NURS Clinical Science Spring Exam 2 Study Guide
1/202
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
203 Terms
What drugs are used to treat dyslipidemia?
HMG-CoA Reductase inhibitors (statins), bile acid sequestrants, fibric acid drugs, ezetimibe, niacin, omega-3-acod ehtyl esters (lovaza)
What drugs fall under HMG-CoA reductase inhibitors (statins)?
atorvastatin, fluvastatin, lovastatin, rosuvastatin, simvastatin, pitavastatin
What are serious adverse events of HMG-CoA Reductase inhibitors (statins)?
rhabdomyolysis, myositis, elevated liver enzymes, teratogenicity
What are Bile acid seqeuestrants?
bind to bile acids increasing excretion of cholesterol through the bowel
What drugs fall under bile acid sequestrants?
cholestyramine, colesevelam, coletipol
What falls under fibric acid drugs?
fenofibrate, fenofibric acid, and gemfibrozil
What are serious adverse events of fibric acid drugs?
rhabdomyolysis, gallbladder disease, pancreatitis
What drugs fall under niacin?
vitamin B3 (nicotinic acid)
What are the lipids in the body?
triglycerides, phospholipids, steroids
What are triglycerides?
used for energy; composed of glycerol and other fatty acids
What are phospholipids?
used to build cell membranes
What are steroids?
used to build cell membranes, are also used to make vitamin D, bile acids, cortisol, estrogen, progesterone, and testosterone
What are diuretic medications for hypertension and heart failure?
angiotensin-converting enzyme inhibitors (ACEI) and angiotensin II receptor blockers (ARBs)
What are diuretics?
affect the renin-angiotensin-aldosterone system
What drugs fall under angiotensin-converting enzyme inhibitors (ACEI)?
“prils”; benazepril, captopril, enalapril, lisiniporil
What are serious adverse events of ACEIs and ARBs?
angioedema, acute renal failure, hyperkalemia, teratogenic
What drugs fall under angiotensin II receptor blockers (ARBs)?
“sartans”; valsartan, losartan, olmesartan
What are diuretic medications for heart failure?
osmotic diuretics, carbonic anhydrase inhibitors, loop diuretics, thiazide diuretics, potassium-sparing
What are osmotic diuretics?
mannitol and glycerin
What are carbonic anhydrase inhibitors?
acetazolamide
What are loop diuretics?
furosemide
What are thiazide diuretics?
hydrochlorothiazide
What are potassium-sparing diuretics?
spironolactone
What are common medications that are nephrotoxic?
NSAIDs, some antiviral drugs, some antibiotics, systemic antifungal drugs, ACEI, some chemotherapies, some immunosuppressants, and contrast dye
What is the normal range for a serum pH?
7.35-7.45
What are common assessments used to monitor fluid balance?
measuring intake and output (I/O), daily weight tracking, and physical examinations
What is water distribution in the human body?
water output normally occurs through the kidneys (may also occur through lungs, skin, feces, and sweat)
What is the composition of normal saline?
0.9% NaCl (isotonic)
What are normal serum values for sodium?
135-145
What are normal serum values for potassium?
3.5-5.0
What are normal serum values for calcium?
4-11
What is metabolic acidosis?
occurs due to severe diarhhea, renal failure, diabetes, excessive alcohol intake, starvation (severe CNS depression)
What is respiratory acidosis?
occurs due to lack of breathing (hypoventilation, airway constriction, damage to the respiratory center in the CNS)
What is metabolic alkalosis?
occurs with hypokalemia due to diuretic therapy, severe vomiting, ingestion of substantial amounts of sodium bicarbonate, severe constipation
What is respiratory alkalosis?
occurs due to hyperventilation (below normal CO2)
What drugs are used to treat hypertension?
diuretics, calcium channel blockers (CCB), adrenergic antagonists, direct vasodilators
What are calcium channel blockers (CCB)?
“pines”; amlodipine, nifedipine and diltiazem and verapamil
What are serious adverse events of calcium channel blockers (CCB)?
liver toxicity, heart failure/attach, angioedema, confusion
What are adrenergic antagonists?
block activation of beta and/or alpha receptors of the sympathetic nervous system
What are the classes of adrenergic antagonists?
beta blockers and alpha blockers
What are beta blockers?
“olols”; propranolol, atenolol, metoprolol, nevicolol
What are serious adverse events of beta blockers?
agrunulocytosis, SJS, larngyospasm, anaphylaxis, rebound hypertension
What are alpha blockers?
“zosins” doxazosin, prazosin, terazosin
What are the serious adverse events of alpha blockers?
first-dose hypotension, tachycardia, dyspnea
What are direct vasodilators?
Hydrazaline and minoxidil
What are serious adverse events of direct vasodilators?
severe hypotension, heart attack, dysrhythmias, shock
What drugs increase blood pressure?
systemic steroids, over-the-counter phenylephrine (OCPs), amphetamines, decongestants, nicotine, erythropoietin
What foods/drinks increase blood pressure?
alcohol, caffeine, foods high in sodium
What is stroke volume?
amount of blood pumped by a ventricle in one contraction
What is heart rate?
the number of times the heart beats in a specified time period
What is cardiac output?
volume of blood pumped/minute
What is ischemia?
loss of oxygen to the heart muscle
What is blood pressure?
cardiac output verus peripheral resistance
Cardiac output calculation?
heart rate x stroke volume
What is angina?
episodes of loss of oxygen to the heart muscle causing chest pain
What is prinzmetal angina?
coronary artery vasospasm
What is CAD?
narrowing or occlusion of coronary arteries
What are causes of CAD?
alochol, intake of food with high saturated or trans-fat, tobacco use, low exervise, and high salt intake
What are diagnostic procedures for CAD?
routine history and physical (H&P), EKG, cardiac stress test, angiogram (cardiac catheterization)
What is an EKG?
shows previous heart attack history
What is an angiogram (cardiac catheterization)?
most specific way to detect CAD and most invasive
What drugs are used to treat CAD?
nitrates
What are nitrates?
coronary artery dilating agents (short and long-acting)
What are short-acting nitrates?
nitroglycerin
What are long-acting nitrates?
isosorbide
What are severe adverse events of nitrates?
severe hypotension and syncope
What are common causes of heart failure?
CAD, mitral valve stenosis, MI/heart attack, chronic unconrolled hypertension, diabetes, dyslipiemia, thyroid disorders
What medication are used to treat heart failure specifically?
cardiac glycosides, entresto, phosphodiestera inhibitors and beta-adrenergic agonist, sacubitril-neprilysin inhibitor, dapagliflozin
What are cardiac glycosides?
digitalis/digoxin
What is digoxin?
increases the strength of myocardial contraction, increases cardiac output and suppresses the elctrical conductivity of the heart
What is entresto?
valsartan/sacubril
What are phosphodiesterase inhibitors and beta-adrenergic agonists?
“fils”; sildenafil (viagra), vardenafil, and tadalafil
What is sacubitril-neprilysin inhibitor?
vasodilatory
What is dapagliflozin?
farxiga; inhibits SGLT2
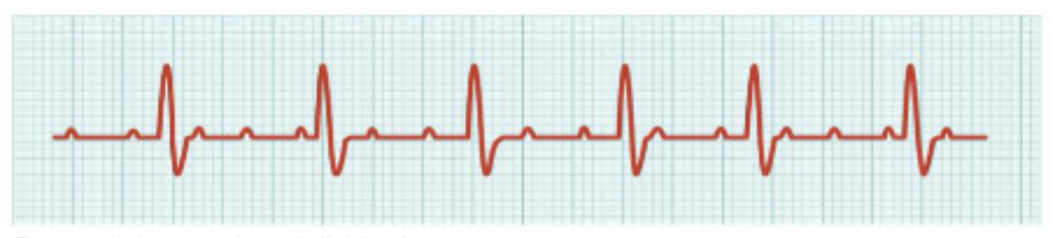
What is this?
second-degree (partial) block
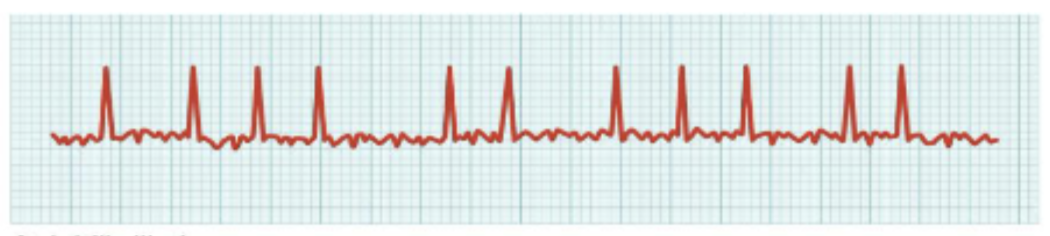
What is this?
atrial fibrillation
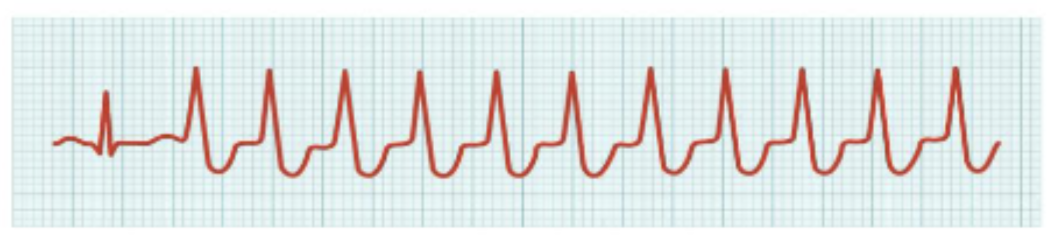
What is this?
ventricular tachycardia
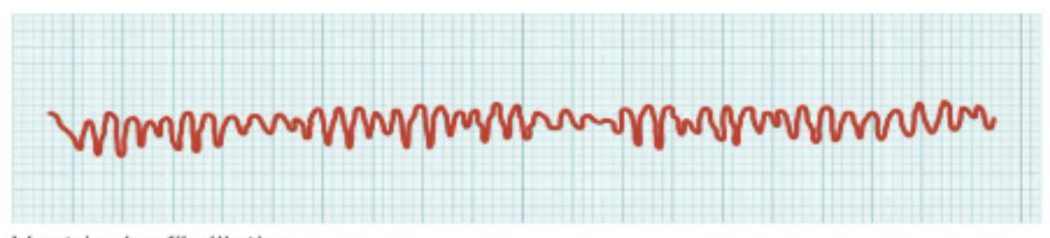
What is this?
ventricular fibrillation
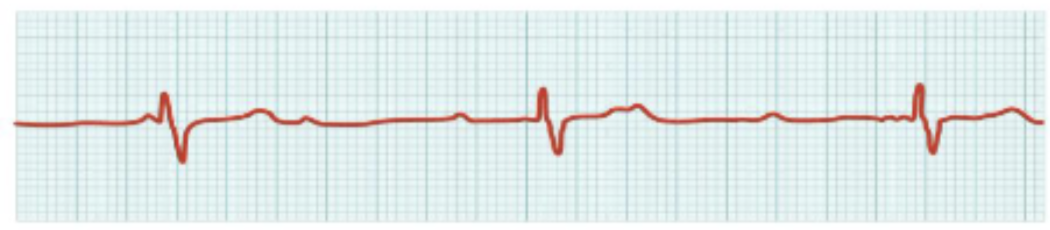
What is this?
third-degree block
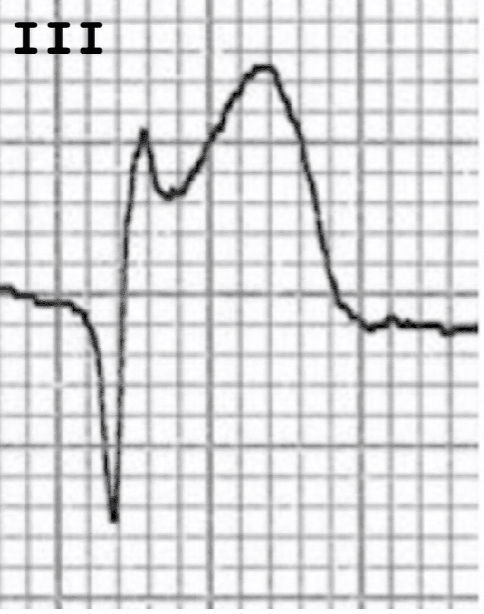
What is this?
ST elevation
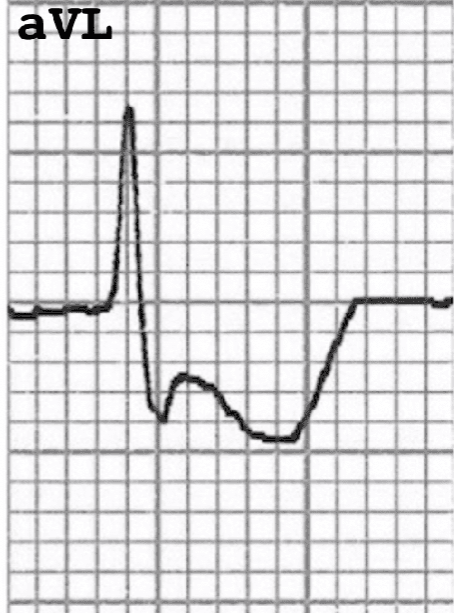
What is this?
reciprocal change
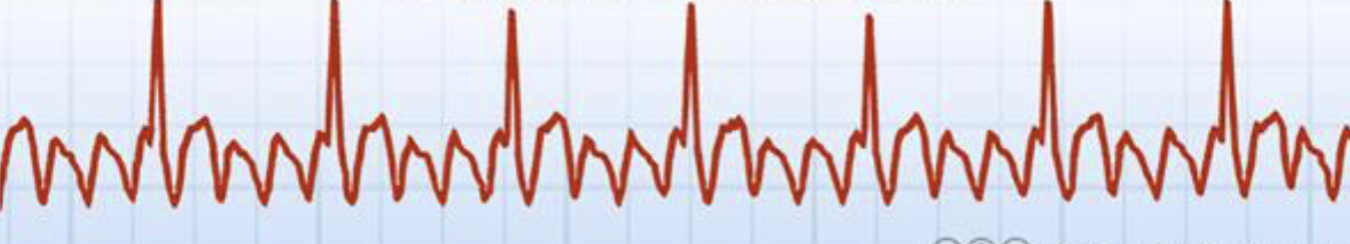
What is this?
Atrial flutter
What are common causes of dysrhythmia?
hypertension, cardiac valve disease, CAD, medications (digoxin), hypokalemia/hypomagnesemia, MI, CVA, DM, heart failure
What drugs are used to treat dysrhythmia?
sodium channel blockers, beta-adrenergic blockers, potassium channel blockers, calcium channel blockers, oral arrhythmia adrugs
What are sodium channel blockers?
prainamide, lidocaine, flecainide
What are beta-adrenergic blockers?
propranolol
What are potassium channel blockers?
amiodarone
What are calcium channel blockers?
verapamil, diltiazem
What are oral arrhythmia drugs?
amiodarone, flecainide, propafenone, beta adrenergic antagonist, and calcium channel blockers
What oral arrhytmia drugs have black box warnings?
amiodarone, flecainide, propafenone, beta-adrenergic antagonist
What are beta adrenergic antagonist?
sotalol
What are parental antiarrhythmics?
atropine, lidocaine, procainamide
What is atropine?
bradycardia; antagonise acetylcholine receptors
What is lidocaine?
ventricular arrhythmia (inhibits sodium ion channels)
What is procainamide?
ventricular/supraventricular arrhythmia (stabilizes membranes)
What is an anaphylatic shock?
severe allergic reaction (usual allergens include PCN, nuts, shellfish)
What is cardiogenic shock?
failure of the heart to pump blood to vital organs
What causes cardiogenic shock?
left heart failure, MI, PE dysrhythmia, myocardial infection
What is hypovolemic shock?
severe loss of blood volume
What causes hypovolemic shock?
massive hemorrhage, burns, severe dehydration (excessive diuresis, N&V, diarrhea)