W22 Inflammation
1/34
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
35 Terms
What is the effect of inflammation?
Mechanism of disease- can trigger/cause tissue damage/cellular death and can either occur systemically or on a localised level
What is inflammation?
A localised response to cellular injury with an overall aim of removing the harmful stimuli and initiating healing
What is the function of inflammation?
Removes dead tissue and cells
Protects against local and spread of infection
Sets up pathway to wound healing requiring white blood cells and cell mediators
What is acute inflammation?
Fast and relatively non-specific (minutes- days)
What is chronic inflammation?
Simultaneous destruction and healing of tissues resulting in prolonged tissue stress or malfunction (weeks-months-years)
What are the 5 cardinal signs of inflammation?
Pain
Heat
Redness
Swelling
Loss of function
What occurs in a normal capillary?
Blood flow is smooth, surrounding tissue is interstitial tissue and occasional lymphocyte/macrophage and blood stays in vessels
What happens to capillaries when inflammation occurs?
Increased blood flow, prompting vasodilation and localised heat- thus causing redness. Leakage of plasma proteins causes edema and hence the cardinal signs of swelling. Neutrophil emigration to site of swelling, hence the pain
What are causes of inflammation?
Trauma
Chemical injury
Radiation
Burns/frostbite
Reduction in blood flow
Infection
Overactive immune system
What is meningitis?
Inflammation of the surface membranes surrounding the brain and spinal cord- this swelling can lead to bursting of blood vessels and can be fatal
What is vasculitis?
Inflammation of a blood vessel- an artery blockage may result in inflammation but it can also be caused by infection, autoimmune disease or cancer
What are examples of superficial inflammation of the cornea?
Punctuate epithelial erosion (PEE)
Punctuate epithelial keratitis (PEK)
Sub epithelial infiltrates
Superficial punctuate keratitis (SPK)
What is harmful inflammation of the cornea?
Deep infiltrates which go through the epithelial and attacking stroma and descement membrane, causing ulceration, melting and vascularisation (vessels growing where they shouldn’t be)
What are corneal infiltrates?
Build up of white blood cells
What’s the pathogenesis of inflammation?
Injury (can be anything)
Cell gives off chemical mediators
This causes increased blood flow (hence redness, heat) and vasodilation (pain, swelling)
What is chemotaxis?
Movement of chemicals generated by chemical mediators
What changes do chemical mediators bring?
Vasodilation and increased vessel permeability
Where can cell mediators derive from in acute inflammation?
Cells or blood plasma
How do mediators come from cells?
They can either be secreted or synthesised: histamine from mast cells are a powerful vasodilator and increase vessel permeability
Where do mediators come from in the blood plasma?
Inactive precursors already in circulation- examples include complement proteins and kinins
What is the benefit of increasing blood flow?
Brings more nutrients and oxygen to the area, increases metabolic rate of tissue cells, leading to healing
What’s the benefit of leaky capillaries and edema (fluid in tissue places?)
As clotting proteins enter the area, this causes fibrin barrier, causing healing
How does white blood cell emigration stimulate healing?
Removal of damaged/dead tissue cells and pathogens from area
How do we get leakage from blood vessels?
Gap junctions between endothelial cells increase
How do we study inflammation to test for leaky vessels?
Inject blue dye into blood vessels, dye leaks out of tissues if there’s been trauma
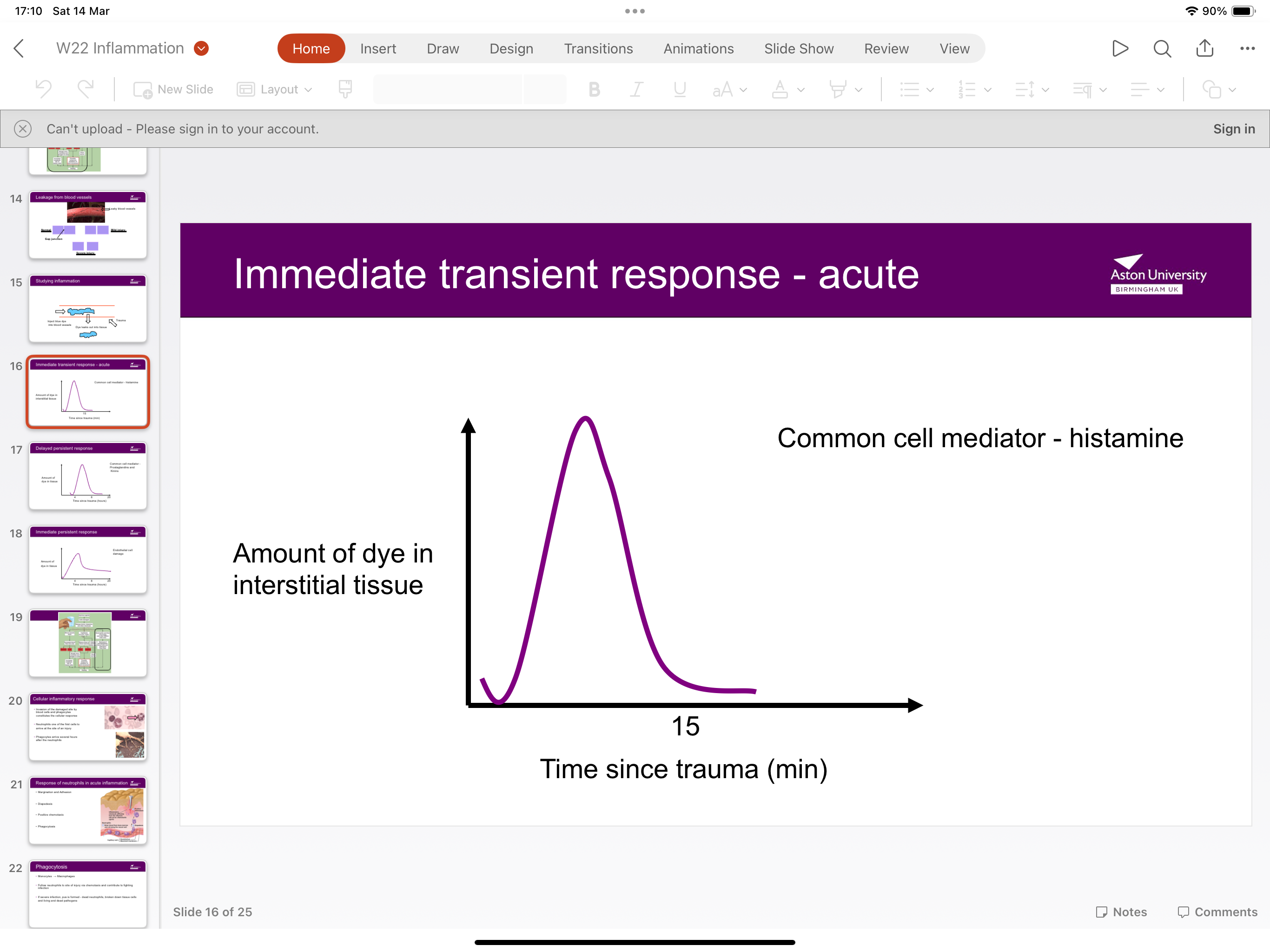
What’s the immediate transient response?
Histamine is commonly cell mediator- amount of dye in interstitial tissue peaks and then falls at 15 mins
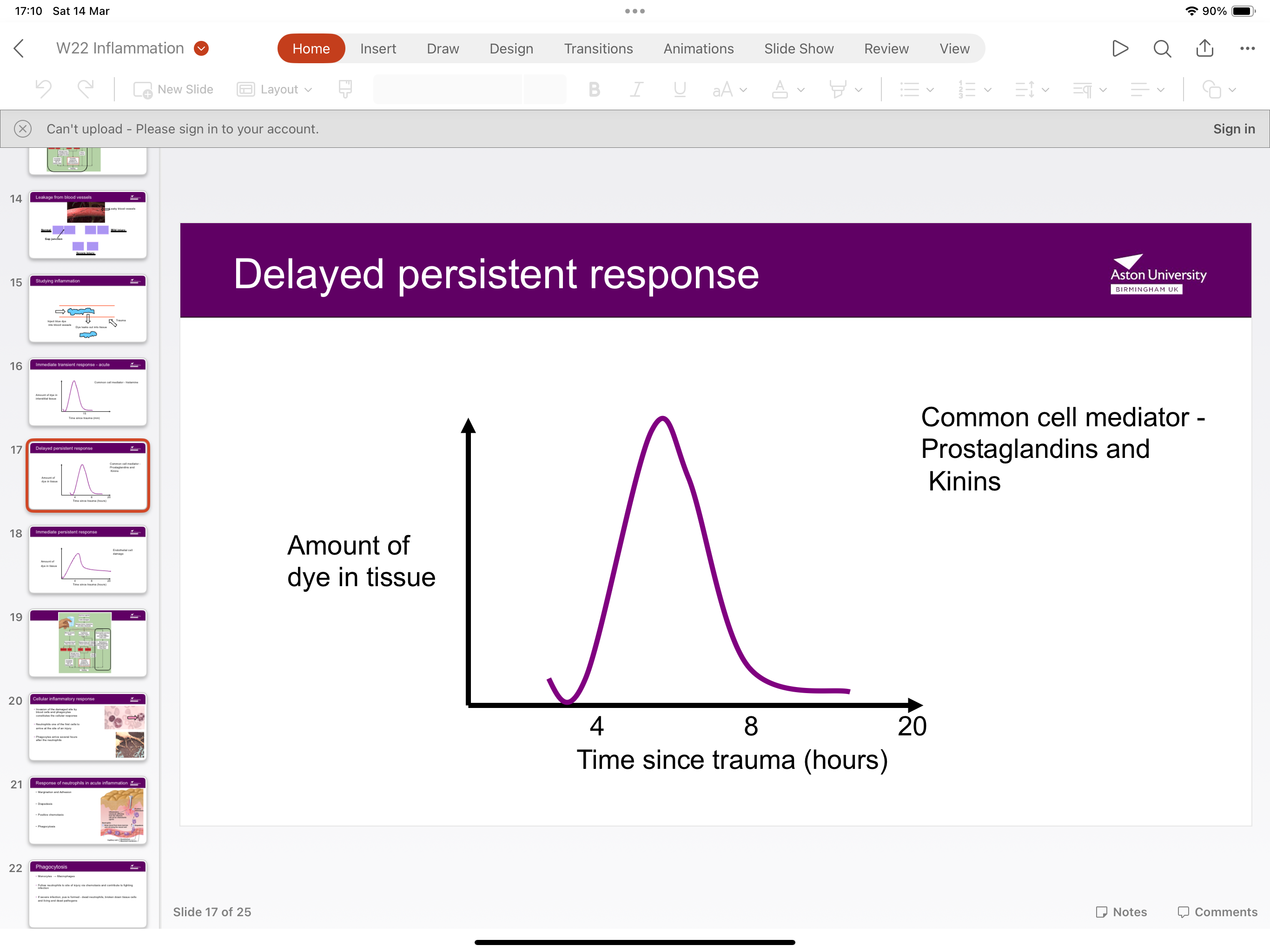
What’s the delayed persistent response?
Cell mediators prostaglandins and kinins- delay time since trauma
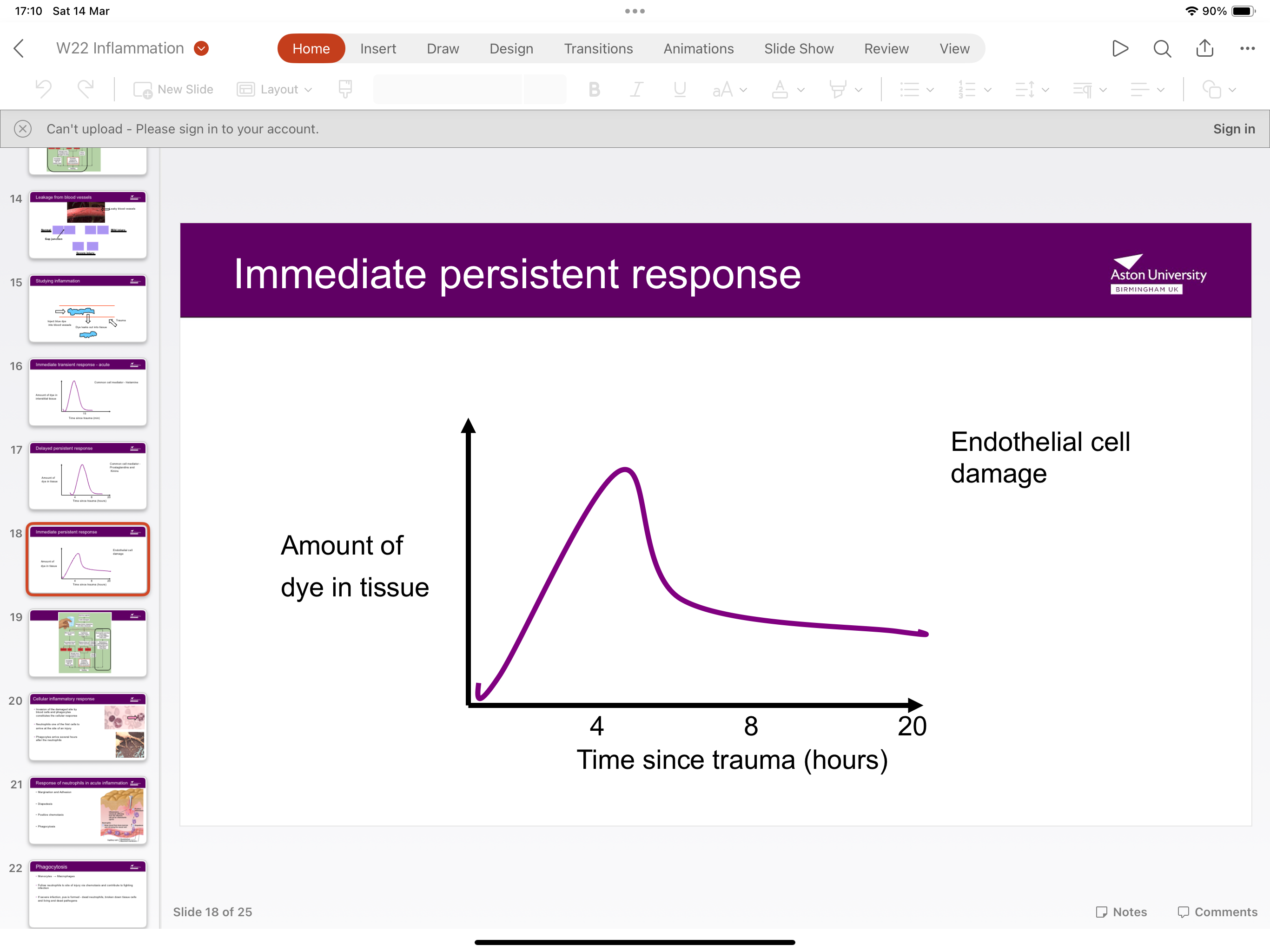
What’s the immediate persistent response?
Amount of dye in tissue will remain/ not go down eventually from endothelial cell damage
What is the cellular inflammatory response?
Invasion of phagocytes and blood cells- neutrophils are one of the the first cells to arrive at the site of injury, phagocytes arrive several hours after the neutrophils
What’s the first step in the response of neutrophils for acute inflammation?
Marination and adhesion- neutrophils enter blood from bone marrow and roll along vessel wall and sticks to endothelial wall of blood vessel
What happens after margination and adhesion?
Diapadesis- neutrophils leave blood vessels to enter tissue
What happens after diapedesis?
Positive chemotaxis- neutrophil moves to site of inflammation as inflammatory chemicals diffused from inflamed site acting as chemotactic agents
What happens after positive chemotaxis?
Phagocytosis- phagocytes take up any dead cells
How does phagocytosis occur?
Monocytes mature into macrophages as they follow neutrophils to site of injury via positive chemotaxis
What happens to a severe infection?
Pus is formed- these are dead neutrophils, broken down tissue cells as well as any living/dead pathogens