Anesthesia - Exam 2: Someone Knock Me Out (Anesthesia Machine to Inhalants)
1/140
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
141 Terms
What is the purpose of an anesthesia machine?
To prepare a precise mixture for delivery into a breathing circuit
What is the most common bulk oxygen tank, with pressure and volume?
H tank, 7000 L, 2000 PSI
What is the most common portable tank, with pressure and volume?
E tank, 700 L, 2000 PSI
If a 700 L tank is at 500 PSI (normal is 2000), how much gas is left in the tank?
175 (500 is 25% of 2000, 175 is 25% of 700)
What color is a cylinder of oxygen?
Green
What system prevents the connection of the wrong gas?
Pin Index Safety System (PISS), where certain gasses and receptors have specific pin locations
What are six safety tips when storing compressed gas?
Secure or lay down tanks,
Use protection (cap),
Store < 125 degrees,
Don't use oil (on tanks),
Only open 1/4 turn, and
Label storage area
What are the units of the flowmeter?
L/min, from 0.2 - 5.0
What does the flush valve do?
Delivers pure oxygen to the system at 50L/min
Why is it not recommended to use the flush valve on a small breathing circuit?
They explode (Barotrauma)
What is the purpose of the vaporizer?
It vaporizes liquid anesthetic and measures a specific concentration into the gas
T/F: Any agent can be used in a modern vaporizer
False, it is agent specific
What is the common gas outlet for the flowmeter and oxygen flush?
Fresh gas outlet
What are the four purposes of a breathing circuit?
Deliver gas
Remove CO2
Secure airway
Provide ventilation
What are the four classifications of breathing circuits?
Open (not clinical),
Semi-open (non-rebreathing)
Semi-closed (circle)
Closed (circle)
What is necessary to wash out CO2 for a non-rebreathing circuit?
High fresh gas flow rate
How does a non-rebreathing circuit work?
Inhale fresh gas, exhale CO2, and fresh gas washes out exhaled gas before inspiration
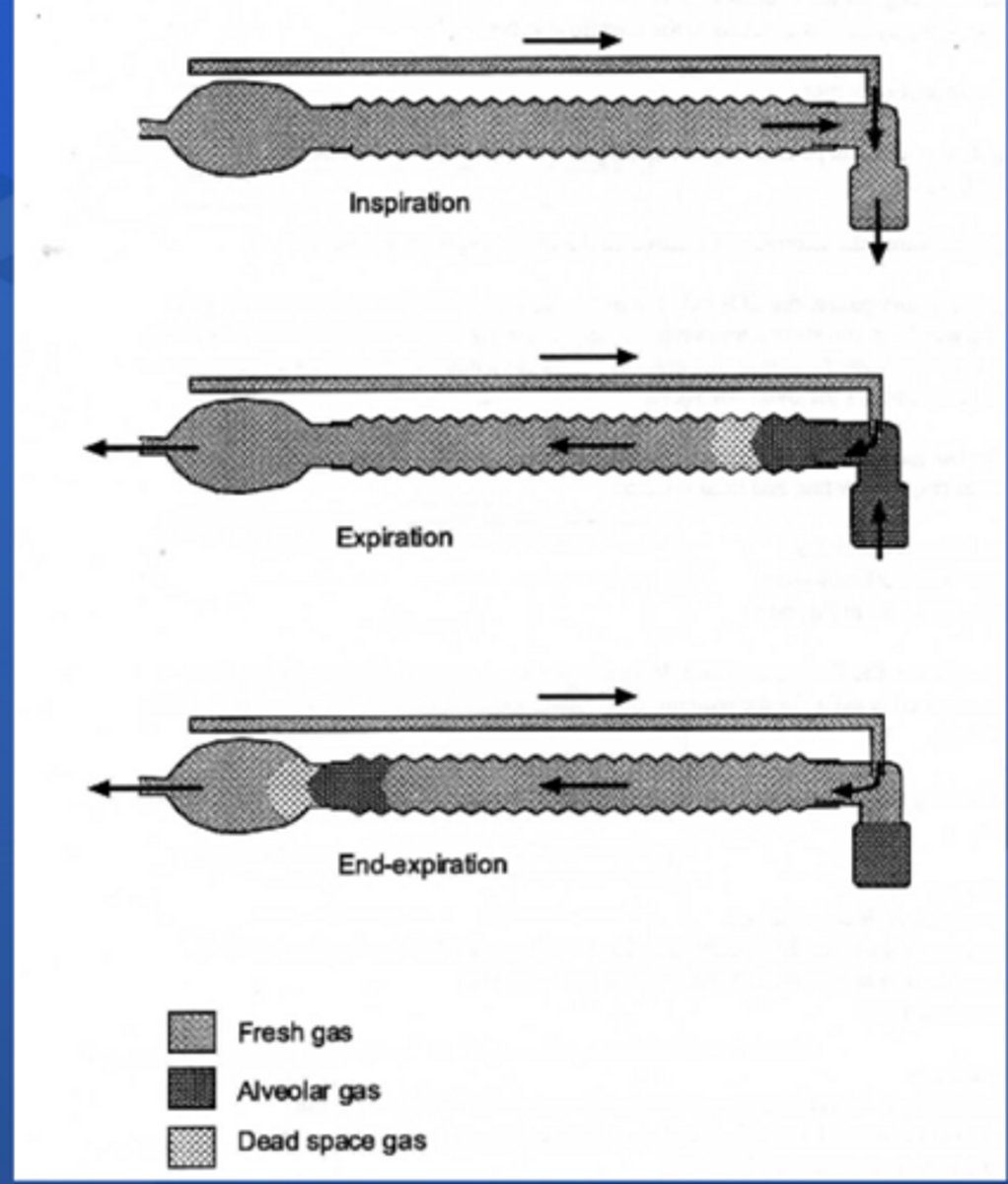
What are four advantages of a non-rebreathing circuit?
Low resistance
Simple
No distance limit
Immediate concentration control
Patients under what weight should use a non-rebreathing circuit?
3 kg
What are the four disadvantages of a non-rebreathing circuit?
High FGF ($)
Loss of heat/moisture
Pollution
Hard to control ventilation
What are the six parts of a circle system?
Fresh gas inlet,
One way valves,
Breathing tube/Y piece,
CO2 absorber,
APL (pop-off), and
Reservoir
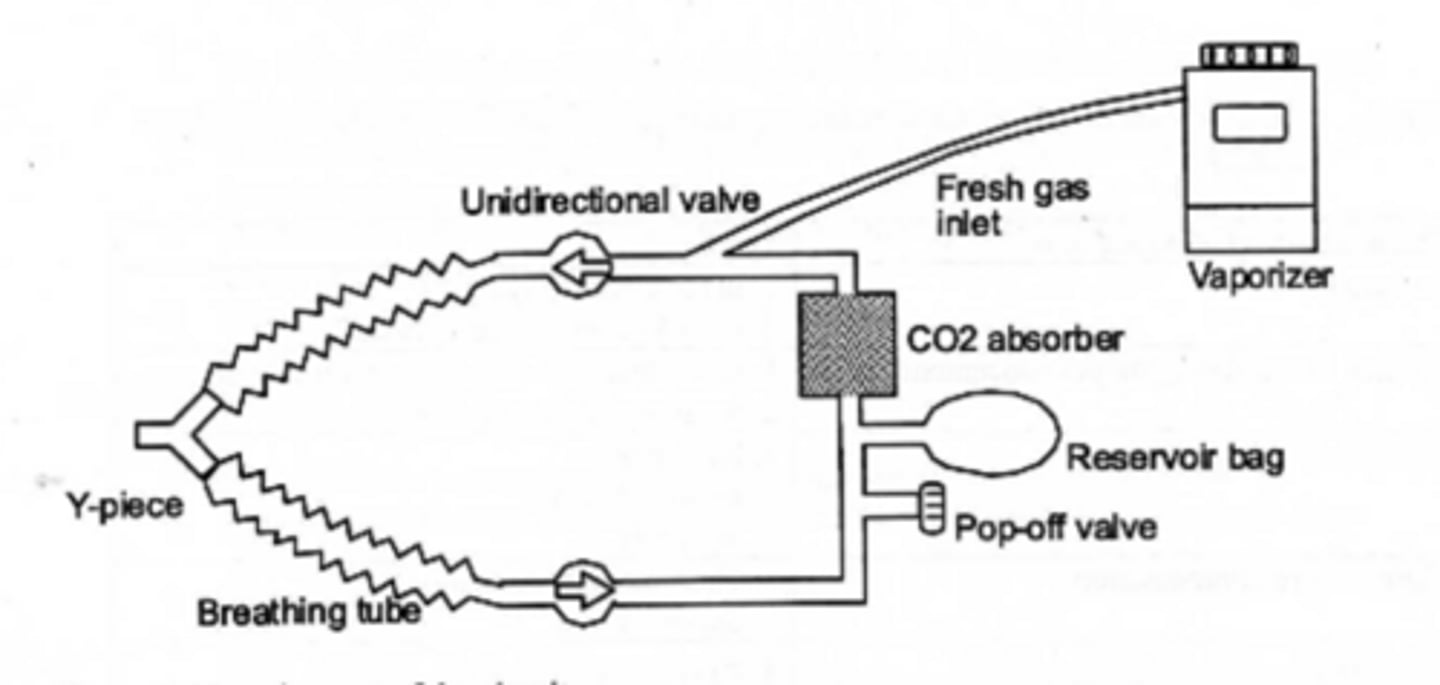
What happens when a circle system valve fails?
It allows bi-directional movement
What is the purpose of Sodasorb?
Scavenge CO2 from expired gas
What are the two byproducts of CO2 and Sodasorb?
Heat and water
What three ways can you tell that Sodasorb is expired?
Inspired CO2
Turns purple
Lack of heat
What happens when Sodasorb is rested?
Color reverts
What are the two purposes of the APL valve?
Vent excess gas (open)
Provide positive pressure (closed)
What are the two purposes of the reservoir bag?
Provide excess capacity
Manual ventilation
How can you determine the correct size of a reservoir bag?
6 x tidal volume
(Tidal volume = 10 - 20 mL/kg)
What are the advantages of the circle system?
Low FGF
Preserve heat/moisture
Less pollution
Easier to ventilate
What are the disadvantages of the circle system?
High resistance
Complex
Distance constraint
Equilibration to new concentration
What is the difference between a semi-closed (partial rebreathing) and a closed (full rebreathing) system?
Semi: FGF exceeds metabolic requirement
Full: FGF meets metabolic requirement
What are the three advantages of closed vs semi-closed?
Conserve gas
Preserve heat/moisture
No pollution
What are the three disadvantages of closed vs semi-closed?
Equilibration
Accuracy
Monitoring
Give the breathing systems in order of most to least FGF required
NRB
Circle
Circle (semi-closed)
Circle (closed)
What is the purpose of activated charcoal?
Remove waste gas from work environment
How can you tell when activated charcoal needs to be replaced?
By weight
What are the four purposes of endotracheal tubes (ETT)?
Patent airway
Reduce aspiration
Aid ventilation
Sample expired gas
What is the purpose of a cuff on ETT?
Reduce leakage of positive pressure ventilation
What are the three advantages of inhalant anesthetics?
Predictable/rapid adjustment
Part of a complete system
Inexpensive
What are the four parts of inhalant anesthetic delivery systems?
Precision vaporizer
Oxygen source
Ability to control ventilation
Removal of CO2
What are the four disadvantages of inhalant anesthetics?
Narrow therapeutic index
Expensive initially
Doesn't block pain input
Side effects (cardio + resp)
What is the primary advantage of isoflurane over sevoflurane?
Better cost
What is the primary advantage of sevoflurane over isoflurane?
Better solubility
T/F: Sevoflurane and isoflurane are administered as a gas
False, vapor
What is the clinically useful way to record the amount of inhalant being administered?
Volume percent
The pressure exerted by one gas in a mixture if it occupied the space alone is what?
Partial pressure
What controls the clinical effect of inhalants on the patient?
Partial pressure of the inhalant on the brain
The air pressure outside is 800 mmHg, and you are administering 2% Sevoflurane. What is the PP of Sevo?
0.02 * 800 = 16 mmHg
At the same partial pressure, the concentration ratio between two phases, such as amount of inhalant in blood versus the amount as a gas, is what?
Solubility
What does blood:gas partition coefficient determine?
Induction and recovery, where MORE soluble means a SLOWER induction and recovery
(1:2 is MORE soluble and SLOWER than 1:10)
What does oil:gas partition coefficient determine?
Potency, where MORE soluble means LOWER concentration for effect, thus HIGHER potency
Sevoflurane has a blood:gas PC of 0.6 while Isoflurane has a PC of 1.4. Which one is going to have a slower induction and recovery time?
Isoflurane, because MORE soluble in blood means SLOWER to move to the brain to induce
Sevoflurane has an oil:gas PC of 50, while Isoflurane has a PC of 99. Which one requires a higher concentration for similar effects?
Sevoflurane, because LOWER potency means it needs a HIGHER concentration for effect.
T/F: If something is more soluble in oil, you need less of it
True
T/F: If something is more soluble in blood, it is slower to induce
True
What is time constant?
The time it takes to fill a container, which is volume in L divided by flow in L/min
What percentage of the volume is replaced after one time constant?
63%
What percentage of the volume is replaced after four time constant?
98%
You have a 5L bucket of water (congrats) and you start to fill it with 10% salt water at a rate of 1 L/min. What is the time constant?
5 minutes (time to fill up bucket if empty)
You have a 5L bucket of water (congrats) and you start to fill it with 10% salt water at a rate of 1 L/min. How long do you have to wait until there is a 98% change in the concentration?
20 minutes (4 time constants)
You have a 5L bucket of water (congrats) and you start to fill it with 10% salt water at a rate of 1 L/min. What is the concentration of the bucket after 20 minutes?
9.8% salt water (98% x 10% salt)
How can you estimate the volume of the circle system?
Reservoir + Breathing circuit + 50% of absorbent
What is the order of distribution of the inhalants from most to least saturated?
Vessel rich (brain, organs),
Muscle,
Fat, and
Vessel poor (bone, cartilage)
What is the undesired effect caused by the distribution of inhalant to tissues other than the VRG?
There is delayed uptake which delays full equilibrium
The effect of inhalants is based on what?
Partial pressure in the CNS
What two factors affect delivery of inhaled anesthetics to the alveoli?
Inspired concentration (Pi)
Alveolar ventilation (Va)
What three factors affect removal of inhaled anesthetics from the alveoli?
Blood:gas PC
Cardiac output
Alveolar-venous concentration difference
What variable reflects the parital pressure present in the brain?
The partial pressure of the alveoli
What is the MOA of inhalants?
Nobody knows
What is the Minimum Alveolar Concentration (MAC)?
The alveolar concentration at which 50% of the population does NOT respond to a supramaximal stimulus, represented as ED50
MAC is an index of what?
Potency, where lower MAC indicates higher potency
How can we calculate ED95?
1.5 x MAC
WHAT IS THE MAC OF ISOFLURANE?
1.3 - 1.6
WHAT IS THE MAC OF SEVOFLURANE?
2.3 - 2.6
What two things increase MAC?
Hyperthermia
CNS stimulants
What four things decrease MAC?
Pregnancy
Hypothermia
Extreme age
Other anesthetics (premed, injectable)
T/F: Duration of anesthesia, gender, anticholinergics, pH, paCO2, paO2, and blood pressure do not affect MAC
True
What are the four beneficial effects of inhalants in order of increasing dose?
Unconciousness,
Muscle relaxation,
Loss of nociception, and
Loss of sympathy (sympathetic response)
What are the cardiovascular side effects of inhalants?
Dose dependent drop in blood pressure by decreasing CO, SVR, or both
What are the respiratory side effects of inhalants?
Decrease in minute ventilation (drop TV) and decreased response to CO2
On a farm call, you give a Poland China pig inhalant anesthesia and they develop rigor, uncontrolled fever and CO2, acidosis, arrhythmia, then dies. This was the owner's favorite pig and now he hates you cuz it's all your fault. You take the verbal abuse for a good five minutes before you walk to your car and drive away. What do you write as the cause of death in your notes so you don't get sued?
Malignant Hyperthermia
What is the pathophysiology for malignant hyperthermia?
Inability to resorb calcium, leading to a hypermetabolic state
T/F: Modern inhalants are metabolized by the liver
False, not metabolized
What is the regulatory limit for workplace exposure to anesthetic gases?
<2 ppm, and if you smell it, it's much higher
What subset of the population is at the greatest risk for health problems due to exposure to waste anesthetic gases?
Limit exposure to everyone, but pregnant people are at a higher risk for everything, so do what you will
What are the four goals for small animal anesthesia?
Unconsciousness,
Loss of movement,
Loss of nociception, and
Homeostasis
What does signalment consist of?
Age
Breed
Sex
How are patients under 11 weeks different when anesthetizing?
They have delayed metabolism of drugs
How are patients over 80% of life different when anesthetizing?
Delayed metabolism and more profound effect
What are the four vital signs assessed during physical exam?
Temperature
Pulse rate
Respiratory rate
Pain
Describe the ASA 1 classification
Healthy patient, elective procedure (spay, dental)
Describe the ASA 2 classification
Systemically healthy, necessary procedure (fracture, TPLO)
Describe the ASA 3 classification
Severe but stable systemic disease (CHF)
Describe the ASA 4 classification
Systemically decompensated, constant threat to life (septic abdomen)
Describe the ASA 5 classification
Less than 24 hours to live (septic shock)
What are three advantages of having NSAIDs in the anesthetic plan?
Long acting
Central + peripheral effects
No drug interaction
What is a disadvantage of NSAIDs in the anesthetic plan?
Inadequate for surgical pain
What are three advantages of having a sedative as a premedication?
Agent reduction
Facilitate handling
Analgesia
What three sedatives can be used as a premed and their class?
Acepromazine (phenothiazine)
Dexmedetomidine (alpha-2-agonist)
Midazolam (benzodiazepine)