skin CS
1/74
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
75 Terms
What are the functions of healthy skin?
Barrier function
Homeostasis
Sensation
Excretion
Immunity
Vitamin D production
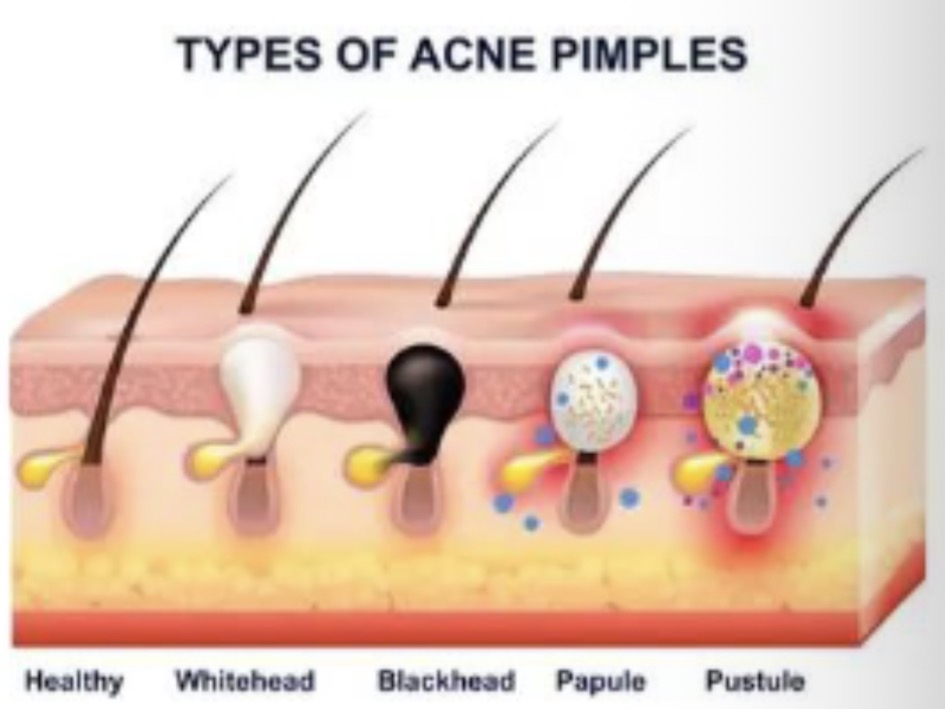
In acne vulgaris, what are the superficial lesions?
Open comedones (blackheads)
Closed comedones (whiteheads)
Papules (small, tender, red bumps)
Pustules (white/yellow spots)
: In acne vulgaris, what are the deeper lesions?
Nodules (large, red, painful lumps)
Pseudocysts (cyst-like swelling)
In acne vulgaris, what are the secondary lesions?
Excoriation (scratched spots)
Erythematous macules
Pigmented macules
Scars
In acne vulgaris, what defines mild acne?
Predominantly non-inflamed lesions (open/closed comedones) with few inflammatory lesions
In acne vulgaris, what defines moderate acne?
More widespread lesions with increased number of inflammatory papules and pustules
In acne vulgaris, what defines severe acne?
Widespread inflammatory papules, pustules, nodules or cysts. Scarring may be present.
In acne vulgaris, what lifestyle advice is recommended?
Avoid excessive cleaning and extreme water temperatures
Avoid squeezing spots (can cause scarring)
Avoid oil-based makeup, skincare, suncare
Remove makeup before bed
Use fragrance-free water-based emollient if dry skin problematic
Wash hair regularly and avoid letting it fall across face
In acne vulgaris, what is first-line cleansing treatment?
Non-alkaline synthetic detergent cleansing product twice daily.
In acne vulgaris, what OTC topical treatment is used?
Benzoyl peroxide gel/cream.
In acne vulgaris, what topical prescription options exist for mild–moderate acne?
12-week course of topical benzoyl peroxide + adapalene
Clindamycin
Topical tretinoin + clindamycin
In acne vulgaris, what are treatment options for moderate–severe acne?
Topical treatment
Systemic antibiotics (e.g., lymecycline)
Combined oral contraceptive
In acne vulgaris, what is used for severe or unresponsive acne?
Consultant dermatologist-led oral isotretinoin.
In acne vulgaris, what are the red flag symptoms?
Moderate/severe acne
Scarring/persistent pigment changes
Age <10 or >40
Symptoms of depression
Acne fulminans/conglobata
Unresponsive to treatment
Females with acne + menstrual irregularities
In allergic rash (urticaria), what are the key features?
Raised bumps/patches anywhere on body
Itchy/sting/burn
May appear pink/red on fair skin
What causes allergic rash (urticaria)?
Histamine release triggered by foods, pollen, animals, etc.
What is the first-line management of allergic rash (urticaria)?
Wash affected area with water.
What oral medication is used for allergic rash (urticaria)?
Non-sedating antihistamines (e.g., loratadine, cetirizine).
What topical treatment is used for allergic rash (urticaria)?
Hydrocortisone 1% cream.
What long-term advice is given for allergic rash (urticaria)?
Identify and avoid triggers.
What are the red flag signs for allergic rash (urticaria)?
No improvement after 2 days
Rash spreading
Recurrence (consider allergies)
High temperature or feeling unwell
Simultaneous swelling under skin
Signs of anaphylaxis
In atopic eczema, which areas are commonly affected?
.
Flexures
Who is commonly affected by atopic eczema?
People of all ages, common in children.
What are the symptoms of atopic eczema?
.
Itchy, dry/cracked/scaly skin, discolouration, blistering/bleeding (if severe)
What causes atopic eczema?
Multifactorial — genetic predisposition, family history of eczema, asthma, hayfever.
What worsens atopic eczema?
Allergens, irritants, heat, infection, stress, hormonal changes.
What is the treatment for mild atopic eczema?
Frequent, liberal emollients (cetraben, dermol, aproderm)
Mild topical corticosteroid (1% hydrocortisone)
Emollients as soap substitute
Creams for inflamed skin, ointments for dry skin
What is the treatment for moderate atopic eczema?
Continue emollients
Moderately potent steroid (betamethasone valerate 0.025% or clobetasone butyrate 0.05%)
What is the treatment for severe atopic eczema?
Continue emollients
Potent steroid (betamethasone valerate 0.1%)
May require antihistamine for itchiness
What advice is given for atopic eczema?
Avoid irritants
Apply emollient frequently, even if improved
Wash with emollient instead of soap
Keep cool, loose clothing
Keep nails short/use mittens
Avoid aqueous cream
What are the red flag signs of atopic eczema?
No improvement
Blistered/crusty/leaking fluid/pus
Painful, swollen, warm skin
Sudden worsening/spreading
Accompanied by high temperature
What is contact dermatitis?
A type of eczema caused by irritants or allergens.
What is irritant contact dermatitis?
Skin damage after exposure to substances (soaps, perfumes, powders, cement, plants).
What is allergic contact dermatitis?
Immune reaction to triggers like cosmetics, metals, rubber, textiles
How is contact dermatitis managed?
Clean skin with warm water
Use gloves
Avoid irritating products
Apply emollients generously
Identify and avoid cause
Topical/oral steroids if necessary
What are the red flags in contact dermatitis?
Signs of infection
Chronic, severe, or recurrent dermatitis
Worsening of stable dermatitis
Associated with recent medications
What is the treatment for blisters?
Clean and pat dry
Cover with soft/padded plaster
If burst, allow fluid to drain before covering
What preventative measures are recommended for blisters?
Wear well-fitting shoes
Thick socks/protective gloves during exercise
Change socks frequently if sweaty
What are red flag signs for blisters?
Recurring
Infection signs
Surrounding redness
Unusual location
Multiple blisters without cause
Burns/scalds/sunburn/allergic reaction
What is a burn?
Dry heat injury.
What is a scald?
Wet heat injury (e.g., steam).
What are symptoms of burns/scalds?
Red/peeling skin, blisters, swelling, white/charred skin.
What immediate actions are recommended for burns/scalds?
Remove from heat
Remove clothing/jewellery if not stuck
Cool under water 20–30 mins
Keep patient warm
Cover with clingfilm
Raise affected area
Pain relief (paracetamol/ibuprofen)
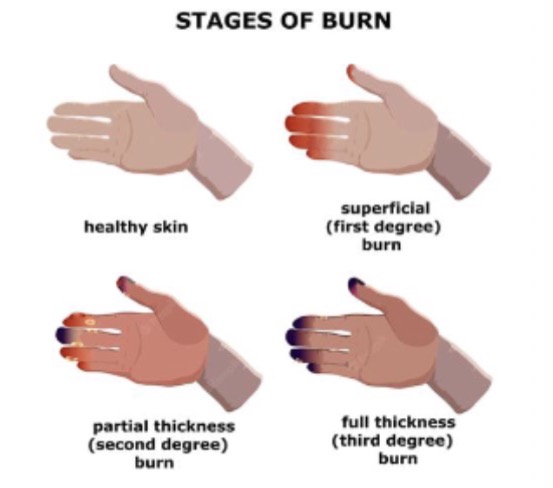
What are the types of burns/scalds?
1st degree: superficial epidermal, red/swollen/painful
Superficial dermal: epidermis + part dermis, pale pink, painful, small blisters
2nd degree/partial thickness: epidermis + dermis, red/blotchy, moist/dry, swollen, blistered
4th degree/full thickness: all layers destroyed, white/black, leathery/waxy, may be painless
What are red flag signs for burns/scalds?
Chemical or electrical burns
Children
Large/deep burns
White/charred skin
Face/neck/hands/feet/joints/genitals
What is sunburn?
Red, painful, peeling skin caused by UV exposure; usually self-resolves in 7 days.
What advice is given for sunburn?
Stay out of sun, cover burnt areas
Cool compress or water
Use aftersun
Drink fluids
Pain relief (paracetamol/ibuprofen)
Don’t use petroleum jelly or ice
Don’t burst blisters
Don’t scratch peeling skin
What are red flag signs for sunburn?
Blistered/swollen
High temp, shivering
Dizzy, sick
Headache/muscle cramps
Young children/babies affected
What is heat rash (prickly heat)?
Small, raised, itchy spots from blocked sweat glands.
What advice is given for heat rash?
Loose cotton clothing
Cool showers
Drink fluids
Cold compress 20 mins
Avoid scratching
Avoid perfumed products
What OTC options exist for heat rash?
Calamine, antihistamine, hydrocortisone cream.
What are red flag signs for heat rash?
Not resolving; unclear cause in babies.
What are moles and how do they behave?
Normal throughout life; can appear or disappear at any stage. Some may indicate melanoma.
How should moles be monitored/prevented?
Avoid strong sun 11am–3pm
Cover up
Sunscreen SPF 30+
Avoid sun beds
What are red flag signs for moles?
Changes in shape, size, or color
Painful or itchy
Inflamed, bleeding, or crusty
New/unusual marks not healing after weeks, >5mm, irregular border
Unusual lesions in patients >70yrs
What is ringworm?
Fungal infection causing red/darker, scaly, itchy patches; can occur anywhere.
How is ringworm treated topically?
Topical imidazoles (clotrimazole 1%, miconazole 2%, econazole 1%) for 12 weeks.
What advice is given for ringworm?
Wash towels/bed sheets regularly
Avoid scratching (prevent spread)
Wash hands and pets if suspected
Take precautions with contaminated objects/soil
When is oral treatment for ringworm needed?
Severe cases, scalp involvement: oral antifungals may be required.
What are red flag signs for ringworm?
Unresponsive to treatment
Large/scalp areas
Immunocompromised
Reinfection from contacts
What are warts/verrucae?
Viral skin growths, often self-limiting.
What is first-line treatment for warts/verrucae (non-facial)?
Topical salicylic acid daily for 12 weeks
Cryotherapy (liquid nitrogen) every 2–4 weeks, up to 6 sessions
Combination therapy: salicylic acid + cryotherapy
How should salicylic acid be applied for warts/verrucae?
Soak skin in warm water
File thickened skin (avoid healthy skin)
Apply daily up to 3 months
Avoid face
Keep away from fire
What are red flag signs for warts/verrucae?
Unresponsive to treatment
Extensive areas
Painful warts
Warts that bleed, itch, or change
Patients >50yrs with first-time wart
Immunocompromised
What are key features of insect bites/stings?
Painful lump; sometimes left stinger/hair embedded.
How should insect bites/stings be managed?
Wash with soap and water
Remove foreign object
Ice pack to reduce swelling
Avoid scratching
Topical/oral antihistamine
Hydrocortisone 1% cream
What are red flag signs for insect bites/stings?
Signs of infection (pus, hot to touch)
Painful
Considerable swelling/itching
Children <1yr
Tick bite symptoms (flu-like, circular rash)
Signs of anaphylaxis
What are key features of scabies?
Intense itching (worse at night)
Rash/spots across body
Burrows on fingers, wrists, hands
How is scabies treated?
Wash clothing/bedding at 60°C
Put non-washable items in sealed bag 3 days
Permethrin 5% w/v cream (children >2 months)
Single oral ivermectin 200 µg/kg for severe cases
Malathion also licensed
What precautions are required for scabies?
Avoid close contact with others for 24h after treatment; children <5yrs avoid nursery/school 24h after first treatment
What are red flag signs for scabies?
Infection
Severe/extensive rash
Institutional outbreaks
Symmetrical pattern; may indicate differential diagnosis
How should wounds be initially managed?
Administer first aid, remove debris, raise affected limb above heart if heavy bleeding.
How should wounds be cleaned?
Use bottled/tap water or sterile wipes; surrounding skin with soap/antiseptic.
How are wounds dressed?
Apply plaster or dressing as needed.
What are red flag signs for wounds?
Signs of infection
Animal/human bites
Large wounds >5cm
Persistent bleeding
Blood spurting, bright red
Loss of sensation or movement
Foreign body present