Lecture 38 (Introduction to Itchy Pattern Recognition)
1/25
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
26 Terms
1. folliculitis
2. pododermatitis
3. yeast dermatitis
4. otitis
5. pruritus (allergy)
6. autoimmune skin disease
7. nonpruritic alopecia
8. keratinization defects
9. lumps, bumps, and draining tracts
10. weirdopathies
what are the core 10 patterns in dermatology?
miliary dermatitis
what type of dermatitis is this?

21-30 days
how long is the typical epidermal turn-over time?
stratum corneum
what is the major physical barrier layer of skin?
-keratinocytes (corneocytes) → these are dehydrated, flattened skin cells that form the "bricks" in the brick-and-mortar model
-lipid bilayer (intercellular lipids) → this serves as the "mortar" between keratinocytes, composed of ceramides, cholesterol, and free fatty acids
what are the two major components of the stratum corneum?
-supports and nourishes the epidermis
-interacts with epidermis during embryogenesis and wound repair
-determines skin thickness
-contains cells, fibers, and ground substance
what is the dermis?
-fibroblasts: produce collagen, elastin, reticulin, ground substance, fibronectin
-mast cells
-histiocytes (dermal macrophages)
-melanocytes (in some species)
what are the 4 cells of the dermis?
-collagen: provides 90% of tensile strength, constantly being synthesized and degraded
-elastin: provides 10% of strength and elasticity
-reticulin: makes up 1%, surrounds appendages, vessels, nerves
what are the 3 fibers of the dermis?
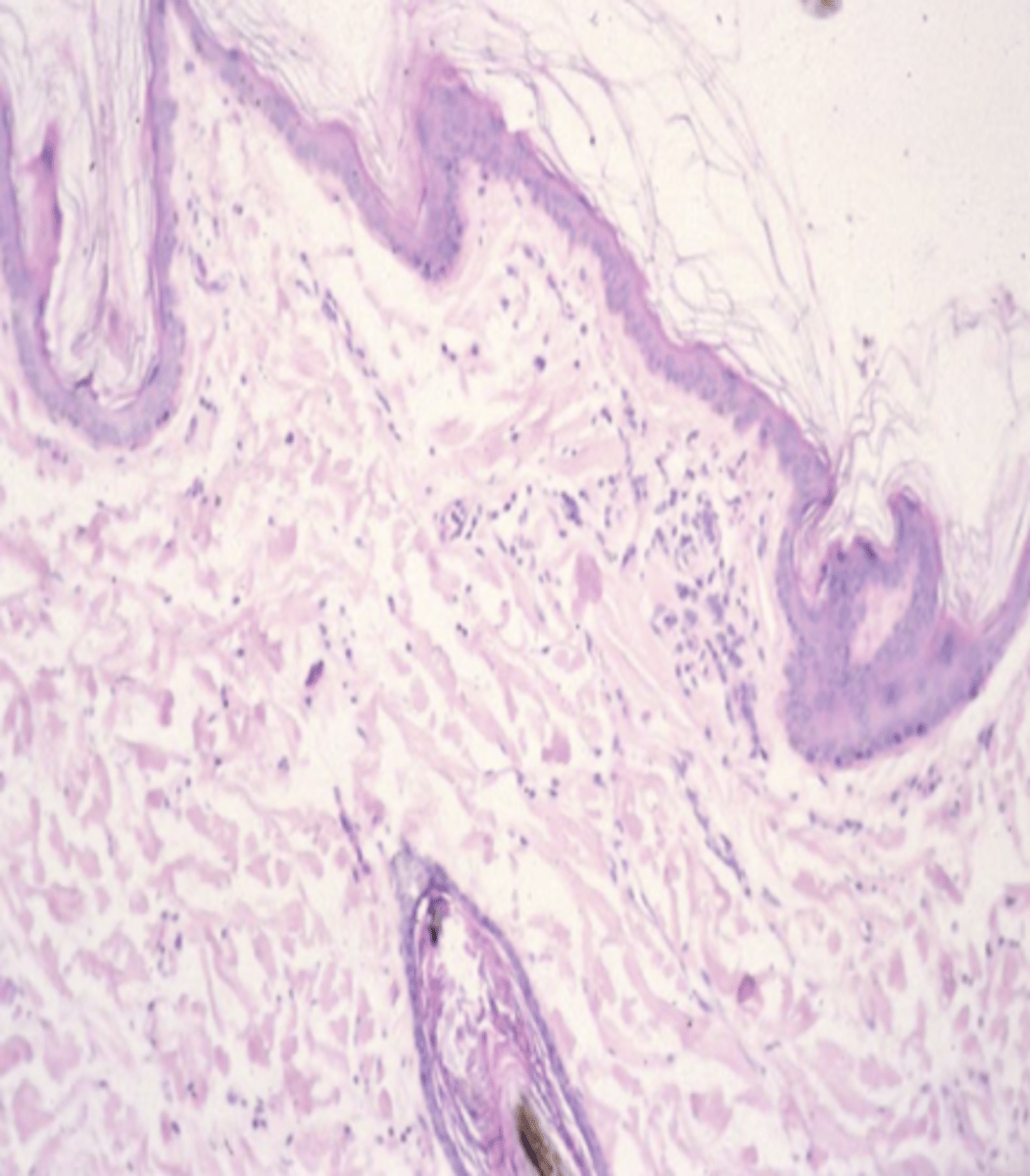
Ehlers-Danlos Syndrome
what syndrome is this?

vitamin B3 (Niacin)
which vitamin helps stimulate healthy blood vessels?
vitamin A (Retinol)
what is the most important vitamin for the epidermis?
-thermoreceptors (warm/cold units)
-tylotrich pads
-merkel's cells (slow adapting mechanoreceptors)
-pacinian corpuscles (vibration and deep pressure)
-meissner or ruffini corpuscles (velocity of skin movement)
-penicillate nerve endings
what are the different sensory receptors/nerve endings of the skin?
-UV light protection
-protection from contact irritants
-physical damage prevention
-temperature regulation
-camouflage
-social interactions
-pheromone distribution
what are the protective functions of hair?
-breakdown in the stratum corneum (e.g., due to keratinization defects, inflammation, or trauma) allows pathogens, allergens, and irritants to penetrate, leading to infections and immune-mediated responses
-loss of lipid layers and increased moisture create an environment conducive to microbial growth
how do breakdowns in the normal structure and function of the skin lead to disease?
-sebaceous glands: produce sebum (oily film); antimicrobial properties
-epitrichial (apocrine) glands: located on chin, feet, rump
-atrichial glands: located on footpads; aid in thermoregulation
what are the 3 glands located in the skin?
-water (for evaporation)
-salts, ammonia, urea
-lubricants
-histamine, prostaglandin, proteases
-glucose
-pheromones
-some medications (ketoconazole, itraconazole)
what is sweat composed of?
-stratum corneum acts as a physical barrier
-sebum has antimicrobial properties
-sweat has antimicrobial properties
-acidic environment inhibits microbial growth
-salt creates an inhospitable environment for microbes
-linoleic acid has antimicrobial properties
-immunoglobulins (IgA, IgG)
-langerhans cells
what are the cutaneous defenses of the skin?
-temperature changes
-moisture changes (warm, moist environments promote bacterial growth)
-altered glandular secretions
-antibody responses
-licking and scratching behaviors
-bacterial binding
which factors alter the skin defenses?
-located in the basal layer (1 per 10-20 cells)
-transfer melanin to keratinocytes
-depend on tyrosinase (requires copper)
what are melanocytes?
Eumelanin and Pheomelanin
what are the two types of melanin produced?
-UV light protection (absorbs radiation, scavenges free radicals)
-camouflage
-decorative
what are the functions of melanocytes?
-primary skin diseases (allergies, endocrine disorders) alter skin temperature, moisture, and sebum composition, creating a favorable environment for microbial overgrowth
-scratching and licking disrupt the barrier, allowing Staphylococcus and Malassezia species to colonize
-changes in immune responses, such as excessive IgE production, promote bacterial binding and persistence
why do secondary bacterial pyoderma or yeast infections occur?
-autoantibodies target desmosomes or basement membrane proteins, disrupting cell adhesion
-this leads to acantholysis (loss of cell connections), causing blisters or ulcers in diseases like pemphigus and lupus
-in lupus or vasculitis, immune complexes lead to inflammation, ischemia, and ulceration
how do autoimmune skin diseases cause blisters or ulcers?
-Th1 cells fight infections by activating macrophages
-Th2 cells promote allergic responses, leading to pruritus and inflammation
-Th17 cells contribute to autoimmune conditions and chronic inflammation
*dysregulation in these cells leads to hypersensitivity reactions, chronic skin disease, or immunosuppression
how do T helper cells benefit or cause disease in the skin?
mast cells release histamine, cytokines, and proteases, triggering itching, swelling, and inflammation seen in allergies and hypersensitivity reactions
why are mast cells especially important in dermatology?
eosinophils are crucial in parasite defense and allergic dermatitis, releasing toxic granules that damage tissues in chronic conditions like atopic dermatitis
why are eosinophils especially important in dermatology?