4.1 sexual reproduction in humans
1/93
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
94 Terms
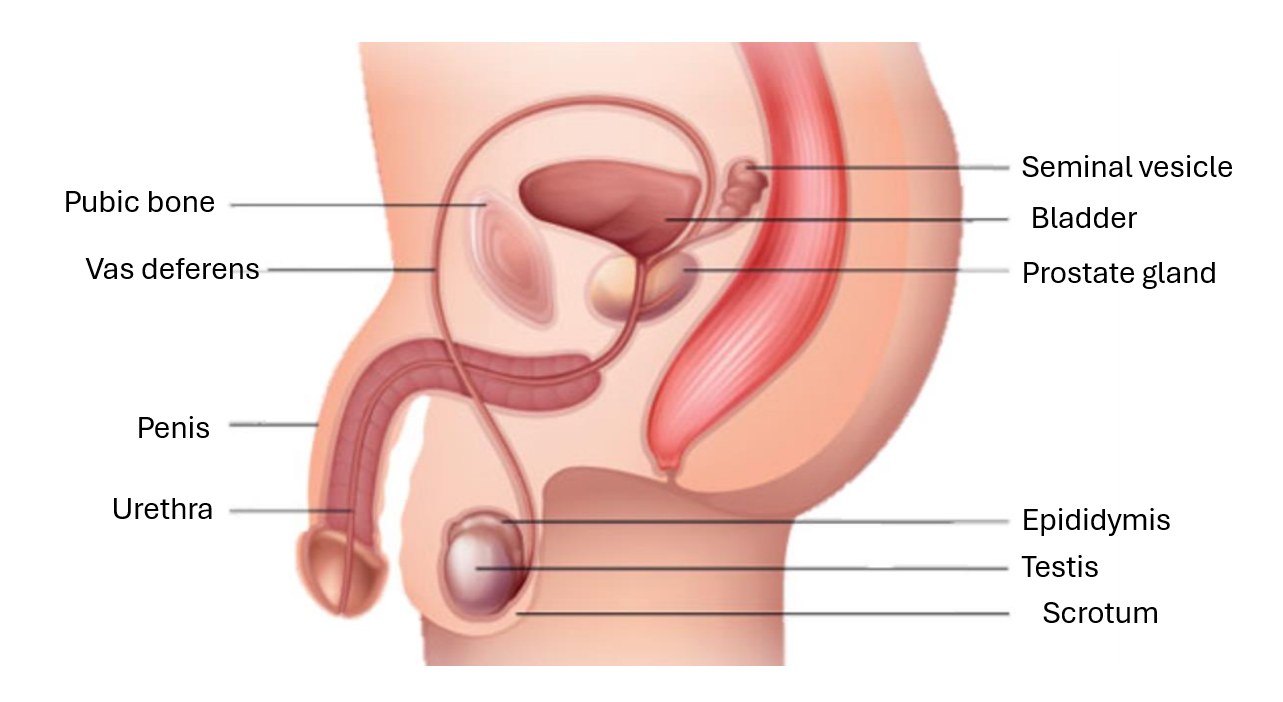
label the side profile of the male reproducitive system
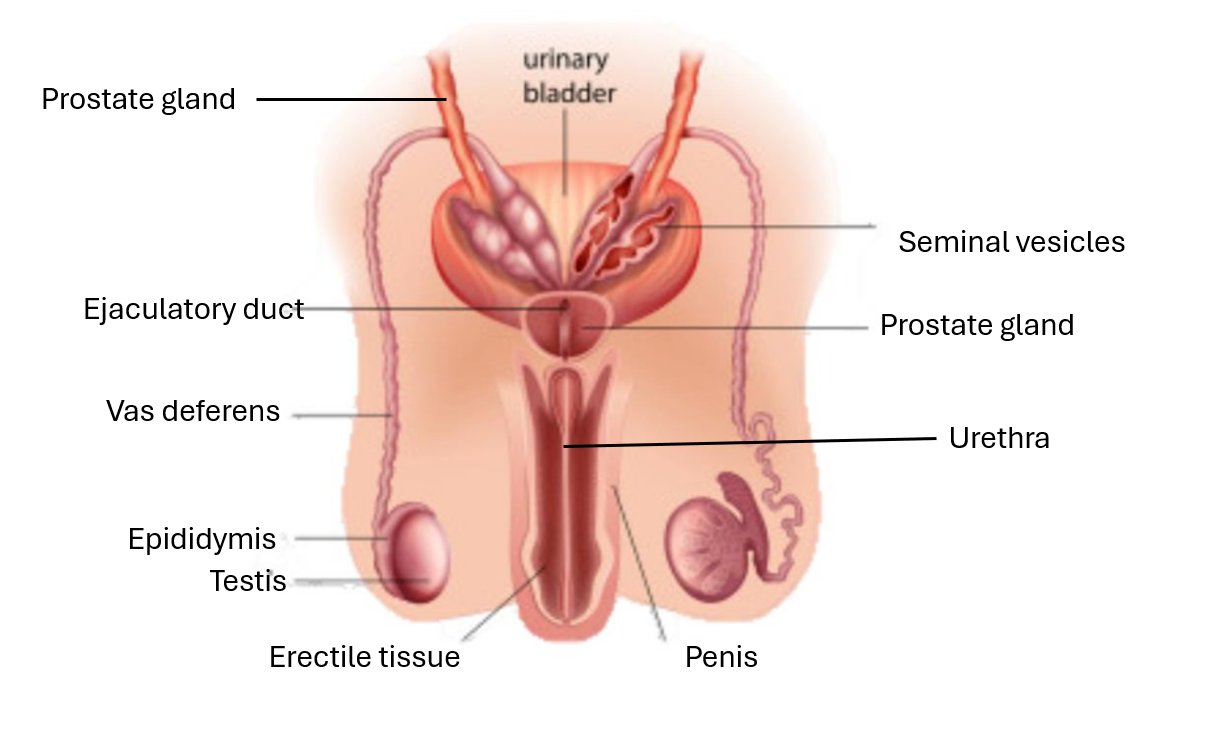
label the front profile of the male reproductive system
what is the function of the scrotum?
external sac of skin containing testes
what is the function of the testes?
produce gametes (sperm from spermatogenesis)
produces testosterone from Leydig cells
what is the function of the epididymis?
sperm stored here and mature to become fully motile
what is the function of the vas deferens?
carries sperm from the epididymis to the urethra during ejaculation
what is the function of the seminal vesicle?
secretes fluid into vas deferens (makes up 60% of semen)
what is in seminal fluid?
rich in mucus and nutrients for sperm
eg fructose for respiration and amino acids
what is the function of the prostate gland?
secretes fluid into vas deferens (makes up 30% of semen)
what is in prostate fluid?
Zn2+ needed by sperm
alkaline - neutralises acidity of urine in urethra and acidity of vaginal tract
what is the function of the urethra?
carries semen through penis and out of body
carries urine from bladder through penis and out of body
what is the function of the penis?
specialised organ adapted to transfer semen to vagina
organ of internal fertilisation
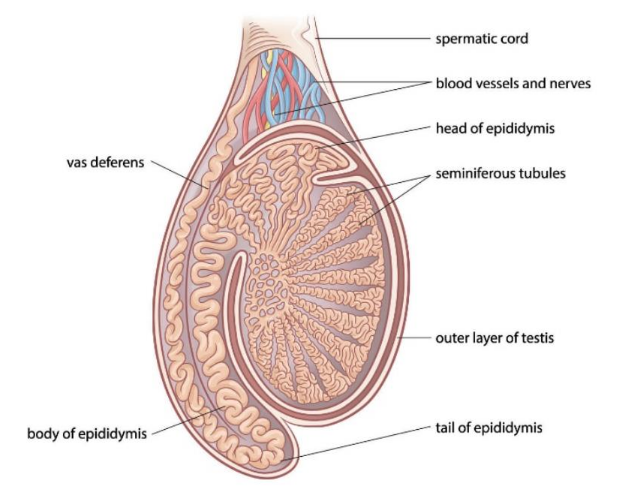
label the TS testis
why do the testis hang outside the body?
sperm production cannot occur at body temp (approx 2° lower)
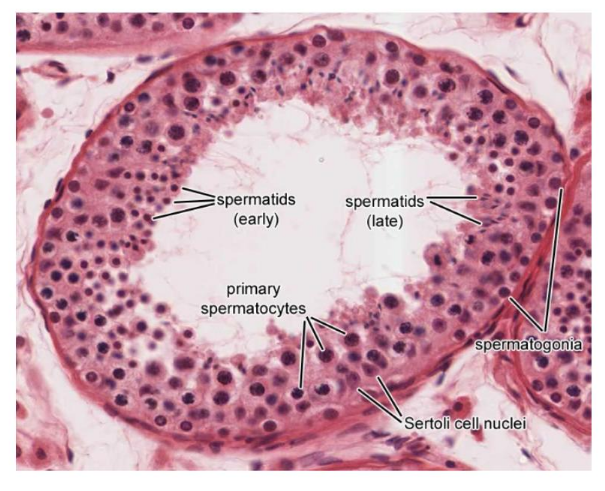
label the TS seminiferous tubule in a testis
what is the function of a Sertoli cell?
provide nourishment for spermatids
protection against male immune system
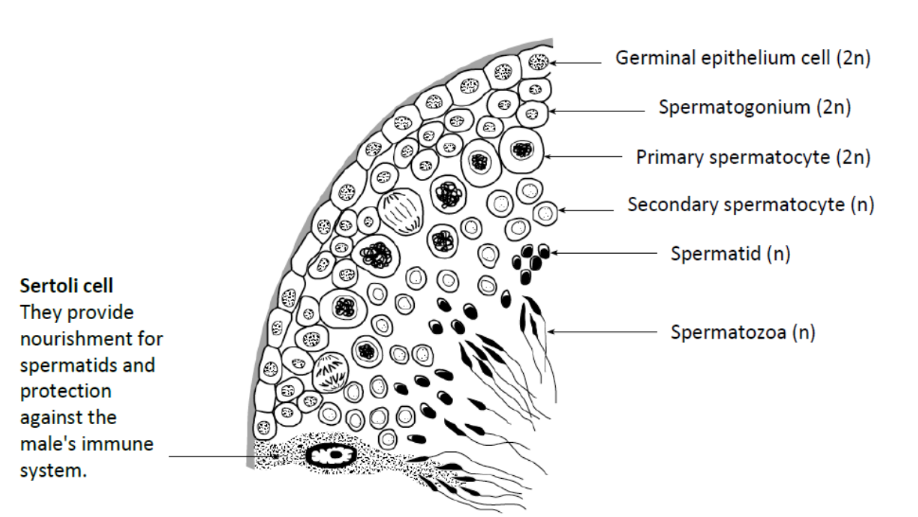
label the seminiferous tubule
how many sperm cells are in each ejaculation?
400 million
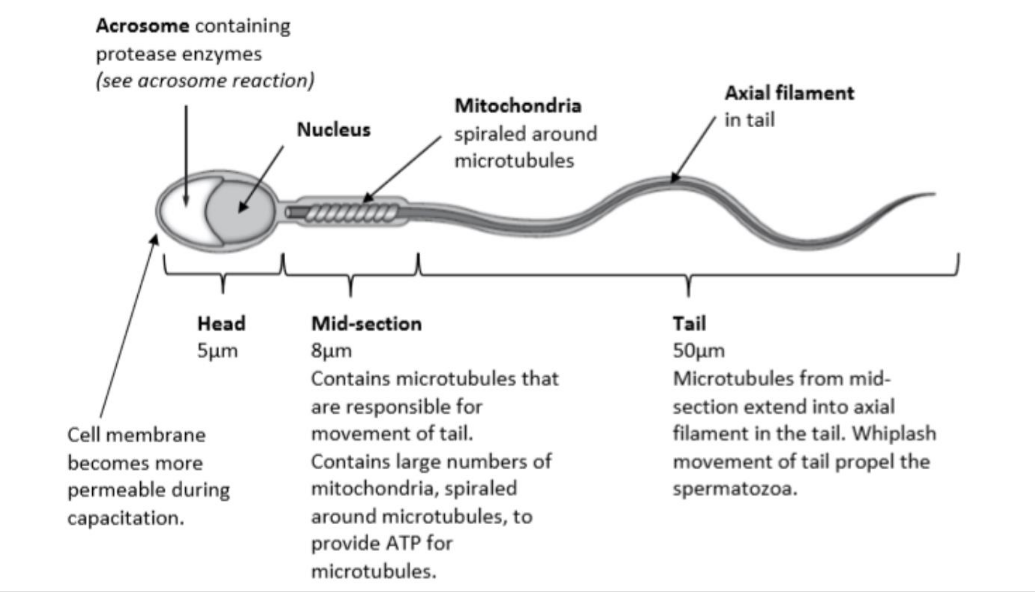
label the sperm cell
what is the function of the head (sperm cell)?
haploid nulceus
restores diploid number of chromosomes after fertilisation of ovum
what is the function of the acrosome?
contains hydrolytic enzymes
needed for successful fertilisation
what is the function of the mid piece (sperm cell)?
many mitochondria - site of aerobic respiration
release energy/make ATP needed for movement of tail
what is the function of the tail/flagellum?
lashing movement
allows sperm to swim through female reproductive system
vagina → cervix → uterus → fallopian tube
what is the sequence of events during spermatogenesis?
primordial germ cell
spermatagonium (2n)
mitotic division
primary spermatocyte (2n)
meiosis I
secondary spermatocyte (n)
meiosis II
spermatids (n)
sperm cells (n)
why is the formation of haploid gametes important?
reforms diploid number of chromosomes after fertilisation of ovum
prevents double fertilisation of chromosomes each generation
what process in meiosis produces genetic variation in the daughter cells?
prophase I - crossing over of chiasmata between non-sister chromatids
metaphase I - independant assortment of homologous pairs
metaphase II - independant assortment of chromatids
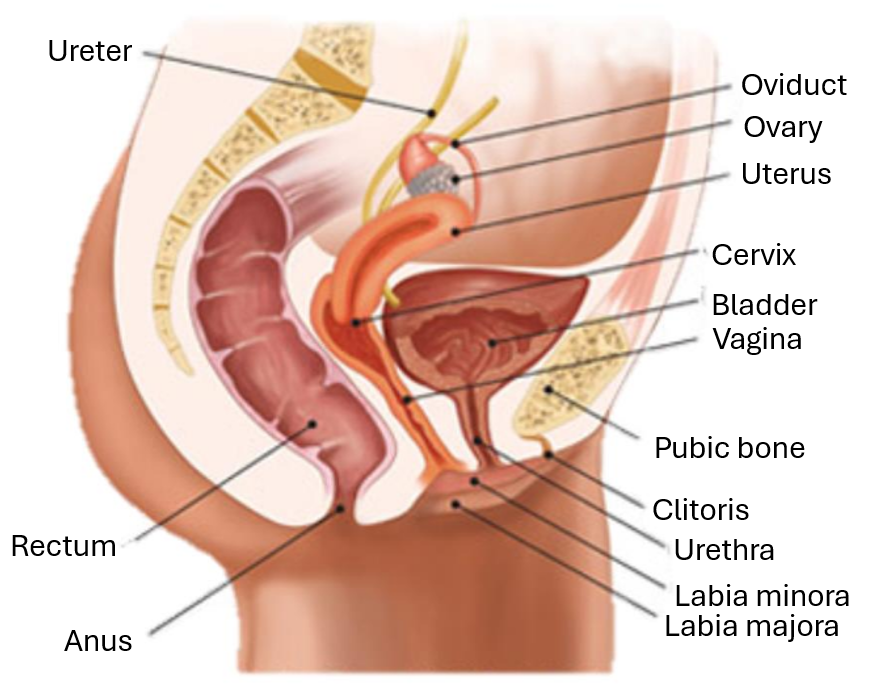
label the side profile of the female reproductive system
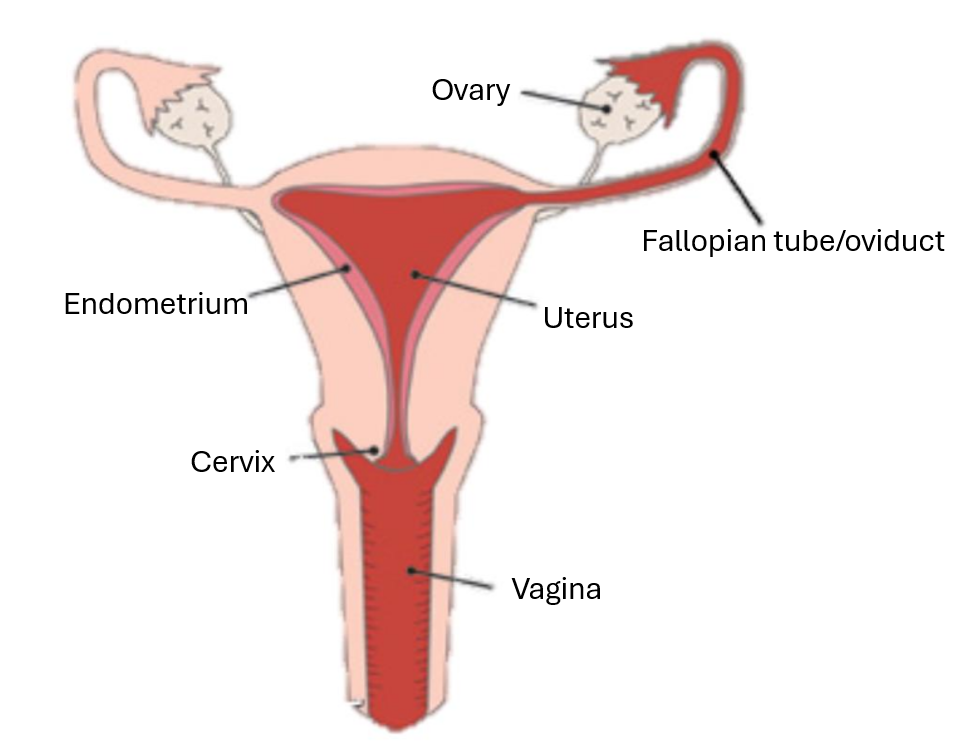
label the front profile of the female reproductive system
what is the function of the ovary?
production of gametes (secondary oocytes formed during oogenesis)
produce oestrogen and progesterone
what is the function of the fallopian tube/oviduct?
lining of ciliated epithelial cells
move secondary oocyte from ovary to uterus
site of fertilisation
what is the function of the uterus?
during pregnancy it expands to accomodate growing fetus
what is the function of the endometrium?
inner most layer of uterus wall
good blood supply
site of embryo implantation
if implantation doesn’t occue then endometrium shed during menstruation
what is the function of the myometrium?
muscle layer that contracts during birth
what is the function of the perimetrium?
outer layer of uterus wall
what is the function of the cervix?
narrow ring of connective tissue and muscle
acts as barrier between uterus and outside environment during pregnancy
during pregnancy - mucus plug forms to seal uterus, preventing pathogen entry
what is the function of the vagina?
muscular walls
opens at vulva
semen deposited in it during sexual intercourse
fetus passes out it during birth
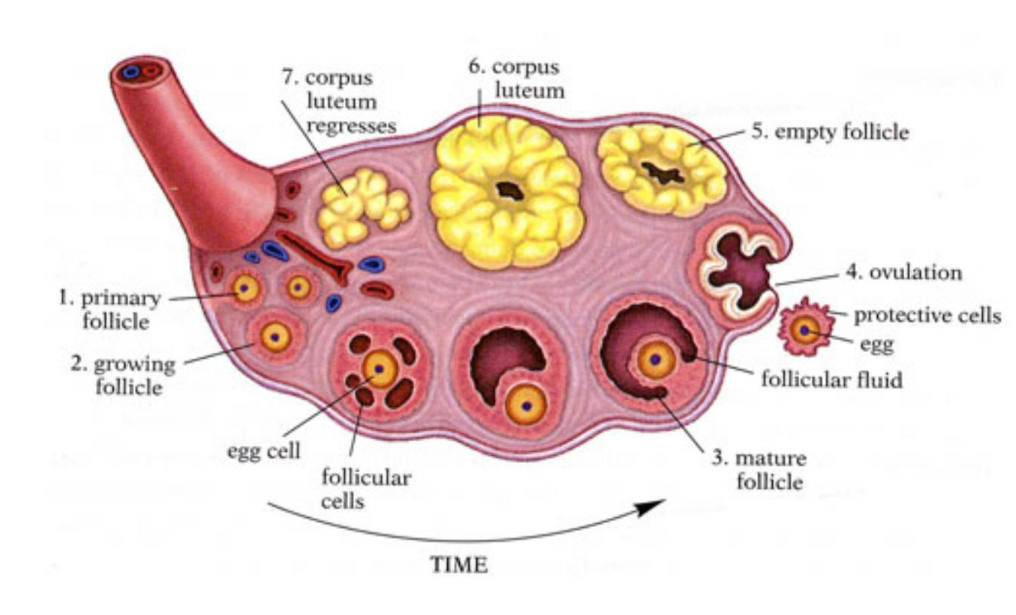
label the ovary structures over time
what process occurs in the ovary?
oogenesis
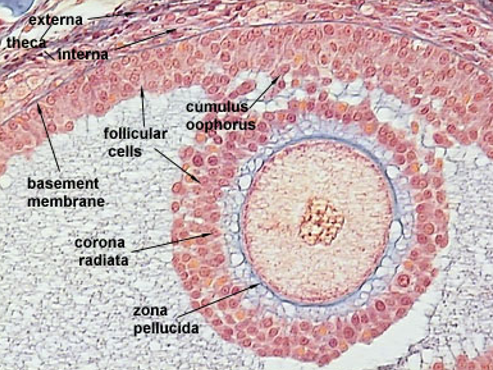
label the mature Graafian follicle
what is the sequence of events in oogenesis?
germinal epithelial cells (2n)
mitosis
oogonia (2n)
mitosis and enlarge
primary oocyte (2n) and follicle cells (2n)
meiosis I
secondary oocyte (n) and follicle cells (2n)
maturation
Graafian follicle
break down oogenesis before birth
germinal epithelium cells (2n) divide by mitosis
produce oogonia (2n)
divide many times by mitosis
form primary oocytes (2n) and follicle cells (2n)
follicle cells surround primary oocyte → primary follicle
primary oocyte begins meiosis I - stops at prophase I until puberty
break down oogenesis from puberty
hormones stimulate primary oocyte to complete meiosis I
produces secondary oocyte (n) and much smaller primary polar body (n)
primary follicles → secondary follicles → Graafian follicles
ovulation - Graafian follicle migrates to ovary surface
secondary oocyte released into fallopian tube
secondary oocyte begins meiosis II - stops at metaphase II until fertilisation
break down oogenesis after fertilisation
meiosis II completed
produces ovum and second polar body
Graafian follicle → corpus luteum
what is the difference between spermatogenesis and oogenesis:
things produced
spermatogenesis: 4 functional spermatazoam produced
oogenesis: 1 functional ovum produced
what is the difference between spermatogenesis and oogenesis:
arrests/suspensions
spermatogenesis: none (continuous)
oogenesis: 2
what is the difference between spermatogenesis and oogenesis:
polar bodies
spermatogenesis: none made
oogenesis: polar bodies made
what is the difference between spermatogenesis and oogenesis:
when in life
spermatogenesis: puberty → old age
oogenesis: puberty → menopause
what is the difference between spermatogenesis and oogenesis:
motility of gametes
spermatogenesis: motile - move itself
oogenesis: non-motile - moved by cilia
what is the difference between spermatogenesis and oogenesis:
cytoplasm present
spermatogenesis: very little cytoplasm in gamete
oogenesis: much cytoplasm in gamete
what causes a penis to become erect?
vasodilation of arterioles supplying blood to penis
vasoconstriction of venules leaving penis
what causes ejaculation?
movement of penis
muscular contractions of smooth muscle in walls of epididymis, vas deferens and penis
ejaculation of semen into vagina
how does semen enter the uterus?
force of ejaculation causes sperm cells to be propelled
cervix → uterus
what is an orgasm?
the combination of physical and psychological events at maximum intensity
what are the stages of fertilisation?
capacitation
acrosome reaction
fusion of sperm and secondary oocyte membrane
cortical reaction
fusion of sperm and ovum
what happens during capacitation?
cholesterol and glycoproteins removed from acrosome membrane
membrane becomes more fluid and more permeable to Ca2+
what happens during the acrosome reaction?
acrosome membrane fuses with cell surface membrane
releases hydrolytic enzymes
digest cells of corona radiata
on contact with zona pellucida - acrosome releases protease
hydrolyses zona pellucida
what happens during the fusion of the sperm and secondary oocyte membranes?
cell membrane of sperm cell fuses with membrane of secondary oocyte
now called ovum
what happens during the cortical reaction?
oocyte smooth endoplasmic reticulum releases Ca2+ into oocyte cytoplasm
cortical granules fuse with cell membrane
release contents by exocytosis
hardening of zona pellucida
forms fertilisation membrane
prevents polyspermy
what happens during the fusion of the sperm and ovum?
entry of sperm triggers meiosis II to complete
sperm nucleus (n) and ovum nucleus (n) → zygote nucleus (2n)
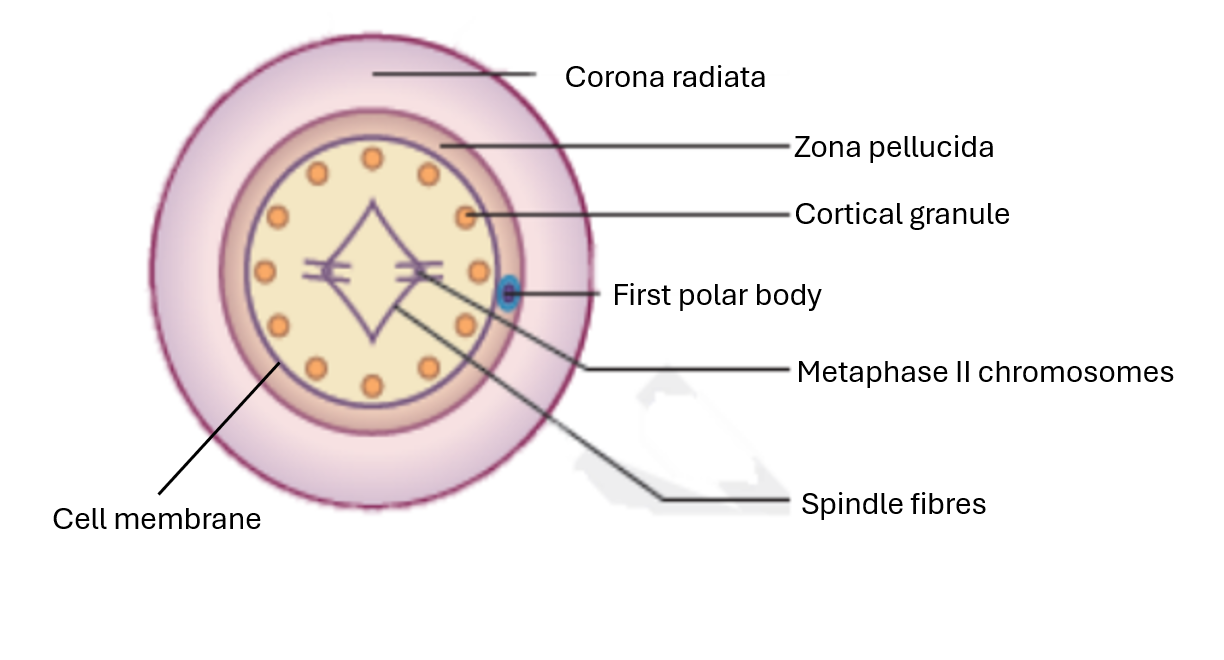
label the secondary oocyte before fertilisation
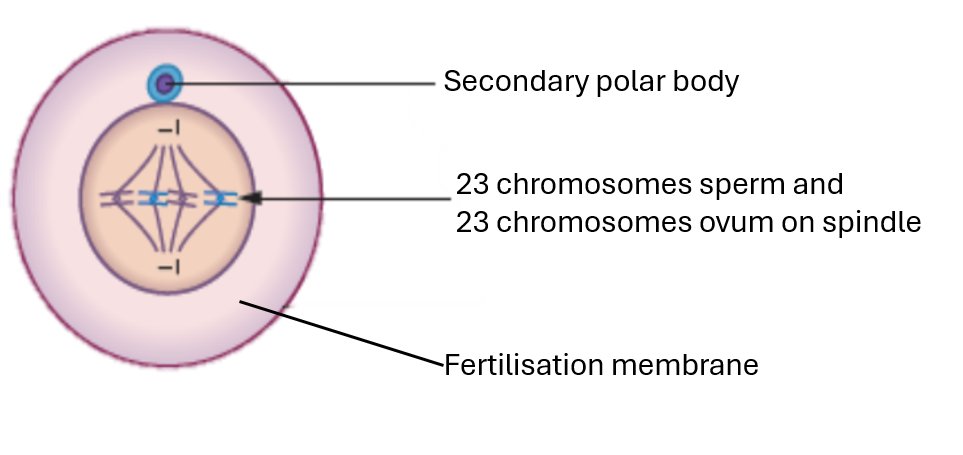
label the secondary oocyte after fertilisation
what happens to the zygote prior to implantation?
zygote undergoes cleavage (series of mitotic divisions)
forms morula - solid ball of 16 cells
cleavage continues
hollow ball of cells form - blastocyst
what is the outer layer of cells of the blastocyst called?
trophoblast
what does the trophoblast develop into?
inner cell mass (embryoblast)
trophoblastic villi
chorion
amnion
what causes the implantation window?
blastocyst moves down fallopian tube
endometrial lining of uterus thickens
receives increased blood supply
endometrium receptive to blastocyst
define implantation
the attachment and sinking in of the blastocyst into the endometrium
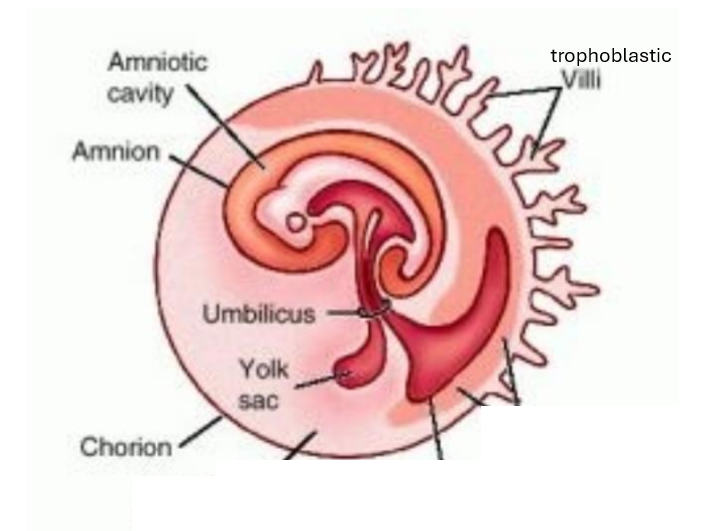
label the diagram
what is the role of the trophoblastic villi?
penetrate endometrium during implantation
increase surface area for absorption of nutrients from endometrium/mother’s blood
what is the role of the amnion?
contains amniotic fluid
acts as shock absorber
protects fetus from physical injury
what is the role of the chorion?
gives rise to chorionic villi
increase efficientcy of exchange between maternal and fetal blood in placenta
what is the role of the placenta?
endocrine gland
exchange site
physical barrier
provides passive immunity
protects from mother’s immune system
what is an endocrine gland?
produces and releases hormones directly into bloodstream
what hormones are produced by the placenta?
hCG
progesterone
oestrogen
what substances are exchanged between the mother and fetus’s blood?
nutrients
waste products
respiratory gases
M → F: glucose, amino acids, fatty acids
F → M: CO2, urea
are the mother’s and fetus’s blood in contact?
no
how is exchange in the placenta maximised?
microvilli - large surface area
thin walls - most effective for exchange (eg diffusion, pinocytosis)
counter current flow - maintains concentration gradient/equilbrium never reached
what is protected from the mother’s high blood pressure?
fragile fetal capillaries
what is passive immunity and how does this occur in the placenta?
antibodies made by someone else
mother’s antibodies cross placenta
provide protection for the fetus
how does the placenta ensure that the mother’s immune system does not generate an immune response towards the fetus?
cell walls of chorionic villi fuse
no space between them
syncitium forms
ensures 2 bloods do not mix
migratory immune cells (granulocytes) cannot get through to fetal blood
when might the placenta not provide immunological protection?
some spontaneous abortions
Rhesus disease
pre-eclampsia
some viruses (eg rubella)
drugs/alcohol cross the placenta
what is Rhesus disease?
Rhesus -ve mother against Rhesus +ve fetus
destruction of blood cells by antibodies
what is pre-eclampsia?
occurs in 2nd trimester
very high blood pressure
1 cause is abnormal immune response towards placenta
how long is the umbilical chord?
approx 60cm
where does the umbilical chord develop from?
the placenta
where does the umbilical artery go?
2 umbilical arteries
away from fetus
deoxygenated
low in nutrients
high in waste
where does the umbilical vein go?
1 umbilical vein
to the fetus
oxygenated
high in nutrients
low in waste