mTBI: physiology, consequences and recovery
Define concussion
Explain the pathophysiology of concussion and why it is difficult to diagnose
Describe the common symptoms of concussion and how they relate to the pathophysiology
Compare and contrast methods of concussion diagnosis and explain the limitations of each
Describe one rehabilitation strategy for each of (1) acute concussion, and (2) persistent post-concussive symptoms
1/37
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
38 Terms
Define concussion
Explain the pathophysiology of concussion and why it is difficult to diagnose
Describe the common symptoms of concussion and how they relate to the pathophysiology
Compare and contrast methods of concussion diagnosis and explain the limitations of each
Describe one rehabilitation strategy for each of (1) acute concussion, and (2) persistent post-concussive symptoms

Acquired Brain Injury (ABI)
• Brain damage that occurs after birth
*any
*not smtg ur born with, smtg that happens to ur brain after ur born
Non-traumatic
-have brain damage because of illness, infection, tumor
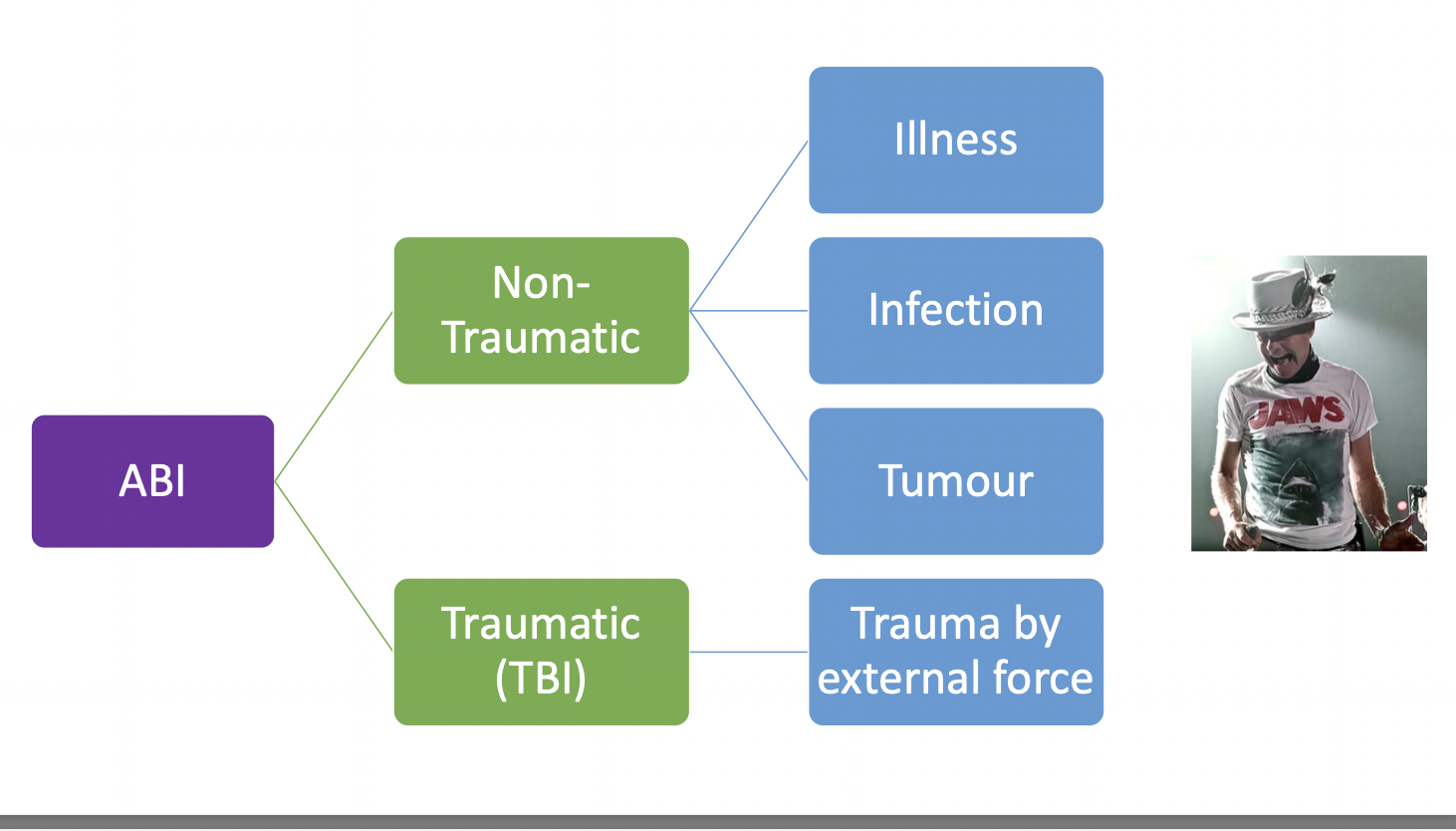
Traumatic
Classifying ABI
mild → moderate → severe
concussion is a form of mild (even when clincians say mod or severe concussion its still moderate)
Concussion
• Type of mild traumatic brain injury (mTBI)
• a complex pathophysiological process that affects the brain and is induced by biomechanical forces (traumatic) (McPherson et al., 2019)
most common in football players*
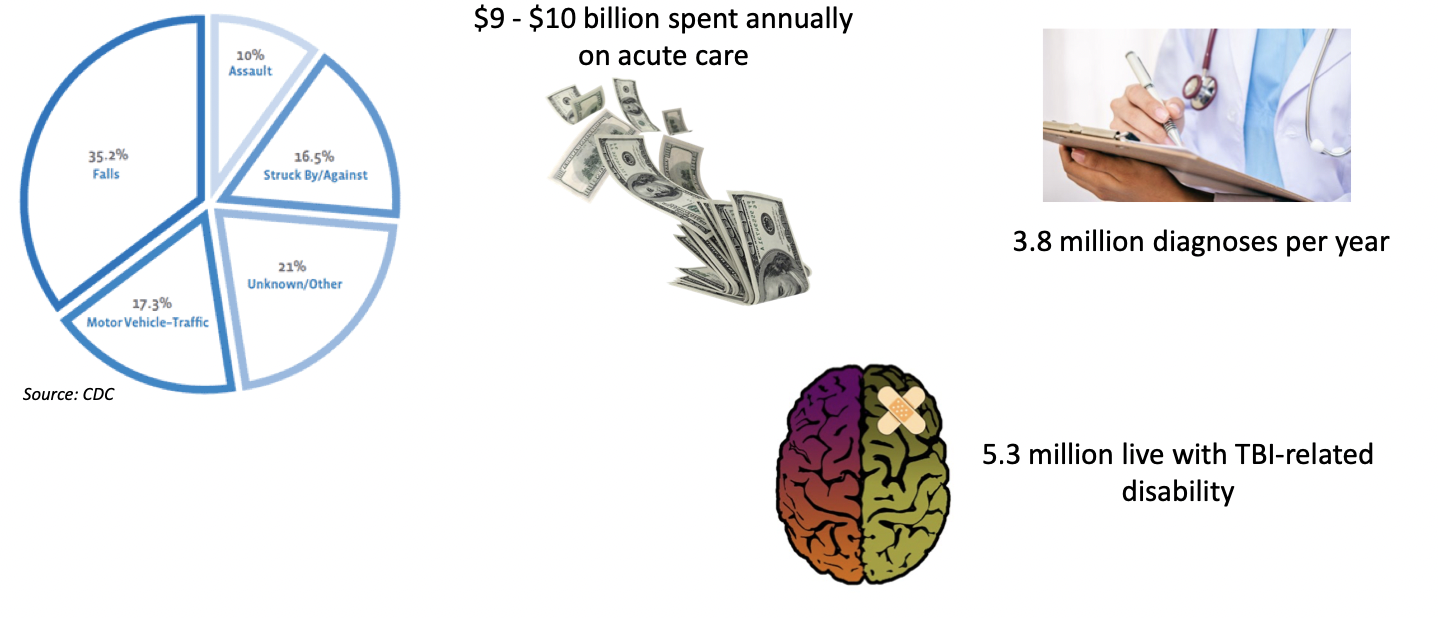
Major Health Concern Beyond Sports
$9 - $10 billion spent annually on acute care
3.8 million diagnoses per year
5.3 million live with TBI-related disability (long term disability after tbi- can occur after a concussion too)
10% from assault- especially domestic assault, very understudied
sport related only 25%
Concussion
• Type of mild traumatic brain injury (mTBI)
• a complex pathophysiological process that affects the brain and is induced by biomechanical forces (McPherson et al., 2019)
• Diffuse/multifocal injury- not rlly one area of brain affected, get damage throughout the brain and can be multiple sites, or just generally brain across the brain
• Neuronal stretching /shearing/ compression (brain hitting skull) /damage
• Cognitive, motor, & physical symptoms
DIRECT- brain hit skull
-hit on head, causes compression
-can sustain a concussion w/o being hit in the head
acceleration/deceleration- very quickly
shearing of the neurons, brain anchored to the brainstorm, starts to move froward but anchor moving backward now you have stretching of those neurons
brainstem moving it one direction and other is pulling it the other way
-could get shearing of those neurons
Blast
-often get concussions during training in soldiers
-more moderate or severe tbis- not the only way they can sustain a blast but most common- they are the most common ppl that will have a blast concussion
**any one of these leads to damage of the neurons
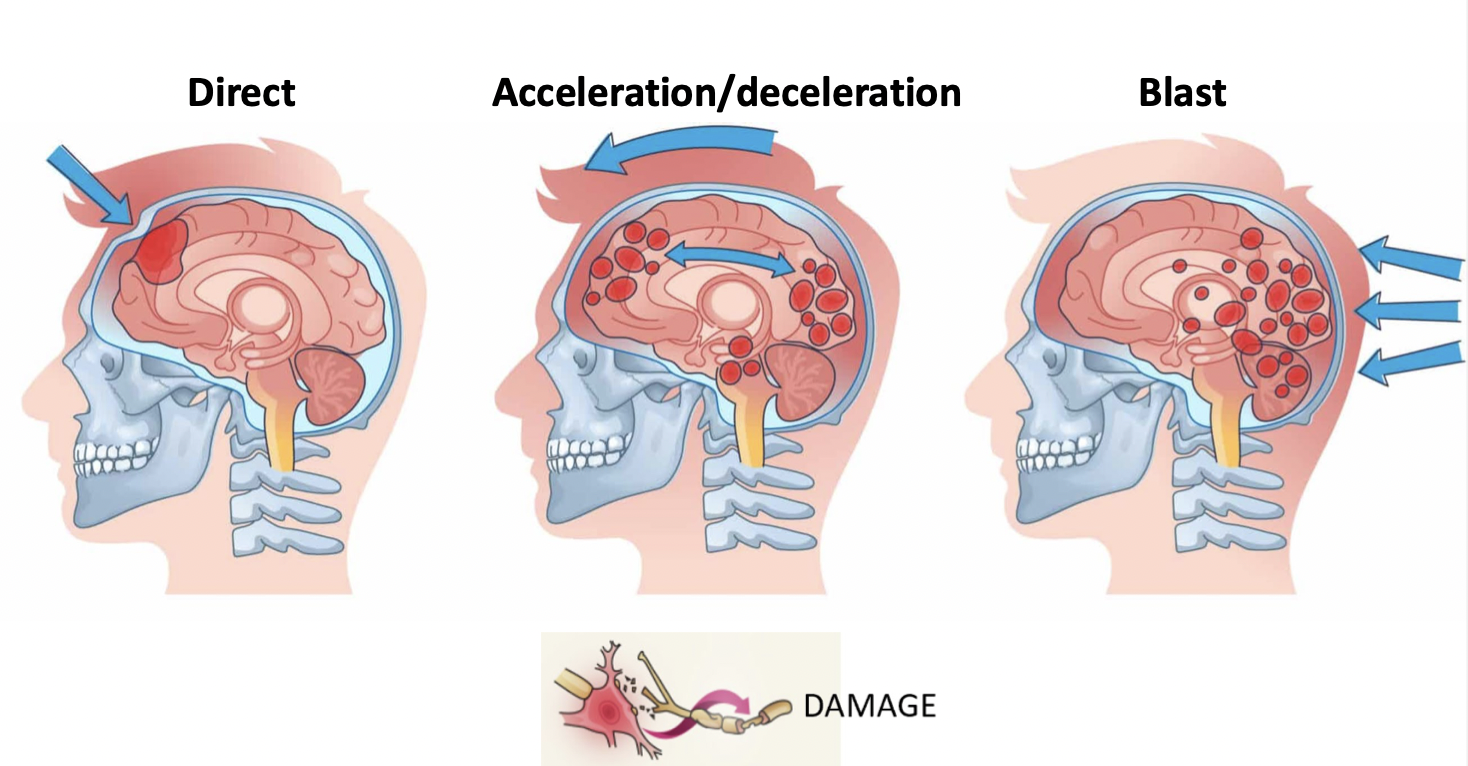
chart on ipad
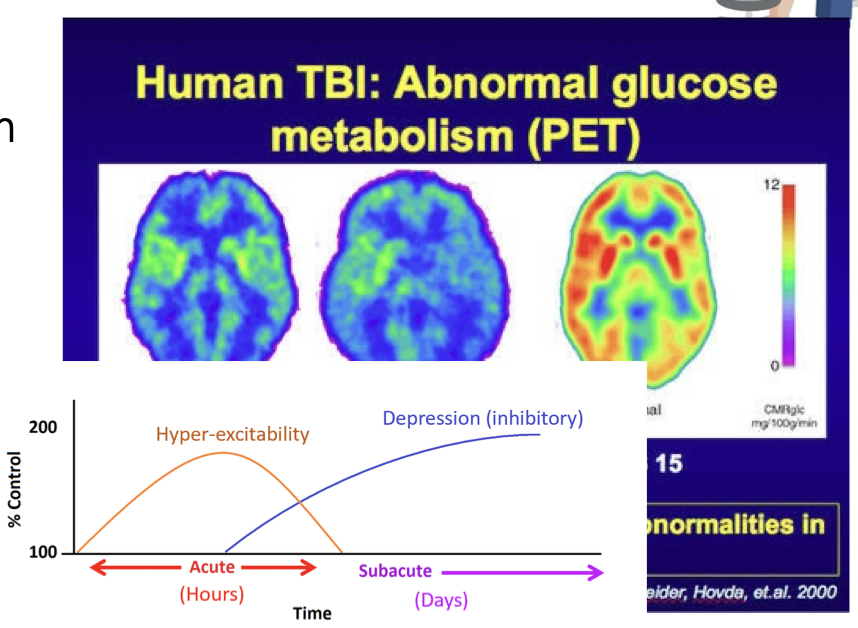
Neurometabolic Cascade
Changes in metabolite and ion concentration in brain after mechanical injury (Giza & Hovda, 2001)
*process of changes in communication over time is called. the neurometabolic cascade
first 24 hours- brain is in hyper excitable state (part of excitotoxicity that we just describe)
-over days you get inhibitory or inhibition so it is harder to activate those brain regions after injury- challenging to study- everyone follows a different route
give animal concussion- hit in same brain region, same force not true for everyone
if you have seen a concussion its just means that concussion
-everyone is different this is a rough timeline
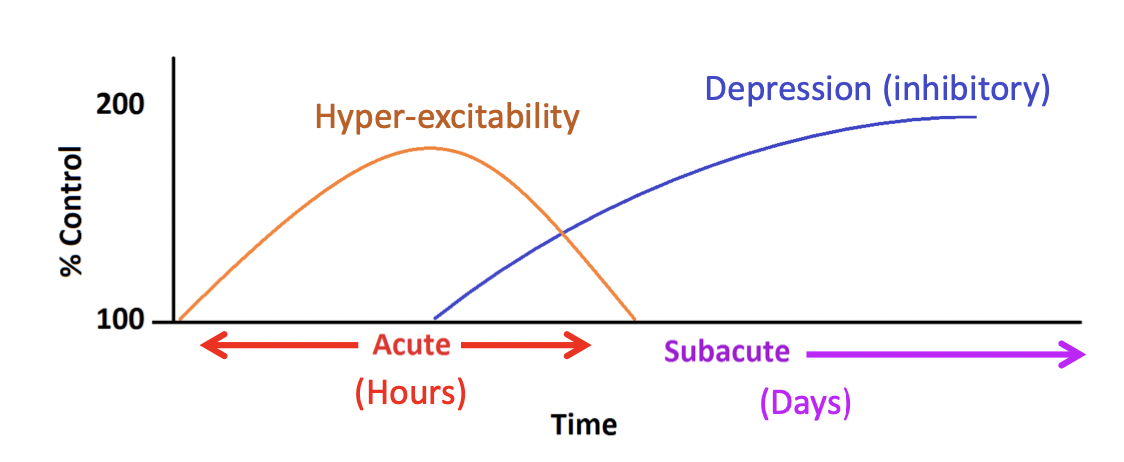
so many brain regions affected
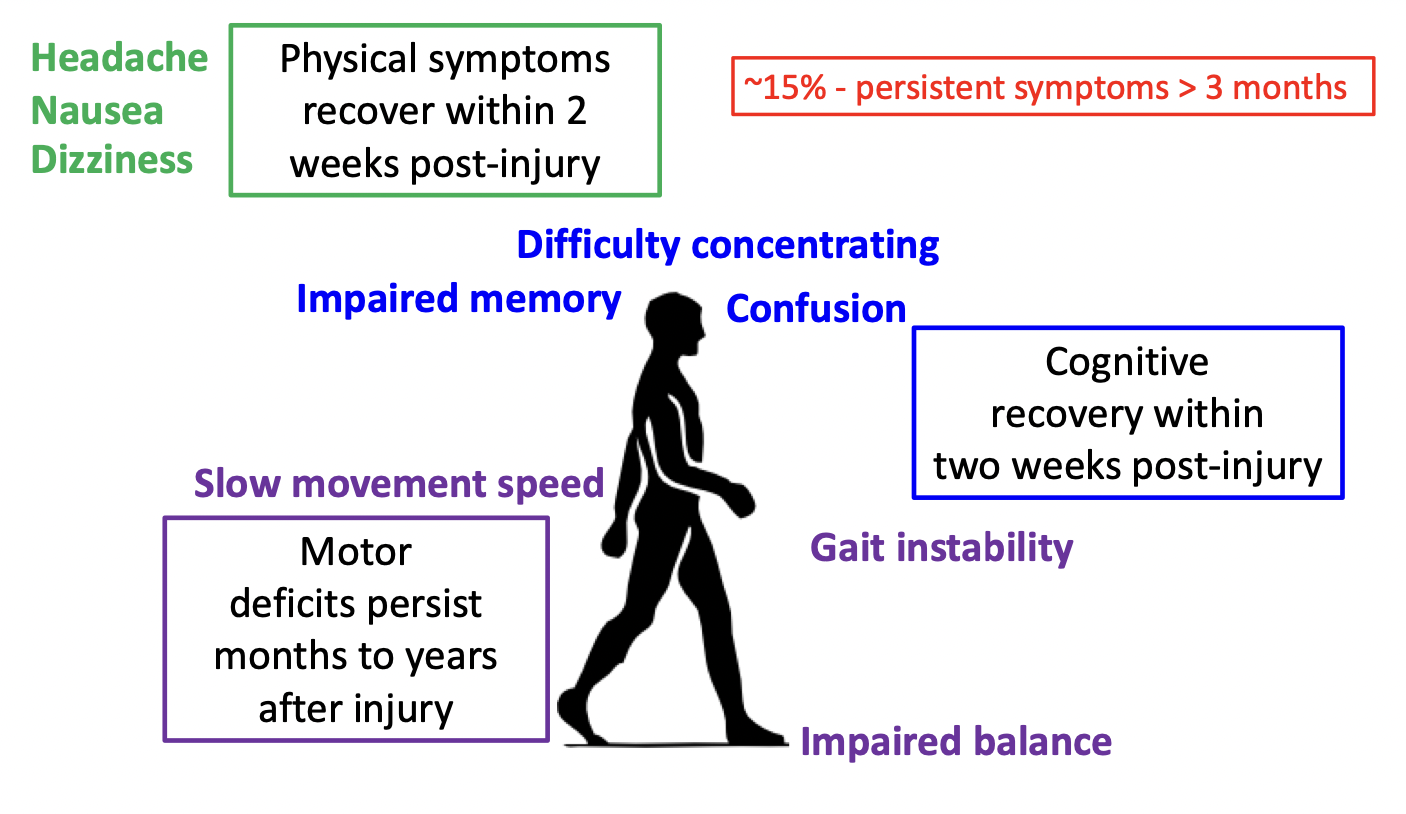
Physical symptoms recover within 2 weeks post-injury (headache, nausea, dizziness) occur almost immediately- timeline varies for different individuals
~15% - persistent symptoms > 3 months
Motor deficits persist months to years after injury- slow movement speeds, impaired balance, gait instability (mediolateral sway)
Cognitive symptoms recovery within two weeks post-injury- can interfere with daily activities (difficulty concentrating, impaired memory, confusion)
*person says my symptoms have recovered but in a lab we can see they are not fully recovered- its not enough that they notice but its there, and its there even more if they are trying to do a motor task in addition to cognitive task
-scary when thinking about athletes returning to field after 2 weeks of injury
15% of those who sustain a concussion there symptoms do not recover within 2 weeks- still experience cognitive and motor deficits
Diagnosing Concussion
Structural imaging (e.g.MRI, CT)
-PET scans
-Blood scans- for the most part have been developed here at western
-Clinical assessment
Diagnosing Concussion
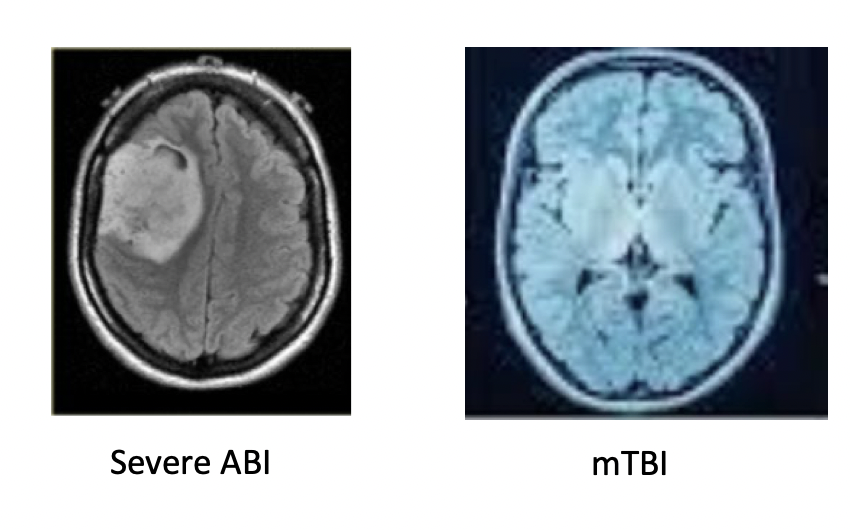
Typically, no visible abnormalities on standard imaging (e.g. MRI, CT)
structural imaging does not work well for diagnosing a concussion
concussion is not severe it is a mild traumatic brain injury
-little tears in the neurons- current imaging not sensitive enough to see individual neurons
*used to rule out a moderate or severe injury- microstructural damage
Abnormal glucose metabolism in the brain after concussion
-pet scans for glucose metabolism
-after a mild brain injury or concussion there is evidence of
red- more glucose metabolism
blue- less glucose metabolism
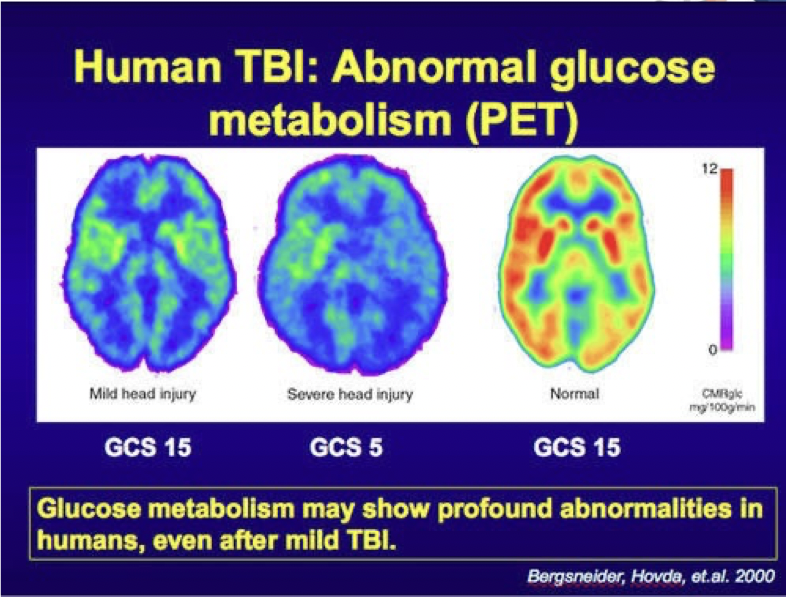
Based on the physiology of concussion, how would you expect glucose metabolism to change in the acute and sub-acute post- concussion stages
-acute phase may be normal or high and the sub-acute stage would be lower
List one limitation of using brain glucose metabolism to diagnose concussion
-would not know definititively if it were a concussion
-differs depending on how diffuse or focal the injury is
-maybe a high glucose diet
-took image during acute phase- glucose metabolsim might look normal
-brain uses glucose for its energy- maybe sickness or smtg causes more glucose uptake- they try to standardize that across people
Abnormal glucose metabolism in the brain after concussion
Limitations
-cost
-access- unless nfl player with scanner locker room
-time sensitive
*in canadian healthcare system it could be days or eeks until you get one
-do not have baseline measures to know whether this is normal or abnormal
Blood Test
Two biomarkers in blood stream after concussion (as a result of inflammation in the brain)
FDA approved in 2023
Used to rule out need for CT- not to diagnose a concussion but to determine if there is smtg going on
Time sensitive-
difficult because people dont feel the need to get it checked out until 48 hours later- arent seeking in the phase where biomarkers there?- more into the subacute phase
“Sideline” Assessments
ImPACT
• Neurocognitive computer test
• Pre/post injury + recovery
*been around the longest, was designed for athletes to have a baseline so if they got injured they could tell
-college sports in the US
SCAT-6
• Neurological screening
• Occulomotor evaluation- eyes and head movings
• Cognitive evaluation
• Patient history- have you had a prior concussion
• Patient-reported Symptoms
Suspected concussion with 1 or more of the following:
Symptoms: somatic (e.g., Headache), cognitive (e.g., fogginess), and/or emotional (e.g., lability)
Physical signs: e.g., LOC, amnesia, neurological deficit
Balance impairment: e.g., gait unsteadiness
Behavioural impairment: e.g., irritability
Cognitive impairment: e.g., slowed reaction time
RED FLAG- nausea, loc
List at least one limitation for each of the ImPACT and SCAT-6 assessments
ImPACT
*need their device and software to administer it- not having access to it
*changes in baseline- differences just because of maturation
SCAT-6
*a lot of players want to keep playing so they will downplay their symptoms
*ppl with learning impairments would not do well
“Sideline” Assessments- LIMITATIONS
IMPACT:
-neurocognitive function only
-potential “cheating” on baseline- athletes learn how they were diagnosed so they did poor on purpose so it did not look a concussion after i have one
-time
SCAT-6
-does not r/o a concussion definitively
-time (15-20 minutes)- how often is this done properly for someone who is under pressure to get back into the game (rushed, skip parts)
-Developed for sports- designed for sideline assessment to clear an athlete
Non-Sport Assessment of Concussion
• Patient history
• Injury description
• Symptom assessment
• Patient reported symptoms
E.g. BSI-18, Rivermead
• Clinician evaluation of symptoms
E.g. GOS-E
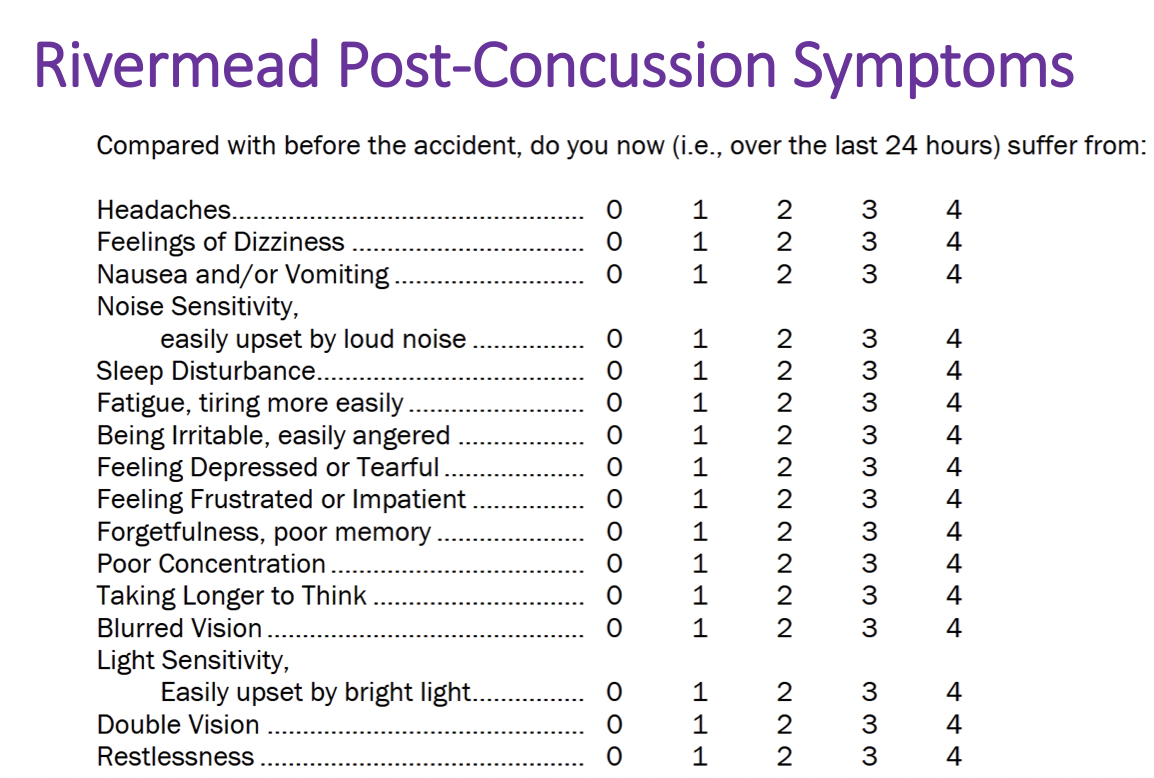
Rivermead Post-Concussion Symptoms
-some of these symptoms are symptoms people experience in everyuday life (fatigue, poor concentration)
GOS-E
dead?- wouldnt be in the clinicians office getting assessed
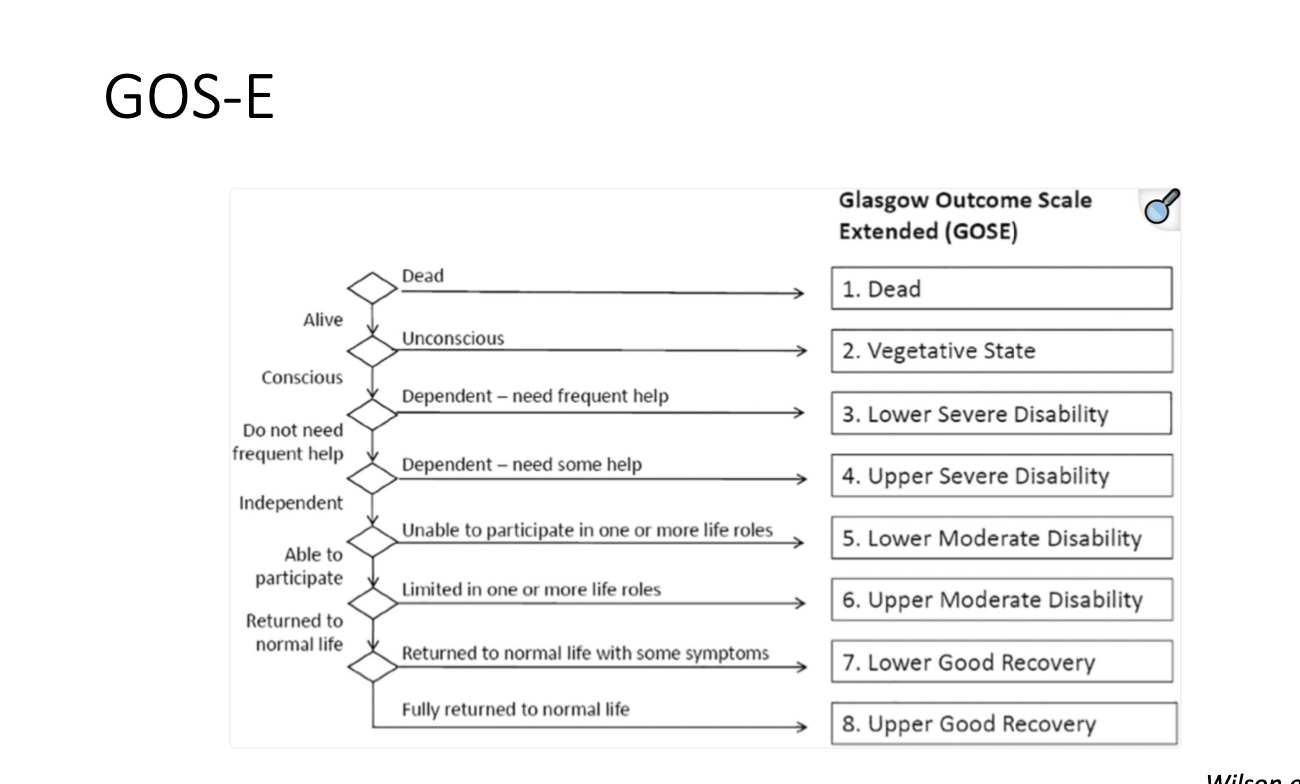
Identify at least one limitation of using symptom scores to diagnose concussion
-everyones interpretation is different
-confirmation bias- doctor gives you form for concussion
-symptoms could occur in everyday
-relying on the person being honest
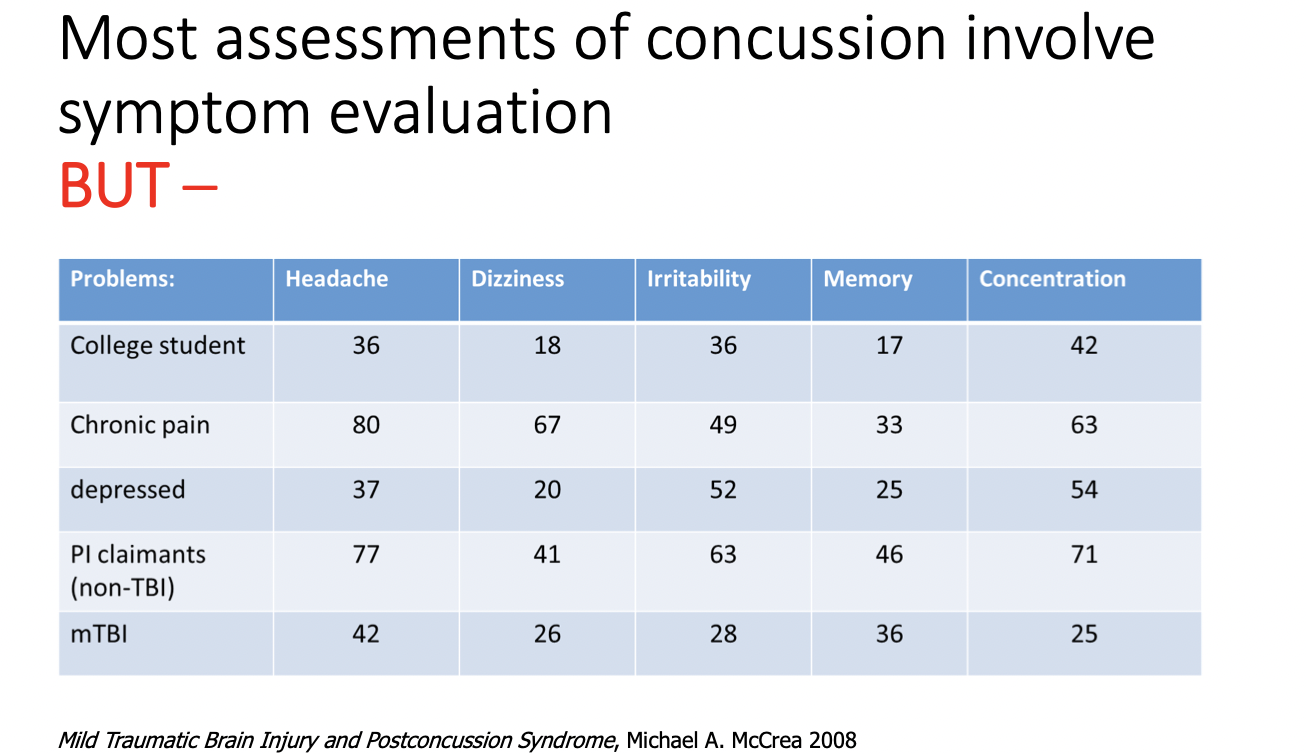
Most assessments of concussion involve symptom evaluation BUT –
*dont memorize these numbers
*no one would score a 0 on rivermead- makes it rlly hard to diagnose because ppl feel things
Additional Considerations
May be racial, SES, and educational differences in symptom reporting
-bias towards higher education person, some language is normal for them but not others whether or not if they have a concussion there are some differences
Females often report more symptoms than males and take longer to recover - WHY?
-more stigma on males for reporting symptoms (feel like they cant say they feel depressed or have a headache)
-neck muscle strength and related to concussion?- some data to support that female might have more severe injuries because neck musculature is weaker
-hormonal influence?
-symptom overlap with menstural cycle symptoms- not related to concussion, but gaining more because of
-honesty in reporting
Rowan’s Law
Named in memory of Rowan Stringer
-passed away after multiple concussions
Goal: To protect amateur athletes
Toolkits for coaches, athletes, parents to improve concussion awareness and safety
When in doubt, take them out
Concussion Recovery/Treatment
-the view has changed a lot in the last 20 years
Previous view:
• Complete cognitive and physical rest
• Wake the patient every hour
Current view:
• Limit screen time
• Social impacts of complete rest may worsen concussion symptoms (take them out of school, sports is more detrimental, especially in kids)
• After 24-48 hours, physical activity is beneficial to recovery
• Sleep is beneficial- waking someone up every hours is not beneficial let them sleep
Buffalo Concussion Treadmill Test
• First group to view physical activity as beneficial to concussion recovery
-this group located at university of buffalo
Assessment:
Walking on a treadmill, increasing incline and speed, until an increase in symptoms
Note heart rate when symptoms increase
Prescription:
• 20-30 minutes, 5 days/week• HR at 80-90% of symptom threshold
• High intensity = negative outcomes
*have patient report how they feel on the likert scale
*most of this has been done in a supervised clinic
*ppl go too high intensity there is a negative effect, recovery slower and symptoms worse
Effects of PA on Concussion Symptoms
Large, positive effect of physical activity on concussion symptom resolution
Regardless of:
- PA type
- Symptom scale
- MOI
- Time since injury
0 line= no effect (good or bad)
bunch of different studies
right= positive effect, shortened recovery time, improved symptoms
*every single study shows a benefit of physical activity on concussion and symptom resolution, regardless of PA
thats acute within 48 hours but what about those
Persistent Post-Concussive Symptoms (PPCS)
used to be call post concussion syndrome
Symptoms lasting longer than expected (>2 weeks)
Definition varies, typically ~3 months post-injury
Most at-risk – unknown
Multiple concussions?
Vestibular symptoms? -balance control or tracking ocular movements
frustrating and debilitating
Rehab of PPCS
• Assessment of symptoms
• Targeted interventions for specific symptoms e.g. pt for physical balance, speech language if problems with language production
• Multidisciplinary teams
• E.g.PT,OT,SLP
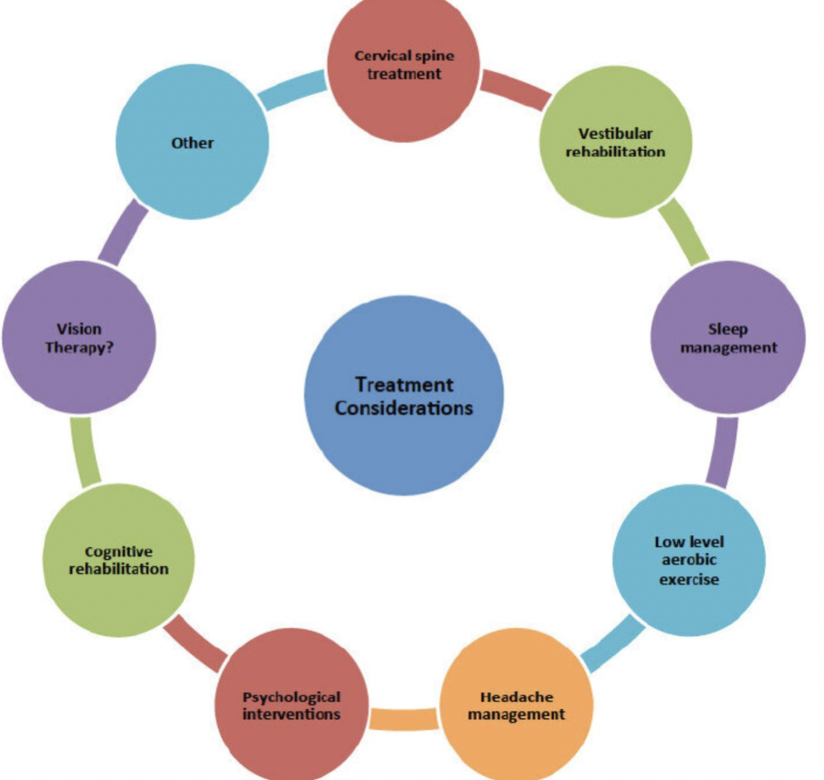
Brain Ex90
Can sign up for this program, waitlist for this program because seems to be working rlly well
• Designed and delivered at Parkwood Hospital
• Physical therapists + occupational therapists
• Weekly 90-minute session
• 30-minute circuit training -usually led by pt
• 20-minute education session- pt
• 30-minute circuit training
• 10-minute self management session (with OT)
Multidisciplinary approach may be beneficial for people with PPCS
Circuit Training:- not only physical but cognitive and balance
• Cognition
• Vision
• Vestibular
• Balance
• Endurance
• Neck dysfunction
Improvement in subjective outcomes:
• Rivermead symptom scores
• Anxiety rating e.g. sit at a computer without symptoms- frustrating, a lot of worries
• Patient satisfaction
• Goal achievement
****this program has shown significant reduction in the anxiety and involvement in program helping improve their function and symptoms