Migraine- Khan
1/38
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
39 Terms
What are the 2 types of migraines?
HA with aura (what is aura? pt. sees spots, feels pins/needles, weakness, aphasia)
HA without aura
What are the 2 phases to the VASCULAR component of migraines?
1st phase: VASOCONSTRICTION (cerebral vasoconstriction and ischemia)
2nd phase: VASODILATION (cerebral vasodilation and pain)
During the 1st phase of a migraine, _________________ is released from CNS neurons and platelets.
serotonin
The NEURO component of migraines includes activation of WHAT system?
trigeminal nerve system (carries pain signals from blood vessels and meninges surrounds brain relayed through trigeminal nucleus (brainstem)—> thalamus+ sensory cortex)
What transmitters are released during pain signaling?
CGRP
glutamate
substance P and K
serotonin
What is CGRP and what is it’s role in migraines?
CGRP= calcitonin-gene related peptide
deals with vasodilation and inflammation
CGRP produces its effects through what receptors?
G protein coupled calcitonin-like receptor and RAMP1
What effect does serotonin in migraines?
vaso__________
may inhibit _____________ and ____________ activity
effects ________ muscle to…
vasoconstrictor
may inhibit calcium channels and glutamate/ CGRP activity
effects smooth muscle —> enhances platelet aggregation, NT in the CNS
What serotonin receptors are involved in migraines? What type of receptor are they?
5-HT1B and 5-HT1D —> GPCRs
Describe the biosynthesis of serotonin:
_________________—>_______________—> serotonin
What enzymes are involved?
L-tryptophan—> 5-hydroxytryptophan—> serotonin
enzymes: tryptophan hydroxylase, aromatic AA decarboxylase
What’s the difference between prophylaxis and abortive drugs for migraine treatment?
FYIIIIIIIII (for understanding)
Prophylaxis: reduce frequency and severity of attacks
Abortive: used for reversing, aborting attacks, reducing pain and others
What drugs are used for migraine PROPHYLAXIS tx?
tricyclic antidepressants
anticonvulsants
antihypertensives
CGRP antagonists
CGRP antibodies
What drugs are used for migraine ABORTIVE tx?
Serotonin agonists (-triptans, -ditans)
Ergot derivatives
NSAIDs
CGRP receptor antagonists
Preferred tricyclic antidepressant for migraine prophylaxis?
amitriptyline
What anticonvulsants can be used for migraine prophylaxis?
valproic acid/ divalproex
topiramate
BBW of valproic acid/ divalproex?
BBW for hepatotoxicity and teratogenicity (neural tube defects, Cat X)
What antihypertensives are preferred for migraine prophylaxis? alternatives?
preferred: b-blockers (propranolol, metoprolol)
alternatives: lisinopril, verapamil
List of the CGRP antagonists used for migraine prophylaxis and abortive tx?
atogepant- only prophylaxis
rimegepant- both
ubrogepant- only abortive

What antibodies are used for migraine prophylaxis? what is their target?
eptinezumab
galcanezumab
fremanezumab
erenumab
target: CGRP antibodies
List the “-triptans”
more of an FYI, not technically in SG
sumatriptan
zolmitriptan
naratriptan
rizatriptan
eletriptan
frovatriptan
almotriptan
Triptans are ____________ agonists.
a. histamine
b. CGRP
c. serotonin
d. glutamate
c.
What are the 2 MOAs of the “-triptans” (ex: sumatriptan)?
results?
activates 5-HT1D/1B receptors in cerebral blood vessels
results: produces VASOCONSTRICTION, inhibits vasodilation to the HA
stimulates presynaptic 5-HT1D/1B receptors
results: inhibits release of pro-inflammatory neuropeptides that cause vasodilation, inflammation, and pain
What are the warnings and precautions of the triptans?
warning: rare but serious CV events (ischemia, MI, arrhythmias)
precaution: increased risk of serotonin syndrome
What 2 triptans have a SLOWER onset and LONGER duration of action compared to the others form the class?
Frovatriptan and naratriptan
What are the ADRs and CONTRAINDICATIONS of the triptans?
ADRs
Paresthesia (tingle/numb)
seizure (suma)
tightness of pressure in neck and chest
route specific ADRs
C/Is
CV—> IHD, uncontrolled HTN, PVD, angina, arteriosclerosis
Cerebrovascular—> TIA, stroke
SEVERE liver/ kidney disease
concurrent MAOI therapy within 2 weeks (suma, riza, zolmi)
What is serotonin syndrome?
What are the 3 major categories?
List the symptoms for each category?
Serotonin syndrome—> triad of symptoms
cognitive: agitation, confusion, hypomania, insomnia, hallucinations
neuromuscular, sweating, fever, diarrhea
somatic/neuromuscular: tremor, hyperreflexia, rigidity, akathisia
WHAT ARE THE 3 IMPORTANT REGIONS in the SAR of triptans?
Core (indole)—> required for activity
Group at position 3—> required (substituted amines preferred), may influence at metabolism
Group at position 5—> enhance activity/selectivity
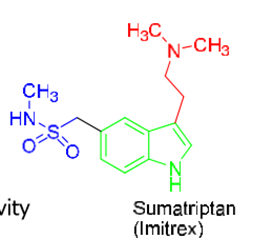
How do modifications at position 3 and 5 do to the activity of triptans?
mod at pos 3: sub of alkyl amines prolongs duration of action
mod at pos 5: sub or addition of heterocycles enhances bioavailability
List the drugs that are ergot derivatives:
ergotamine
dihydroergotamine
List the receptors that ergot derivatives MAY act on:
a-adrenergic receptors (antagonists/partial agonists)
5-HT receptors (partial agonists)
dopamine receptors (partial agonists)
What are the symptoms of chronic ergot toxicity
“Saint Anthony’s Fire”—> Painful convulsions, mania/psychosis, hallucinations, n/v, vasoconstriction/gangrene
What are the contraindications and precautions with ergot derivatives?
SAME C/I as triptans (vascular disease, severe renal/hepatic disease)
C/I with strong CYP3A4 inhibits (life-threatening peripheral ischemia)
PREGNANCY X (avoid)
avoid with other vasoconstrictors
What is the chemical difference between ergotamine and dihydroergotamine?
identical except for double bond placement
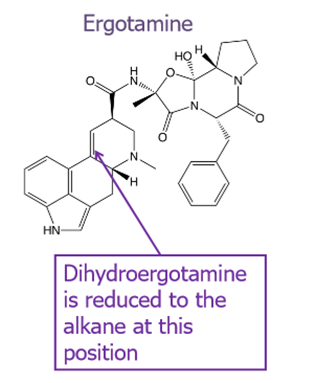
What is the ROA of each of the ergot derivatives?
ergo: oral tablet, suppository
dihydroergo: IM, SQ, IV, or nasal
CYP___ is involved in the metabolized of ergot derivatives.
3A4
What is the role of caffeine in Cafergot (brand name of Ergotamine)?
caffeine enhances absorption (remember low oral bioavailability)
What OTC agents can be used for prophylactic and abortive therapy in migraines? examples?
NSAIDs and APAP
(ex: aspirin, ibuprofen, naproxen)
What is the only NSAID that’s an OTC product that has an indication for migraines?
Excedrin migraine
How is Lasmiditan different from the triptans?
Lasmiditan—> selective 5-HT1F agonists and does NOT cause vasoconstriction
Triptans—> 5-HT1D/1B agonists and causes vasoconstriction and inhibits release of pro-inflammatory neuropeptides