14. Hormonal Contraception
1/17
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
18 Terms
What is hormone-based contraceptives?
A variety of hormonal contraceptive methods are available
Although highly effective at preventing pregnancy, hormonal methods do not offer protection against STIs
What is Progestogen?
Umbrella term
Progesterone – natural hormone
Progestogen/Progestin – can also include synthetic versions
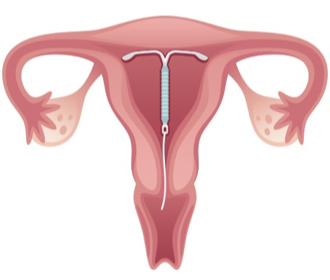
What are intrauterine devices?
IUD: Device inserted inside the uterus; T-shaped, fans out in uterus.
Types: Progestogen (hormonal) IUD.
Mechanism:
Delivers steady daily hormone.
HPG axis adjusts → silences natural hormonal fluctuations.
Eliminates natural cycle peaks and dips; body senses constant hormone levels.
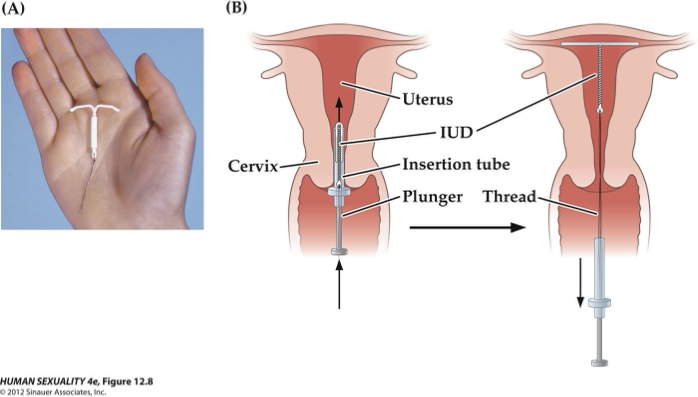
What are progestogen IUDs?
Levonorgestrel IUD - common progestin in IUDs
Releases progestin regularly, providing steady hormone level
Mechanism/Onset of Action
Foreign body at uterus prevents fertilization, impairs sperm transport
Slow release of levonorgestrel causes thickening of cervical mucus, antiproliferative effect on endometrium and suppression of ovulation
Therapeutic Regimen
Inserted by a trained clinician and replacement depends on product expiry (3 vs. 5 years)
How do 28-day combined hormonal contraceptive tablets work and why is there a 7-day hormone-free period?
Structure: 28-day pack → 21 days of hormone + 7 days no hormone.
Mechanism:
21 days: Steady hormonal support → suppresses natural cycle fluctuations.
Prevents thickening of endometrium → lighter periods.
7 days hormone-free:
Causes light withdrawal bleeding (“period”).
Originally included for user comfort/normalcy based on clinical trial feedback.
Clinical impact: Heavy periods are reduced because endometrial lining doesn’t thicken much.

What are estrogen and progestogen combinations?
Combined Oral Contraceptives (COCs) a.k.a. “The Pill”
Contain varying amounts of estrogen & progestogens
Different options available
Mechanisms of Action
Primarily inhibits ovulation
Thickens cervical mucus
Interfere with fertilization by altering tubal motility of ovum
Inflammation and atrophy of the endometrial lining

What is monophasic, biphasic, and triphasic?
Monophasic: Fixed Dose. Same estrogen/progestogen dose for 21 days
Biphasic: Usually estrogen stays constant, progestogen increases halfway
Triphasic: Estorgen and/or progestogen levels change each week
Purpose of variations: Tailored for individual tolerance; can reduce side effects like headaches, bloating, mood changes, tiredness.
Special considerations:
People with family history of blood clots, stroke, or cardiovascular disease may use progestin-only pills to avoid estrogen-related risks.

What do POPs (Progestin-only pills) do?
POPs thicken cervical mucus, making it difficult for sperm to swim into the uterus or to enter the fallopian tube
POPs alter the normal cyclical changes in the uterine lining and may result in unscheduled or breakthrough bleeding (disrupting uterine lining → prevents implantation)
Some may inhibit ovulation – although not consistently
What are hormones and non-oral routes?
Depo-Provera
Slow-release progestogen, administered by injection and lasts 3 months (sits in the muscle and is slowly released)
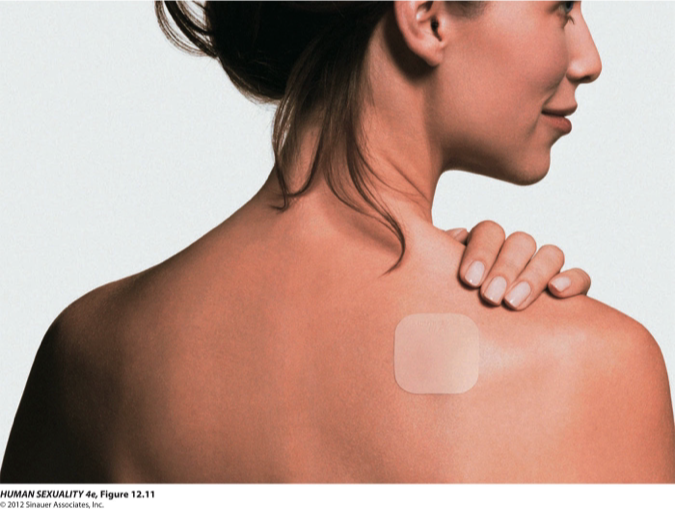
Transdermal patches
Contain an estrogen and progestogen, with replacement every week
Vaginal rings
Release a combination of an estrogen and a progestogen and remain in place for three weeks
Implantable rods
Release progestogen and are extremely reliable, replaced every three years
What is Depo-Provera?
Injectable progestogen
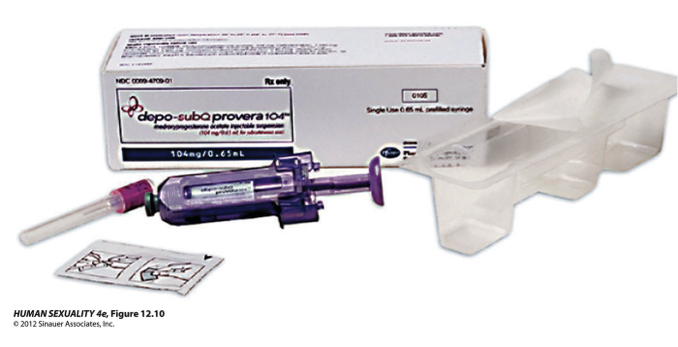
What is Depot Medoxyprogesterone Acetate (DMPA)?
Commonly known as Depo-Provera
Can be considered if estrogen is contraindicated/poorly tolerated (ex: symptoms/clinical history of cardiovascular disease or blood clots)
Mechanism/Onset of Action
Suppresses ovulation
Absorbed slowly from injection site
Therapeutic Regimen: Injected intramuscularly every 3 months
What is the Ortho Evra Patch?
Replace every week
Contain varying amounts of ethinyl estradiol and norelgestromin (synthetic progestogen)
Mechanisms of Action
Primarily inhibits ovulation
Thickens cervical mucus
Interfere with fertilization by altering tubal motility of ovum
Inflammation and atrophy of the endometrial lining
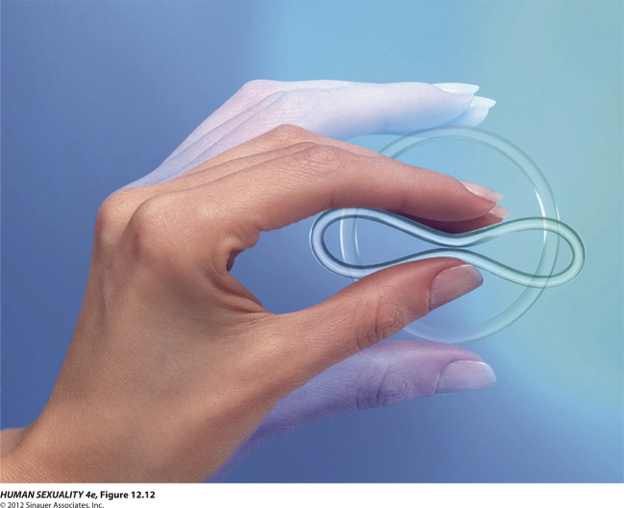
What is the NuvaRing?
21 days inside with a 7-day free break
Contain varying amounts of ethinyl estradiol and etonogesteral (synthetic progestin)
Mechanisms of Action
Primarily inhibits ovulation
Thickens cervical mucus
Interfere with fertilization by altering tubal motility of ovum
Inflammation and atrophy of the endometrial lining
What is Implanon and how does it work?
Implanon: Subdermal rod containing synthetic progestin (lab-made progesterone).
Mechanism: Placed just under the skin → slowly releases hormone over time.
Purpose: Provides steady hormonal contraception; choice can be adjusted based on individual tolerance or side effects.
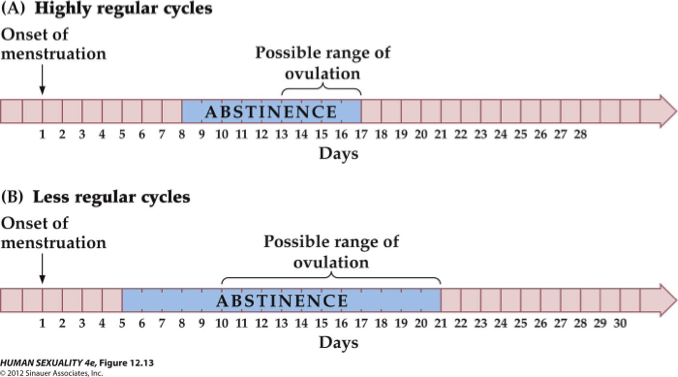
How does the Behavioural (fertility awareness) Method of contraception work, and what are its limitations?
Method: Track menstrual cycle (usually ~28 days) → avoid sex during possible ovulation window (~day 8–16).
Considerations: Sperm can survive several days; ovulation timing varies, especially with irregular cycles.
Limitations: Unreliable alone; best used in combination with hormonal contraceptives.
What is emergency hormonal contraception?
Progestogen-Only (Levonorgestrel) or “Plan B”
Ulipristal acetate (UPA)
What is Progestogen-Only (Levonorgestrel) or “Plan B”?
Mechanism of Action
Inhibits ovulation, thickening of cervical mucus, interference with implantation. No effect on existing pregnancy.
Most effective within 72 hours of unprotected intercourse or suspected contraceptive failure (the earlier the better). May be effective up to 5 days.
Therapeutic Regimen: 1 complete dose to be taken as soon as possible after unprotected intercourse or suspected contraceptive failure (ideally within 72 hours).
What is Ulipristal acetate (UPA) - Ella One?
Mechanism of Action
Prevents progesterone from occupying its receptor by competitive inhibition
Inhibits/delays ovulation by preventing LH peak and postponing follicular rupture
Most effective within 120 hours of unprotected intercourse or suspected contraceptive failure (the earlier the better)
Therapeutic Regimen: 1 complete dose to be taken within 120 hours of unprotected intercourse or suspected contraceptive failure
Drug Interactions: Consider avoiding use with CYP 3A4 P450 inducers and other hormonal contraceptives (anti-seizure, HIV treatment/antiretroviral drugs, narcolepsy medication)