HIV-AIDS
1/38
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
39 Terms
How does HIV manifest: GI/Neurologic
GI: diarrhea, abdominal pain, nausea
Neurologic: seizures & dementia
What bacterial infections manifest in HIV?
1. NUG/NUP
3. Necrotizing Stomatitis
2. Linear gingival erythema
What fungal infections manifest in HIV?
1. recurrent candidiasis
2. deep fungal infections
What viral infections manifest in HIV?
1. HSV
2. Varicella-Zoster
3. EBV - hairy leukoplakia
4. HPV
5. Kaposi Sarcoma
What is the most commonly observed fungal infection in HIV?
candidiasis
- resistant to treatment
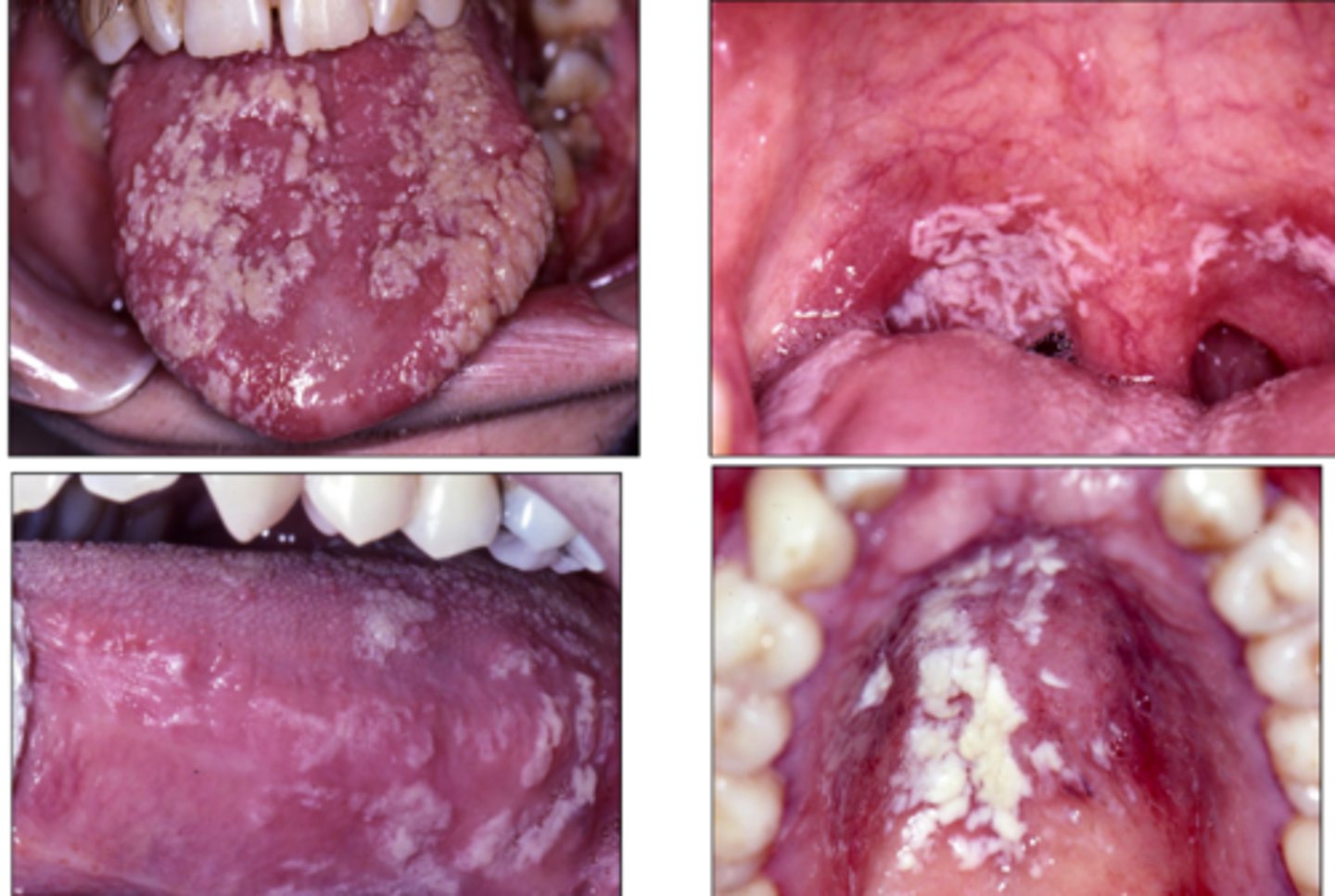
Histoplasmosis is a deep fungal infection with what kind of inflammation?
Oral presentation?
Granulomatous inflammation
- painful, non-healing ulcers
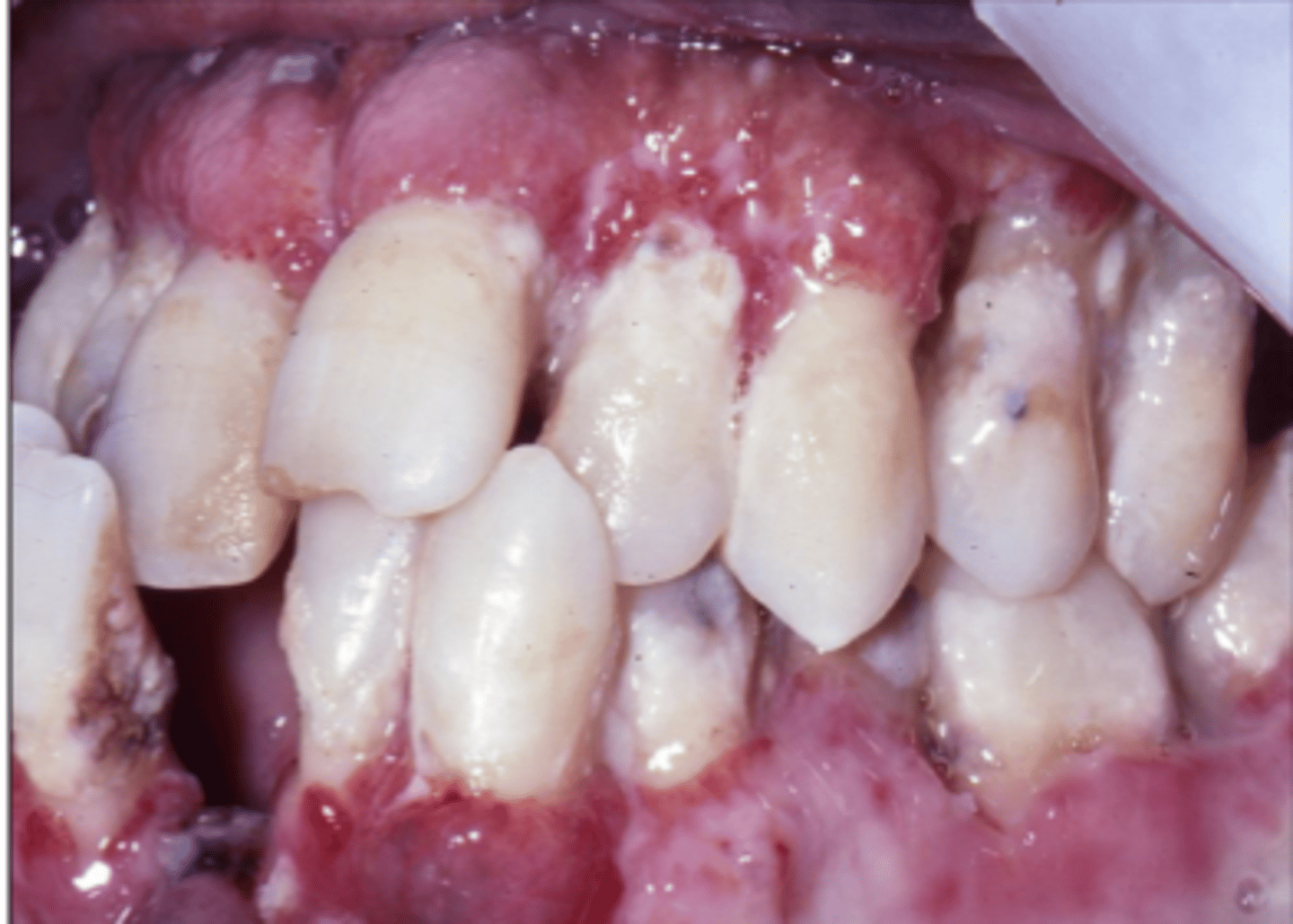
_______ is an AIDS defining illness. What does this mean?
histoplasmosis ; If a patient is diagnosed with HIV, presentation of this diseases is a sign of crossing over into AIDS
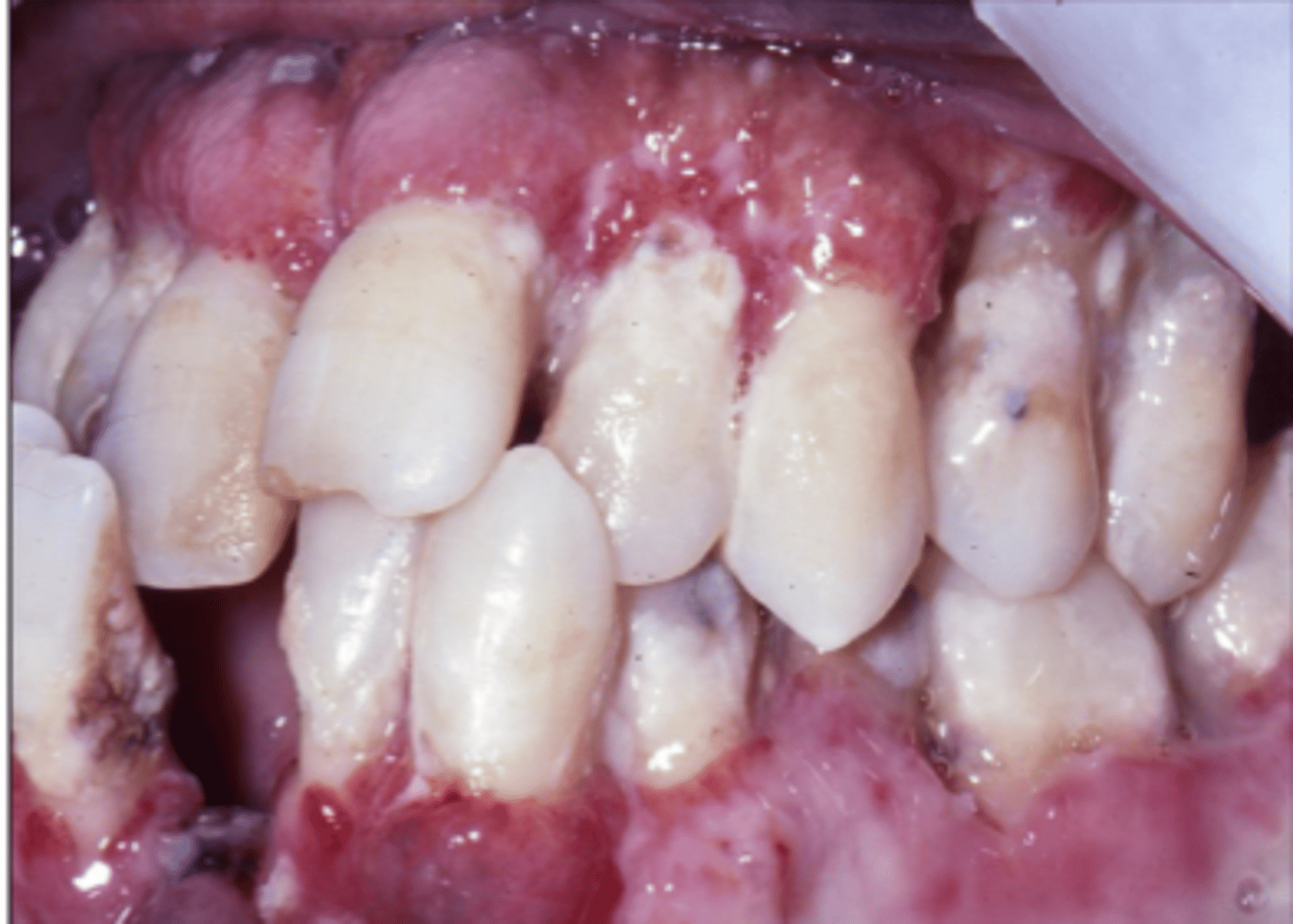
What is linear gingival erythema?
- how does it present?
red linear band at marginal gingiva
- spontaneous bleeding & petechiae may be present
does NOT respond to improved OH
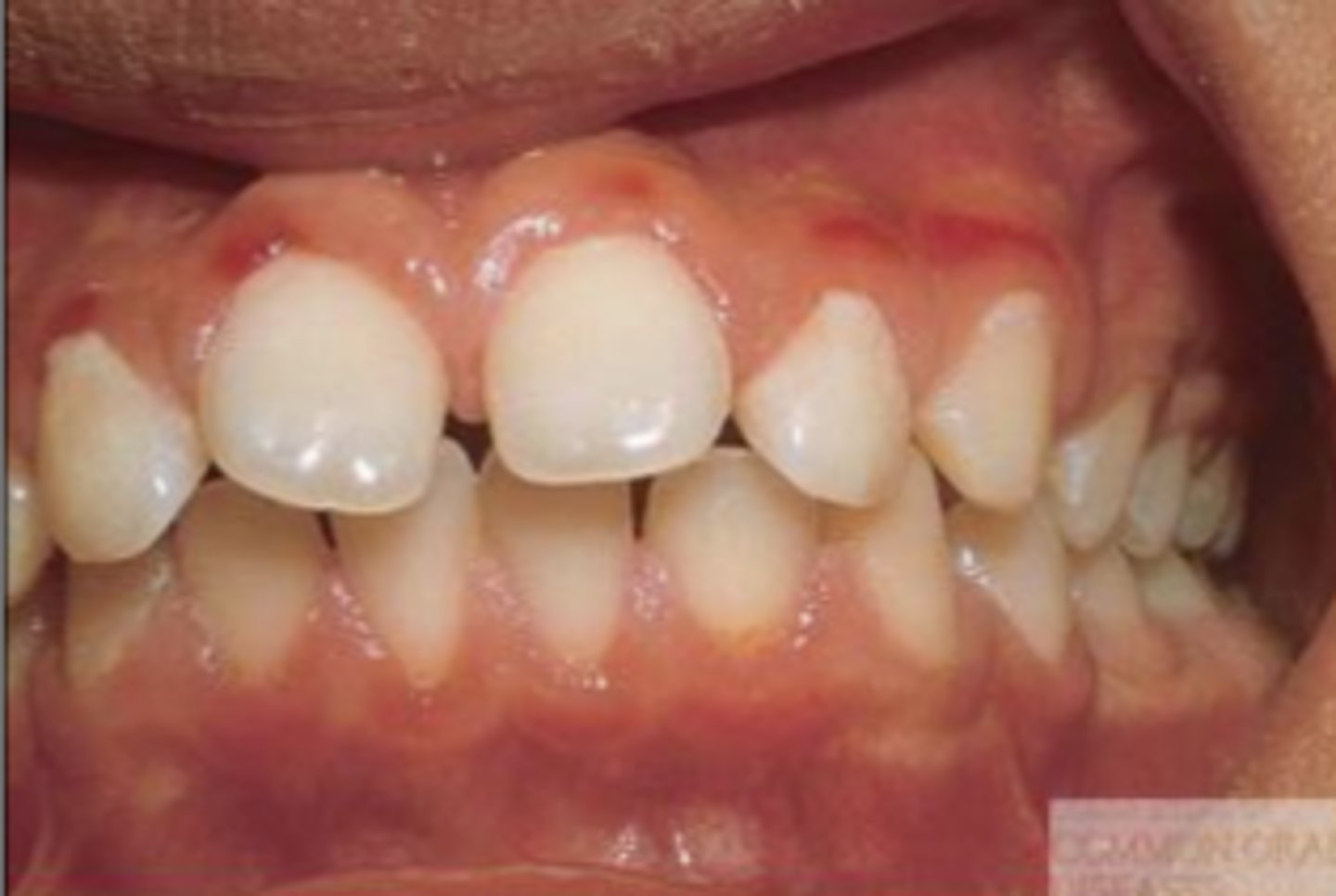
(T/F): Necrotizing Ulcerative Gingivitis (NUG) presents similarly as in nonimmunocompromised patients
True, but with relatively few local factors
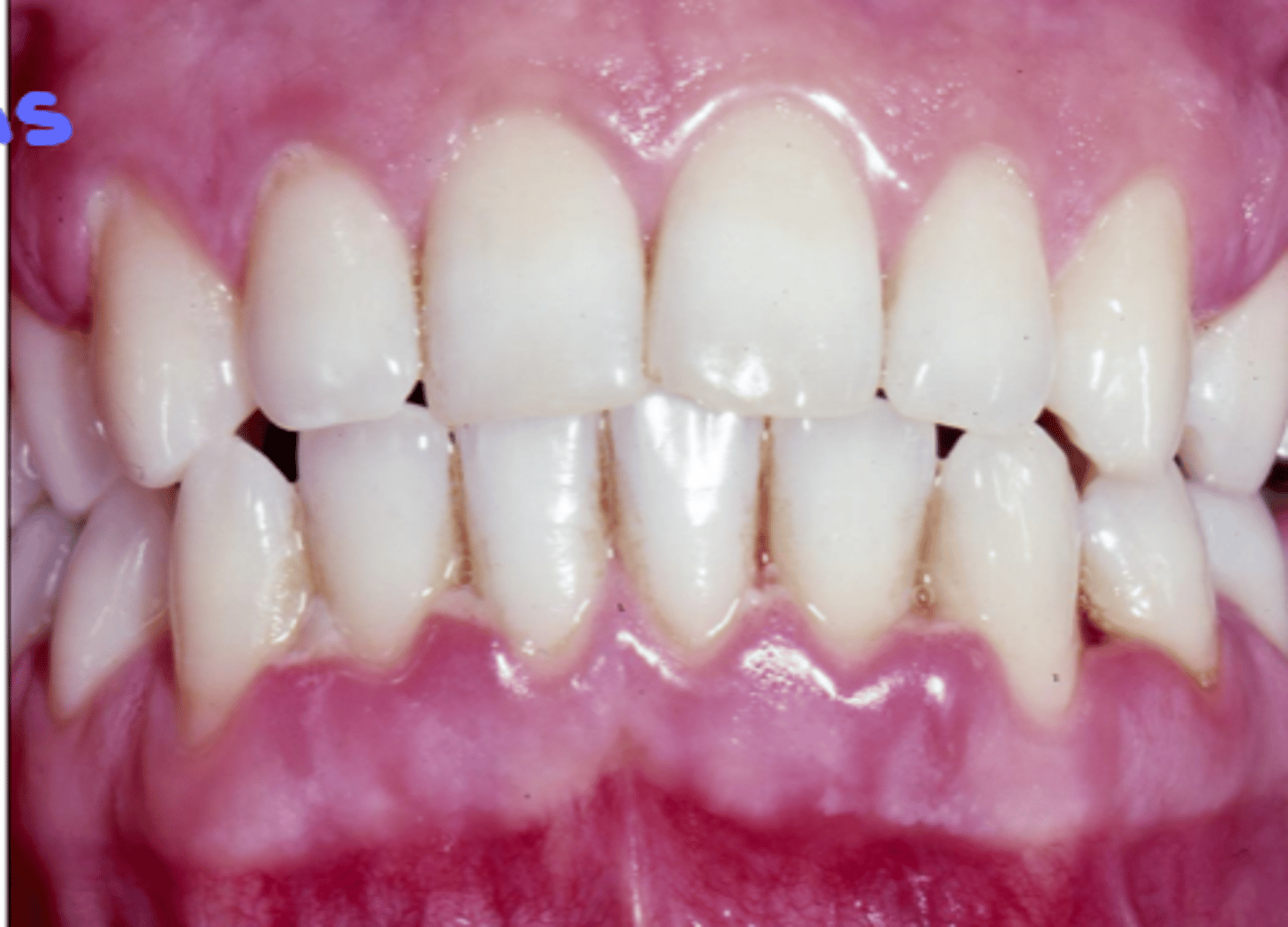
(T/F): Necrotizing Ulcerative Periodontitis (NUP) presents similarly as in NON-immunocompromised patients
true
may present with relatively few local factors & destroys attachment apparatus
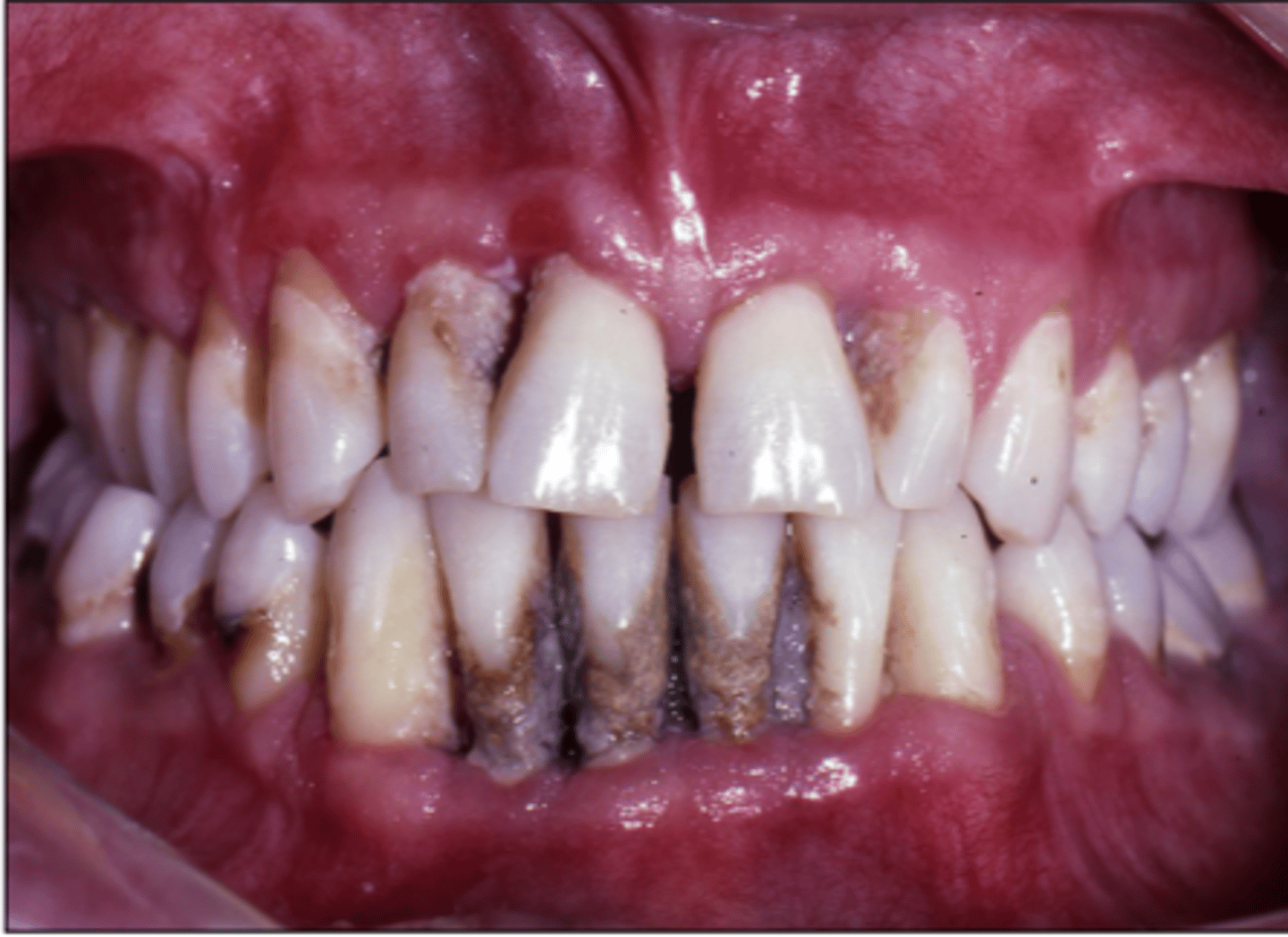
Necrotizing stomatitis leads to extensive destruction of what?
gingiva, periodontal bone, adjacent soft tissue & osseous structures
NUG > NUP > Necrotizing Stomatitis
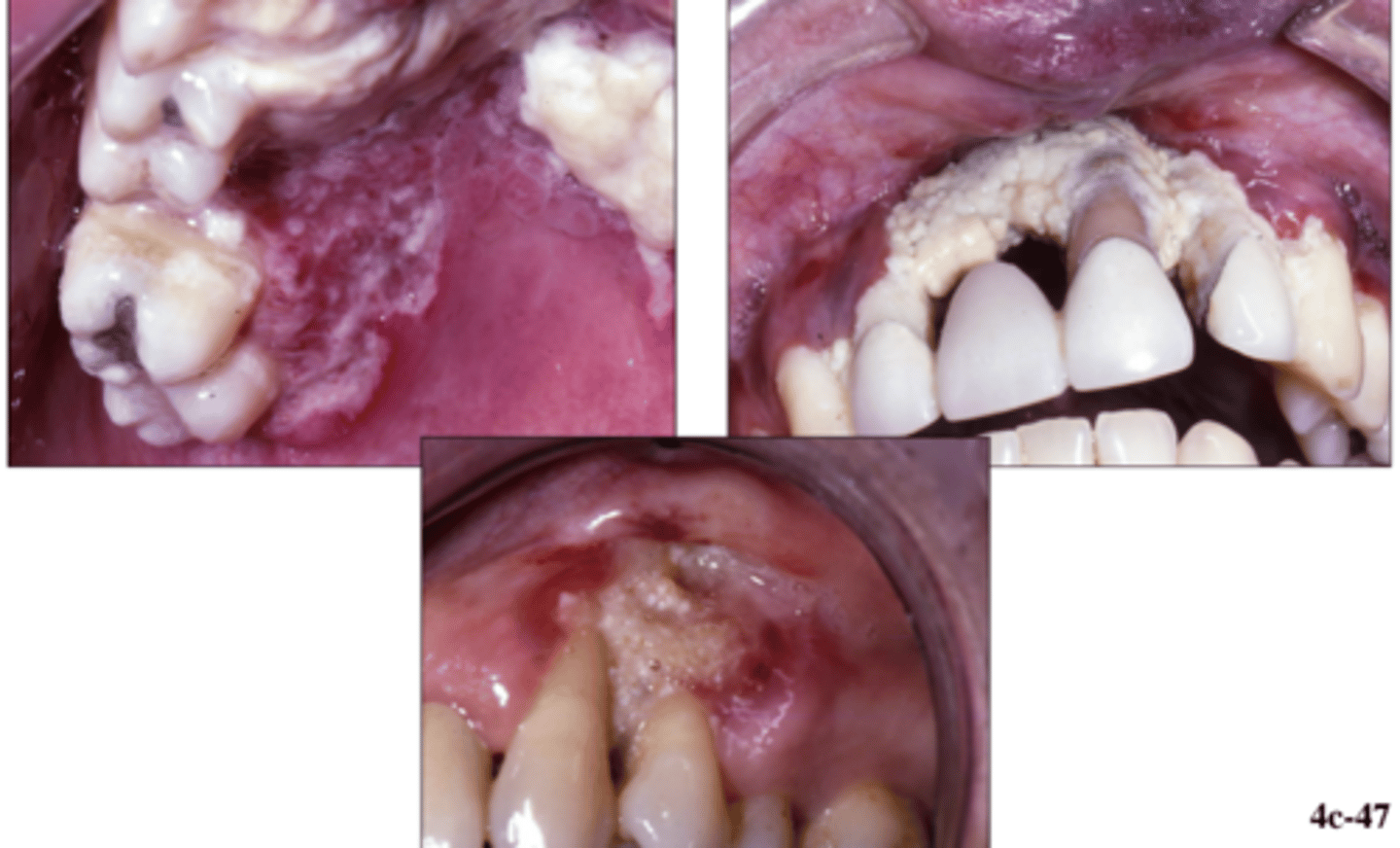
what does recurrent herpes simplex in HIV patients look like? How do you treat them?
In HIV positive patients, the lesions are more widespread and present with an a-typical pattern. They are treated with acyclovir
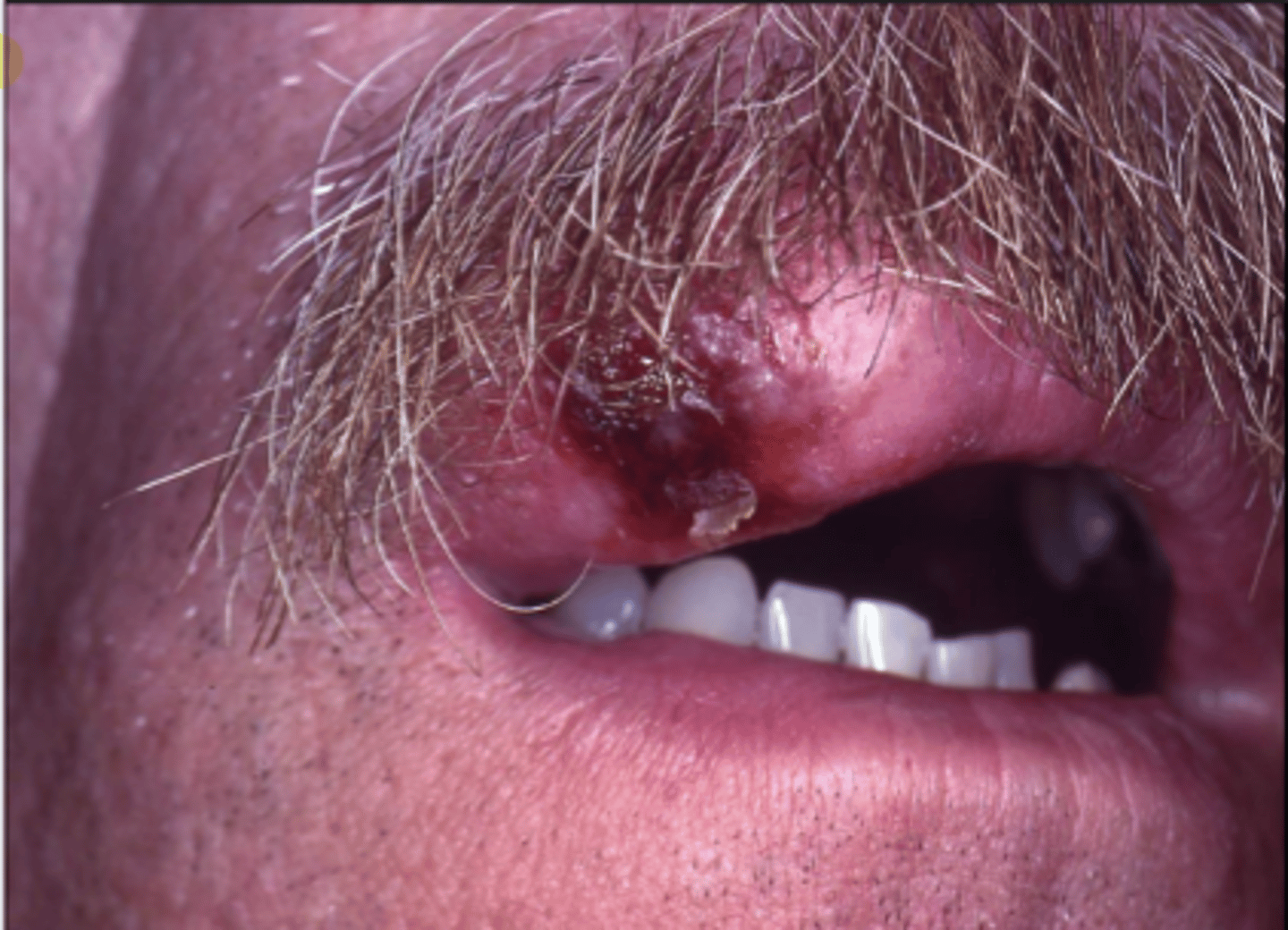
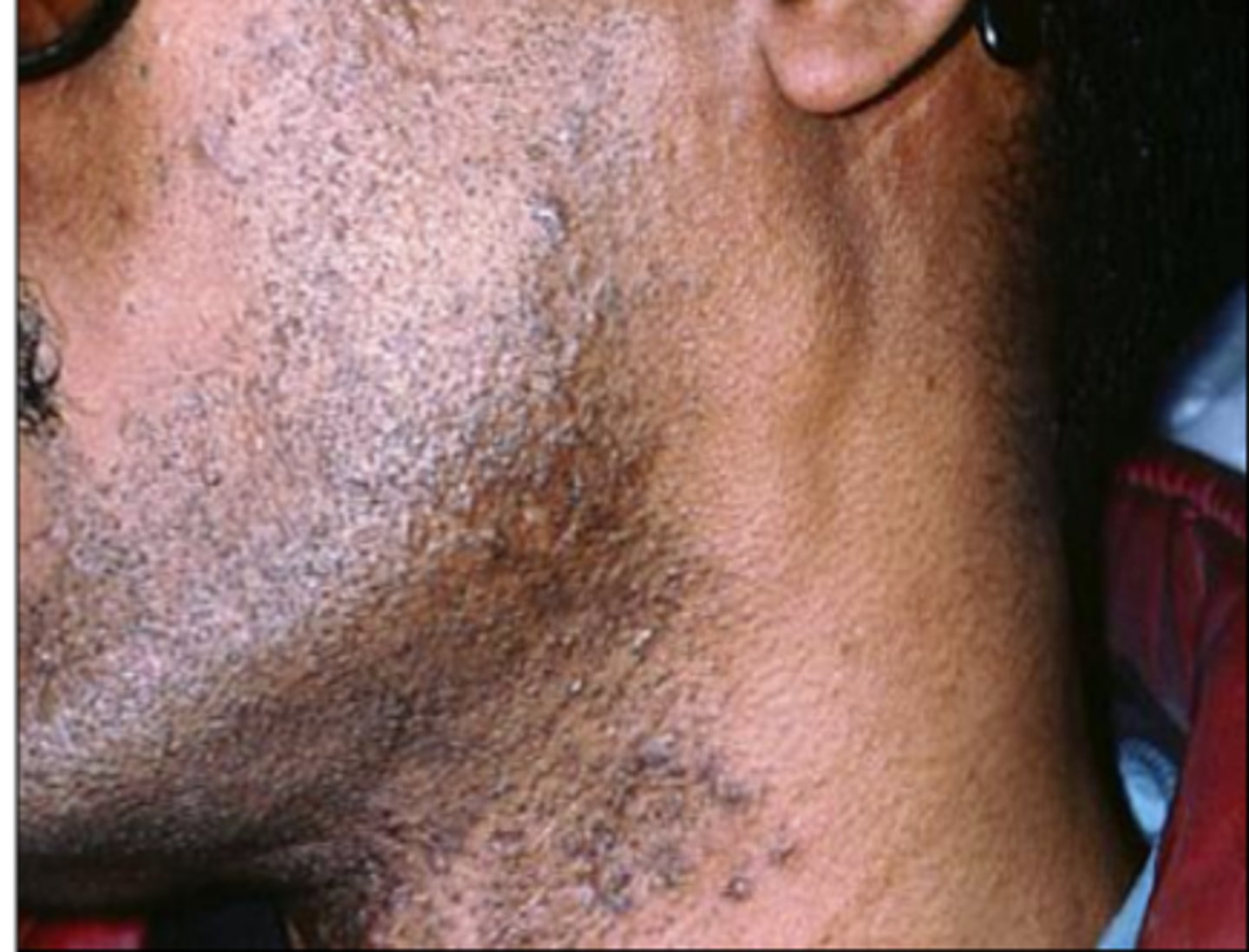
How does varicella-zoster present in HIV positive patients?
population
seen in younger populations, under 40!!
unilateral vesicles and ulcers - intense pain
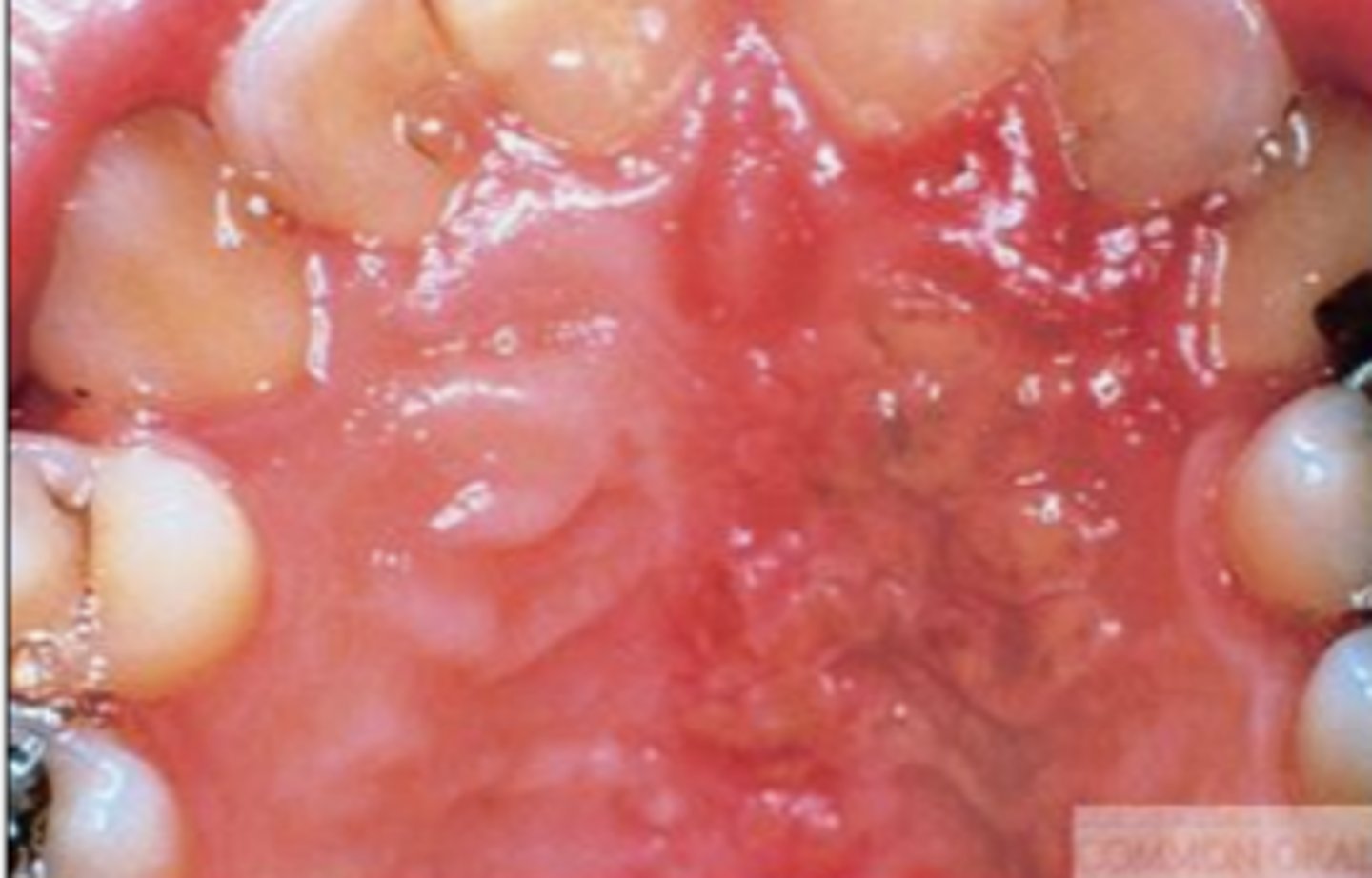
What causes hairy leukoplakia?
- how does it present
- treatment
Epstein-Barr Virus
- presents as non-removed white plaques of lateral tongue
- no treatment/asymptomatic
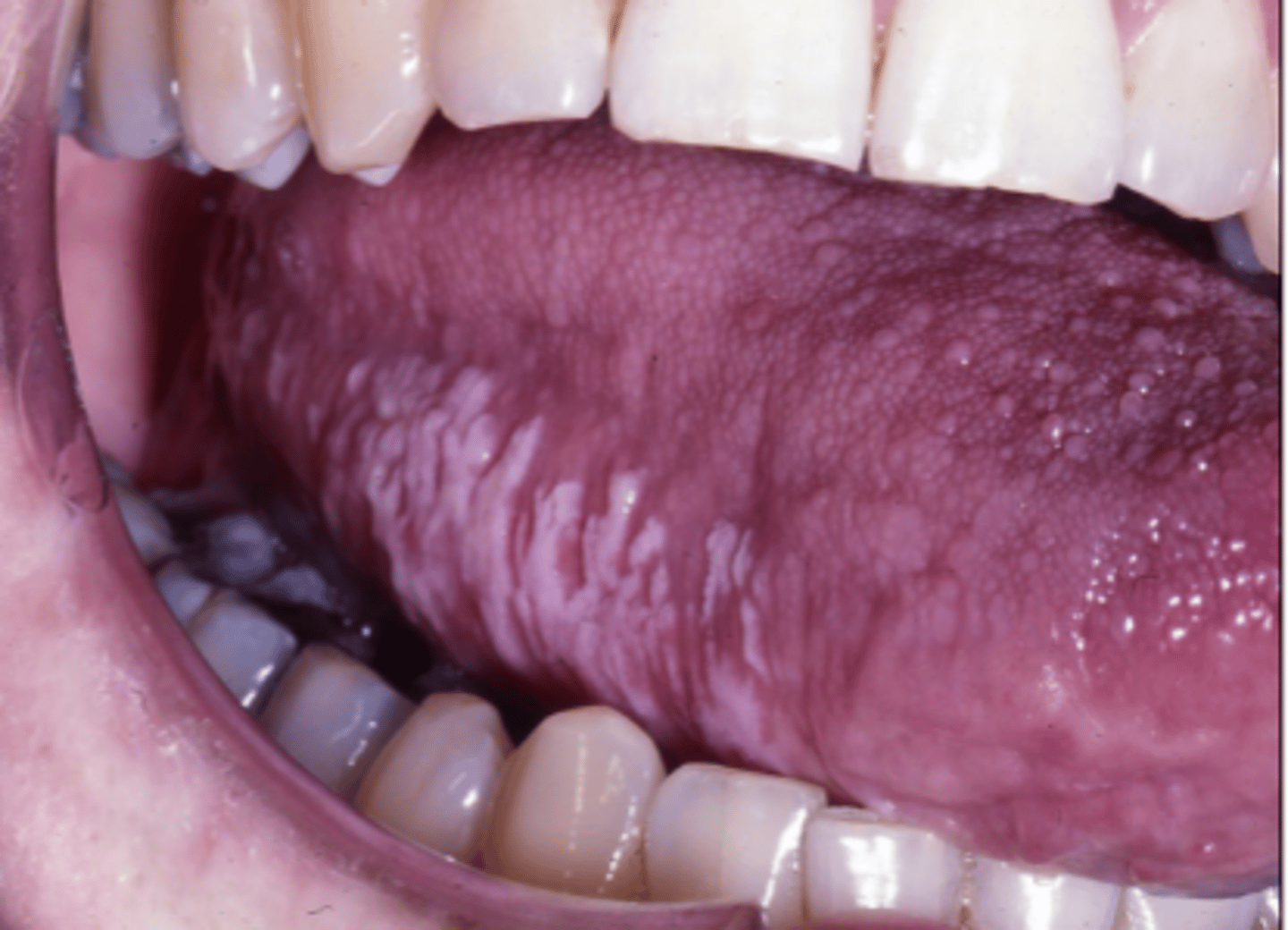
Human Papillomavirus (HPV) is composed of intraoral _______ lesions caused by several different HPVs
- how does it appear clinically in hiv and hiv negatives?
exophytic
- clinically: multiple lesions / proliferation & recurrence
In HIV negative patients, it usually occurs as a single lesion and does recur
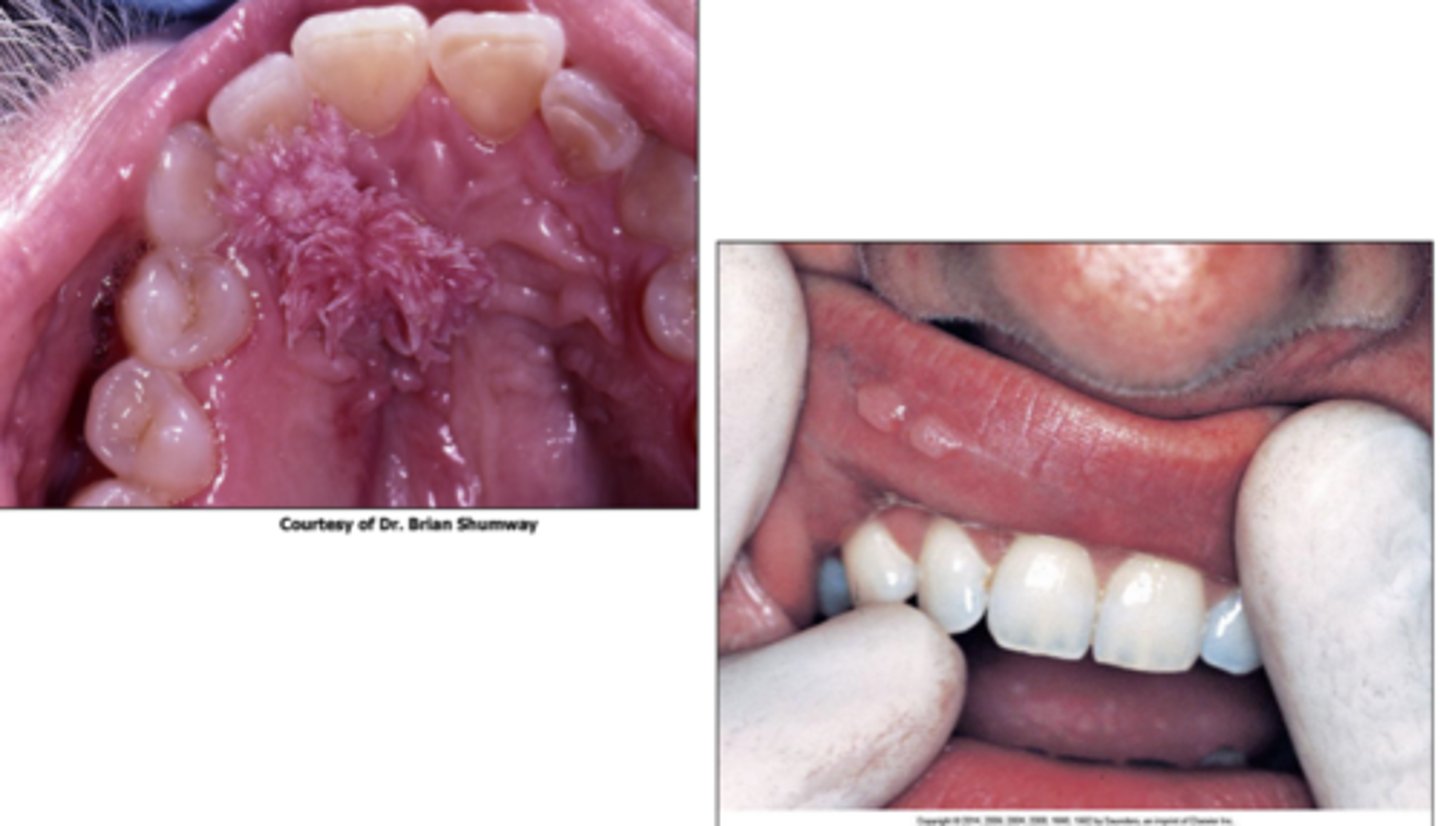
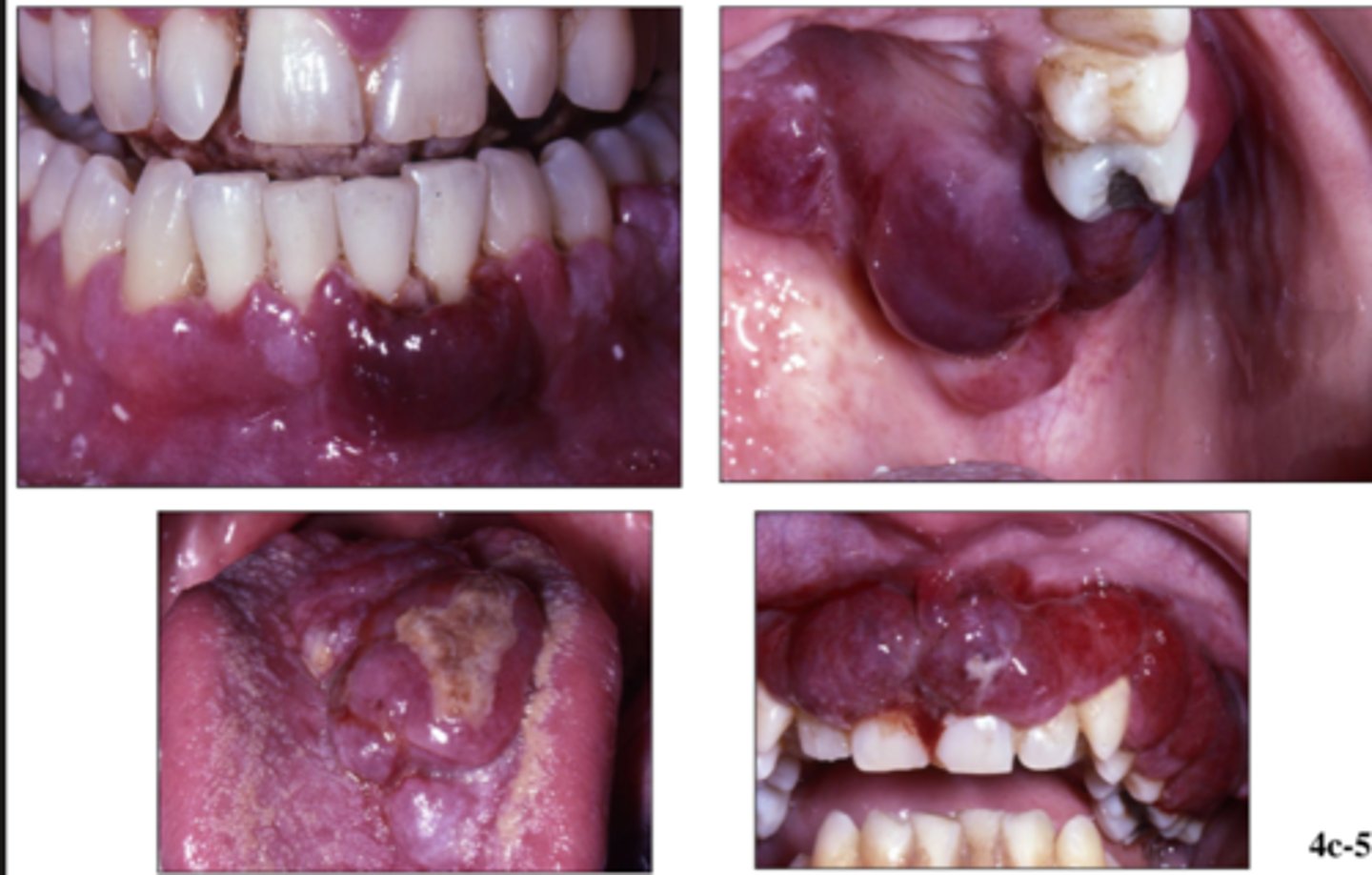
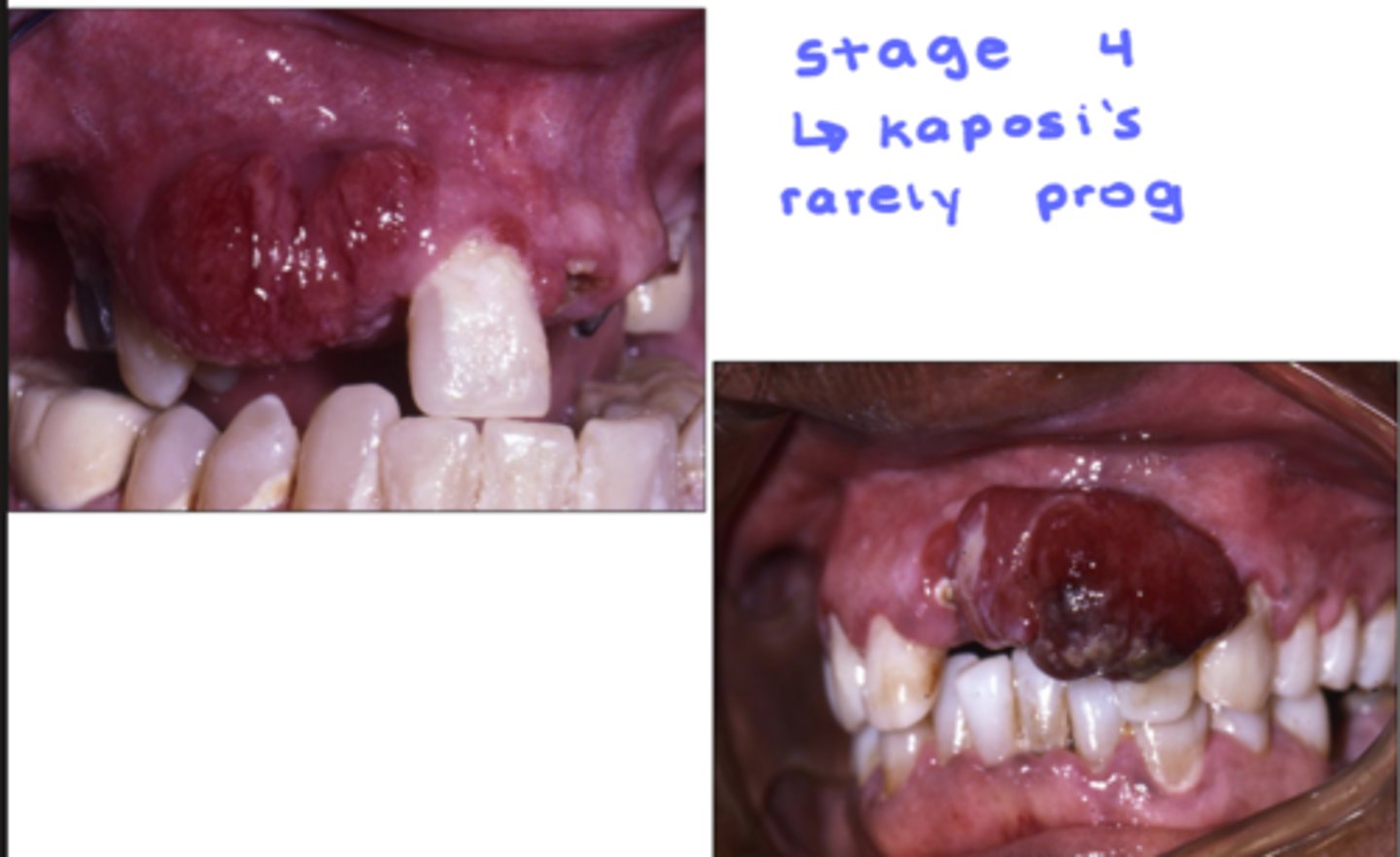
Kaposi Sarcoma is HHV8, associated ONLY with _______
- how does it appear clinically?
- prognosis?
HIV
clinically:
- reddish-purple
- on palate or gingiva
- multiple lesions
- 50% will present with intra oral lesions
prognosis is rarely fatal
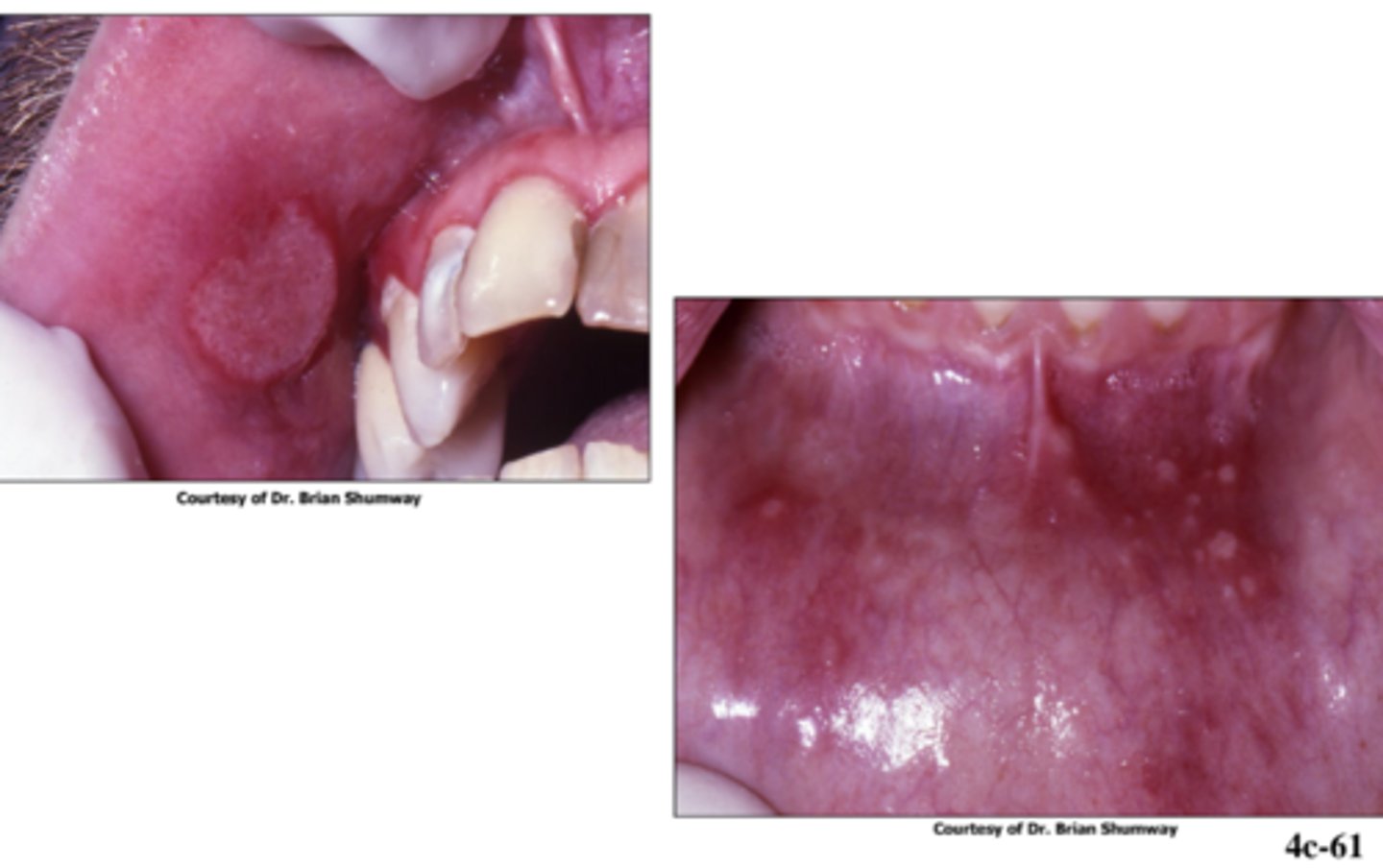
Aphthous-like ulcerations are probably ______ mediated
- how do they present clinically?
- treatment?
immune
- single or multiple lesions / painful & persistent
- topical corticosteroids
How does persistent lymphadenopathy appear clinically?
often involves cervical lymph nodes and is non-tender
Salivary gland involvement usually presents ______ and ______ may be present
bilaterally ; xerostomia
What is the most common malignancy among AIDS patients in the US?
AIDS-related lymphoma
often associated with HIV
How does AIDS related lymphoma present clinically?
5 things
intraoral lesions may resemble kaposi's sarcoma
- presents with diffuse bone loss
- involves CNS or GI tract
usually very aggressive w/poor prognosis
Only an estimated ____% of HIV patients know their status.
60%
______ million people globally have HIV
______ million children globally have HIV
people globally > 37.9 million
children globally > 1.7 million
_______ million people in the US have HIV
1.2 million
Pertaining to HIV, what is the most affected region? Who faces the greatest burden of HIV?
Sub-Saharan Africa ; African Americans > 45% of HIV diagnoses
Men make up ____% of the HIV population
81%
HIV - U.S.
_____% (13,920) were aged 20-29
_____% (9,973) were aged 30-39
37% ; 26%
Geographically, the south made up ____% of diagnoses in 2018
16%
When is a diagnosis of AIDS made?
When a person is HIV+ and one of the following:
- CD4 levels below 200
- CD4 levels less than 14% of all lymphocytes
- diagnosis of one or more of the AIDS-defining illnesses
HIV prevalence
the number of people living with aids w/ or w/out diagnosis at a point in time
HIV incidence
the number of people who become newly infected with HIV in a given period
Define the stages of HIV
Stage 0: early infection, recognized by negative HIV test within 6 months of HIV diagnosis
Stage 1: CD4=500+ or 26%+
Stage 3 (AIDS): CD4=200- or 14%-
How can HIV be transmitted?
1) Transfusions of infected blood
2) Exposure to HIV before or during birth or through breast feeding
3) Sexual contact
4) Sharing needles
5) Occupational exposure
How do we prevent transmission of HIV in the dental office?
prophylaxis prep - combination of drugs taken daily for 4wks before the appt
HIV risk from exposure:
Approximately ____% following percutaneous exposure (needle/instrument stick)
Approximately ____% following mucous membrane exposure
0.3% ; 0.9%
What are the seven steps in the HIV life cycle
1. binding > attaches to CD4 cell
2. fusion > fuses to CD4 cell
3. reverse transcription > combine's DNA with CD4
4. integration > converts CD4 to HIV DNA
5. replication > creates HIV proteins
6. assembly > cells move to surface and assemble immature HIV
7. budding > infection pushes outside the cell and eventually forms mature, infectious HIV
What drugs control HIV and help prevent transmission?
Anti-retroviral drugs (ARV)
(T/F): Referral for infection control is acceptable
False
What is the "golden rule" approach when treating HIV+ patient?
the mode of infection is irrelevant, treat them with compassion, respect and hope