Human Physiology Exam 3
1/148
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
149 Terms
Skeletal Muscle
Striated muscle
voluntary
Cardiac
Muscle found only in heart
Involuntary
Striated
Smooth
Organ muscle
Involuntary
Nonstriated
Skeletal Muscle
Number of muscle fibers bound by connective tissue
Muscle fiber is a muscle cell
Linked to bones by tendon
Components of Skeletal muscles
Sarcolemma
Sarcoplasm
Myofibrils
Myofibrils
Contractile elements of muscle fiber
Composed of myofilaments
Myosin
Thick filaments
Heads form cross bridges between thick and thin filaments
Actin
Thin Filament
Contractile filament
A Bands
Lots of Myosin
Dark Bands
I Bands
Light Bands
No myosin
Motor unit
Single motor neuron and all the muscle fibers it innervates
Innervates more than just 1 muscle fiber
Motor end plate
Area of the muscle fiber sarcolemma where a motor neuron stimulates skeletal muscle
Neurotransmitter: Acetylcholine
Sarcomere
Functional unit of contraction
Between 2 Z-discs
Regions: A band, H zone, M line, I band
Myosin Heads
Actin binding site
ATP Bind site
ATPase
Tropomyosin
Resting, covers myosin binding sites blocking interaction
Blocks binding sites on actin for myosin
Troponin
Made of 3 units
Binds to tropomyosin
Binds to actin
Binds with Ca2+
Calcium binds to troponin to move it to allow binding
Sliding filament Mechanism
Contraction is accomplished by thin filaments from opposite sides of each sarcomere sliding closer together between thick filaments
Power Stroke
Sliding filament mechanism
Attachment of a myosin cross bridge to a thin filament
Swiveling of myosin head = power stroke
Detachment of the cross bridge from the thin filament
Reattach to a new actin biding site
Repeat cycle
Cross Bridge Cycle
Asynchronous power stroke of myosin heads
Functions of ATP in Contraction
Energizes X-bridge, providing energy for power stroke
Binding of ATP relaxes muscle
Ca+
the Link between excitation and contraction
During cross bridge cycling
Excitation-Contraction Coupling
At rest low calcium intracellular
-Stored in sarcoplasmic reticulum (intracellular storage)
Increases in intracellular Ca++ leads to contraction
-Release from SR
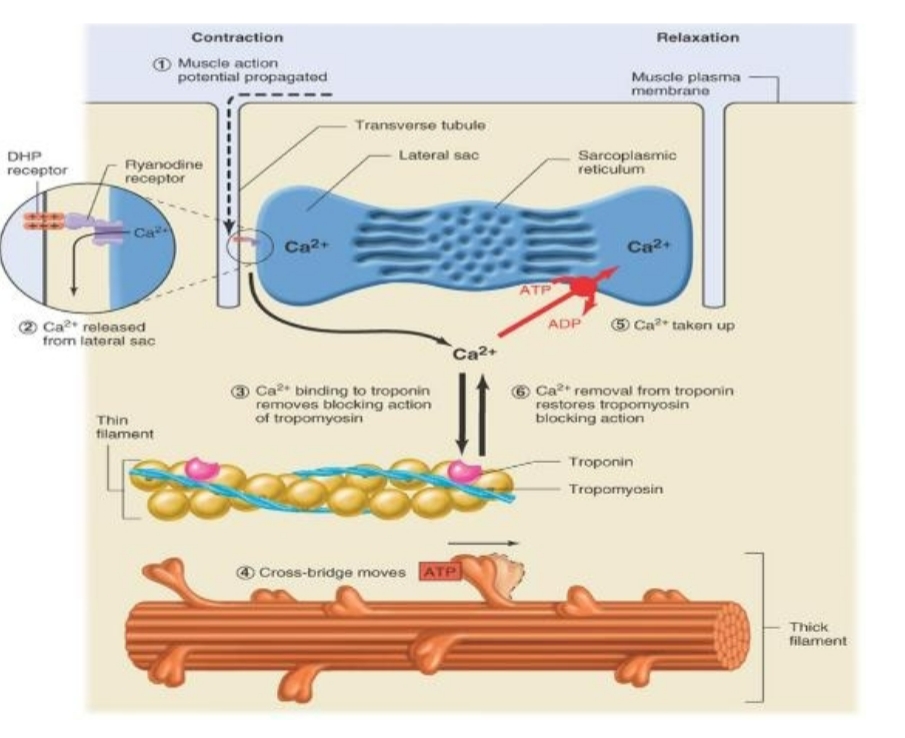
SR calcium Release
AP propagated into interior by transverse tubules
Voltage gated Ca++ channels in SR
Release of Ca++ from sarcoplasmic reticulum
Binds to Troponin to move Tropomyosin
Neural Activation
Leads to muscle contraction
AP travels down somatic motor neuron axon to axon terminal
Exocytosis of ACh
ACh binds to nicotinic ACh receptors and opens them
End Plate Potential
Induces AP in sarcolemma of muscle fiber
AP results in release of Ca2+ inside muscle fiber
Muscle Relaxation
AP stops
Active reuptake of Ca2+ into SR
Ca++ ATP pump
ATP need
Splitting of ATP by mosin ATPase provides energy
Tension
Force exerted on an object by contracting muscle
Load
Force exerted on the muscle by weight of the object
Twitch
Response of a single muscle fiber to a single AP
Latent period - takes time for everything to get triggered and stimulated to move
Contraction Time
Relaxation Time
Muscle contractions
Force Velocity Curve
For muscles to contract, they must generate force that is greater than the opposing forces
The greater the force, the slower the contraction
Isotonic Contraction
Change in muscle length
Concentric and eccentric
Concentric Contraction
Muscle Shortens
Eccentric
Muscle lengthens
Isometric
Muscles can’t shorten because the load is too great
Can be voluntary
Nervous System
Muscle tension Control in skeletal muscle
Frequency of Stimulation
Motor Unit Recruitment
Muscle
Muscle tension control
Properties of skeletal muscles control tension
Frequency of Stimulation
Because a muscle twitch is fairly slow compared to an action potential many action potentials can arrive before a single twitch is completed
Generation of a force that is greater than a single twitch
Summation
Muscle summation
Muscle is stimulated again before relaxation leads to summation
Tetanus
Contraction is usually 3-4 greater than a single twitch
Max contraction of a muscle releasing max calcium
Summation of many action potentials (lots of calcium being released)
Summation
Increase of AP frequency
How many muscle fibers in each motor unit
High Variation in number of muscle fibers in each motor unit
Precise delicate movements and course powerful movements
Motor Unit Recruitment
Increasing the number of active motor units
Increase tension
Increase velocity to lift a given load
Increasing Tension in Skeletal muscles
In nervous system: frequency of stimulation and motor unit control
In skeletal muscle: Length of fiber at onset of contraction, type of skeletal muscle, extent of fatigue, x-sectional of fiber
Length of Fiber at onset of contraction
Length-tension relationship
Overlap of Actin over myosin - lower tension
Overextension of muscle - lower tension
Optimal Overlap of actin over myosin - Maximal amount of tension
Skeletal Muscle Energy Metabolism
Big energy demand for ATP
-Myosin ATPase and Ca++ pump
Small supply of stored ATP
Formation of ATP by muscle
Creatine phosphate
Oxidative phosphorylation
Glycolysis
Creatine Phosphate
Utilized at onset of contractile activity
Limited by CP stores
Stores used initially in seconds
Types of Skeletal Muscle Fibers
Based on
Maximal velocity of shortening
Major pathway used to form ATP (oxidative or glycolytic)
All 3 types are represented in a typical skeletal muscle
All muscle fibers in a single motor unit are the same fiber type
3 Types of skeletal muscle fibers
Slow-oxidative (type 1)
Fast-oxidative Glycolytic (type 2a)
Fast-glycolytic (type 2x)
Activates from type 1 → type 2a → type2x based on increasing resistance
Muscle characteristics
Speed of Contraction - fast twitch fibers (type 2)
Fatigue resistance - endurance fibers (type 1)
Myoglobin Content - type 1 fibers
Mitochondria - type 1 fibers
Oxidative Phosphorylation Capacity - type 1
Enzymes - type 2
Glycogen content - type 2
Size Differences - strength differences
Fatigue
Decline in muscle tension as a result of previous contractile activity, even though stimulation continues
Dependent on Type of skeletal muscle, intensity/duration, and individual fitness
Muscle Fatigue Factors
Internal acidity
K+ accumulation
Glycogen Depletion
Reduced SR calcium release
Central fatigue
Skeletal Muscle Tension Factors
Frequency of stimulation
Length of fiber at onset of contraction
Extent of fatigue
Cross-sectional area of skeletal muscle
Peak force production is related to the physiological cross-sectional area
Adaptation to Endurance Training
Type 1 Fibers
Increased ability to use fatty acids as fuel and increased intracellular triglyceride storage
Increase capillary density
Increase in number of mitochondria
Increase in Krebs cycle enzymes
Muscle does not change in size
Adaptation of Skeletal Muscle
Resistance training promotes hypertrophy of fast glycolytic fibers
Skeletal muscles atrophy when not used
Control of Motor Movement
Input from primary motor cortex
Input from brain stem
Input from afferent neurons
Muscles need sensory feedback from muscles for optimal function
Muscle spindles
Golgi tendon organs
Muscle spindle
Parallel to extrafusal muscle fibers
Contains intrafusal muscle fibers
Innervated by gamma motor neurons
Function to sense muscle length
Sensory Info from Muscle Spindles
Purpose is to resist tendency for passive stretch of muscles by gravitation forces when a person is upright
Stretch of muscle - increases firing leads to contraction of muscle
Intrafusal
Muscle spindles own muscles
Gamma motor neuron
Muscle spindles own nervous supply
Alpha-Gamma Co-activation Alpha and Gamma motor neurons activate extrafusal and intrafusal respectively.
Patellar knee-jerk reaction
Muscle spindles mediate this
Golgi Tendon Organs
Found in Tendons
Senses muscle tension
Inhibitory synapses on motor neurons of the contracting muscle
Excitatory synapses on motor neurons of ipsilateral antagonists
Cardiac and Smooth Muscles
Involuntary
Regulated by autonomic nervous system
Contraction is due to myosin/actin cross bridges
Stimulated by rises in intracellular calcium
Cardiac Muscle
Striated
Myosin and actin filaments form sarcomeres
Contraction occurs by means of sliding thin filaments
Unlike skeletal muscle fibers, these fibers are connected via gap junctions found at intercalated discs
Myocardium
A mass of cardiac muscle cells connected to each other via gap junctions
Action potentials that occur at any cell in a myocardium can stimulate all the cells in the myocardium
It behaves as a single function unit
Smooth Muscle
Found in walls of hollow organs and tubes
No striations - Not arranged in sarcomere pattern found in skeletal and cardiac muscle
Spindle-shaped cells with single nucleus
Muscle cells usually arranged in sheets
Smooth Muscle Layers
Thick Myosin Filaments
Thin actin filaments - Contain tropomyosin but lack troponin
Intermediate filaments
Intermediate Filaments
Do not directly participate in contraction
Form part of cytoskeletal framework that supports cell shape
Single unit smooth muscle
Cells electrically linked by gap junctions
act as one unit
Multiunit smooth muscle
Units must be separately stimulated by nerves to contract
Excitation contraction coupling in smooth muscle
Begins with rise in intracellular calcium concentrations
Small amounts come from Sarcoplasmic Reticulum
Most by extracellular following opening of voltage gated calcium channels
Action of Calcium in E-C Coupling
Calcium binds to calmodulin
Activates myosin light chain kinase (MLCK)
MLCK phosphorylates myosin light chains
Phosphorylated myosin forms cross bridges with actin to initiate contraction
Cardiovascular system
Consists of Blood, Heart, and blood vessels
Blood
Transport medium (cells suspended in fluid)
Represents about 8% of total body weight
Average blood volume = 5L
Consists of Erythrocytes, Leukocytes, Platelets, Plasma
Erythrocytes
Red blood cells
Contains hemoglobin for o2 transport
No nucleus or organelles
Biconcave discs - provides larger surface area for diffusion of O2
Flexible membrane - Allows RBCs to travel through narrow capillaries without rupturing
Leukocytes
White blood cells
Platelets
Cell fragments
Lack nuclei
Have organelles
Function in hemostasis
Come from megakaryocyte cells
Also called Thrombocytes
Plasma
90% water
7-9% proteins
Maintain osmotic pressure of blood
Lipid transport
Immunity - Antibodies
Clotting factors
Various enzymes
Erythropoiesis
Erythrocyte product
RBCs survive about 120 days
Spleen removes most of old erythrocytes
Replaced at rate of 2-3 million cells per second
Occurs in bone marrow
Multipotent
Signaled by Erythropoietin
Anemia
Refers to a below-normal O2 carrying capacity of the blood
Caused by dietary deficiencies, blood loss, bone marrow failure, hemolytic anemia
Thrombopoietin
Hormone produced by liver increases number of megakaryocytes and therefore increases platelet production
Hemostasis
Prevents blood loss from a broken blood vessel
Vascular spasm
Formation of a platelet plug
Blood coagulation
Vascular spasm
Reduces blood flow through a damaged vessel
Formation of a platelet plug
Platelets aggregate on contact with exposed collagen in damaged wall of the vessel
Platelets release ADP which causes surface of nearby circulating platelets to become sticky
Blood coagulation
Clotting
Coagulation proteins in blood activate
Platelets at Rest
Inhibited by prostacyclin, and nitric oxide
Formation of platelet plug
Activate clotting factors
Clot Formation
Reinforces platelet plug by formation of clot
Clotting factors are always present in blood plasma in inactive precursor form
Vessel damage that exposes collagen initiates cascade of reactions that involve successive activation of clotting factors
Converts fibrinogen → Fibrin
Intrinsic Pathway
Blood clot formation
Activated by exposed collagen
Extrinsic Pathway
Blood clot formation
Released from damaged formation - Tissue Factor
Fibrinogen
Turns into fibrin during blood clot formation
Leukocytes
White blood cells
Mobile units of body’s immune defense system
Immune system, recognizes and destroys or neutralizes materials within body that are foreign to normal self
Defends against invading pathogens
Identifies and destroys cancer cells that arise in body
Functions as a cleanup crew that removes worn out cells and tissue debris
Heart Structure
Hollow, Muscular organ
Located in thoracic cavity
4 chambers (2 atria and 2 ventricles)
Pumps constantly - variable rate
Pulmonary (right) and systemic (left) blood circuits
Heart valves
Atrioventricular valves from atria to ventricles
Semilunar valves
Used to prevent backflow of blood in heart
Sounds are called murmurs - heart valves closing and opening
Heart Valve Opening
When pressure is greater behind the valve, it opens
Atrium → AV valve → Ventricle → Aortic or Pulmonary Semilunar valve → Aorta or pulmonary system
Heart Valve Closed
When pressure is greater in front of the valve it closes. Note that when pressure is greater in front of the valve, it does not open in the opposite direction, that is, it is a one-way valve
Blood Flow in Heart
Deoxygenated blood enters right side through vena cavae
→right atrium → right AV valve → right ventricle → pulmonary semilunar valve → pulmonary trunk and arteries → lungs (pulmonary circuit)
Cardia Cycle
Consists of 2 phases
Systole - Ventricles Contract, Atria Relaxed
Diastole - Ventricles fill and relax, Atria contract for a portion of Diastole phase
Systole
Isovolumertric contraction
Ejection
Sequence of events
Isovolumetric contraction
Ventricles contract, but no blood ejected
Blood pressure rises above pressure in atria
Atrioventricular valves shut
Semilunar valves shut
Ejection
Blood pressure in ventricle exceeds pressure in arteries
Blood flows out of ventricles, causing pressure in ventricles to fall