6.2 - the blood system
1/64
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
65 Terms
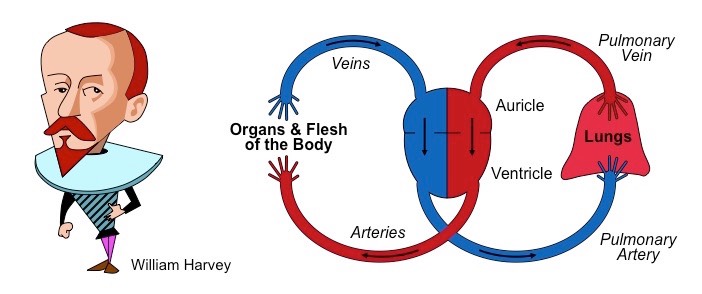
What were the beliefs about circulation before Harvey’s findings
Arteries and veins were separate blood networks
Veins were thought to pump natural blood produced by the liver
Arteries were thought to pump heat produced by the heart via the lungs (for cooling – like bellows)
What did William Harvey propose?
Arteries and veins were part of a single connected blood network (he did not predict the existence of capillaries however)
Arteries pumped blood from the heart (to the lungs and body tissues)
Veins returned blood to the heart (from the lungs and body tissues)
Human heart composition
The human heart is a four chambered organ, consisting of two atria and two ventricles
What does the atria act as
The atria act as reserviors, by which blood returning to the heart is collected via veins (and passed on to ventricles)
What do the ventricles act as?
The ventricles act as pumps, expelling the blood from the heart at high pressure via arteries
Why are there two sets of atria and ventricles
because there are two distinct locations for blood transport
The left side of the heart pumps oxygenated blood around the body - systemic circulation
The right side of the heart pumps deoxygenated blood to the lungs - pulmonary circulation
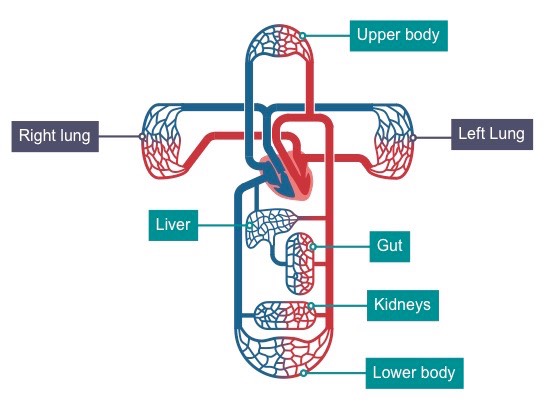
Why will the left side of the heart have a much thicker muscular wall
as it must pump blood much further because it pumps blood around the body
What is the function of arteries?
to convey blood at high pressure from the heart ventricles to the tissues of the body and lungs
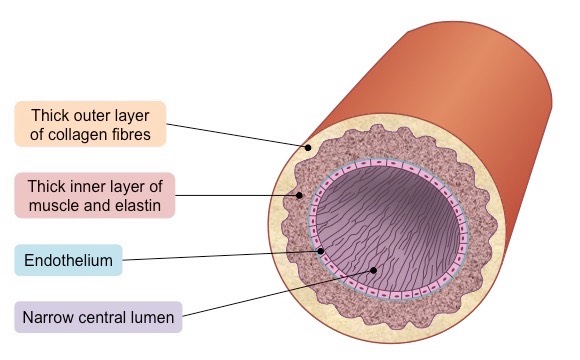
What are arteries’ specialised structure to accomplish their task?
They have a narrow lumen (relative to wall thickness) to maintain a high blood pressure (~ 80 – 120 mmHg)
They have a thick wall containing an outer layer of collagen to prevent the artery from rupturing under the high pressure
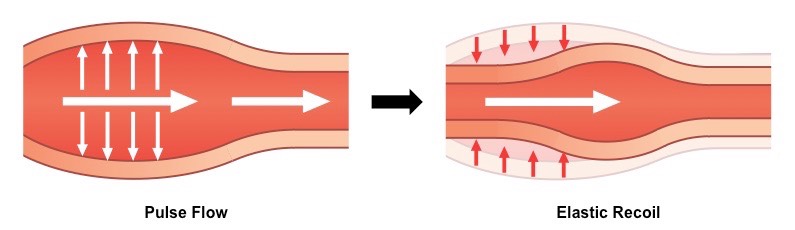
The arterial wall also contains an inner layer of muscle and elastic fibres to help maintain pulse flow (it can contract and stretch)
Flow of blood in arteries (where is it expelled from and then where does it flow?)
Blood is expelled from the heart upon ventricular contraction and flows through the arteries in repeated surges called pulses
How do muscle fibers in arteries help with blood flow?
The muscle fibres help to form a rigid arterial wall that is capable of withstanding the high blood pressure without rupturing
Muscle fibres can also contract to narrow the lumen, which increases the pressure between pumps and helps to maintain blood pressure throughout the cardiac cycle
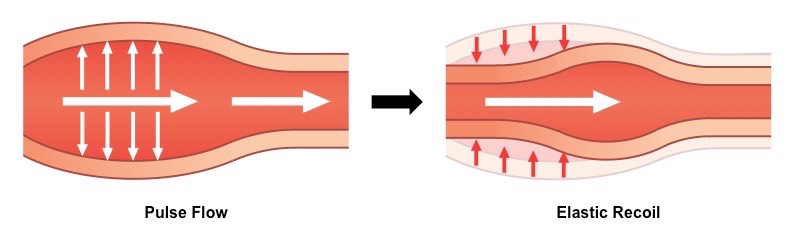
How do elastic fibers in arteries help with blood flow?
they allow the arterial wall to stretch and expand upon the flow of a pulse through the lumen.
The pressure exerted on the arterial wall is returned to the blood when the artery returns to its normal size
This helps to push the blood forward through the artery and maintain arterial pressure between pump cycles
What is the function of capillaries?
to exchange materials between the cells in tissues and blood travelling at low pressure
relationship between arteries, cappilaries, veins
Arteries split into arterioles which then split into capillaries, decreasing arterial pressure because the total volume of the vessel increased
The branching of arteries into capillaries therefore ensures blood is moving slowly and all cells are located near a blood supply
After material exchange has occurred, capillaries will transfer their blood to venules which will turn into larger veins
How do capillaries have specialised structures in order to accomplish their task of material exchange? (4 points)
very small diameter which allows passage of only a single red blood cell at a time (optimal exchange)
The capillary wall is made of a single layer of cells to minimise the diffusion distance for permeable materials
They are surrounded by a membrane which is permeable to necessary materials
They may contain pores to further aid in the transport of materials between tissue fluid and blood
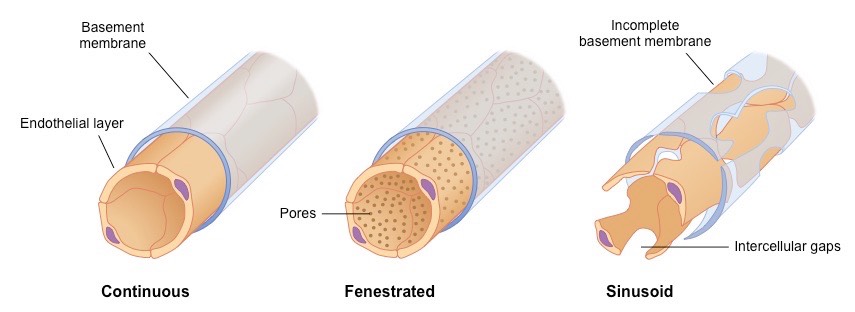
How can capillaries’ structure vary ?
The capillary wall may be continuous with endothelial cells held together by tight junctions to limit permeability of large molecules
In tissues specialised for absorption (e.g. intestines, kidneys), the capillary wall may be fenestrated (contains pores)
Some capillaries are sinusoidal and have open spaces between cells to be permeable to large molcules and cells (e.g. in liver)
Blood flows through the capillaries…. to allow for…..
Blood flows through the capillaries very slowly and at a very low pressure in order to allow for maximal material exchange.
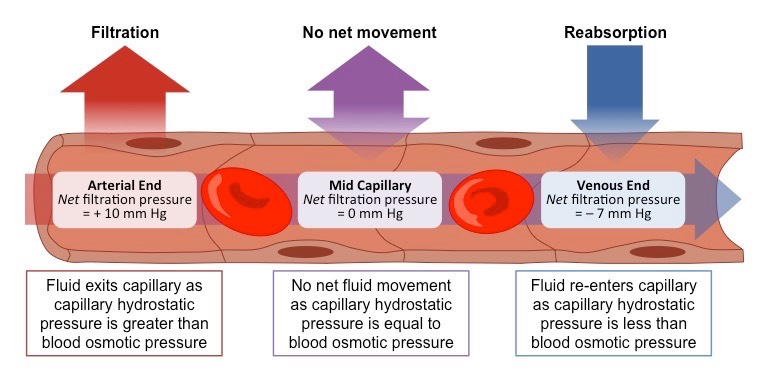
Consequence of higher hydrostatic pressure at the arteriole end of the capillary?
This forces material from the bloodstream into the tissue fluid
Material that exits the capillaries into the cells include oxygen and nutrients (needed by the cells for respiration)
Consequence of the lower hydrostatic pressure at the venule end of the capillary?
This allows materials from the tissues to enter the bloodstream.
Materials that enters the capillaries from cells include carbon dioxide and urea (wastes produced by the cells)
Material Exchange in the Capillaries
What is the function of veins?
to collect the blood from the tissues and move it at low pressure to the atria of the heart
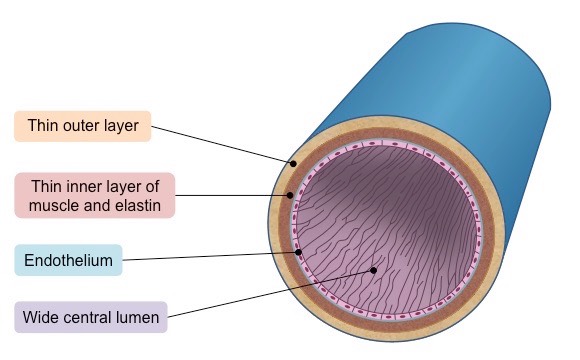
How do veins have a specialised structure to accomplish their task?
They have a very wide lumen (relative to wall thickness) to maximise blood flow for more effective return
They have a thin wall containing less muscle and elastic fibres as blood is flowing at a very low pressure (~ 5 – 10 mmHg)
Because the pressure is low, veins possess valves to prevent backflow and stop the blood from pooling at the lowest points
Role of valves in veins / why
Blood is at very low pressure in the veins which can make it difficult for the blood to move against the downward force of gravity
The veins contain numerous one-way valves in order to maintain the circulation of blood by preventing backflow
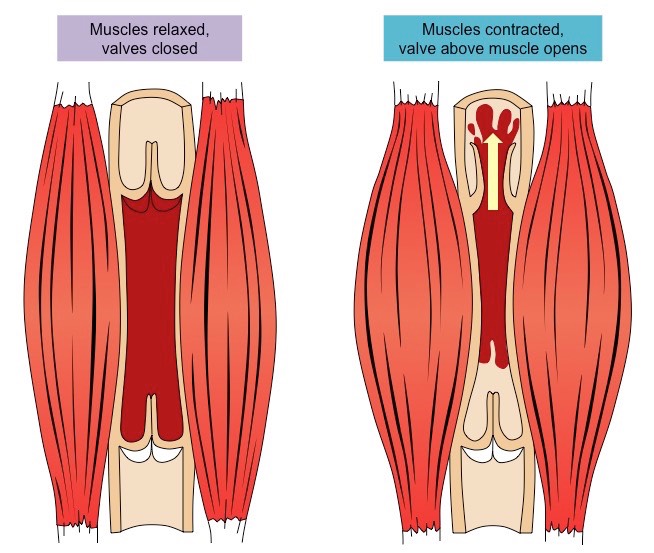
The role of skeletal muscles in venous blood flow
Veins typically pass between skeletal muscle groups, which facilitate venous blood flow via periodic contractions
When the skeletal muscles contract, they squeeze the vein and cause the blood to flow from the site of compression
Veins typically run parallel to arteries, and a similar effect can be caused by the rhythmic arterial bulge created by a pulse
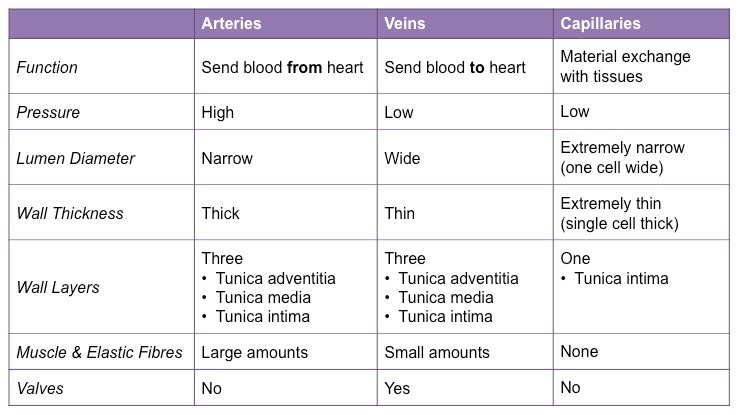
Difference in structure in arteries, capillaries and veins and how is it attributed to their respective functions?
Arteries have thick walls and narrow lumens because they transport blood at high pressure
Capillaries have walls that are only a single cell thick because they exchange materials between blood and tissue
Veins have thin walls with wide lumens and valves because they transport blood at low pressure
Comparison of blood vessel structure table
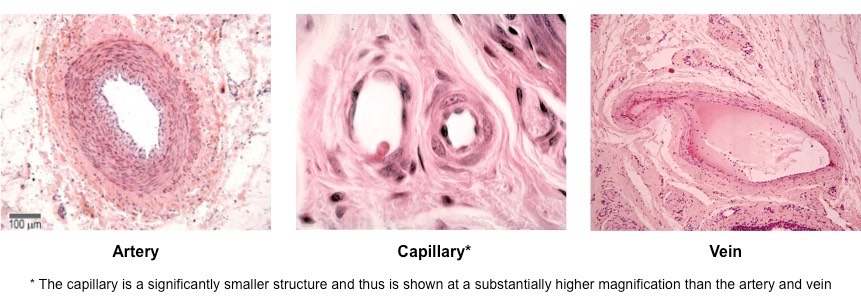
How can the different blood vessels be identified?
Arteries have thick walls composed of three distinct layers
Veins have thin walls but typically have wider lumen (lumen size may vary depending on specific artery or vein)
Capillaries are very small and will not be easily detected under the same magnification as arteries and veins
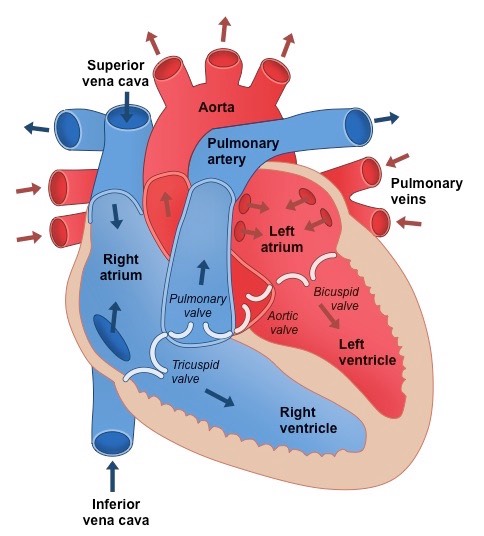
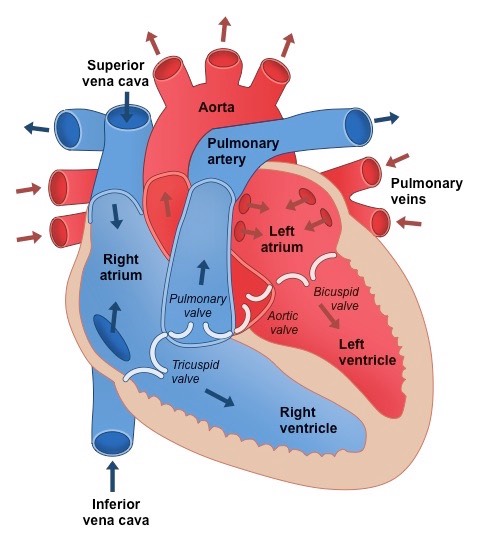
How to identify heart structure from an image?
A heart is labelled as it would appear in a chest, so the left side of an image represents the right side of the heart (and vice versa)
The left ventricle pumps blood around the entire body and so has a noticeably thicker myocardium than the right ventricle
Diagram of a human heart
3 key components of human heart structure? C HV BV
chambers
heart valves
blood vessels
Heart chambers - what are they made up of?
Two atria (singular = atrium) – smaller chambers near top of heart that collect blood from body and lungs
Two ventricles – larger chambers near bottom of heart that pump blood to body and lungs
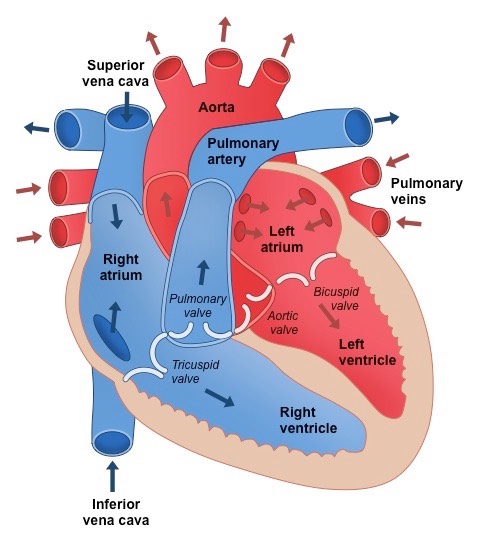
Heart Valves - what are they made up of?
Atrioventricular valves (between atria and ventricles) – bicuspid valve on left side ; tricuspid valve on right side
Semilunar valves (between ventricles and arteries) – aortic valve on left side ; pulmonary valve on right side
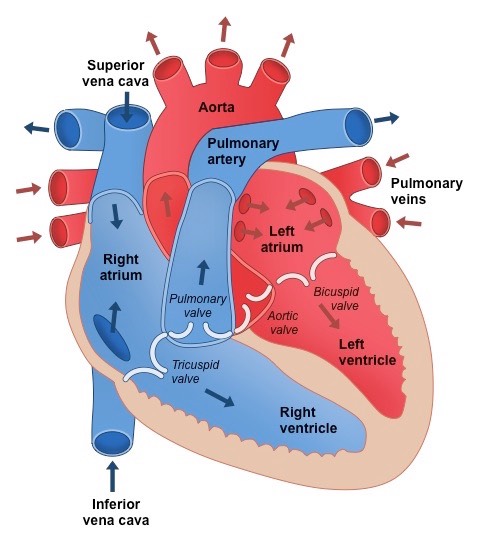
Heart blood valves - what are they made up of?
Vena cava (inferior and superior) feeds into the right atrium and returns deoxygenated blood from the body
Pulmonary artery connects to the right ventricle and sends deoxygenated blood to the lungs
Pulmonary vein feeds into the left atrium and returns oxygenated blood from the lungs
Aorta extends from the left ventricle and sends oxygenated blood around the body
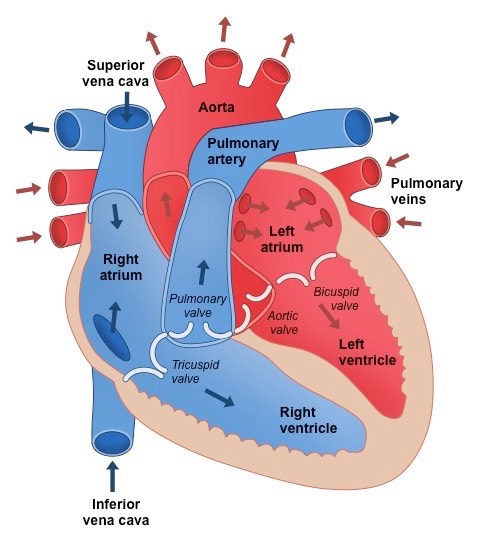
Why is the contration of the heart known as myogenic
This means that the signal for cardiac compression arises within the heart tissue itself
In other words, the signal for a heart beat is initiated by the heart muscle cells (cardiomyocytes) rather than from brain signals
What directs the contraction of heart muscle tissue?
A cluster of heart muscle cells that are collectively called the sinoatrial node (SA node or SAN)
found within the wall of the right atrium
How does the sinoatrial node act as a primary pacemaker?
By controlling the rate at which the heart beats (i.e. pace ‘making’)
The SA node triggers roughly 60 – 100 cardiac contractions per minute
What happens if the SA node fails?
a secondary pacemaker (AV node) may maintain cardiac contractions at roughly 40 – 60 bpm
If both fail, a final tertiary pacemaker (Bundle of His) may coordinate contractions at a constant rate of roughly 30 – 40 bpm
What happens when the pacemakeres are not working? and what needs to happen after
This will lead to the irregular and uncoordinated contraction of the heart muscle (fibrillation)
When fibrillation occurs, normal sinus rhythm may be re-established with a controlled electrical current (defibrillation)
Role of a pacemaker recap.
No pacemaker = cardiac cells act independently
Pacemaker = cardiac cells act in unison
Steps for the electrical conduction of a heart beat?
The sinoatrial node sends out an electrical impulse that stimulates contraction of the myocardium (heart muscle tissue)
This impulse directly causes the atria to contract and stimulates another node at the junction between the atrium and ventricle
This second node – the atrioventricular node (AV node) – sends signals down the septum via a nerve bundle (Bundle of His)
The Bundle of His innervates nerve fibres (Purkinje fibres) in the ventricular wall, causing ventricular contraction
Delay between atrial and ventricular contractions - what does it allow for?
caused by the steps for the electrical conduction of a heart beat
results in two heart sounds
This delay allows time for the ventricles to fill with blood following atrial contractions so as to maximise blood flow
How can the heart rate be regulated? other than pacemakers (2 ways)
While the basal heart rate is determined within the heart by the pacemaker, it can be regulated by external signals
Nerve signals from the brain can trigger rapid changes, while endocrine signals can trigger more sustained changes
Changes to blood pressure levels or CO2 concentrations (and thereby blood pH) will trigger changes in heart rate
How is the pacemaker controlled?
The pacemaker is under autonomic (involuntary) control from the brain, specifically the medulla oblongata (brain stem)
How does the medulla oblangata regulate heart rate?
Two nerves connected to the medulla regulate heart rate by either speeding it up or slowing it down:
The sympathetic nerve releases the neurotransmitter noradrenaline (a.k.a. norepinephrine) to increase heart rate
The parasympathetic nerve (vagus nerve) releases the neurotransmitter acetylcholine to decrease heart rate
What are hormones?
Hormones are chemical messengers released into the bloodstream that act specifically on distant target sites (like the heart)
How does the heart rate prepare for vigorous physical activity?
The heart rate can undergo a sustained increase in response to hormonal signalling
The hormone adrenaline (a.k.a. epinephrine) is released from the adrenal glands (located above the kidneys)
Adrenaline increases heart rate by activating the same chemical pathways as the neurotransmitter noradrenaline
Regulation of heart rate diagram
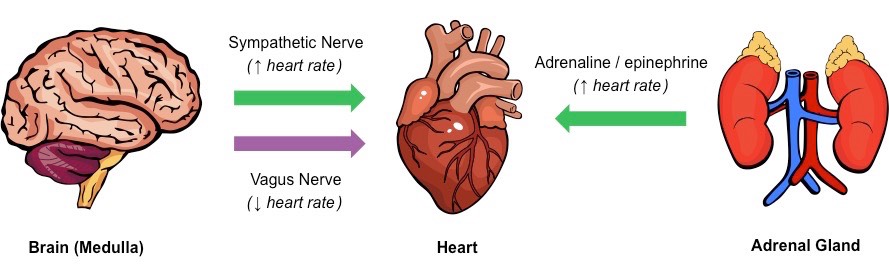
What is the cardiac cycle? what 2 main parts does it consist of
The cardiac cycle describes the series of events that take place in the heart over the duration of a single heart beat
It is comprised of a period of contraction (systole) and relaxation (diastole)
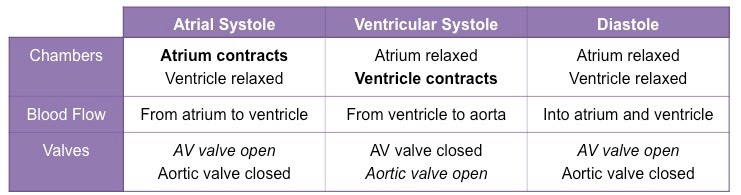
What is the process of systole?
Blood returning to the heart will flow into the atria and ventricles as the pressure in them is lower than the surroundings (due to low volume of blood)
When ventricles are ~70% full, atria will contract (atrial systole), increasing pressure in the atria and forcing blood into ventricles
As ventricles contract, ventricular pressure exceeds atrial pressure and AV valves close to prevent back flow (first heart sound)
With both sets of heart valves closed, pressure rapidly builds in the contracting ventricles (isovolumetric contraction)
When ventricular pressure exceeds blood pressure in the aorta, the aortic valve opens and blood is released into the aorta
What is the process of diastole?
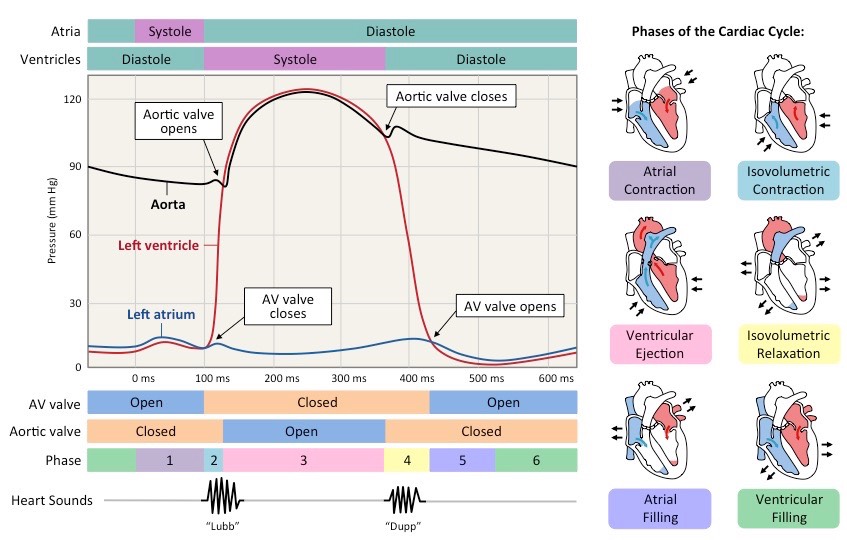
As blood exits the ventricle and travels down the aorta, ventricular pressure decreases
When ventricular pressure drops below aortic pressure, the aortic valve closes to prevent back flow (second heart sound)
When the ventricular pressure drops below the atrial pressure, the AV valve opens and blood can flow from atria to ventricle
Throughout the cycle, aortic pressure remains quite high as muscle and elastic fibres in the artery wall maintain blood pressure
Overview of Cardiac Cycle Events
Pressure Changes in Left Side of Heart During the Cardiac Cycle diagram
Role of coronary arteries
Blood pumped through the heart is at high pressure and cannot be used to supply the heart muscle with oxygen and nutrients
Coronary arteries are the blood vessels that surround the heart and nourish the cardiac tissue to keep the heart working
What happens if coronary arteries become occluded (blocked, closed-up)
the region of heart tissue nourished by the blocked artery will die and stop functioning
What is the cause of coronary oclusion?
Atherosclerosis - the hardening and narrowing of the arteries due to the deposition of cholesterol
Atherosclerosis process
Atheromas (fatty deposits) develop in the arteries and significantly reduce the diameter of the lumen (stenosis)
The restricted blood flow increases pressure in the artery, leading to damage to the arterial wall (from shear stress)
The damaged region is repaired with fibrous tissue which significantly reduces the elasticity of the vessel wall
As the smooth lining of the artery is progressively degraded, lesions (damage or abnormal change in the tissue) form called atherosclerotic plaques
If the plaque ruptures, blood clotting is triggered, forming a thrombus that restricts blood flow
If the thrombus is dislodged it becomes an embolus and can cause a blockage in a smaller arteriole
Consequences of atherosclerosis?
Atherosclerosis can lead to blood clots which cause coronary heart disease when they occur in coronary arteries
Myocardial tissue requires the oxygen and nutrients transported via the coronary arteries in order to function
If a coronary artery becomes completely blocked, an acute myocardial infarction (heart attack) will result
How is blockage of coronary arteries treated'?
Blockages of coronary arteries are typically treated by by-pass surgery or creating a stent (e.g. balloon angioplasty)
Risk Factors for Coronary Heart Disease?
Mnemonic: A Goddess
Age – Blood vessels become less flexible with advancing age
Genetics – Having hypertension predispose individuals to developing CHD
Obesity – Being overweight places an additional strain on the heart
Diseases – Certain diseases increase the risk of CHD (e.g. diabetes)
Diet – Diets rich in saturated fats, salts and alcohol increases the risk
Exercise – Sedentary lifestyles increase the risk of developing CHD
Sex – Males are at a greater risk due to lower oestrogen levels
Smoking – Nicotine causes vasoconstriction, raising blood pressure