Digestive System: Anatomy, Processes, and Regulation
1/74
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
75 Terms
What are the two main groups of organs in the digestive system?
Alimentary canal (GI tract) and accessory digestive organs.
What is the function of the alimentary canal?
It digests food and absorbs fragments.
List the organs that make up the alimentary canal.
Mouth, pharynx, esophagus, stomach, small intestine, large intestine.
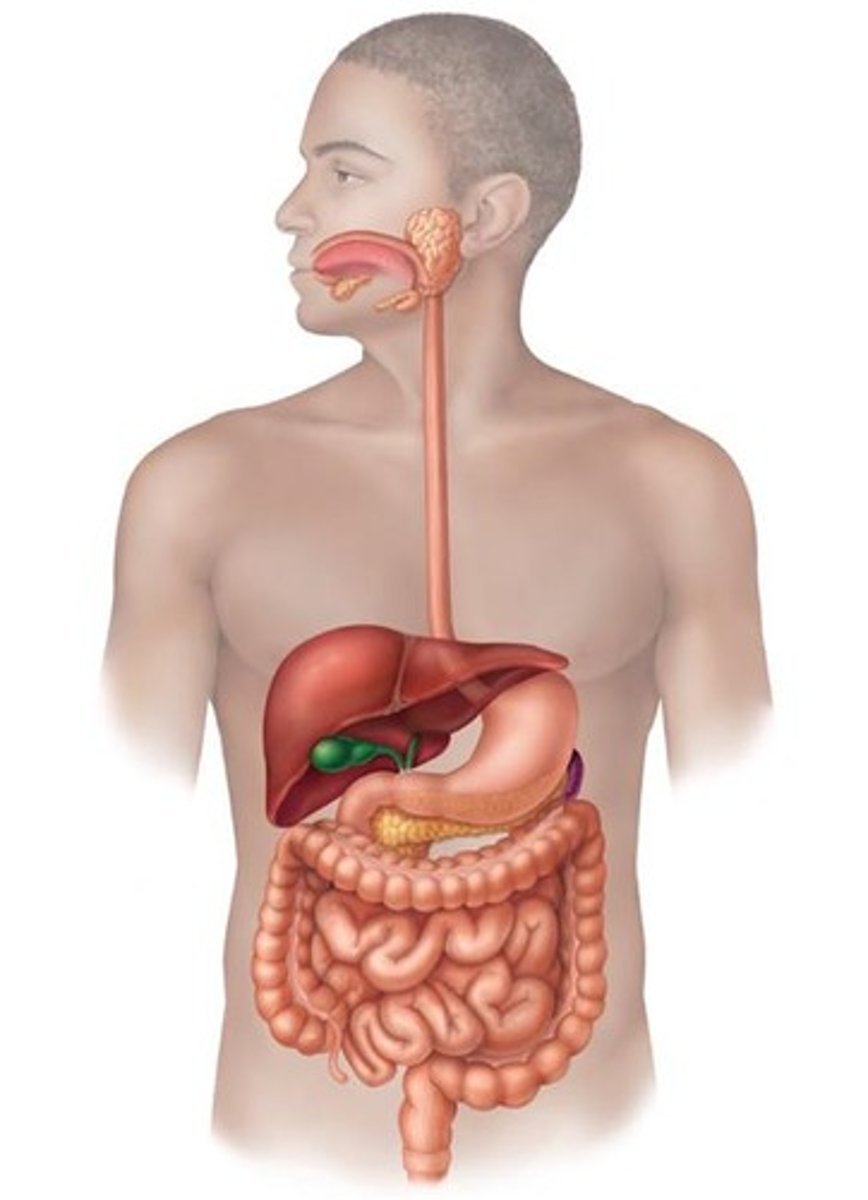
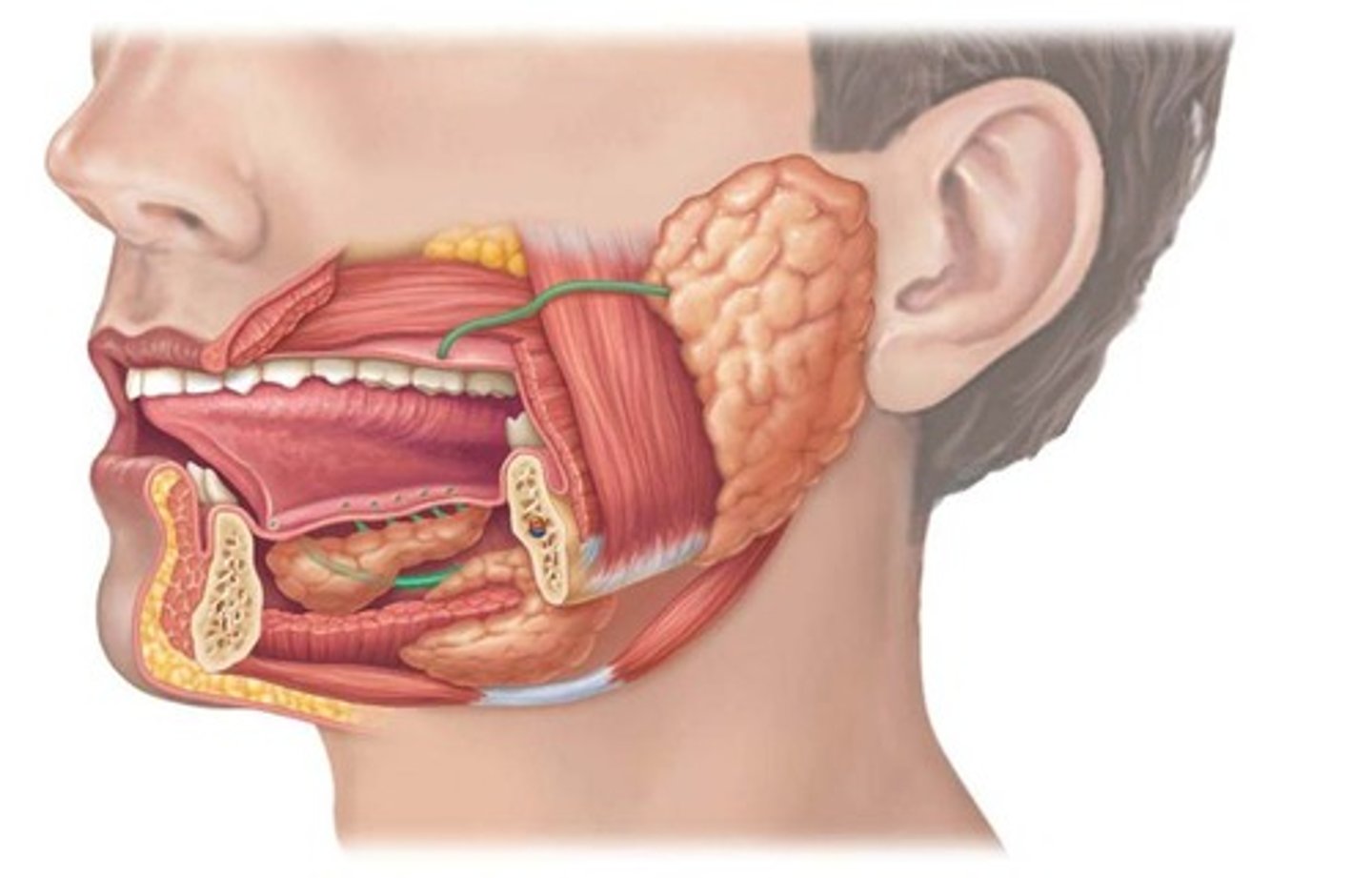
What are the accessory digestive organs?
Teeth, tongue, gallbladder, salivary glands, liver, pancreas.
What are the six essential activities of digestion?
Ingestion, propulsion, mechanical breakdown, digestion, absorption, defecation.
What types of receptors are involved in GI tract regulatory mechanisms?
Mechanoreceptors and chemoreceptors.
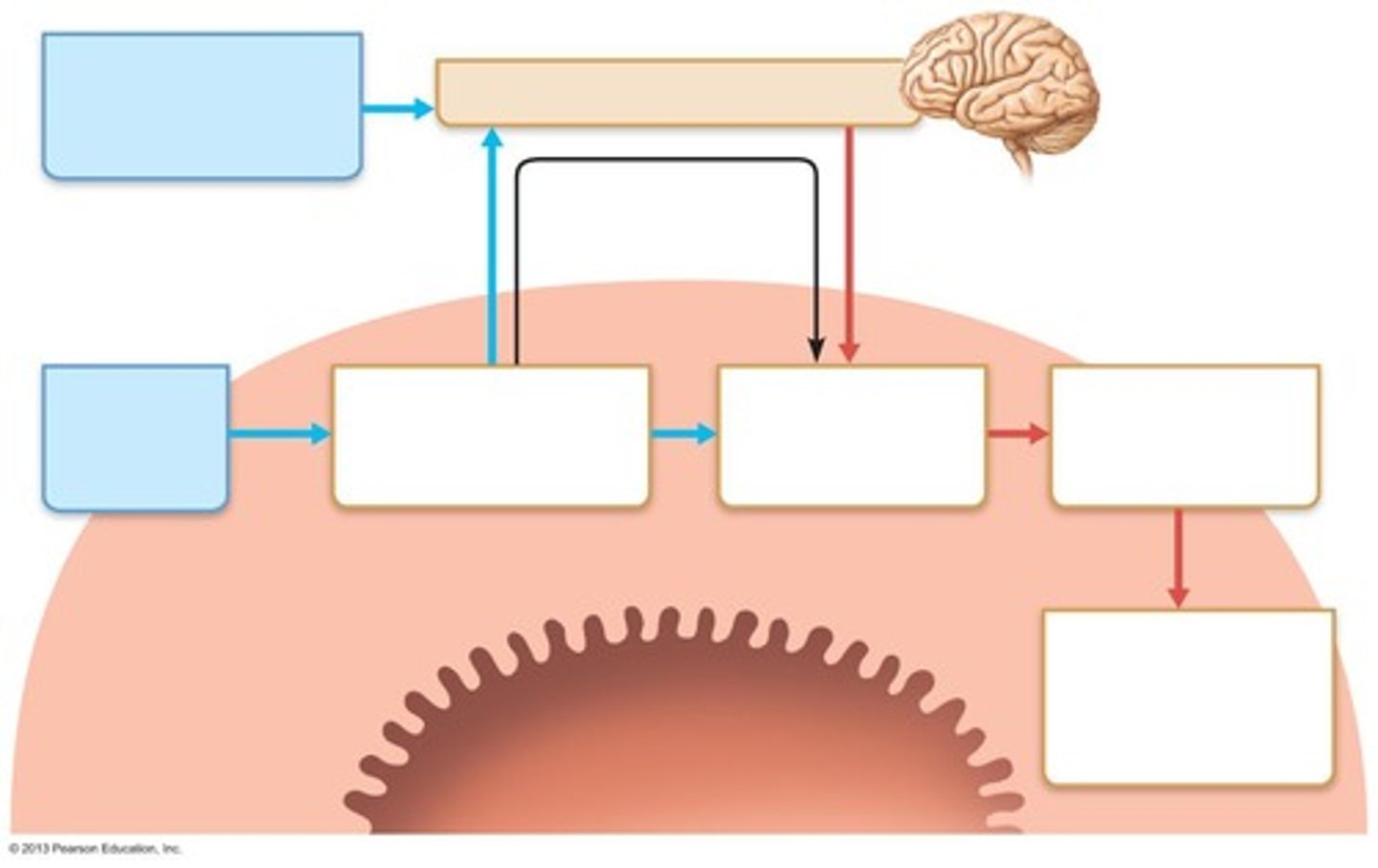
What stimuli do mechanoreceptors and chemoreceptors respond to?
Stretch, changes in osmolarity, pH, presence of substrate, end products of digestion.
What are the two types of controls in GI tract regulation?
Intrinsic and extrinsic controls.
What are short reflexes in the GI tract?
Reflexes that respond to stimuli within the GI tract via enteric nerve plexuses.
What are long reflexes in the GI tract?
Reflexes that involve CNS centers and autonomic nerves responding to stimuli inside or outside the GI tract.
What is the peritoneum?
A serous membrane of the abdominal cavity.
What is the difference between visceral and parietal peritoneum?
Visceral peritoneum covers the external surface of most digestive organs, while parietal peritoneum lines the body wall.
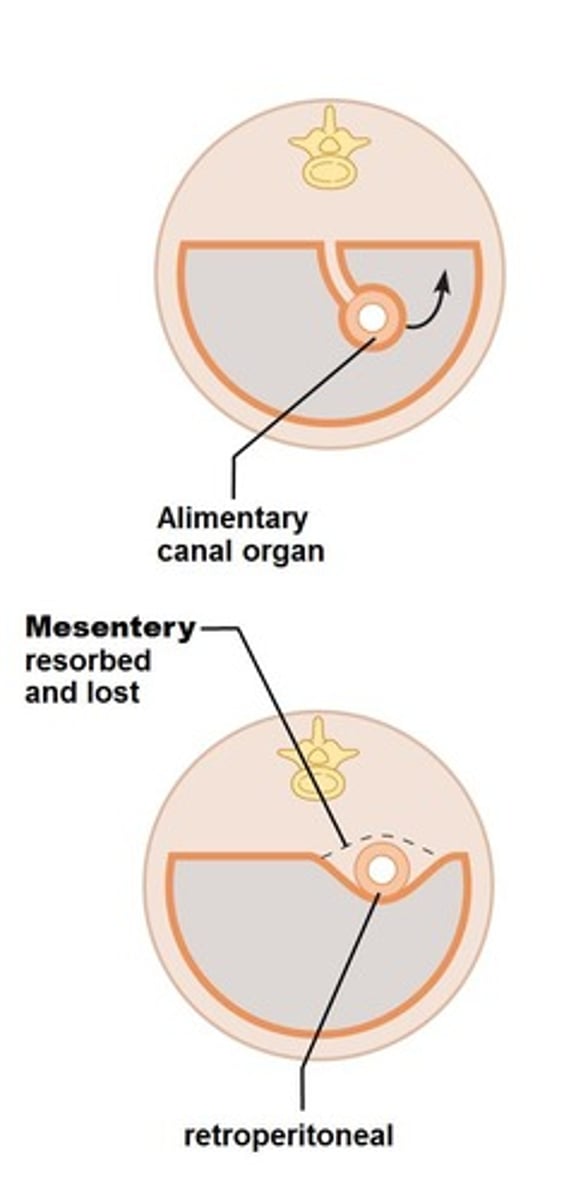
What is the peritoneal cavity?
The space between the visceral and parietal peritoneum, containing fluid that lubricates mobile organs.
What is the function of the mesentery?
It routes blood vessels, lymphatics, and nerves, holds organs in place, and stores fat.
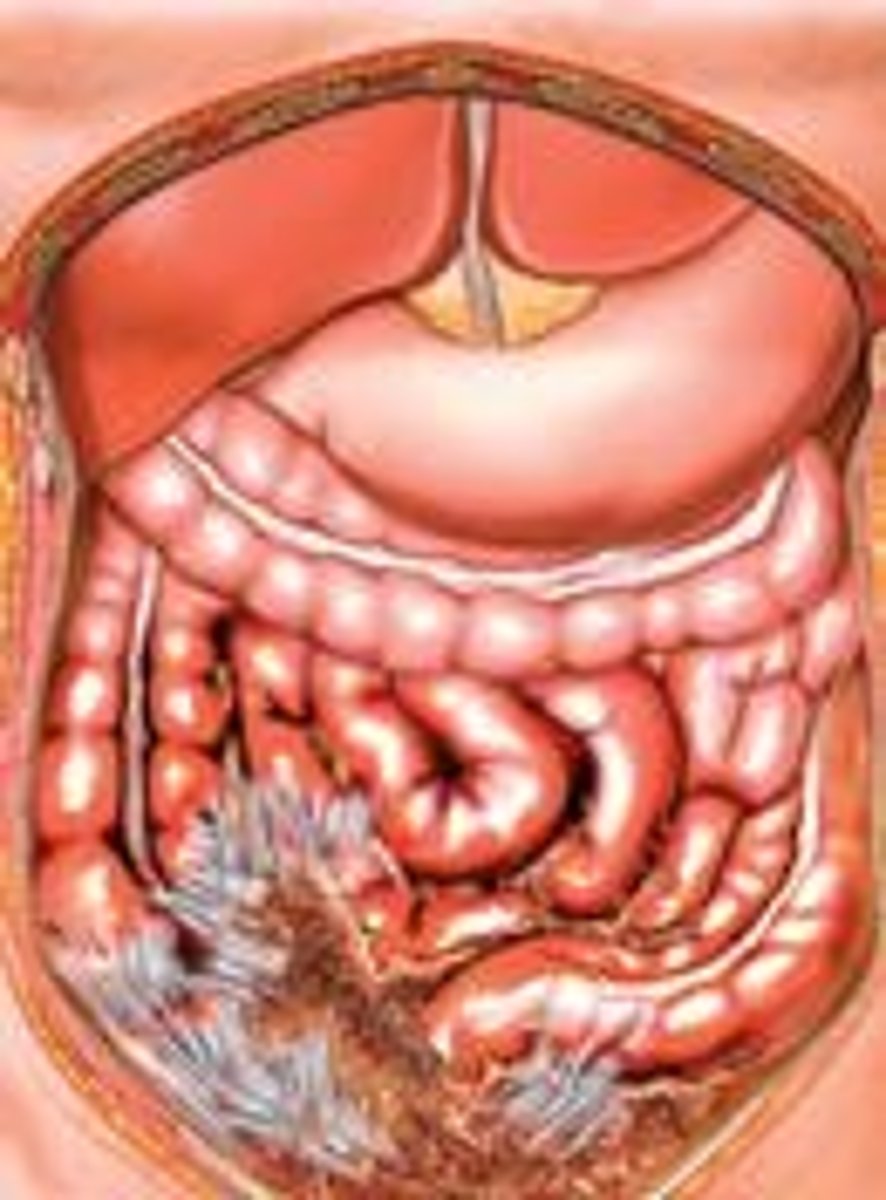
What are intraperitoneal organs?
Organs that are completely surrounded by peritoneum.
What are retroperitoneal organs?
Organs that are located posterior to the peritoneum.
Give an example of an intraperitoneal organ.
The stomach.
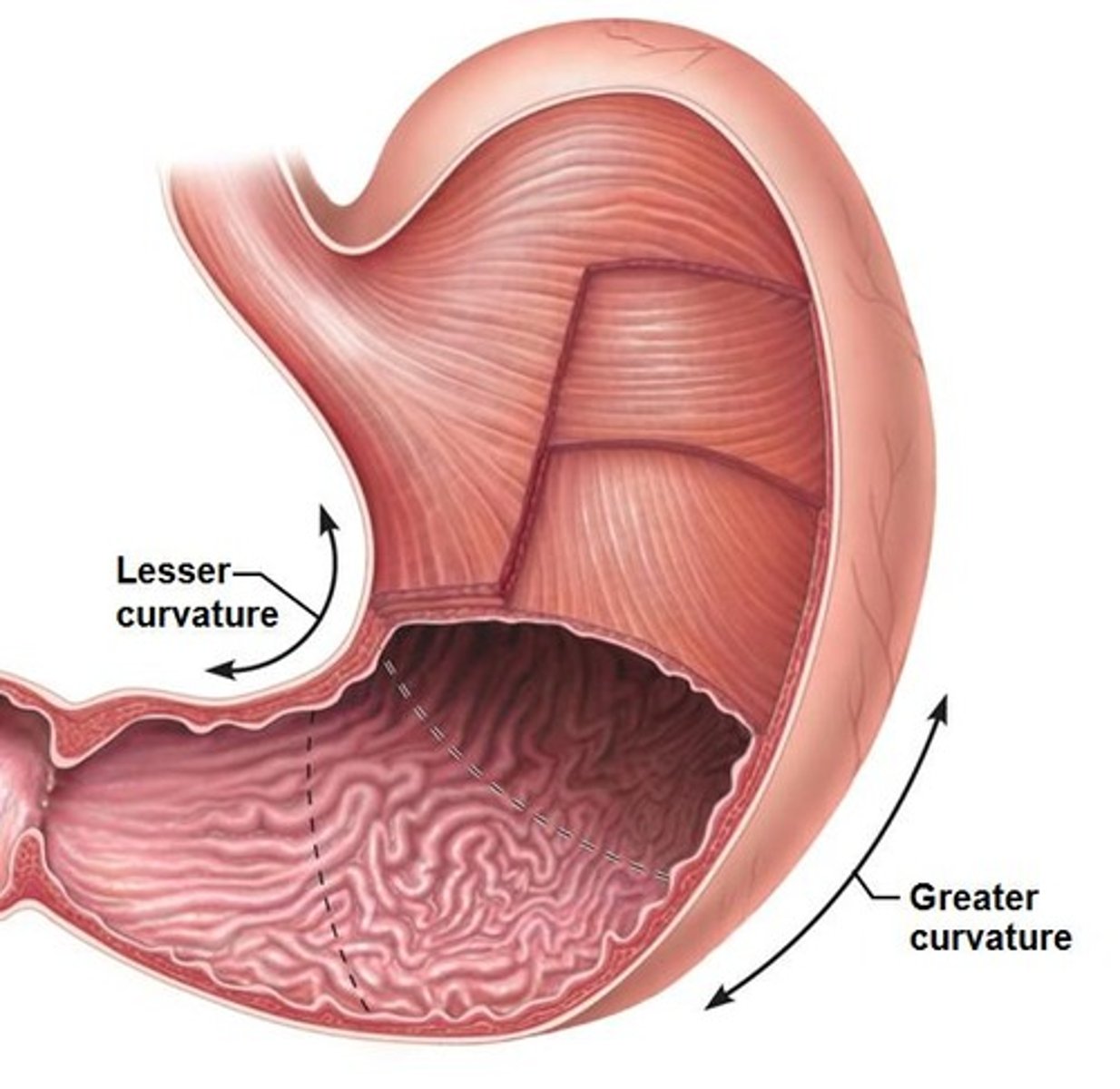
Give an example of a retroperitoneal organ.
The kidneys.
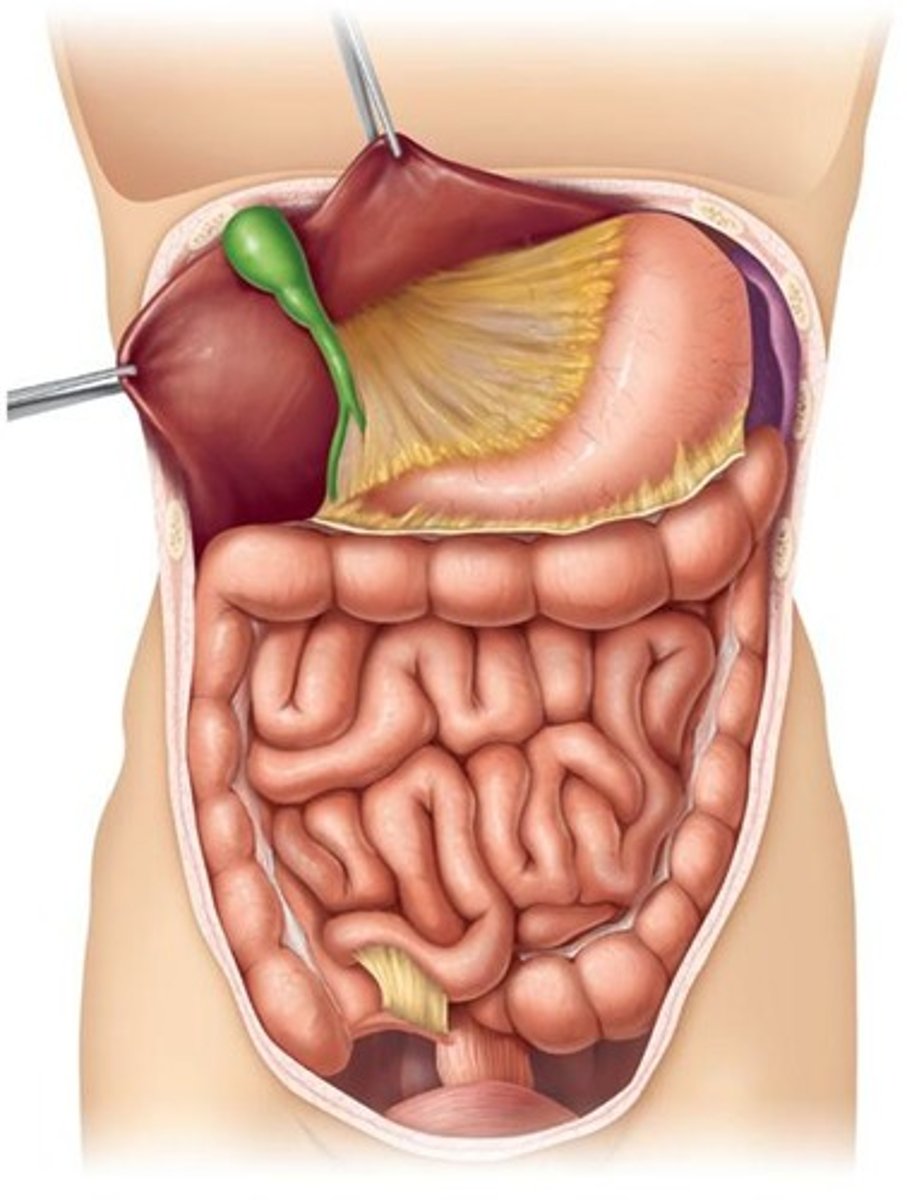
What initiates reflexes that activate or inhibit digestive glands?
Stimuli detected by mechanoreceptors and chemoreceptors.
What does the term 'defecation' refer to?
The elimination of indigestible substances from the body.
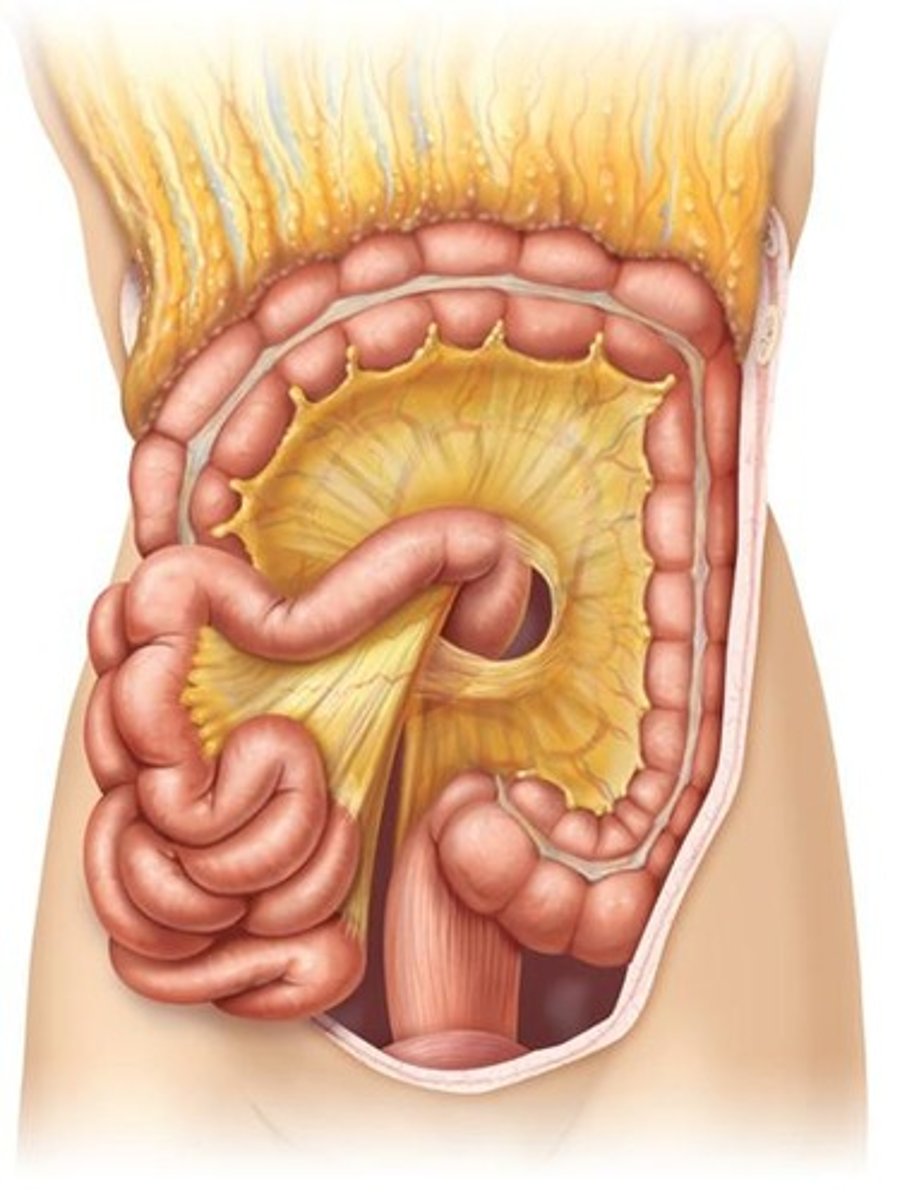
What is the role of the smooth muscle in the GI tract?
To mix and move lumen contents.
What is peritonitis?
Inflammation of the peritoneum, often caused by a piercing abdominal wound, perforating ulcer, or ruptured appendix.
What are the four basic layers of the alimentary canal?
Mucosa, Submucosa, Muscularis externa, and Serosa.
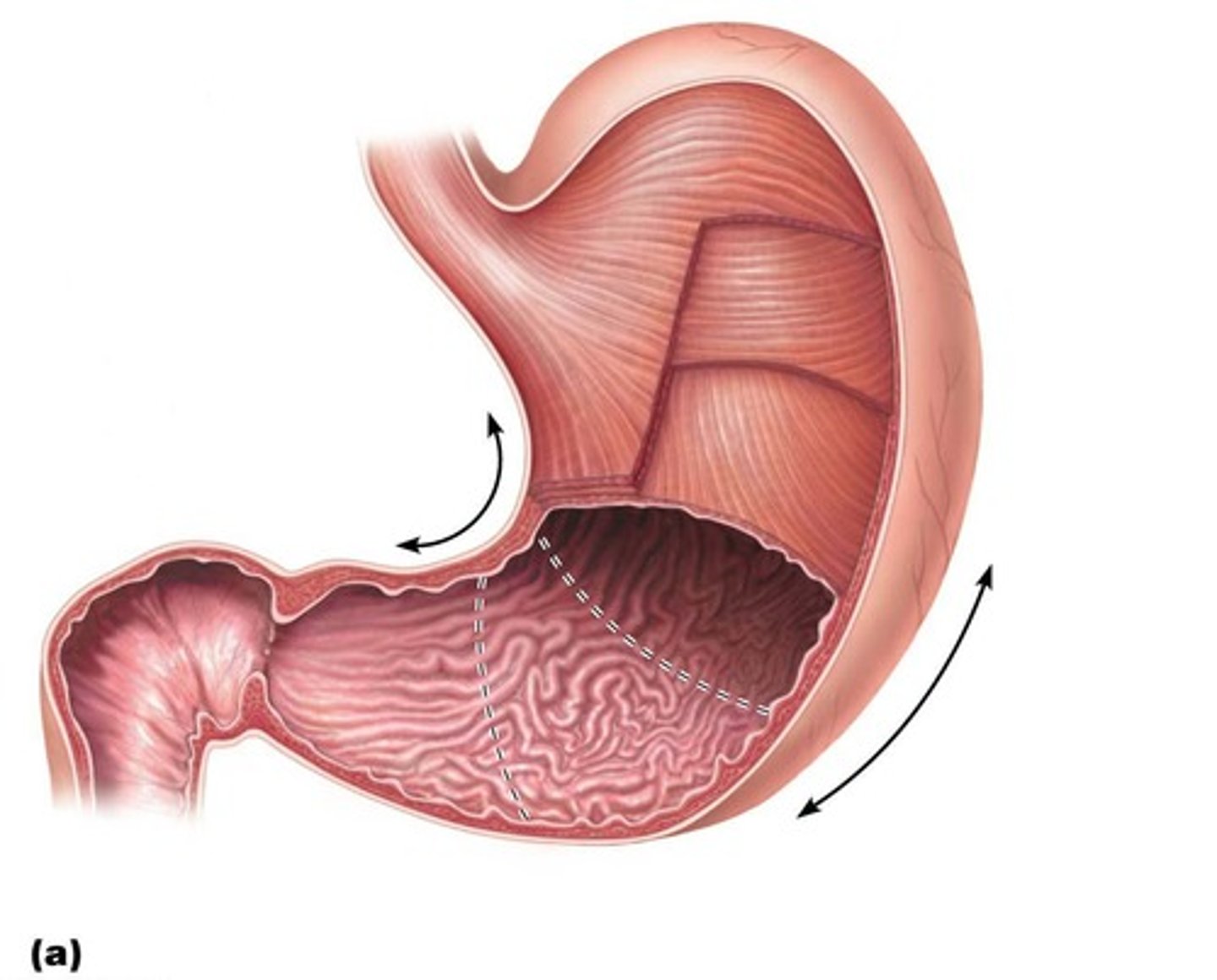
What is the function of the mucosa?
Secretes mucus, digestive enzymes, and hormones; absorbs end products of digestion; protects against infectious disease.
What are the three sublayers of the mucosa?
Epithelium, Lamina Propria, and Muscularis mucosae.
What type of epithelium lines the mucosa of the alimentary canal?
Simple columnar epithelium with mucus-secreting cells.
What is the role of the muscularis mucosae?
Smooth muscle that facilitates local movements of the mucosa.
What does the submucosa contain?
Areolar connective tissue, blood and lymphatic vessels, lymphoid follicles, and the submucosal nerve plexus.
What is the function of the muscularis externa?
Responsible for segmentation and peristalsis, with inner circular and outer longitudinal layers.
What is the myenteric nerve plexus?
A nerve plexus located between the two muscle layers of the muscularis externa that controls GI tract motility.
What is the serosa?
The visceral peritoneum, which is areolar connective tissue covered with mesothelium in most organs.
What is the enteric nervous system?
The intrinsic nerve supply of the alimentary canal, controlling motility and linked to the CNS.
What are the major functions of the mouth?
Repositioning and mixing food, formation of bolus, initiation of swallowing, speech, and taste.
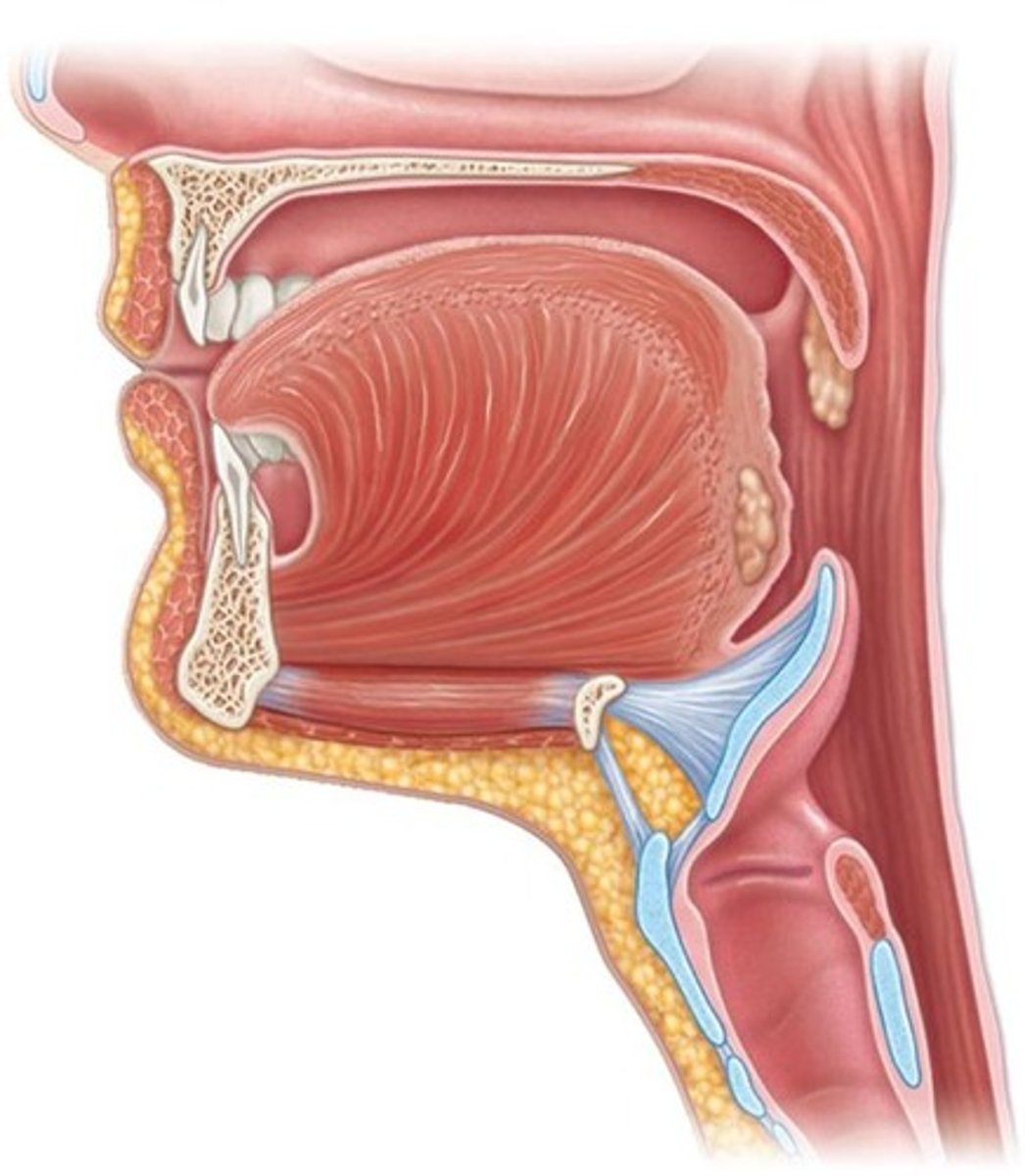
What forms the hard palate?
Palatine bones and palatine processes of maxillae.
What is the function of the uvula?
Closes off the nasopharynx during swallowing.
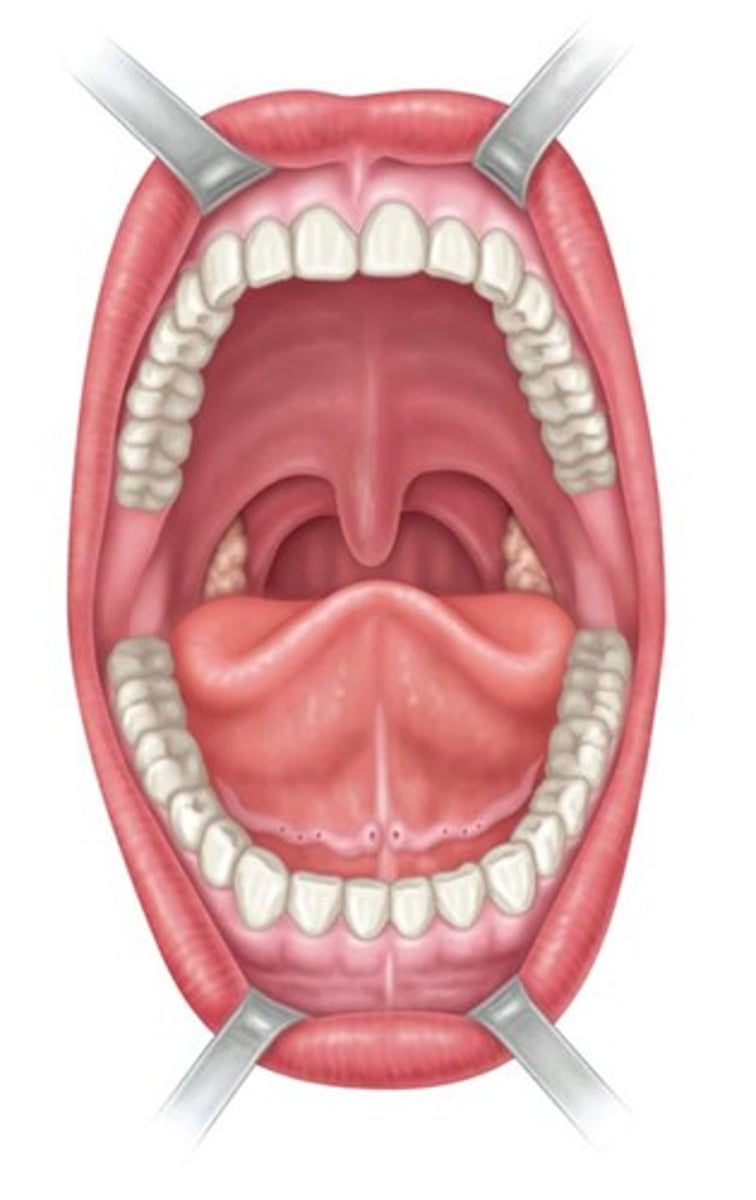
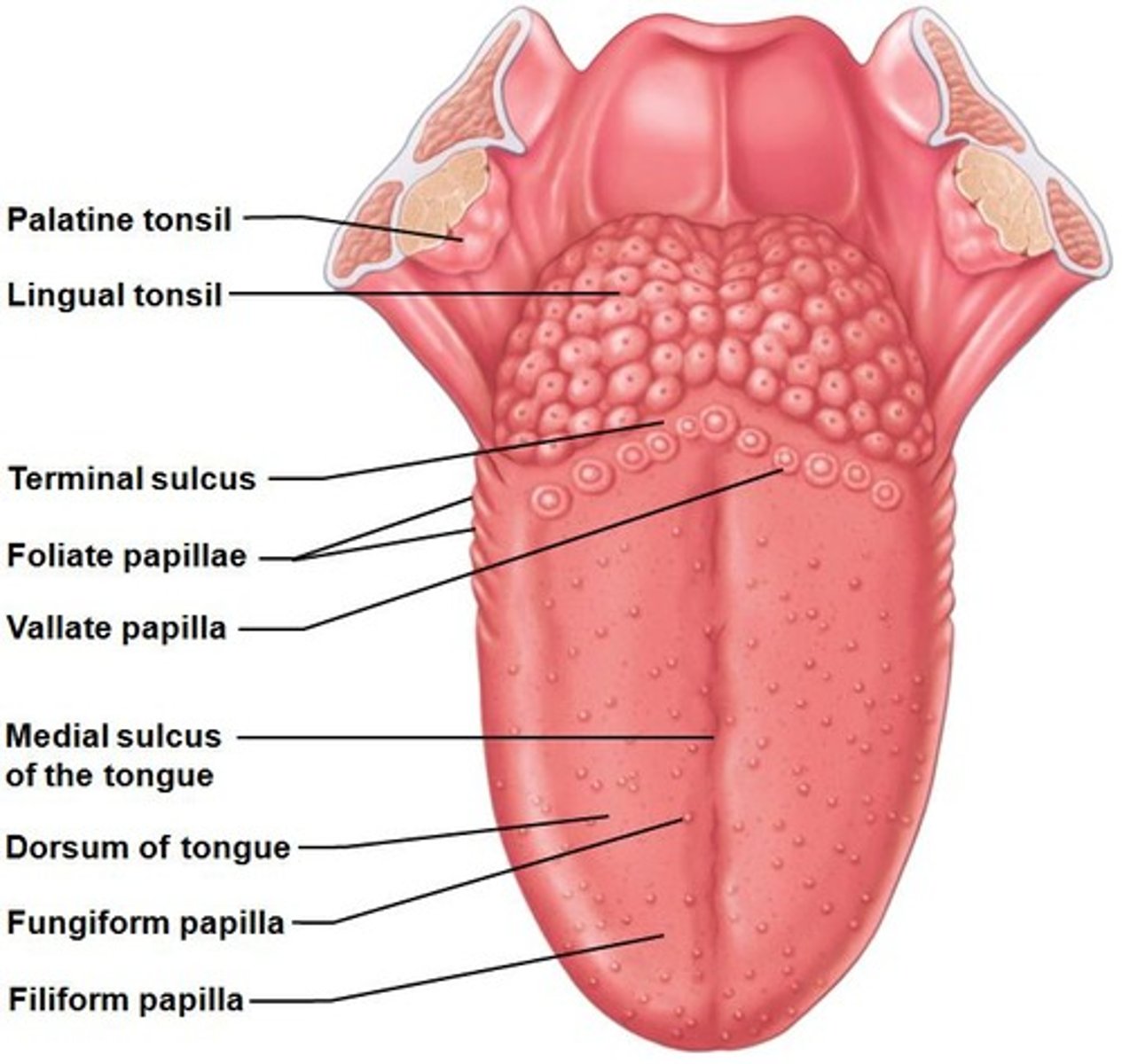
What are the intrinsic muscles of the tongue responsible for?
Changing the shape of the tongue.
What is the primary function of saliva?
Cleanses the mouth, dissolves food chemicals for taste, moistens food, and begins breakdown of starch.
What are the three types of extrinsic salivary glands?
Parotid, Submandibular, and Sublingual glands.
What is the composition of saliva?
97-99.5% water, electrolytes, salivary amylase, lingual lipase, mucin, and metabolic wastes.
What stimulates salivation?
Parasympathetic nervous system activation when food stimulates chemoreceptors and mechanoreceptors in the mouth.
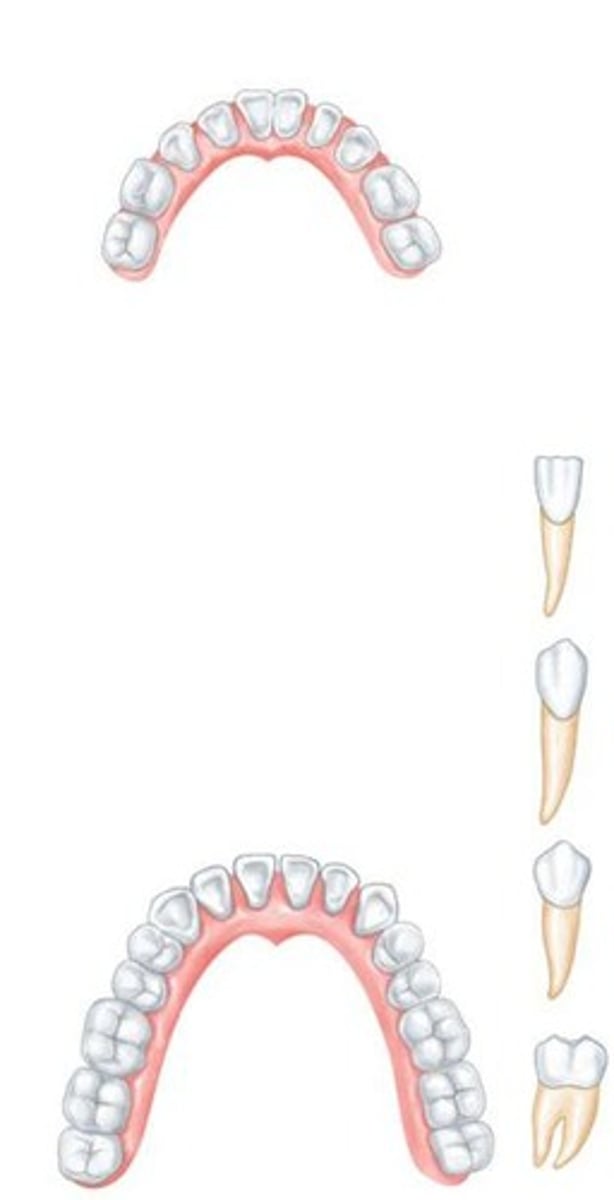
What are the classes of teeth?
Incisors, Canines, Premolars, and Molars.
What is the crown of a tooth?
The exposed part above the gingiva, covered by enamel.
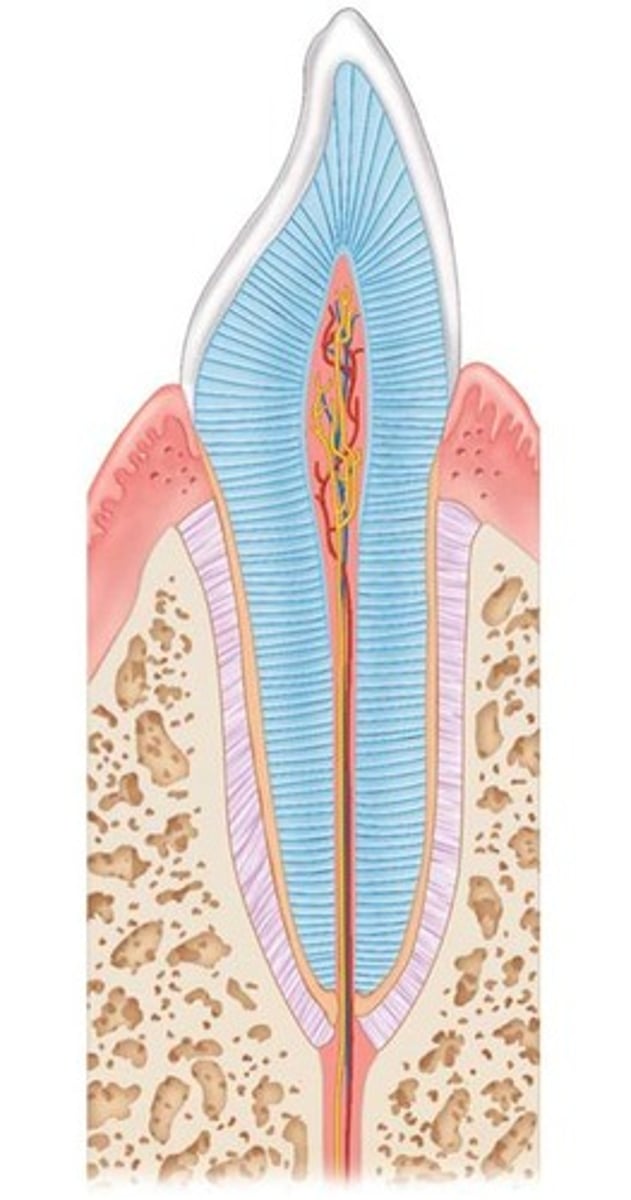
What is the role of the periodontal ligament?
Anchors the tooth in the bony socket, forming a fibrous joint called gomphosis.
What is dentin?
A bonelike material under enamel, maintained by odontoblasts of the pulp cavity.
What is the pulp cavity?
The space surrounded by dentin containing connective tissue, blood vessels, and nerves.
What is the apical foramen?
The entry point for blood vessels and nerves at the proximal end of the root.
What is the function of the lingual lipase?
A fat-digesting enzyme secreted by serous cells in the tongue.
What is xerostomia?
Dry mouth resulting from strong sympathetic stimulation that inhibits salivation.
What is the function of the pulp cavity in a tooth?
It houses the tooth's nerve and blood supply.
What causes dental caries?
Demineralization of enamel and dentin from bacterial action.
What is dental plaque?
A film of sugar, bacteria, and debris that adheres to teeth.
What is gingivitis?
Inflammation of the gums caused by plaque buildup.
What is periodontitis?
A severe gum infection that can lead to tooth loss and affects the periodontal ligament.
What are the risk factors for periodontitis?
Smoking, diabetes mellitus, and oral piercing.
What is the role of the pharynx in digestion?
It allows the passage of food, fluids, and air.
What is the esophagus?
A flat muscular tube that connects the laryngopharynx to the stomach.
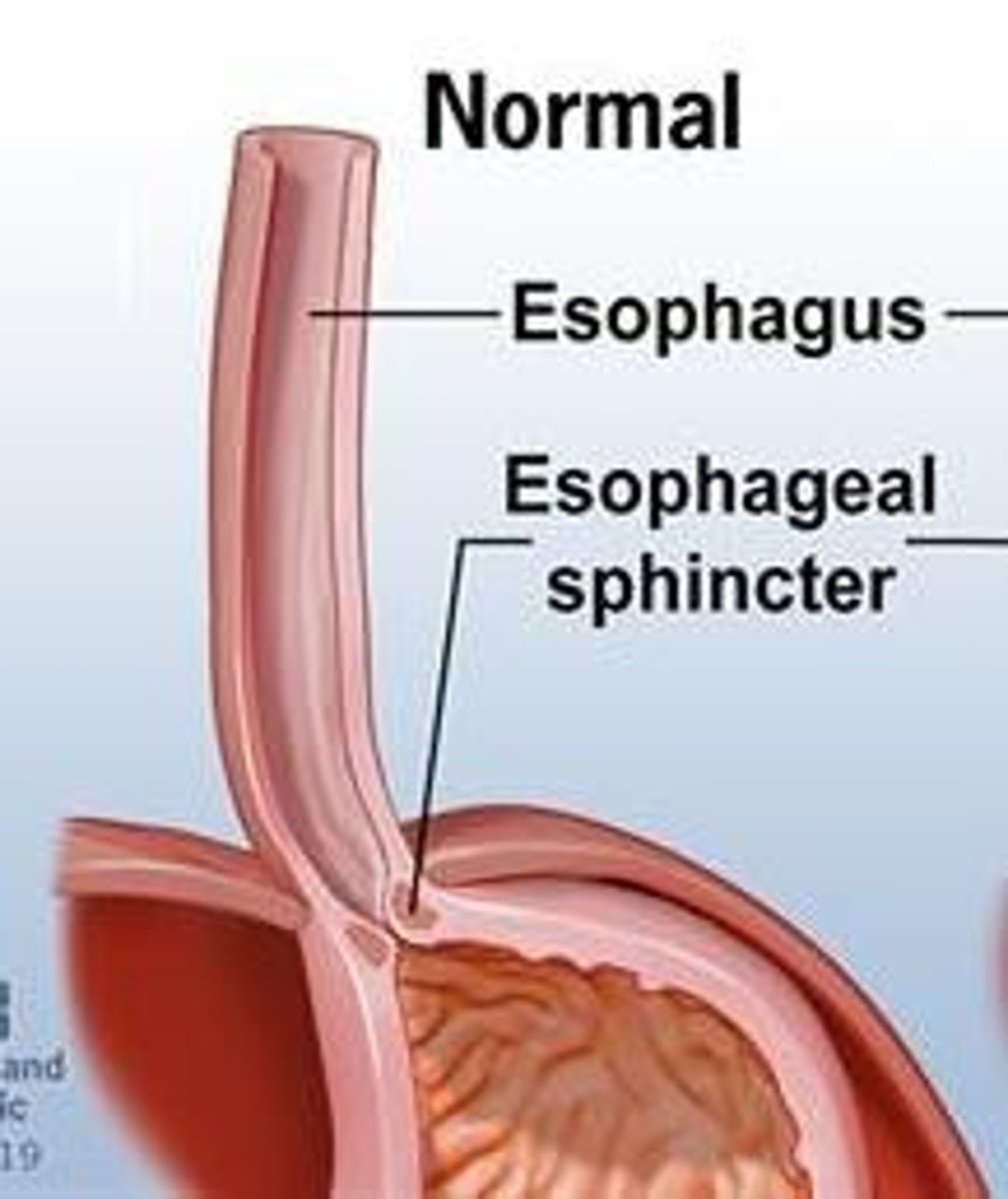
What is heartburn?
A condition where stomach acid regurgitates into the esophagus.
What type of epithelium is found in the esophagus?
Stratified squamous epithelium.
What is the function of the gastroesophageal sphincter?
It surrounds the cardial orifice and prevents acid reflux.
What are the main digestive processes that occur in the mouth?
Ingestion, mechanical digestion, propulsion, and chemical digestion.
What is deglutition?
The process of swallowing food.
What are the four tunics of the stomach?
Mucosa, submucosa, muscularis externa, and adventitia.
What is the function of the gastric glands?
They produce gastric juice for digestion.
What is the role of hydrochloric acid (HCl) in the stomach?
It denatures proteins, activates pepsin, and kills bacteria.
What is intrinsic factor?
A glycoprotein required for the absorption of vitamin B12 in the small intestine.
What is the function of pepsinogen?
It is an inactive enzyme that is activated to pepsin by HCl.
What is the mucosal barrier in the stomach?
A thick layer of bicarbonate-rich mucus that protects the stomach lining.
What can cause gastritis?
Anything that breaches the mucosal barrier, leading to inflammation.
What are peptic ulcers?
Erosions of the stomach wall, often caused by Helicobacter pylori bacteria.
What is the primary function of the stomach?
To secrete intrinsic factor for vitamin B12 absorption and to digest food.
What is the significance of the rugae in the stomach?
They allow the stomach to expand and increase surface area for digestion.
What is the role of enteroendocrine cells in the gastric glands?
They secrete hormones and chemical messengers that regulate digestion.
What is the function of the greater omentum?
It drapes over the intestines and contains fat deposits and lymph nodes.
What is the pyloric valve?
A sphincter that controls stomach emptying into the duodenum.
What is the primary function of the small intestine?
To absorb nutrients from digested food.