BY 202 Chapter 22 Willems
1/97
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
98 Terms
Male Reproductive System
What are the primary tissues/sex organs of males?
the testes
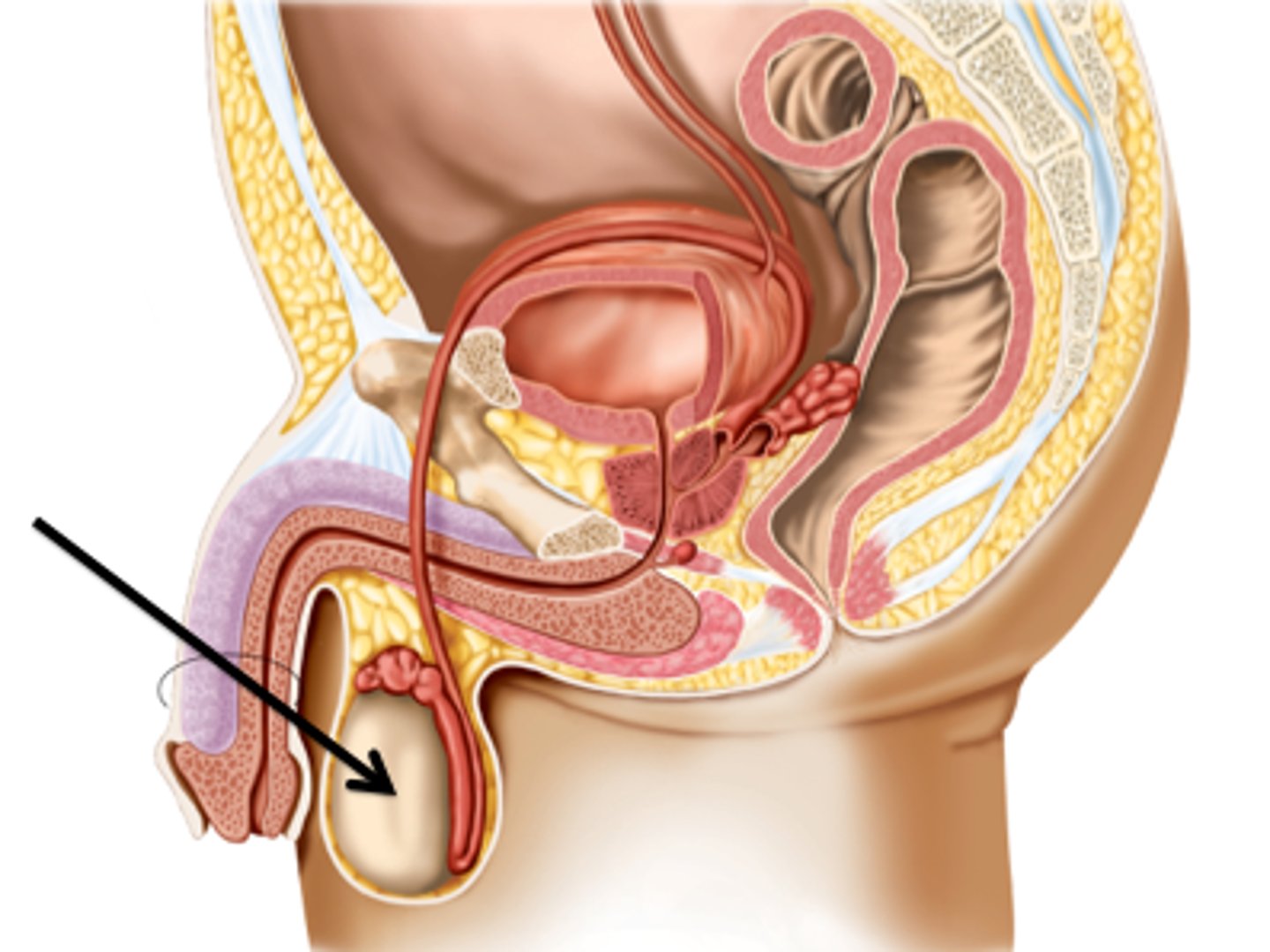
What do the testes produce?
-male gametes (sperm)
-androgens
Androgens stimulate the secretion of...
testerone
Androgens also promote secondary characteristics.
What are secondary characteristics?
-facial hair
-increase in connective tissues
-increase in RBC count
-thickening of larynx (deepening of voice)
-increased muscle mass; decreased fat
The testes are suspended and attached by the...
spermatic cord
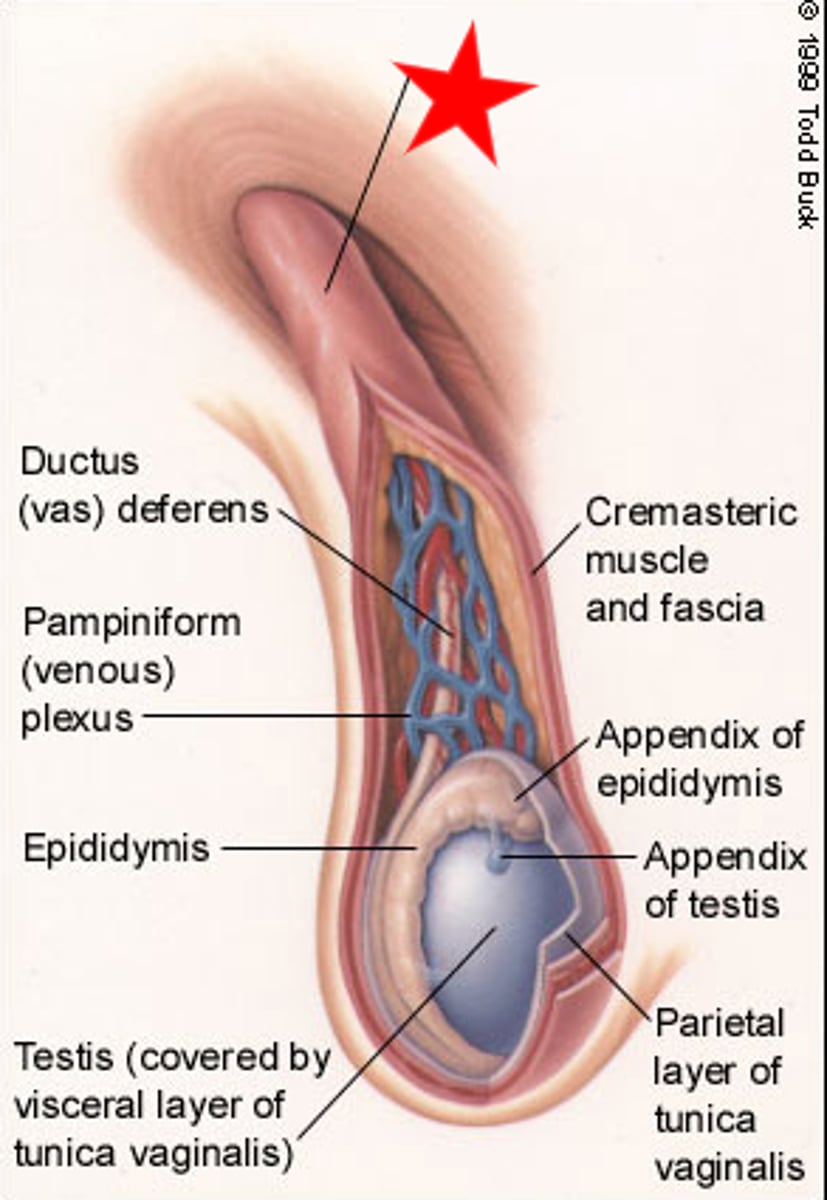
In a male fetus, the testes originate by the kidneys.
The testes must descend through the... canal of the abdominal wall to the scrotum.
inguinal canal
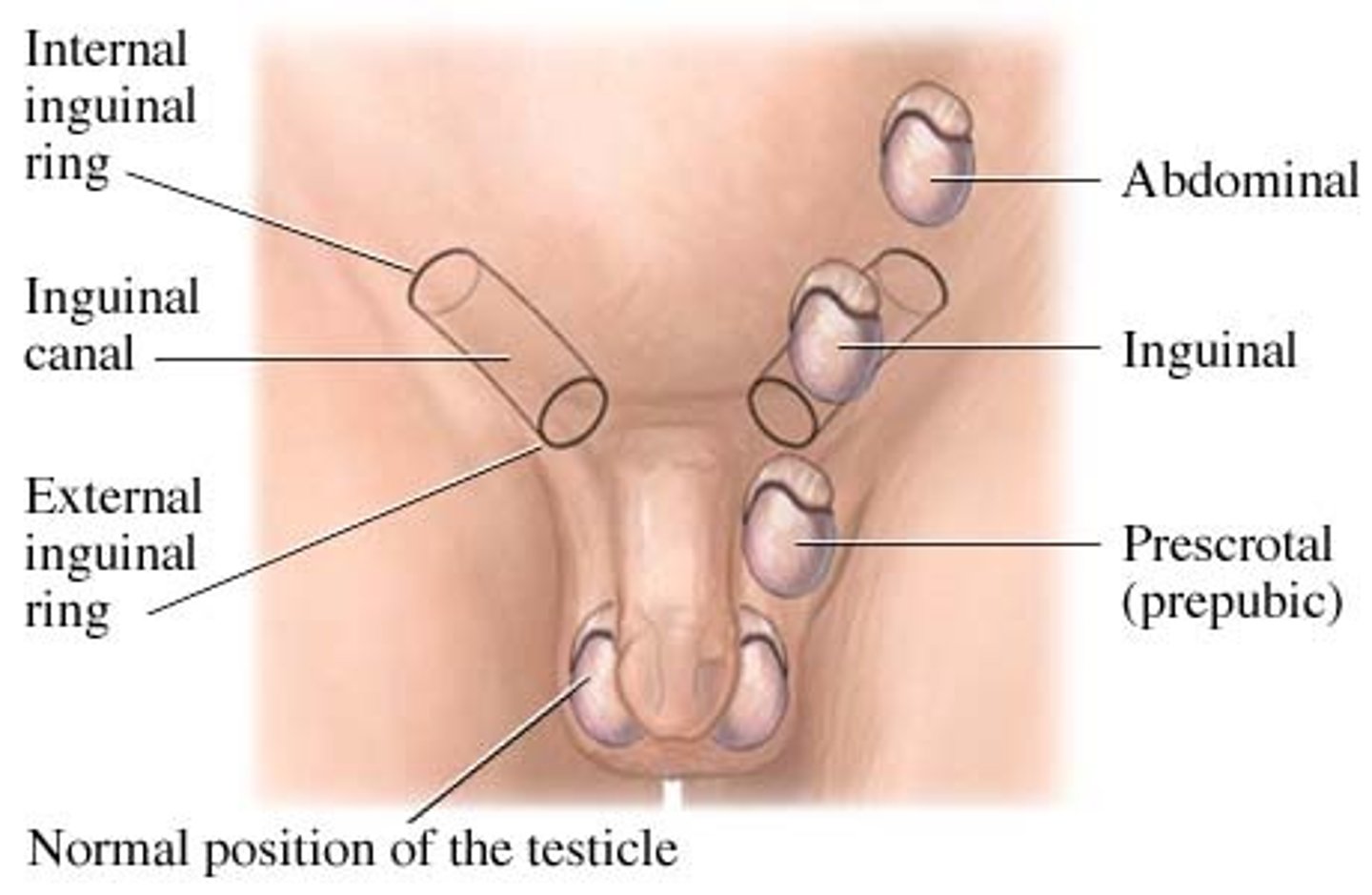
What is cryptorchidism (ch-k)?
the testes do not lower out of the body cavity
What were to happen if the testes did not descend and stay within the body cavity?
the temperature in the body cavity would be too high to produce sperm
*need to be around 20 C not 37 C
If the inguinal canal does not close, when happens?
the intestine can bulge through causing a hernia
*this is most frequent site for hernias in males
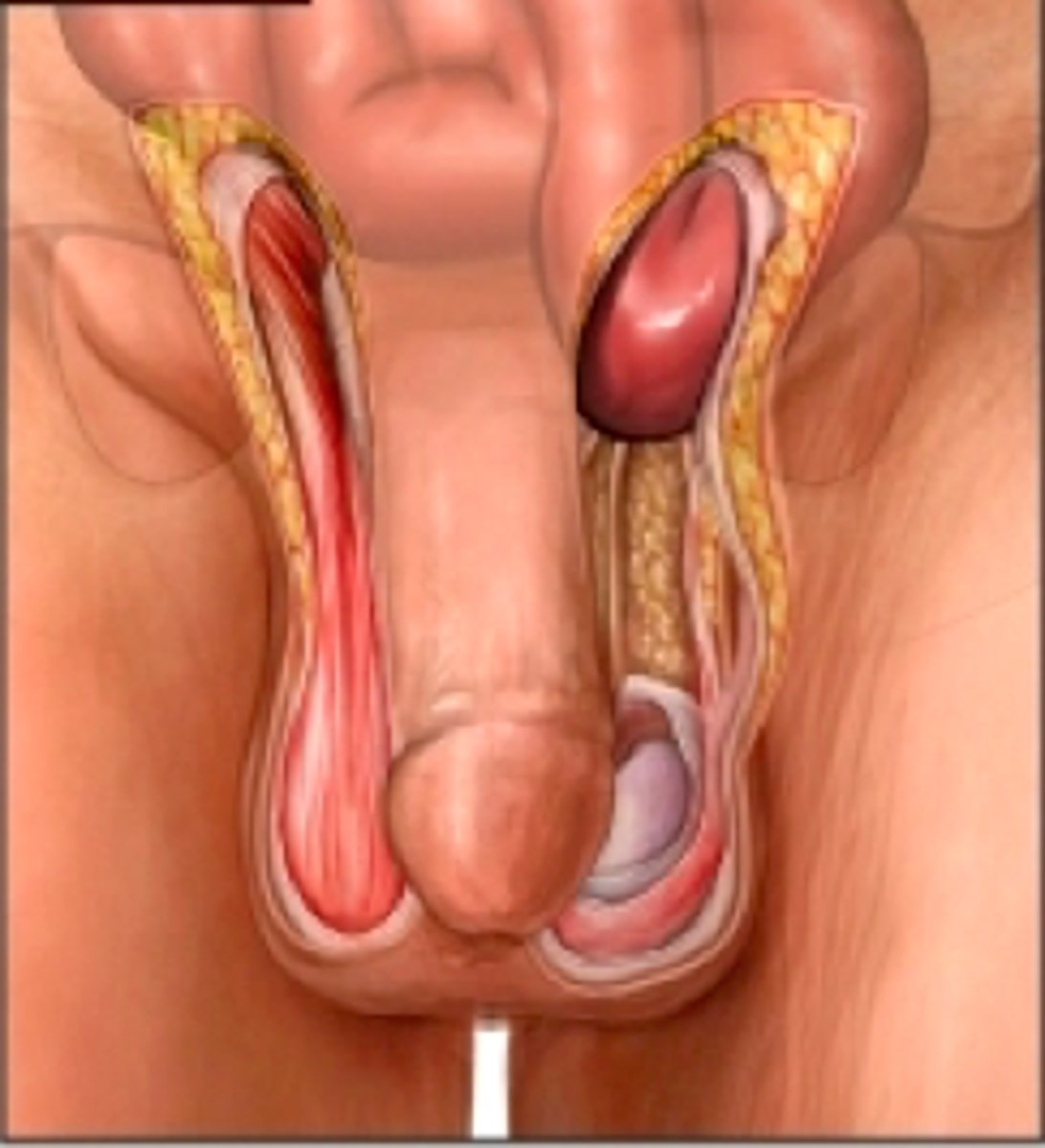
Within the testes are highly coiled tubules called...
seminiferous tubules
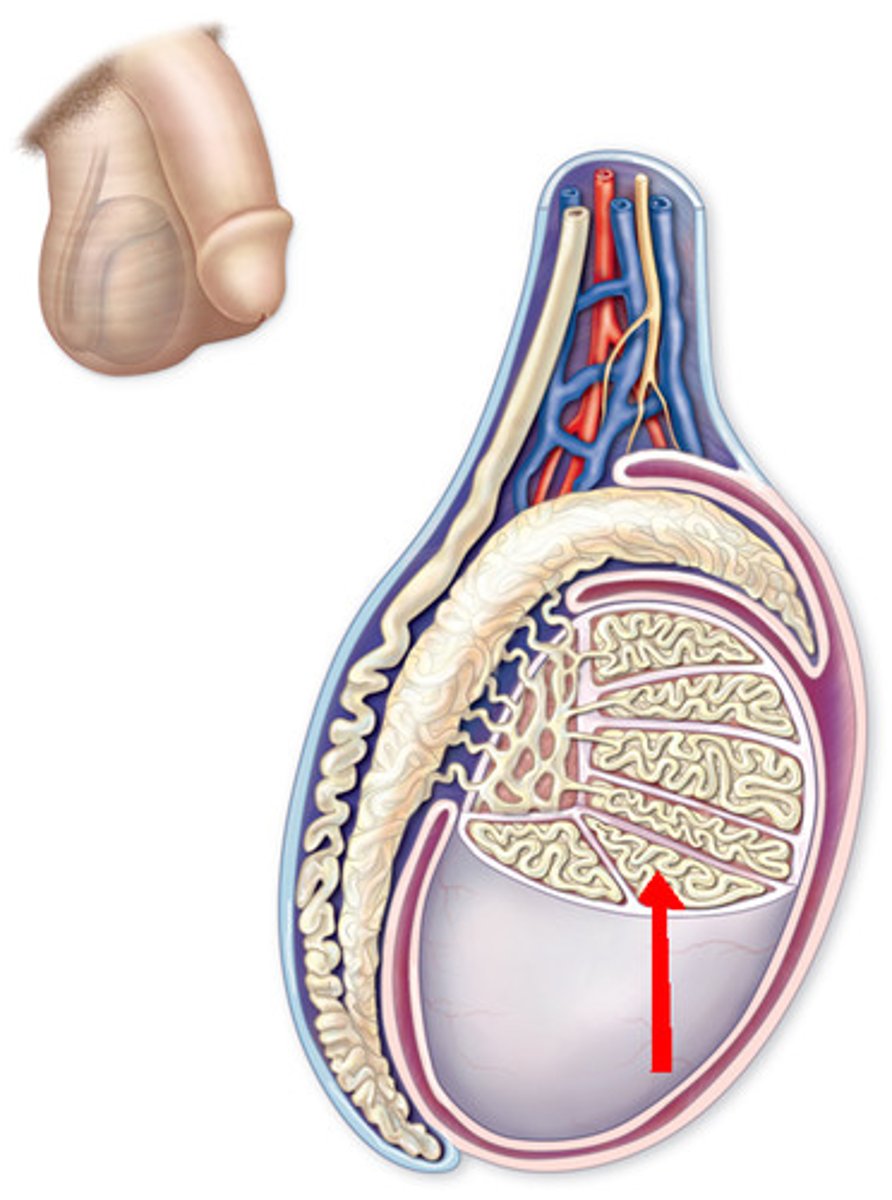
What type of cell is found between the seminiferous tubules?
interstitial (Leydig's) cells
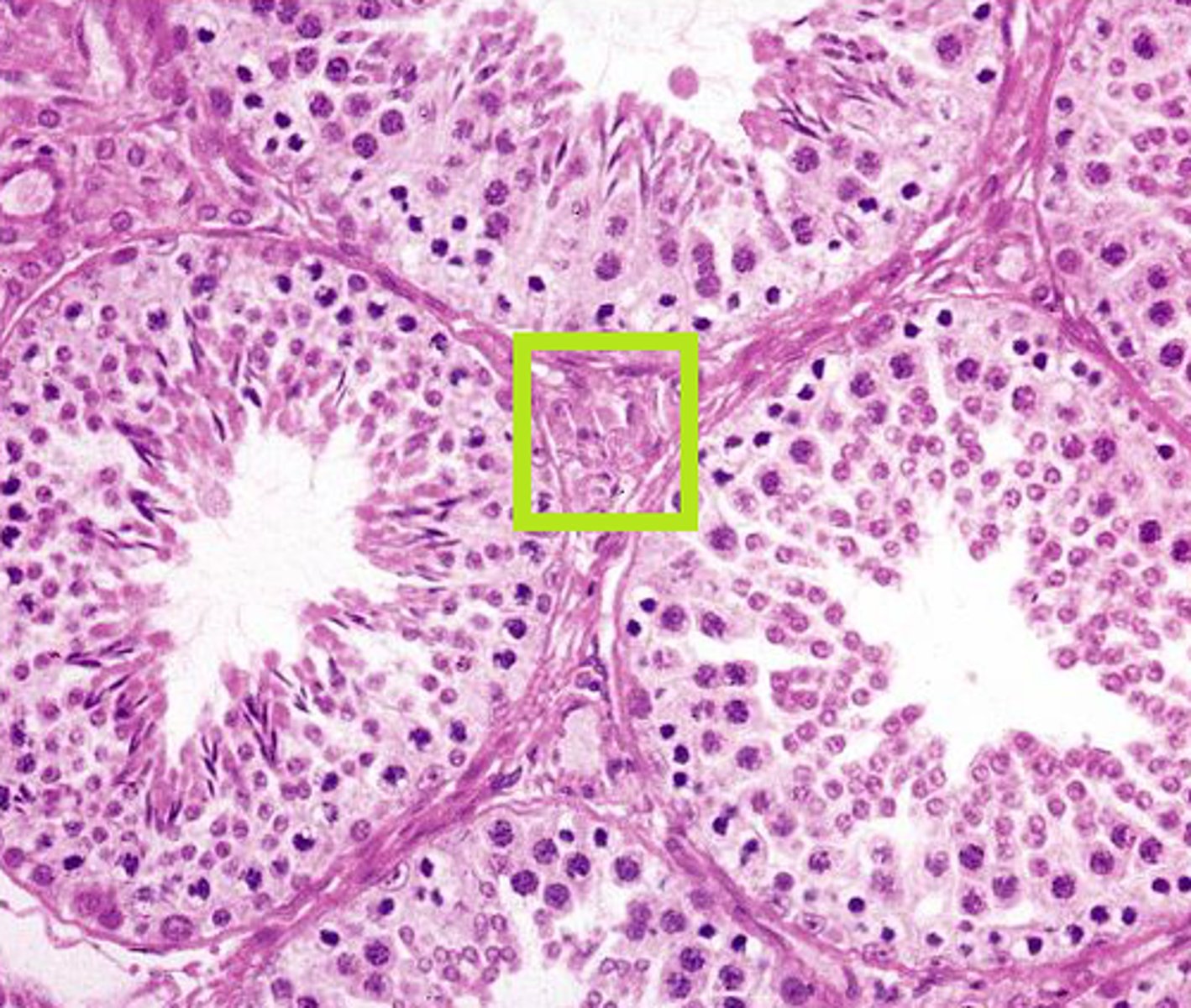
What is the purpose of interstitial (Leydig's) cells?
they produce testosterone
What type of cell is found primarily in the testicles that provides support?
sustentacular (sertoli) cells
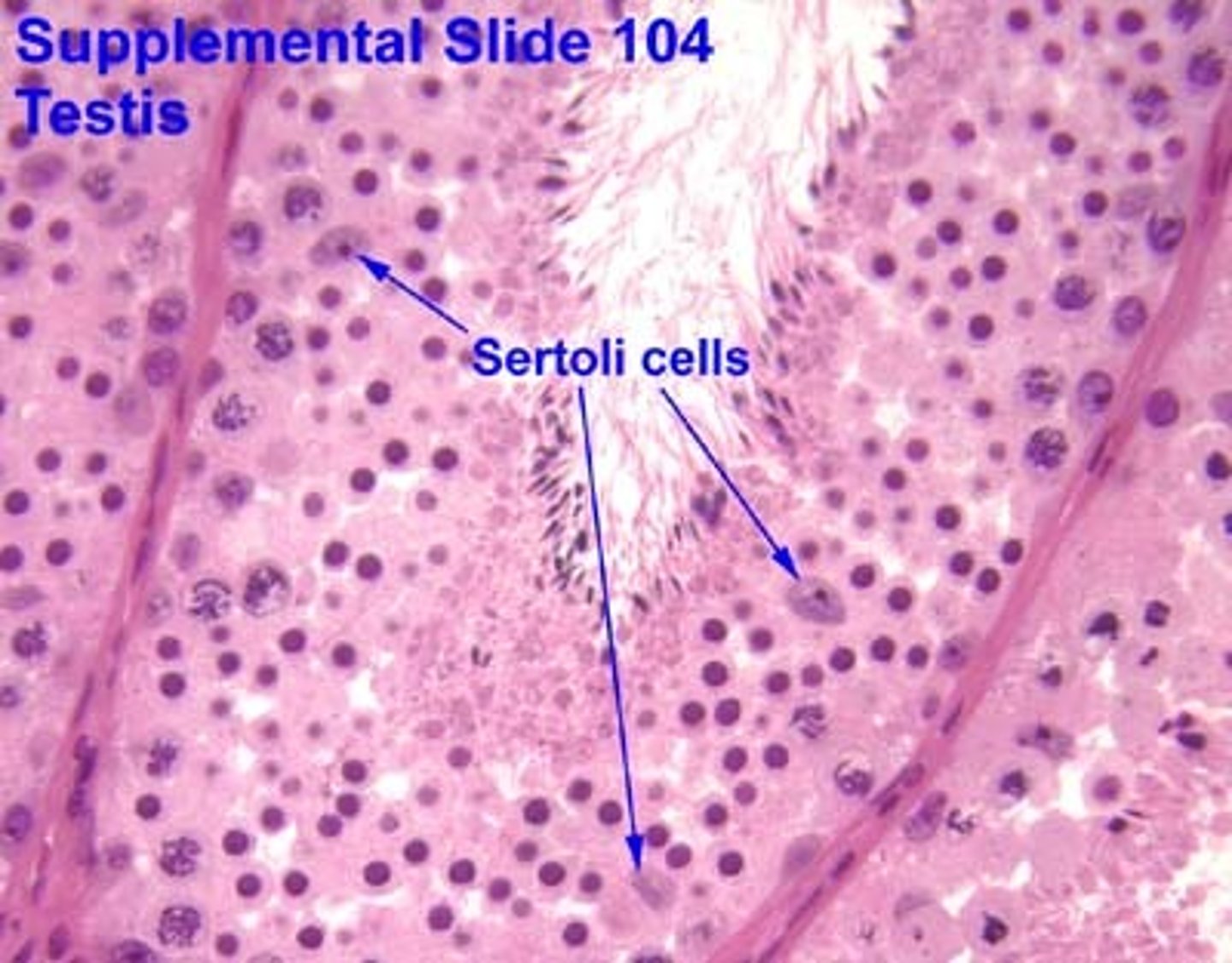
Sertoli cells also secrete an important glycoprotein called..
Androgen Binding Protein (ABP)
ABP binds to testosterone to stimulate...
sertoli cells
When sertoli cells are stimulated they produce...
-sperm
-inhibin
What is purpose of inhibin?
to inhibit (regulate) the pituitary gland's secretion of FSH
*negative feeback
What inhibits LH & GnRH?
androgens
The hypothalamus secretes Gonadatropin Releasing Hormone (GnRH) which stimulates the pituitary gland to secrete FSH and LH.
What is FSH used for in males?
to stimulate the sertoli cells to secrete ABP
*FSH- follicle stimulating hormone
What is LH used for in males?
to stimulate Interstitial Cell Stimulating Hormone (ICSH) to release testosterone
*LH- lutenizing hormone
Review: Pathway of Hormone Secretions for Sperm
1) hypothalamus secretes Gonadatropin Releasing Hormone (GnRH)
2) GnRH stimulates pituitary gland to secrete FSH & LH
3a) FSH stimulates sertoli cells to secrete ABP
3b) LH stimulates Interstitial Cell Stimulating Hormone (ICSH) to release testosterone
4) ABP and testosterone bind stimualting sertoli cells to produce sperm & inhibin
5) Inhibin inhibits FSH to regulate sperm production
6) Androgens inhibit LH & GnRH to regulate
The process of producing sperm is called...
spermatogenesis
Sperm beings as...
spermatogenic cells
Spermatogenic cells orginate at the _____________ epithelium.
germinal
Spermatogenic cells undergo mitosis to produce...
1) primary spermatocyte
2) spermatogonium*
*stays behind to make more sperm
BEFORE puberty, what happens to the primary spermatocyte now?
it STOPS
AT/AFTER puberty, what happens to the primary spermatocyte?
it undergoes meiosis 1
*because at puberty there is an increase in testosterone
Meiosis 1 of the primary spermatocyte gives rise to..
2 secondary spermatocytes
Each secondary spermatocyte undergoes meiosis 2 to produce...
4 spermatids
*which mature into sperm cells
The process of spermatogenesis takes about...
62-72 days
What disease, if gotten after puberty, can sterilize a male because WBC destroy the sperm? How?
mumps
because the infection causes inflammation in the testes which increasing permeability and WBC can enter and attack sperm in trying to attack the infection
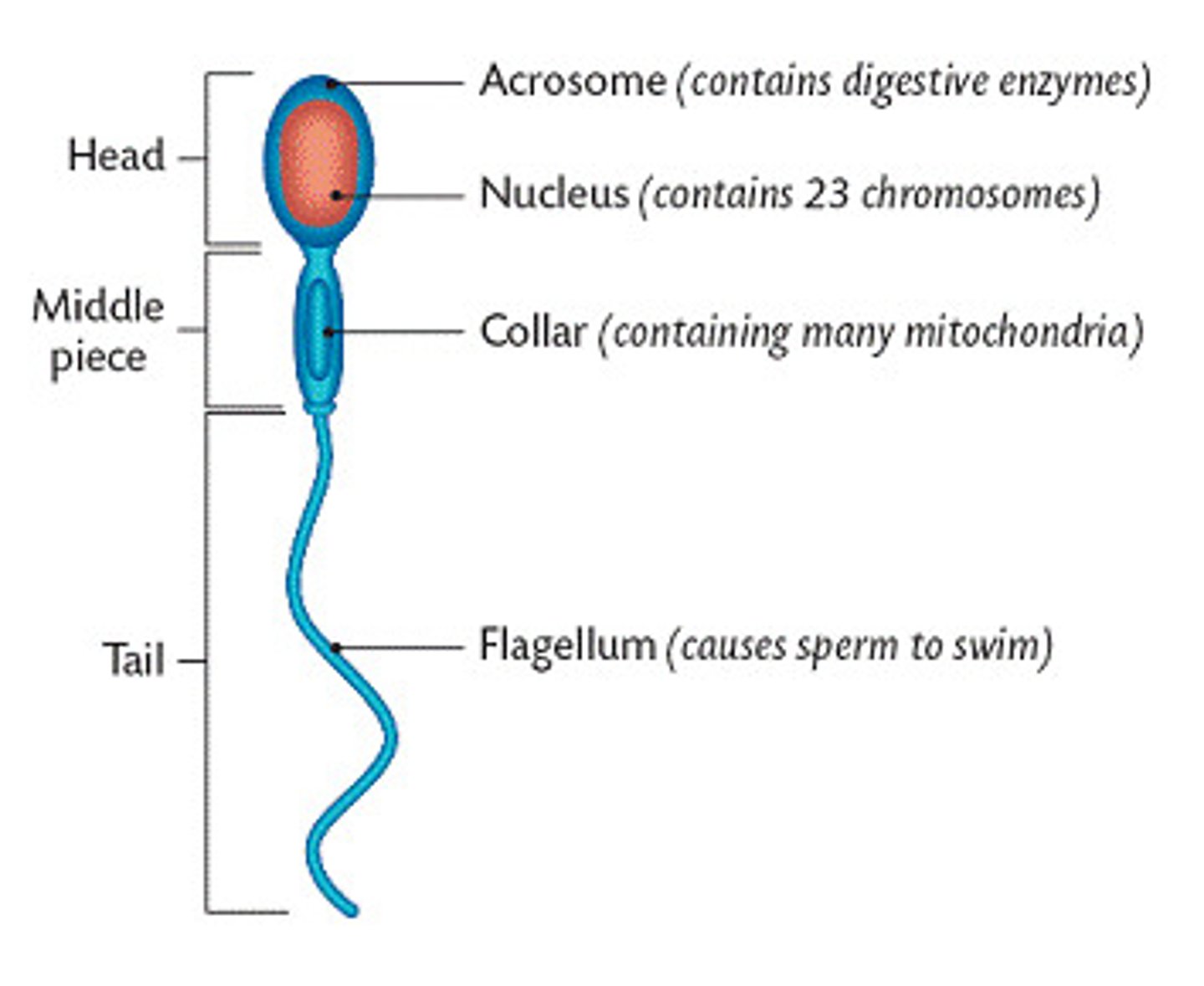
A mature sperm is comprised of what 3 part?
1) head
2) body (middle piece)
3) tail (flagellum*)
*an extend of the original cell membrane- not grown
In addition to the testes, the male reproductive system is composed of many accessory structures.
The seminiferous tubules give rise to ducts that join to a tube coiled on the outer surface of the testis called the...
epididymis
*sperm cells mature here
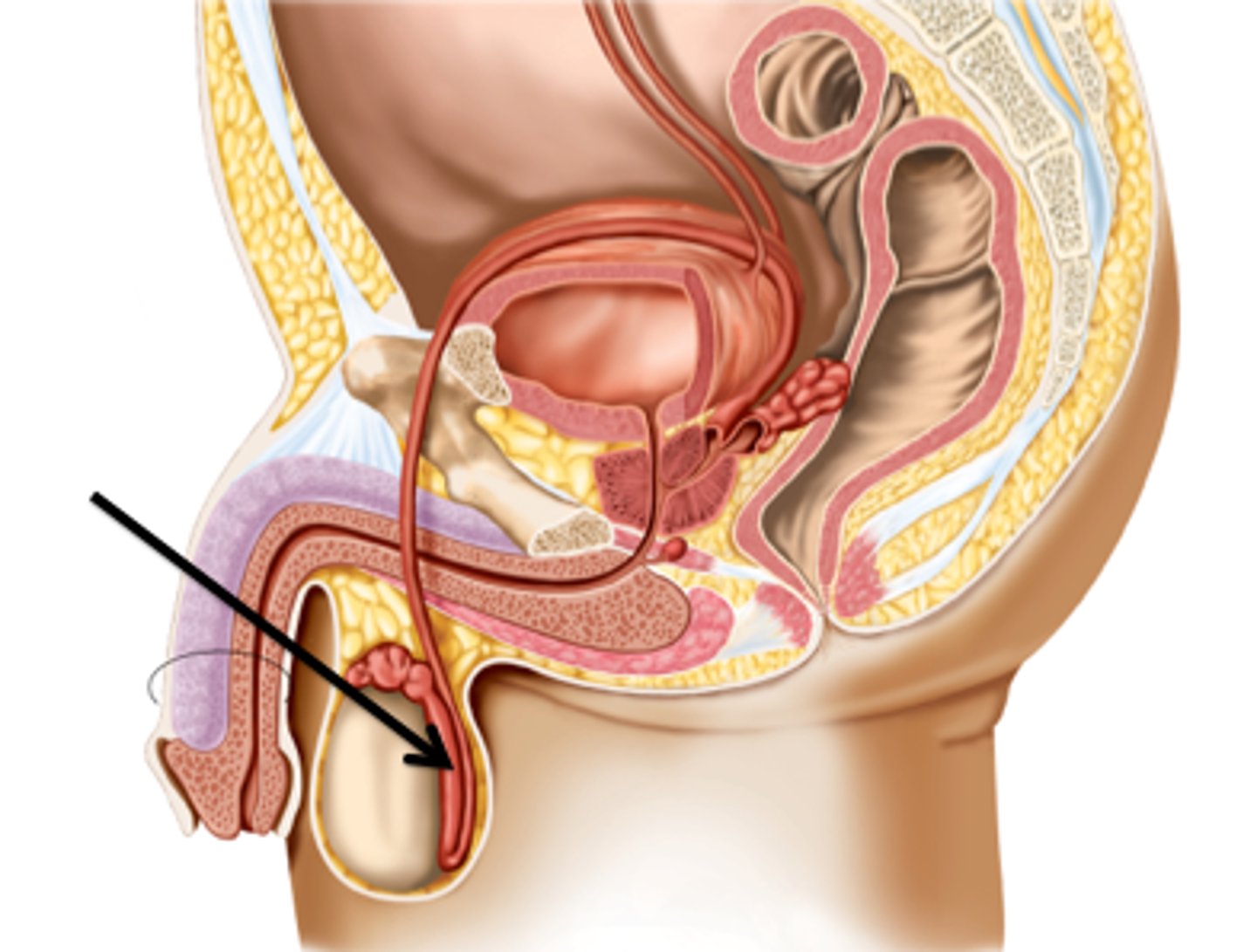
The epididymis then become the...
vas deferns
*this is what is cut in a vasectomy
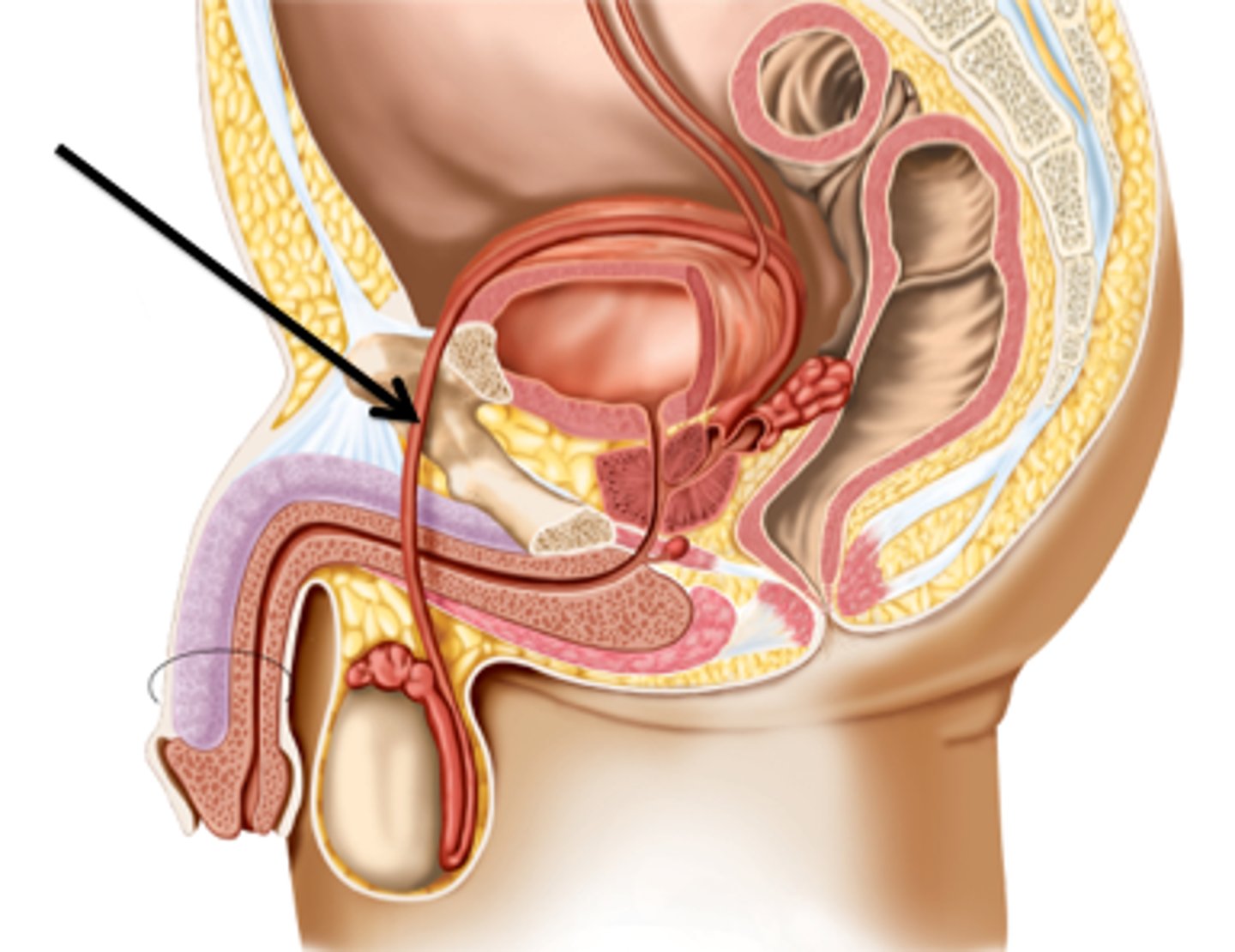
The vas deferns extends upward into the abdominal cavity and ends behind the bladder where it joins the duct of the...
seminal vesicle (#5)
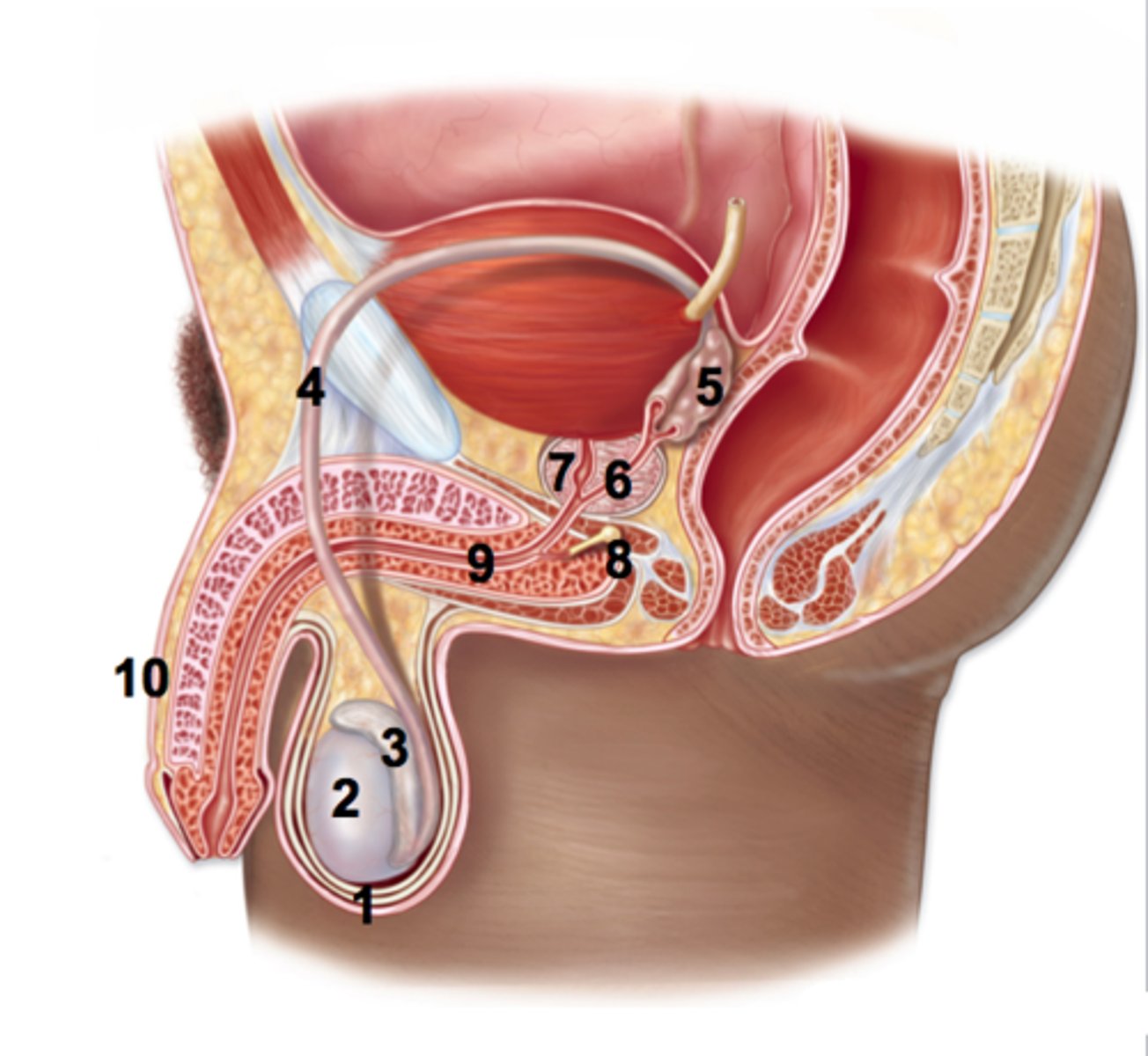
What do secretions of the seminal vesicle include? What do they do?
-fructose: for sperm nutrients
-prostaglandins: slow/stop smooth muscle contractions in the female aiding in sperm movement to egg
When sperm joins the fluid of the seminal vesicle what does the alkaline nature of the seminal fluid do?
activates the sperm
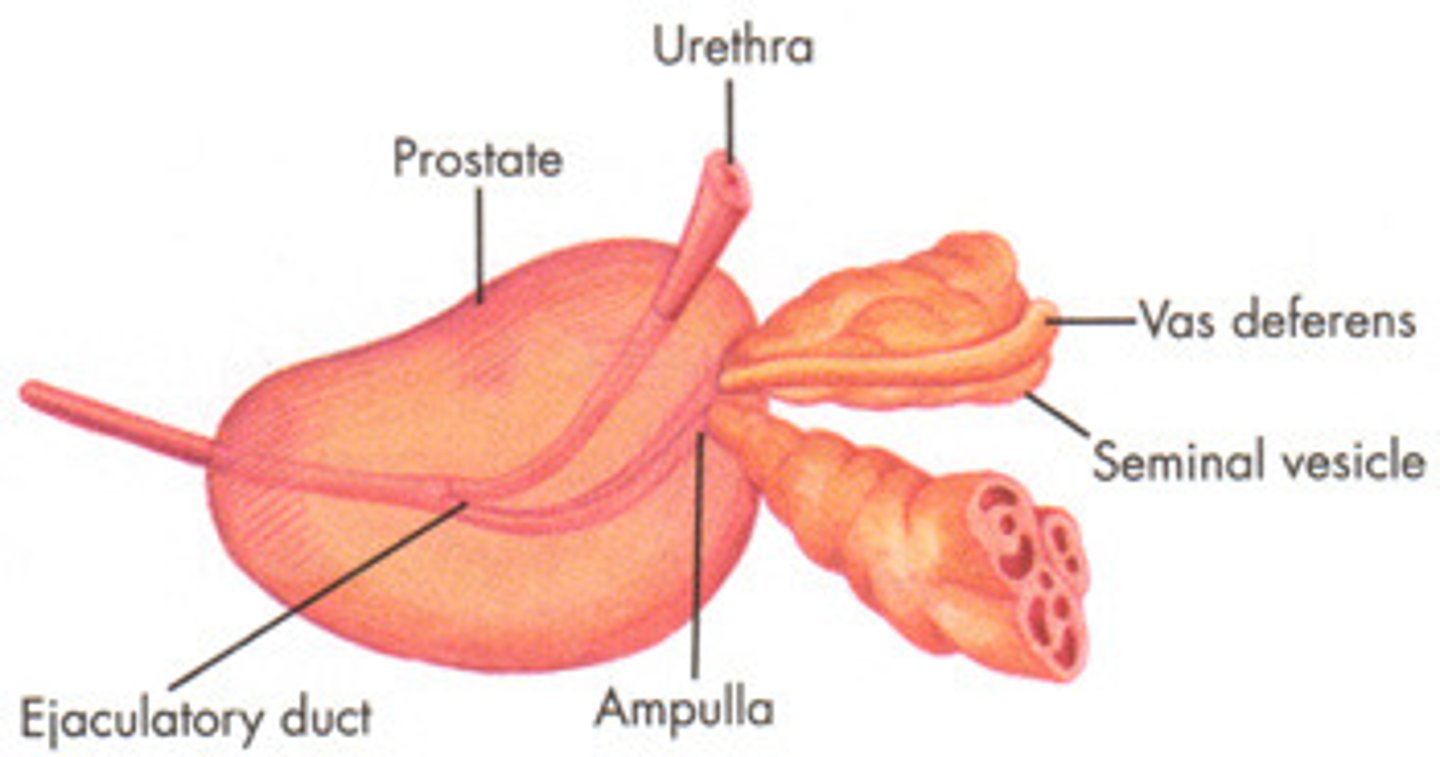
The vas deferns tube and the duct of the seminal vesicle form the.... duct.
ejaculatory duct (#6)
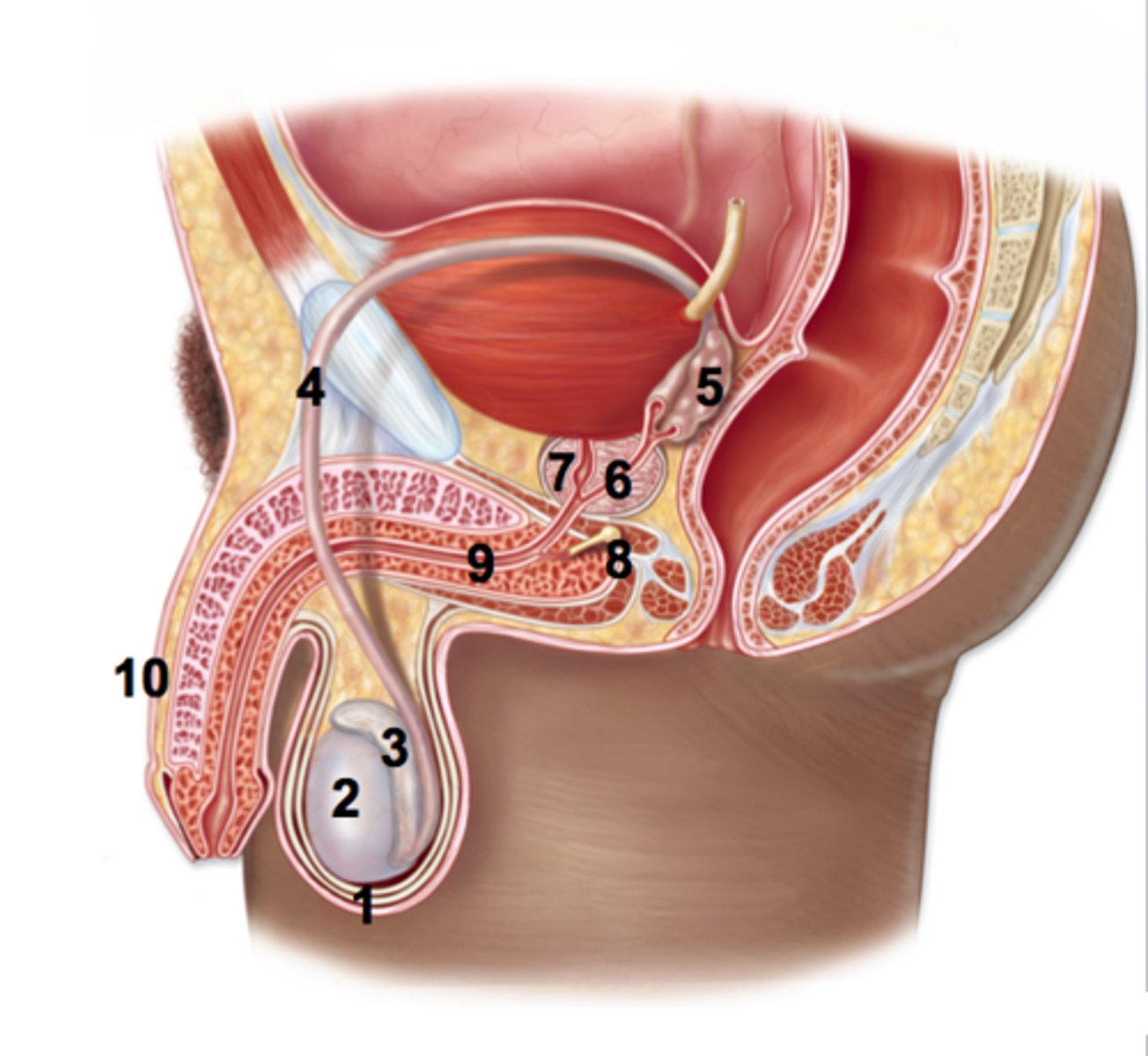
The ejaculatory duct joins to the...
urethra (#9)
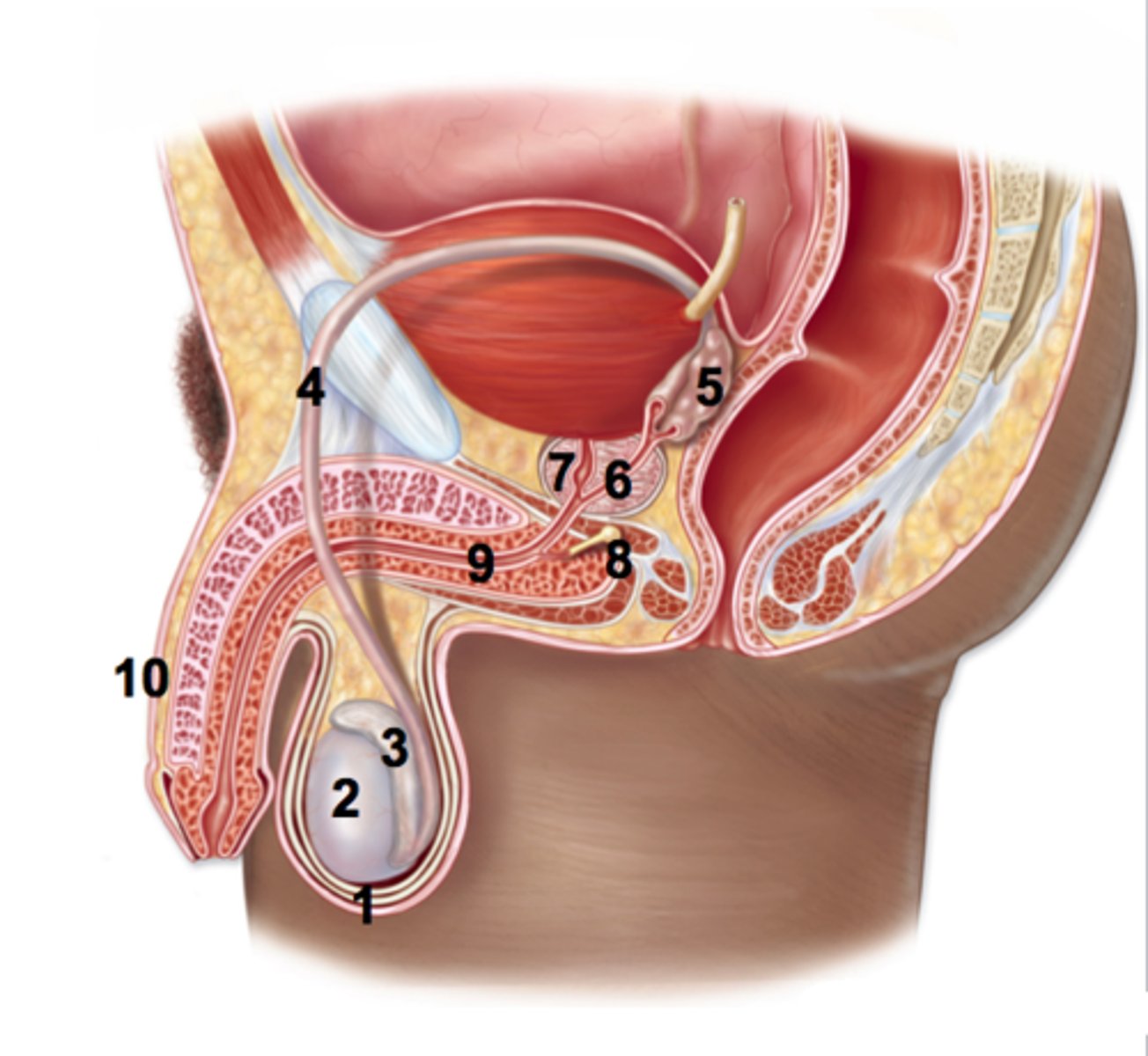
What gland deposits a slightly acidic fluid into the urethra to combine with seminal fluid to make it more fluid-like?
the prostate gland
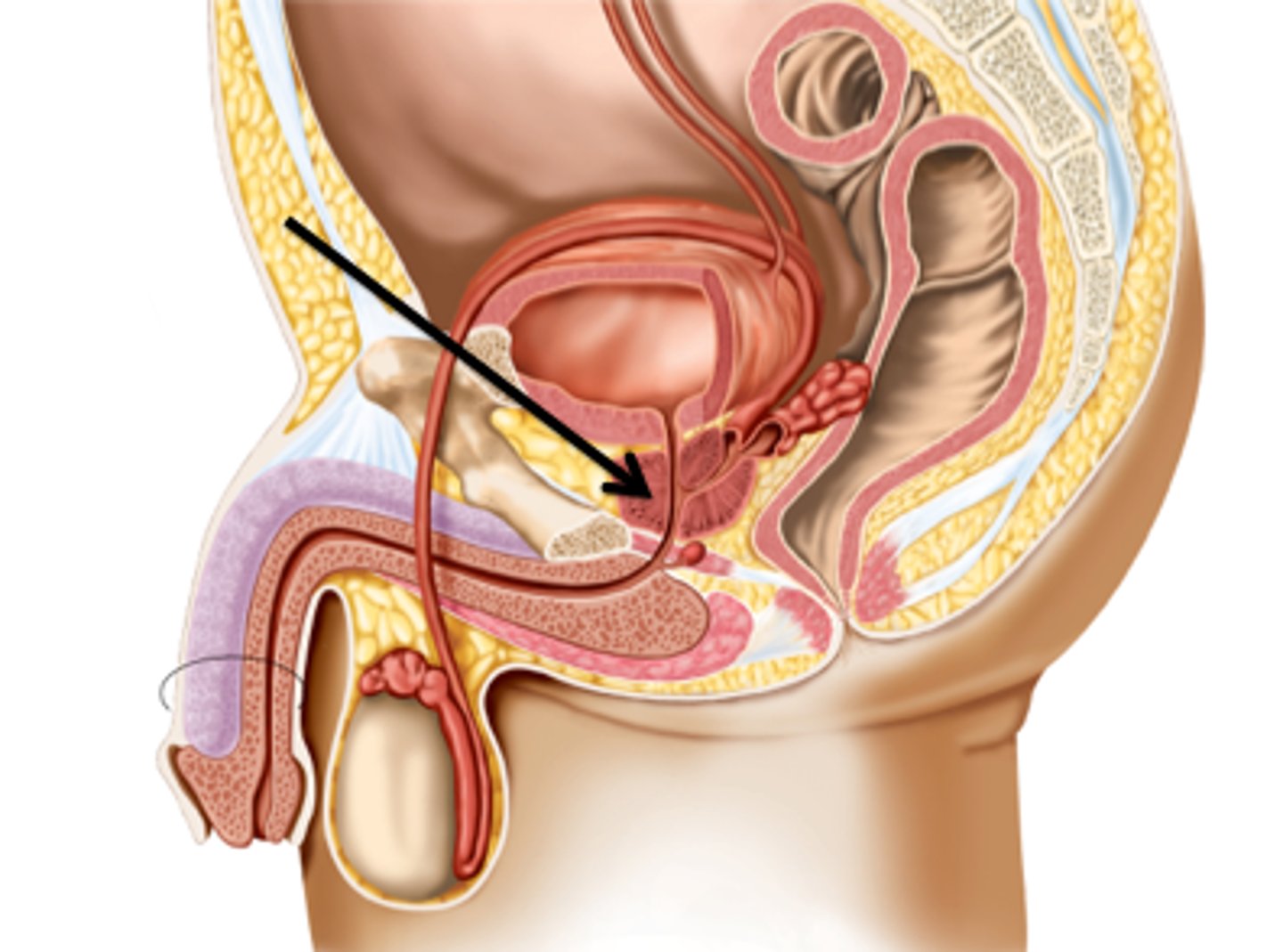
Note: How all the tubules come together at the urethra.
What glands (2) are found inferior to the prostate gland?
bulbourethal (Cowper's) glands
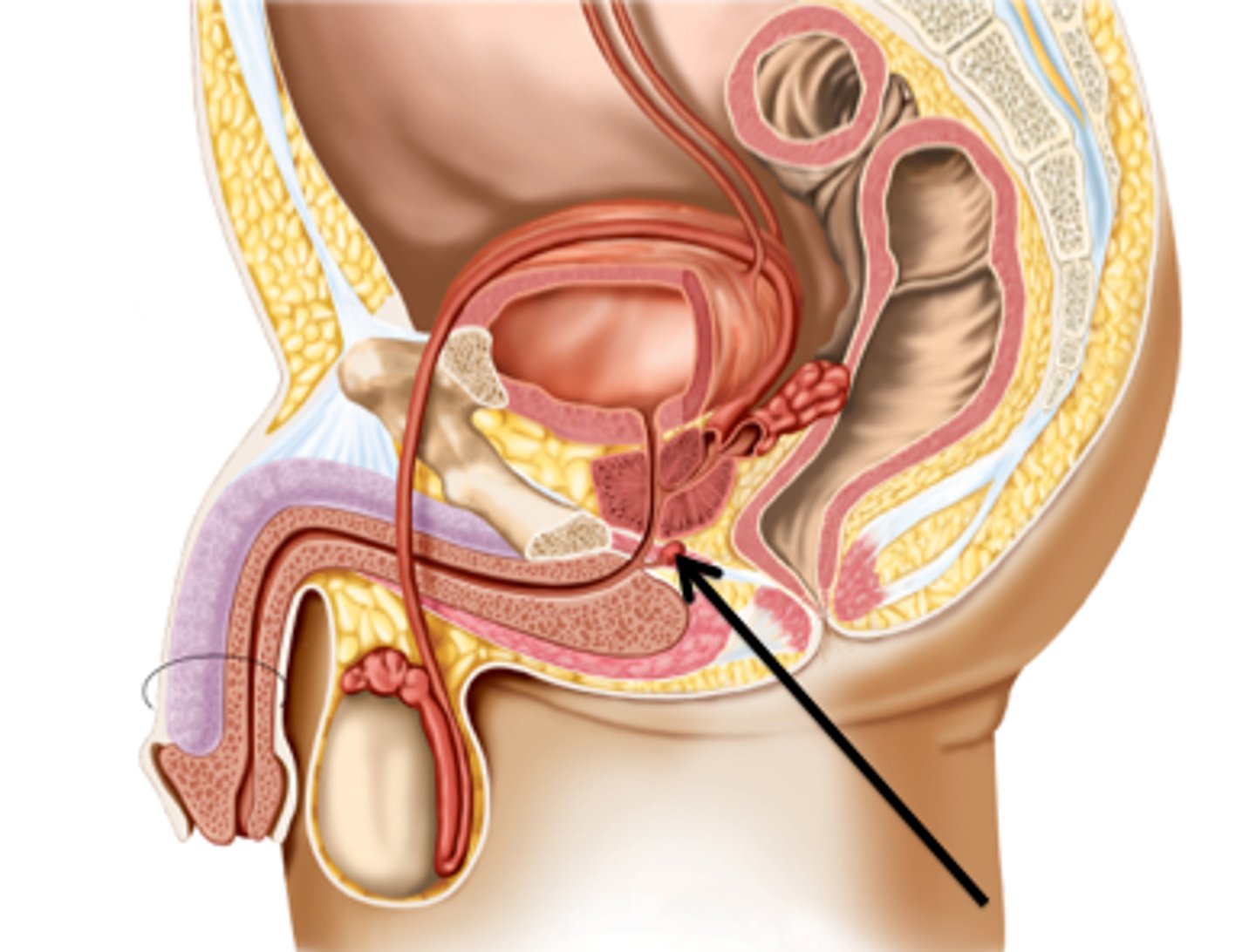
What do the oil-like secretions of the bulbourethal glands provide?
-secreted in response to sexual stimulation ahead of semen to clear urethra for any acidic substance (urine)
-lubricates
Out of all male cancers, what cancer is responsible for 42% of them?
prostate cancer
*typically in North Americans residents (including African Americans) and Western European's
American Americans in Africa are not affected
Female Reproductive System
What are primary tissues/sex organs for females?
the ovaries
What do the ovaries produce?
-ovum (egg)
-hormones (mainly estrogens)
What some of primary functions of estrogens?
-stimulate growth of reproductive organs
-thicken endometrium of uterus (development of uterus wall)
-secondary characteristics
What are the female secondary characteristics?
-development of mammary glands and ductile system
-increased deposits of adipose tissue around breasts
What other main hormone does the ovaries produce?
progesterone
What does progesterone do?
-maintains uterine lining
-promotes changes in uterus during reproductive cycle (makes more vascular)
-affects mammary glands
-affect GnRH & pituitary hormone secretions
What do estrogens and progesterone inhibit?
secretions of FSH & LH
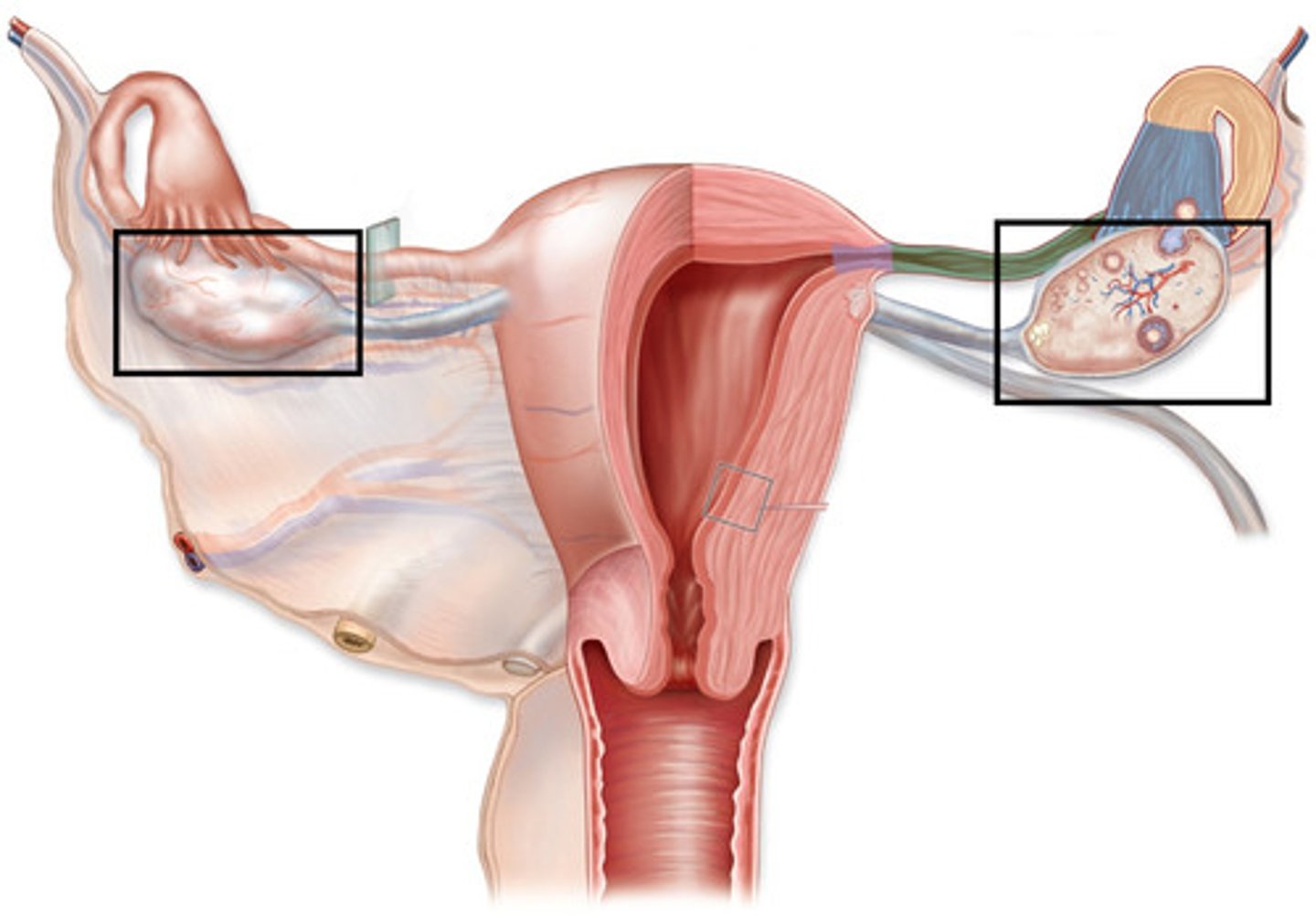
How are the ovaries attached?
3 ligaments:
1) Broad
2) Ovarian
3) Round
*also attaches uterus
Note: Broad Ligament
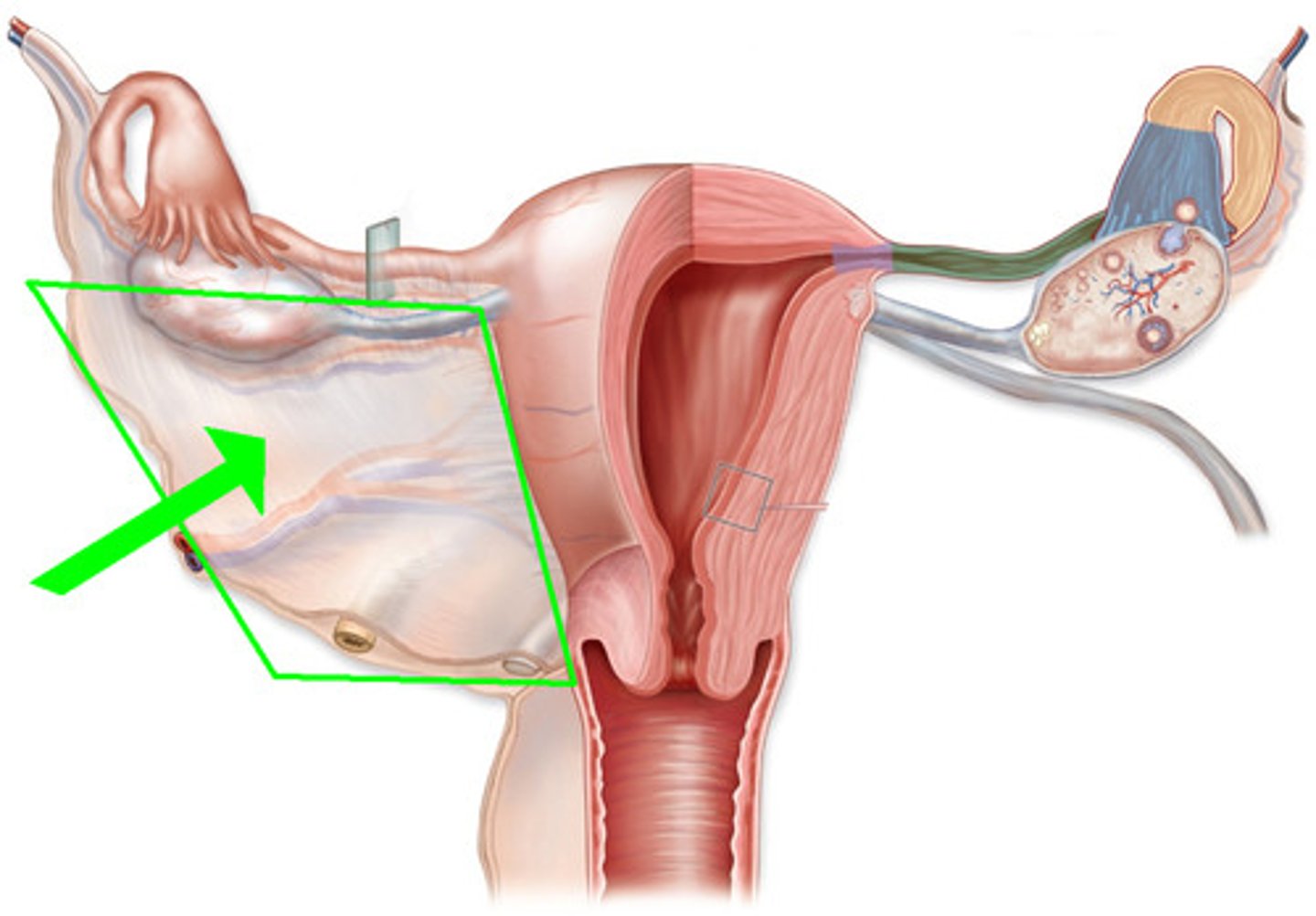
Note: Ovarian Ligament
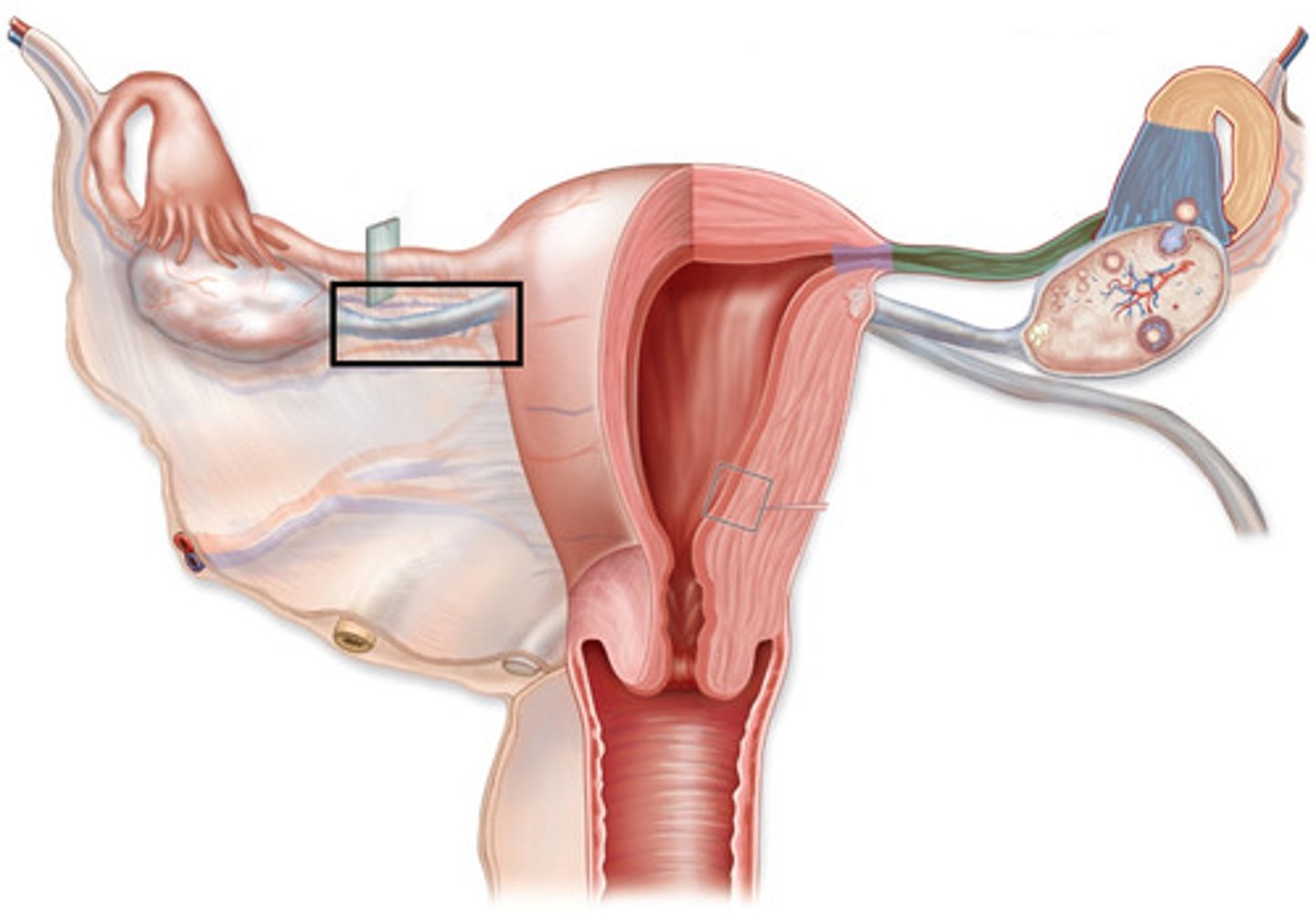
Note: Round (suspensory) ligament
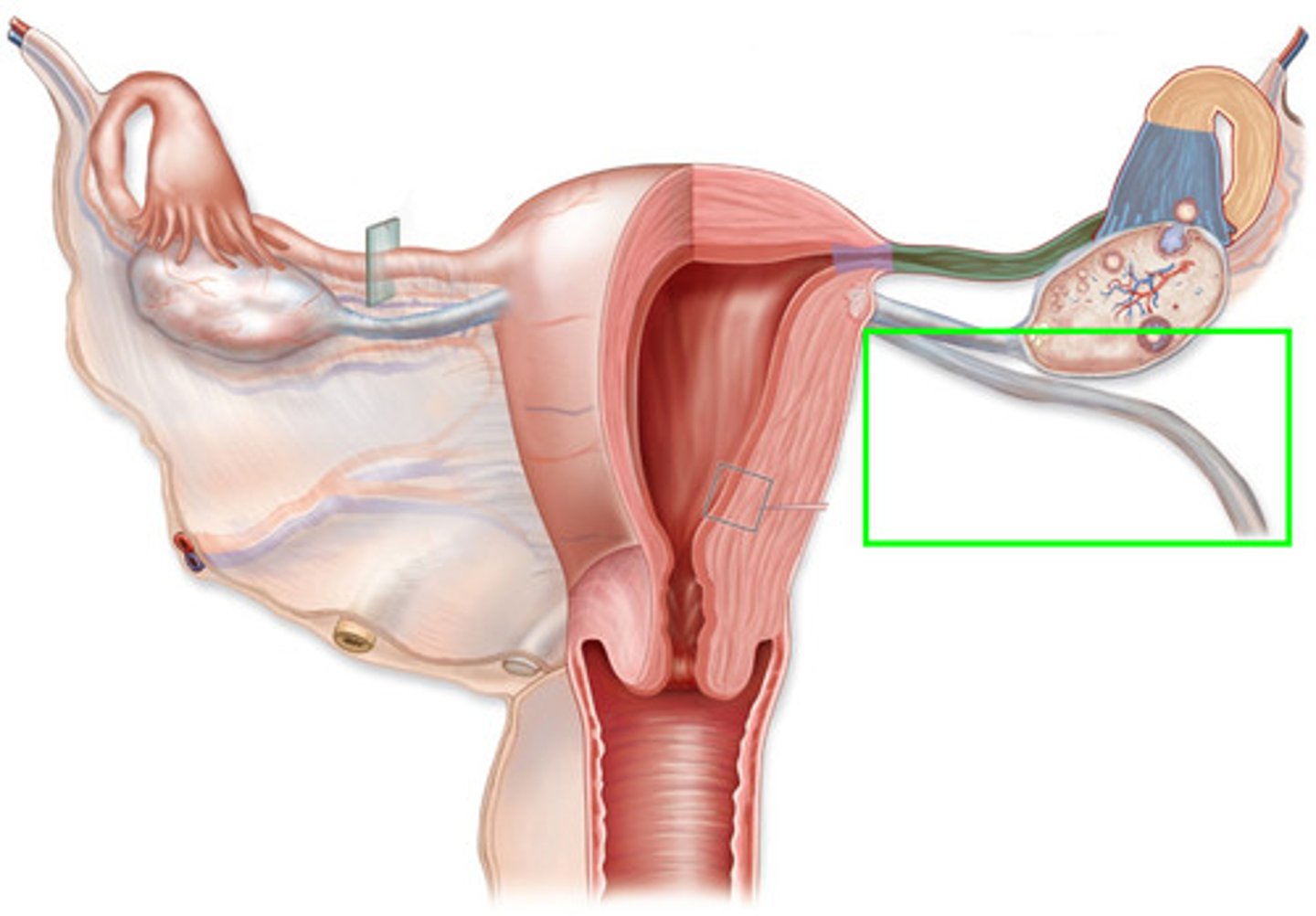
Within the ovary, formation of the egg begins a process called...
oogenesis
Egg development and growth occurs with..
ovarian follicles
An egg begins as..
oogenia
Before birth, oogenia begins to develop into...
primary oocytes
What type of follicle surrounds primary oocytes?
primordial follicle (#8)
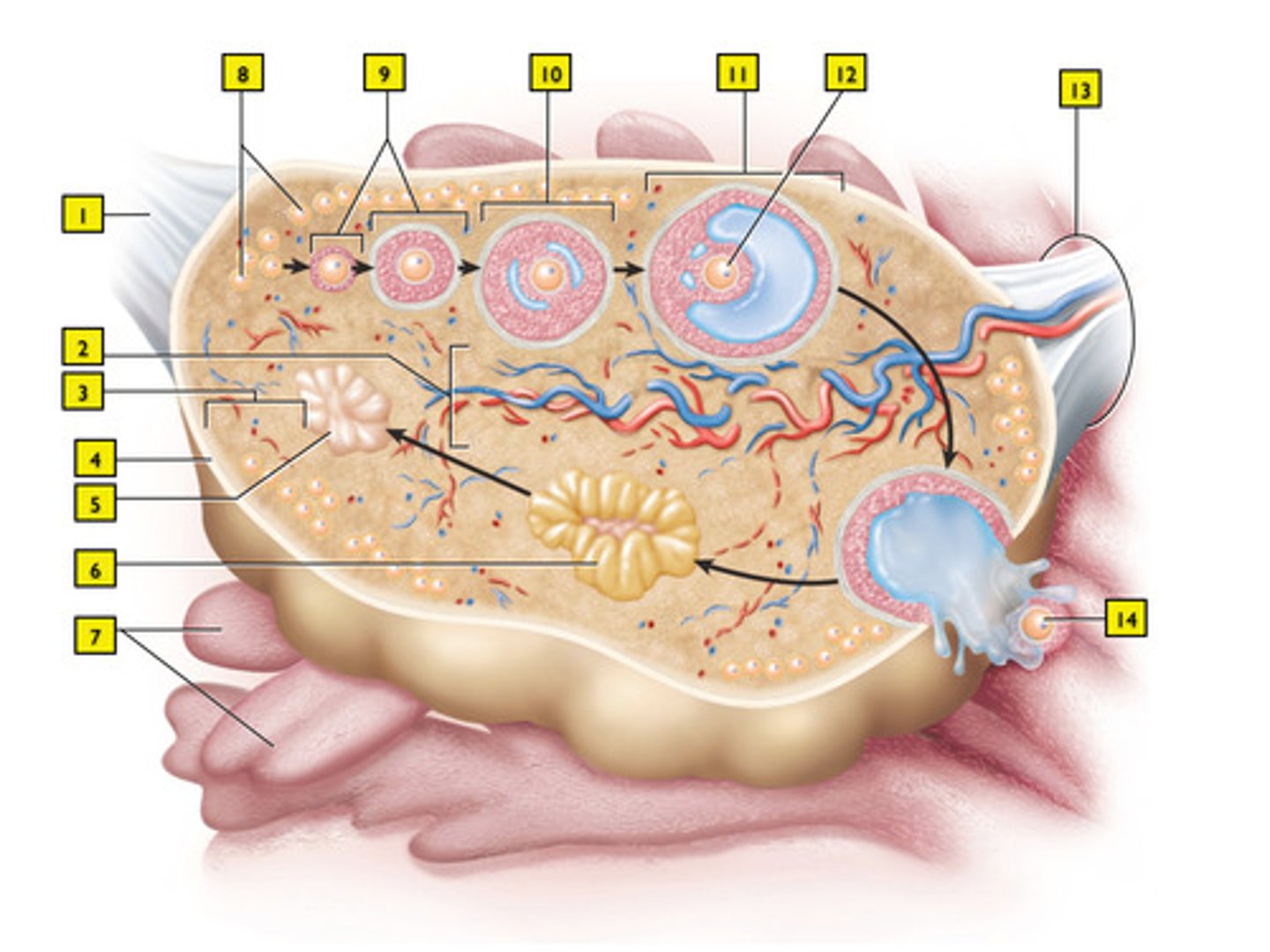
Primary oocytes begin to undergo meiosis 1 but what happens?
[remember this is still prenatal]
it STOPS until puberty
*meanwhile primary oocytes and primordial follicles keep forming determining the number eggs a female has before birth
At puberty, the hypothalamus will begin to secrete...
gonadatropin releasing hormone (GnRH)
What does GnRH stimulate?
the anterior pituitary gland to secrete FSH & LH
*follicle stimulating and lutenizing hormone
What does FSH do?
-stimulates maturation of ovarian follicles
-stimulates cells of the follicle to produce and secrete estrogens
What does LH do?
stimulates ovulation and development of the corpus luteum
At/after puberty, what happens to the primary oocytes in primordial follicles? Why?
they mature into primary follicles with a primary oocyte (#9)
because of increase levels of FSH
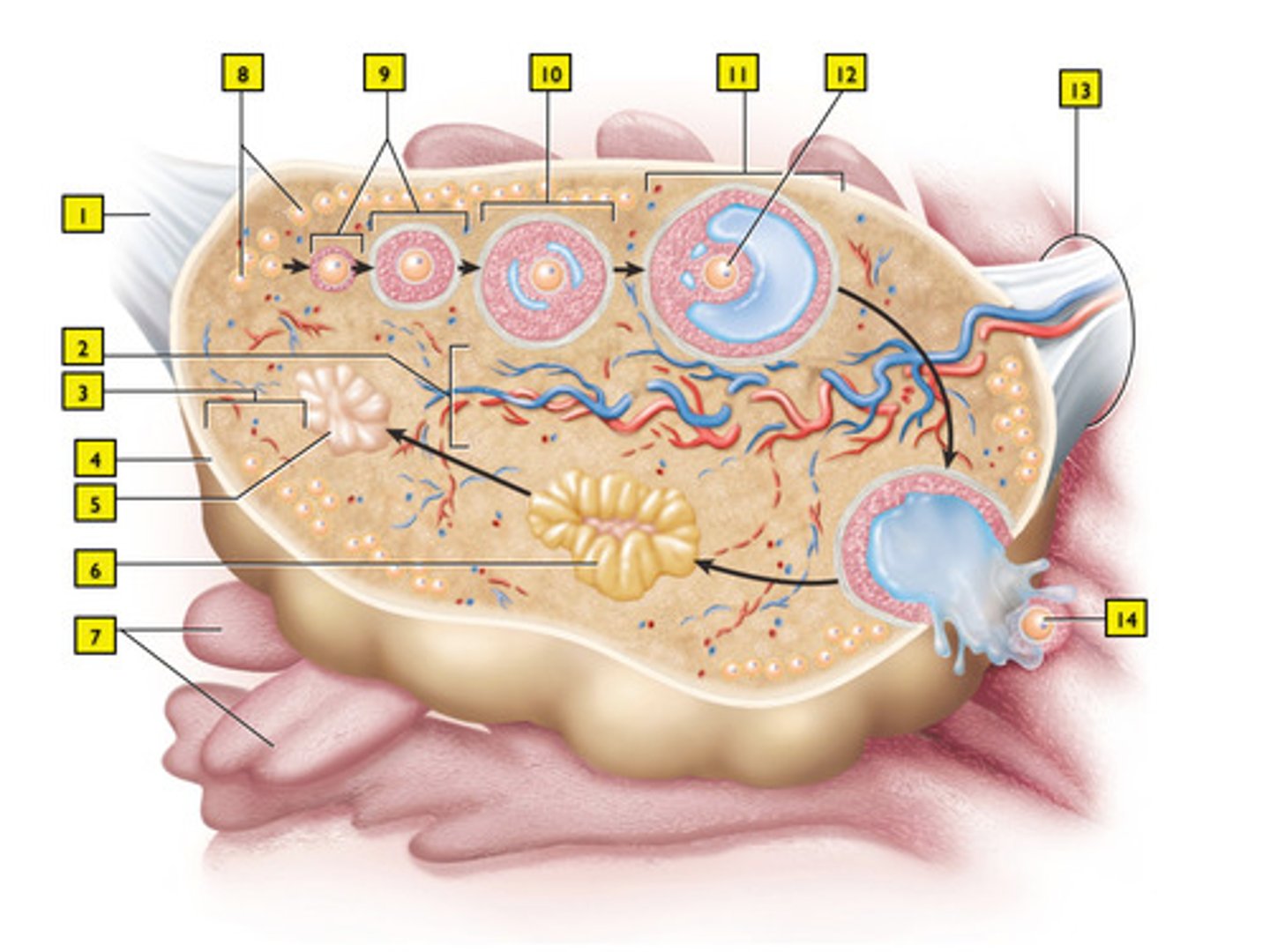
An average female form axp. 400,000-500,000 eggs, but 90% of them die. How many does a female typically use in a lifetime?
400-500
As the primary follicle matures, the zona pellucida forms separting what?
the egg from the corona radiata
Primary oocytes then complete meiosis 1 and divided into...
-1 secondary oocyte
-1 polar body (degernates)
*cytoplasm is divided UNequally in oogenesis
The primary follicle is now called a... with the secondary oocyte.
secondary follicle (#10)
*0.2mm
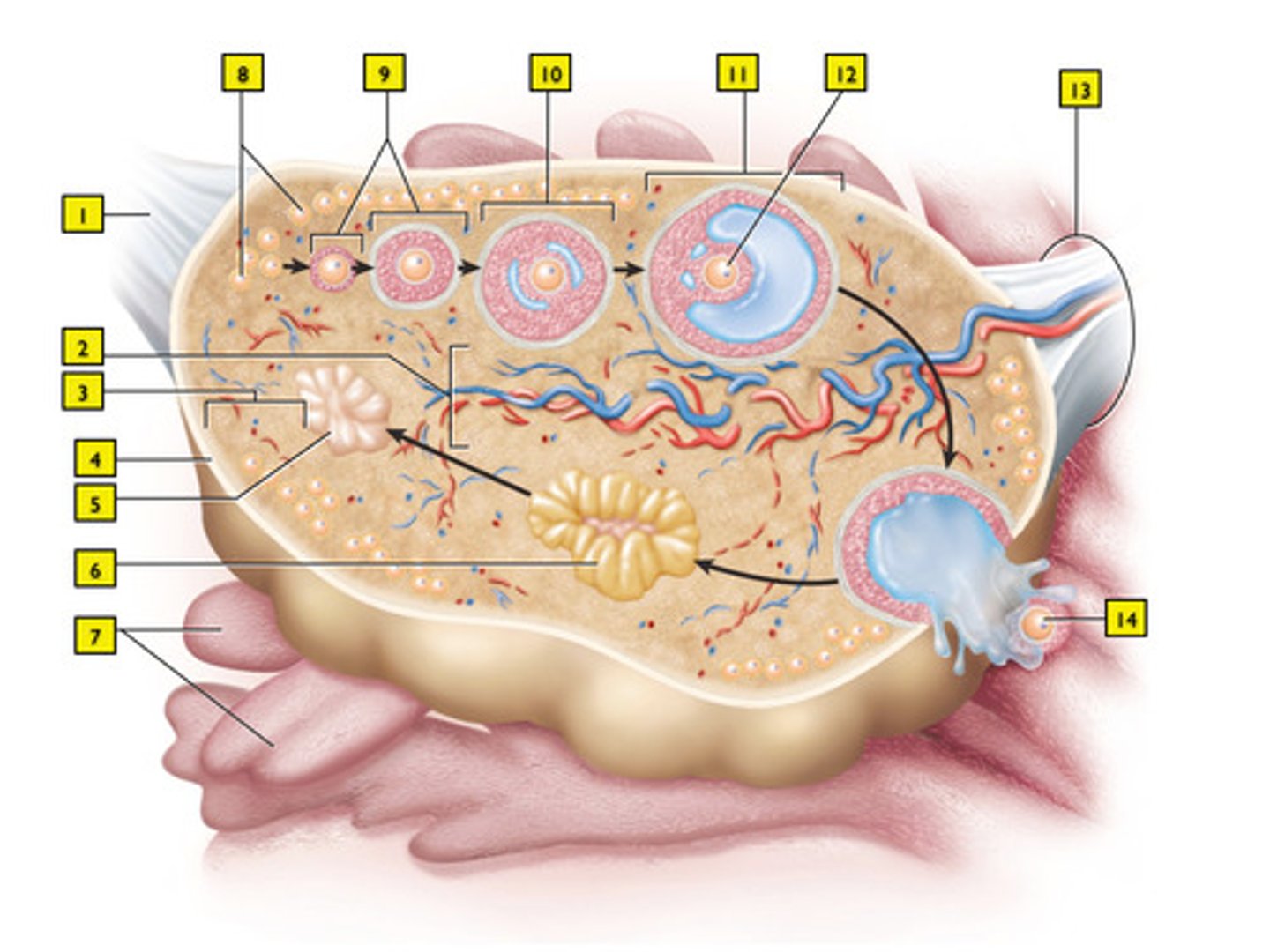
The secondary follicle is now surrounded in.... cells.
thecal cells
What do the thecal cells do?
convert female testosterone to estrogens
The secondary follicle with the secondary oocyte then matures into a...
mature (Graafian) follicle (#11)
*10-20mm
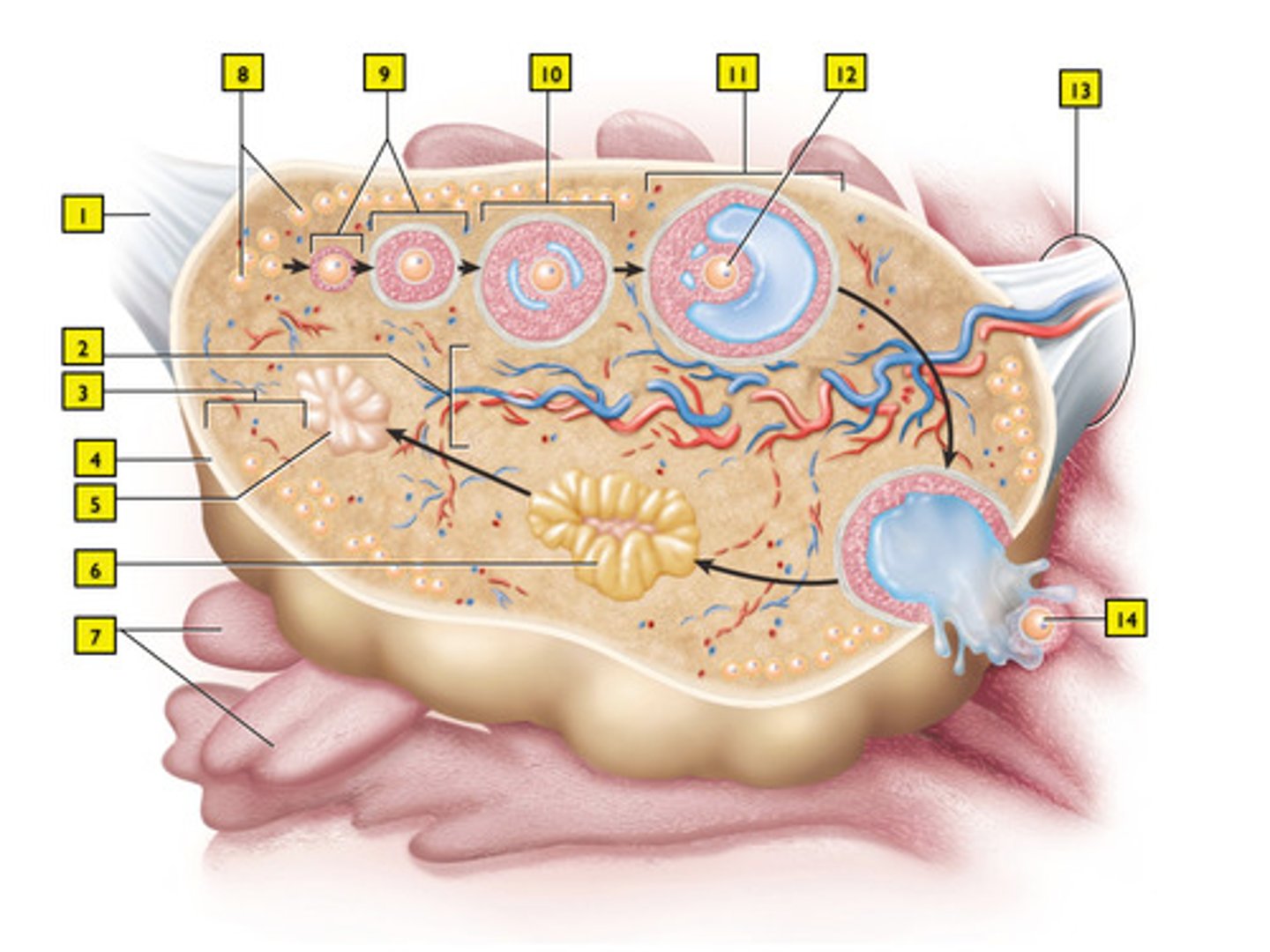
The process called... release the secondary oocyte from the mature follicle.
ovulation
What hormones play a role in follicle maturation for ovulation?
FSH & LH* (one specific follicle & egg always takes a presidency over the others)
*LH typically only at the beginning
What causes the mature follicle to weaken and rupture ovulating the secondary oocyte?
increase in LH
What happens to the ruptured follicle?
it becomes the corpus luteum (#6)
*used later if fertilized to secrete estrogens & progesterone
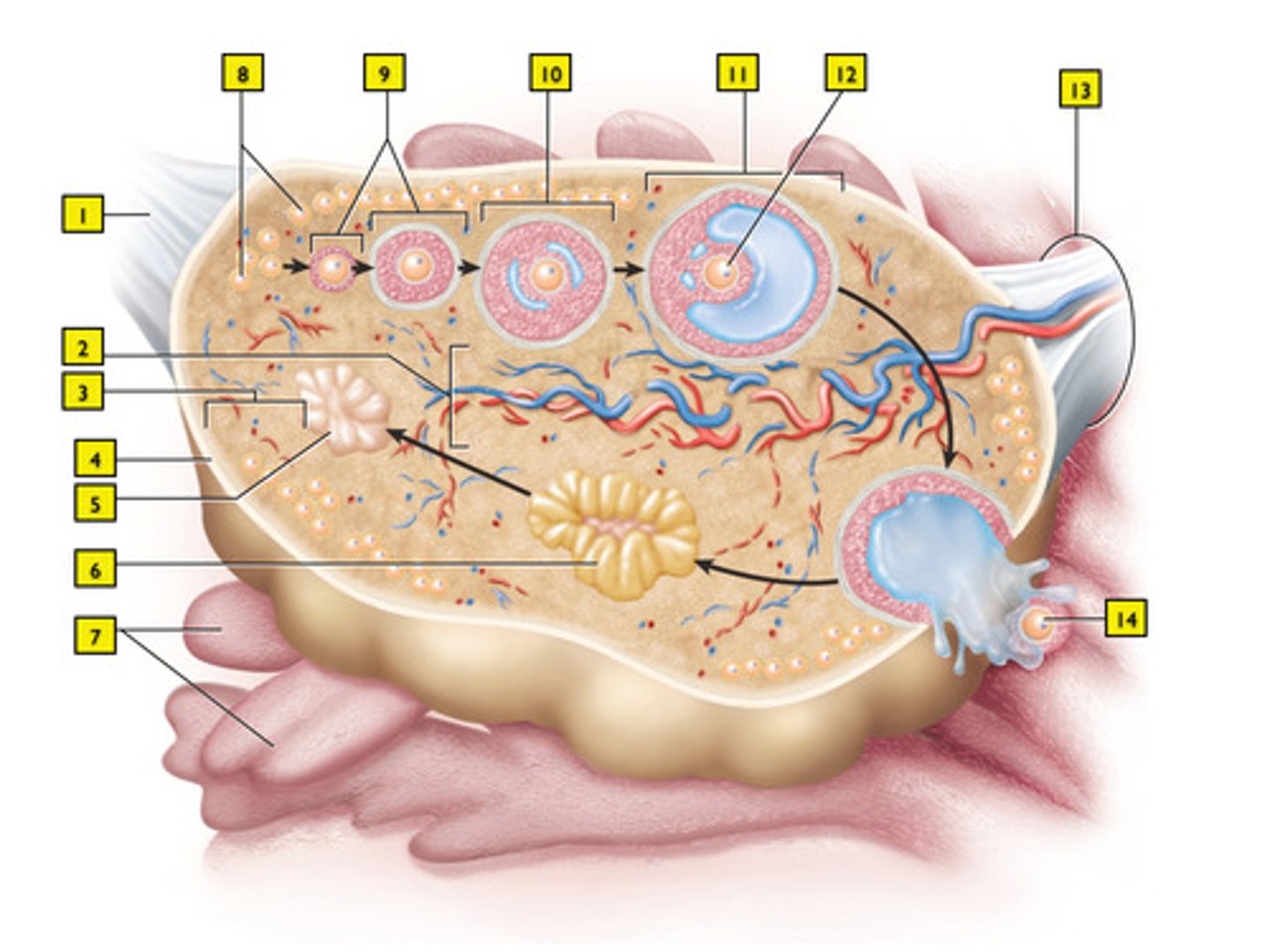
After ovulation, LH is also responsible for...
keeping the corpus luteum alive till fertilization
*if not, it becomes connective tissue (also no longer produces estrogens and progesterone)
In addition to the ovaries, the female reproductive system is composed of accessory structures.
What tubular structure is near the ovary and "catches" the ovulated egg?
the uterine tube (oviducts aka Fallopian tubes)
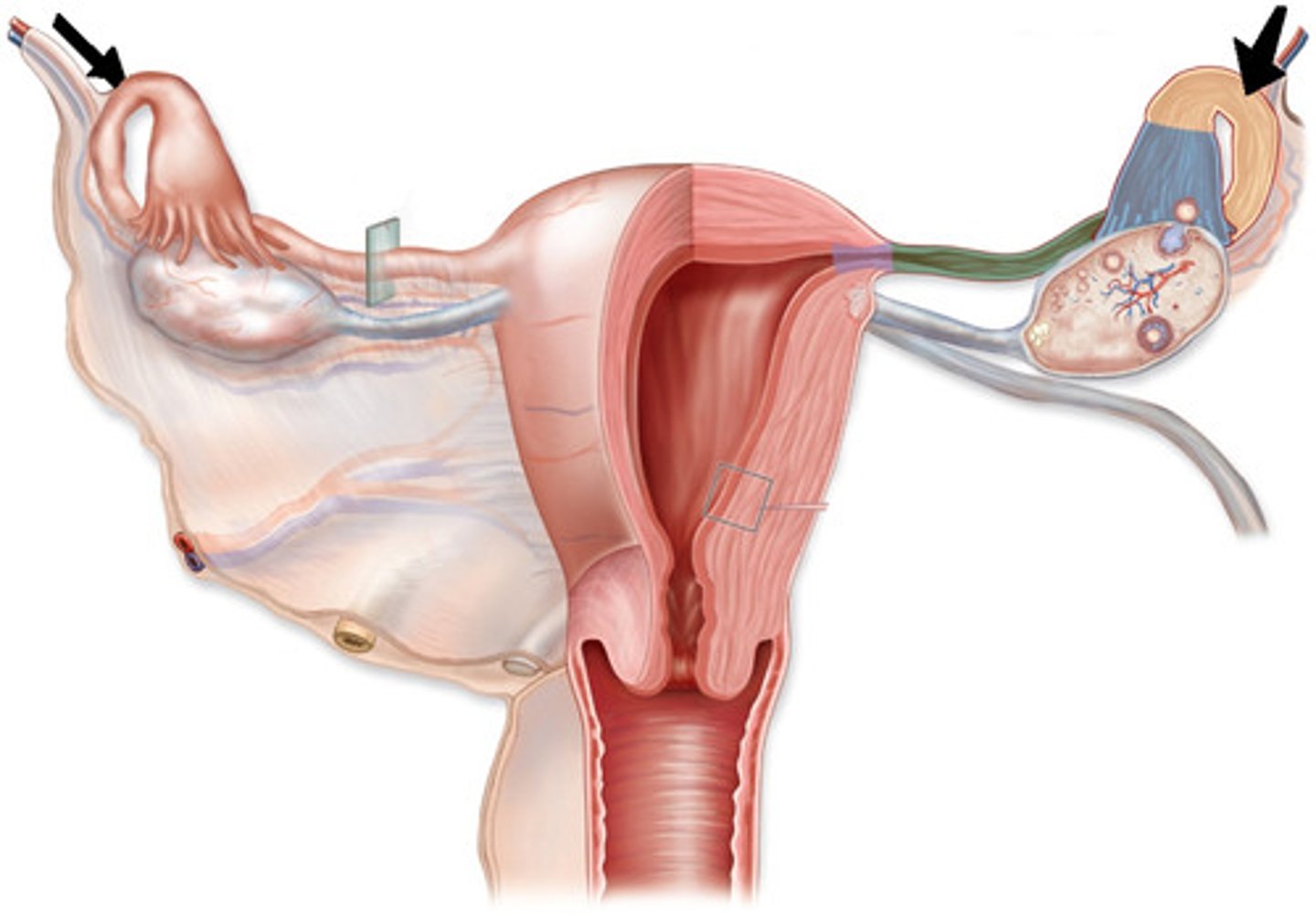
Uterine tubes are axp. ____cm x ____cm.
10 cm x 0.7 cm
The _______________, the funneled part, and the ______________, the finger-like projections, connect to the ovary.
infundibulum; fimbriae*
*the part that actually touches the ovary
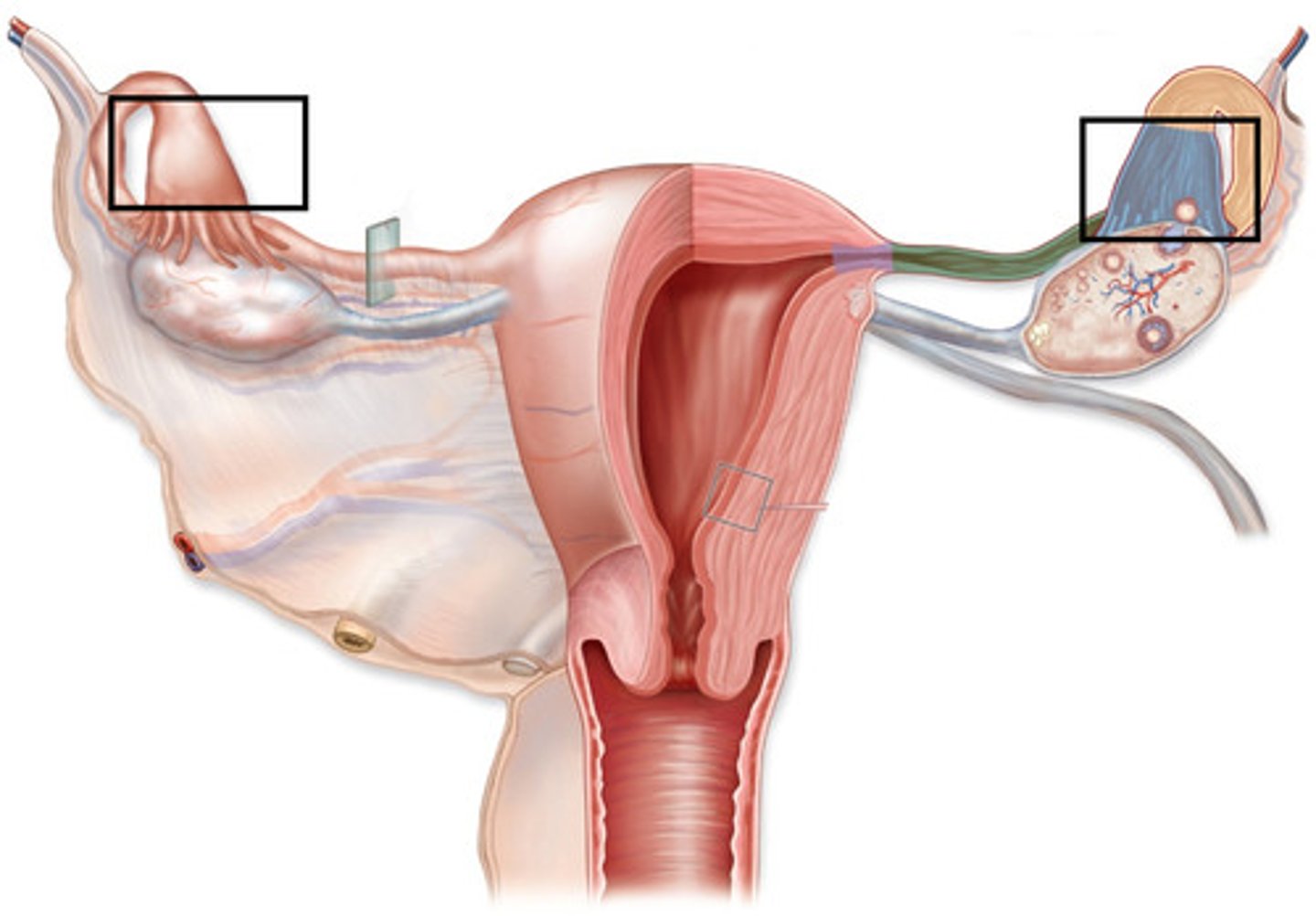
What do the uterine tubes contain that help move the egg along?
cilia
It is in the uterine tube that secondary oocyte and sperm union (fertilization) occur.
When the cell is fertilized it undergoes meiosis 2 to produce...
-ovum (zygote)
-a second polar body (degenerates)
*if not fertilized within hours the secondary oocyte degenerates too
Where do the uterine tubes travel to?
the uterus
The uterus is made up 2 main portions. What are they
-body
-cervix [pictured]
![<p>-body</p><p>-cervix [pictured]</p>](https://knowt-user-attachments.s3.amazonaws.com/f10dba8e-bd5d-46fc-9f97-2e1c96f2e4b1.jpg)
The wall of uterus is comprised of 3 layers. What are they?
1) endometrium (epithelium)
2) myometrium (smooth muscle)
3) perimetrium (serosa)
In which uterine layer does implantation of the embryo occur?
the endometrium
The female reproductive cycle is characterized by the regular reoccurring changes in the...
endometrium
Leading up to fertilization, the body increases the endometrium in the _________________ phase (Day 4-14).
proliferative
On day 14, ovulation occurs.
If the secondary oocyte is NOT fertilized, what part that once was producing estrogens & progesterone begins deteriorating?
the corpus luteum
When the corpus luteum deteriorates and ceases hormone production this causes...
blood vessels in the the endometrium to constrict
When the blood vessels constrict and slow blood supply to the endometrium this phase is called the...
secretory phase (Day 14-28)
The constricted blood vessels eventually cause the endometrium (uterine lining) to...
degenerate
*this is bleeding
This process is a cycle because now that estrogens and progesterone are no longer being produced, what hormones are no longer inhibited?
FSH & LH
*this begins the cycle again
How long does the egg survive without fertilization?
24 hours
How long does the sperm survive in the woman's body without the egg?
72-120 hours