BIOC 4331 Lecture 15
1/33
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
34 Terms
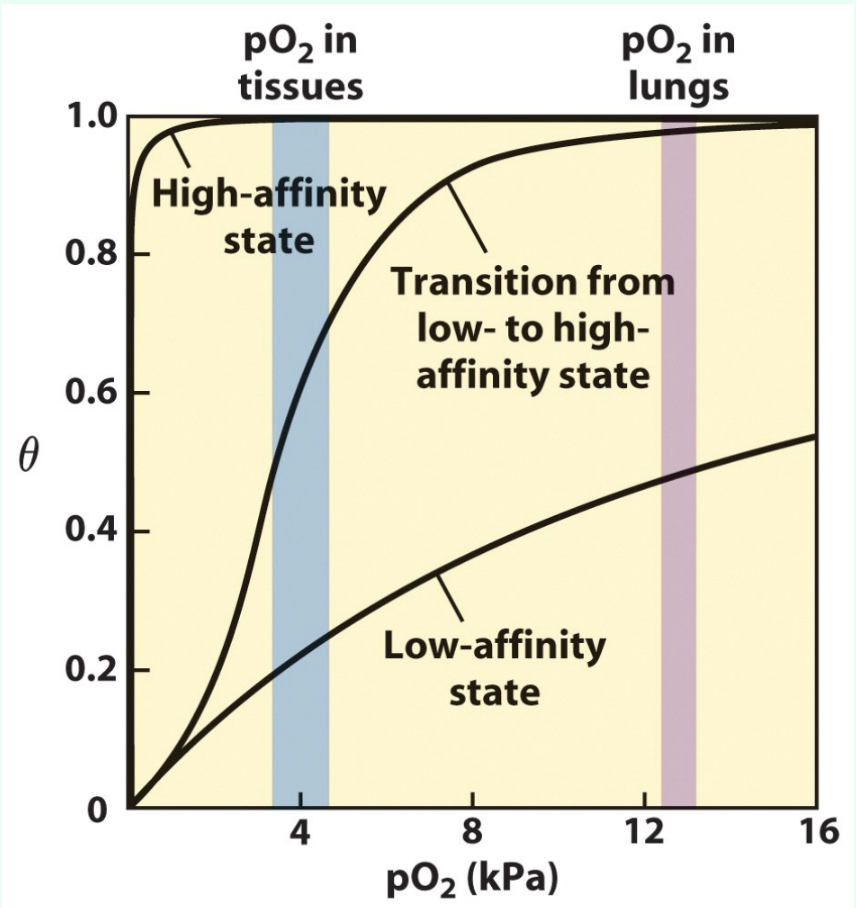
Do NOT mix these up: what is n vs nH?
n = number of binding sites
nH = Hill coefficient (degree of cooperativity).
What’s the key difference between Kd and P50?
Kd is global (encompasses all binding sites)
P50 is an average dissociation measure for each site
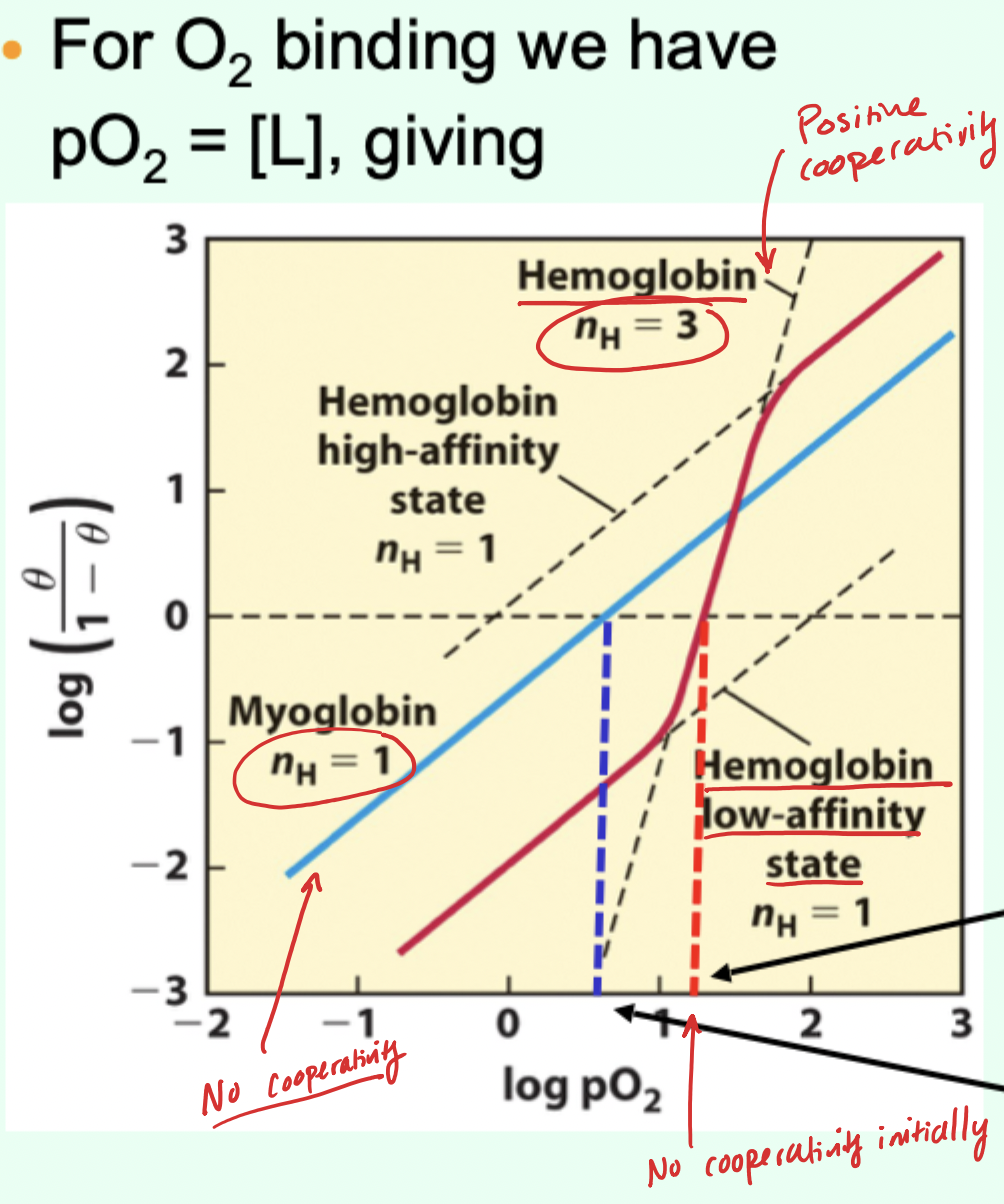
In a Hill plot, what is plotted on x-axis?
log[L] (free ligand concentration).
![<p><strong>log[L]</strong> (free ligand concentration).</p>](https://assets.knowt.com/user-attachments/17c29df9-ffc0-44ab-98c9-36985e239d22.png)
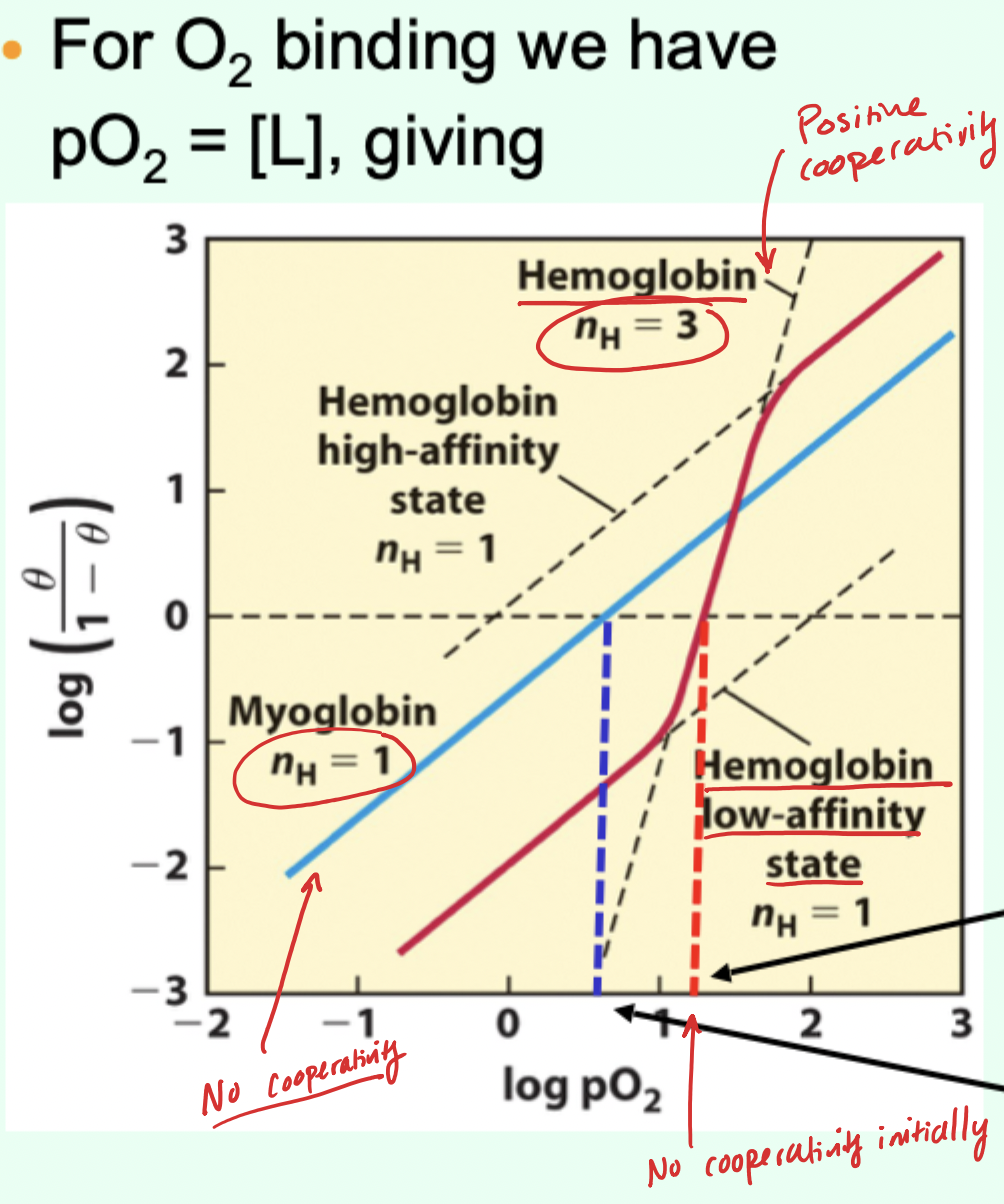
When the left side of the O2 Hill plot equation equals 0, what is pO2?
pO2 = P50.
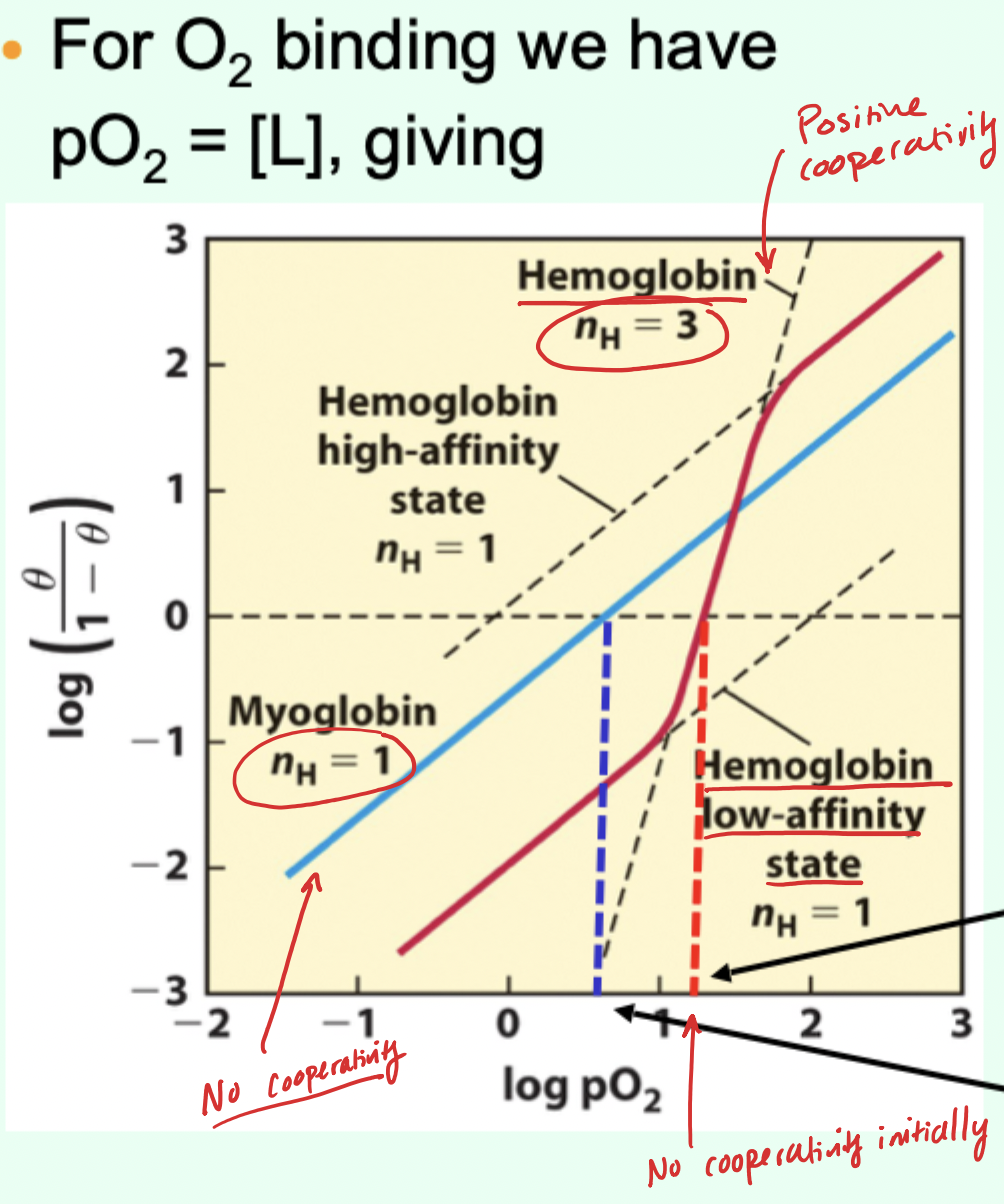
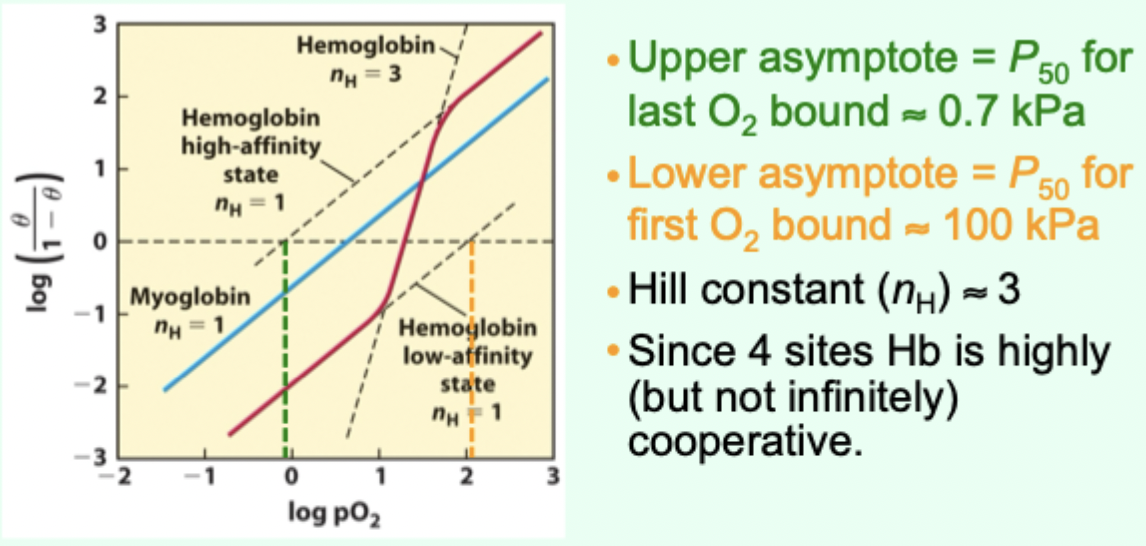
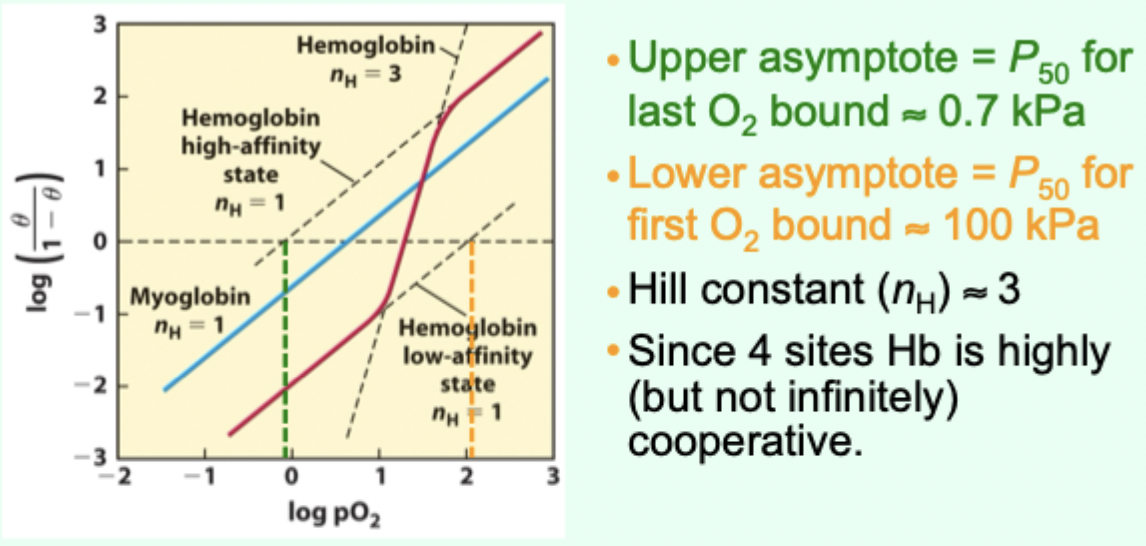
Why is hemoglobin “highly (but not infinitely) cooperative”?
It has 4 sites, but nH is ~3 (not 4).
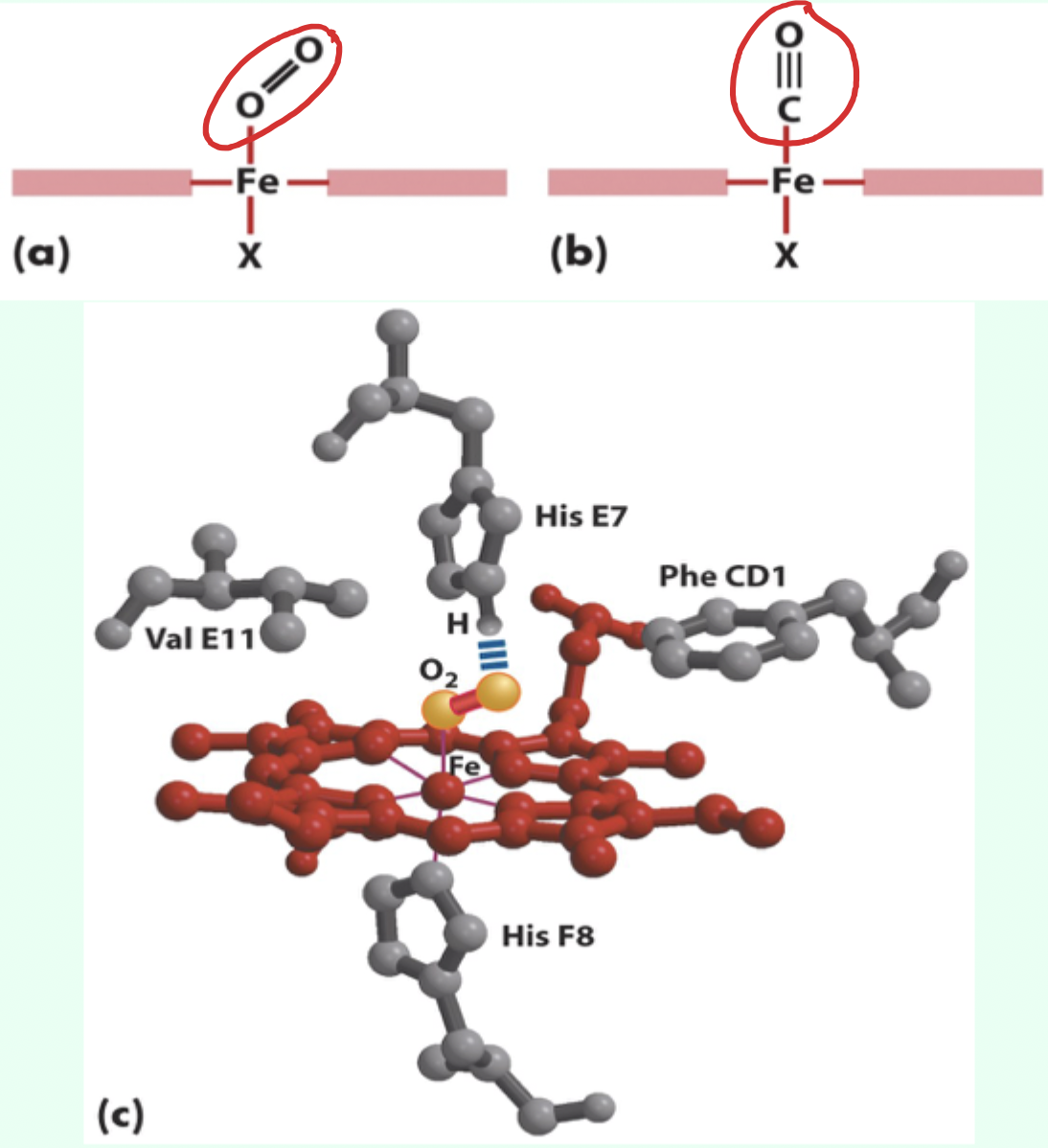
Free heme binds CO with what relative affinity vs O2?
~20,000× higher affinity than O2.
When heme is bound to Mb or Hb, how does CO affinity change?
Bound: Reduced ~100-fold; only ~200× (Mb) or ~250× (Hb) higher than O2.
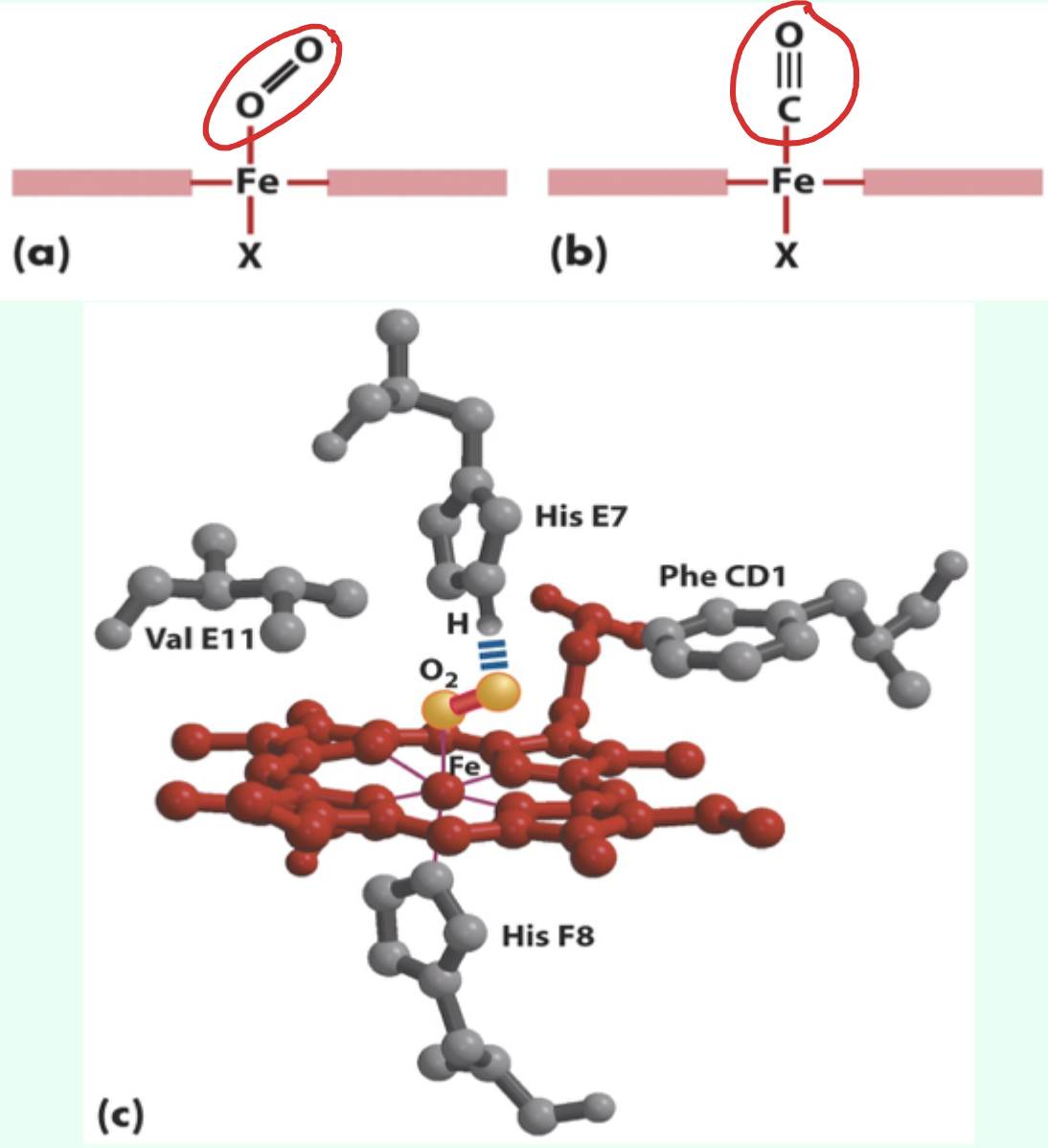
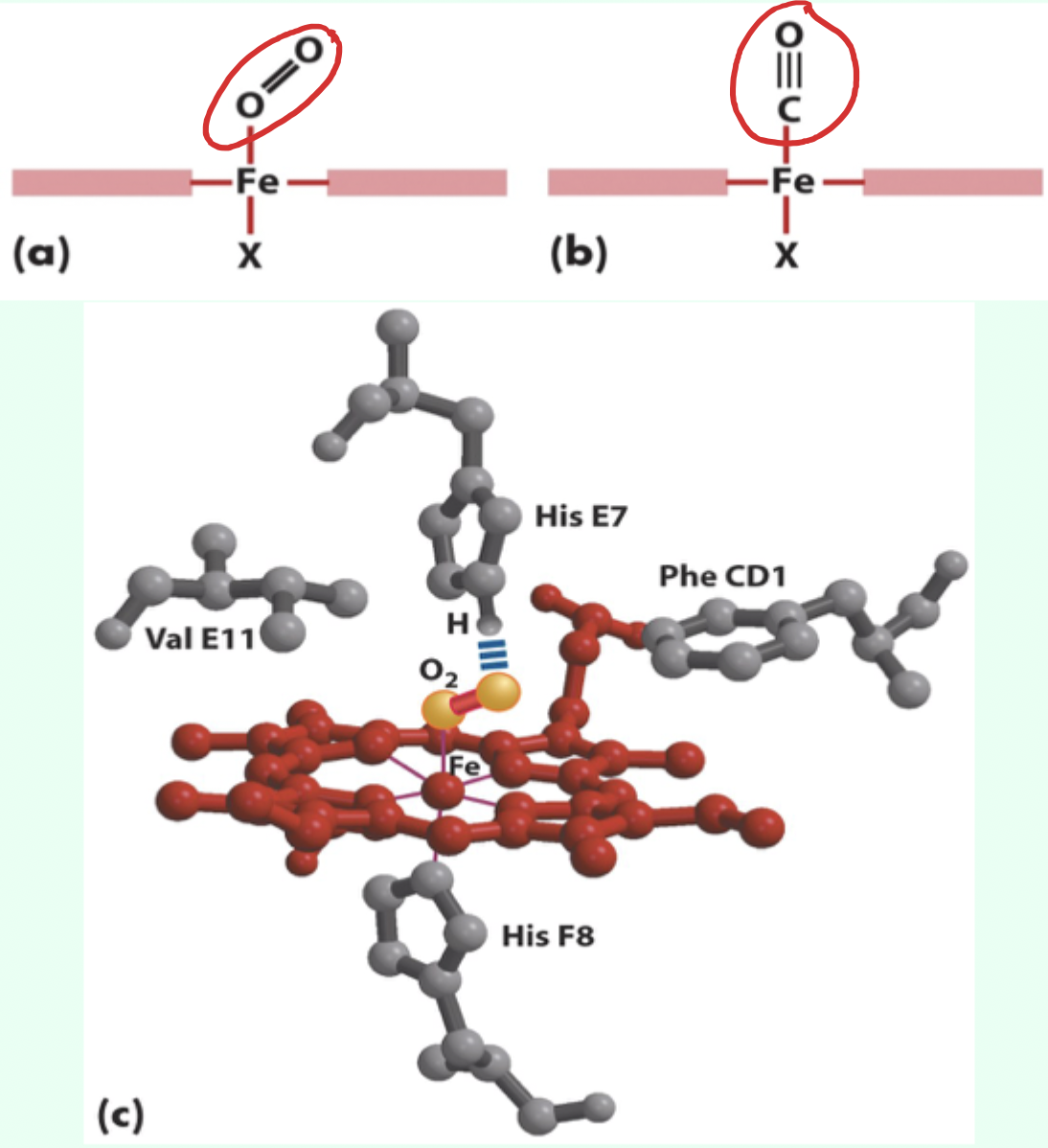
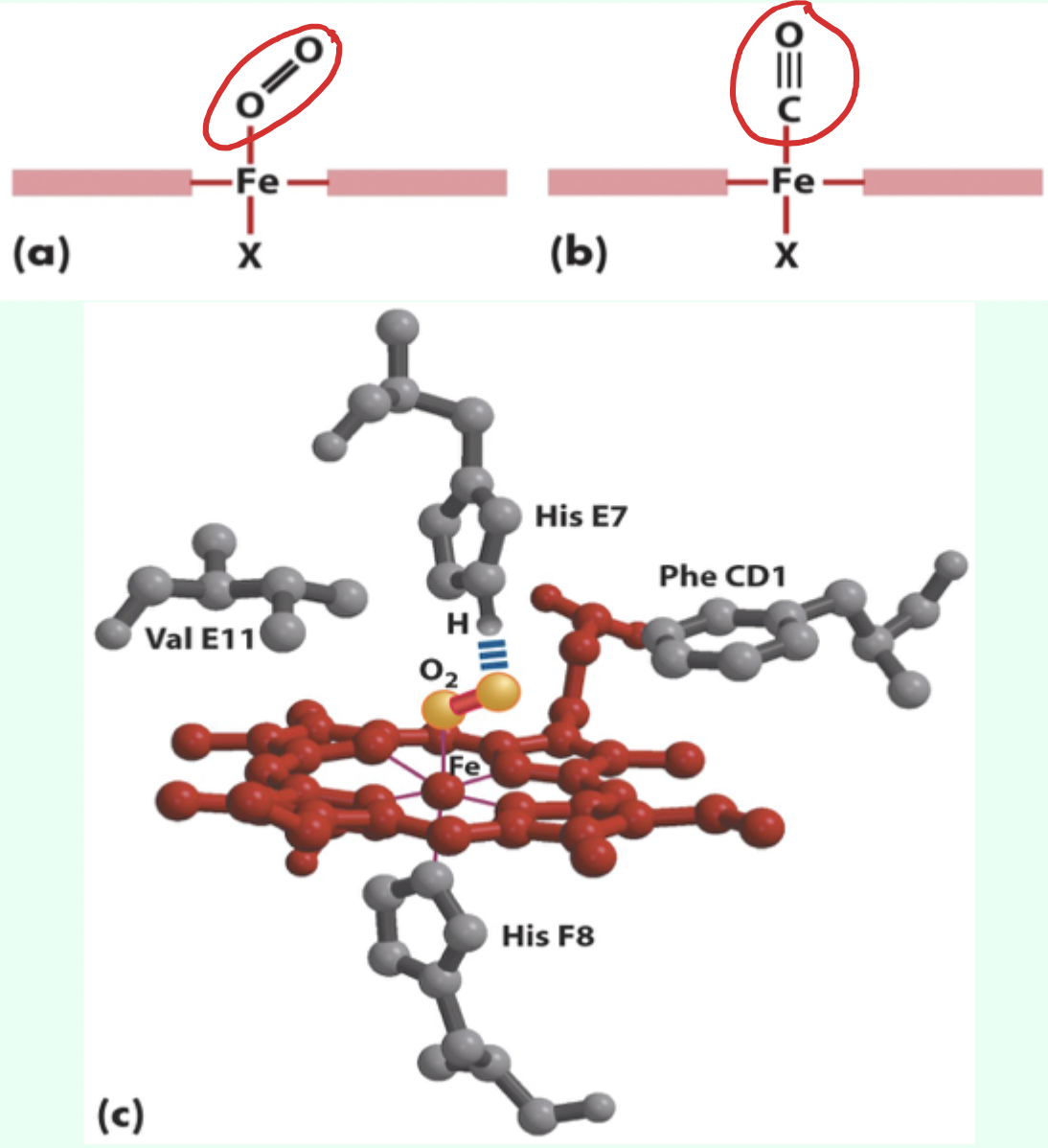
What residue causes steric hindrance affecting CO binding?
His (E7).
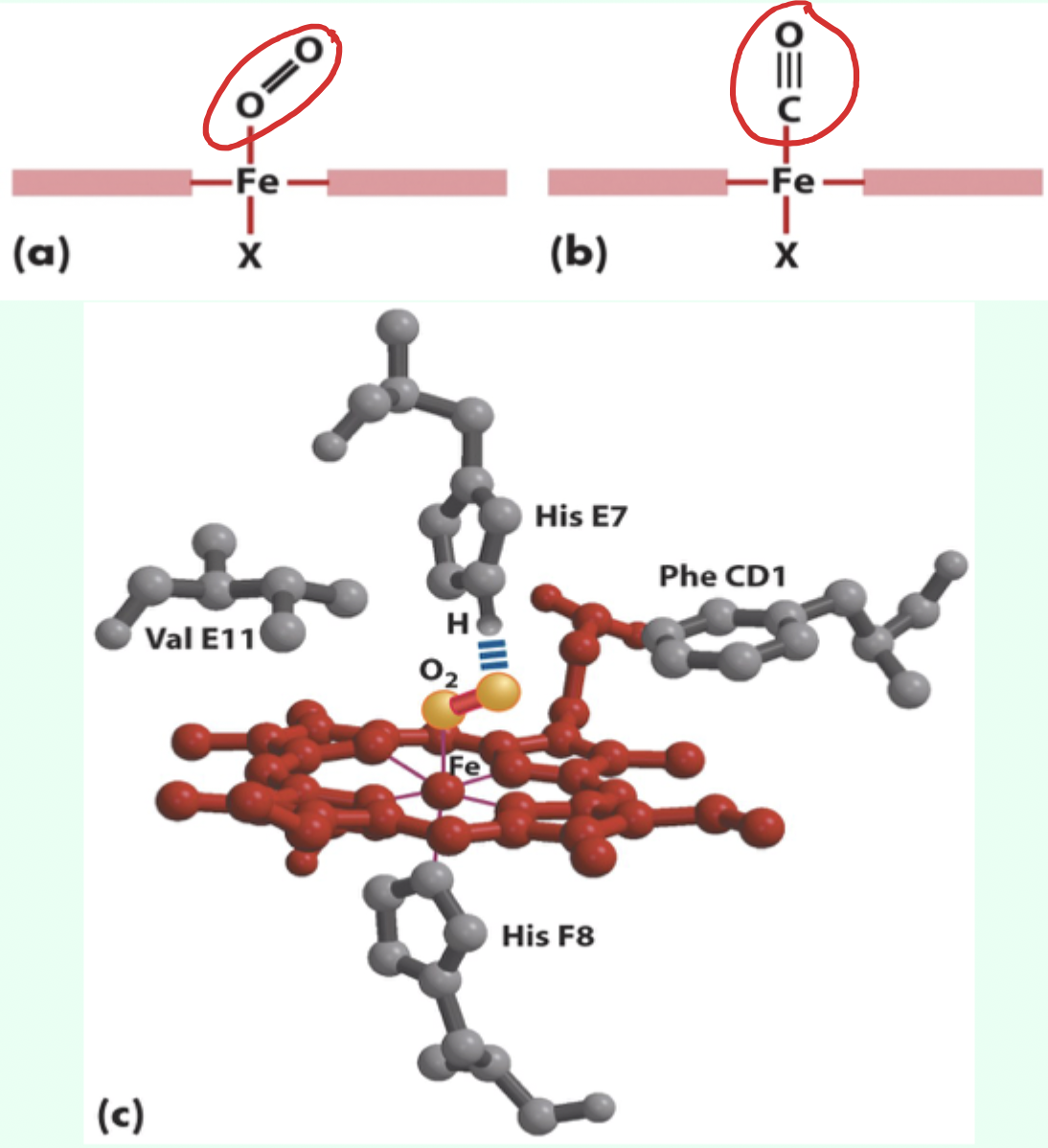
What exactly can’t CO do because of His (E7)?
CO cannot form its optimal linear conformation that maximizes orbital overlap.
CO poisoning: two main problems?
CO massively outcompetes O2 for binding sites.
CO bound to 1–2 Hb subunits increases O2 affinity of remaining subunits → very little O2 released at tissues.
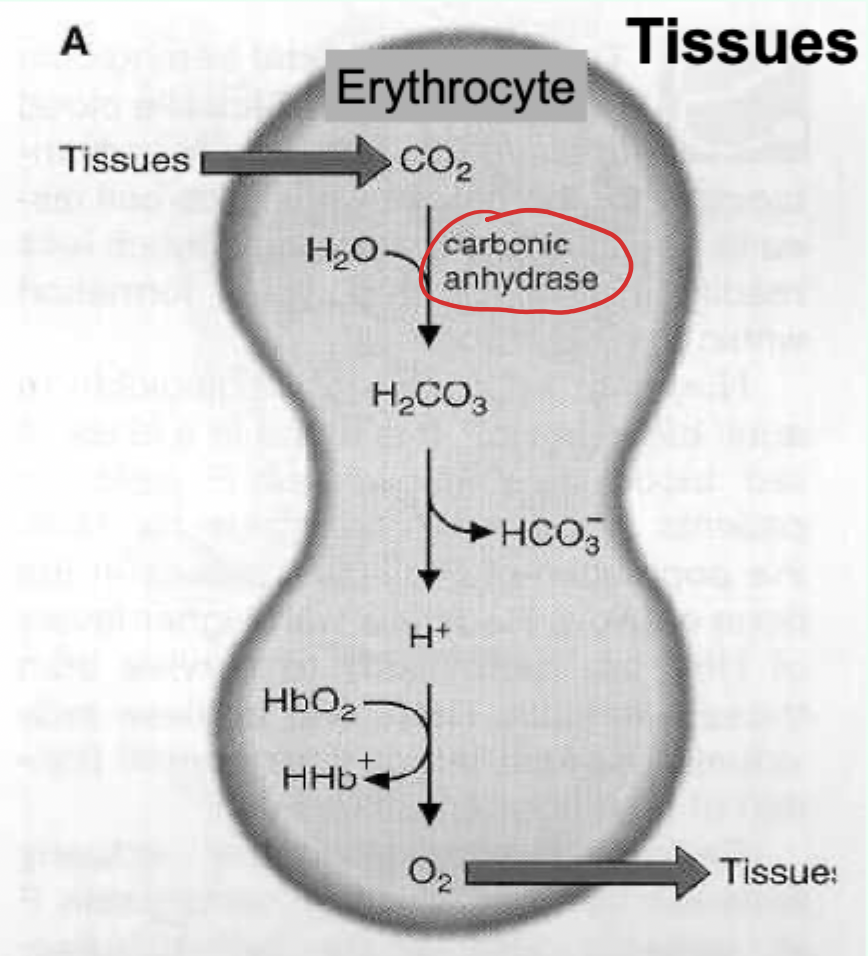
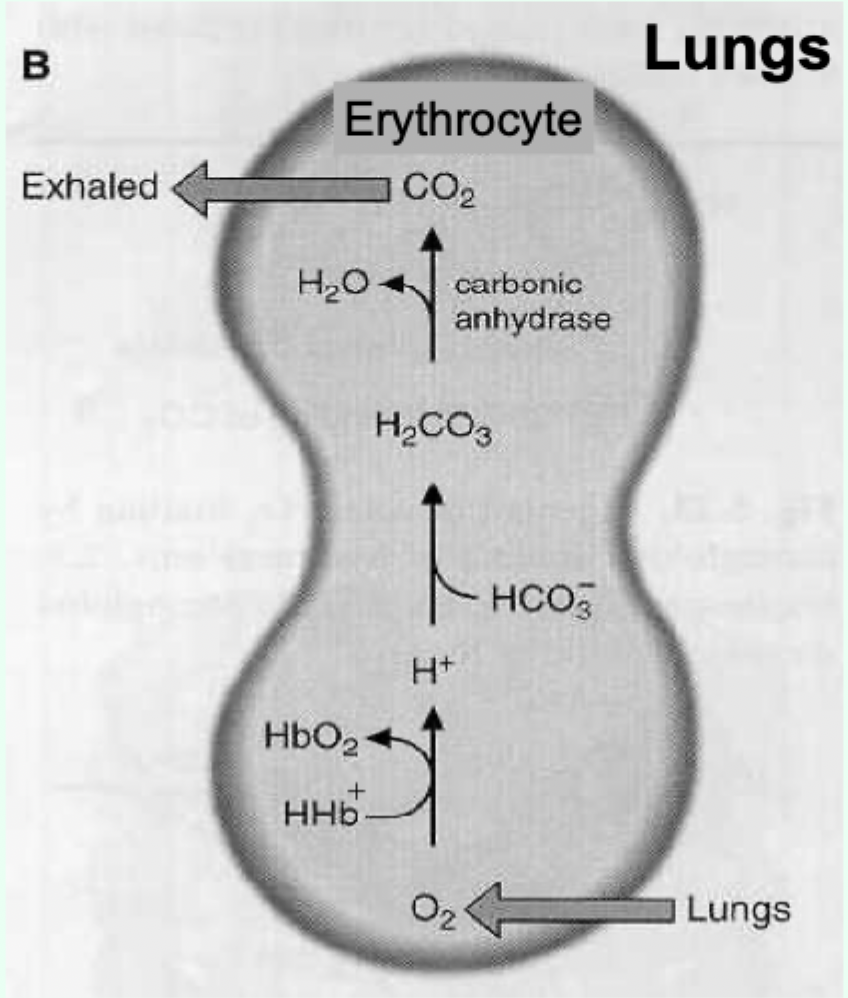
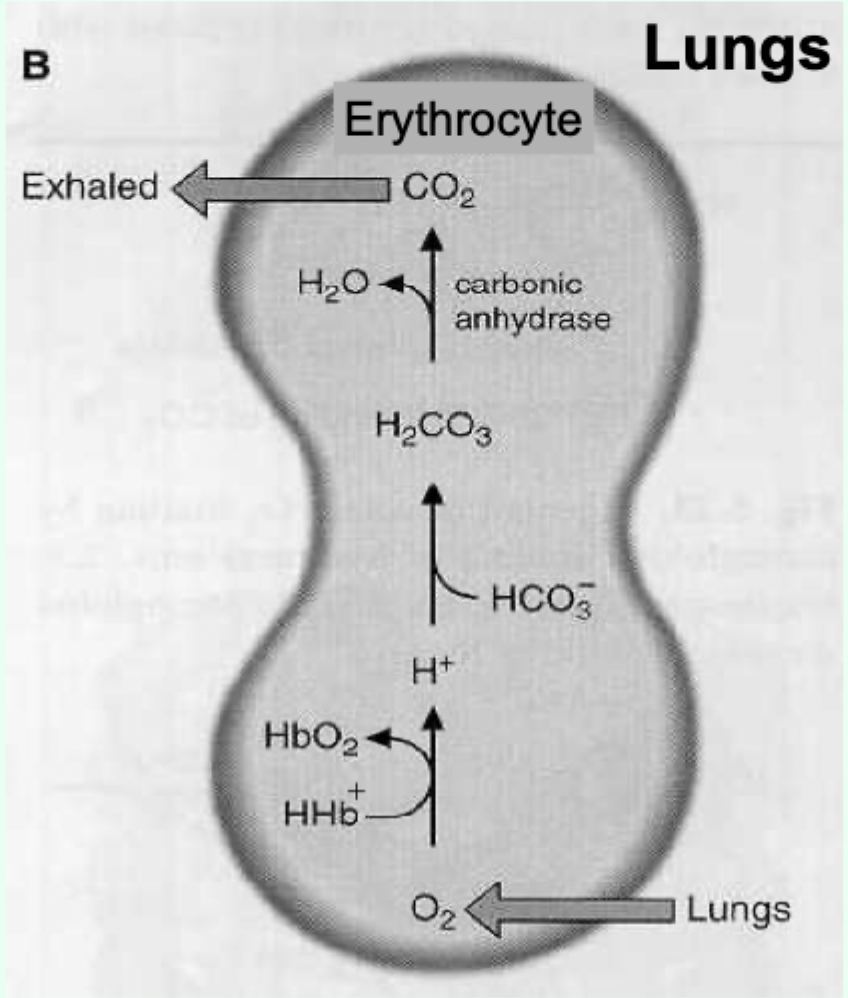
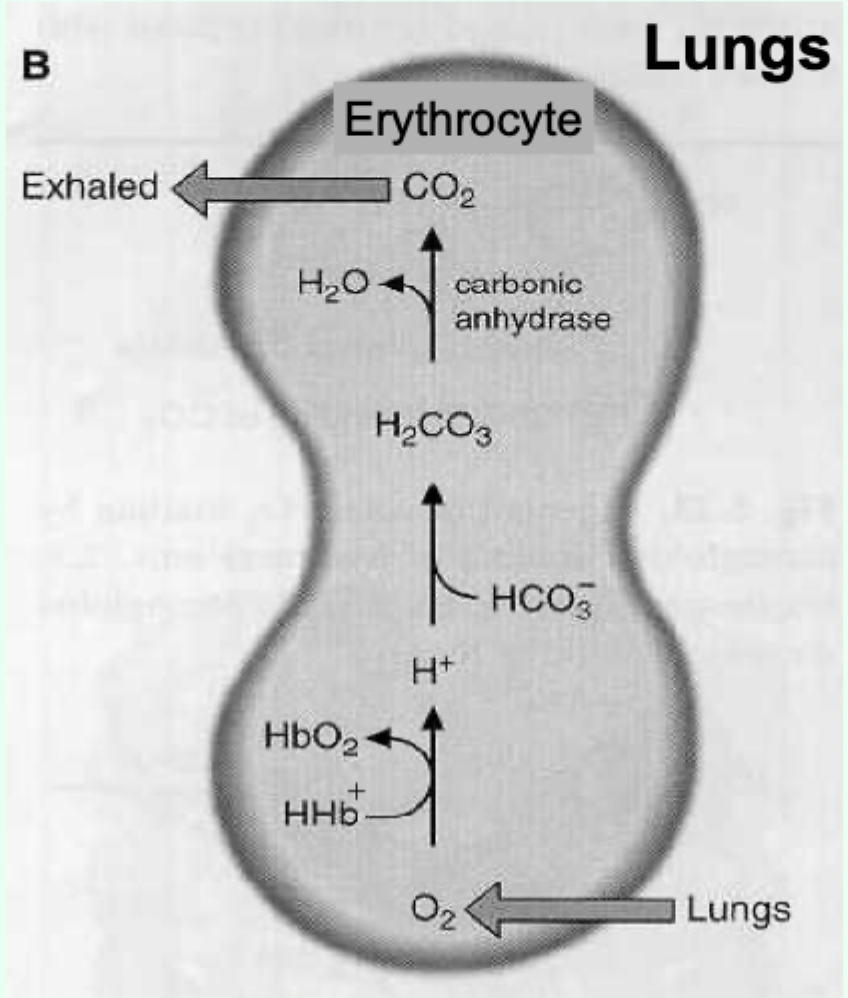
Bohr effect: what enzyme converts CO2 to carbonic acid in erythrocytes?
Carbonic anhydrase.
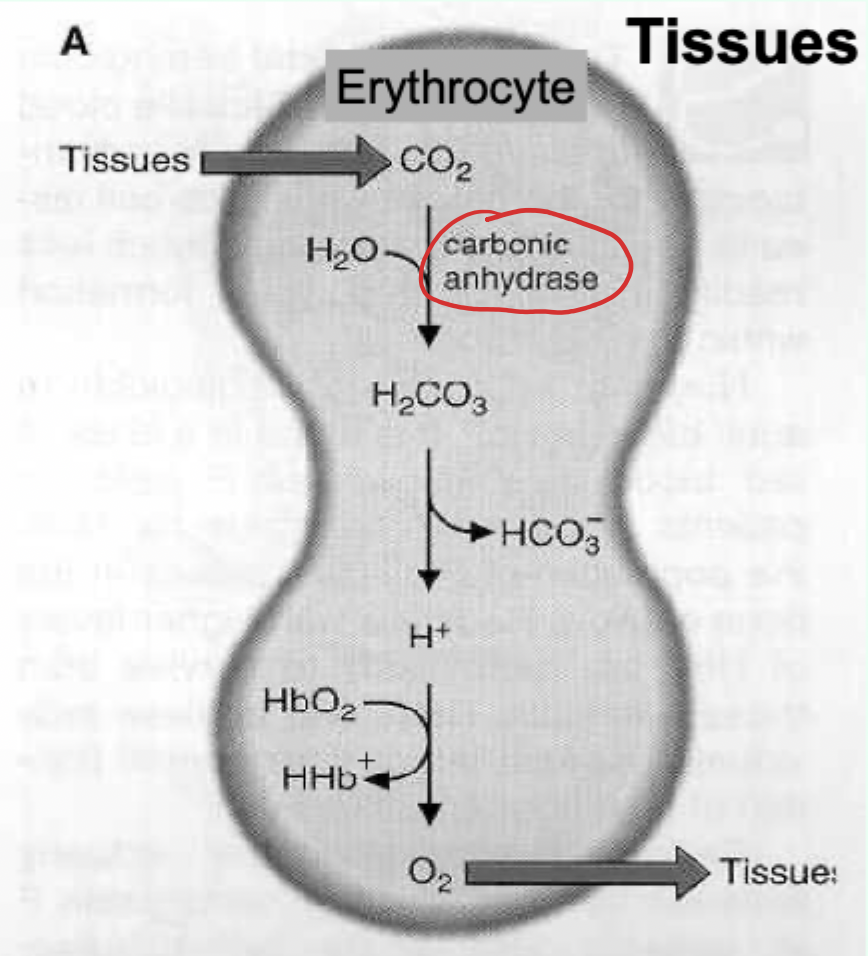
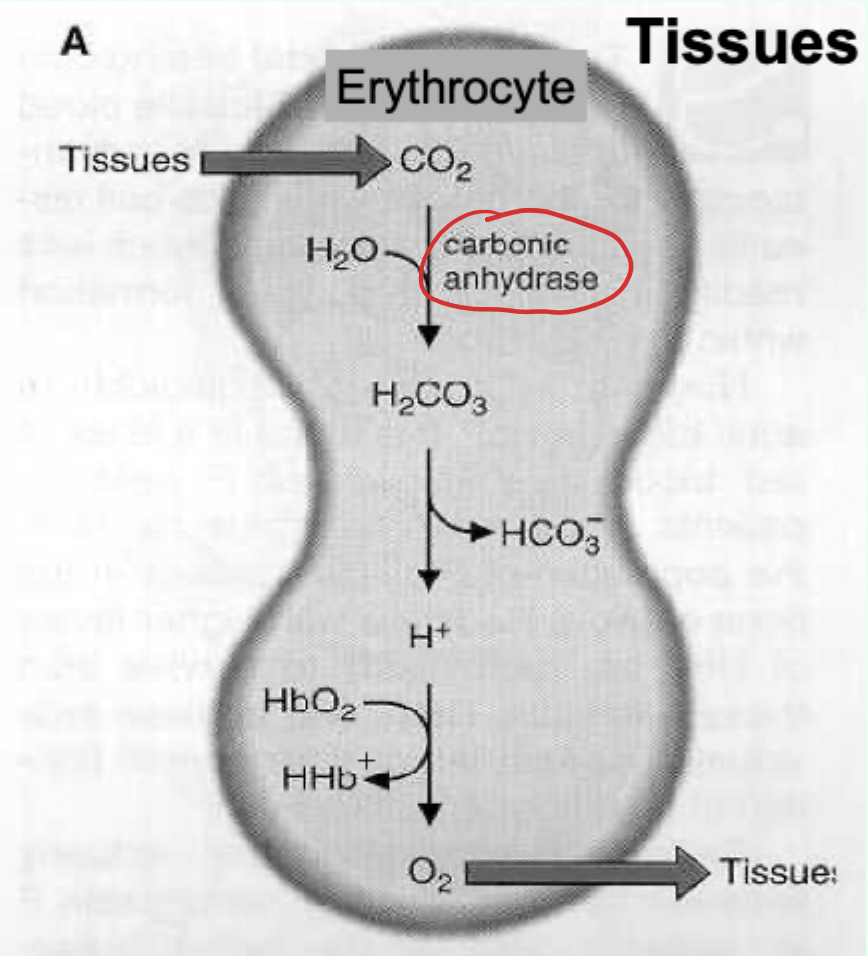
Key reaction (Bohr effect): CO2 hydration/dissociation.
CO2 + H2O ⇌ H2CO3 ⇌ H+ + HCO3−
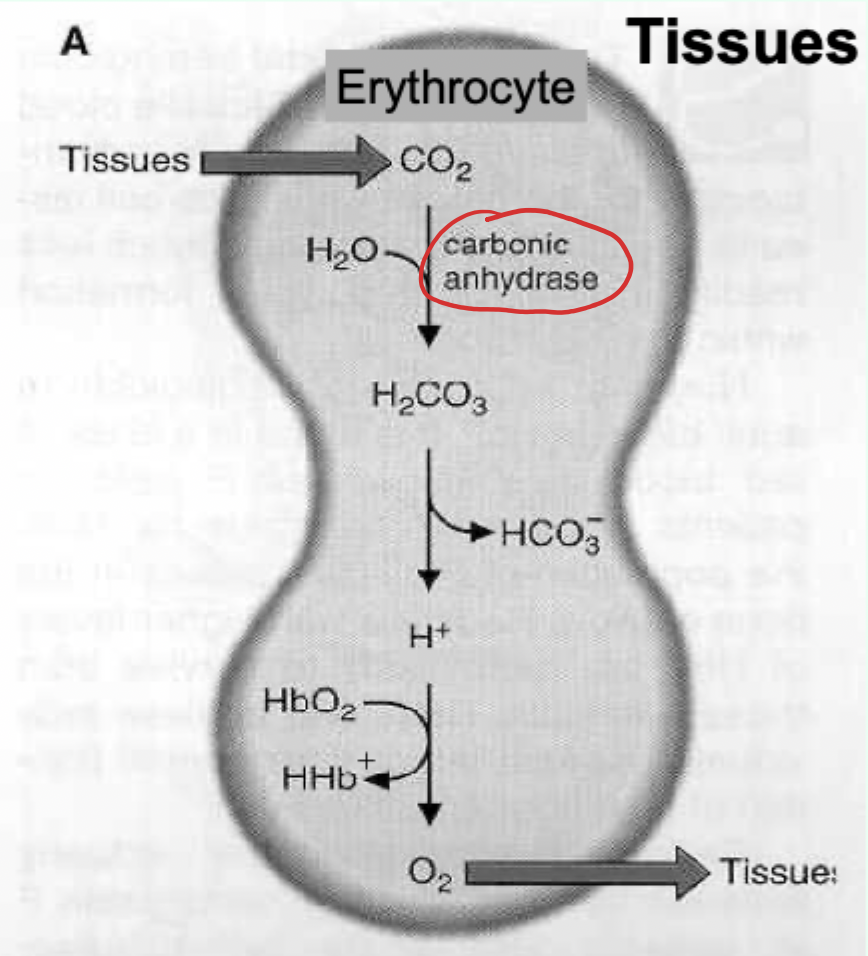
Bohr effect: what does increased H+ do to Hb’s behavior?
Favors T state and facilitates O2 release.
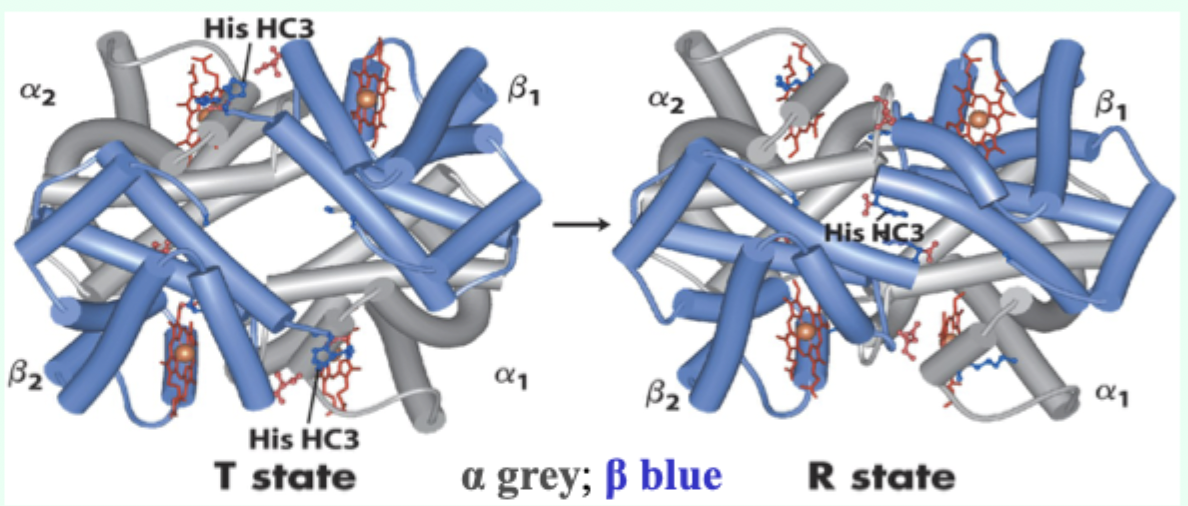
In the R state, what happens to that ion pair and pKa?
Ion pair absent; pKa drops.
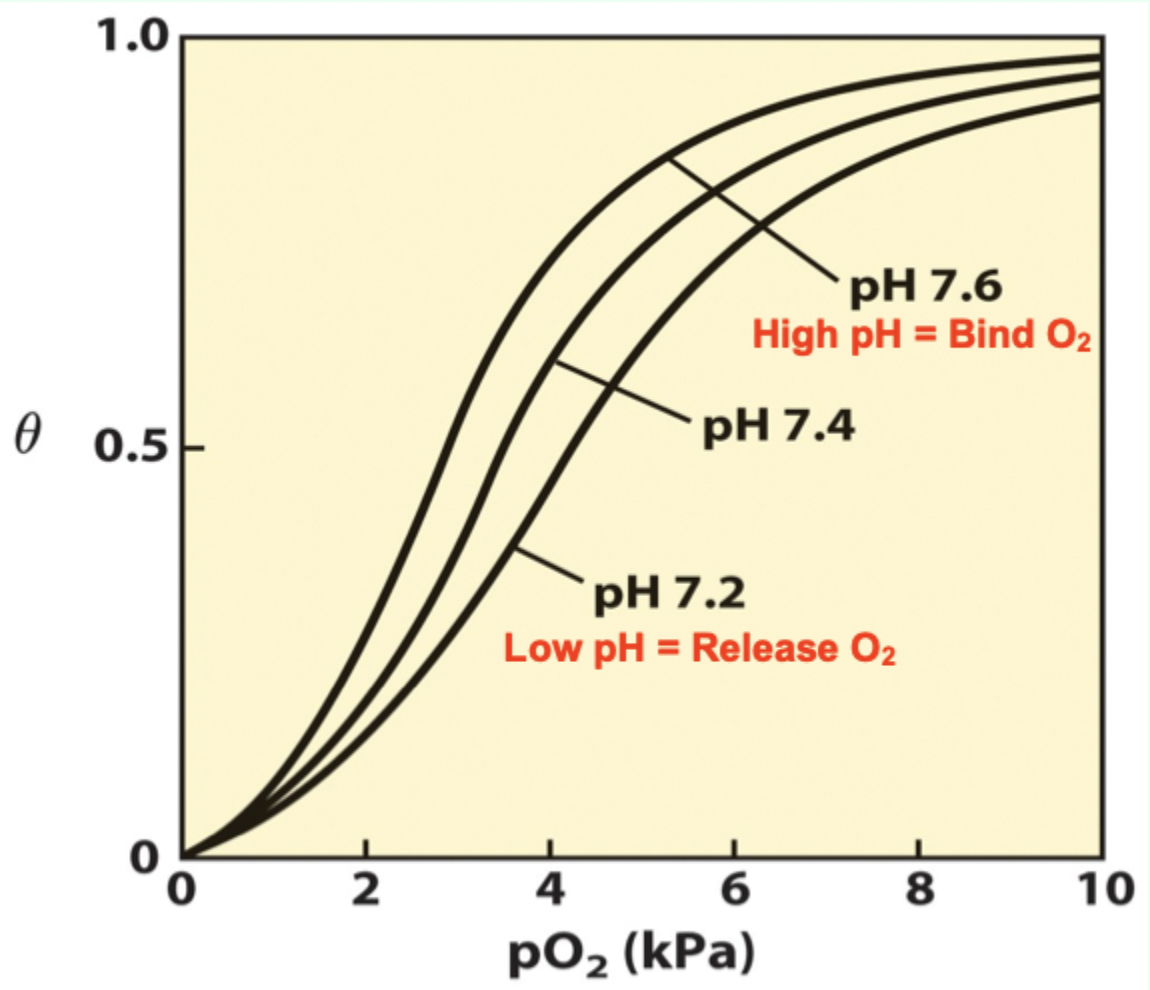
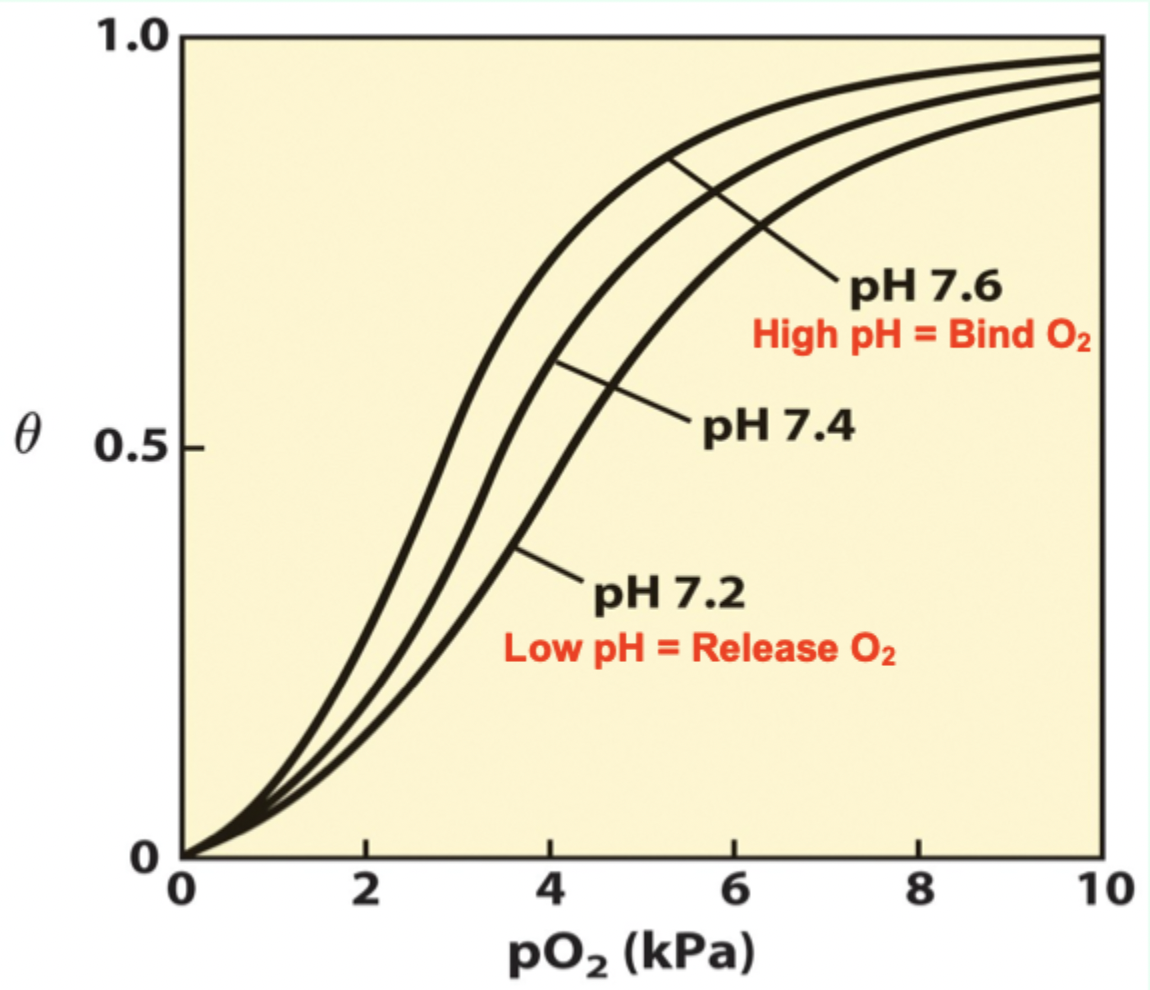
At pH 7.6 (lungs), Hb has…
Higher affinity for O2.
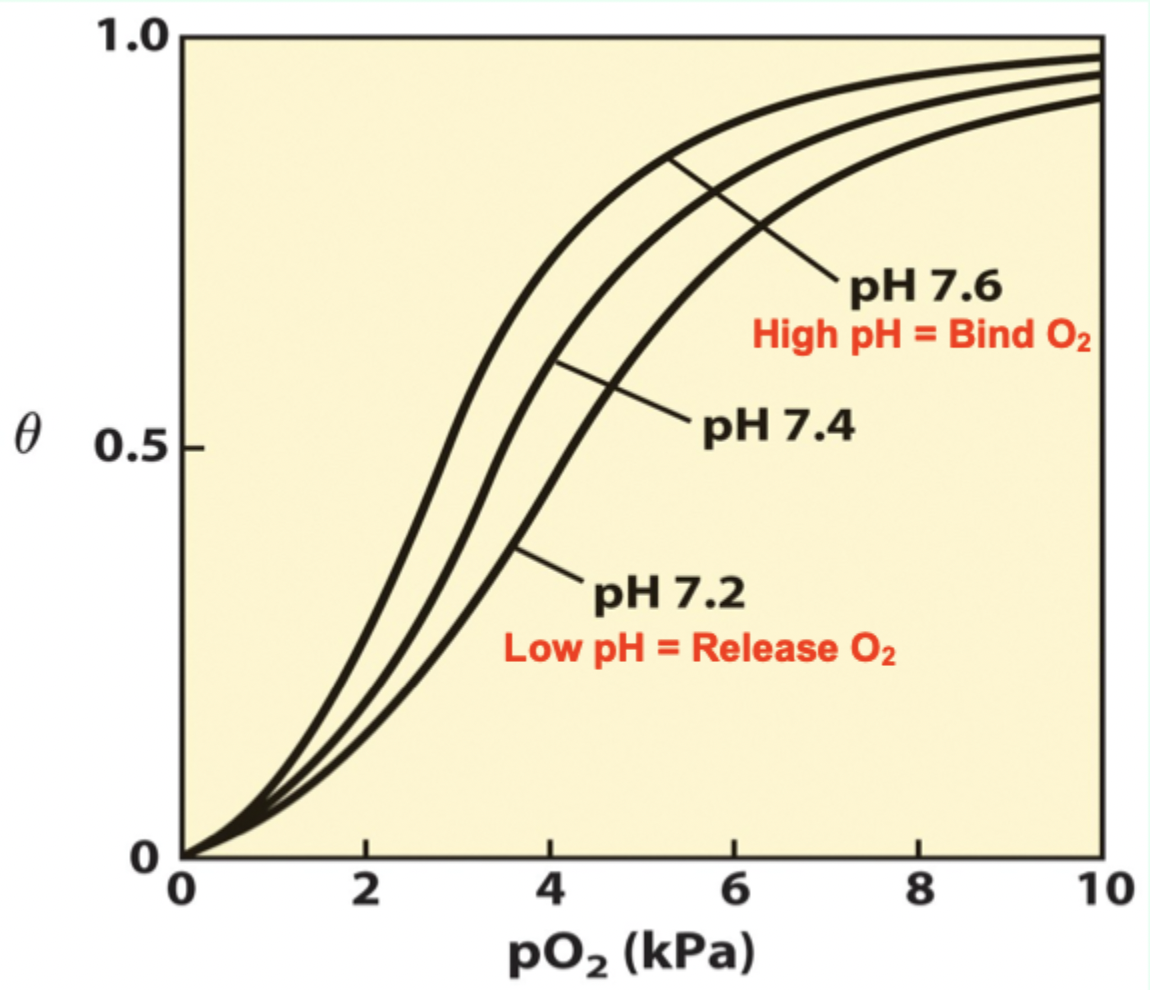
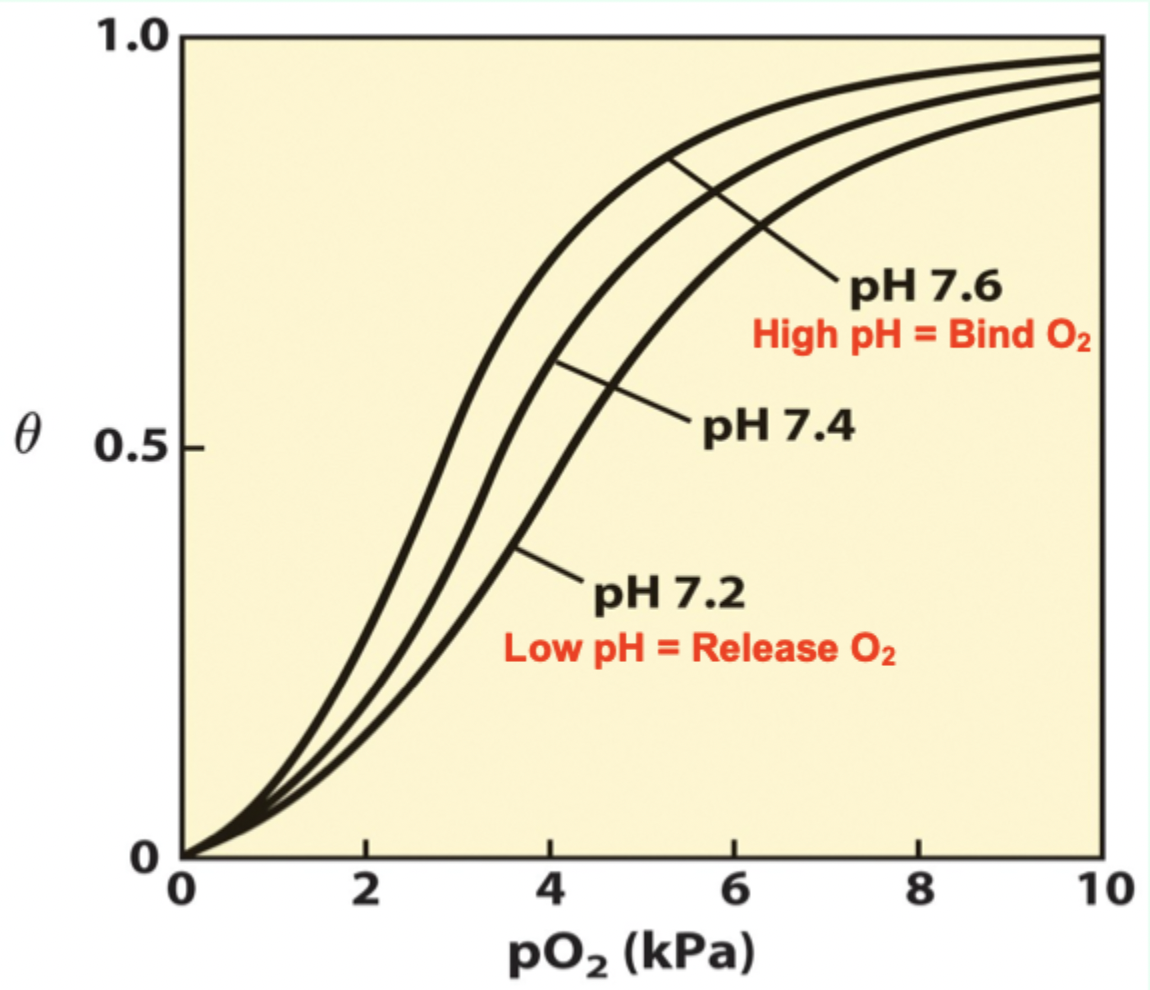
As pH drops in metabolizing tissues, what happens?
T state is favored → more O2 released.
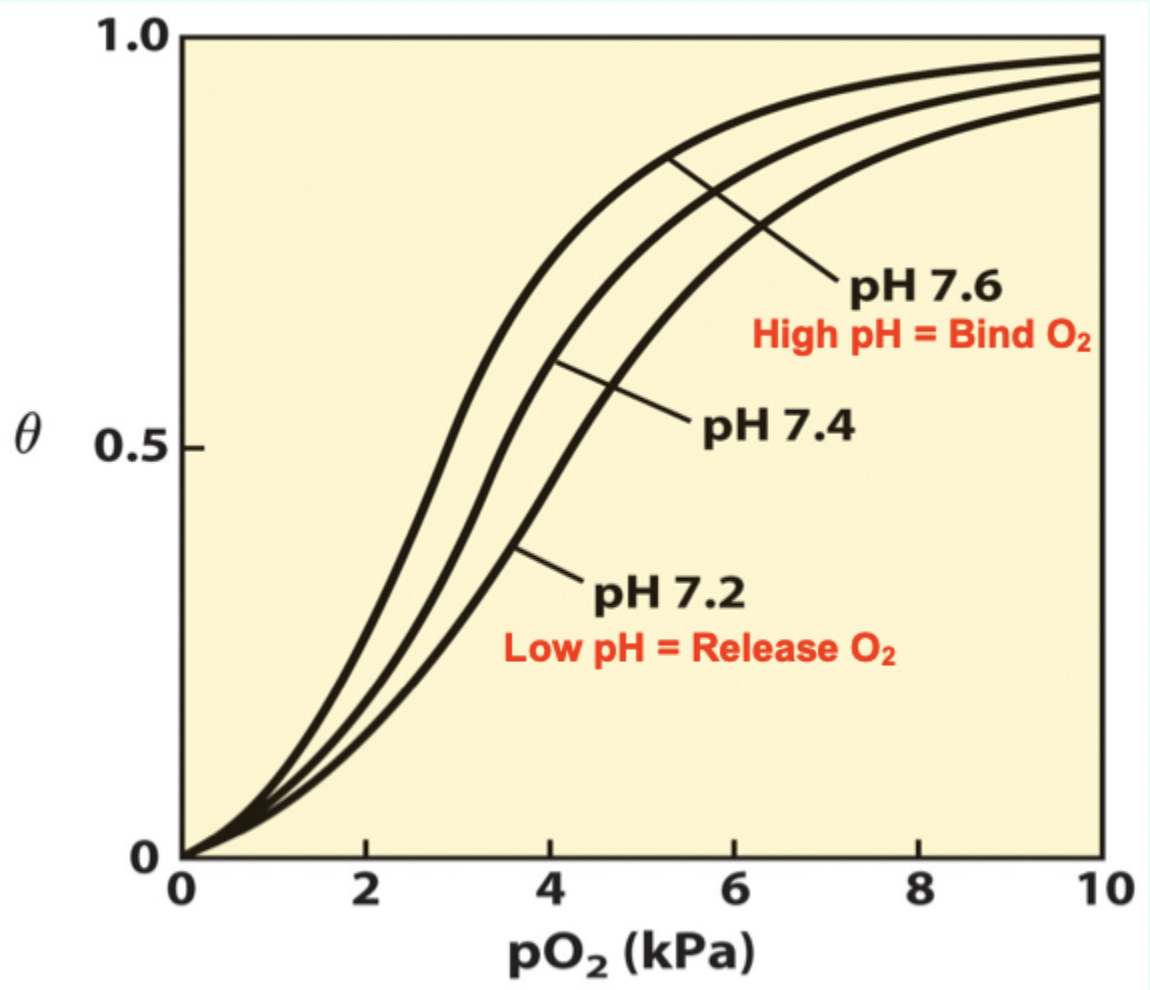
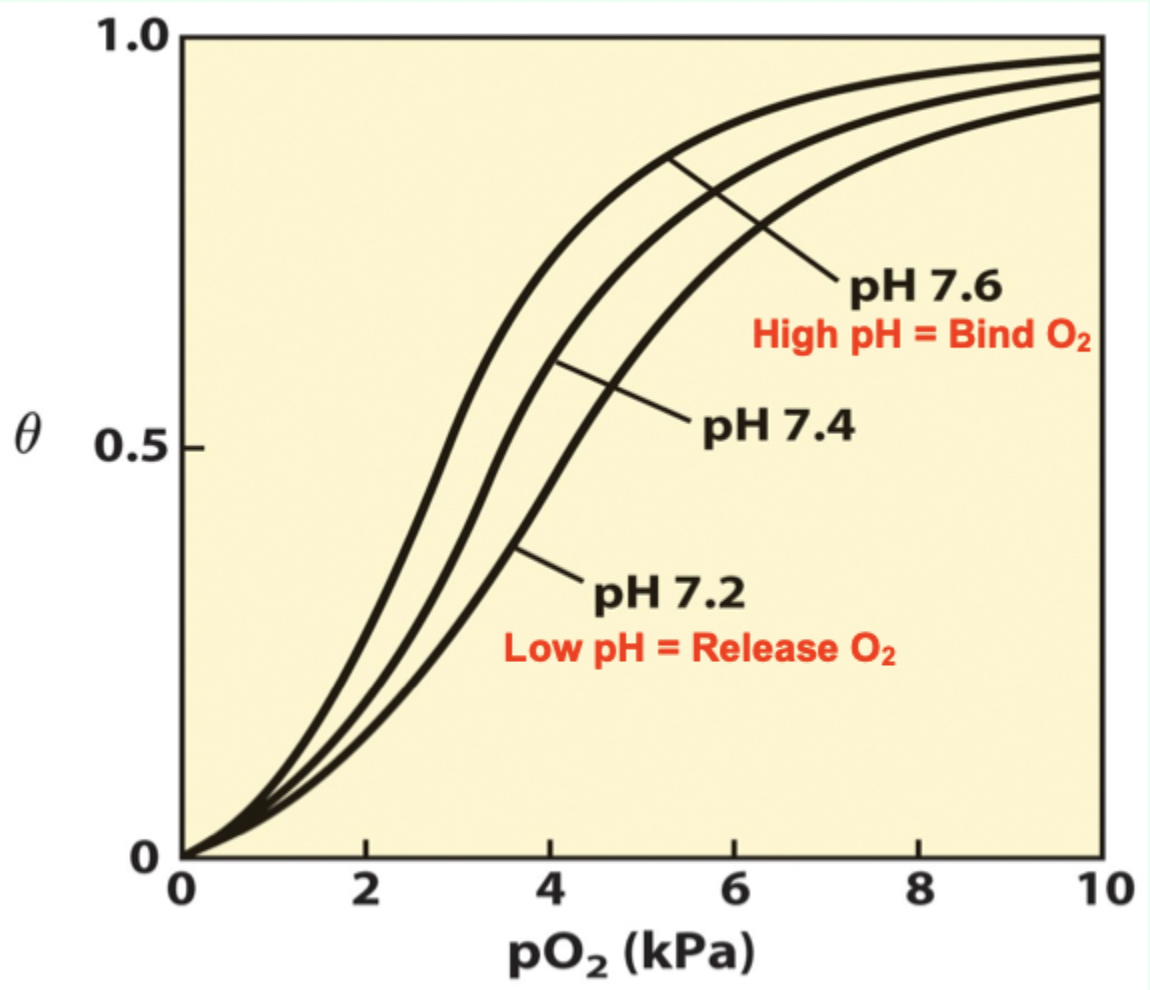
H+ binding to Hb is ____ to O2 binding.
Antagonistic.
How is most metabolic CO2 transported to the lungs?
As soluble bicarbonate (HCO3−).
About what fraction of CO2 reacts with Hb N-termini and travels as a covalent adduct?
~15%.
CO2 binding to Hb is also ____ to O2 binding.
Antagonistic.
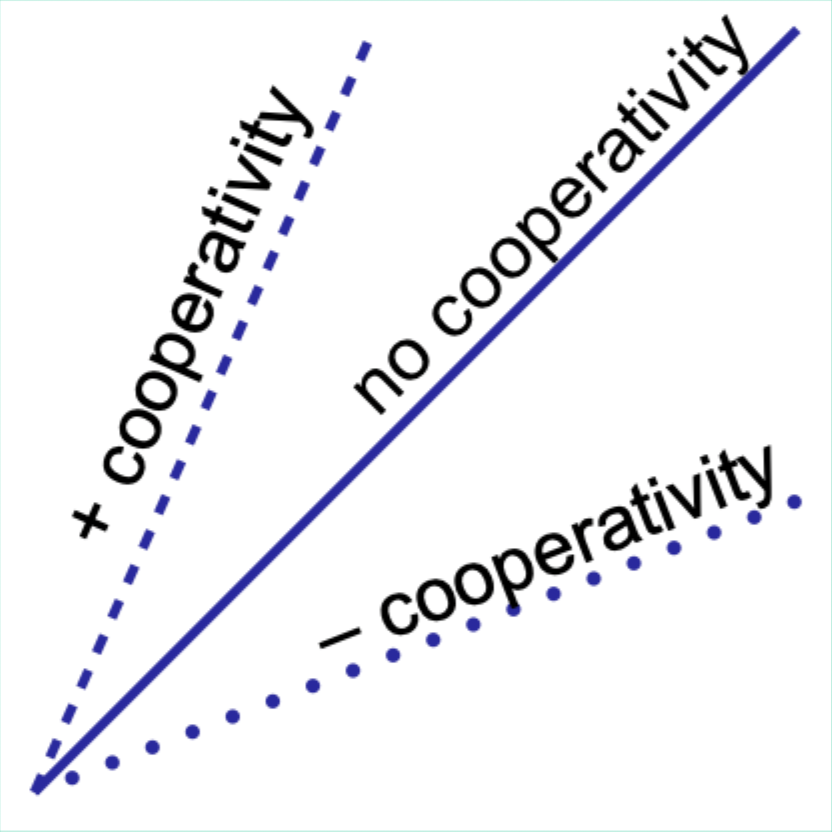
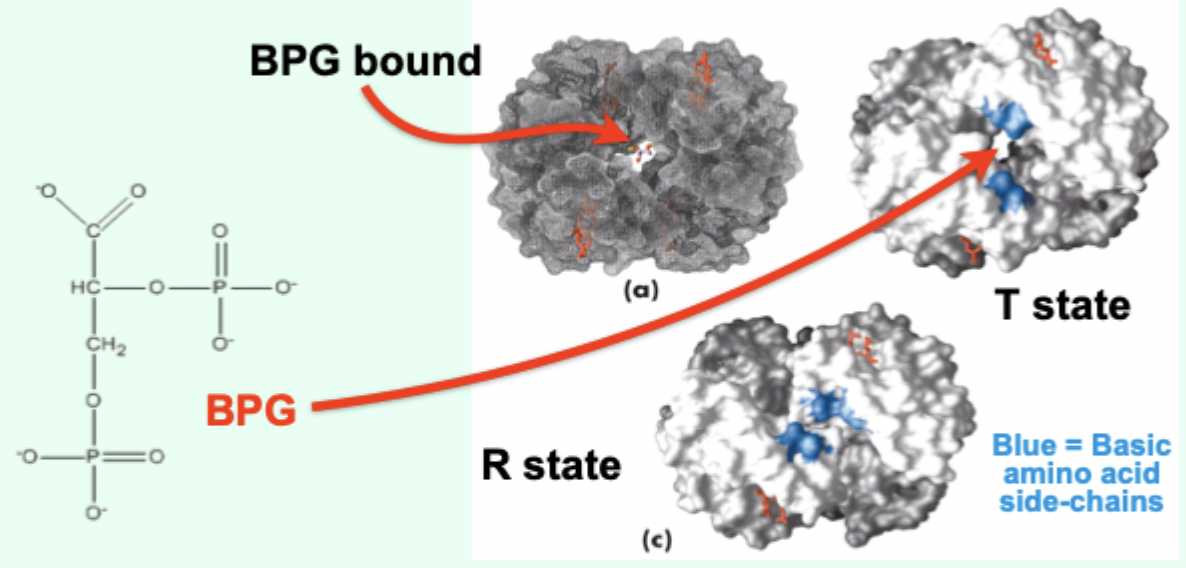
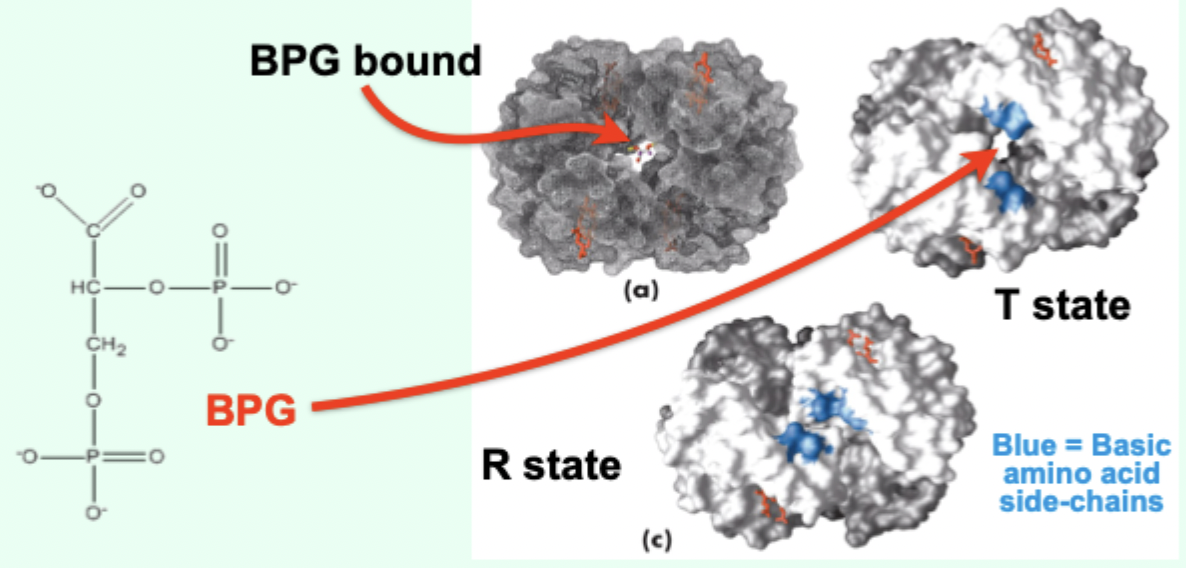
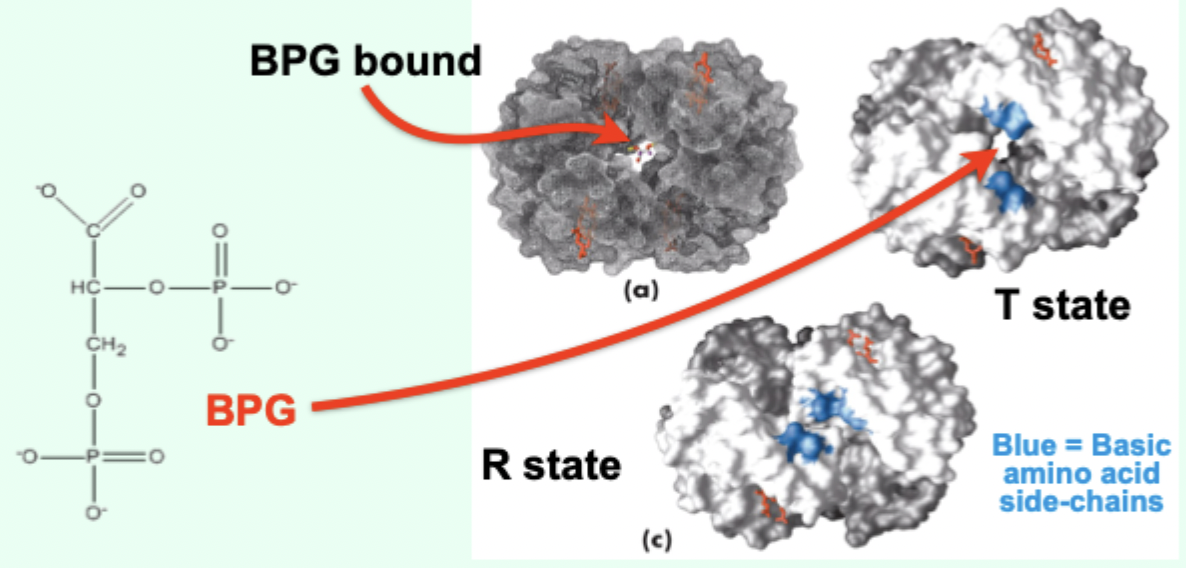
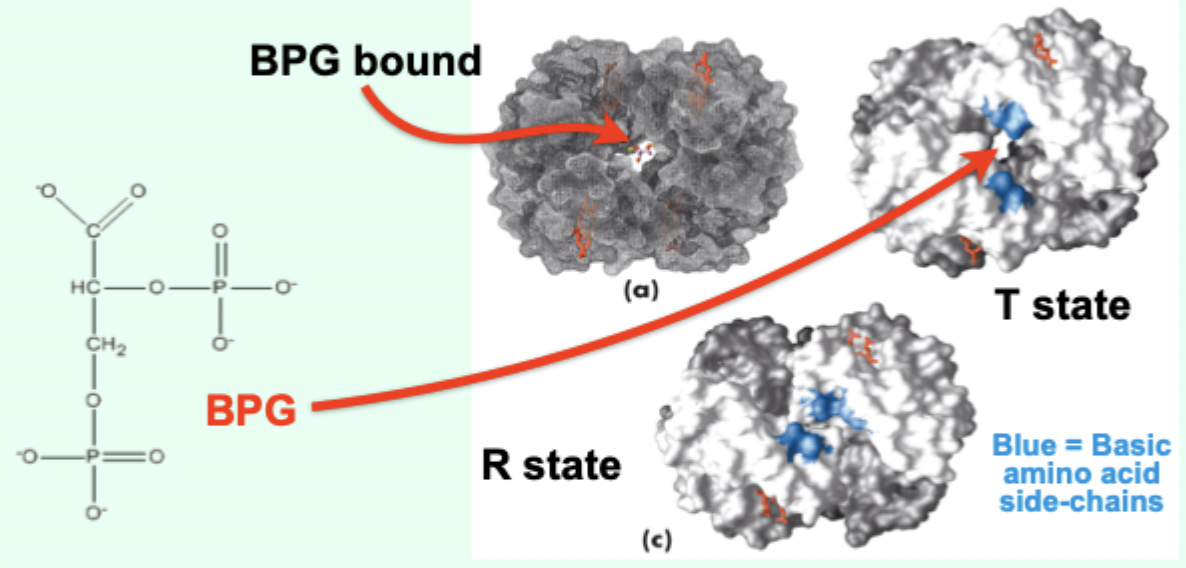
What is BPG and where is it formed?
2,3-bisphosphoglycerate; formed in erythrocytes (RBCs) from a glycolytic intermediate.
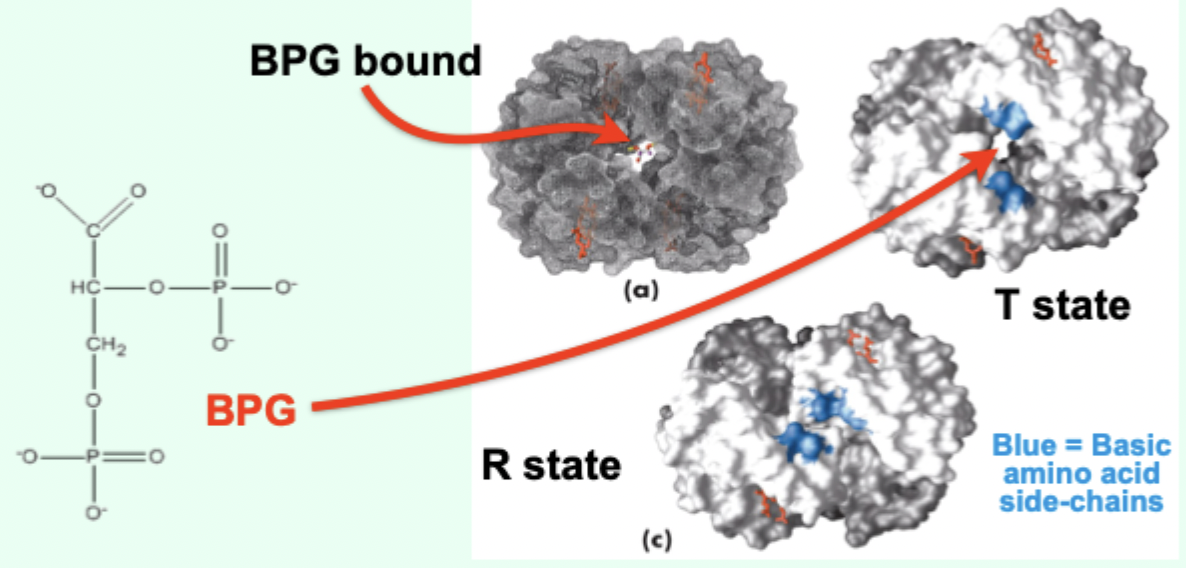
BPG is what kind of regulator of Hb?
A heterotrophic allosteric modulator.
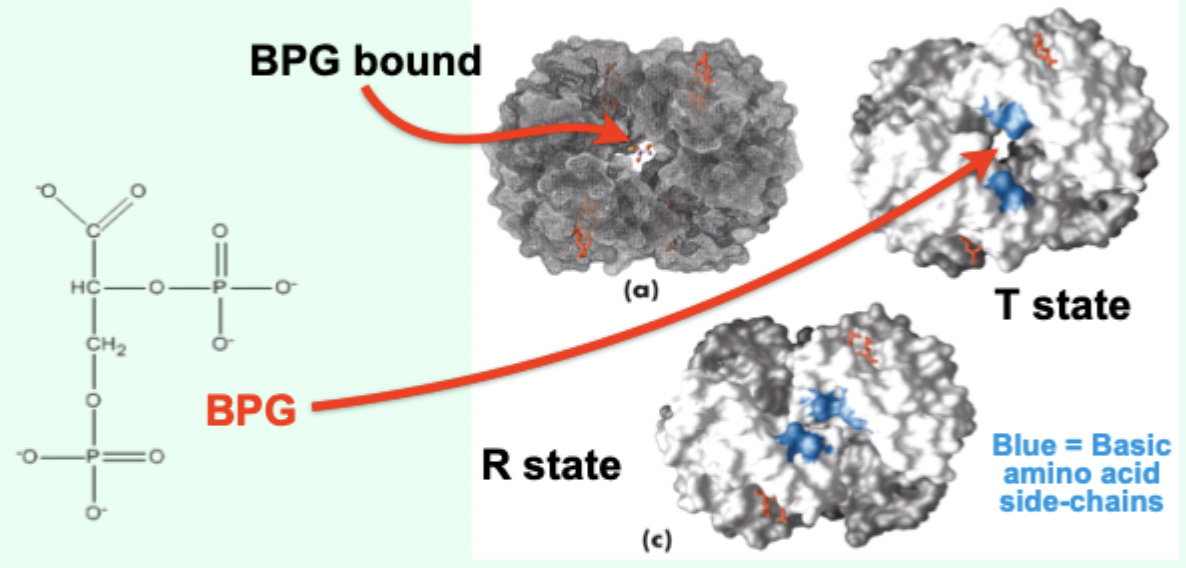
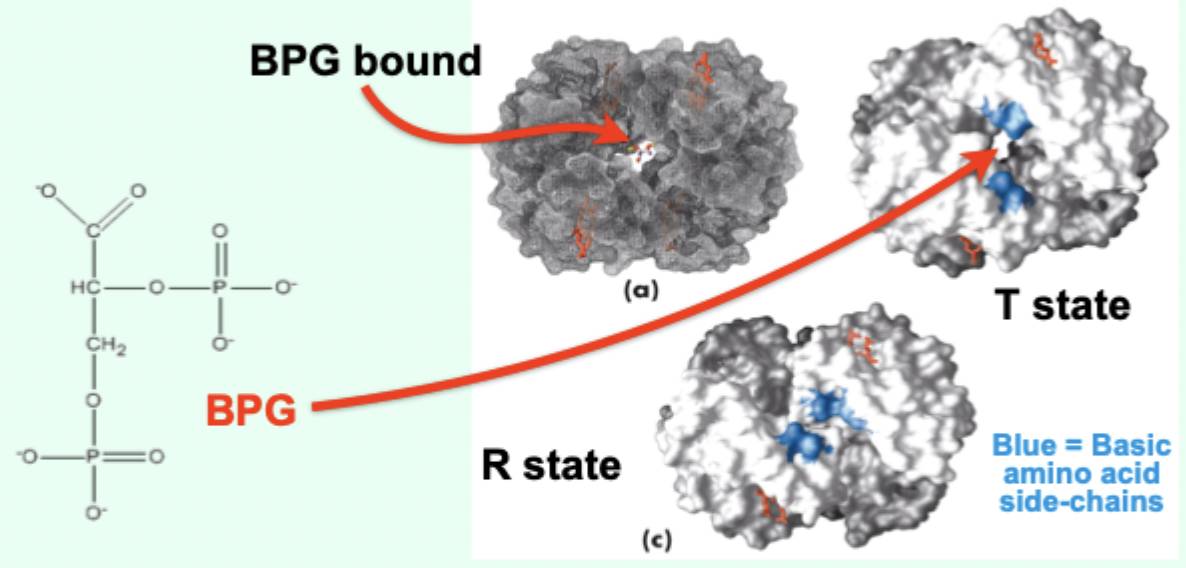
Where does BPG bind on Hb?
In a positively charged cavity between subunits (T state).
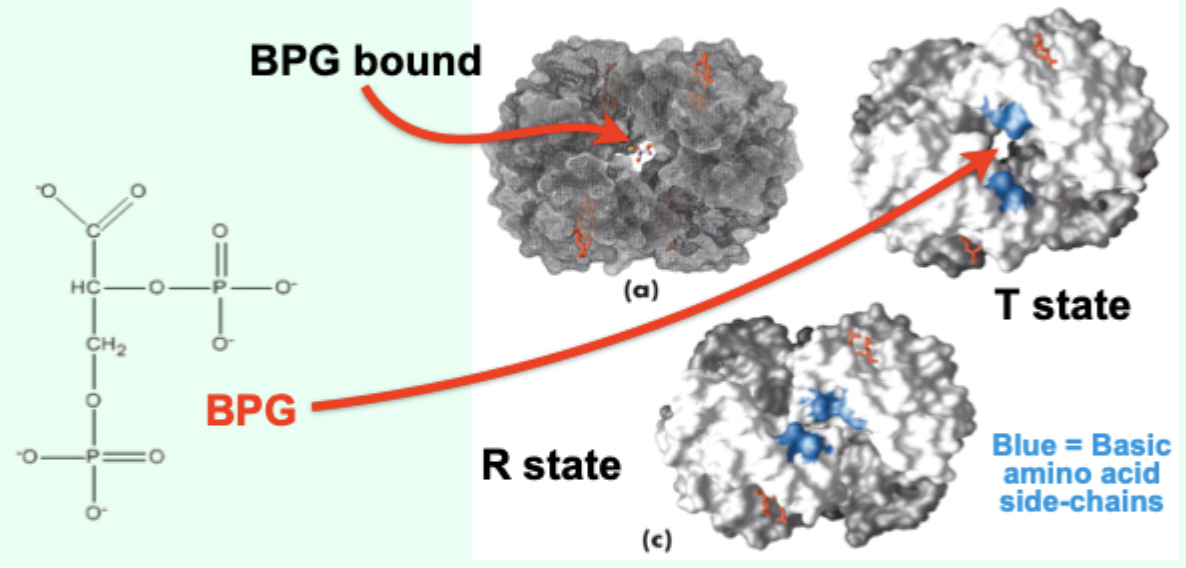
What does BPG binding do to the T → R transition?
Makes the transition to R state more difficult.
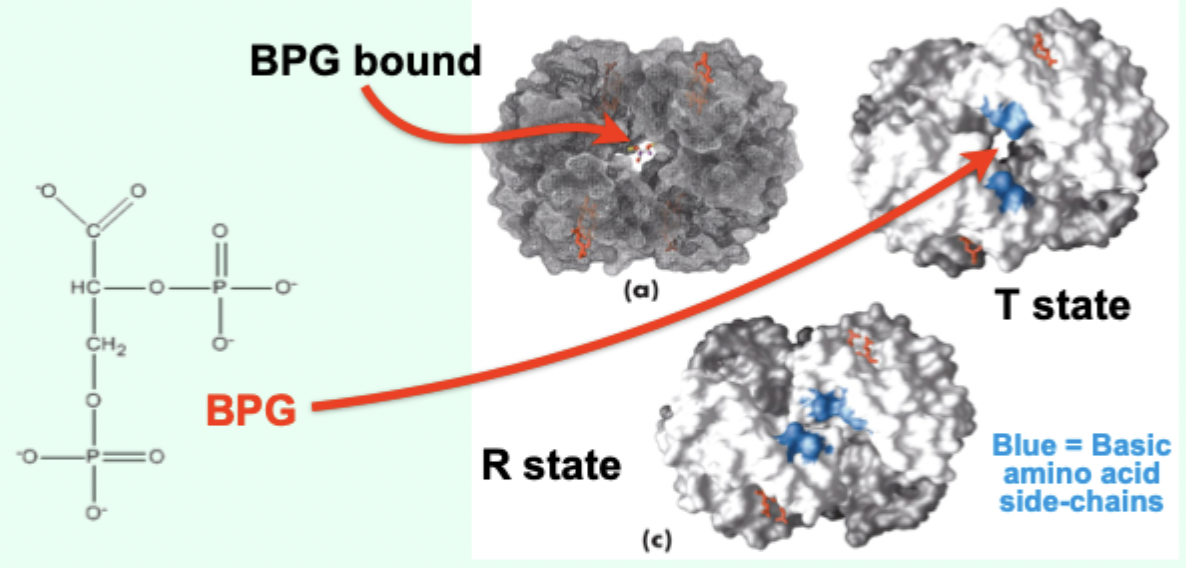
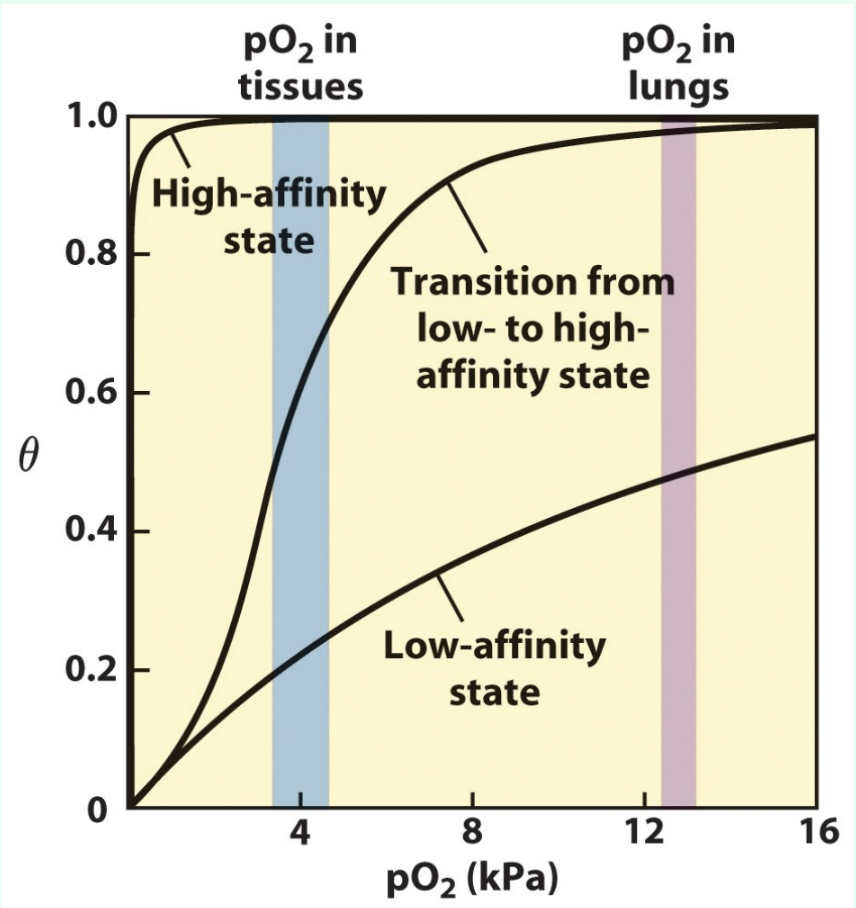
Net effect of BPG on Hb O2 affinity?
Lowers Hb affinity for O2.
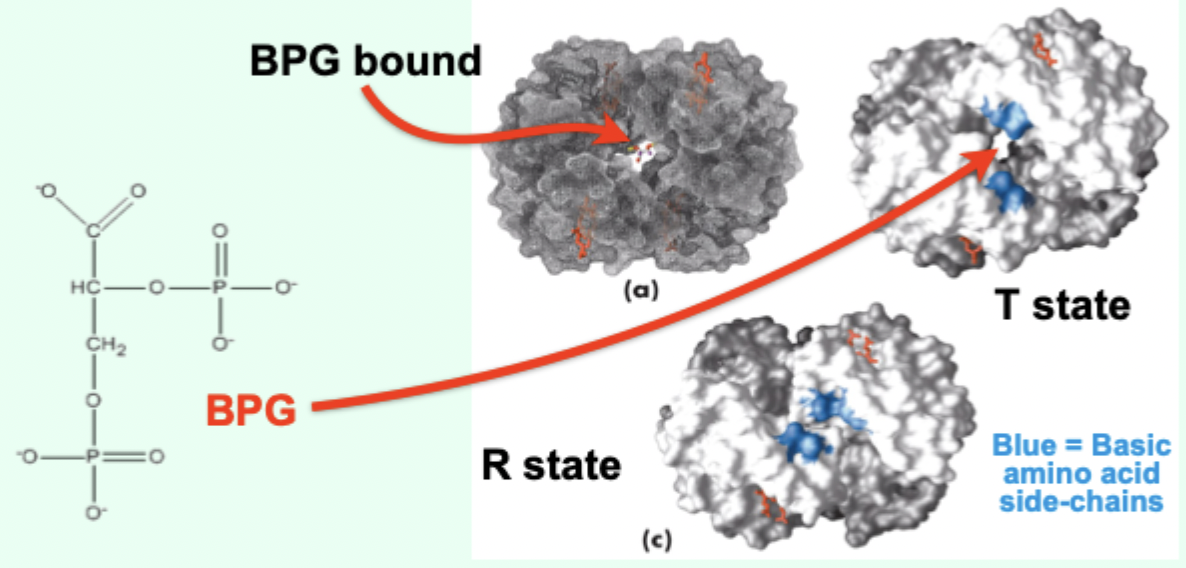
BPG is essential for what?
Correct physiological O2 binding and releasing characteristics of Hb.
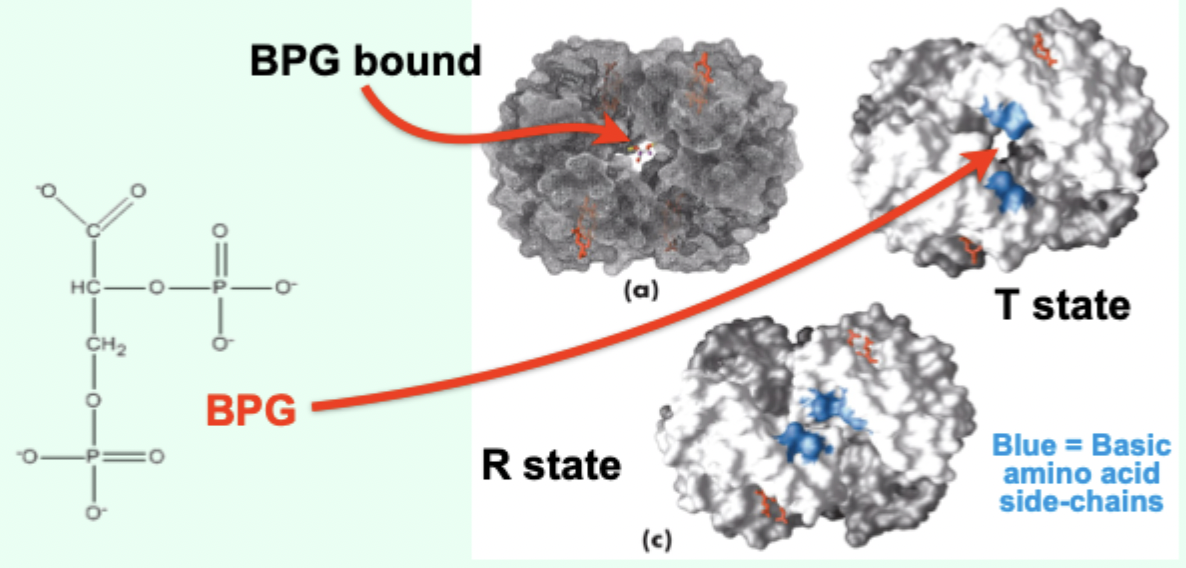
True/false: some BPG is always bound to Hb.
True.
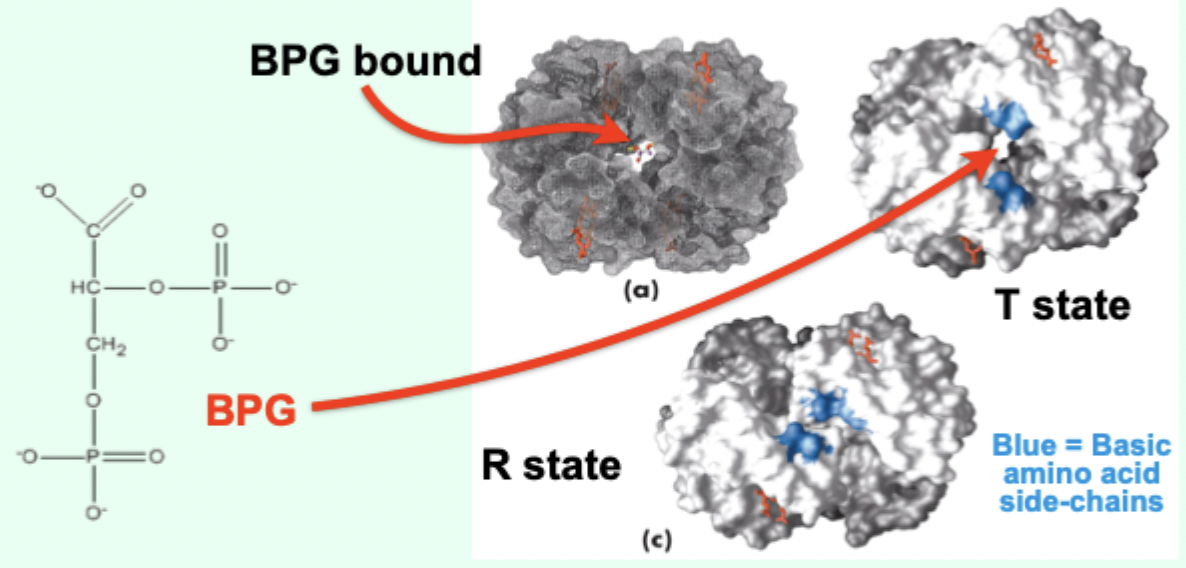
What does BPG help Hb do at the tissues?
Release O2.
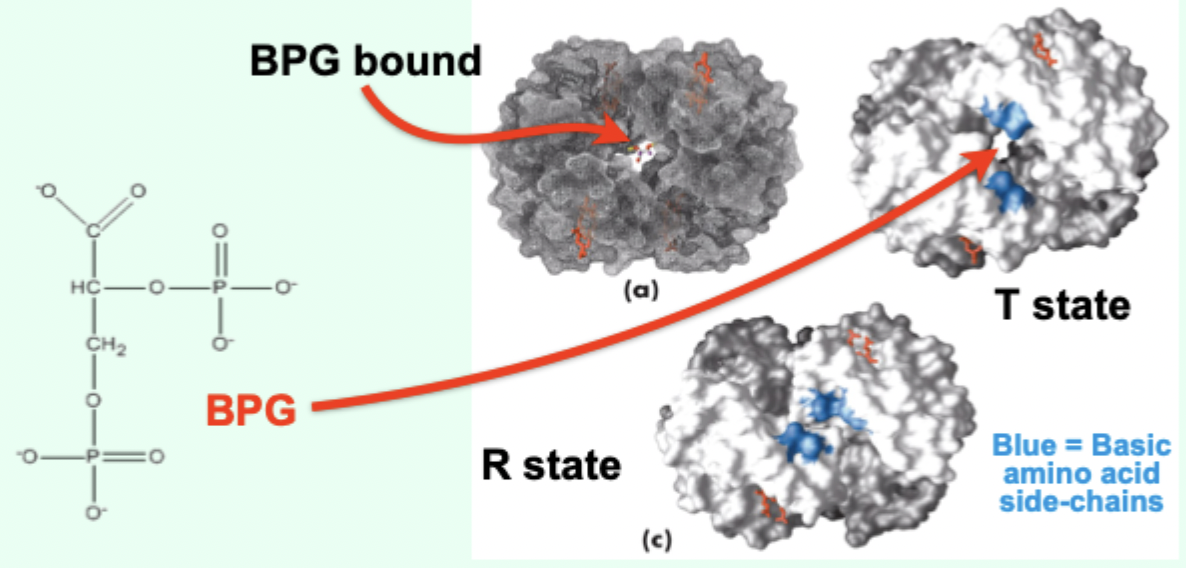
Under normoxic conditions, without BPG what happens?
Not enough O2 would be released from Hb at the tissues.
BPG has little effect on O2 pickup at the lungs but a substantial effect on…
O2 release at the tissues.
BPG helps O2 transport under what conditions?
Hypoxic conditions.
At sea level, about how much O2 is delivered to tissues vs max possible?
~40% of the maximum possible.
What happens to BPG levels with rapid ascent to high altitude?
BPG rises.
What does increased BPG do to Hb O2 affinity at high altitude?
Decreases Hb O2 affinity (mentioned with altitude sickness).