Peds: Infection and Skin Disorders
1/86
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
87 Terms
The nurse is preparing to administer an immunization to a toddler. For each of the interventions listed, note if the intervention is indicated or contraindicated: confirm informed consent
The nurse is preparing to administer an immunization to a toddler. For each of the interventions listed, note if the intervention is indicated or contraindicated: provide the VIS
The nurse is preparing to administer an immunization to a toddler. For each of the interventions listed, note if the intervention is indicated or contraindicated: restrain the child
The nurse is preparing to administer an immunization to a toddler. For each of the interventions listed, note if the intervention is indicated or contraindicated: administer acetylsalicylic acid
The nurse is preparing to administer an immunization to a toddler. For each of the interventions listed, note if the intervention is indicated or contraindicated: use comfort positioning
impetigo, cellulitis
What are bacterial skin infections?
molluscum contagiosum, herpes simplex (oral/genital), varicella zoster (chickenpox/shingles), fever blisters
What are viral skin infections?
tinea corporis (ringworm), candidiasis
What are fungal skin infections?
lice (pediculosis), scabies, bed bugs, pinworms
What are parasitic skin infections?
A.
The nurse has finished teaching a parent about caring for their child with impetigo. What statement indicates more teaching is necessary?
A. This is caused by a virus
B. I will administer antibiotic ointment to the crusts
C. I will encourage my child to avoid scratching
impetigo, cellulitis (bacterial skin infections)
Caused by Staph aureus or Strep pyogenes; spread by contact or minor skin trauma.
honey-colored crusts (impetigo), redness, swelling, warmth (cellulitis); fever possible.
What is the nursing assessment for bacterial skin infections?
clinical exam; wound culture if severe.
What are the diagnostics for bacterial skin infections?
topical mupirocin; oral cephalexin or clindamycin. severe cases parenteral antibiotics
What are the medications for bacterial skin infections?
contact precautions, hygiene education (trim nails, avoid scratching), monitor for systemic spread
What are the interventions for bacterial skin infections?
impetigo
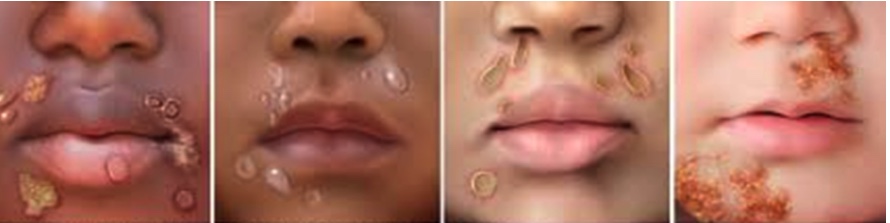
scarlatina (scarlet fever)
Caused by Group A β-hemolytic Streptococcus
sick contacts, recent Strep infection, abrupt onset of fever, sore throat, headache, malaise, nausea/vomiting, sandpaper rash
What is the nursing assessment for scarlatina?
strawberry tongue, fine, sandpaper rash, Pastia’s lines, throat culture, CBC
What are the diagnostics for scarlatina?
infection control: hygiene, droplet precautions until 24 hours, change toothbrush, supportive care: fluids soft foods, gargle, monitor I&O
What are the nursing interventions for scarlatina?
antibiotic therapy, fever reducer
What are the medications for scarlatina?
C.
A child has ringworm of the body. What should the nurse include in the teaching plan?
A. Take antibiotics for 7-10 days
B. Ringworm is not contagious
C. Do not share grooming items
fungal infections
Superficial ___________ (dermatophyte)
tinea corporis, candidiasis, thrush
What are examples of fungal infections?
ring-shaped lesions, scaling, itching, redness, peeling
What is the assessment of tinea?
white patches, erythema, thrush, diaper rash.
What is the assessment of candida?
parasitic/infestation disorders
Infestation by insects or mites; spread through close contact or contaminated objects.
lice, scabies, bed bugs, pinworms
What are examples of parasitic/infestation disorders?
insect bites/stings: general management
• Most insect bites are harmless, know your risk based on geographic area
• Prevent secondary infections
• Children at risk for severe reactions/anaphylaxis should wear a medical alert bracelet:
Prevent bites
Avoid tall grass
Use insect repellent
Avoid contact with insects
Avoid wood piles
Inspect and treat pets, carpets, furniture
Avoid flowery prints and bright clothing
Avoid perfumes and colognes
vector-borne diseases
Borrelia burgdorferi (spirochete bacteria) via tick bite.
B.
The nurse is caring for a child with atopic dermatitis. When is the best time to apply moisturizer to the child?
A. In the morning
B. After a bath
C. When the skin is dry and cracked
lyme disease (bulls-eye rash)
What is an example of vector-borne diseases?
inflammatory/allergic skin conditions
immune hypersensitivity reaction; genetic and environmental triggers.
atopic dermatitis, contact dermatitis, poison ivy exposure, urticaria, angioedema
What are examples of inflammatory/allergic skin conditions?
pruritus, erythema, vesicles or hives, swelling, family history of eczema, asthma, food allergies, or allergic rhinitis (genetic predisposition)
What is the s/s of inflammatory/allergic skin conditions?
history, clinical presentation, patch testing for contact dermatitis, allergen testing
What are the diagnostics of inflammatory/allergic skin conditions?
antihistamines, topical corticosteroids (systemic if widespread), emollients, epinephrine for angioedema
What are the medications of inflammatory/allergic skin conditions?
avoid triggers, avoid overheating, avoid scratching, skin hydration, teach gentle skincare, use mild soap and moisturizers, colloid baths, emergency preparedness for anaphylaxis
What are the interventions of inflammatory/allergic skin conditions?
A.
The nurse is caring for a 12-month-old child that is burned over 20% of their total body surface area. What is a priority for this child?
A. Fluid replacement
B. Protein replacement
C. Antibiotic therapy
cutaneous burns
thermal or chemical injury to skin.
injury to skin and underlying tissues caused by heat, chemicals, electricity, radiation, or friction; classified by depth
What are the clinical symptoms to cutaneous burns?
pain, erythema, burn depth/classification
What is the nursing assessment to cutaneous burns?
clinical; burn severity classification, TSA
What is the testing to cutaneous burns?
silver sulfadiazine, bacitracin, honey, aloe vera, pain relief
What are the medications to cutaneous burns?
ABCs, burns involving more than 10% of TBSA require fluid resuscitation, fluid balance for burns.
What are the interventions to cutaneous burns?
Lund and Browder chart
a medical tool used to estimate the total body surface area (TBSA) providing a more accurate calculation than simpler methods like the "Rule of Nines," especially for children.
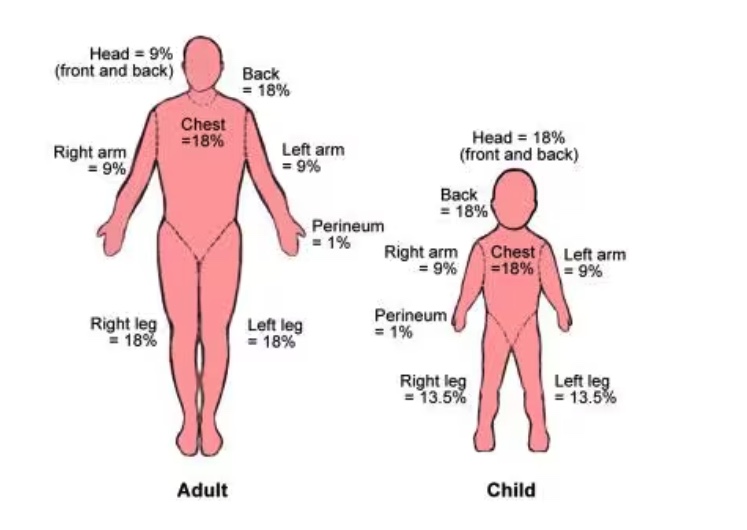
Parkland Formula for Fluid Replacement (for adults/teens)
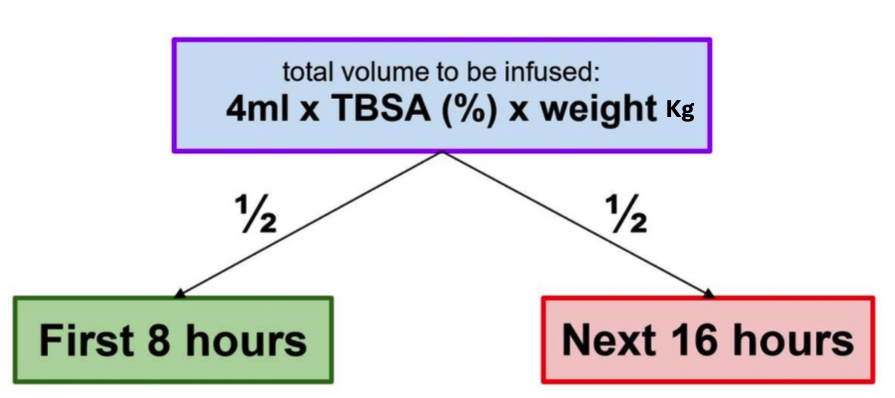
crystalloids; colloids
For pediatric burn fluid resuscitation, ___________ are the initial choice, often with the use of the Parkland formula.
________ are considered a "rescue" treatment for severe burns that require more fluid, as they can help expand blood volume more effectively.
acne vulgaris
Inflammation of sebaceous glands
blackheads, whitehead, papules, pustules, nodules, cysts
What are the clinical symptoms to acne vulgaris?
history and a physical examination type, severity, and location of lesions, as well as their psychosocial impact
What is the assessment to acne vulgaris?
clinical presentation
What is the diagnostic to acne vulgaris?
benzoyl peroxide, retinoids, antibiotics, isoretinoin
What are the medications to acne vulgaris?
skin hygiene, avoid picking, monitor infection
What are the nursing interventions to acne vulgaris?
fever, poor perfusion, tachycardia, tachypnea, shock
What are the s/s to neonatal/pediatric sepsis?
neonatal/pediatric sepsis
Systemic inflammatory response to infection
ABCs, respiratory distress, fluid resuscitation, thermoregulation
What is the nursing assessment to neonatal/pediatric sepsis?
blood cultures, CBC, CRP
What is the testing to neonatal/pediatric sepsis?
broad-spectrum antibiotics, respiratory support, circulatory support
What are the medications to neonatal/pediatric sepsis?
early recognition, monitor vitals, IV fluids and meds, assess infection risks and monitor for S/S
What are the interventions to neonatal/pediatric sepsis?
B.
An adolescent is diagnosed with mononucleosis. What education should the nurse provide?
A. Mononucleosis is only contagious for the first 7 days of the illness
B. Avoid contact sports and strenuous activities
C. Take antibiotics for the full 10 days of treatment
mononucleosis
Epstein-Barr virus (EBV). The virus infects B lymphocytes (white blood cells) in the oropharynx (throat).
fever, flu-like symptoms, sore throat, lymphadenopathy, hepatosplenomegaly
What is the s/s of mononucleosis?
asking about symptoms like fever, fatigue, sore throat, and swollen lymph nodes, fever, pharyngitis, lymphadenopathy
What is the nursing assessment to mononucleosis?
EBV titers, monospot, ESR, CRP, CBC
What is the testing to mononucleosis?
early recognition, monitor vitals, IV fluids, family education on rest and infection control. supportive care for mono
What are nursing interventions to mononucleosis?
ENT and mucosal infections
Viral/bacterial infection of conjunctiva or ear canal/middle ear.
conjunctivitis, otitis media, otitis externa
What are examples of ENT and mucosal infections?
redness, discharge, pain, decreased hearing, fever
What are s/s of ENT and mucosal infections?
otoscopic exam, ophthalmoscopic exam culture if needed
What is the testing of ENT and mucosal infections?
antibiotic or antiviral drops, analgesics
What are the medications of ENT and mucosal infections?
hygiene (no towel sharing), eye care, warm compresses, Eye/ Ear drop administration teaching, no Q-tips
What are the interventions of ENT and mucosal infections?
live vaccines
like the MMR vaccine, are contraindicated in individuals who are pregnant or immuno-compromised. Additionally, if planning to become pregnant, the individual should wait at least 4 weeks to conceive after receiving one.
• Examples: MMR, varicella, nasal spray flu, rotavirus, shingles (adults)
viral exanthems
Viral infections producing characteristic rashes and systemic
skin rashes or eruptions caused by a viral infection, and they often appear with other symptoms like fever, body aches, and fatigue
What is the s/s to viral exanthems?
Koplik spots (rash spreading face → body)
What is the presentation of measles?
parotid gland swelling
What is the presentation of mumps?
fine rash, lymphadenopathy
What is the presentation of rubella?
“slapped cheek” rash
What is the presentation of Fifth Disease?
serologic testing, clinical features
What are tests to viral exanthems?
supportive (antipyretics, fluids)
What are medications to viral exanthems?
isolation precautions, hydration, comfort measures, vaccination education
What are interventions to viral exanthems?
B.
The nurse is admitting a child with measles (rubeola). What is the nurse's best action?
A. Initiate droplet precautions
B. Initiate airborne precautions
C. Initiate protective isolation
C.
On assessment the school nurse notes that the child has a rash the nurse suspects that the child has erythema infectiosum 5th disease because the skin assessment revealed a rash that has which characteristics:
A. A highly periodic perfuse macular to papular rash on the trunk
B. A discreet pinkish red maculopapular rash that is spreading to
the trunk
C. An erythema on the face that has a “slapped face” appearance
D. Discreet rose pink maculopapular rash on the trunk
C.
The nurse is caring for a child with Parvovirus (5th disease). What information in the patient's history or assessment should most concern the nurse?
A. The child broke their femur 6 months ago
B. The child is nauseous
C. The child has sickle cell disease
parvovirus (fifth disease) erythema infectiosum
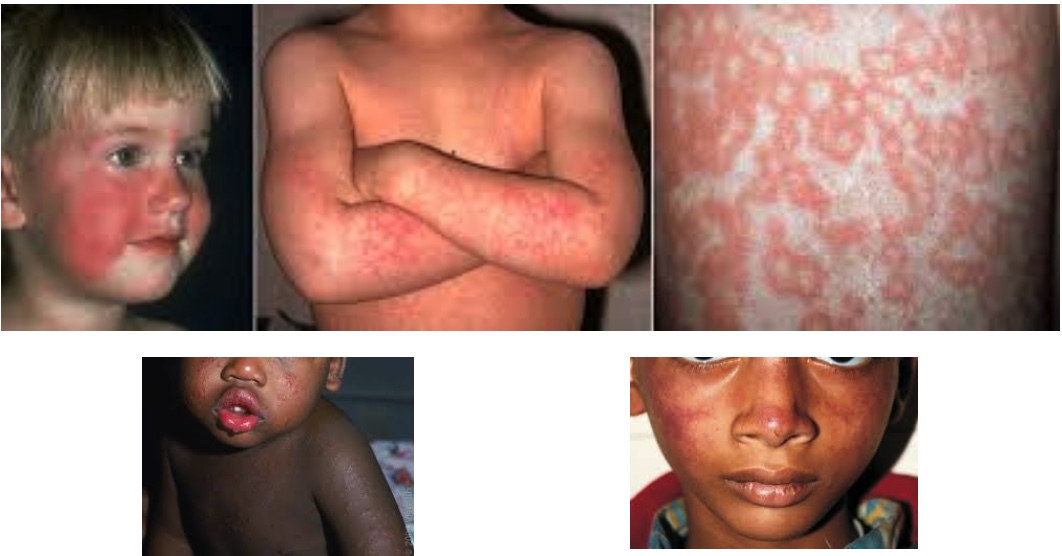
aplastic crisis
a serious complication of fifth disease
can occur in children who already have depleted red blood cells (iron deficiency anemia, sickle cell, etc.)