heart and thorax 2026
1/78
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
79 Terms
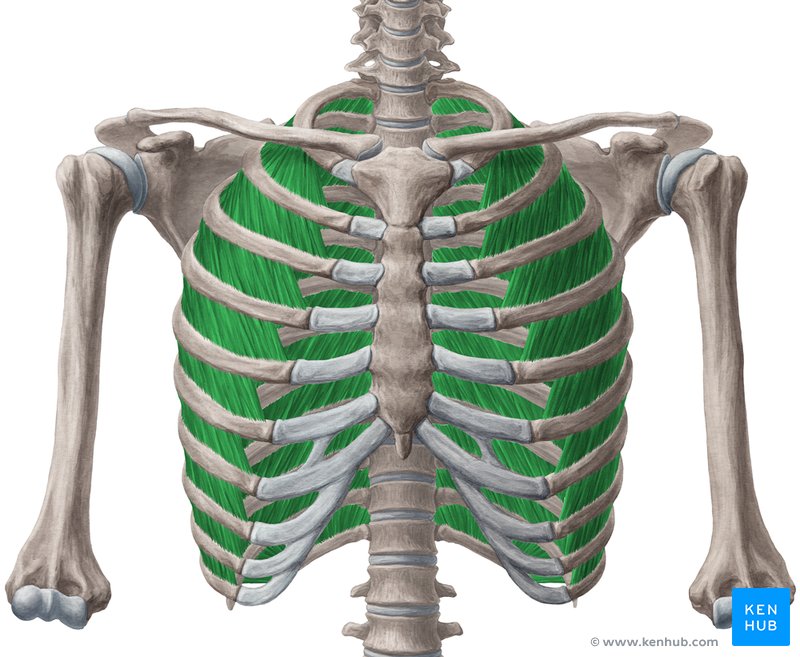
External Intercostals
Location: Between ribs, superficial intercostal layer
Layer/Compartment: Superficial layer of three intercostal muscle layers
Position: Superficial to internal intercostals; fibers run obliquely downward and anteriorly (hands in pockets direction)
Origin: Inferior border of rib above
Insertion: Superior border of rib below
Action: Elevate ribs (inspiration/inhalation); expand thoracic cavity
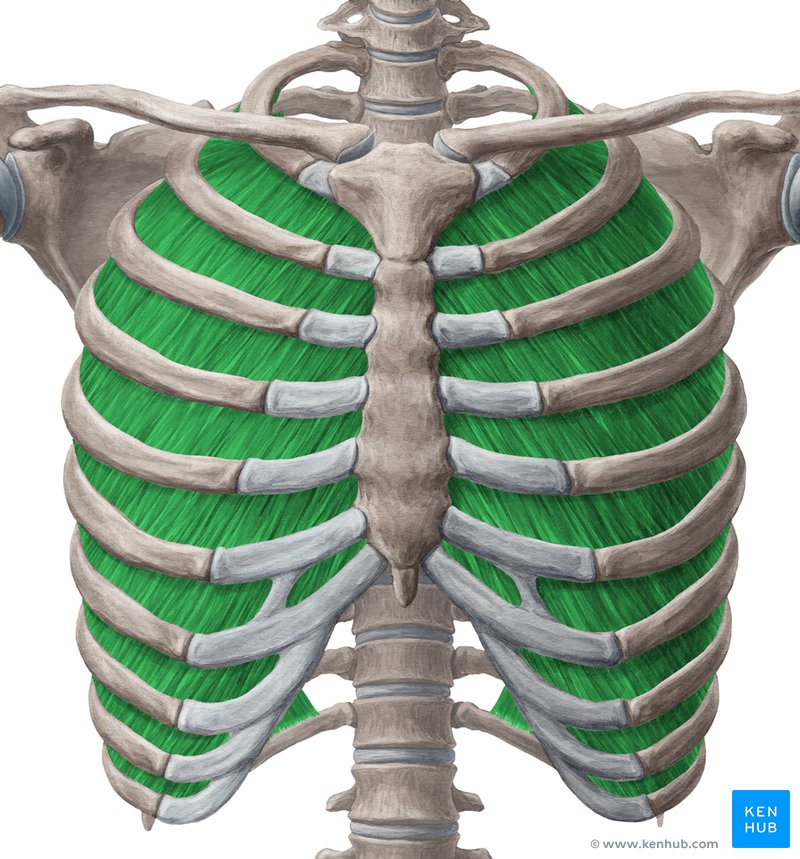
Internal Intercostals
Location: Between ribs, middle intercostal layer
Layer/Compartment: Middle layer of three intercostal muscle layers
Position: Deep to external intercostals, superficial to innermost intercostals; fibers run obliquely downward and posteriorly (perpendicular to external intercostals)
Origin: Superior border and costal groove of rib below
Insertion: Inferior border of rib above
Action: Depress ribs (forced expiration); decrease thoracic cavity volume
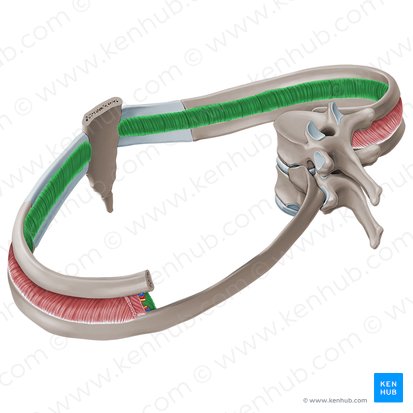
Innermost Intercostals
Location: Between ribs, deepest intercostal layer
Layer/Compartment: Deepest layer of three intercostal muscle layers
Position: Deep to internal intercostals; fibers run same direction as internal intercostals
Origin: Superior border of rib below
Insertion: Inferior border of rib above
Action: Depress ribs (forced expiration); assist internal intercostals
Note: Separated from internal intercostals by intercostal neurovascular bundle
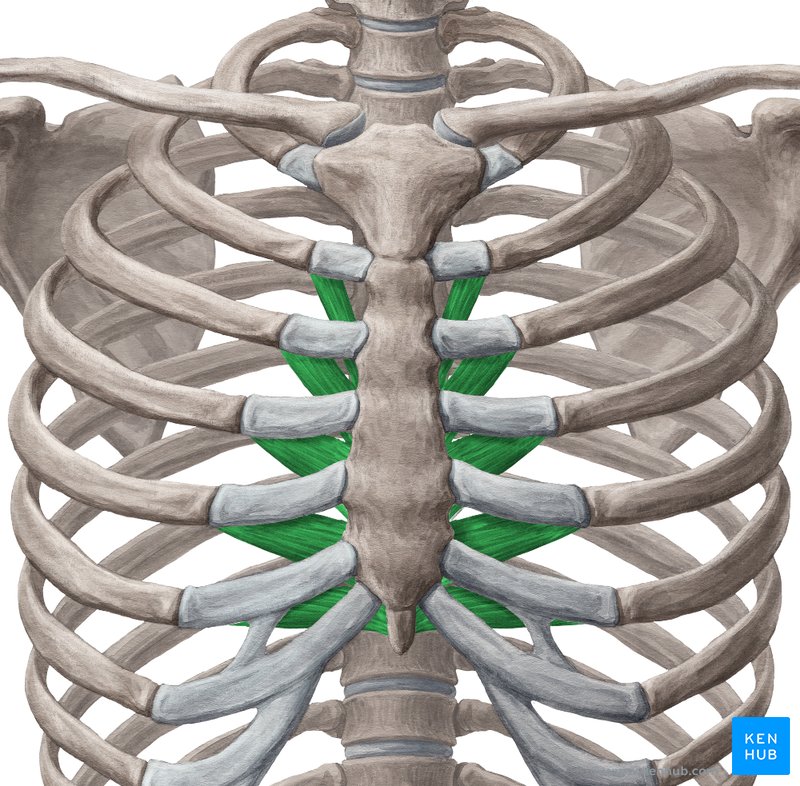
Transversus Thoracis
Location: Internal (deep) surface of anterior thoracic wall
Layer/Compartment: Deep to sternum and costal cartilages
Position: Posterior surface of sternum and costal cartilages; continuous with transversus abdominis
Origin: Posterior surface of xiphoid process and body of sternum
Insertion: Internal surfaces of costal cartilages 2-6
Action: Weakly depresses ribs (assists forced expiration)
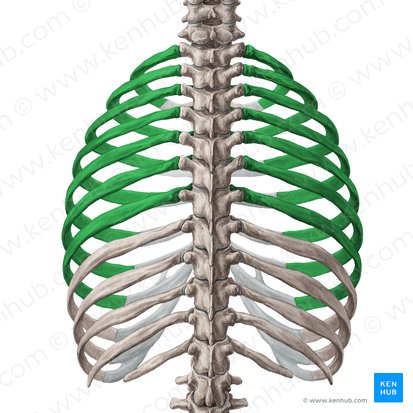
True ribs (1-7): Attach directly to sternum via own costal cartilage
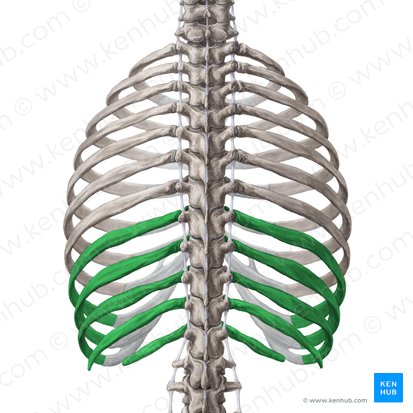
False ribs (8-10): Attach indirectly to sternum (costal cartilages join cartilage of rib 7)
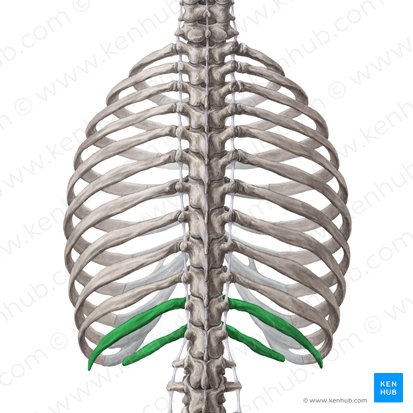
Floating ribs (11-12): No anterior attachment to sternum

Head (of Rib)
Location: Posterior medial end of rib
Function: Articulates with vertebral bodies (superior and inferior costal facets)
Articulations: Usually articulates with two adjacent vertebral bodies and intervertebral disc

Neck (of Rib)
Location: Short section between head and tubercle
Function: Connects head to tubercle; narrow region

Tubercle (of Rib)
Location: Posterior aspect of rib, at junction of neck and body
Function: Articulates with transverse process of corresponding vertebra (transverse costal facet)
Parts: Articular part (smooth facet) and non-articular part (roughened, for ligament attachment)

Body (Shaft of Rib)
Location: Main curved portion of rib
Function: Forms thoracic cage wall; protects thoracic organs
Features: Costal groove on inferior internal surface (houses intercostal neurovascular bundle); angle of rib (where rib curves anteriorly)
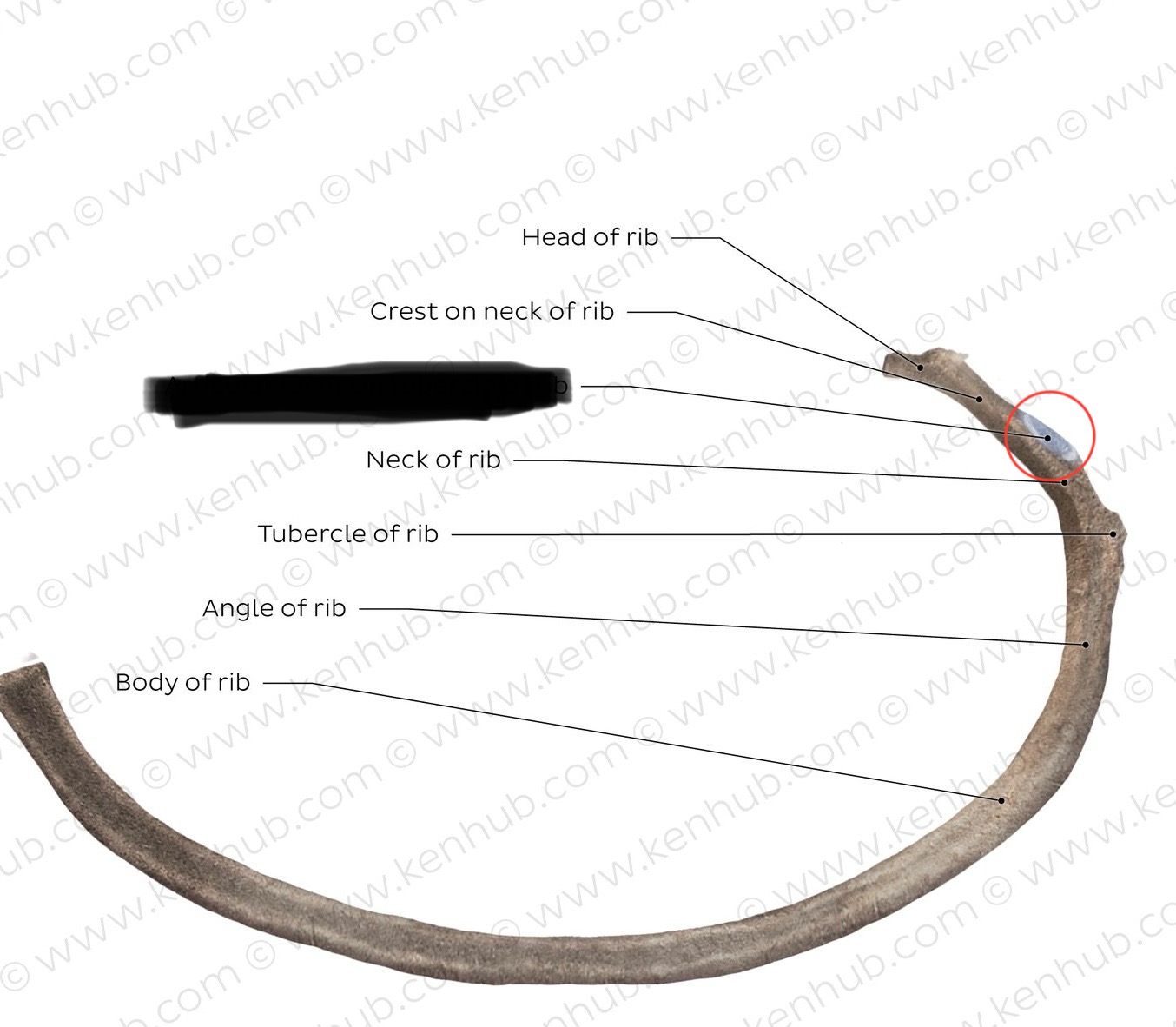
Facets (of Rib)
Location: On head and tubercle of rib
Function: Articular surfaces for vertebral articulations
Head facets: Superior and inferior facets articulate with vertebral bodies
Tubercle facet: Articulates with transverse process
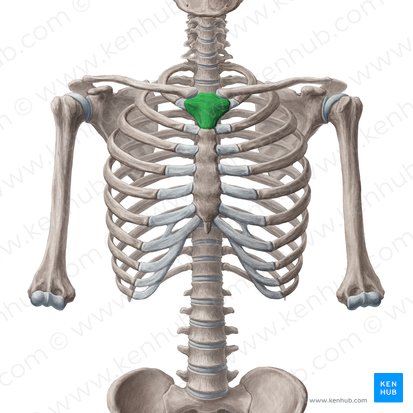
Manubrium
Location: Superior portion of sternum
Function: Articulates with clavicles (sternoclavicular joints) and first two ribs
Features: Jugular notch (superior), clavicular notches (lateral), facets for ribs 1-2
Landmark: Sternal angle (manubriosternal joint with body, at rib 2 level - T4-T5 vertebral level)
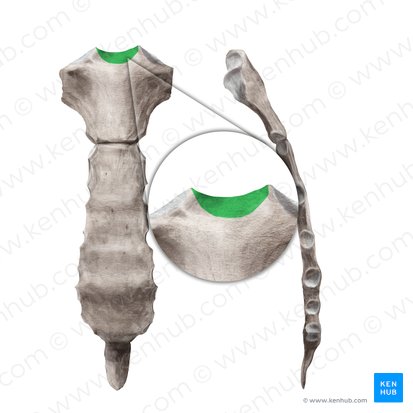
Jugular Notch (Suprasternal Notch)
Location: Superior border of manubrium, midline
Function: Palpable landmark; U-shaped depression
Clinical: Palpable at base of neck
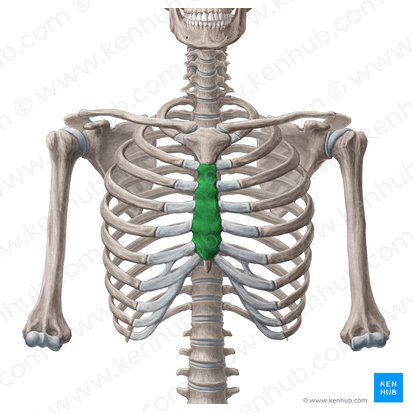
Body (of Sternum)
Location: Middle and largest portion of sternum
Function: Articulates with ribs 2-7 via costal cartilages
Features: Facets for costal cartilages along lateral borders
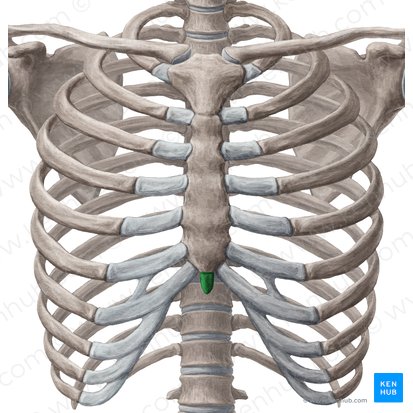
Xiphoid Process
Location: Inferior tip of sternum
Function: Attachment point for diaphragm and abdominal muscles
Features: Variable shape (pointed, bifid, or perforated); ossifies late in life
Clinical: Landmark for CPR hand placement (avoid pressing directly on xiphoid)
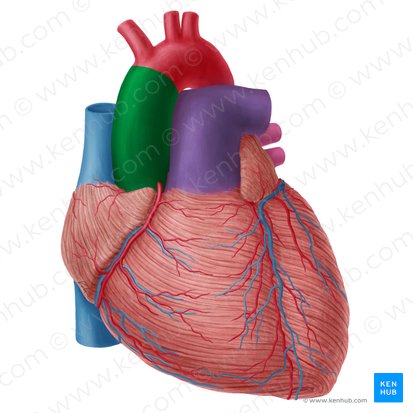
Ascending Aorta
Location: Begins at left ventricle, ascends in middle mediastinum
Course: Ascends 5cm from aortic valve to aortic arch
Region Supplied: Heart via coronary arteries (right and left coronary arteries branch from ascending aorta immediately above aortic valve)
Contained within: Pericardial sac
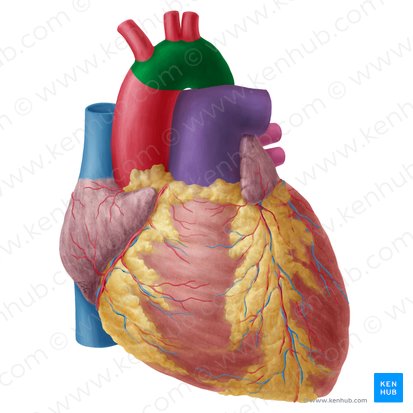
Aortic Arch
Location: Superior mediastinum, arches over left main bronchus
Course: Curves posteriorly and to left, becomes descending aorta at T4-T5
Branches (anterior to posterior): Brachiocephalic artery, left common carotid artery, left subclavian artery
Region Supplied: Head, neck, upper limbs via branches
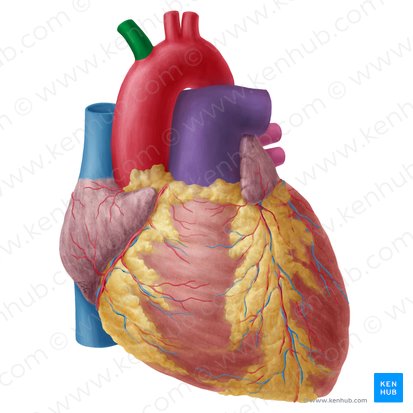
Brachiocephalic Artery
Location: First branch of aortic arch (right side only)
Course: Ascends right, divides into right common carotid and right subclavian
Region Supplied: Right side of head, neck, right upper limb
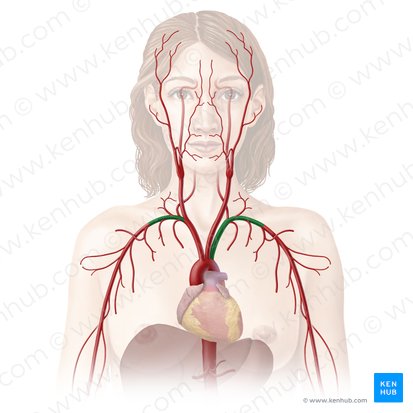
Subclavian Arteries
Location: Base of neck, arches over first rib
Right: Branches from brachiocephalic artery
Left: Branches directly from aortic arch (third branch)
Region Supplied: Upper limb, brain (via vertebral artery)
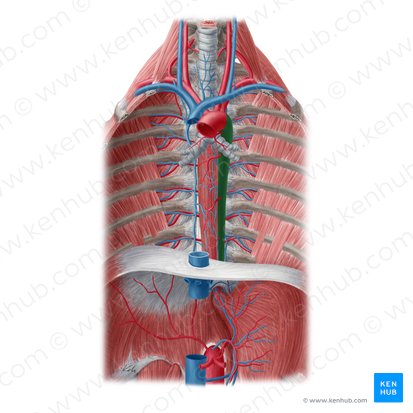
Descending Thoracic Aorta
Location: Posterior mediastinum, left of midline
Course: Descends from T4-T5 to T12, passes through diaphragm (becomes abdominal aorta)
Branches: Posterior intercostal arteries (pairs 3-11), bronchial arteries, esophageal arteries, pericardial branches
Region Supplied: Thoracic wall, esophagus, bronchi, pericardium
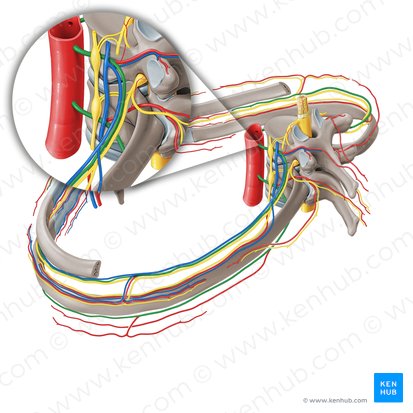
Posterior Intercostal Arteries
Location: Run along inferior border of ribs in costal grooves
Origin: Pairs 1-2 from supreme intercostal artery (from subclavian); Pairs 3-11 from descending thoracic aorta
Course: Run with intercostal vein (superior) and intercostal nerve (inferior) in costal groove - "VAN" arrangement
Region Supplied: Intercostal muscles, thoracic wall, spinal cord (via spinal branches)
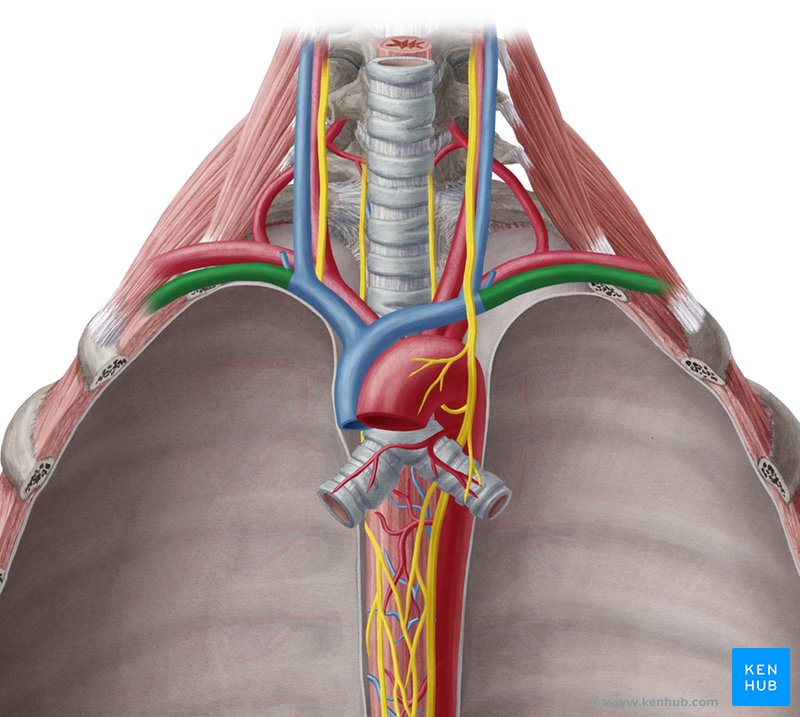
Subclavian Veins
Location: Anterior to subclavian artery, anterior to anterior scalene muscle
Course: Continuation of axillary vein; joins internal jugular vein to form brachiocephalic vein
Region Drained: Upper limb
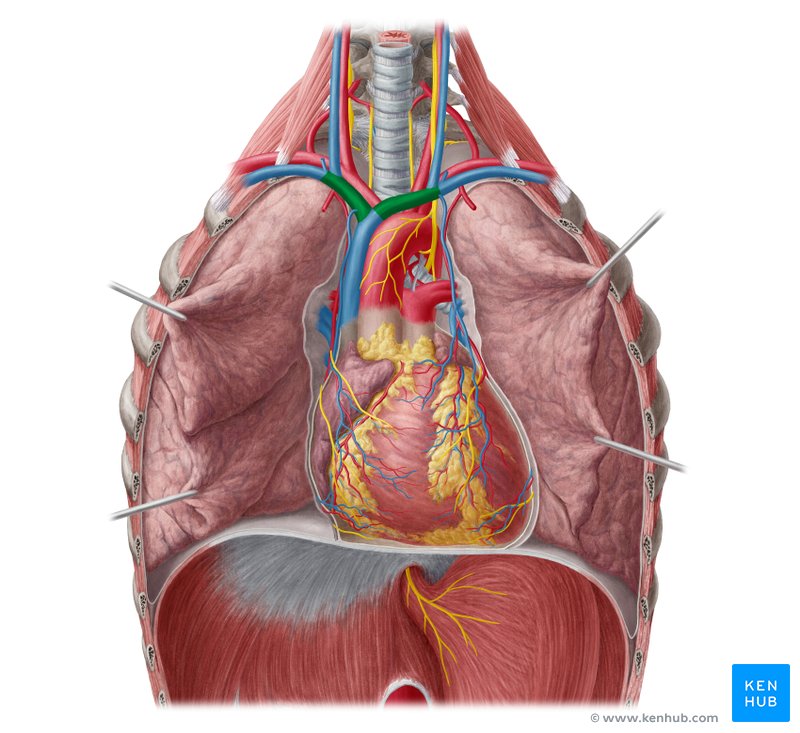
Brachiocephalic Veins
Location: Superior mediastinum
Course: Left and right brachiocephalic veins (formed by junction of subclavian and internal jugular veins) unite to form superior vena cava
Right brachiocephalic: Short and vertical
Left brachiocephalic: Longer, crosses midline anterior to aortic arch branches
Region Drained: Head, neck, upper limbs
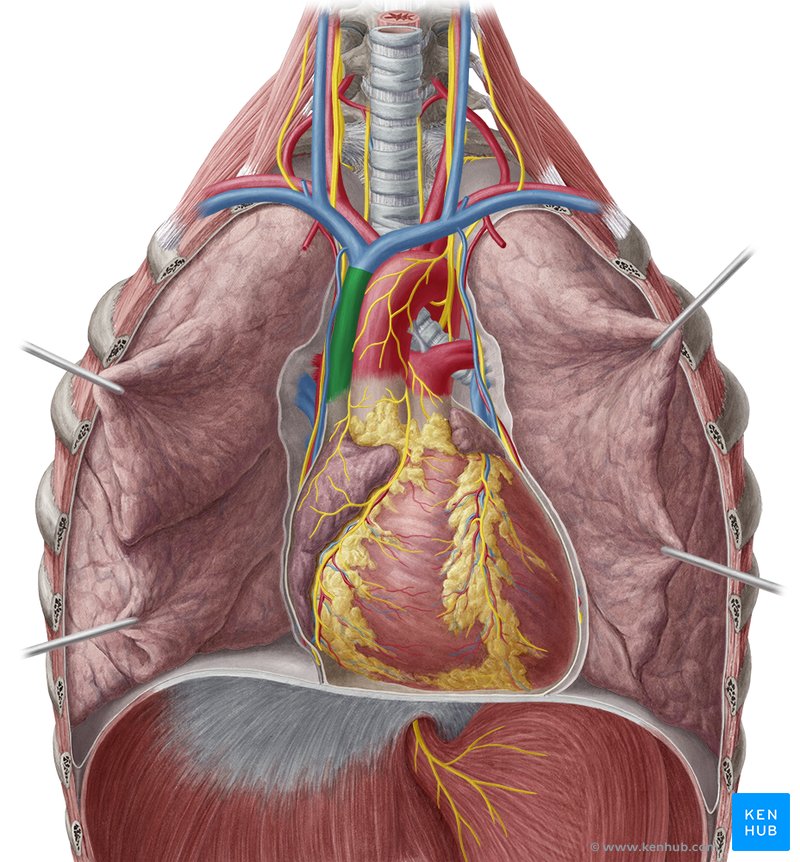
Superior Vena Cava
Location: Superior and middle mediastinum, right side
Course: Formed by union of left and right brachiocephalic veins; descends and enters right atrium
Region Drained: All structures above diaphragm (head, neck, upper limbs, thoracic wall)
Tributaries: Azygos vein (enters posteriorly)
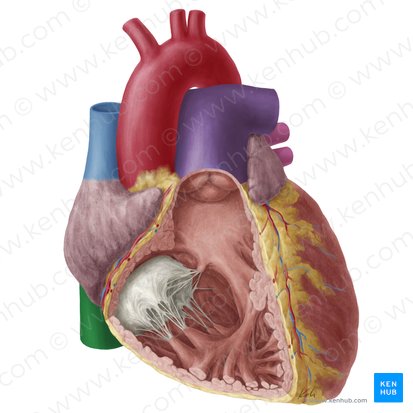
Inferior Vena Cava
Location: Passes through diaphragm at T8 level; brief course in middle mediastinum
Course: Ascends through abdomen, pierces diaphragm, immediately enters right atrium
Region Drained: All structures below diaphragm (abdomen, pelvis, lower limbs)
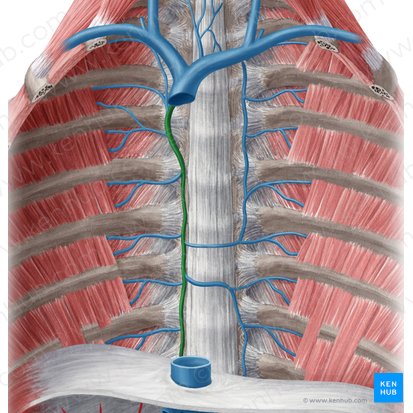
Azygos Vein
Location: Posterior mediastinum, right of vertebral column
Course: Ascends right side of vertebral column; arches over right main bronchus to enter SVC
Tributaries: Right posterior intercostal veins, hemiazygos vein, accessory hemiazygos vein, esophageal veins, bronchial veins
Region Drained: Thoracic wall, mediastinal structures
Function: Provides collateral circulation between SVC and IVC systems
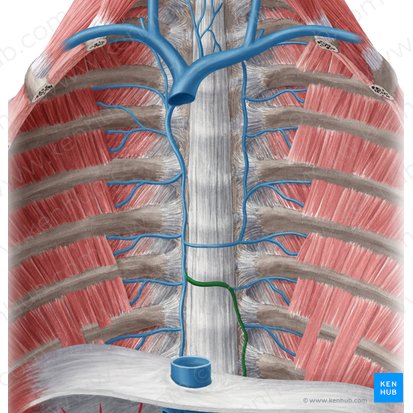
Hemiazygos Vein
Location: Posterior mediastinum, left of vertebral column (lower half)
Course: Ascends left side (T9-T12 level); crosses midline at T8-T9 to drain into azygos vein
Tributaries: Lower left posterior intercostal veins (9-11), left subcostal vein
Region Drained: Lower left thoracic wall
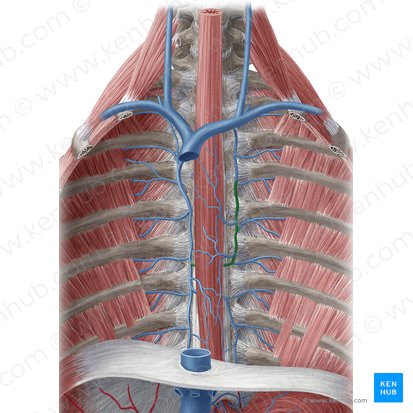
Accessory Hemiazygos Vein
Location: Posterior mediastinum, left of vertebral column (upper half)
Course: Descends left side (T5-T8 level); crosses midline to drain into azygos vein
Tributaries: Upper left posterior intercostal veins (4-8), left bronchial veins
Region Drained: Upper left thoracic wall
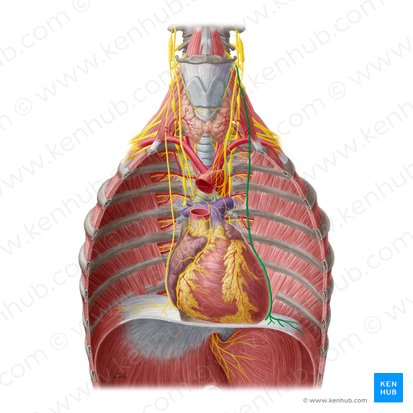
Phrenic Nerve
Location: Anterior mediastinum and middle mediastinum
Origin: C3, C4, C5 nerve roots ("C3, 4, 5 keeps the diaphragm alive")
Course: Descends anterior to anterior scalene muscle in neck; enters thorax; descends along lateral pericardium (between pericardium and mediastinal pleura); passes through diaphragm
Function: Motor innervation to diaphragm (primary muscle of respiration); sensory to central diaphragm, pericardium, mediastinal pleura
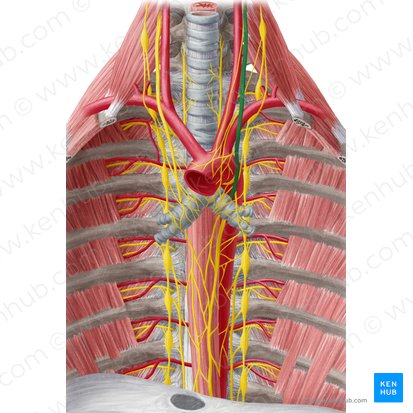
Vagus Nerve (CN X)
Location: Posterior mediastinum
Origin: Brainstem (medulla oblongata)
Course: Descends through neck in carotid sheath; enters thorax; right vagus passes posterior to root of right lung and along esophagus; left vagus passes anterior to aortic arch and along esophagus
Branches in thorax: Recurrent laryngeal nerves, cardiac branches, pulmonary branches, esophageal branches
Function: Parasympathetic innervation to heart (slows heart rate), lungs (bronchoconstriction), esophagus (peristalsis)
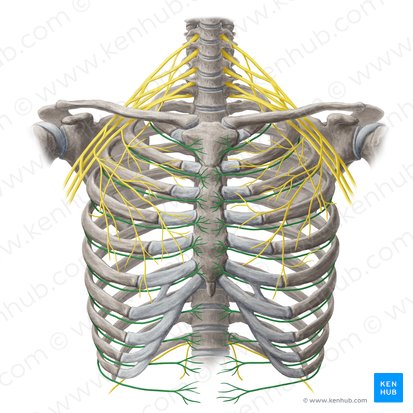
Intercostal Nerves
Location: Between ribs, in costal grooves
Origin: Ventral rami of thoracic spinal nerves T1-T11 (T12 is subcostal nerve)
Course: Run in costal groove with posterior intercostal artery and vein - "VAN" arrangement (Vein, Artery, Nerve from superior to inferior)
Function: Motor to intercostal muscles; sensory to thoracic and abdominal wall skin (dermatomal distribution)

Primary Bronchi
Location: Middle mediastinum
Course: Right and left primary bronchi branch from trachea at carina (T4-T5)
Right primary bronchus: Wider, shorter, more vertical (foreign objects more likely to enter right side)
Left primary bronchus: Narrower, longer, more horizontal (passes under aortic arch)
Function: Conduct air from trachea to lungs; each bronchus enters lung
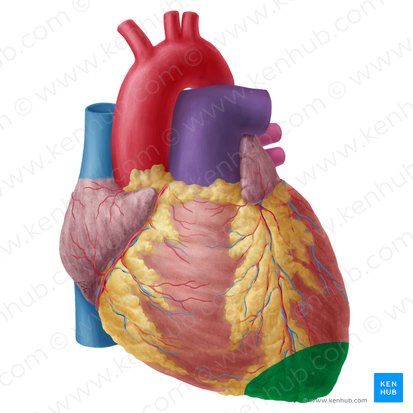
Apex (heart)
Location: Inferior, left, anterior tip of heart
Position: Points downward, anteriorly, and to the left; typically at 5th intercostal space, left midclavicular line
Formed by: Left ventricle
Function: Where apical impulse (heartbeat) can be palpated
Clinical: "Point of maximal impulse" (PMI)
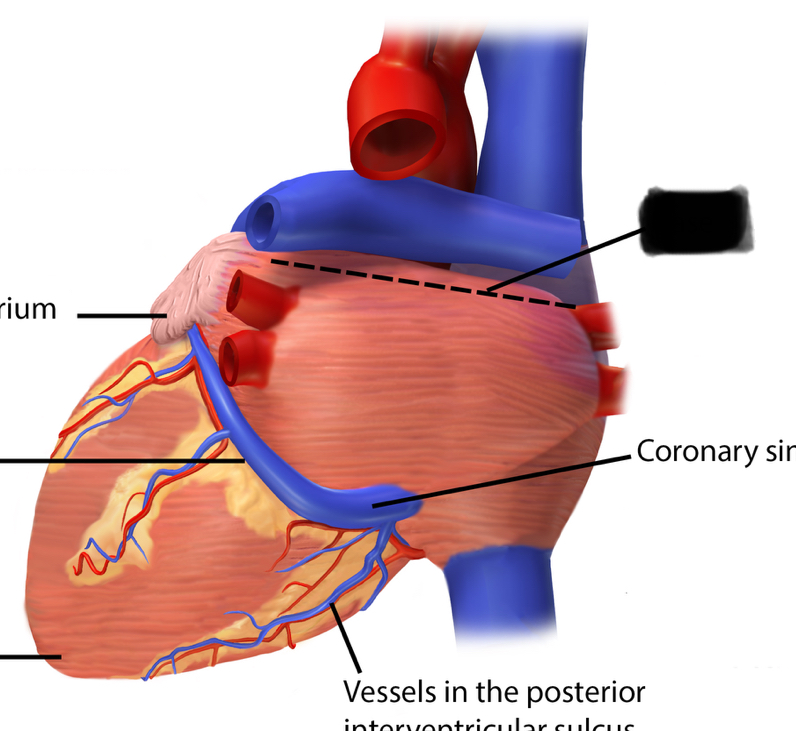
Base
Location: Posterior, superior surface of heart
Position: Opposite the apex; directed posteriorly and superiorly
Formed by: Mainly left atrium, with some contribution from right atrium
Function: Where great vessels enter and exit heart
Note: Base is NOT the inferior surface (common misconception)
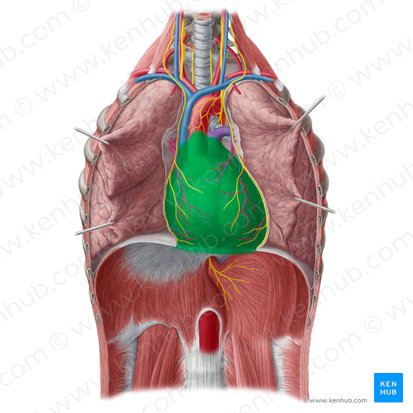
Pericardium
Location: Surrounds heart and roots of great vessels
Function: Protects heart, prevents overdistension, anchors heart in mediastinum, reduces friction
Layers: Fibrous pericardium (outer tough layer), serous pericardium (inner, divided into parietal and visceral layers)
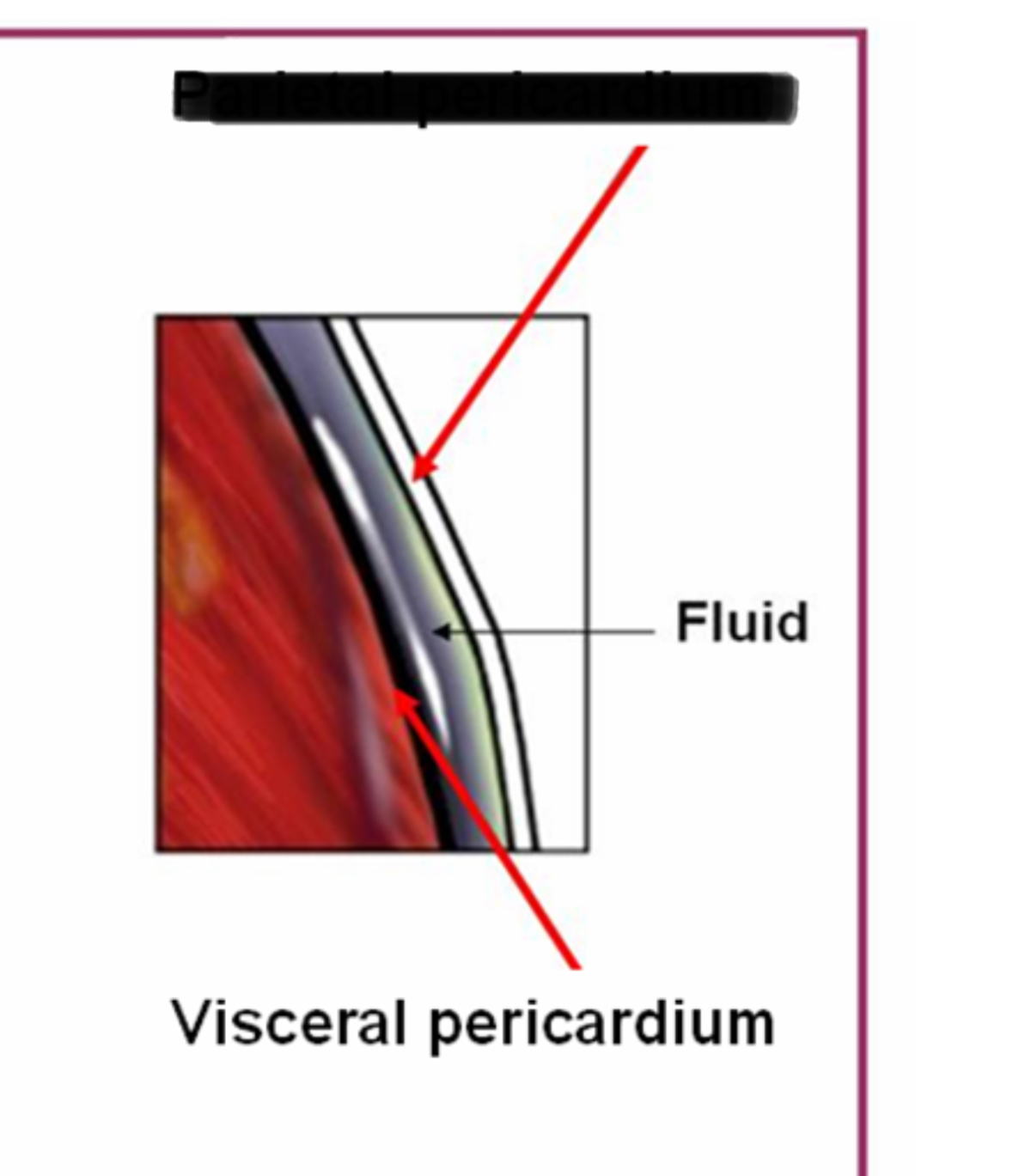
Parietal Pericardium
Location: Inner layer of fibrous pericardium
Position: Lines inner surface of fibrous pericardium
Function: Secretes pericardial fluid into pericardial cavity
Continuous with: Visceral pericardium (epicardium) at reflection points around great vessels
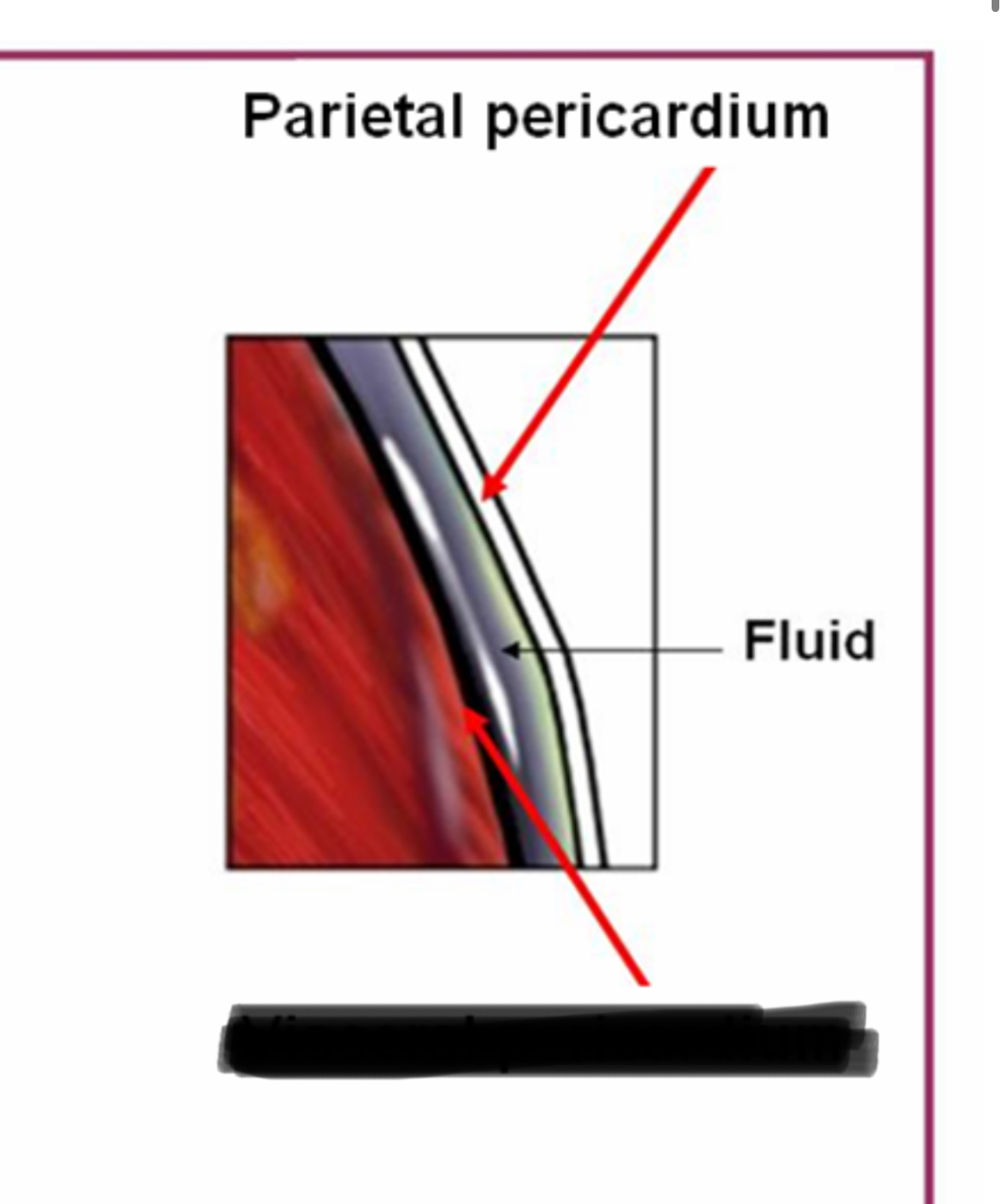
Visceral Pericardium (Epicardium)
Location: Outer layer of heart wall, adheres directly to myocardium
Position: Innermost layer of serous pericardium
Function: Secretes pericardial fluid; outer layer of heart wall
Continuous with: Parietal pericardium at great vessel roots
Pericardial Cavity: Potential space between parietal and visceral pericardium containing small amount (~15-50mL) of pericardial fluid for lubrication

Myocardium
Location: Middle layer of heart wall
Position: Between epicardium (outer) and endocardium (inner)
Structure: Cardiac muscle tissue; thickest in left ventricle, thinner in atria
Function: Contracts to pump blood; generates force for circulation
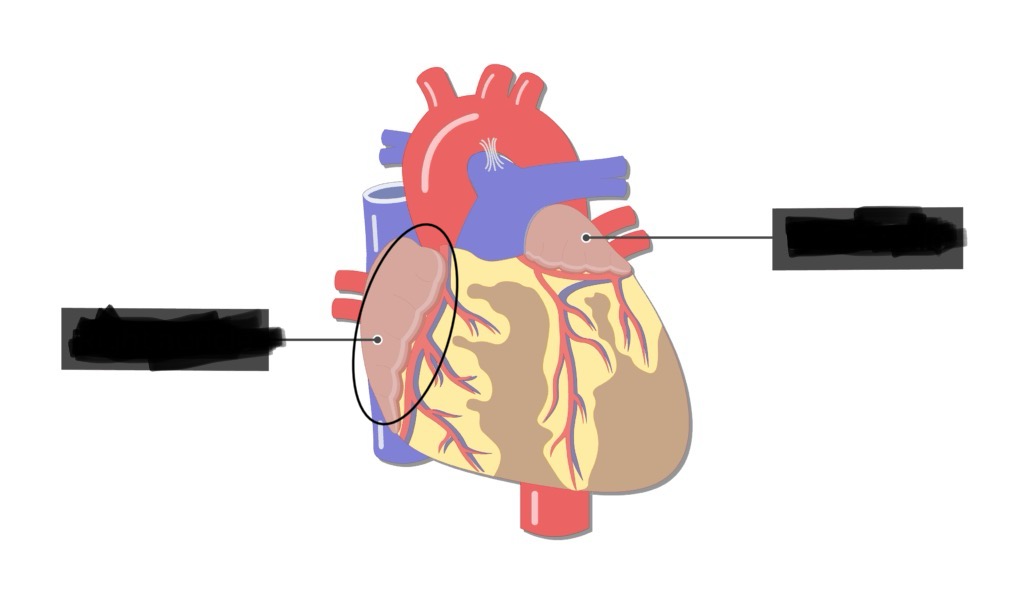
Right Atrial Auricle (Right Atrial Appendage)
Location: Small pouch-like extension of right atrium
Position: Projects anteriorly from right atrium; wraps around aortic root
Function: Increases atrial volume; contains pectinate muscles
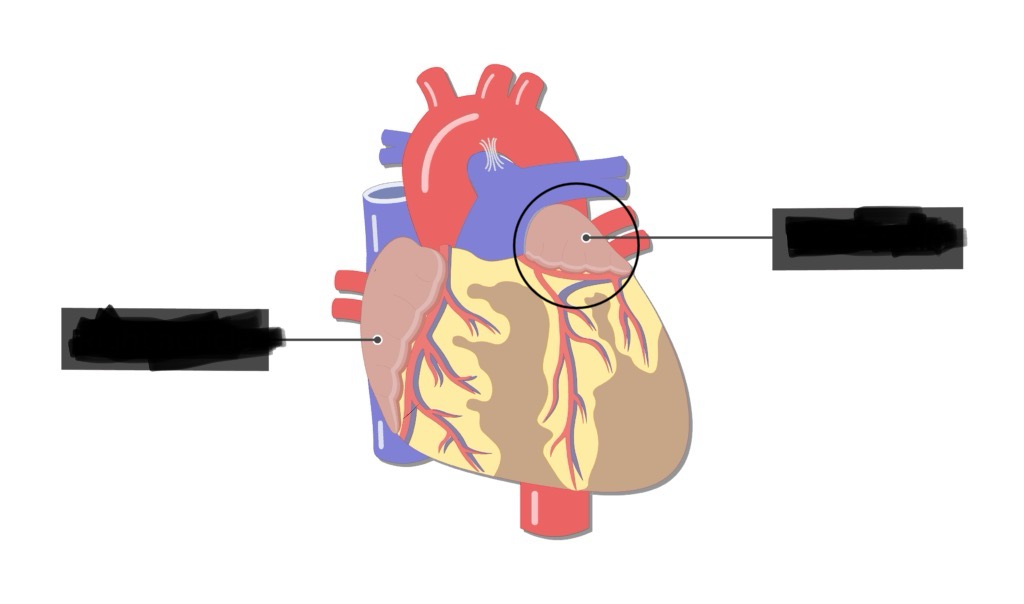
Left Atrial Auricle (Left Atrial Appendage)
Location: Small pouch-like extension of left atrium
Position: Projects anteriorly from left atrium; lateral to pulmonary trunk
Function: Increases atrial volume; contains pectinate muscles
Clinical: Common site of thrombus formation in atrial fibrillation
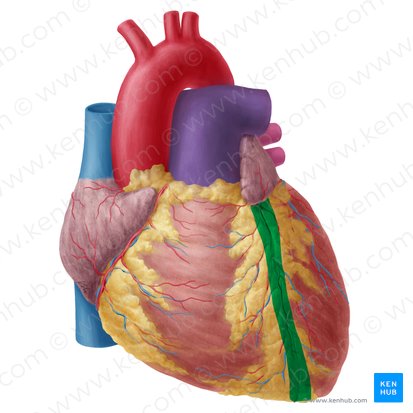
Anterior Interventricular Sulcus
Location: Groove on anterior surface of heart between right and left ventricles
Position: Runs from coronary sulcus (atrioventricular groove) toward apex
Function: External landmark indicating position of interventricular septum
Contains: Left anterior descending artery (LAD), great cardiac vein, fat
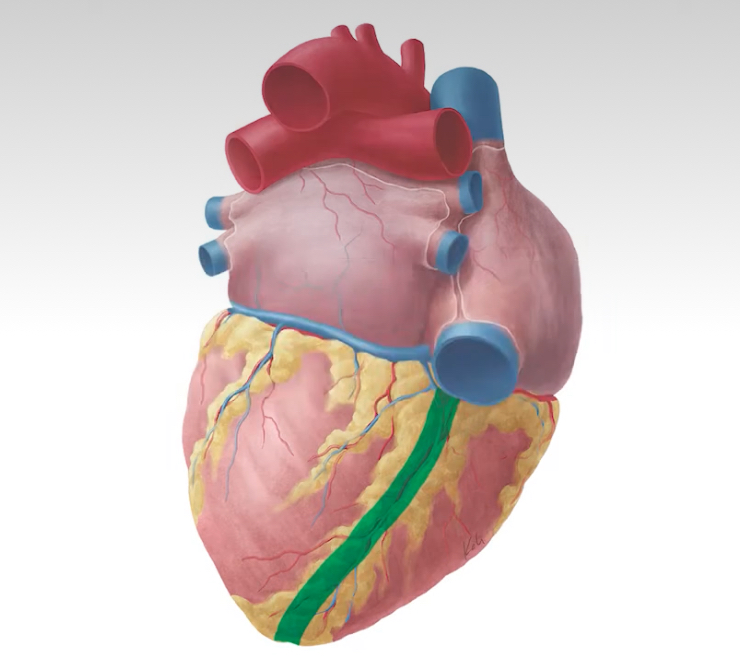
Posterior Interventricular Sulcus
Location: Groove on posterior (diaphragmatic) surface of heart between ventricles
Position: Runs from coronary sulcus toward apex on posterior surface
Function: External landmark indicating position of interventricular septum
Contains: Posterior descending artery (PDA), middle cardiac vein, fat
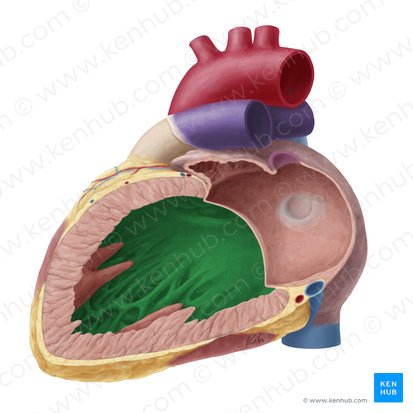
Interventricular Septum
Location: Wall separating left and right ventricles
Position: Runs between ventricles from base to apex
Parts: Muscular portion (thick, inferior 2/3), membranous portion (thin, superior 1/3)
Function: Prevents mixing of oxygenated and deoxygenated blood
Contains: AV node and bundle of His in membranous portion (part of conduction system)
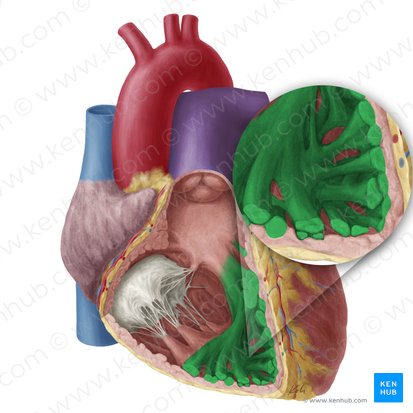
Trabeculae Carneae
Location: Inner surface of ventricles
Position: Irregular muscular ridges projecting into ventricular chambers
Function: Increase surface area; prevent suction effect during contraction; assist in ventricular contraction
Note: More prominent in ventricles than in atria
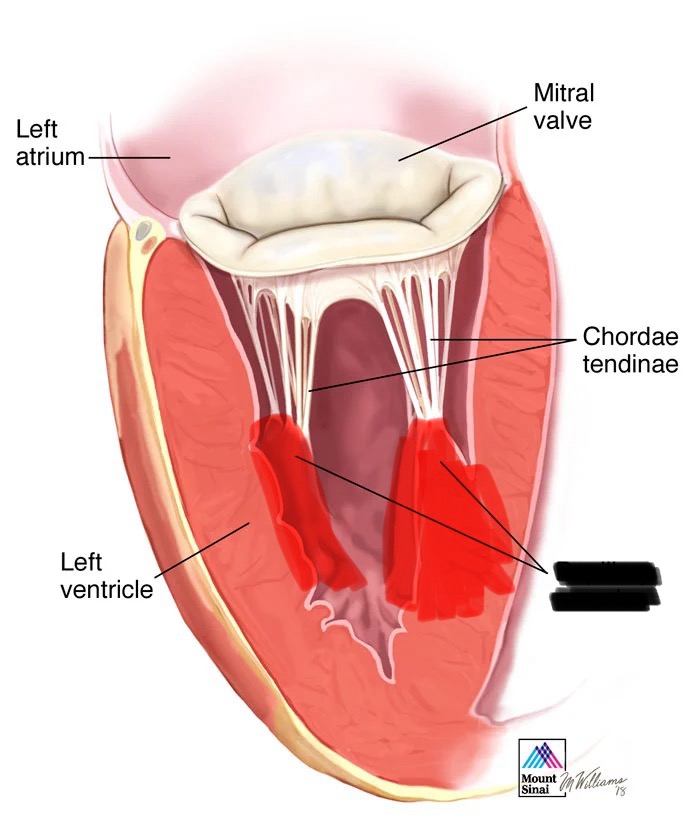
Papillary Muscles
Location: Project from ventricular walls (anterior, posterior, septal)
Position: Arise from ventricular myocardium; project into ventricular cavities
Function: Anchor chordae tendineae; contract during systole to prevent valve prolapse
Location specifics: Right ventricle has 3 (anterior, posterior, septal); left ventricle has 2 (anterior, posterior)
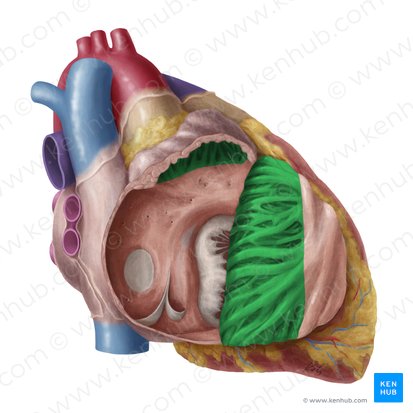
Pectinate Muscles
Location: Interior of atria (especially atrial auricles)
Position: Parallel muscular ridges in atrial walls
Function: Increase atrial contractility; increase surface area
Extent: Separated from smooth posterior atrial wall by crista terminalis (right atrium)
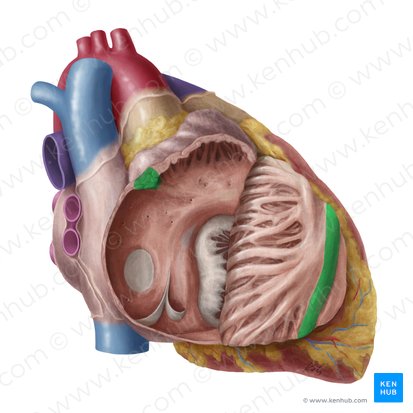
Crista Terminalis
Location: Right atrium
Position: Vertical muscular ridge on internal surface; separates rough anterior portion (pectinate muscles) from smooth posterior portion
Function: Landmark; embryological junction; contains sinoatrial (SA) node at superior end
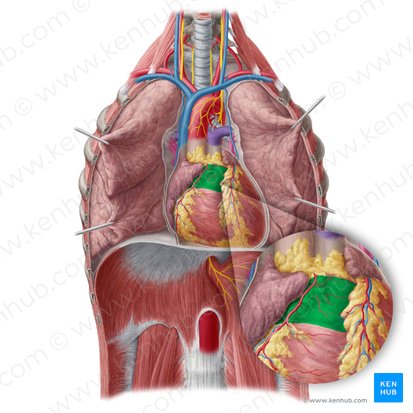
Conus Arteriosus (Infundibulum)
Location: Superior portion of right ventricle
Position: Smooth-walled outflow tract leading to pulmonary valve and pulmonary trunk
Function: Funnel-shaped region directing blood from right ventricle to pulmonary trunk
Note: Smooth-walled (no trabeculae) unlike rest of right ventricle
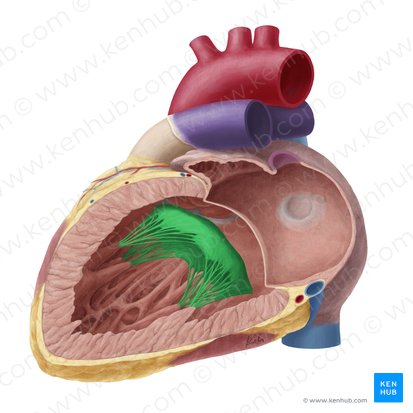
Mitral Valve (Bicuspid Valve)
Location: Between left atrium and left ventricle
Structure: Two cusps/leaflets (anterior and posterior)
Function: Prevents backflow of blood from left ventricle to left atrium during systole
Attachments: Chordae tendineae connect cusps to papillary muscles
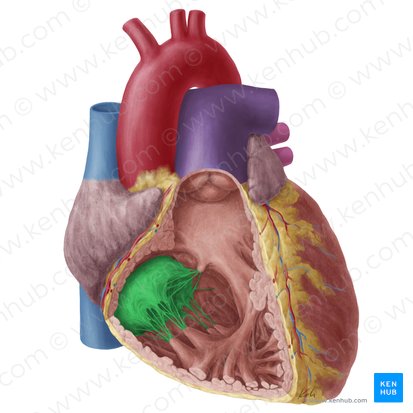
Tricuspid Valve
Location: Between right atrium and right ventricle
Structure: Three cusps/leaflets (anterior, posterior, septal)
Function: Prevents backflow of blood from right ventricle to right atrium during systole
Attachments: Chordae tendineae connect cusps to papillary muscles
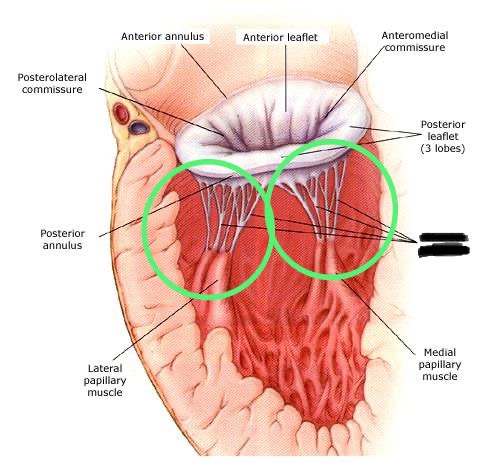
Chordae Tendineae
Location: Attach valve cusps to papillary muscles
Structure: Fibrous cords ("heart strings")
Function: Prevent valve leaflets from prolapsing (everting) into atria during ventricular contraction
Action: Papillary muscles contract → tension on chordae → hold valve leaflets in place
Valve Flap (Leaflet)
Location: Mobile portions of valves
Structure: Thin fibrous tissue covered by endocardium
Function: Opens to allow blood flow, closes to prevent backflow
Valve Cusps
Location: Individual leaflets of valves
Function: Mitral has 2 cusps; tricuspid has 3 cusps; semilunar valves have 3 cusps each
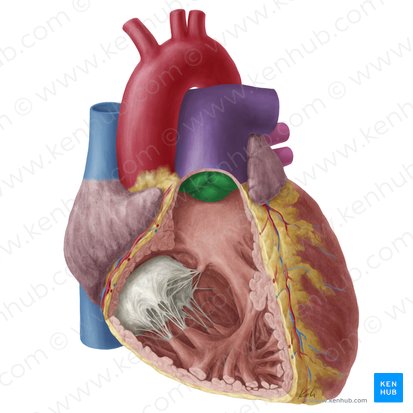
Pulmonary Valve
Location: Between right ventricle (conus arteriosus) and pulmonary trunk
Structure: Three semilunar cusps (left, right, anterior)
Function: Prevents backflow from pulmonary trunk to right ventricle during diastole
Action: Opens during ventricular systole; closes during ventricular diastole
Note: No chordae tendineae or papillary muscles (unlike AV valves)
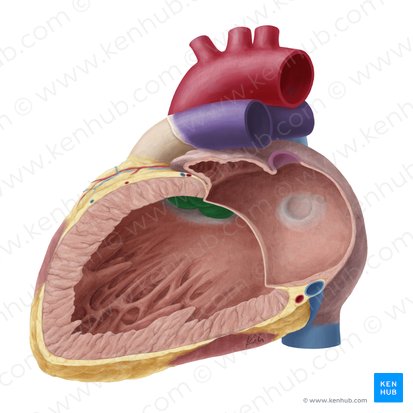
Aortic Valve
Location: Between left ventricle and ascending aorta
Structure: Three semilunar cusps (left, right, posterior/non-coronary)
Function: Prevents backflow from aorta to left ventricle during diastole
Action: Opens during ventricular systole; closes during ventricular diastole
Special feature: Coronary artery ostia (openings) located immediately above left and right cusps (coronary arteries fill during diastole)
Ostia to Coronary Arteries
Location: In aortic sinuses (dilations in ascending aorta immediately above aortic valve cusps)
Position: Left coronary ostium above left aortic cusp; right coronary ostium above right aortic cusp
Function: Openings where coronary arteries originate from ascending aorta
Filling: Coronary arteries fill during diastole (when aortic valve is closed and aortic pressure is higher)
Right Coronary Artery (RCA)
Location: Originates from right aortic sinus
Course: Descends in right atrioventricular (coronary) sulcus; wraps around to posterior surface
Branches: Right marginal artery, posterior descending artery (PDA) in 70% of people (right-dominant), SA nodal artery (60%), AV nodal artery
Supplies: Right atrium, right ventricle, inferior wall of left ventricle, SA node (usually), AV node (usually)
Left Coronary Artery (LCA)
Location: Originates from left aortic sinus
Course: Short main stem (1-2cm); bifurcates into LAD and circumflex
Branches: Left anterior descending (LAD), left circumflex
Supplies: Most of left ventricle, interventricular septum, left atrium
Left Circumflex Artery
Location: Branch of left coronary artery
Course: Continues in left atrioventricular sulcus; wraps around to posterior surface
Branches: Left marginal artery, posterior descending artery (in 10% - left dominant)
Supplies: Left atrium, lateral and posterior walls of left ventricle, SA node (40%)
Left Anterior Descending Artery (LAD / Anterior Interventricular Artery)
Location: Branch of left coronary artery
Course: Descends in anterior interventricular sulcus toward apex
Branches: Diagonal branches, septal perforating branches
Supplies: Anterior wall of left ventricle, most of interventricular septum, apex
Clinical: "Widowmaker" — most critical coronary artery; occlusion causes massive anterior MI
Posterior Descending Artery (PDA / Posterior Interventricular Artery)
Location: Usually branch of RCA (70% right-dominant), sometimes from circumflex (10% left-dominant), or both (20% co-dominant)
Course: Descends in posterior interventricular sulcus toward apex
Supplies: Posterior interventricular septum, inferior walls of both ventricles
Coronary Sinus
Location: Posterior atrioventricular sulcus (coronary sulcus) on posterior surface
Course: Runs in coronary sulcus; drains into right atrium (between IVC and tricuspid valve)
Tributaries: Great cardiac vein, middle cardiac vein, small cardiac vein, posterior vein of left ventricle, oblique vein of left atrium
Function: Main venous drainage of heart (collects ~75% of cardiac venous blood)
Great Cardiac Vein
Location: Accompanies LAD in anterior interventricular sulcus
Course: Ascends in anterior interventricular sulcus; turns left in coronary sulcus; continues as coronary sinus
Drains: Anterior left ventricle, interventricular septum, left atrium
Small Cardiac Vein
Location: Accompanies right marginal artery
Course: Runs along right margin of heart; drains into coronary sinus
Drains: Right atrium, right ventricle
Middle Cardiac Vein
Location: Accompanies posterior descending artery in posterior interventricular sulcus
Course: Ascends in posterior interventricular sulcus toward base; drains into coronary sinus
Drains: Posterior walls of ventricles, posterior interventricular septum
Describe and trace the path/sequence of the circulatory loops from left ventricle back to left atrium