Lids /Lashes /Ocular Adnexa/Orbit Disease
1/19
Earn XP
Description and Tags
Lids
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
20 Terms
Bump on lid
Questions: How long? (Acute vs chronic), Pain vs no pain? Does it come and go? Does it change in size or color or texture (thickening)? Any recent trauma or surgery?
Chalazion: Blocked gland that causes a painless lump on the eyelid, often resolving on its own but sometimes requiring treatment.
Treatment: 10 minutes warm compress BID with lid massage. If persists longer than 3-4 weeks, then referral to oculoplastics for incision and drainage or steroid injection.
Hordeolum: Blocked gland that results in acute tender infection and painful swelling on the eyelid, often referred to as a stye. Associated with preseptal cellulitis. If recurrent may be associated with blepharitis/staph/acne rosacea/SebCC
Treatment: Recommend warm compress BID with lid massage. Consider Bacitracin ointment BID for 2 weeks or Augmentin QID for 7-10 days. IF recurrent consider low dose doxycycline 20mg BID for long term.
DDx
Pyogenic granuloma
Benign, red, pedunculated conj lesion. Can have assoc hordeola, trauma, surgery. Excise or treat with combo drop like Maxitrol QID for 2 weeks
Preseptal: Eyelid and periorbital erythema, edema, and warmth
Sebaceous carcinoma
Older patient with recurrent chalazia, lid thickening, madarosis, chronic unilat bleph


Droopy Eyelid
Questions: Onset, duration, congenital? Past surgery/trauma, worsen throughout the day? Diplopia or headache, trouble breathing/swallowing, autoimmune dx?
A condition characterized by the drooping of one or both eyelids, which may be caused by various factors such as muscle weakness (MG or levator issue from muscular dystrophy), nerve damage (horner or CN3 palsy), mechanical problem (edema/tumor/chalazion) or congenital condition.
Most common cause is aponeurotic ptosis (levator weakening) that can be caused by aging, eye rubbing, removing GPs, orbital surgery
Examination includes assessing pupil reactions (Horner’s or CN 3 palsy), Hertel exophthalmometry, margin reflex distance, levator function , upper eyelid crease position of both eyes.
Horner: Apraclonidine (will dilate +), cocaine (won’t dilate +), hydroxyamphetamine (preganglionic), 1% phenylephrine (post).
CN3 Palsy - blown pupil vs pupil spared? blown pupil URGENT!
Muller muscle ptosis test: Phenyl 2.5% in the ptotic eye. If improved in 5 min, good surgery candidate
Myasthenia Gravis Test: Ice test for 2 minutes, acetylcholinesterase inhibitor edrophonium all improves ptosis
Kearns Sayre CPEO: genetic disorder the causes progressive weakness of eye muscles, hearing problems, pigmentary retinopathy and heart conduction abnormalities → heart block → life threatening! symptoms start showing age 20. Plan: order urgent ECG and cardio consult + refer to cardiology
Plan:
Traumatic: observation for 6 months before consideration of surgery. Usually improve or completely resolve
Horner: CTA/MRA of head and neck if suspect carotid dissection due to horner’s or PCA aneurysm due to CN 3 palsy. Chest CT for lung mass suspicion
Follow up:
CN 3 palsy: new-onset palsy can be related to tumors/aneurysms (pupil involving) (ORDER CTA/MRA to RO), trauma, viral infection, ischemic microvascular disease (refer to PCP to RO diabetes/hypertension by checking BP, fasting BSL, hemoglobin A1C). RO GCA if indicated by ordering ESR, CRP , CBC, and platelet blood.
Follow up 1-3 months (1 month if pupil involving)
Congenital: monitor for amblyopia, strab or abnormal head posture. Refer for surgery if indicated. RTC q6m
Myasthenia gravis: Referral to PCP
Referral to cardiology/neurology if Kearns Sayre CPEO (URGENTLY) to order urgent ECG and cardio consult. can treat double vision with prism
Surgical options: surgical Blepharoplasty, frontalis suspension, surgery to mueller or levator.
Acute: Monitor for infection and hemorrhage.
Subacute: Monitor for exposure keratopathy and asymmetry that may require postoperative readjustment. Mild lagophthalmos is common for 2 to 3 weeks after surgical repair and usually resolves.
Chronic: Monitor for ptosis recurrence and exposure keratopathy
Tear, irritate, red, mucous, or asymptomatic
Questions: Recent Surgery, trauma or burn? Hearing loss?
Ectropion a condition that an outward turning of the eyelid margin secondary to
Involutional ectropion - Most common. Laxity from age
Paralytic - CN7 palsy
Cicatricial: Burn, surgery, actinic damage, chronic inflam, skin disease
Mechanical: Herniated orbital fat or tumor
Congenital: Facial syndrome. Down syndrome
Signs: Lid margin turns out. SPK, injection, thickening and keratinization. Lid scarring.
Exam: Orbicularis function, lid laxity, punctum location. Look for lid tumor, scar, herniated orbital fat. Slit lamp for SPK, exposure Keratopathy
Plan:
Order MRI if CN 7 + 8 issue (hearing loss) → r/o acoustic neuroma
Treat dry eyes/ prophylaxis due to exposed cornea: Lubricant, warm compress, bacitracin or erythro QID, tape lids. RTC as needed.
If surgery indicate - refer to oculoplastics for lid surgery
Irritation, FBS, tear, red
Questions: comes and goes? constant? recent burn or trauma (cicatricial)? hard blinks (blepharospasm)? Infection (trachoma, simplex,zoster)
Entropion is a condition that results in an inward turning of the eyelid margin due to a variety of reasons:
Types: involutional, congenital, cicatricial (Conj scarring in ocular pemphigoid, lid scarring from SJS, burn, trauma, trachoma), spastic (Orbicularis contraction from trauma, ocular irritation, blepharospasm)
Signs: Inward turn of lid margin that pushes lashes into globe. SPK, injection, corneal epi defect, thin, or ulcer.
DDx:
Trichiasis: misdirected lashes that are hitting your eyeball. This could be due to infections, autoimmune problem (ocular cicatricial pemphigoid), inflammatory or stevens-johnson syndrome or vernal keratoconjunctivitis). It could be from trauma after surgery, chemical or thermal burns to face and lids
Plan: epilate or Radiofrequency, cryo, electrolysis, lid resection + antibiotic ung for SPK or bleph), epiblepharon (redundant lid tissue (seen in asian kids), chronic bleph (inflamed lid margin that can cause lashes to go inward).
Distichiasis - second row of lashes coming from MG opening (associated with trauma, chronic inflammation)
Trichotillomania – urge to pull lashes
Treatment: Aggressive lubrication and antibiotic ointment. Evert lid away from globe with tape Escalate: surgery
Follow up: None if cornea isn't involved. Sooner if cornea is involved
Chronically red, irritated eyes with mucous. Worse upon waking, both sides
Diagnosis: Floppy Eyelid syndrome (informed of possible systemic associations including sleep apnea, obesity, male, down syndrome, keratoconus)
Etiology/Patho: Abnormality of collagen/elastin fibers resulting in spontaneous eversion of the upper eyelid during sleep.
DDx.
VKC (Seasonal, itch, giant papillae)
SLK (Hyperemia, thickening, inflam of sup conj, limbus, and cornea. Assoc thyroid, dry eye, rheumatoid, friction)
Signs: Upper lids easily everted. Rubbery, atrophic sup tarsal plate. Injection, papillae, SPK, ptosis
Workup: Pull the lid away from eye and see if spontaneously everts or is lax. NaFl for sup conj papillae and SPK.
Treatment: Erythromycin ointment BID, artificial tears, tape lids or shield at night. Don't sleep facedown. If severe, recommend surgical tighting of lids. Refer for sleep study to confirm sleep apnea if indicated.
Follow up: Few days to weeks initially.
Uncontrolled/involuntary blinks
Both eyes or one? hard or soft blink? Face/neck spasm? just eye or whole face? , limbs involved? Disappears during sleep? (if doesn’t then hemifacial spasm)
Diagnosis: Blepharospasm is a condition that causes involuntary blinking. Associated with
Meige syndrome: oral facial dystonia involving blinking and chin thrusting, sometimes lip pursing or tongue movements, and occasionally shoulder movement.
Etiology/Patho: idiopathic, but assoc with dysfunction in dopaminergic pathway in basal ganglia (controls movement)
DDx:
Hemifacial spasm: Unilat contractures of whole half of face that don't disappear during sleep. Idiopathic or CN7 palsy so do MRI of pons to RO. Tx options: Observe, botox, or surgical decompression.
Myokymia: Subtle lid twich from stress, caffeine, alcohol, ocular irritation. Unilat lower lid. Self limited.
Apraxia Lid in Parkinson’s. Not orbicularis spasm, just can't open lids voluntarily
Workup: Slit lamp for dry eye, foreign body, neuro exam
Treatment: tx underlying dx, botox, surgery on orbicularis. No follow up generally
Discharge, red, tender at upper or lower puncta (no tenderness NLDO), gritty sensation, Pain (more swelling/pain/tenderness → dacryocystitis)
Diagnosis: canaliculitis
Etiology/patho: infection/inflammation of the inner corner of your eyes. Associated with bacterial or fungal infection.
Signs: Red pouting punctum, red skin surrounding. Expression of mucopurulent discharge or concretions.
Workup: Push on puncta with cotton swab to look for discharge or concretions. Smears and culture: gram, giemsa, saabouraud
Treatment: Remove concretions/retained plugs. Irrigate with antibiotic solution. Polytrim or moxi QID and oral doxy 100mg bid for 1-2 week. Warm compress QID
Treatment if fungal: Nystatin and irrigate
Follow up: 5-7 days. Not urgent
DDx
Dacryocystitis: Infection of lacrimal sac with more swelling, pain, tenderness than canalic
NLDO: Tearing, no erythema or tenderness at punctum
Pain, red, swellling on the inner lower lid (over the lacrimal sac). Tear, discharge, fever, chills. ask ear, nose, throat, sinus infection. Past trauma?
Diagnosis: Dacryocystitis
Patho/etio: Inflammation of the lacrimal sac which primarily caused by NLDO, or gram positive bacteria. Rarely caused by trauma or lac sac tumor
Signs: Red, tender, swelling. Expresses mucous discharge when pushed
Risk of progression: Lacrimal sac abscess, orbital or facial cellulitis
Work Up: Push with cotton swab to get discharge. Gram stain, blood culture agar for haemophilus from punctum discharge. Consider pupils, motilities, proptosis and CT if concerned about orbit
Treatment: Oral antibiotic: augmentin 875/125mg BID. If MRSA, TMP 160/SMX 800 Q12H for 10-14 days. Warm compress, digital massage. Acetaminophen.
Escalation: Incision and drainage. After resolution, probe and irrigate. Consider surgery if blocked.
Follow up: daily until improving. IF worsens then hospitalize for IV antibiotics
Ddx
Preseptal cellulitis - Facial cellulitis in canthal region, No discharge, lacrimal system is not obstructed
Dacryocele
Enlarged but not inflamed lacrimal sac in an infant. NLDO or trapped mucous/amniotic fluid in lac sac. Unilat. Do digital massage, warm compress
Acute ethmoid sinusitis
Pain, tender, nasal obstruction, erythema over nasal bone. Diagnose with imaging. Patient is febrile/has fever. Recommend antibiotics (if suspect bacterial), nasal steroids to reduce inflammation.acetaminophen prn, warm compress to ease sinus pressure,
Eye lid swelling
Questions: Pain on eye movement, diplopia, past etiology, sinus congestion, recent vaccine, past resistance to antibiotics?, fever?
Tests: Motilities, proptosis, APD, color, disc edema, CN5: facial sensation in V1 and V2 distribution. Palpate lymph nodes. Check vitals.
Workup:
CT of orbit and sinus. Consider MRI of cavernous sinus.
Gram stain if open wound is present.
CBC and blood culture if fever.
DDx
Preseptal cellulitis is an infection of the soft tissues ANTERIOR to orbital septum (membrane that separates lid from eye socket) likely from bacterial infection. Upper resp infection, trauma, Abrasion, injury, hordeolum, insect bite, dacryocystitis can lead to condition.
Obj: Lid edema, erythema, warm, tender. May not be able to open eye. Possible blur and monocular diplopia from swollen lids
Treatment: 10-14 days of: Amoxicillin/clavulanate 875/125 mg BID. If MRSA suspect: doxycycline 100mg bid. (kids: clindamycin)
Follow up: daily until improvement then every 2-7 days. Admit to hospital for CT scan/IV antibiotics if not better
Orbital Cellulitis: infection of eye ( likely from recent sinus infection) that can spread to the brain, needs PROMPT treatment.
Signs: Proptosis, optic neuropathy, muscle restriction, conj injection, or pain on eye movement.
Admit to hospital for IV antibiotics (ampicillin–sulbactam 3 g i.v. q6h for adults).
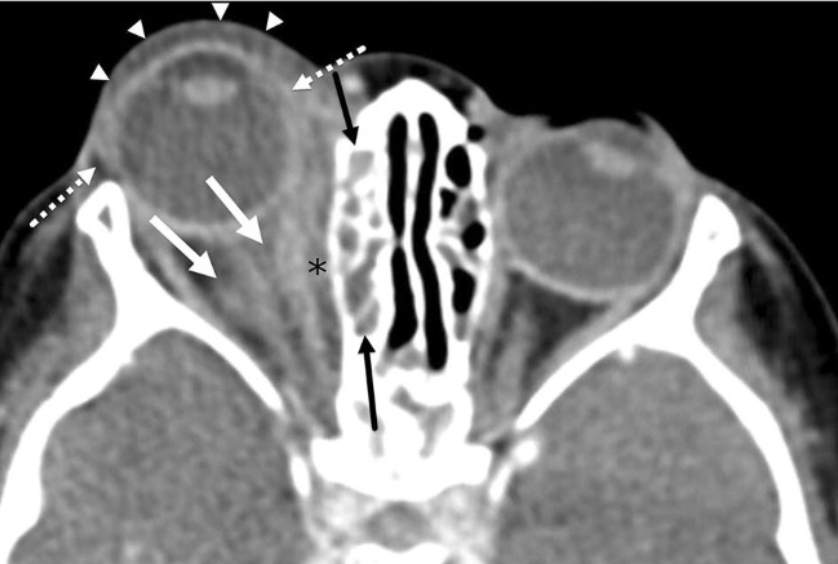
Cavernous sinus thrombosis is caused by blood clot occuring in the ICA at CS. Most commonly caused by infection/facial trauma.
Proptosis with multiple cranial neuropathies (CN 3, 4, 6, V1,V2)
Workup: CN testing, order MRI or CT scan to confirm
Treatment: admit to hospital for IV antibiotics + heparin
Follow up
Viral conjunctivitis: lid swelling + follicles in palpebral conj.
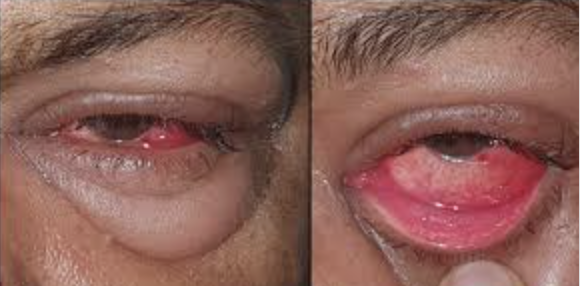
Rash/vesicles on skin
Questions: fever and chills? (Erysipelas), previous history of chicken pox (zoster)
Herpes Zoster: Vesicular rash on the dermatome, respects midline
Herpes Simplex: Vesicular rash not on the dermatome. Assoc follicular conjitis
Erysipelas: Rapidly advancing strep cellulitis with fever and chills. Can affect skin elsewhere. Augmentin 875 mg bid (ceftriaxone if allergic to penicillin)
Lesion/growth/cyst on eyelid
Questions: Onset? growth, how fast? Color? texture? bleeding? Double vision? Lid distorted?
Workup: Speed of onset, past history. External exam. Slit lamp for ulveration, abnormal color, texture (thickend), bleeding. telangiectasia, madarosis, meibomian destruction. Evert lids. Photo, draw, measure. Biopsy.
- Benign lid lesions present for at least 6 months with no disruptions of lashes or skin, no changes in color, bleeding or ulceration, if recurrence after removal then may be malignant. If enlarging and pigmented then suspicious.
Follow up for lid tumor removal: 1-4 weeks for healing then 6-12 months.
Seborrheic keratosis: Old pt. Brown, circumscribed, crusty lesion. Elevated. Shave biopsy
Cyst of Zeiss: Clear or yellow oil gland, which has become blocked but continues to produce fluid or oil. Circumscribed, white-yellow-clear lesion on lid margin or under skin. Will transilluminate. Can excise.
Cyst of moll: clear fluid
Sebaceous cyst: Can occur anywhere, filled with oil. Excise
Molluscum contagiosum: viral infection usually in kids. Associated with follicles and HIV if more widespread, larger, persistent and severe.
Plan: Self resolve 6-9 months if healthy. Treat if chronic, genital area, suspect HIV/weakened immune response, bothersome. Treatment includes: referral to dermatology for cantharidin tx - cream applied to each bump. (blisters within 24-48 hours and heals within 2 weeks). May need 2 in office treatments.
Refer to PCP for Antiretroviral therapy - HIV/weakened immune response.
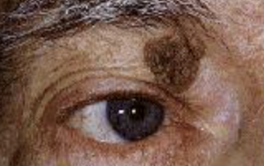
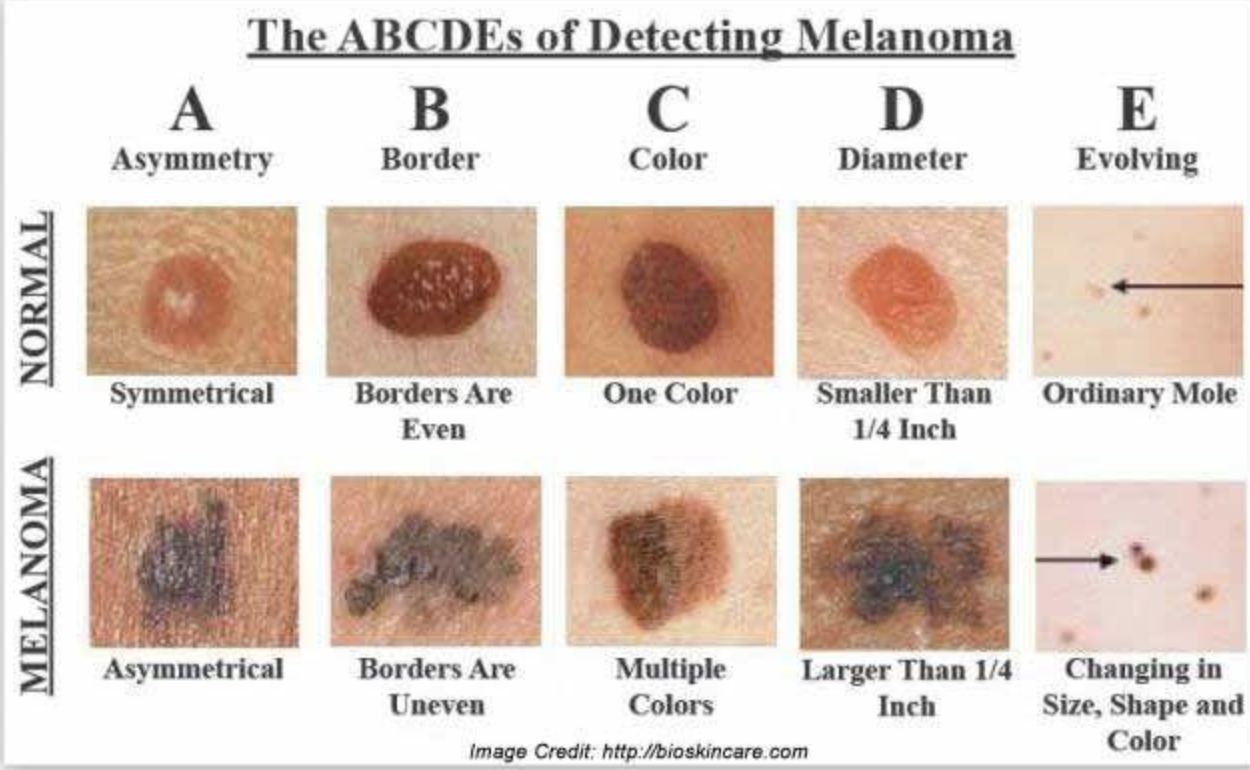
Nevus: Brown, melanocytic neoplasm on dermis or dermis-epidermis junction. Congenital or appear in puberty. Can morph into melanoma. Biopsy if suspicious.
Xanthelasma: Bilat soft yellow plaque of lipids/macrophages in medial upper and lower lids. If <40 YO, run cholesterol and lipid panels. Can excise surgically
Viral Wart (verruca): non pigmented papules, finger like. Caused by HPV: Plan: Referral to dermatologist for cryotherapy to prevent viral spread.
Papilloma: most common benign lesion of lid from overgrowth of skin. Skin colored lesion. Smooth, round, or pedunculated. Can grow and multiply. Spon regression or excise and biopsy. Risk of squamous carcinoma (5-16%).
Actinic Keratosis: precancerous skin lesion caused by prolonged exposure to ultraviolet (UV) radiation from the sun or artificial sources, such as tanning beds. Round, red, premalignant lesion with scaly surface on sun exposed area. Excise and biopsy. Risk of squamous carcinoma (10%)
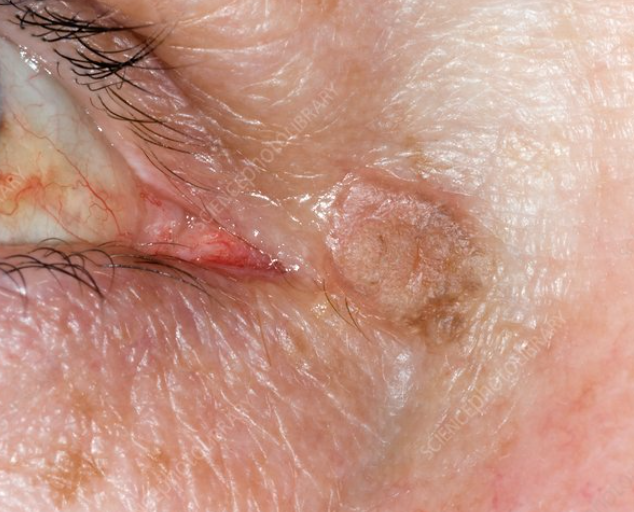
Keratoacanthoma: Elevated lesion with rolled margin and central ulcer with keratin. Slow spon resolution but can destroy tissue. Low grade squamous cell carcinoma. Excise.
CANCER LESIONS
Basal Cell Carcinoma (80-90%): Most common malig lid tumor. Lower or medial canthus. Rare metastasize. Nodular or infiltrative. Ulcerated with telangiectasia. Plan: Excise with Mohs. Use sun protection.
Squamous cell carcinoma (5%): Regional metastasis. Preceded by actinic keratosis. Scaly, red, flat lesion. Excise, refer to oncologist and systemic workup
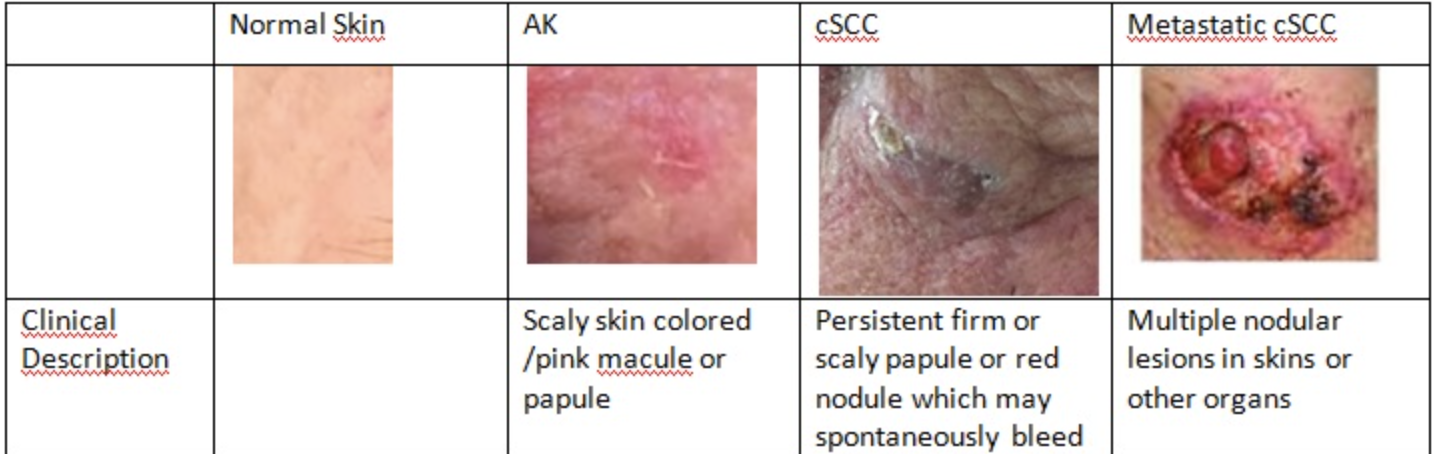
Sebaceous carcinomas (1-5%): Most common in elderly women. Upper lid. Looks like recurrent chalazia. Madarosis, meibomian destruction. Excise, refer to oncology for systemic workup.
Malignant melanoma: Wide surgical excision. Lymph node biopsy.
Kaposi Sarcoma: caused by infection with a virus from human herpesvirus 8. If have weakened immune system (HIV), then increased chance for injection to lead to kaposi sarcoma. It is a cancer that develops from cells that line BV and lymph nodes. Refer for excision.

Red lesion
Any associated symptoms? pain? Onset? growth?
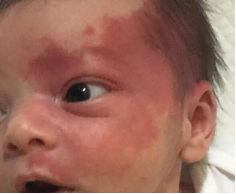
Capillary hemangioma: Most common vascular lesion in childhood (5-10% of infants) - 75% regress to some extent by 7 years.
Small, red or purple dots on the skin. Risk factors: low birth weight, female. blanches with pressure -> confirmation
Plan: monitor, may grow deeply and bleed a lot. Most self-resolve by age 10. Some stay small and persist. If causes ptosis, RE and amblyopia then refer to pediatric ophthalmologist to asses for risk factors and provide treatment like steroids, excision, beta blockers
consider topical timolol 0.25% or 0.50% Gel Forming Solution (GFS) BID for 3-4 months for superficial hemangiomas
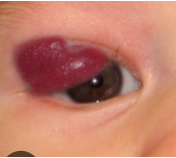
Port wine stain: birthmark, present at birth, dark red to blue color, may gradually become raised and thicker as child grows. 18% associated with glaucoma. If also sturge weber syndrome then 40-60% chance of glaucoma. Plan: referral to pediatric ophthalmologist for laser treatment. Monitor pressures yearly due to increased risk of glaucoma.
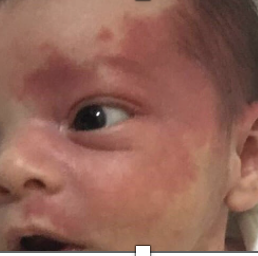
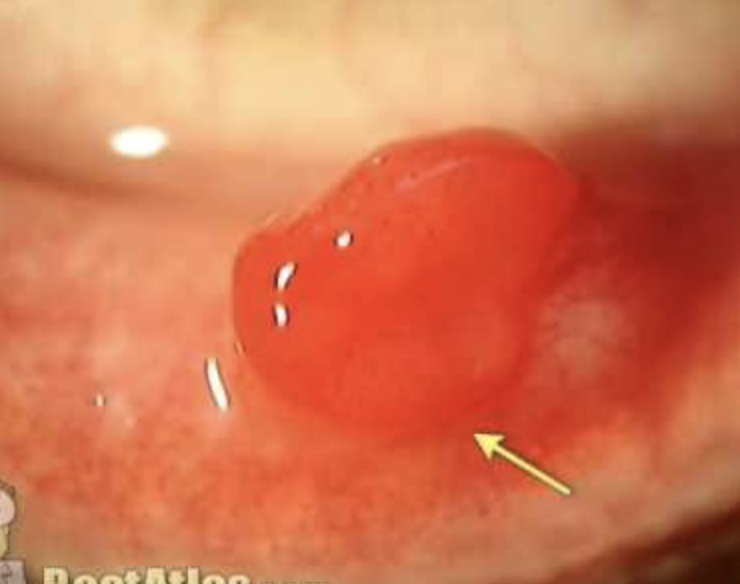
Pyogenic granomla: common, Benign, deep-red, pedunculated conjunctival lesion often associated with chalazia, hordeola, trauma, or surgery.
Plan: topical antibiotic–steroid combination such as neomycin/polymyxin B/dexamethasone q.i.d. 10 days. Monitor IOP due to steroid. RTC 10 days follow up.
Kaposi Sarcoma: caused by infection with a virus from human herpesvirus 8. If have weakened immune system (HIV), then increased chance for injection to lead to kaposi sarcoma. It is a cancer that develops from cells that line BV and lymph nodes. Refer for excision.
Inflamed Lid Differentials
Inflamed orbit:
1. TED – auatoimmune response against CT and aadipise tissue within the orbit. TENDONS SPARED. Commonly in middle aged female, bilateral/uni Proptosis, Von Graefe, Kocher, Dalrymple signs, tendons spared, IMSLO EOM involvement. Plan: manage symtpoms (dry eye, double vision), referral to PCP for blood work (TSH, T3,T4) and management.
Follow up 1 year or sooner if symptoms
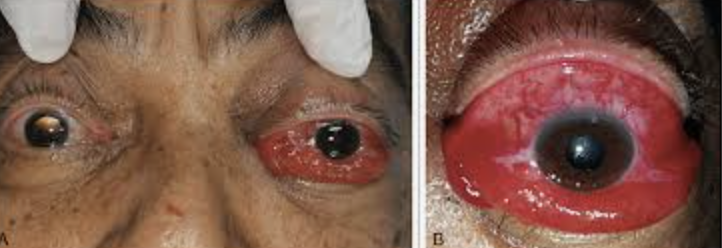
2. Carotid Cavernous fistula – abnormal communication between arterial and venous blood supply in cavernous sinus → back flow of fluid → painful red eye, chemosis, pulsatile proptosis and ocular bruit, mostly nontraumatic cause/spontaneous. Plan: urgent referral to neurosurgeon for Endovascular Embolization. Follow up as indicated by surgeon.
3. Orbital pseudotumor disease – EVERYTHING inflamed, tendons NOT spared. young/middle aged, rare, unilateral pain, proptosis and chemosis. Plan: Prednisone (1 mg/kg) 60 to 100 mg daily for 1 to 2 weeks with a 5- to 6-week taper. Order MRI/CT scan to RO conditions. Follow up every 1-2 weeks until resolved
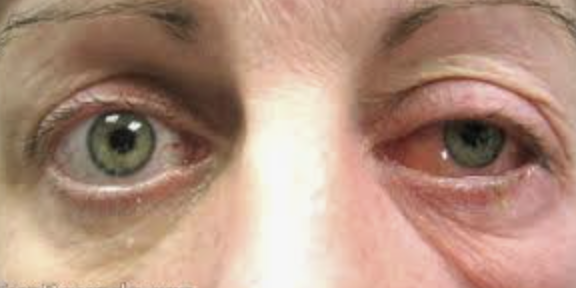
4. Tolosa Hunt Syndrome – inflammation of SOF and CS → acute painful exopthalmoplegeia and diplopia + loss of sensation for V1 and V2. Plan: Prednisone (1 mg/kg) 60 to 100 mg daily for 1 to 2 weeks with a 5- to 6-week taper. Order MRI/CT scan to RO conditions. Follow up every 1-2 weeks until resolved
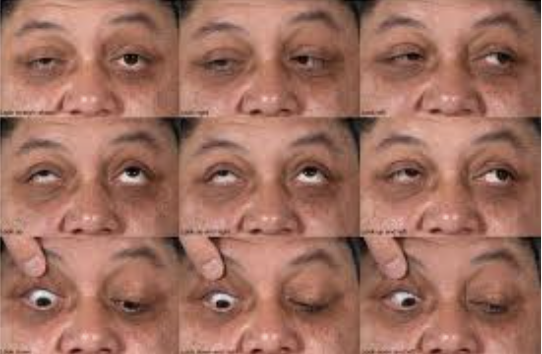
5. Contact dermatitis – delayed allergic response bilateral swelling, itchiness. Oral anithistamines and corticosteroid cream.
6. Orbital Tumor – unilateral, painless progressive vision loss, proptosis, diplopia and APD. Plan: Urgent referral to opthamologist for removal.
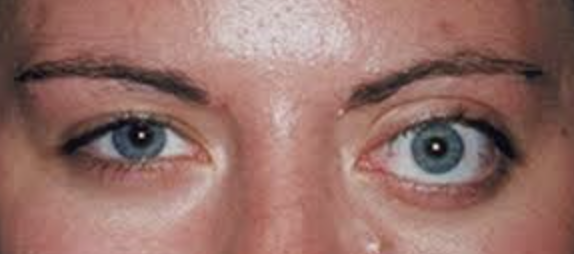
a. Lymphangioma: younger pts, acute proptosis, ecchymosis, external ophthalmoplegia. Plan: Urgent referral to neuropthomologist for removal.
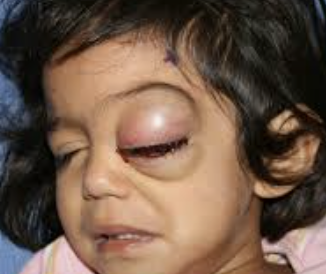
7. Orbital cellulitis – recent infection, EOM pain/restriction, exophthalmos (main reason for children), fever, proptosis, chemosis, dec VA, diplopia
8. Preseptal Cellulitis – mild/no pain, hard to the touch, ptosis, infection ant septum
9. Orbital hemorrhage – recent hx of trauma or surgery, dec vision, bleeding disorder
10. Severe orbital emphysema (“tension pneumo-orbit”): Tight orbit, tight eyelids, crepitus, and decreased extraocular motility; may follow orbital fracture with or without nose blowing.
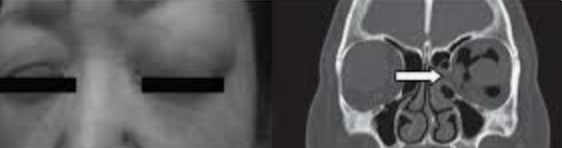
11. Orbital fracture: Limited extraocular motility, enophthalmos, or proptosis may be present.
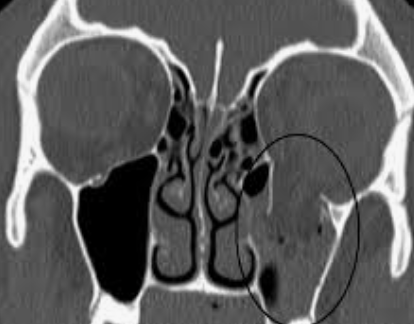
12. Ruptured globe: Subconjunctival edema and hemorrhage may mask a ruptured globe. MEDICAL EMERGENCE Plan: Urgent referral to opthamologist for repair.
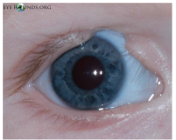

-Birth defects?Corneal problems? FHx of colobomas? |
Eyelid Coloboma: Eyelid defect due to failure of eyelid to form during development. We want to protect your cornea by using lubricants, taping and patching at night etc. We can surgically reconstruct your eyelid as well.
Objective findings: trichiasis, dermoid tumors, conj injection, symblepharon, malformation of caruncle, exposure keratopathy, corneal scarring, iris coloboma, anterior cataract, subluxation
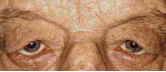

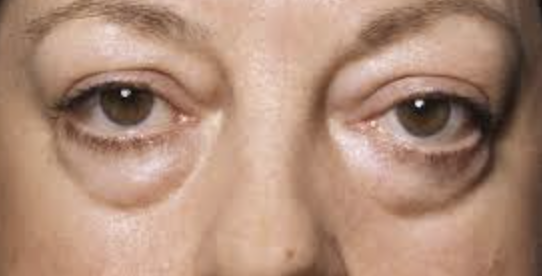
Dermatochalasis
You skin has loss of elastic tissue in skin from weakened orbital septum. This can be a result of age, trauma, edema, chronic dermatitis, floppy eyelid syndrome. We can recommend blepharoplasty surgery if it is impacting your visual field. Ancillary testing: VF
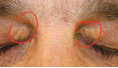

High cholesterol? Bothersome?
Xanthelasma: You have lipid deposits that have accumulated on your eye lid. This is common with people who have high cholesterol. Option for laser treatment but may recur.
Order labs to see cholesterol levels
Autoimmune/ skin conditions that can have lid manifestations
Ocular Rosacea: Sebaceous glands effected (Zeis and MG)-> chronic ocular surface disease - redness in face, with papules and pustule. Has telangiectasia on nose and cheeks and rhinophyma. Dietary and environmental triggers like spice, alcohol, chocolate, sun, wind, exercise, stress etc.
Ocular rosacea causes lid disease due to abnormal glands including MGD, blepharitis, hordeola, which results in surfaces disease like SPK, phlyctenules, corneal neo (greatest inferior), dry eye
Poliosis: You have lashes that are white. This is caused by an absence of melanin in the hair follicle. This can be from a number of different conditions including VKH is an autoimmune disease that attacks the melanin in your skin.
Plan: treat underlying disease and referral for melanoma or systemic condition
Vitiligo: The uneven pigment on your skin is a result of a skin condition called vitiligo that is caused by thyroid abnormality. It worsens over time, so our goal is to protect your skin from the sun. We can refer you to dermatologist to do melanocyte stimulation.
Plan: Refer to PCP for thyroid testing. Recommend to Protect skin from sun. Referral for dermatology consult for melanocyte stimulation and skin color blending with amino acids, topical steroids.
Irritation, itching, burning, foreign body sensation, crusts on lashes, stuck together lashes, red, irritated lashes, tender lids (may have recurrent hordeolum or chalazion), dry eye complaitns
Blepharitis: a condition that is caused by natural bacteria on the skin triggering an infection of the lashes and lid margins. We want to make sure the area is clean by using lid hygiene This is a chronic condition so it can come and go and we can use medication for acute flare ups.
Meds: (topical antibiotic/steroid combination like Tobradex Q2h (every 2 hours) or qid (4x) for 10 days. RTC 2 -4 weeks)
marginal infiltrate/phlyctenule present, staph bleph
Bacitracin or erythromycin ung qpm for angular bleph (dry and scaly at canthus)
lubricants - Use artificial tears qid (4x) or prn (as needed)
Esp for Meibomian Seborrheic Blepharitis (+)warm compress
Lid hygiene – lid scrub (can use baby shampoo or hypochlorous acid - spray, gel, or wipes that can be used daily
If Demodex: have an infestation of mites that are living in your eyelashes. They can carry bacteria on their surface which is triggering an immune reaction and giving you these symptoms. We want to kill the mites and the eggs with our treatment.
Plan: Xdemvy opth soln 1gtt OU BID 6 weeks + lid scrubs BID
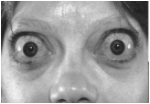

dry eyes, puffy lids, angry looking eyes, bulging eyes, diplopia, visual loss, VF loss, dyschromatopsia (distortion of colors that the patient sees), photopsia on upgaze, ocular pressure or pain
Thyroid Eye Disease: thyroid is being overactive resulting in the release of excess thyroid hormones. This is an autoimmune disease that goes against the connective tissue (fibroblast) and adipose tissue within the orbit resulting in eyeballs being pushed forward and problems with the optic nerve due to it getting compressed. These things are causing your visual symptoms. We will work with your PCP and endocrinologist to get your thyroid under control while helping treat the symptoms of your visual complaints.
Objective Findings: Proptosis (unilateral or bilateral - most common causes in middle aged pts, lid retraction, dec color vision, EOM restriction, APD, Inc IOP in primary and upgaze
Ancillary Testing: Forced ductions (EOM restriction), CT/MRI (enlargement of EOMs), exophthalmometry (proptosis measurement - 12-22 mm for Caucasians, 12-24 mm for AA, 12-18 mm for Asians, Abnormal if >3 mm), VF (optic nerve compression -> field loss), blood work – TSH/T3/T4, TSI, TSAb, TRAb
Plan:
Referral to endocrinologist to treat thyroid problem
refer to PCP for blood work, CT and MRI -> refer for surgery depending on EOM abnormalities
TED treatment using ocular lubricants, topical steroids and or antibiotics, and


tepezza (to block infla of tissue in orbit)
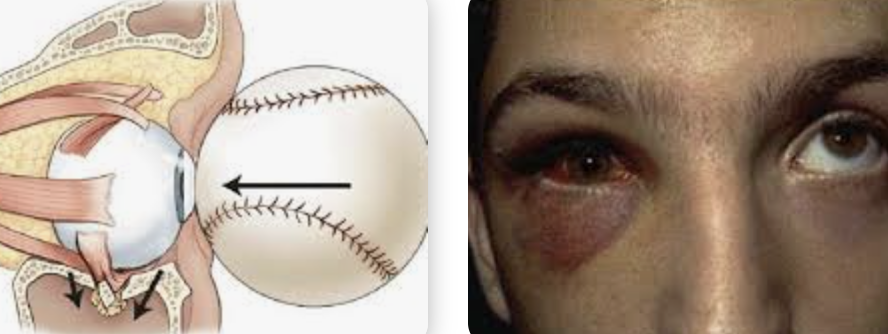
Recent trauma, Pain, double vision, crackling noise on palpation of medial orbital area or after nose blowing (patient hears it
Orbital blow out fracture: The bone below the eye is the thinnest and most susceptible for fracture. During the blunt trauma, it fractured that bone resulting in the muscle located there to get stuck. This makes it difficult for your eyes to do vertical movements resulting in your double vision especially when looking up. This should resolve over time when swelling decreases. If it doesn’t resolve, then can consider surgery.
Objective: enophthalmos, diplopia, globe ptosis, infraorbital hypoesthesia (bc infraorbital nerve damaged), asymmetric monocular PDs, hyphema, angle recession, Eyelid ecchymosis – black eye from leaking BV in subcutaneous tissue
RO muscle Entrapment. occurs when the fracture creates a "trapdoor" effect, where the bone fragments trap the surrounding tissues, including muscles and fat → atrophy of IR muscle so need to send to oculoplastics
symptoms: Nausea and vomiting, Bradycardia (slowed heart rate), Pain: Especially with attempted eye movement.
Ancillary testing: forced duction test, don’t do gonio until 4 weeks after trauma, Order CT scan of the orbit (coronal scan)
Plan:
Steroid to decrease swelling
while diplopia may be an initial concern immediately after the injury, it often resolves over time on its own without surgical intervention
Order CT scan of the orbit (coronal scan)
Ed pt that nose-blowing could lead to orbital or soft tissue emphysema and is discouraged for 4-6 weeks after the injury.
RTC 1 week for progress check