Blood Banking BOC (All questions)
1/437
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
438 Terms
The minimum hemoglobin concentration in a fingerstick from a male blood donor is:
a 12.0 g/dL (120 g/L)
b 12.5 g/dL (125 g/L)
c 13.0 g/dL (130 g/L)
d 13.5 g/dL (135 g/L)
c 13.0 g/dL (130 g/L)
A cause for indefinite deferral from blood donation is:
a a reactive test for Babesia species
b residence in an endemic malaria region for 5 years
c positive test for Trypanosoma cruzi
d history of chicken pox vaccination
c positive test for Trypanosoma cruzi
Present or past clinical or laboratory evidence of infection with Trypanosoma cruzi (Chagas disease) is cause for an indefinite deferral from blood donation.
Babesia species is a 2-year deferral, residence in a malarial endemic area for 5 years is a 3-year deferral after departure, and chicken pox vaccination is a 4-week deferral.
Which of the following prospective donors would be accepted for blood donation?
a 62-year-old female with a blood pressure of 210/80
b 18-year-old female who weighs 100 lb
c 40-year-old male with a pulse of 115
d 82-year-old male with a hemoglobin of 13.5 g/dL
d 82-year-old male with a hemoglobin of 13.5 g/dL
Which one of the following constitutes permanent deferral status of a donor?
a tattoo 5 months previously
b recent close contact with a patient with viral hepatitis
c 2 units of blood transfused 4 months previously
d confirmed positive test for HBsAg 10 years previously
d confirmed positive test for HBsAg 10 years previously
A prospective donor with which of the following health histories would be accepted for blood donation?
a hepatitis B immune globulin 2 months ago
b HIV prevention drugs 6 months ago
c blood transfusion 2 months ago
d travel to malaria endemic country 1 month ago
b HIV prevention drugs 6 months ago
An individual taking HIV prevention drugs (PrEP & PEP) is eligible to donate 3 months after the last dose. Hepatitis B immune globulin administration is a 12-month deferral. A potential donor is deferred for 3-months after receiving a blood transfusion. Travel to a malarial-endemic area is a 3-month deferral after departure.
In order to be a plateletpheresis donor, the platelet count must be at least:
a 150,000/uL
b 200,000/pL
c 250,000/UL
d 300,000/pL
a 150,000/uL
Prior to blood donation, the intended venipuncture site must be cleaned with a scrub solution containing:
a hypochlorite
b green soap
c 10% acetone
d povidone iodine
d povidone iodine
A donor who has just donated 2 units of Apheresis Red Blood Cells will be deferred from further blood donation for a minimum of how many weeks?
a 8
b 12
c 16
d 24
c 16
Which of the following infectious agents relies solely on donor questioning to avoid transmission from transfused blood products?
a Trypanosoma cruzi
b Plasmodium falciparum
c HCV
d CMV
b Plasmodium falciparum
Which of the following practices at the time of blood collection helps minimize bacterial contamination of platelet products?
a use of 18-gauge needle
b diversion pouch
c green soap scrub
d UV irradiation
b diversion pouch
If a unit of autologous Red Blood Cells is collected and transfused in the same facility, which of the following is not required?
a ABO and Rh typing
b a physician's order
c infectious disease screening
d evaluation for risk of bacteremia
c infectious disease screening
According to AABB Standards, what is the minimum hemoglobin level for an autologous donor?
a 11.0 g/dL
b 12.0 g/dL
c 12.5 g/dL
d 13.0 g/dL
a 11.0 g/dL
Which of the following must be included on the label of a unit of Red Blood Cells Leukocytes Reduced?
a known leukocyte count for the unit
b phlebotomist identification
c unique collection facility identifier
d date of blood collection
c unique collection facility identifier
All donor blood testing must include:
a complete Rh phenotyping
b anti-CMV testing
c direct antiglobulin test
d serological test for syphilis
d serological test for syphilis
Which of the following is not a useful strategy to reduce bacterial contamination in platelet components?
a using green soap scrub to disinfect venipuncture site
b diverting the first 10-40 mL of donor blood from the main blood bag
c performing culture-based testing on all platelet components
d applying pathogen reduction technology to platelet components
a using green soap scrub to disinfect venipuncture site
Which of the following practices has been useful in reducing the incidence of transfusion related acute lung injury (TRALI)?
a use of Fresh Frozen Plasma from male donors
b use of Fresh Frozen Plasma from female donors
c pathogen reduction treatment of Fresh Frozen Plasma
d leukocyte-reduced Fresh Frozen Plasma
a use of Fresh Frozen Plasma from male donors
In allogeneic blood donation, which of the following infectious agents must also include a nucleic acid testing (NAT) assay?
a HBV
b HTLV I/II
c syphilis
d cytomegalovirus
a HBV
What is the primary reason that infectious agents can be transmitted following blood transfusion?
a pathogen reduction technology failure
b donor in the window period of early infection
c leukocyte-reduction failure
d donor history questionnaire not completed
b donor in the window period of early infection
Apheresis Platelets that will undergo pathogen reduction technology do not require:
a hepatitis B virus NAT
b culture-based testing for bacteria
c West Nile virus NAT
d ABO and Rh testing
b culture-based testing for bacteria
c perform weak D testing on donor RBCs
The results in this table are obtained on a blood donor sample at immediate spin. Before labeling blood components from this donation, what additional testing must be completed?
a test donor RBCs with anti-A,B
b test donor RBCs with anti-H
c perform weak D testing on donor RBCs
d test donor serum with Az cells

Which of the following courses of action must be performed immediately if a sample from an Apheresis Platelet undergoing culture-based testing indicates bacterial growth?
a set up another culture to confirm positivity
b determine sensitivity to antibiotics
c retrieve the unit if issued for transfusion
d identify the organism
c retrieve the unit if issued for transfusion
A sample of blood from each donation is tested for which of the following infectious disease agents?
a HIV-1/2, HTLV-I/II, WNV, HCV
b HBV, HCV, CMV, T. cruzi
c HBsAg, HIV-1/2, P. falciparum, Babesia species
d dengue virus, syphilis, HCV, HBV
a HIV-1/2, HTLV-I/II, WNV, HCV
The transport temperature for Red Blood Cells Leukocytes Reduced is:
a 1-6°C
b 1-10°C
c 18-20°C
d 20-24°C
b 1-10°C
The transport temperature for Apheresis Platelets is:
a 1-6°C
b 1-10°C
с 18-20°С
d 20-24°C
d 20-24°C
A unit of Red Blood Cells expiring in 35 days is split into 5 small aliquots using a sterile pediatric quad set and a sterile connecting device. Each aliquot must be labeled as expiring in
a 6 hours
b 12 hours
c 5 days
d 35 days
d 35 days
When platelets are stored on a rotator set on an open bench top, the ambient air temperature must be recorded:
a once a day
b twice a day
c every 4 hours
d every hour
c every 4 hours
Which of the following is the correct storage temperature for the component listed?
a Cryoprecipitated AHF, 4°C
b Fresh Frozen Plasma (FFP), -20°C
c Red Blood Cells, Frozen, -40°C
d Platelets, 37°C
b Fresh Frozen Plasma (FFP), -20°C
Six units of Red Blood Cells are issued to the OR at 9 AM in a cooler, validated to maintain a temperature of 1-10°C for 2 hours. The cooler containing the units of blood is returned to the units of blood is returned to the blood bank 40 minutes later because surgery is cancelled. What should be done with these a discard the units?
a discard the units as they were issued to a specific patient
b inspect units and establish that appropriate temperature has been maintained
c continue to store in cooler since surgery is rescheduled for tomorrow
d put units back into inventory as only 40 minutes has elapsed since issue
b inspect units and establish that appropriate temperature has been maintained
An acceptable storage temperature for Red Blood Cells, Frozen is:
a -80°C
b -20°C
c -12°C
d 4°C
a -80°C
Red Blood Cells, Leukocytes Reduced must be stored at:
a 1-6°C
b 1-10°C
с 1-20°С
d 20-24°C
a 1-6°C
If the seal is entered or broken on a unit of Red Blood Cells stored at 1-6°C, what is the maximum allowable storage period, in hours?
a 6
b 24
c 48
d 72
b 24
Cryoprecipitated AHF must be stored at:
a ≤-10°C
b ≤-18°C
c 1-6°C
d 1-10°C
b ≤-18°C
Plasma Frozen Within 24 Hours After Phlebotomy (PF24) and thawed for transfusion has an expiration of:
a 6 hours
b 12 hours
c 24 hours
d 5 days
c 24 hours
Apheresis Platelets must be stored at:
a 1-6°C
b 1-10°C
c 10-18°C
d 20-24°C
d 20-24°C
Cryoprecipitated AHF, if maintained in the frozen state at -18°C or below, has a shelf life of:
a 42 days
b 6 months
c 12 months
d 36 months
c 12 months
Thawed Plasma must be stored at:
a ≤-18°C
b 1-6°C
c 1-10°C
d 20-24°C
b 1-6°C
During storage, the concentration of 2,3-diphosphoglycerate (2,3-DPG) decreases in a unit of:
a Platelets
b Fresh Frozen Plasma
c Red Blood Cells
d Cryoprecipitated AHF
c Red Blood Cells
Upon inspection, a unit of Apheresis Platelets is noted to have visible clots, but otherwise appears normal. The technologist should:
a issue without concern
b filter to remove the clots
c centrifuge to express off the clots
d quarantine for Gram stain and culture
d quarantine for Gram stain and culture
Upon expiration, a unit of thawed Plasma Frozen Within 24 Hours (PF24) is converted to thawed Plasma. This thawed Plasma can be stored for an additional:
a 1 day
b 4 days
c 14 days
d 28 days
b 4 days
The transfusion service is preparing aliquots from a unit of Red Blood Cells Leukocytes Reduced with the aid of a sterile connecting device for a pediatric patient. When checking the weld for one of these aliquots, it is noted that the weld is incomplete and leaking. This unit is then resealed with an acceptable weld. What will the expiration date of this unit be?
a 6 hours
b 24 hours
c 3 days
d original expiration date
b 24 hours
A patient with a platelet count of 10,000/uL receives one unit of Apheresis Platelets, Leukocytes Reduced. After transfusion, the patient's platelet count is 50,000/uL. These results indicate:
a The presence of HLA antibodies and refractoriness to transfusion
b The patient is actively bleeding but still producing platelets
c The platelet count is the expected posttransfusion increment
d The patient's pre-transfusion platelet count was incorrect
c The platelet count is the expected posttransfusion increment
Red Blood Cells Leukocytes Reduced must be prepared by a method known to reduce the leukocyte count to:
a <8.3 × 10^5
b <5.0 × 10^6
c <5.5 × 10^10
d <3.0 × 10^11
b <5.0 × 10^6
A unit of Red Blood Cells that expires in 32 days has just been irradiated. The expiration date of this unit will:
a remain the same
b be reduced by 4 days
c be reduced by 14 days
d be increased by 2 days
b be reduced by 4 days
Cryoprecipitated AHF must be transfused within what period of time following thawing and pooling without the use of a sterile connection device?
a 4 hours
b 8 hours
c 12 hours
d 24 hours
a 4 hours
According to AABB Standards, Fresh Frozen Plasma must be infused within what period of time following thawing?
a 24 hours
b 36 hours
c 48 hours
d 72 hours
a 24 hours
Cryoprecipitated AHF:
a is indicated for fibrinogen deficiencies
b should be stored at 4°C prior to administration
c will not transmit hepatitis B virus
d is indicated for the treatment of hemophilia B
a is indicated for fibrinogen deficiencies
Which Apheresis Platelets product should be irradiated?
a autologous unit collected prior to surgery
b random stock unit going to a patient with DIC
c a directed donation given by a mother for her son
d a directed donation given by an unrelated family friend
c a directed donation given by a mother for her son
Irradiation of a unit of Red Blood Cells is done to prevent the replication of donor:
a granulocytes
b lymphocytes
c red cells
d platelets
b lymphocytes
Plastic bag overwraps are recommended when thawing units of FFP in 37°C water baths because they prevent:
a the FFP bag from cracking when it contacts the warm water
b water from slowly dialyzing across the bag membrane
c the entry ports from becoming contaminated with water
d the label from peeling off as the water circulates in the bath
c the entry ports from becoming contaminated with water
Which of the following blood components must be prepared within 8 hours after phlebotomy?
a Red Blood Cells
b Fresh Frozen Plasma
c Red Blood Cells, Frozen
d Cryoprecipitated AHF
b Fresh Frozen Plasma
Which of the following is proper procedure for preparation of Platelets from Whole Blood?
a light spin followed by a hard spin
b light spin followed by 2 hard spins
c 2 light spins
d hard spin followed by a light spin
a light spin followed by a hard spin
Of the following blood components, which one should be used to prevent HLA alloimmunization of the recipient?
a Red Blood Cells
b Granulocytes
c Irradiated Red Blood Cells
d Leukocyte-Reduced Red Blood Cells
d Leukocyte-Reduced Red Blood Cells
Quality control of Apheresis Granulocytes must demonstrate which of the following granulocyte counts in 75% of units tested?
a 1.0 × 10^10
b 2.0 × 10^10
c 3.0 × 10^10
d 4.0 × 10^10
a 1.0 × 10^10
An important determinant of platelet viability during storage is:
a plasma potassium concentration
b plasma pH
c prothrombin time
d activated partial thromboplastin time
b plasma pH
According to ABB Standards, Apheresis Platelets shall demonstrate with 95% confidence that >75% of units contain ≥ how many platelets?
а 5.5 × 10^10
b 6.5 × 10^10
c 3.0 × 10^11
d 5.0 × 10^11
c 3.0 × 10^11
According to AABB Standards, Platelets prepared from Whole Blood shall have at least:
a 5.5 × 10^10 platelets per unit in at least 90% of the units tested
b 6.5 × 10^10 platelets per unit in 90% of the units tested
c 7.5 × 10^10 platelets per unit in 100% of the units tested
d 8.5 × 10^10 platelets per unit in 95% of the units tested
a 5.5 × 10^10 platelets per unit in at least 90% of the units tested
According to AABB Standards, Apheresis Platelets shall demonstrate with 95% confidence that >95% of units
have what minimum pH at the time of issue?
а 6.0
b 6.2
с 6.8
d 7.0
b 6.2
What percentage of red blood cells must be retained when preparing Red Blood Cells Leukocytes Reduced?
a 50%
b 70%
c 85%
d 100%
c 85%
In a quality assurance program, Cryoprecipitated AHF must contain a minimum of how many international units of Factor VIII?
a 60
b 70
c 80
d 90
c 80
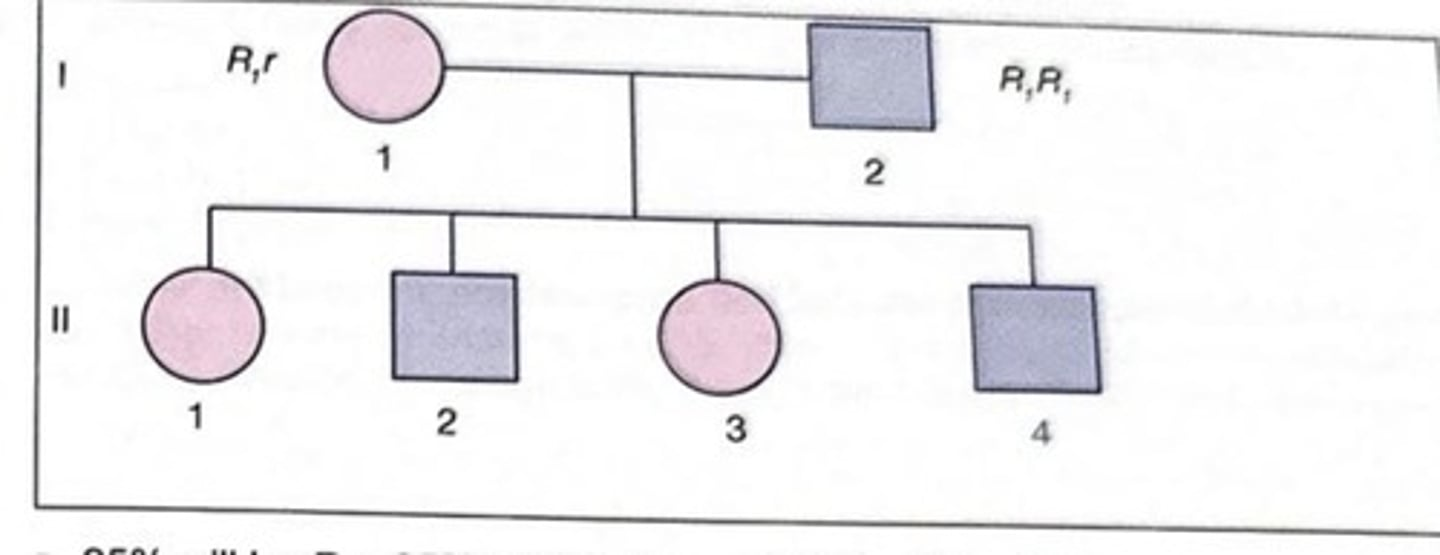
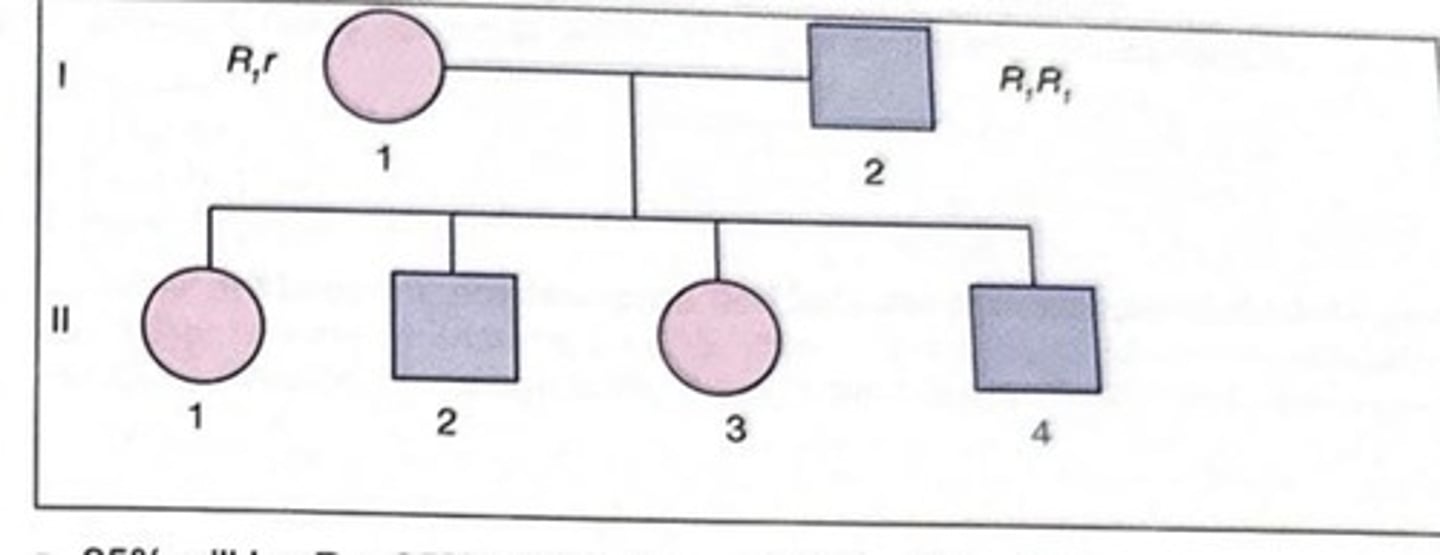
Given the most probable genotypes of the parents shown in this figure, which statement best describes the most probable Rh genotypes of the 4 children?
a 25% will be R0r, 25% will be R1r, and 50% will be R1R1
b 50% will be R1r and 50% will be R1R1
c 100% will be R1r
d 100% will be R1R1
b 50% will be R1r and 50% will be R1R1
The linked HLA genes on each chromosome constitute a(n):
a allele
b trait
c phenotype
d haplotype
d haplotype
Most blood group system genes and their resulting genetic traits display what type of inheritance?
a sex-linked dominant
b sex-linked recessive
c autosomal recessive
d autosomal codominant
d autosomal codominant
The mating of an Xg(a+) man and an Xg(a-) woman will only produce:
a Xg(a-) sons and Xg(a-) daughters
b Xg(a+) sons and Xg(a+) daughters
c Xg(a-) sons and Xg(a+) daughters
d Xg(a+) sons and Xg(a-) daughters
c Xg(a-) sons and Xg(a+) daughters

The observed phenotypes in a particular population are shown in the table. What is the gene frequency of Jka in this population?
a 0.31
b 0.45
c 0.55
d 0.60
c 0.55
Hardy-Weinberg equation: p² + 2pq + q² = 1.0.
In this example, the gene frequency of Jka is represented by p and the gene frequency of Jkb is represented by q and is expressed in the formula p + q = 1.0. p² is the homozygous population of Jka, or those who are Jk(a+b-).
The square root of p² = p, which is the gene frequency of Jka in this population. Out of 400 people, 122, or 30% are homozygous. The square root of 0.30 = is 0.55.

In a random population, 16% of the people are Rh-negative (rr). What percentage of the Rh-positive population is heterozygous for r?
a 36%
b 48%
c 57%
d 66%
b 48%
The Hardy-Weinberg equation states p + q= 1.0. When the equation is expanded, it is p2 + 2pq + q2 = 1.0. p2 equals those that are homozygous for D, 2pq equals those that are heterozygous for D and q2 represents those that are D-negative (rr). Homozygous population that is D-negative equals 0.16 (rr). The square root of 0.16 is 0.4 (q) and p can be determined by subtracting q from 1 where p equals 0.6 (0.4+0.6=1.0). Use this in the expanded equation to determine the D-positive population that is heterozygous for D, or 2pq or 2(0.6)(0.4) = 0.48 or 48%.
Which phenotype could not result from the mating of a Jk(a+b+) female and a Jk(a-b+) male?
a Jk(a+b-)
b Jk(a+b+)
c Jk(a-b+)
d Jk(a-b-)
d Jk(a-b-)
Which of the following phenotypes is the result of homozygous inheritance of the corresponding genes?
a Le(a+b-)
b M+N+
c Fy(a-b+)
d Jk(a+b+)
c Fy(a-b+)
What do the Oh (Classical Bombay), group O, and Lu(a-b-) phenotypes have in common?
a result from inheritance of identical sex-linked dominant genes
b result from inheritance of identical sex-linked recessive genes
c result from inheritance of identical autosomal dominant genes
d result from inheritance of identical autosomal recessive genes
d result from inheritance of identical autosomal recessive genes
Which of the following antibodies is usually clinically insignificant?
a anti-P
b anti-P1
c anti-Pk
d anti-p
b anti-P1

An individual's red blood cells give the reactions with Rh antisera shown in the table. The individual's most probable genotype is:
a DCe/DcE
b DcE/dce
c Dce/dce
d DCe/dce
d DCe/dce

A blood donor has the genotype: hh, AB. Using anti-A and anti-B antisera, the donor's red cells will type as group:
a A
b B
c O
d AB
c O
An individual has been sensitized to the k antigen and has produced anti-k. What is the most probable KEL system genotype for this individual?
a KK
b Kk
c kk
d K0K0
a KK
Anti-Fy3 will fail to react with which of the following enzyme-treated red cells?
a Fy(a+b-)
b Fy (a-b+)
c Fy(a-b-)
d Fy(a+b+)
c Fy(a-b-)
A mother has the red cell phenotype D+C+E-c-e+ with anti-c (titer of 32 at AHG) in her serum. The father has the phenotype D+C+E-c+e+. The baby is Rh-negative and not affected with hemolytic disease of the newborn. What is the baby's most probable Rh genotype?
a r'r'
b r'r
c R1R1
d R1r
a r'r'
In an emergency situation, Rh-negative red cells are transfused into an Rh-positive person of the genotype CDe/CDe. The first antibody most likely to develop is:
a anti-c
b anti-d
c anti-e
d anti-E
a anti-c
d R1R2
A patient's red cells type as shown in the table. Which is the most probable genotype?
a R1R1
b R1r'
c R0r"
d R1R2


A patient's red cells type as shown in the table. Which of the following genotype would be consistent with these results?
a R0R0
b R1r
c R1R2
d Rzr
a R0R0

The red cells of a nonsecretor (se/se) will most likely type as:
a Le(a-b-)
b Le(a+b+)
c Le(a+b-)
d Le(a-b+)
c Le(a+b-)
Which of the following phenotypes will react with anti-f?
a rr
b R1R1
c R2R2
d R1R2
a rr
a R1R2
A patient's red blood cells gave the reactions shown in the table. The most probable genotype of this patient is:
a R1R2
b R2r"
c Rzr
d RzRz

A woman types as Rh-positive. She has an anti-c titer of 32 at AHG. Her baby has a negative direct antiglobulin test (DAT) and is not affected by hemolytic disease of the newborn. What is the father's most likely Rh phenotype?
a rr
b r"r
c R1r
d R2r
c R1r
The baby appears to lack c since no HDFN is evident. The mom is most likely R1R1, SO had to pass R, onto the baby. The father must have passed on an Rh gene that also did not produce c. Given the choices, the father has to be R,r.
Which of the following red cell typings are most commonly found in the African American donor population?
a Lu(a-b-)
b Jk(a-b-)
c Fy(a-b-)
d K-k-
c Fy(a-b-)
b R1r
A donor is tested with Rh antisera with the results shown in the table. What is his most probable Rh genotype?
a R1R1
b R1r
c R0r
d R2r

d B35
A family has been typed for HLA because 1 of the children needs a stem cell donor. Typing results are listed in the table. What is the expected B antigen in child #3?
a A1
b A2
с B12
d B35

Which of the following is the immunodominant sugar responsible for the A antigen?
a fucose
b N-acetylgalactosamine
c galactose
d N-acetylglucosamine
b N-acetylgalactosamine
Which of the following is considered to be a high-prevalence antigen?
a Vel
b Jsa
c S
d K
a Vel
The reason that group O individuals have the most amount of H antigen on their red cells compared to other ABO phenotypes is:
a group O individuals produce more precursor type I chain
b group A, B and AB individuals are heterozygous for the H gene
c the O gene produces more transferase enzyme, which produces more H antigen
d H antigen is left unchanged by the absence of A and/or B transferase enzymes
d H antigen is left unchanged by the absence of A and/or B transferase enzymes
c Ax; with an anti-A1
A patient is typed with the results shown in the table. The most probable reason for these findings is that the patient is group:
a O; confusion due to faulty group O antiserum
b O; with an anti-A1
c Ax; with an anti-A1
d A1; with an anti-A

c A3
Given the serologic reactions shown in this table, what is the most likely A subgroup?
a A1
b A2
c A3
d Ax

The enzyme responsible for conferring H activity on the red cell membrane is alpha-:
a galactosyl transferase
b N-acetylgalactosaminyl transferase
c L-fucosyl transferase
d N-acetylglucosaminyl transferase
c L-fucosyl transferase
Even in the absence of prior transfusion or pregnancy, individuals with the Bombay phenotype (Oh) will always have naturally occurring:
a anti-Rh
b anti-Ko
c anti-U
d anti-H
d anti-H
Which of the following antibodies in the LU (Lutheran) system is most likely to be IgM and detected as a direct agglutinin?
a anti-Lua
b anti-Lub
c anti-Lu3
d anti-Aua
a anti-Lua
Which of the following antibodies is neutralizable by pooled human plasma?
a anti-Kna
b anti-Ch
c anti-Yka
d anti-Csa
b anti-Ch
Antibodies from which of the following blood group systems are notorious for causing delayed hemolytic transfusion reactions?
a Rh
b KEL
c FY
d JK
d JK
HLA antibodies are:
a naturally occurring
b induced by multiple transfusions
c directed against granulocyte antigens only
d frequently cause hemolytic transfusion reactions
b induced by multiple transfusions
Genes of the major histocompatibility complex (MHC):
a code for HLA-A, HLA-B, and HLA-C antigens only
b are linked to genes in the ABO system
c are the primary genetic sex-determinants
d contribute to the coordination of cellular and humoral immunity
d contribute to the coordination of cellular and humoral immunity
Isoimmunization to platelet antigen HPA-1a and the placental transfer of maternal antibodies would be expected to cause newborn:
a erythroblastosis
b leukocytosis
c leukopenia
d thrombocytopenia
d thrombocytopenia
What antigens would be found in the saliva of an individual with the genotype Sese Lele AO HH?
a A, H
b Leb, A, H
c Lea, Leb, A, H
d Lea
c Lea, Leb, A, H
Which of the following genes is not in the MHC class I region?
a HLA-A
b HLA-B
c HLA-C
d HLA-DR
d HLA-DR
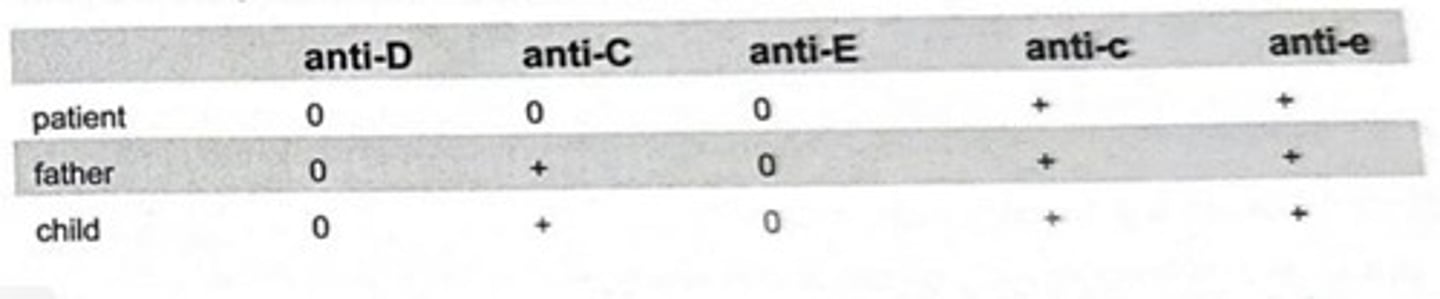
Anti-D and anti-C are identified in the serum of a pregnant woman, gravida 2, para 1. Ten months previously she received Rh immune globulin (RhIG) at 28 weeks' gestation. Test results of the patient, her husband, and the child are shown in the table. The most likely explanation for the presence of anti-D is that this antibody is:
a actually anti-Cw
b from the RhIG dose
c actually anti-G
d naturally occurring
c actually anti-G