EM E1: CV
1/128
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
129 Terms
How soon should an EKG be ordered if a pt present to the ED w/ CP?
w/in 10 minutes
What is chest wall pain?
somatic, sharp, localized pain, reproducible by palpation, movement
What is pleuritic or respiratory chest pain?
somatic, sharp pain worsened by breathing or coughing
What is visceral chest pain?
poorly localized pain described as aching or heaviness
Which type of pain is precisely located?
Somatic
Which type of pain is imprecisely localized (discomfort, heaviness, or aching)?
Visceral
What are RF for aortic dissection?
middle aged, male gender, HTN, Marfan syndrome
What causes ACS sx?
myocardial ischemia
What are the 3 types of ACS?
unstable angina, NSTEMI, STEMI
Who has a higher incidence of ACS?
males
How do women w/ ACS present?
w/o typical symptoms
*leads to failure to initially dx
What is angina?
sensation of chest pressure or heaviness, reproduced by activities increase myocardial oxygen demand
T/F: In ED, you must assume all angina is unstable until proven otherwise
True
Which type of angina:
Involves episodic pain lasting 5-15 minutes; provoked by exertion & relieved by rest or nitro
Stable angina
Which type of angina:
angina at rest or new-onset exertional angina; increasing frequency or duration or refractory to ntiro
Unstable angina
Pt w/ unstable angina have an inc risk for what?
adverse cardiac event (MI or death)
Which type of angina:
occurs primarily at rest, triggered by smoking, thought to be due to coronary vasospasm
Variant angina (Prinzmetal)
Which type of angina has ST segment elevation that is nearly impossible to differentiate from AMI?
Variant angina (Prinzmetal)
How might an elderly patient with ACS present?
only AMS
What is the preferred biomarker for diagnosis of ACS? (greatest sensitivity/specificity)
Troponin
*detectable after 2-6 hrs, lasts 14 days
CK-MB can also be used to detect an MI. How early does it appear?
detectable w/in 4 hr, peaks 18-24 hrs, subsides day 3 or 4
*level w/in reference range does NOT exclude MI
Which biomarker is the earliest detected (2hrs), and has the highest sensitivity for an MI, but poor specificity?
Myoglobin
What is a super sensitive troponin?
AKA Gen 5 -can detect the smallest of troponin leaks
What do you look for when analyzing a Super Sensitive Troponin?
change (delta) between 2 values
When should Troponins be drawn?
0, 1, and 3 hr
What are you looking for in labs w/ an MI?
CBC -anemia
CMP -K+ and Mag (correct levels if needed)
What pts should automatically get an EKG?
> 45 y/o and is experiencing any form of thoracoabdominal discomfort
What EKG results indicate high probability of MI?
ST elevation > 1 mm in 2 contiguous leads OR presence of new Q-waves
What EKG results that indicate intermediate probability of MI?
ST segment depression, T wave inversion, nonspecific ST-T wave changes
T/F: A normal EKG rules out cardiac event
False
What is the 1st diagnostic test when evaluating a patient with angina in the ED?
EKG
What is PCI used for?
establish coronary reperfusion -more effective than thrombolysis
door-to-ballon = 90 minutes
What is the empirical tx of suspected STEMI?
Morphine, O2, NTG, ASA (chewable)
(MONA)
What are the CI to NTG?
SBP < 90, HR < 60 or > 100, RV infarction, PDE5 inhibitor
How soon should be thrombolytic therapy be initiated for an MI?
30 minutes
(door-to-drug)
What are the preferred thrombolytics for MI?
streptokinase, alteplase, tenecteplase, reteplase
What should you give in addition to ASA & unfractionated heparin to pts with continuing ischemia & pts in whom PCI is planned?
Platelet glycoprotein IIb/IIIa-receptor antagonist
(Eptifibatide, Tirofiban, Abciximab)
What are absolute CI to thrombolytic therapy?
Hx of ICH
Hx of ischemic stroke within the last 3 months
Cerebral vascular malformation/intracranial malignancy
Aortic dissection
Bleeding diathesis/Active bleeding
Significant closed head trauma within the last 3 months
What BP med should be given in tx of MI within first 24 hours?
ACEIs → Captopril
(or ARB)
What is the HEART score used for?
tool to assess CP patients in the ED; evaluates risk of major adverse cardiac events
(higher score = greater 6 week risk)
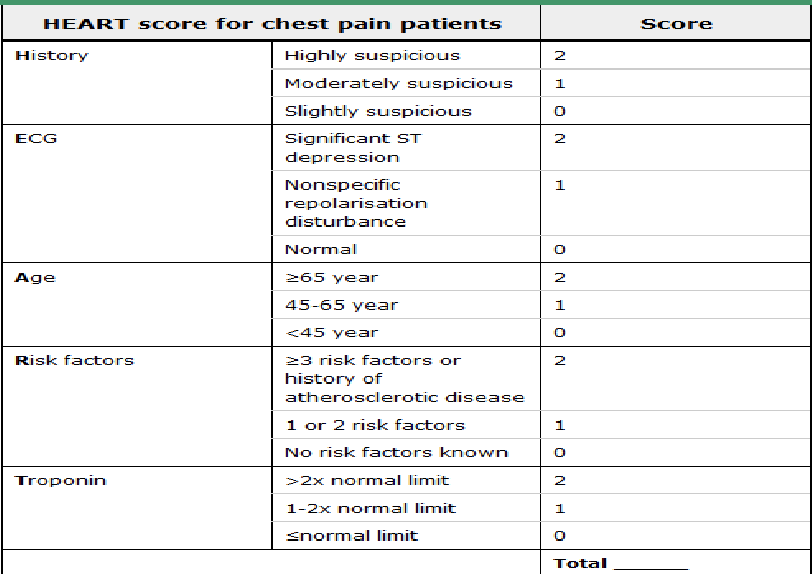
What are the categories of HEART score?
History, EKG, Age, Risk factors, Troponin
How were pts w/ a HEART score of 0-3 managed?
discharged
How were pts w/ a HEART score of 4-6 managed?
admitted to hospital
How were pts w/ a HEART score of > 7 managed?
candidates for early invasive measures
When should you get another EKG?
ANY change in sx
Total occlusion of the vessel for how long results in irreversible myocardial necrosis?
> 4-6 hours
What type of CHF is the MC form of ischemic heart disease and has a low EF (< 40%)?
Systolic
Which type of CHF has a normal or high EF?
Diastolic
How does isolated left sided HF present?
dyspnea, fatigue, weakness, cough, paroxysmal noctural dyspnea, orthopnea
How does isolated right sided HF present?
peripheral edema, JVD, RUQ pain
What causes high output HF?
anemia, thyrotoxicosis, large atrioventricular shunts, beriberi, Pagets
What are sx that are highly associated w/ CHF?
cough that produces pinky, frothy sputum, peripheral edema, JVD, and tachycardia
What is the diagnostic lab test for CHF?
BNP
When is BNP falsely elevated?
ESRD
What CXR findings indicate CHF?
cardiomegaly, Kerley B lines, pleural effusion, interstitial edema
What indicates successful management of BP & cardiac filling pressure in CHF?
marked improvement in respiratory status
-seen long before any significant diuresis
What analgesic should be avoided in treatment of CHF?
NSAIDs
(ASA is okay)
What is the 1st line tx for CHF?
Loop diuretic (Furosemide), Nitrates, ASA, Inotropic agents
Why is Digoxin not used for emergency management of CHF?
delayed absorption and diminished efficacy at times of inc sympathetic tone
Patients with hypotension presenting with CHF are treated w/ which inotropic agents?
Dopamine & Dobutamine
What murmurs warrant a cardio eval & Echo?
diastolic murmur or a new murmur with symptoms at rest
What is the MCC of mitral stenosis?
Rheumatic heart disease
How does mitral stenosis present?
exertional dyspnea, mid-diastolic rumbling crescendo murmur, followed by a loud opening snap
What is the tx of mitral stenosis?
Intermittent diuretics, tx afib, anticoagulation
What are common causes of mitral regurgitation?
MVP, MI, rheumatic heart disease, CAD, collagen-vascular disease
How does mitral regurgitation present?
dyspnea, high pitched holosystolic murmur, active apical impulse, thrill at the apex
What is the 1st sx of chronic mitral regurgitation?
Exertional dyspnea (afib)
What will be seen on CXR/EKG of mitral regurgitation?
LV & LA enlargement, LVH
What is the tx for asymptomatic mitral regurgitation?
None
What are sx of mitral valve prolapse?
atypical CP, palpitations, fatigue, exertional dyspnea, midsystolic click
± pectus excavatum, scoliosis, straight thoracic spine
What is the pt education for mitral valve prolapse?
avoid alcohol, tobacco, and caffeine, can give ASA (80-325mg)
What are common causes of aortic stenosis in adults?
degenerative heart disease, calcific aortic stenosis, rheumatic heart disease
What is the MCC of aortic stenosis in children?
congenital
What is the TRIAD of sx associated w/ aortic stenosis?
syncope, angina, dyspnea
How does aortic stenosis present?
harsh systolic ejection murmur, paradoxical splitting of S2, syncope in the setting of a new systolic murmur, pulse lag
What meds should be used with caution in patients with aortic stenosis?
Nitrates
What is the MCC of acute aortic regurgitation?
Infective endocarditis
*2nd = aortic dissection
What are sx of aortic regurgitation?
dyspnea, pink frothy sputum, systemic emboli, tachycardia
+ fever and chills (endocarditis)
+"tearing" CP that radiates btwn shoulder blades (dissection)
What is the tx for aortic regurgitation?
acute: O2, nitroprusside, dobutamine
chronic: vasodilators - ACEI or nifedipine
What are sx of dilated cardiomyopathy?
CHF symptoms
*sx dictate therapy
What are EKG findings with dilated cardiomyopathy?
LA & LV enlargement
What are sx of hypertrophic cardiomyopathy?
dyspnea on exertion, chest pain, palpitations, syncope, FH of cardiac death, sudden death in the young athlete
What is the tx for hypertrophic cardiomyopathy?
BB, avoid vigorous exercise
What are sx of restrictive cardiomyopathy?
CHF sx, S3, rales, JVD, Kussmaul, hepatomegaly, edema
What is the tx for restrictive cardiomyopathy?
Diuretics & ACEIs
*sarcoidosis → cortiosteroids
*hemochromatosis → chelation
What are sx of pericarditis?
sharp precordial or retrosternal CP, may radiate to the back or left arm, relieved when patient leans forward while sitting, pericardial friction rub
What are EKG findings of pericarditis?
diffuse ST elevation & PR depression
What is the initial test of choice for pericarditis?
TEE
What is the tx for pericarditis?
- No pericardial effusion: d/c
- Small/med pericardial effusion: admit & serial echos
- Large pericardial effusion: pericardiocentesis/pericardial window
What is the MCC of pericardial effusion?
malignancy
What is Beck's triad?
*assoc w/ tamponade
JVD, hypotension, muffled heart sounds
What is the testing is done for cardiac tamponade?
Echo = test of choice
EKG = electrical alternans (pathognomonic)
What is the tx for tamponade?
pericardiocentesis
What are common causes of restrictive pericarditis?
trauma, pericardiotomy, fungal or TB pericarditis, CRF
How does restrictive pericarditis present?
+JVD, Kussmaul sign, paradoxical pulse, pericardial "knock" at the apex, hepatomegaly, ascites, edema, chest pain, SOB, fatigue
What are EKG findings of restrictive pericarditis?
low-voltage QRS complexes, inverted T-waves
What is the tx for severe restrictive pericarditis?
Pericardiectomy
What is the classic presentation of a pulm embolism?
(doesn’t usually present like this)
abrupt pleuritic CP, SOB, hypoxia
What is Virchow's triad?
*for blood clots
hypercoagulability, endothelial damage, venous stasis
What is the gold standard test for pulmonary embolism?
Pulmonary CTA