Topic 9 - X-Ray Image Detectors
1/80
Earn XP
Description and Tags
ONCOL 234 - Equipment and Imaging. University of Alberta
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
81 Terms
what is the basic idea of x-ray imaging
to produce an image containing clinically relevant information
general sequence of x-ray imaging
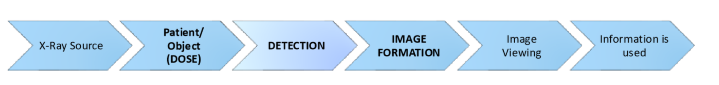
what type of imaging is x-ray imaging?
projection imaging
radiation is transmitted through a region of interest and detected by a detector on the other side
what is the image quality and dose to the patient controlled by?
the mAs and kVp of the x-ray source
what is the tube voltage of diagnostic x-rays
80-150 kVp
what type of anode does it have
rotating anode with tungsten/tungsten-rhenium target
kVp impacts ____
mAs impacts ___
kVp: beam quality
mAs: beam quantity
What happens when a radiation beam enters a patient?
It deposits dose if it interacts with tissue.
What factors affect the amount of dose deposited?
The material’s attenuation coefficient and the beam energy
What are the primary types of photon interactions in tissue at this energy?
Compton scattering and photoelectric absorption.
What is the attenuation coefficient (u)?
It is a property of a material that describes how much the material reduces the intensity of a beam of radiation as it passes through.
the higher the u, the ____ the HVL
lower the HVL
material attenuates radiation better
What does the dose received by the patient depend on?
it depends on the thickness of the region being imaged.
How are most x-rays deposited during imaging?
Most x-rays are deposited as dose, with very few reaching the detector and even fewer being detected.
Why is detector efficiency important?
High detector efficiency helps reduce the dose a patient receives.
What happens during photoelectric absorption?
The photon is absorbed, and all its energy is deposited as dose.
what is the attenuation relationship for photoelectric absorption
Attenuation is proportional to Z³ (more in bone) and 1/E³ (more at low energy).
What happens during Compton scattering?
The photon is scattered, transferring some energy to an electron and depositing some dose.
What is the attenuation relationship for Compton scattering?
Attenuation is independent of Z and only depends on the material's density.
How does photon energy affect attenuation for low energy photons?
For low energy photons, attenuation increases as photon energy increases.
What is the difference between good and bad dose in radiation therapy?
Good dose is delivered to the target, while bad dose is delivered to the surrounding tissue.
What is the ideal situation in imaging regarding dose?
The ideal situation is low dose and high image quality.
What are the 4 main factors impacting radiation dose?
SSD
depth
kVp
mAs
what effect does SSD increase have on dose and quantity of x-rays
dose: decreases
x-rays: ISL - reduction of x-rays
what effect does depth have on dose and x-ray quantity
dose: decrease in dose with depth
x-rays: ISL and exponential attenuation decreases x-rays
what effect does kVp increase have on dose and x-ray quantity
dose: decreases dose
x-rays: more high quality x-rays
what effect does mAs have on dose and x-ray quantity
dose: proportional
x-rays: increases with mAs
How can detector exposure be increased?
Detector exposure can be increased by increasing mAs or kVp.
What is the double dose 15% rule?
Increasing kVp by 15% has the same effect as doubling mAs, both causing the dose received by the patient and the exposure received by the detector to double.
An x-ray tube is operated at 90kVp and 50mAs but the resulting image is underexposed and a 25% increase in exposure is required.
By how much do you have to increase the mAs to achieve this increase in exposure?
To achieve a 25% increase, multiply the original mAs by 1.25.
New mAs = 50mAs × 1.25 = 62.5mAs.
By how much do you have to increase the kVp to achieve this increase in exposure?
Use the 15% rule: increasing kVp by 15% doubles the exposure.
To get a 25% increase, you need to calculate how much 15% plus an additional 10% will increase the exposure.
First increase by 15%: 90kVp × 1.15 = 103.5kVp.
Then, increase by 10%: 103.5kVp × 1.10 = 113.85kVp.
So, the kVp should be increased to approximately 114kVp.
what three broad categories do x-ray detectors fall into?
screen-film radiography
computed radiography
digital radiography
What is screen-film radiography?
Screen-film radiography uses film (analog) to capture the x-ray image.
What is computed radiography?
Computed radiography involves a physical cassette that stores a latent x-ray image, which is then read out and digitized by a machine.
What is digital radiography?
Digital radiography creates the x-ray image as a digital image, either through direct digital radiography (x-ray directly creates an electric signal) or indirect digital radiography (x-ray creates light photons, which then create an electric signal).
Why is screen-film radiography rarely used?
It is rarely used due to newer, more accurate technologies, but is still a cheap method for creating x-ray images.
How does radiation interact with film in screen-film radiography?
Radiation causes a chemical change in the film, which results in a darker region after development.
How is the amount of darkening in screen-film radiography measured?
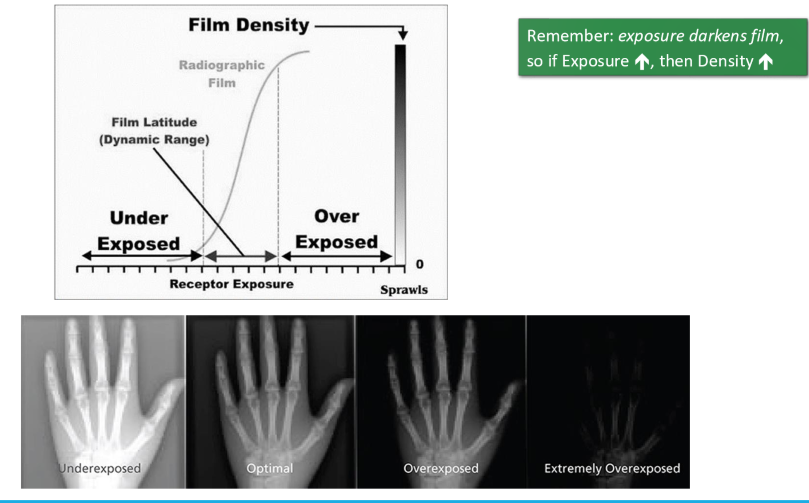
It is measured as optical density (OD) and compared with an H&D curve to determine the exposure.
What is an H&D curve?
An H&D curve (Hurter and Driffield curve) is a graph that shows the relationship between the exposure of film to radiation and the resulting optical density (OD), used to evaluate film sensitivity and exposure.
What is a disadvantage of screen-film images?
They are very sensitive to exposure and can easily be overexposed or underexposed.
what happens to the film when it is exposed to x-rays?
exposure darkens the film
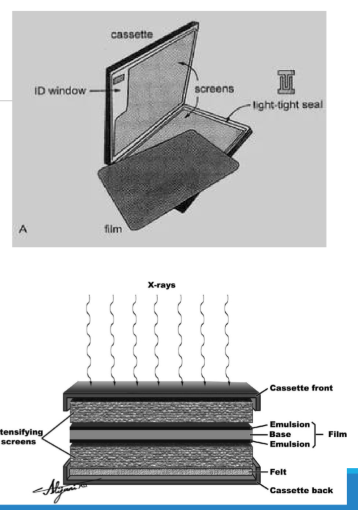
How is screen-film carried in radiography?
Screen-film is carried in a cassette that forms a light-tight seal to protect the film.
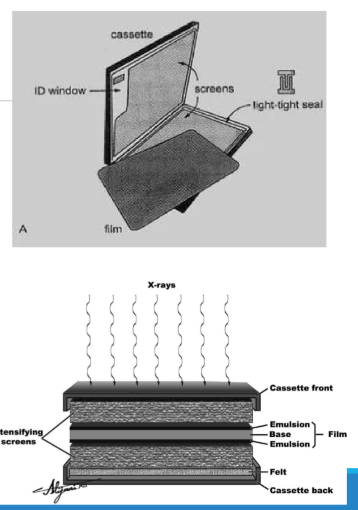
What is the purpose of the foam or felt in the cassette?
The foam or felt helps maintain pressure between the film and the intensifying screens.
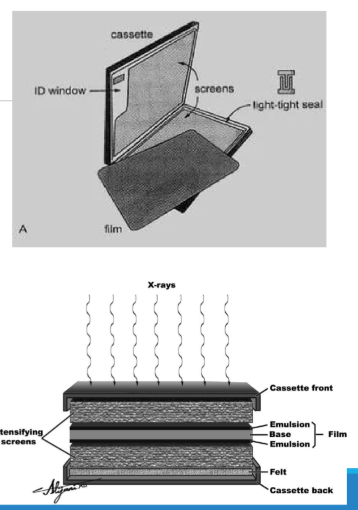
What role do the intensifying screens in the cassette play?
The intensifying screens amplify the x-ray signal, with one screen in front and one behind the film.
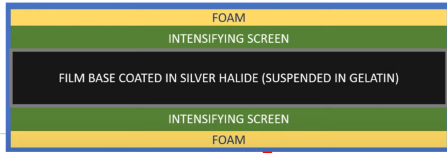
What is the function of the foam in a cassette?
The foam helps maintain pressure between the film and the intensifying screens.
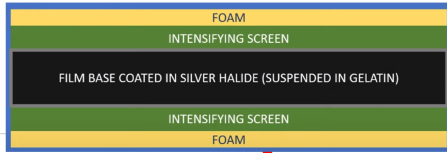
what type of material does the intensifying screen contain?
The intensifying screen contains scintillating material that converts x-rays into visible light, which can be detected by the film.
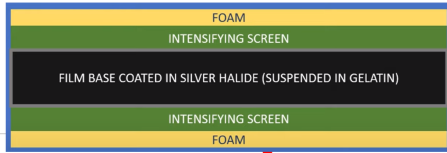
What are the layers of film in a cassette?
The film contains a protective layer, base layer, and the active emulsion layer, which is composed of silver ions (Ag+) and halide ions (Br- or I-) to form silver halide grains.
What is the function of the intensifying screen in screen-film radiography?
The intensifying screen is made of scintillating material that quickly produces light photons after absorbing an x-ray (fluorescence).
What is the most common material used in diagnostic x-ray intensifying screens?
The most common material is gadolinium oxysulfide (Gd2O2S), which is an unstructured scintillating crystal.
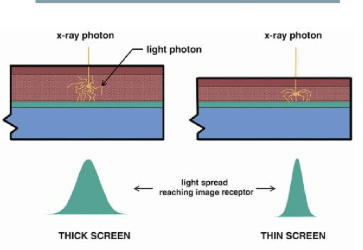
How does the thickness of the intensifying screen affect sensitivity and resolution?
A thicker intensifying screen increases sensitivity but results in worse spatial resolution.
5 steps to screen-film image formation
x-rays hit intensifying screen and are converted into hundreds of photons
these photons hit the the film and cause the reduction of Ag+ into Ag
a latent (not visible) image is formed by neurtal silver atoms on the film
the film is developed to amplify and fix metallic silver in place via chemicals
image can then be seen on a light-box
is image density proportional to exposure
no, it follows a sigmoidal H&D curve
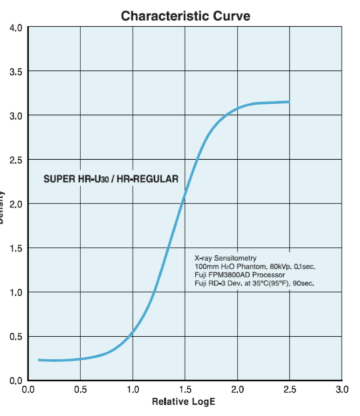
why is dynamic range (latitude) a good thing for x-ray imaging
protects from over/under exposure
What is the scintillation phenomenon?
The scintillation phenomenon is the conversion of X-rays into visible light, used in X-ray imaging detectors.
What is a scintillator in X-ray imaging?
A scintillator is a solid-state detector that converts X-rays into light, typically using phosphor layers of fine grain scintillating powder.
How much more X-rays can scintillation screens absorb compared to film alone?
Scintillation screens absorb 50 times more X-rays than film alone.
What is Computed Radiography (CR)?
Computed Radiography is a two-step process that uses a photostimulable phosphor (PSP) detector to capture and read out X-ray images.
What is a photostimulable phosphor (PSP)?
A PSP is a material, often Barium Fluorohalide (BaFBr), used inside a CR cassette to capture latent images.
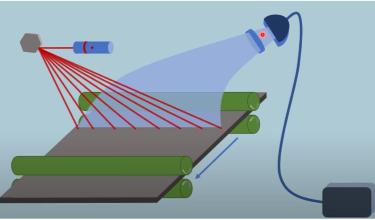
How is the latent image read in Computed Radiography?
The latent image is read out by scanning the PSP with a red laser, which stimulates the emission of blue light.
What happens to the light emitted from the photostimulable phosphor during CR?
The emitted light is collected by a photomultiplier tube (PMT) and converted into an electronic signal.
How is the CR plate prepared for reuse?
The CR plate is erased by bright light after the image is read out and is then ready for reuse.
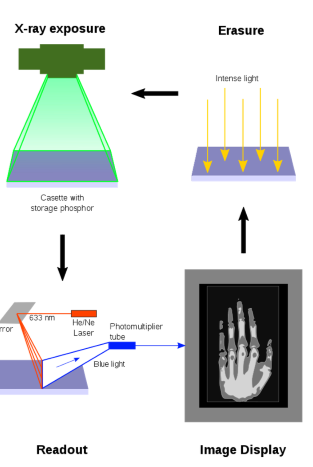
How does Computed Radiography (CR) capture x-ray energy?
CR uses a phosphorescent material that captures x-ray energy in electron traps, which are later released through light stimulation.
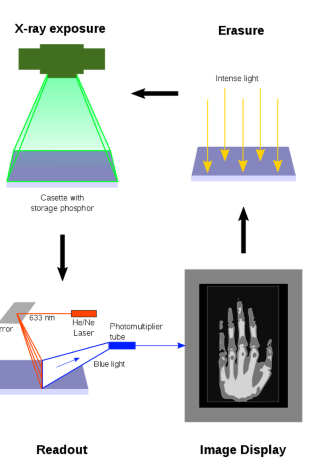
How is light stimulation in CR similar to OSLDs?
Like OSLDs, CR releases trapped electrons through light stimulation to produce an image.
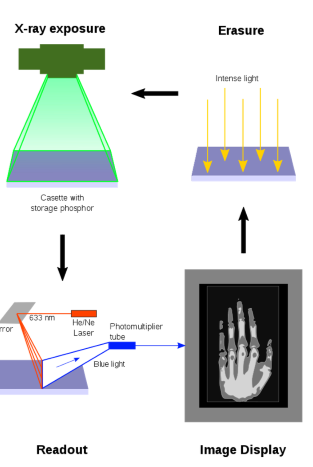
What happens after the cassette is exposed in Computed Radiography (CR)?
The electrons are trapped in the F-centers, creating a latent image in the CR plate that contains the information for the visible image.
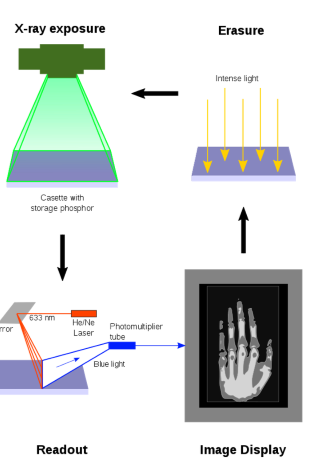
How is the latent image in the CR plate formed into a visible image?
The electrons in the F-centers are released by stimulating them with red laser light (≈700nm), allowing them to escape the traps.
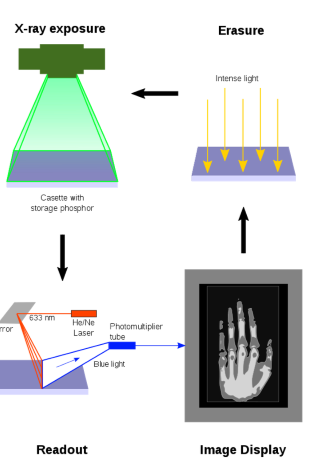
What happens when the electrons in the F-centers are released in CR?
The electrons recombine with Eu3+ ions, emitting a blue photon (≈400nm) in the process.
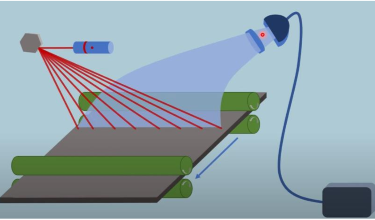
How is the blue light captured during the CR read-out process?
The blue light is captured by a light pipe, which filters out red light and directs the blue light towards a photomultiplier tube (PMT).
What happens after the blue light is captured by the PMT?
The PMT converts the blue light photons into an electric signal, which is then converted into an image.
What happens to the CR plate after an image is digitized and stored?
The CR plate is usually erased so it can be reused for a new image.
How is the CR plate erased?
Bright white light is shone on the CR plate to release all the trapped electrons.
What is Digital Radiography (DR)?
Digital radiography refers to the process of capturing radiographic images using digital detectors, with no physical cassettes involved.
How is the image made in Digital Radiography (DR)?
The image is created digitally almost immediately after exposure.
What are the two main types of Digital Radiography (DR)?
1. Indirect digital radiography:
X-rays create light photons, which are converted into an electric signal.
2. Direct digital radiography:
X-rays directly create an electric signal.
What is used in Indirect Digital Radiography to convert X-rays into visible light?
A scintillating layer made of crystalline cesium iodine (CsI) is used to convert X-rays into visible light.
What is the role of the tubular structure in CsI crystals?
The tubular structure of CsI crystals helps direct light photons towards the detector, improving spatial resolution.
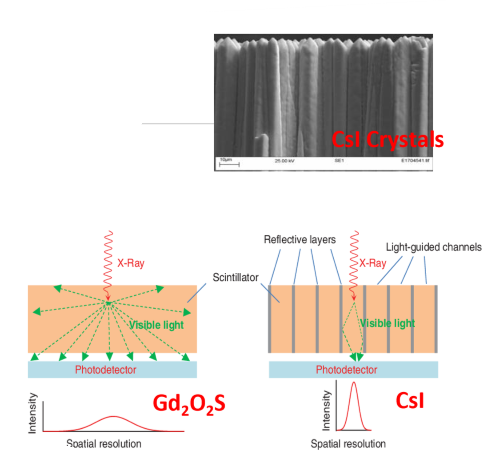
How is the light from the scintillating layer detected in Indirect Digital Radiography?
The light is directed towards small detectors that convert it into electricity and then into pixel values.
What are the three most common photodetectors used in modern systems?
charged coupled devices (CCD)
thin film transistors (TFT)
complementary metal-oxide-semiconductors (CMOS).

How do CCDs work to create an image?
Light releases electrons that accumulate on the CCD, and the charge is read out line by line and converted into a digital pixel value.
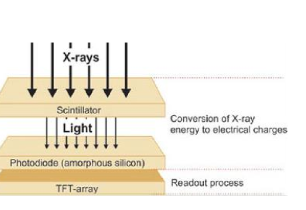
What is the function of photodiodes in TFT systems?
Photodiodes are semiconductors with a p-n junction that convert visible light into electrons.
How does Direct Digital Radiography (DR) work?
In direct DR, X-rays are directly converted into electrons, with no intermediate scintillating step.
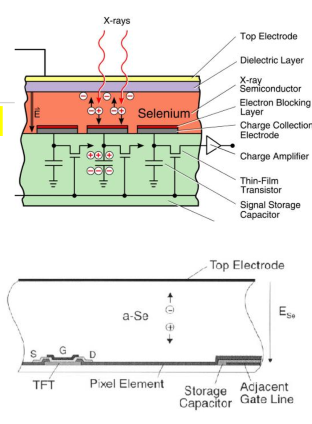
What happens to the X-rays in Direct Digital Radiography?
X-rays are converted into electron-hole pairs in an amorphous selenium semiconductor.