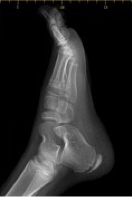
3.4 - peds orthopedics 2
1/80
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
81 Terms
arthrogryposis multiplex congenita
_______________ is a condition that is described as a non-progressive neuromuscular syndrome that is present at birth with severe joint contractures of 2 or more body areas that are present at birth
amyoplasia (**most recognized)
central nervous system (not compatible with life)
heterogeneous
what are the 3 types of arthrogryposis multiplex congenita?
which is the most common?
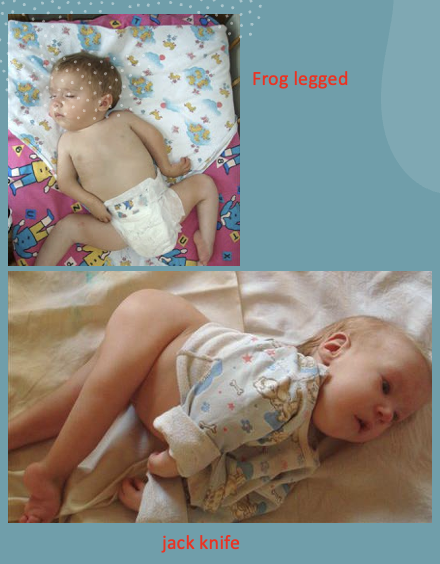
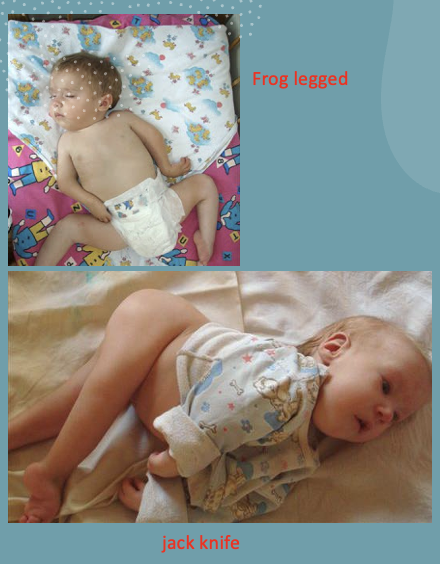
frog legged
jack knifed
what are the 2 presentations of arthrogryposis multiplex congenita
T
T/F: clubfoot is common in BOTH frog legged and jack knifed positions of arthrogryposis multiplex congenita

knee extension
hip IR and adduction
what is the presentation of jack knife position in arthrogryposis multiplex congenita
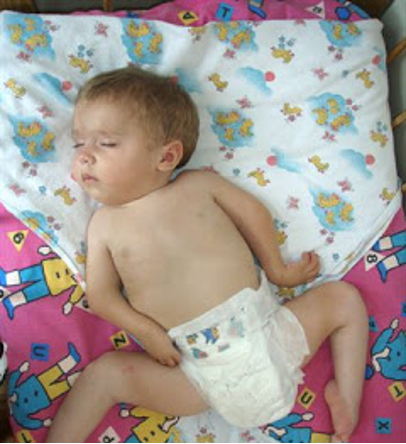
hip abduction and ER
what is the presentation of frog legged position in arthrogryposis multiplex congenita
contractures
muscle weakness
fibrosis
what are the 3 body structure and function abnormalities associated with arthrogryposis multiplex congenita
fetal akinesia (lack of movt in whomb) or possible insult during first trimester (hyperthermia, infection, vascular compromise, uterine fibroids and septum in uterus, fetal crowding, decreased amniotic fluid)
what is the etiology of arthrogryposis multiplex congenita
osteogenesis imperfecta
_______________ is a condition that is described as brittle bone disease
11; 1
PT = 1, 3, 4, 5, 6, 11, mild 7
there are ________ types of osteogenesis imperfecta, type _______ is the most common
which types are appropriate for physical therapy?
FALSE!!!!!!!!!! DO NOT STRETCH THEM THEY WILL BREAK
T/F: passive stretching is effective for treating a child with osteogenesis imperfecta
C5-6
what nerves does erb’s palsy affect?
C5-T1
what nerves does global palsy affect?
T1 - sympathetic ganglion
what nerves does horner’s syndrome affect?
C8-T1
what nerves does Klympke’s palsy affect?
waiters tip
erb’s palsy is also called ___________
klympke’s
does erb’s palsy or klympke’s have more shoulder innervation?
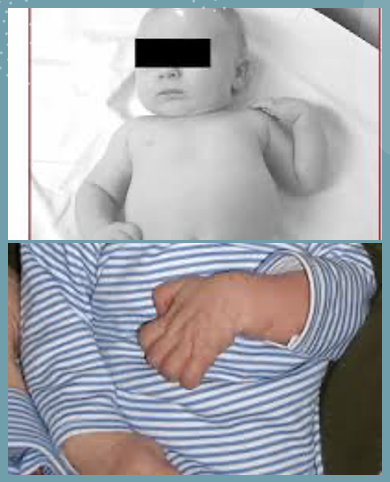
erb’s palsy (note the shoulder IR)
what neurological injury is this picture demonstrating?

1mm/day
what is the rate of nerve growth?
klumpke’s palsy
what neurological injury is this picture demonstrating?
long
neonatal brachial plexus injuries are more common when labor is (short or long)
high
neonatal brachial plexus injuries are more common when the birth weight is (low or high)
brachial plexus and hip dysplasia
breech deliveries often cause _____________ and _____________ injury

active movement scale (AMS)
the ________________ test is used to assess upper-extremity motor function in infants and children with obstetric brachial plexus palsy (OBPP)

birth to 3
what age range does the active movement scale apply to

0
4
7
grading for Active Movement Scale (AMS)
a score of ______ is no contraction
a score of ______ is full motion gravity eliminated
a score of ______ is full motion against gravity
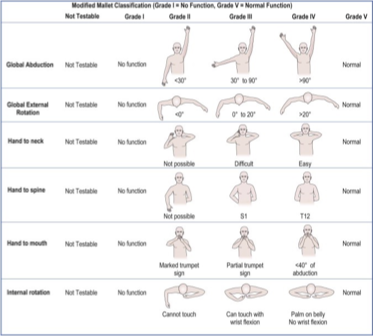
3+ years
what age range does the mallet’s classification of function apply to
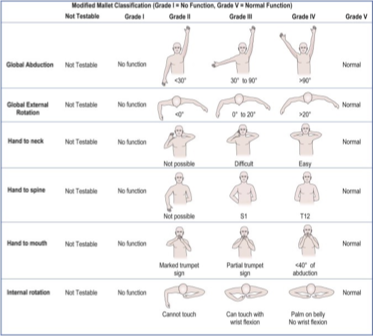
5
1
grading for the mallet’s classification of function:
grade ______ is normal
grade ______ is no function
FLACC
what test would you use to assess an infant’s pain
torticollis
hip dysplasia
what are 2 conditions can co-occur with a brachial plexus injury
left
female
first born
developmental dysplasia of the hip:
more likely for left or right
more likely for female or male
more likely for first born or siblings
breech delivery
+ family history
post-maturity birth
increased weight
likelihood factors of hip dysplasia (4)
torticollis
hip dysplasia
what other conditions are likely to be present with a brachial plexus injury
torticollis
metatarsus adductus
what other conditions are likely to be present with a hip dysplasia injury
< 4 months
ultrasound is the gold standard for diagnosing hip dysplasia if the child’s age is ____________
ultrasound (if under age 4 months)
______________ is the gold standard for diagnosing hip dysplasia
4-6+ months
radiographic imaging for hip dysplasia is for if the child’s age is __________
barlow (pop hip out, “bar” = we going out)
ortolani (go back in)
what are the special tests for hip dysplasia
barlow (the “dislocate”/”out” part of the test)
when conducting the hip dysplasia tests, the ____________ test puts the babies legs in an adducted position and applies a mild posterior force
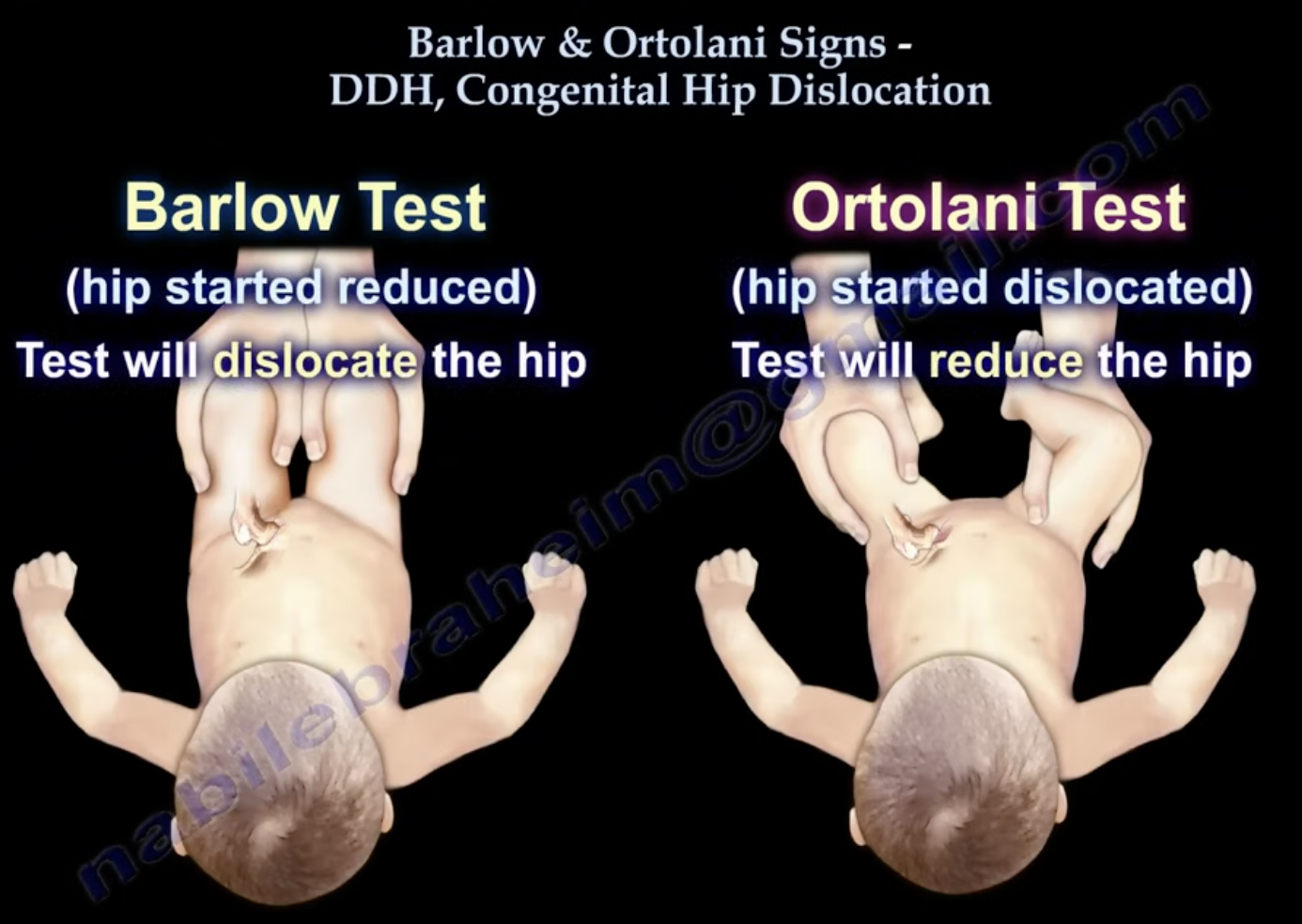
ortolani
when conducting the hip dysplasia tests, the ____________ test puts the babies legs in an abducted position to reduce the hip
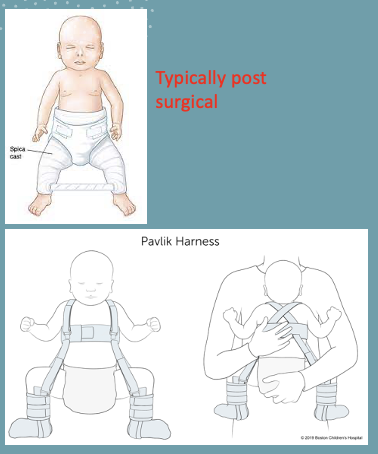
spica cast; pavlik harness
______________ or _____________ can be applied to help correct hip dysplasia
flexion, abduction, ER; 23hrs/day
the casting to correct hip dysplasia puts the hip in a _____________ position and wear for __________ amount of time
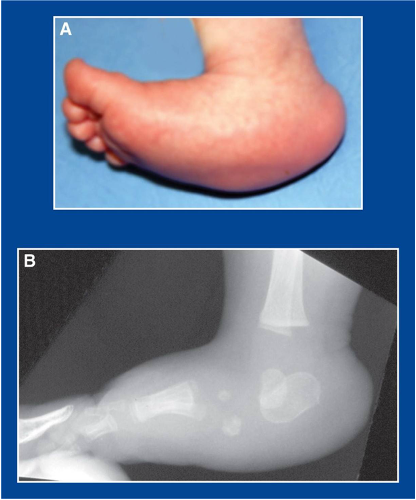
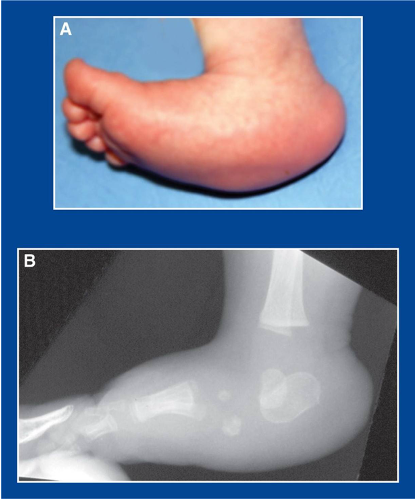
clubfeet/talipes equinovarus
what condition?
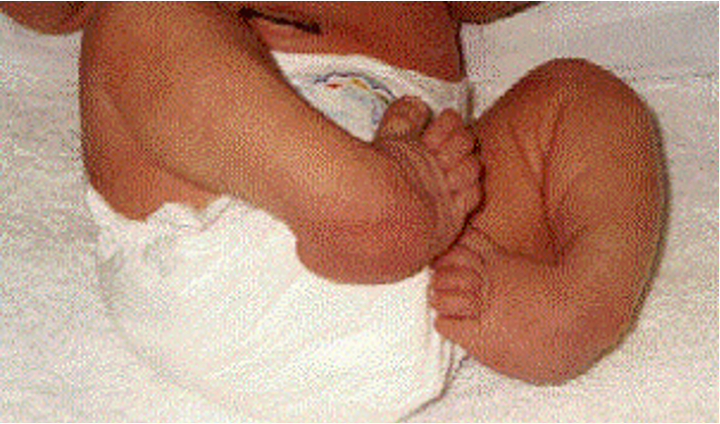
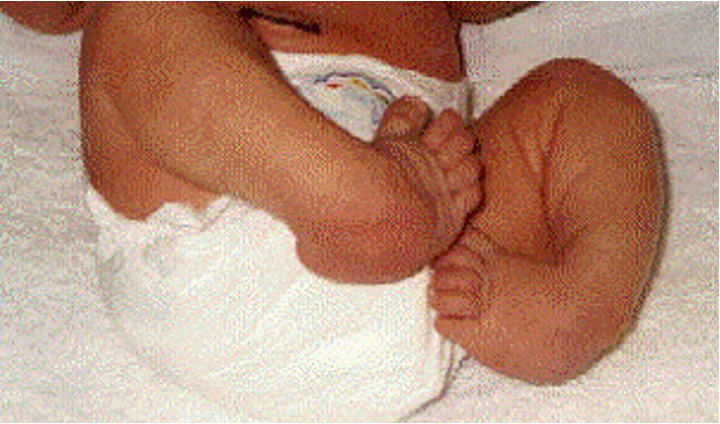
talipes equinovarus
clubfeet is also called ________________
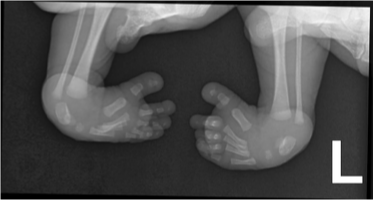
adductus
varus
equinus (limited dorsiflexion)
positioning of club feet/talipes equinovarus:
forefoot ____________
hindfoot ____________
ankle ______________
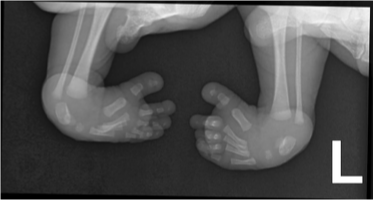
thickened
hypoplastic
small (flattened superior surface)
downward and medial
affected structures in club feet/talipes equinovarus:
ligaments: ______________
muscles: ______________
talus: ______________
navicular: ______________
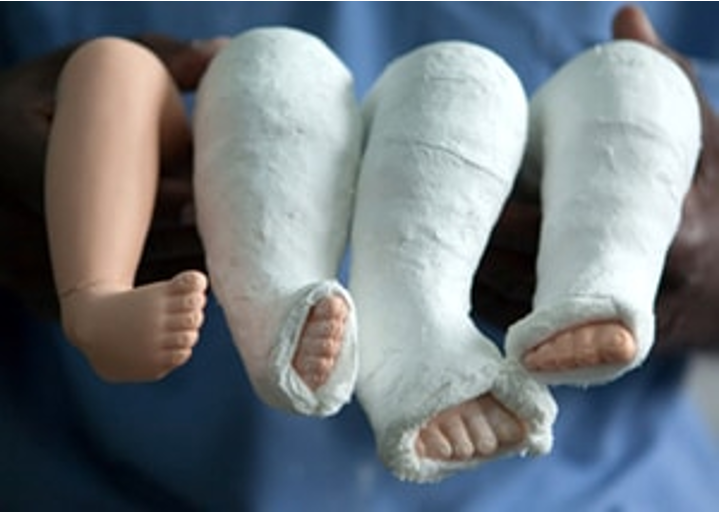
ponseti
_______________ casting is used to help correct clubbed foot
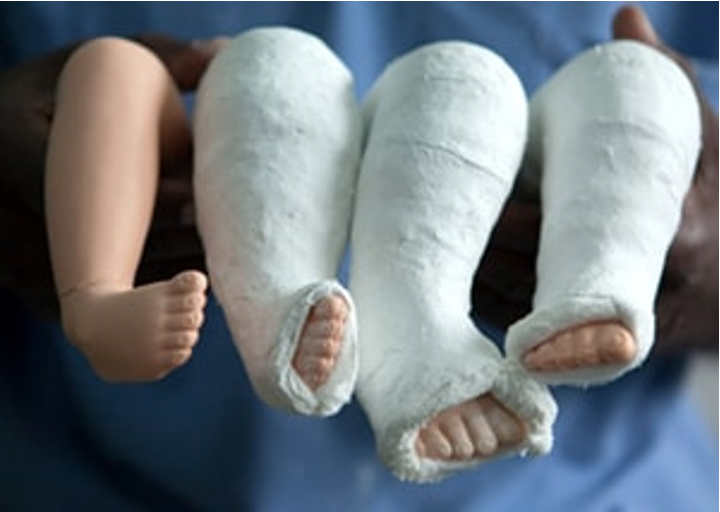
forefoot (correct one plane at a time)
the first stage of ponseti casting to correct club feet/talipes equinovarus would be correcting the ____________ part of the foot
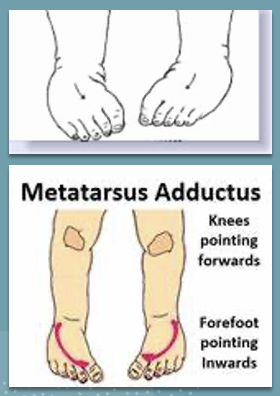
medial
metatarsus adductus is a (medial or lateral) forefoot curve
intrauterine
anterior tibialis; posterior tibialis
cuneiform
club foot
contributing factors for metatarsus adductus:
______________ positioning
different insertion point for ________ and ________ muscles
abnormal ____________ shape
_______________
1
grade _________ metatarsus adductus:
mild, flexible, can correct beyond midline
2
grade _________ metatarsus adductus:
moderate, can correct to midline
3
grade _________ metatarsus adductus:
severe, cannot correct to midline
casting
surgery (if child is 4+ years)
what are the invention options for metatarsus adductus
T
T/F: flat foot usually does NOT need treatment
flat foot
which has less problems:
flat foot or high arch
DF
calcaneal valgus is excessive (DF or PF)
laterally
the forefoot in calcaneal valgus is curved (medially or laterally)
varus
clubbed feet is calcaneal (valgus or varus)
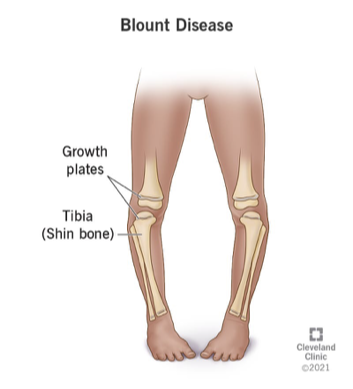
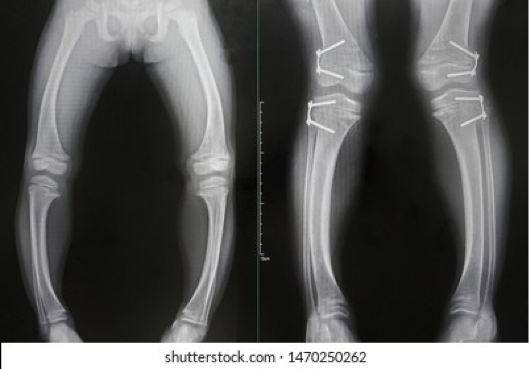
vara; medial
in blount’s disease, there is tibia _______ and (medial or lateral) growth plate dysfunction
D
rickets disease is a vitamin ________ deficiency

C
scurvy is a vitamin ______ deficiency

scurvy
signs/sx of ___________ disease:
joint pain
swollen and bleeding gums
petechial hemorrhaging
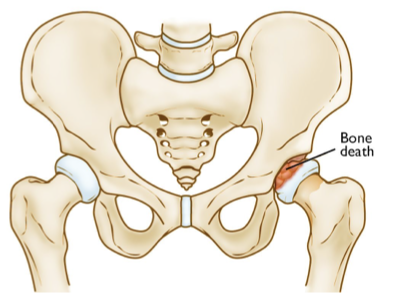
legg-calve perthes
_______________ is avascular necrosis of the hip in childhood
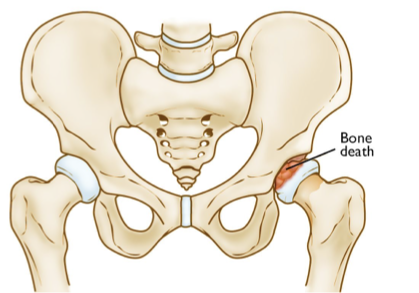
epiphyseal plate
legg-calve perthes is decreased blood to the ______________
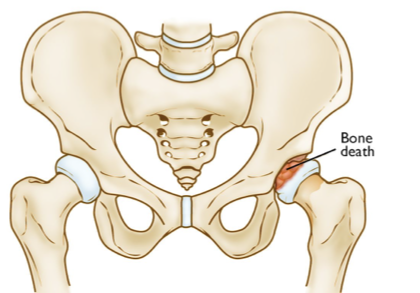
3-12
5-7
legg-calve perthes occurs from ages _____-_____ but is most common from ages ______-_____
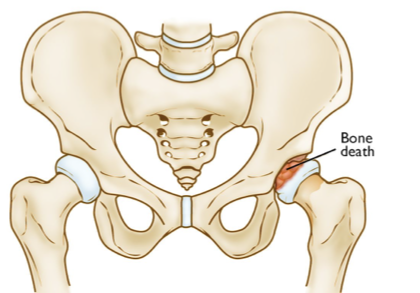
males
legg-calve perthes occurs more in (females or males)
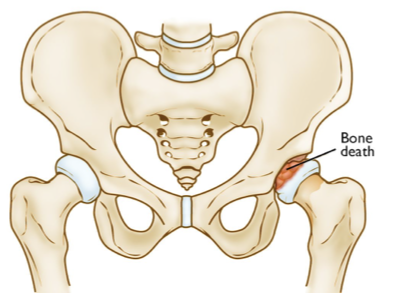
T
T/F: maternal smoking and secondhad smoke can play a factor in a child developing legg-calve perthes

it’s the same but legg-calve perthes is non-weight bearing
what’s the difference in hip dysplasia and legg-calve perthes casting
less than 6
if the a child has legg-calve perthes and they are age ________, conservative treatment is recommended
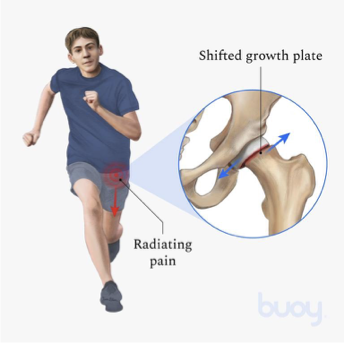
F
T/F: Slipped capital femoral epiphysis is more common in females
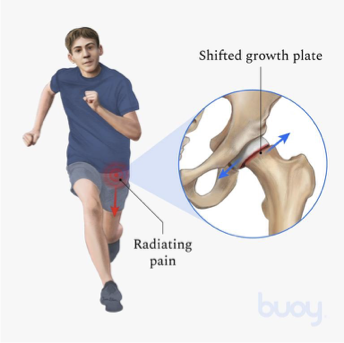
peri-puberty
males = 10-16
females = 10-14
what age does slipped capital femoral epiphysis typically occur in males and females
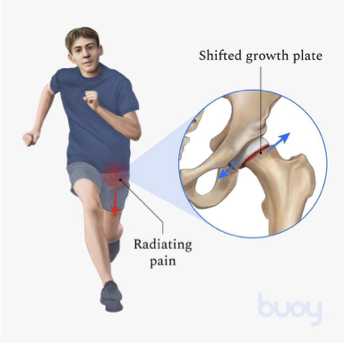
flexion and IR
someone with slipped capital femoral epiphysis will have decreased ROM in…..
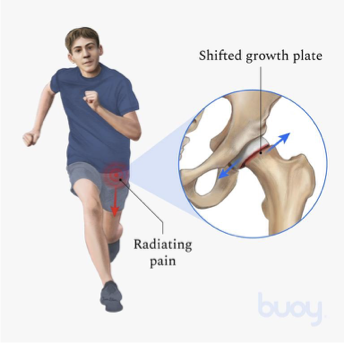
PT
surgical pins
treatment options for slipped capital femoral epiphysis
covex
scoliosis is labeled via the __________ side
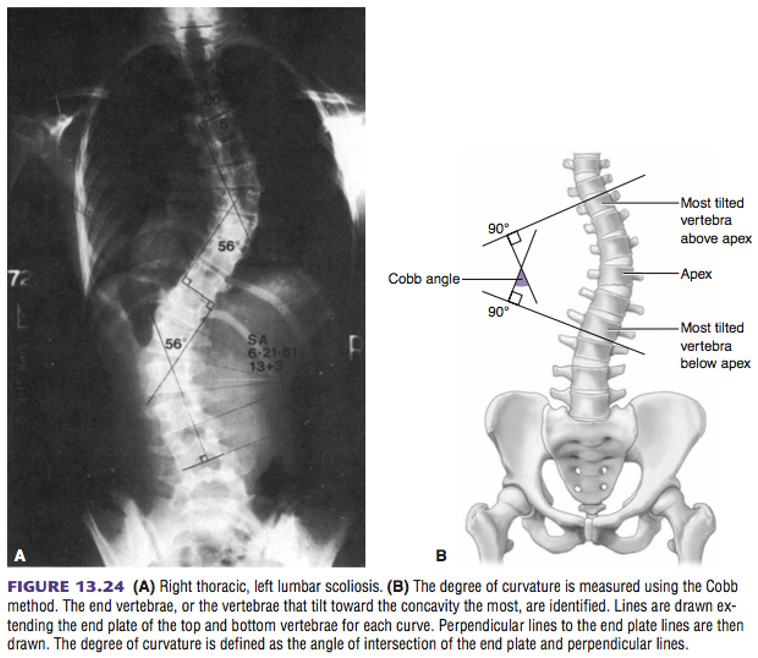
cobb angle
the _____________ is used to measure the angle of scoliosis
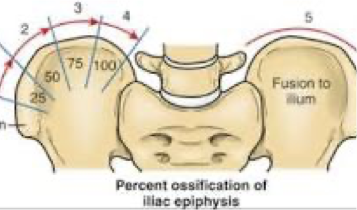
risser’s sign
________________ is a radiographic grading system that assesses skeletal maturity by measuring the ossification and fusion of the iliac crest apophysis on a pelvic X-ray which is used to test for scoliosis
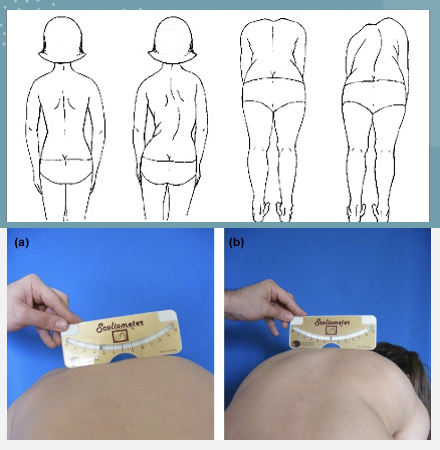
presence of structural scoliosis
what does the forward bending test asses
schroth
the _____________ technique is used to treat scoliosis and it involves stretching the concave side and strengthening the convex side
osgood schlatters
what condition?
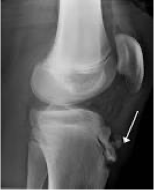
severs
what condition?