Lectures 1-3
1/62
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
63 Terms
Arterial blood pressure
Force exerted by blood on arterial walls determined by cardiac output and systemic vascular resistance
Pulse pressure
Difference between systolic and diastolic pressure
Mean arterial pressure (MAP)
Diastolic plus one third pulse pressure
Neural regulation of BP
Fast, short-term control via autonomic nervous system and cardiovascular center in medulla
Norepi channels/effects in heart
Sympathetic, Beta 1 (most), Beta 2 and Alpha 1 → + inotropy/contraction, + chronotropy/heart rate, + dromotropy/conduction velocity AV node, exercise= cardiac sympathetic fibers release (not adrenal medulla)
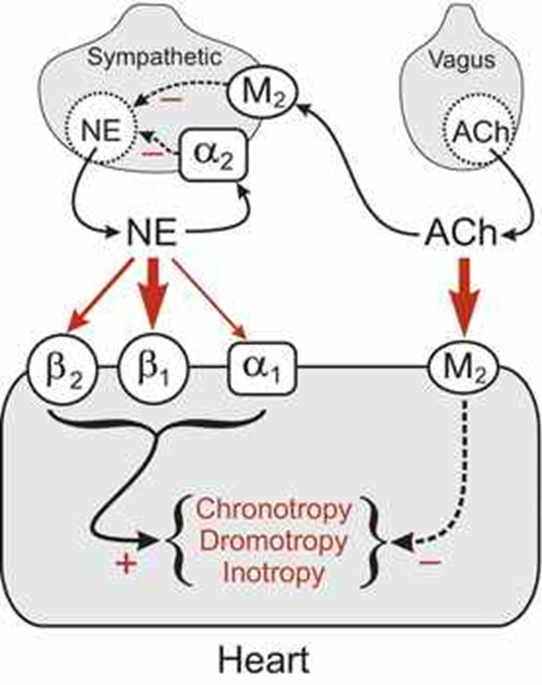
ACh channels/effects in heart
Parasympathetic, M2 → - inotropy/contraction, -chronotropy/heart rate, - dromotropy/conduction velocity AV node
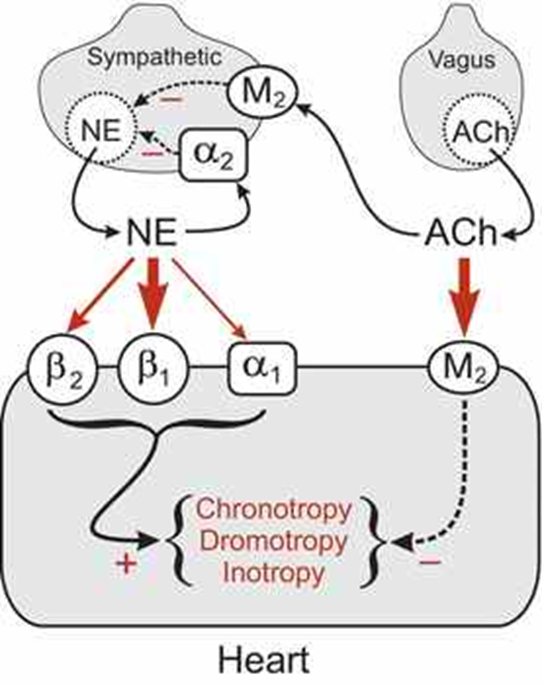
Norepi channels/effects in blood vessels
Sympathetic, Alpha 1 (most), alpha 2 and beta 2 → increased vascular tone
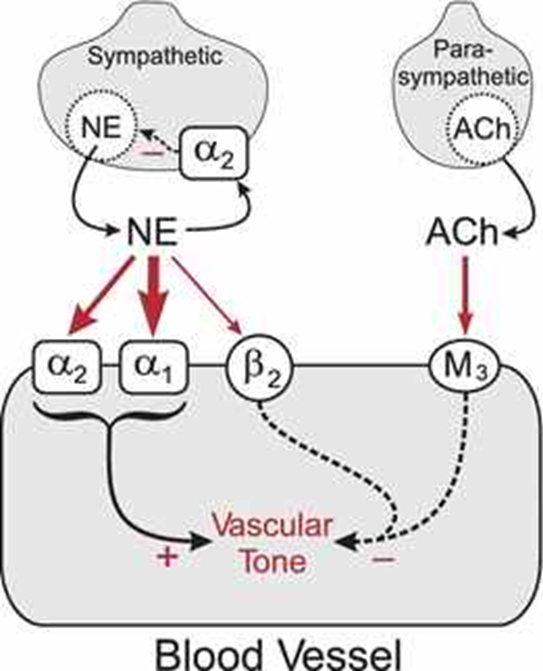
ACh channels/effects on blood vessels
Parasympathetic, M3 → decreased vascular tone
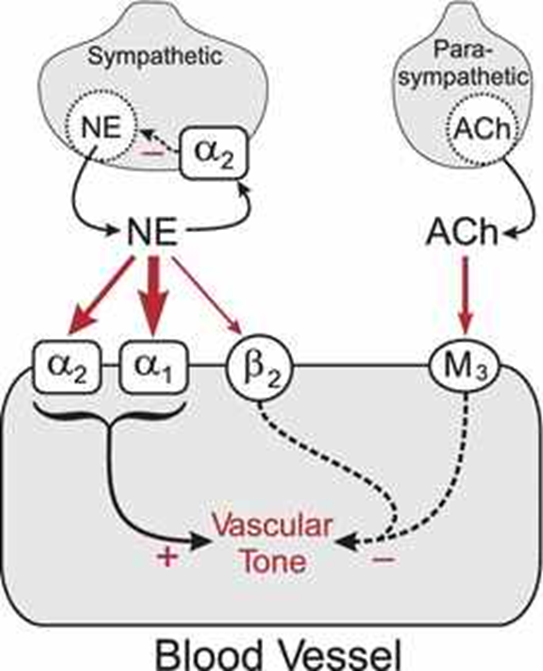
Renal regulation of BP
Long-term control via regulation of extracellular fluid volume and RAAS
Hormonal regulation of BP
Uses circulating hormones to cause vasoconstriction or vasodilation
Local regulation of BP
Uses local vasoactive substances to adjust vessel diameter
Cardiovascular center
Located in medulla integrates input to regulate heart and vessels
Baroreceptor reflex
Primary short-term mechanism responding to stretch in carotid sinus and aortic arch (increased BP= increased firing, decreases sympathetic and increases parasymp to lower BP)
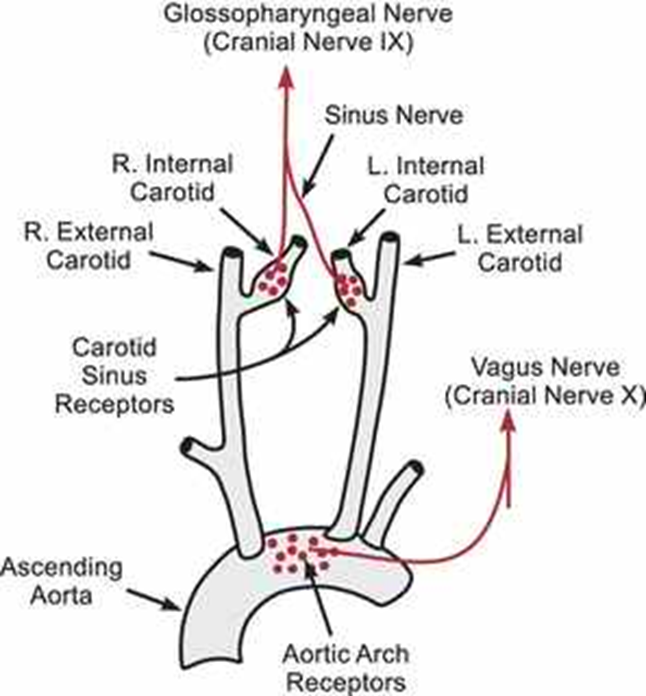
Baroreceptors locations
Aortic arch → vagus nerve, carotid body → glossopharyngeal nerve
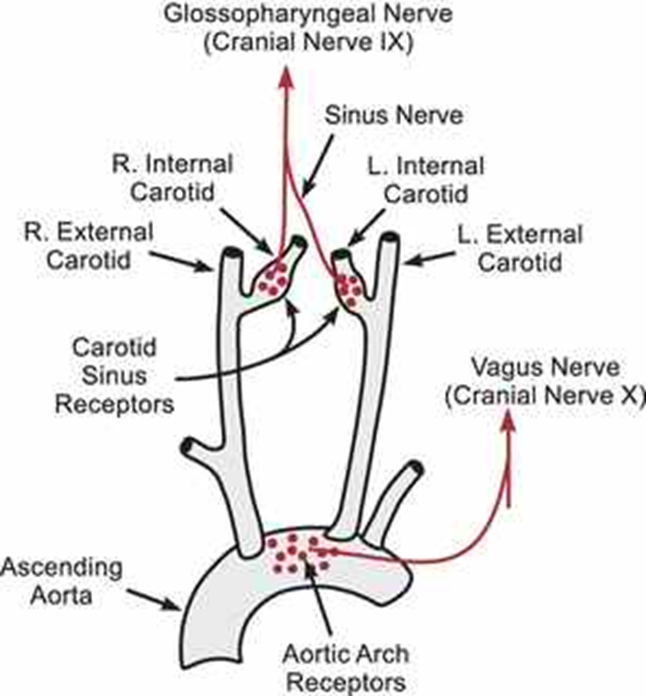
Chemoreceptors
Respond to low oxygen, high carbon dioxide, and low pH to increase sympathetic activity, peripheral (near carotid/aorta) and central (medulla)
Ischemic brain reflex
Severe hypotension causes insufficient blood flow to brain + intense sympathetic response/systemic constriction to raise BP (increased MAP)
Cushing reflex
Increased intracranial pressure leads to ischemia to brainstem → strong sympathetic reaction leadding to increased BP/MAP and reflex bradycardia
Pain reflex
Pain from myocardial ischemia/infarction → increases sympathetic activity raising BP and heart rate, sweating
Vasovagal reflex/Syncope
Increased vagal tone → sympathetic withdrawal of vascular tone, decreases heart rate and BP/MAP causing fainting (blood flow to brain decreases)
Long-term BP regulation
Primarily controlled by kidneys, hormones and local vascular mechanisms
Effective circulating volume
Volume of blood effectively perfusing tissues regulated by renal and hormonal systems
Renin-angiotensin-aldosterone system (RAAS)
Hormonal system increasing BP via vasoconstriction and fluid retention
Angiotensin II
Potent vasoconstrictor increasing calcium and vascular tone
Atrial natriuretic peptide (ANP)
Decreases BP by promoting sodium and water excretion and vasodilation
Vasopressin (ADH)
Increases water reabsorption and causes vasoconstriction increasing BP
Local autoregulation
Ability of tissues to maintain constant blood flow despite pressure changes
Active hyperemia
Increased blood flow in response to increased metabolic activity
Reactive hyperemia
Increased blood flow following temporary occlusion
Myogenic response
Vascular smooth muscle contracts when stretched and relaxes when pressure decreases
Metabolic vasodilation
Hypoxia and metabolites cause vasodilation to increase blood flow
Endothelial function
Maintains balance between vasodilation and vasoconstriction via released factors
Nitric oxide (NO)
Key vasodilator that also has anti-inflammatory and anti-thrombotic effects
Prostaglandin I2 (PGI2)
Endothelial vasodilator derived from arachidonic acid
Endothelin
Potent vasoconstrictor produced by endothelium
Histamine
Vasodilator released during inflammation increasing capillary permeability
Control of arterioles
Basal tone local metabolites and sympathetic vasoconstriction regulate diameter
Control of veins
Sympathetic tone and pressure regulate venous capacitance and blood distribution
Microcirculation
Includes arterioles capillaries and venules responsible for exchange and resistance
Role of arterioles
Primary resistance vessels controlling blood flow and pressure
Role of capillaries
Site of exchange of gases nutrients and waste
Role of venules
Capacitance vessels determining blood volume distribution
Precapillary sphincters
Regulate entry of blood into capillaries
Vasomotion
Intermittent contraction of sphincters controlling capillary perfusion
Capillary types
Continuous fenestrated and sinusoidal differing in permeability
Bulk flow
Movement of fluid driven by pressure gradients across capillaries
Diffusion in capillaries
Movement of solutes down concentration gradients following Fick’s law
Starling forces
Hydrostatic and oncotic pressures determining fluid movement across capillaries
Net filtration pressure (NFP)
Net force driving fluid out of or into capillaries
Filtration vs reabsorption
Filtration dominates at arterial end and reabsorption at venous end
Lymphatic system
Returns excess interstitial fluid to circulation and maintains fluid balance
Lymphatic pump
Uses vessel contraction skeletal muscle and valves to move lymph
Edema
Excess accumulation of fluid in tissues due to imbalance of filtration and removal
Causes of edema
Increased hydrostatic pressure decreased oncotic pressure increased permeability or impaired lymph drainage
Special circulations
Organ-specific blood flow regulation based on metabolic and functional needs
Coronary circulation
Primarily regulated by local metabolites to match oxygen supply to demand
Coronary blood flow timing
Greatest during diastole due to vessel compression in systole
Cerebral circulation
Highly regulated to maintain constant flow and prevent pressure changes
Cerebral blood flow control
Driven by CO2 pH metabolic activity and autoregulation
Functional hyperemia in brain
Increased blood flow to active brain regions
Skeletal muscle circulation
Regulated by metabolites during exercise overriding sympathetic tone
Skeletal muscle blood flow changes
Increases dramatically during exercise to meet oxygen demand
Cutaneous circulation
Regulates heat loss via changes in blood flow to skin
Thermoregulation in skin
Sympathetic control adjusts vasoconstriction or vasodilation based on temperature