrowing of the arteries due to the deposition of cholesterol
occurs when fatty deposists devlop in the artery significantly reducing the diameter of the lumen
consequently this increases pressure + damage on the arterial wall
damaged is repared with fiberous tissue(sig less elastic)
As the smooth lining of the artery is progressively degraded, lesions form called atherosclerotic plaques
If the plaque ruptures, blood clotting is triggered, forming a thrombus that restricts blood flow
If the thrombus is dislodged it becomes an embolus and can cause a blockage in a smaller arteriole
consequences of coronary occlusion
heart attack
blod clots
coronary heart disease
-treated by bipass surgery or creating a stent
risk factors for coronary occlusion
Age – Blood vessels become less flexible with advancing age
Genetics – Having hypertension predispose individuals to developing CHD
Obesity – Being overweight places an additional strain on the heart
Diseases – Certain diseases increase the risk of CHD (e.g. diabetes)
Diet – Diets rich in saturated fats, salts and alcohol increases the risk
Exercise – Sedentary lifestyles increase the risk of developing CHD
Sex – Males are at a greater risk due to lower oestrogen levels
Smoking – Nicotine causes vasoconstriction, raising blood pressure