Red Lesions
1/163
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
164 Terms
what are raised, fluid-filled lesions less than 1 cm?
vesicle
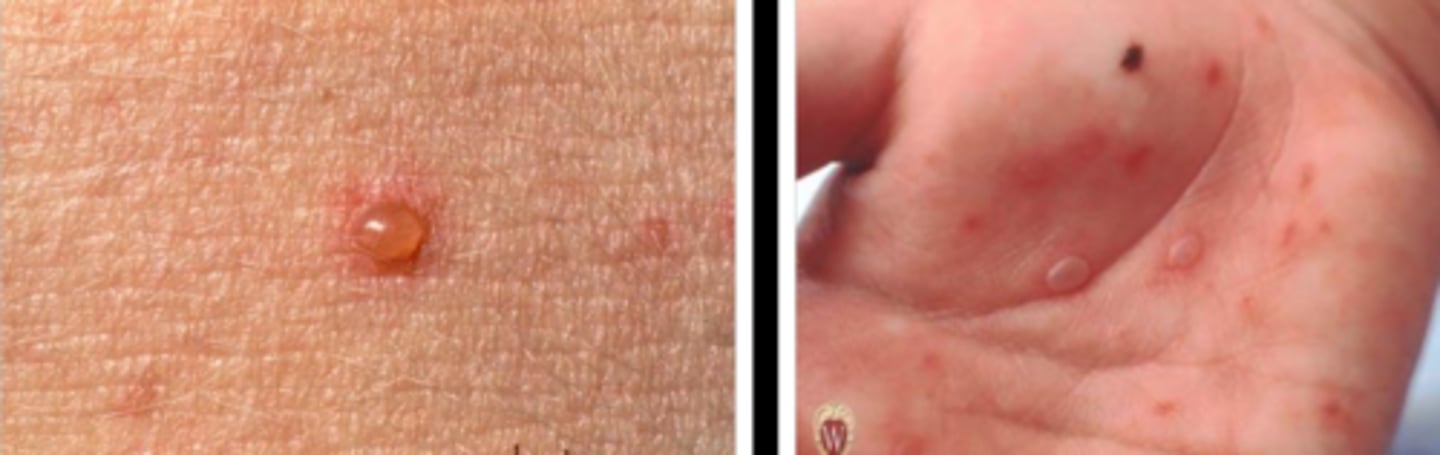
what are raised, fluid-filled lesions more than 1 cm?
bulla
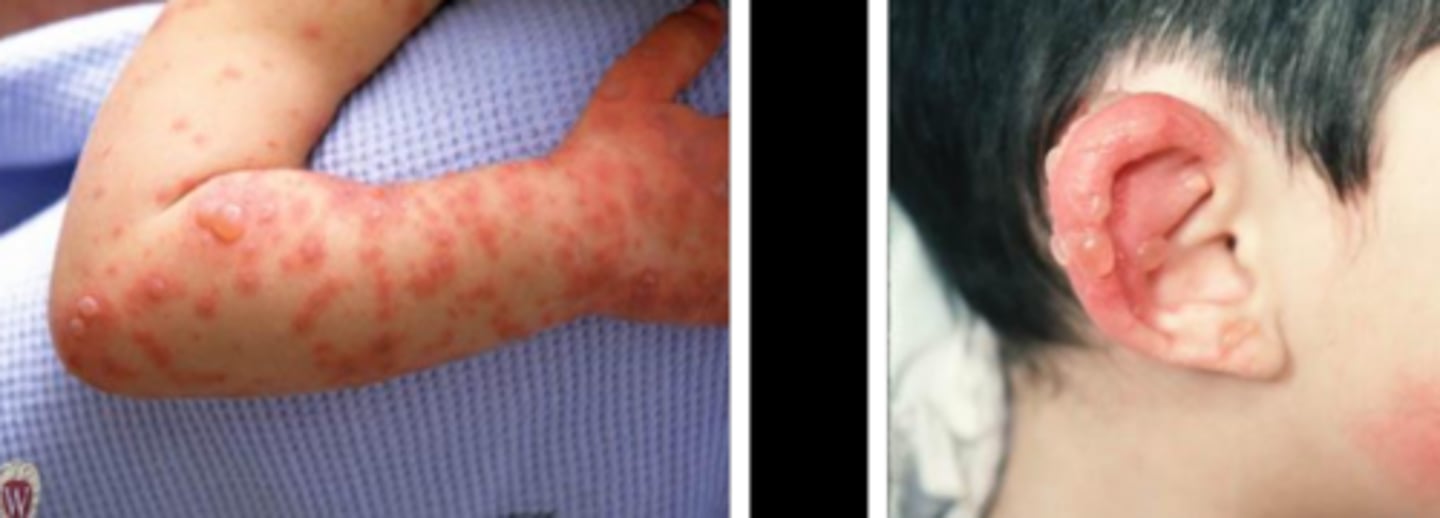
(erosions/ulcers) present with a ring of red epithelium
ulcers
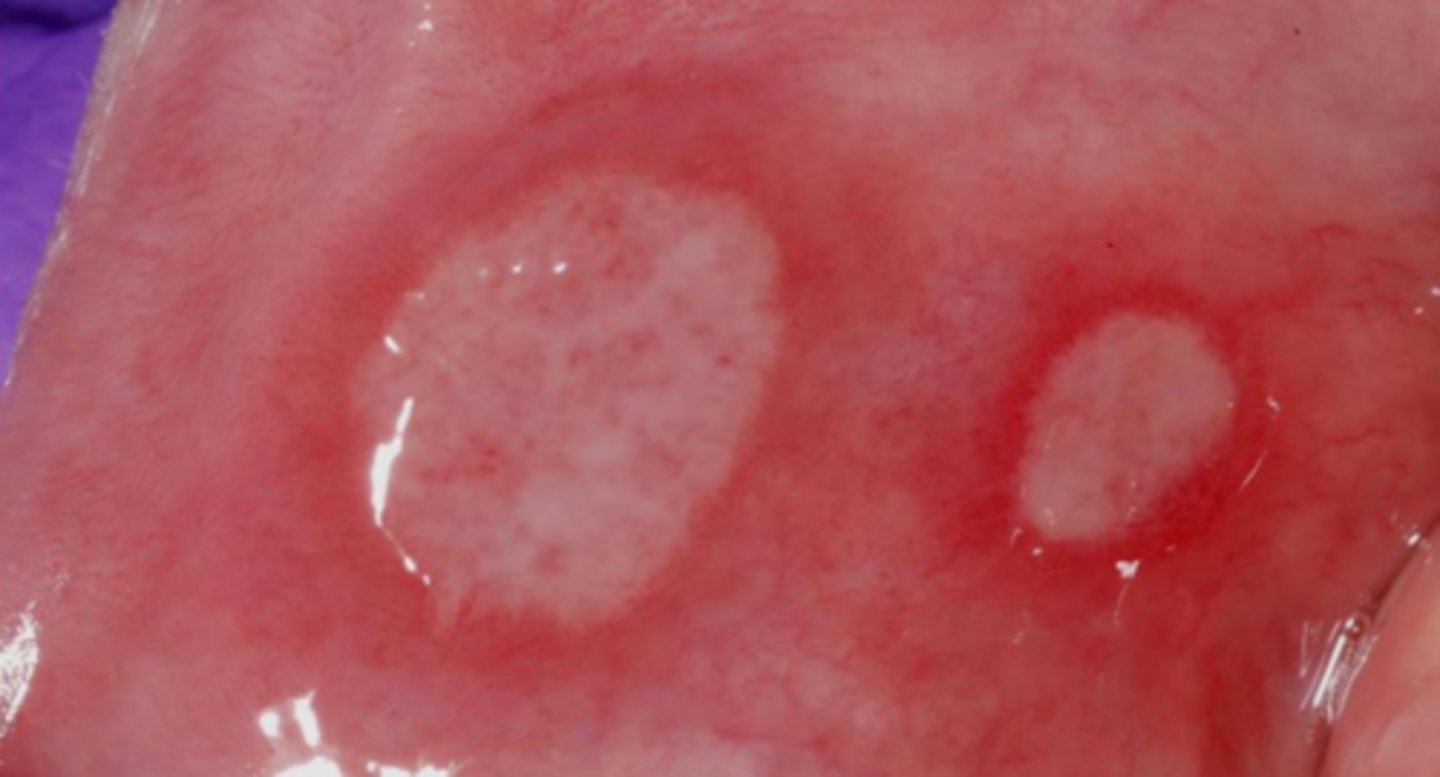
a vesicle that eventually loses the overlying epithelium present as an _______
ulcer
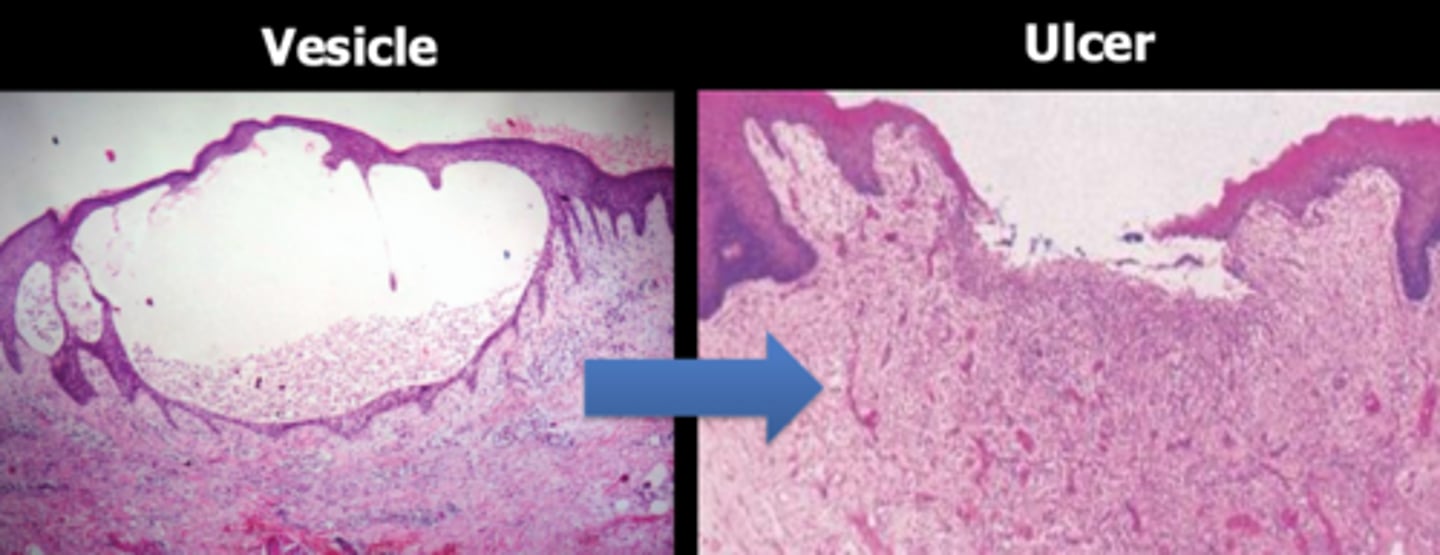
(t/f) vesicles are often not seen because they rupture early
true; presents as an ulcer
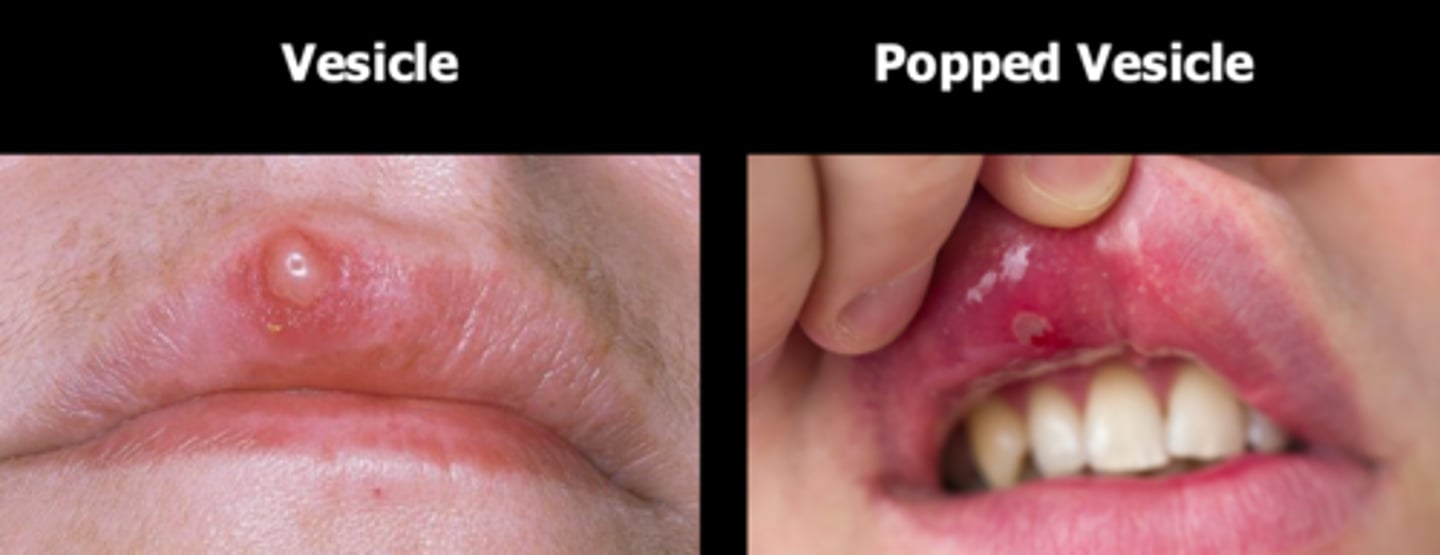
what kind of vesicular surface lesions often give patients oral discomfort as the chief complaint, may be local or generalized, are transient, and associated with Nikolsky sign?
vesicular-ulcerated surface lesions
(t/f) vesicular-ulcerated surface lesions are always acute and last 1-2 weeks
false; vesicular-ulcerated surface lesions can be acute or chronic, lasting months
what kind of vesicular surface lesions includes epidermyolysis bullosa?
vesicular-bullous lesions (hereditary)
what kind of vesicular surface lesions includes herpes simplex, herpes zoster, varicella, herpangina, HFM disease, mononucleosis, and measles?
vesicular-bullous lesions (viral)
what kind of vesicular surface lesions includes erosive lichen planus, pemphigus vulgaris, mucous membrane pemphigoid, bullous pemphigoid, and lupus erythematosus?
vesicular-bullous lesions (autoimmune)
(t/f) most vesicular-bullous lesions start as vesicles then turn into ulcers. depending when you see the patient, they may present with only vesicles, only ulcers, or both.
true
what vesicular-bullous lesion is a hereditary defect in the attachment mechanisms of epithelial cells?
epidermolysis bullosa
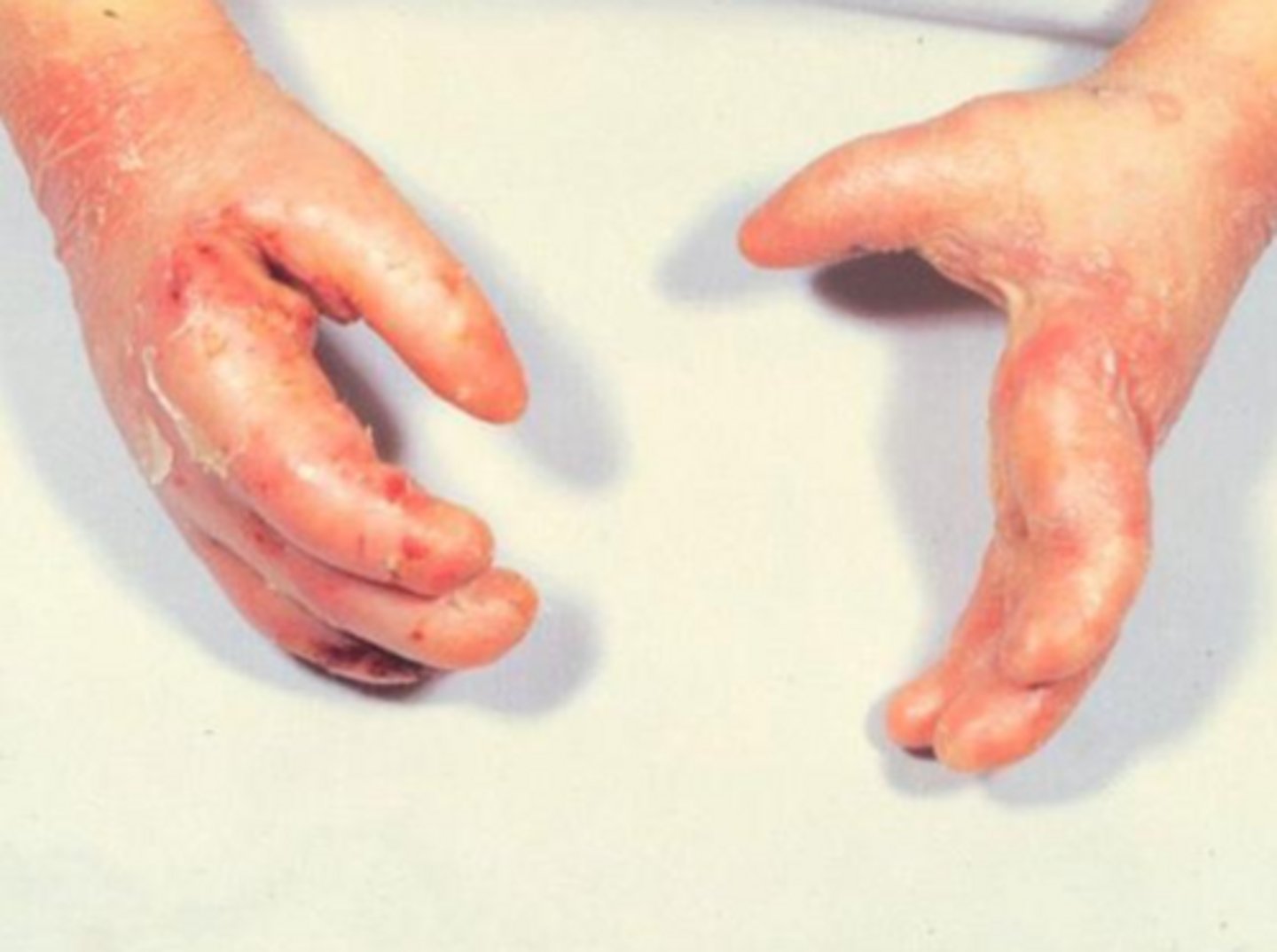
(t/f) epidermolysis bullosa has no cure and requires supportive management
true
(t/f) vesicles and bullae associated with epidermolysis bullosa are caused by major traumas. oral lesions will heal with scarring, but have no impact on oral function.
false; vesicles and bullae associated with epidermolysis bullosa are caused by major traumas. oral lesions will heal with scarring, and restrict opening.
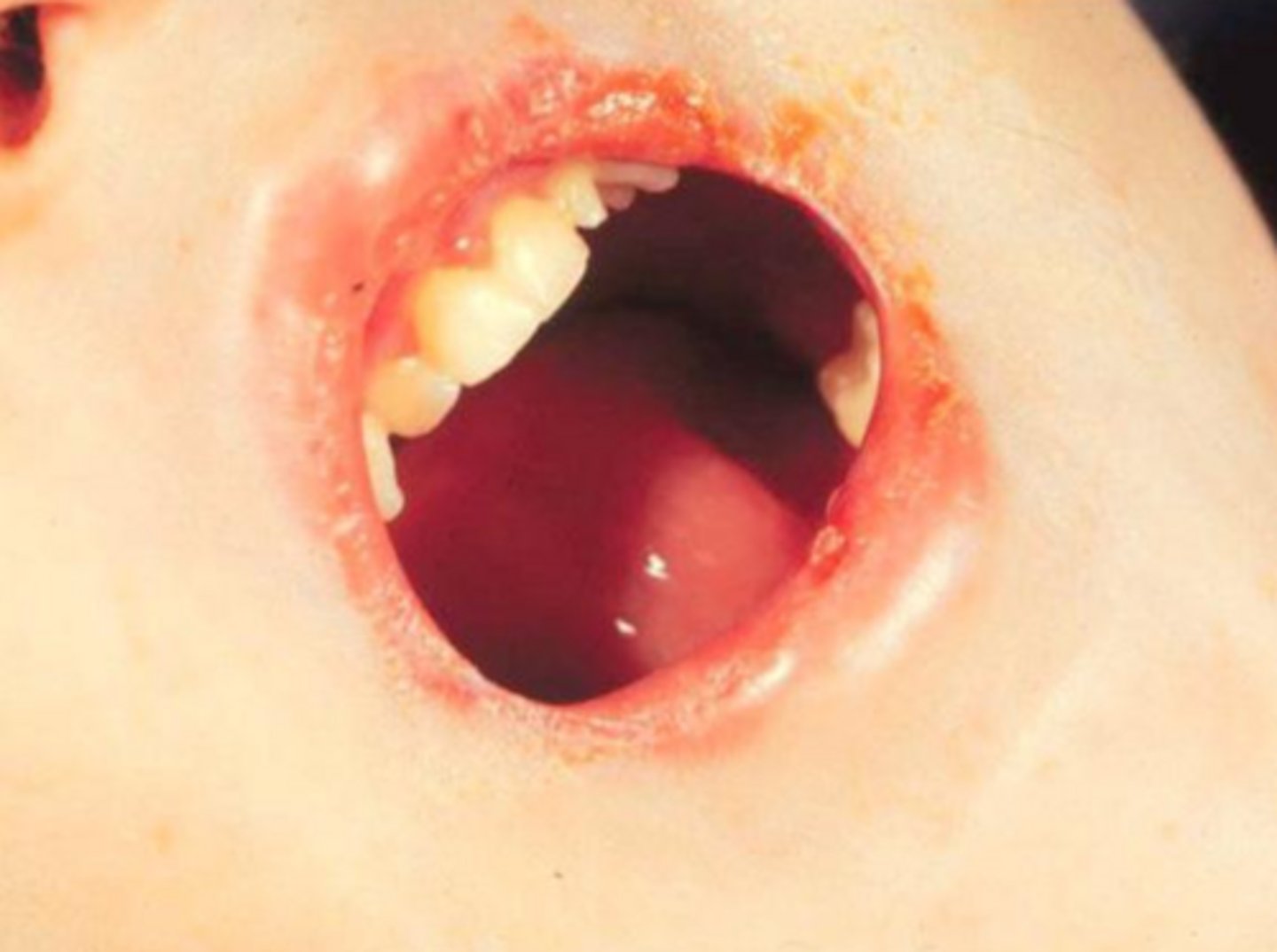
what hereditary vesicular-bullous lesion leads to hypoplastic teeth, is treated with antibiotics and corticosteroids, and can be avoided by being careful to not cause trauma?
epidermolysis bullosa
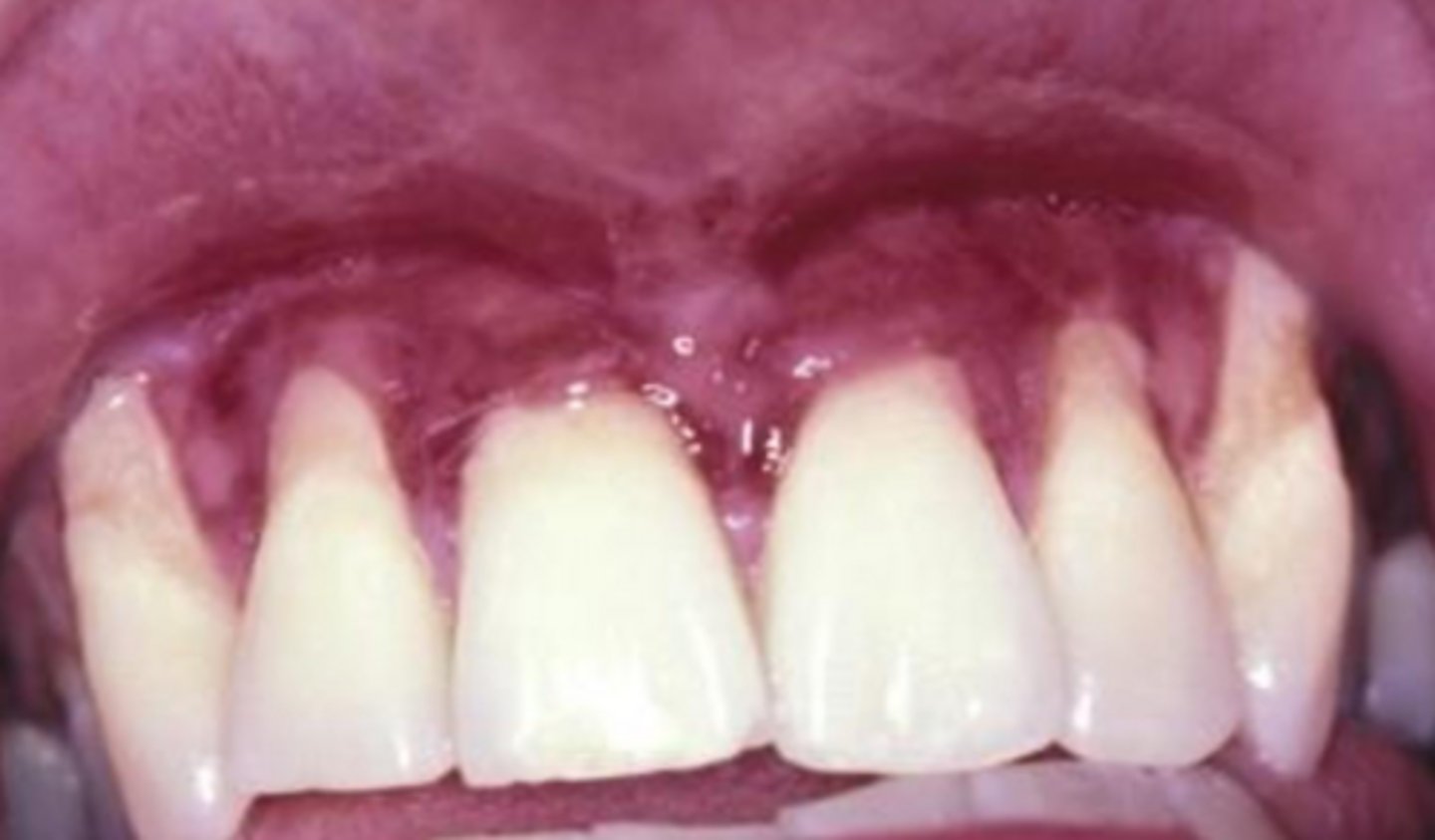
viral vesicular-bullous lesions have a(n) (acute/chronic) onset. what are the 3 signs they all present with (except recurrent herpes and zoster)?
acute;
1. malaise
2. fever
3. lymphadenopathy
(t/f) viral vesicular-bullous lesions present with multiple ulcers and all have a vesicle stage
false; viral vesicular-bullous lesions present with multiple ulcers and all have a vesicle stage EXCEPT infectious mononucleosis (no vesicle formation)
what are the 2 viral vesicular-bullous lesions that recur?
1. herpes simplex (HSV1 and HSV2)
2. herpes zoster
what human herpesvirus is human herpes virus 1 (HSV1)?
HHV1
what human herpesvirus is human simplex virus 2 (HSV2)?
HHV2
what human herpesvirus is the varicella-zoster virus (VZV)?
HHV3
what human herpesvirus is the epstein-barr virus (EBV)?
HHV4
what human herpesvirus is the kaposi sarcoma herpes virus (KSHV)?
HHV8
what 2 human herpesviruses are herpes simplex?
1. HHV1
2. HHV2
which herpes simplex spreads predominantly through infected saliva or active perioral lesions, adapted best to the oral, facial, and ocular areas, and is common in developed nations (20% exposure at age 5 and 50-60% at adulthood)?
HSV1
which herpes simplex is adapted best to the genital zones and transmitted through sexual contact (typically involving the genitalia)?
HSV2
(t/f) genital HSV1 and oral/pharyngeal HSV2 is impossible
false; genital HSV1 and oral/pharyngeal HSV2 is possible but infrequent
which phase of herpes simplex is the initial exposure of an individual without antibodies to the virus?
primary herpes (primary herpetic gingivostomatitis)
which phase of herpes simplex is often asymptomatic or subclinical (60-80%)?
primary herpes (primary herpetic gingivostomatitis)
(t/f) the primary infection of herpes simplex typically occurs at a young age
true
during which phase of herpes simplex is the virus taken up by sensory nerves?
latency
what is the most common site for HSV1 in the latency phase?
trigeminal ganglion
which phase of herpes simplex occurs when the virus reactivates (from UV radiation, trauma, immunosuppression)?
recurrent
during which phase of herpes simplex is the epithelium supplied by the sensory ganglion affected?
recurrent
which phase of herpes simplex is associated with fever, malaise, and lymphadenopathy?
primary herpes (primary herpetic gingivostomatitis)
which phase of herpes simplex causes gingival swelling, erythema, and multiple vesicles and ulcers?
primary herpes (primary herpetic gingivostomatitis)
(t/f) primary herpes (primary herpetic gingivostomatitis) presents with oral symptoms 60-80% of the time
false; primary herpes (primary herpetic gingivostomatitis) presents with subclinical symptoms 60-80% of the time, but oral symptoms are seen 20-40%
(t/f) primary herpes (primary herpetic gingivostomatitis) can present with ulcerations on the keratinized (gingiva, hard palate, tongue) or non-keratinized tissues (soft palate, buccal mucosa, ventral tongue)
false; primary herpes (primary herpetic gingivostomatitis) must present with ulcerations on the keratinized AND non-keratinized tissues
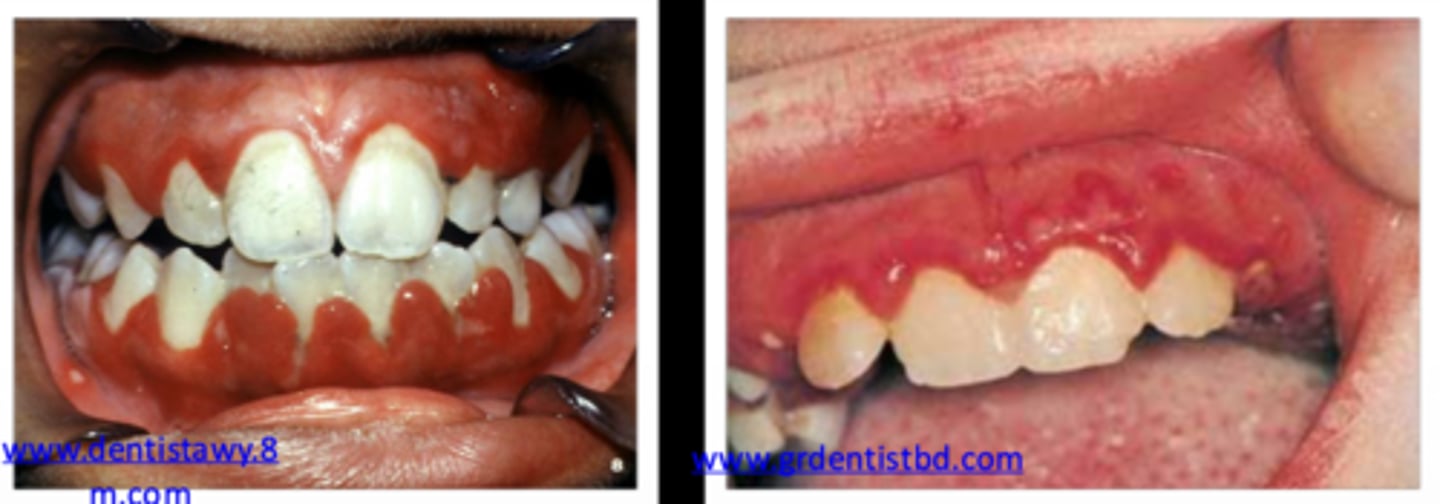
which phase of herpes simplex will numerous pinhead vesicles develop that rapidly rupture (developing central ulcerations) and sometimes appear with yellow fibrin that can coalesce?
primary herpes (primary herpetic gingivostomatitis)
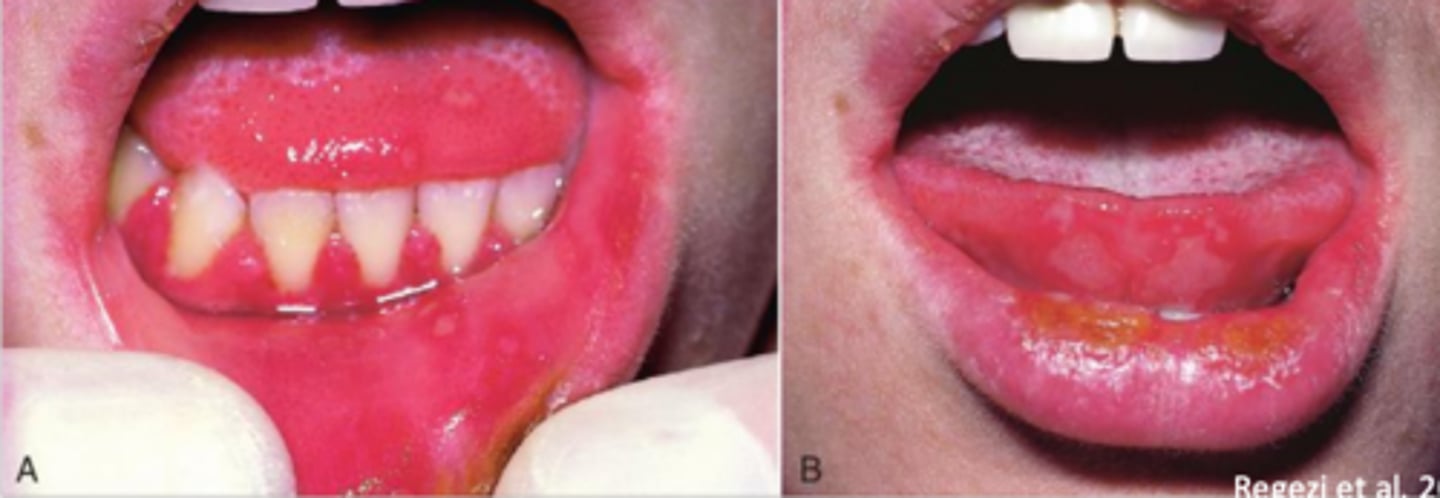
which phase of herpes simplex will the gingiva always enlarge and be painful and extremely red?
primary herpes (primary herpetic gingivostomatitis)
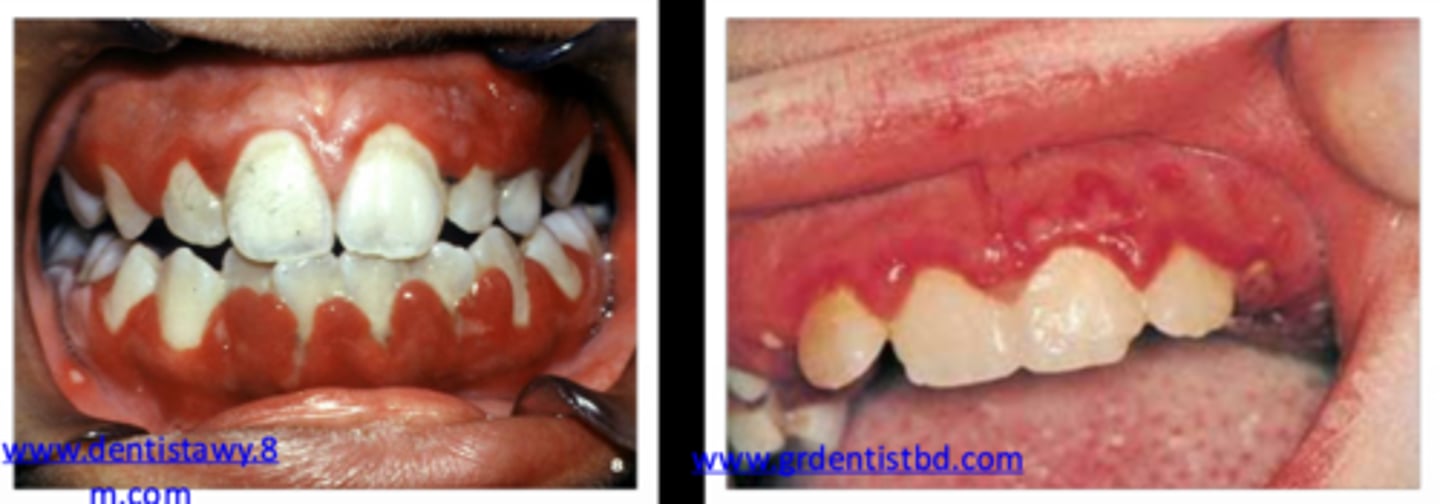
(t/f) primary herpes (primary herpetic gingivostomatitis) may involve the vermillion of the lips, cause satellite vesicles on the skin, self inoculate, and resolves in 7-14 days
true
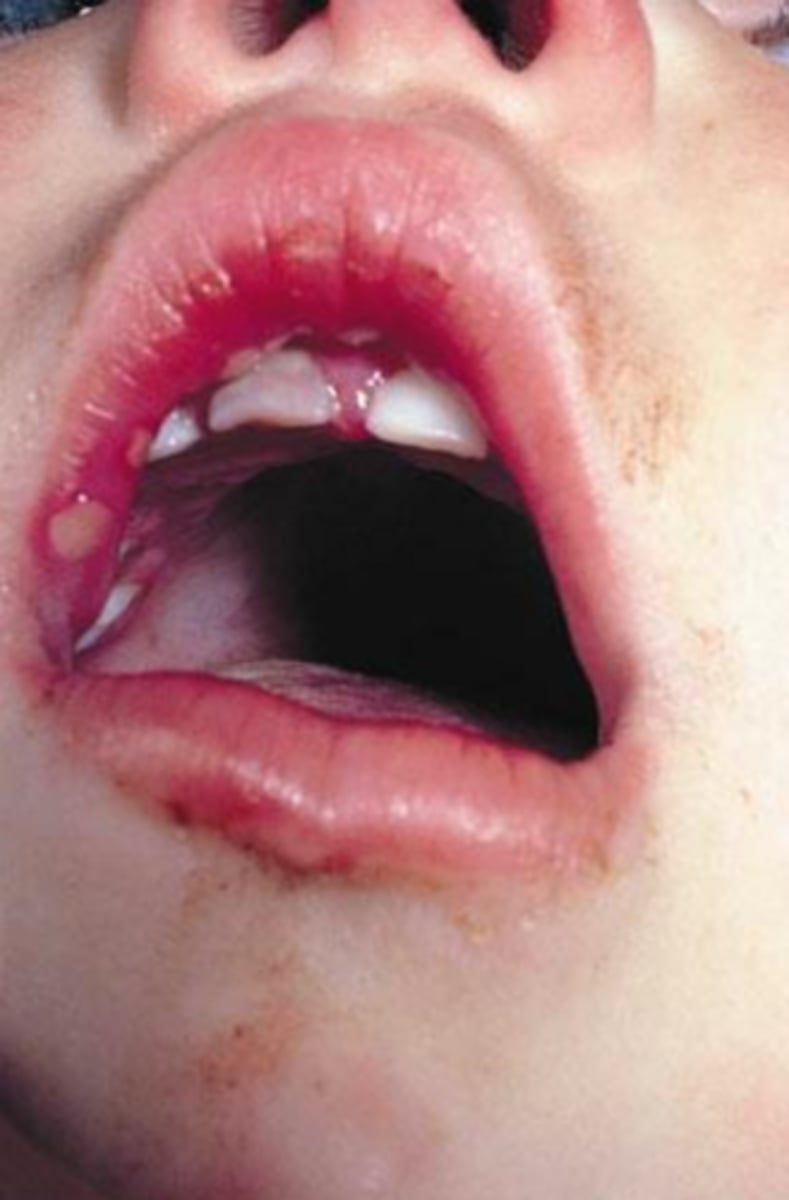
(t/f) primary herpes (primary herpetic gingivostomatitis) is treated with antibiotics within 5 days after the onset of symptoms
false; primary herpes (primary herpetic gingivostomatitis) is treated with antivirals within 5 days after the onset of symptoms
(t/f) latent herpes simplex remains in the regional nerve ganglion of ONE single nerve
true
during which phase of herpes simplex can asymptomatic viral shedding occur (virus comes out of nerve and into mouth)?
latent
which phase of herpes simplex is associated with tingling, burning, and paresthesia?
recurrent; these are the prodrome of reactivation
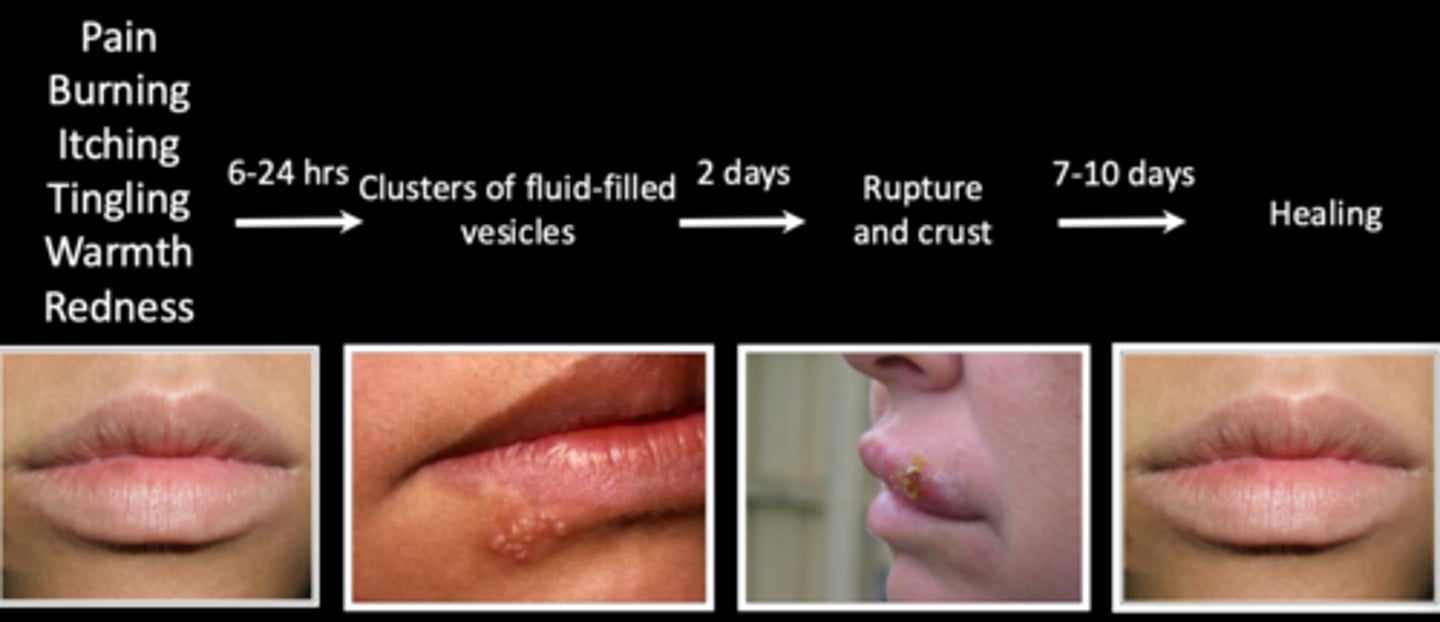
which phase of herpes simplex is referred to as a cold sore or fever blister and is common in the US population?
recurrent
which phase of herpes simplex manifests with small clusters of vesicles and ulcers and appears on the perioral skin and keratinized oral mucosal surfaces?
recurrent
what type of herpes is a recurrent infection that appears on the vermillion vorder and adjacent skin of the lips?
herpes labialis
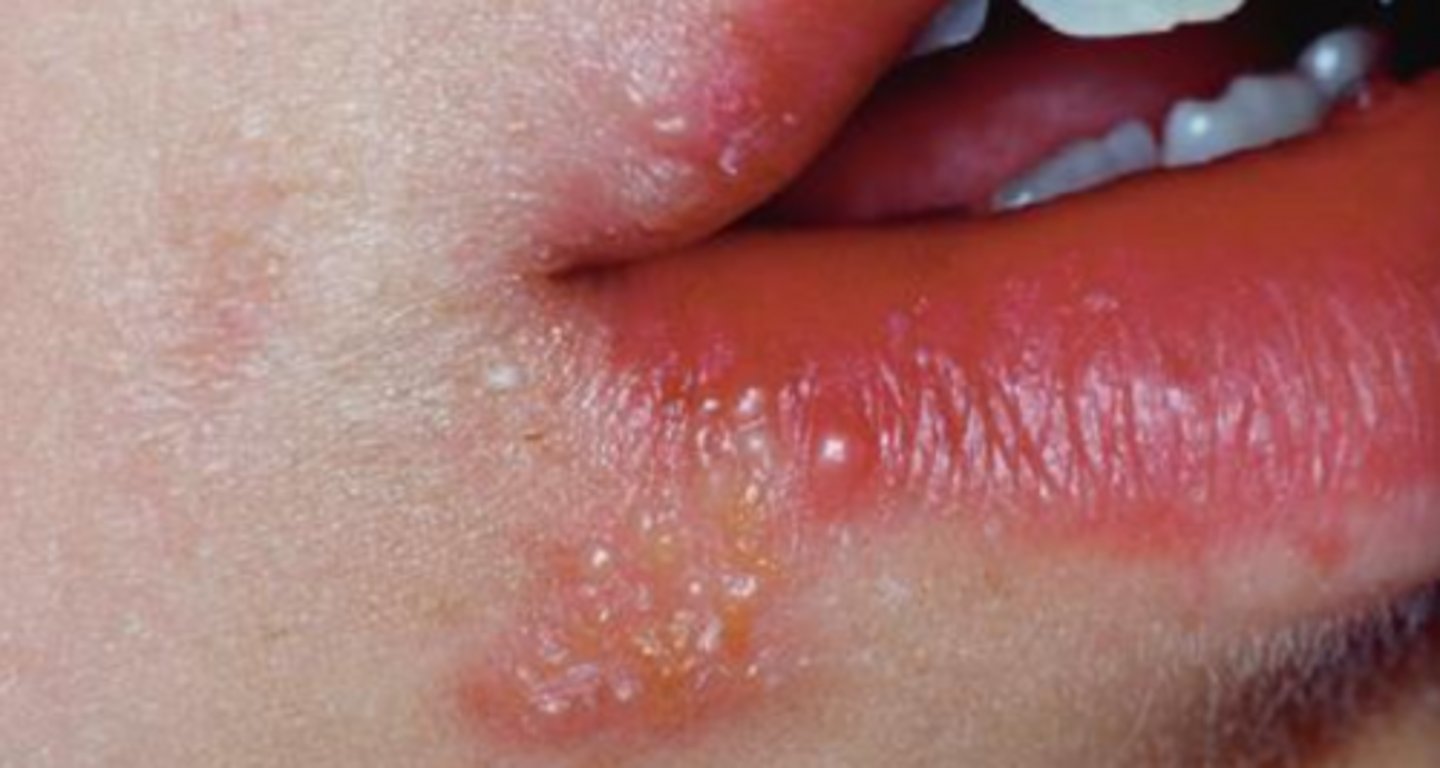
which phase of herpes simplex will NOT appear with lymphadenopathy, fever, or malaise?
recurrent
(t/f) recurrent herpes presents with ulcerations limited to the keratinized tissues (gingiva, hard palate, tongue)
true
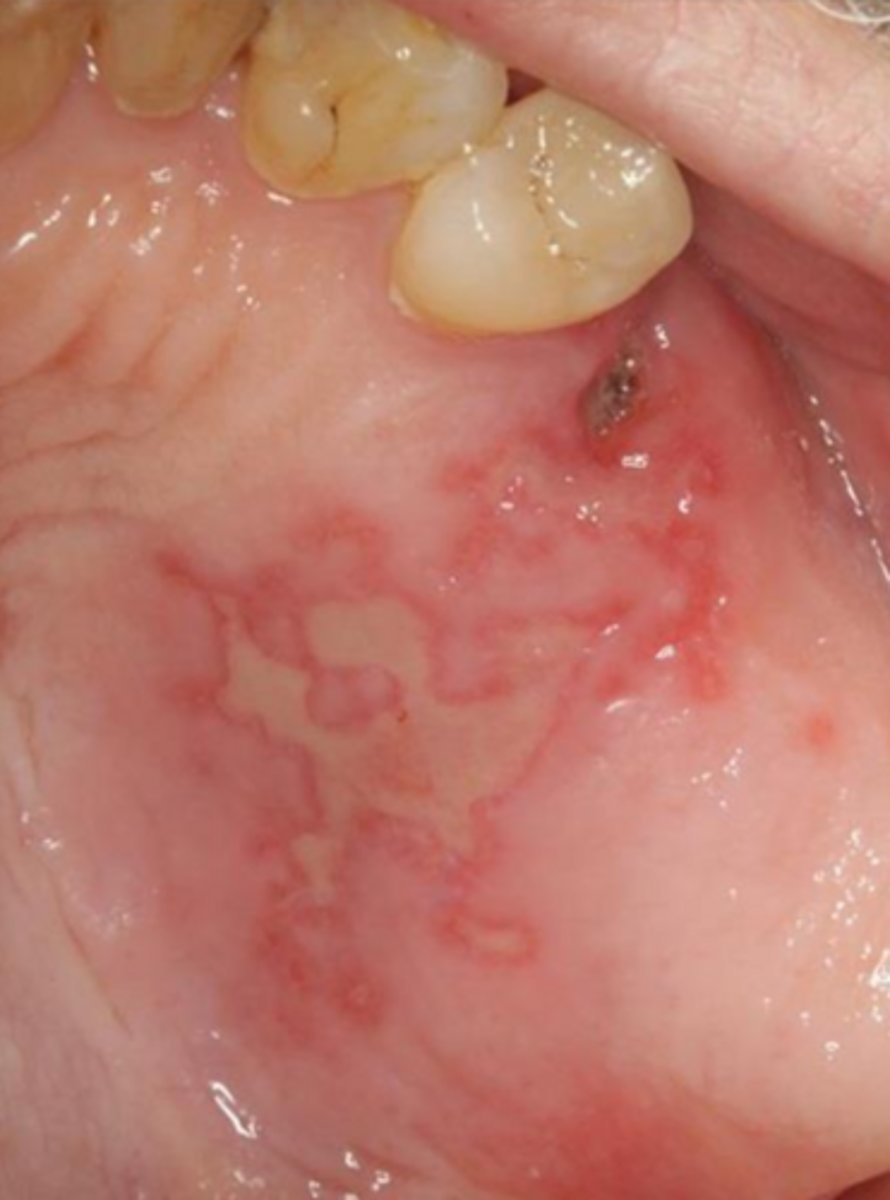
what are the free floating epithelial cells commonly seen in recurrent herpes (but not specific to herpes)?
tzanck cells
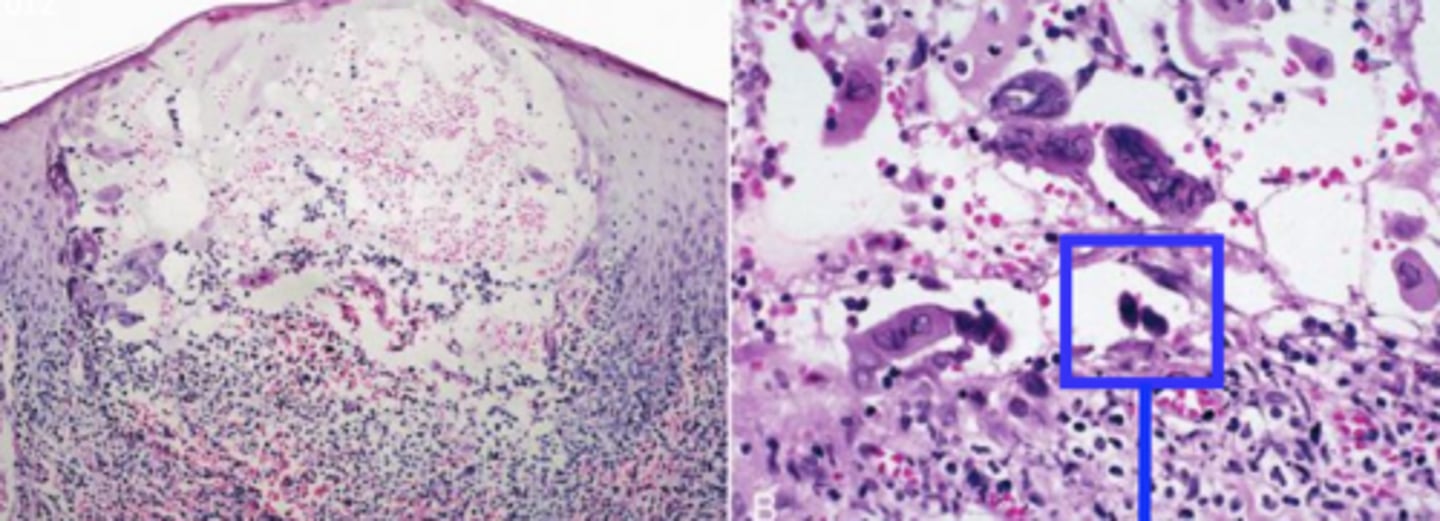
(t/f) recurrent herpes is treated with antivirals and is most effective taken before the onset of the prodrome
false; recurrent herpes is treated with antivirals and is most effective when taken at the prodrome, but antiviral can be useful for prophylactic maintenance therapy
what herpes presentation is an infection of the fingers or thumbs (used to most common with dentists)?
herpetic whitlow
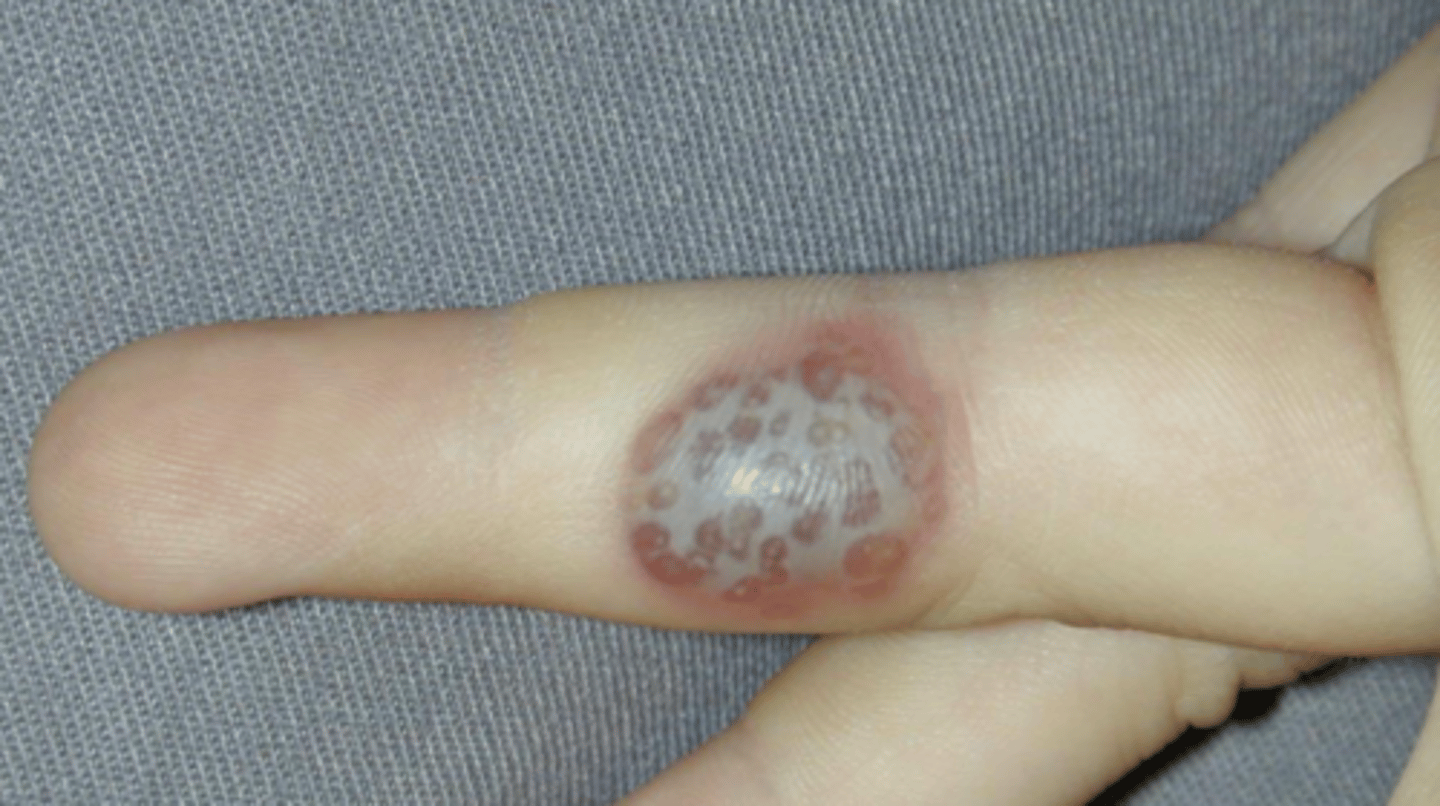
what herpes presentation is an infection found in wrestlers or rugby players with contaminated abrasions?
herpes gladiatorum/scrumpox
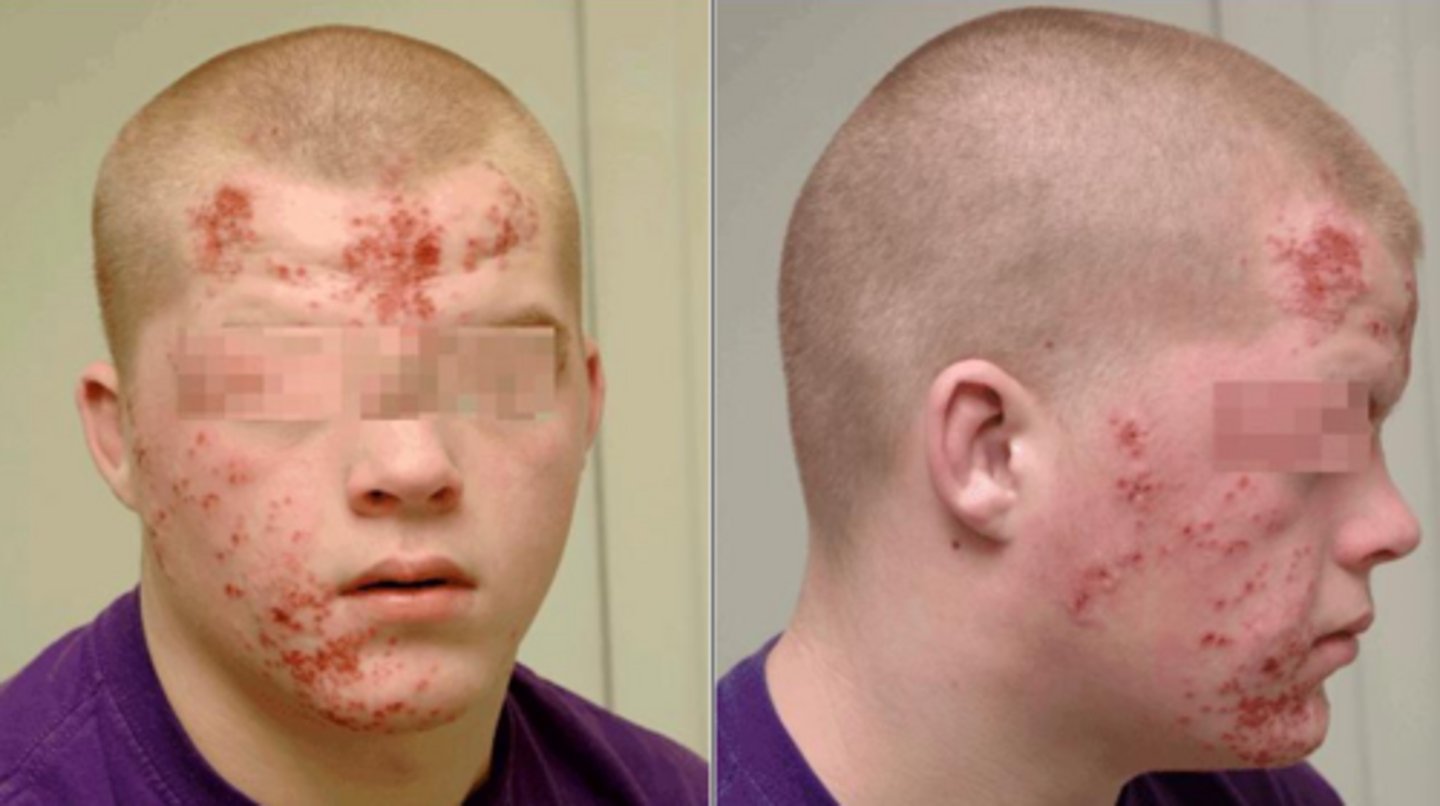
what herpes presentation is an infection over the beard region from minor injuries created by daily shaving?
herpes barbae
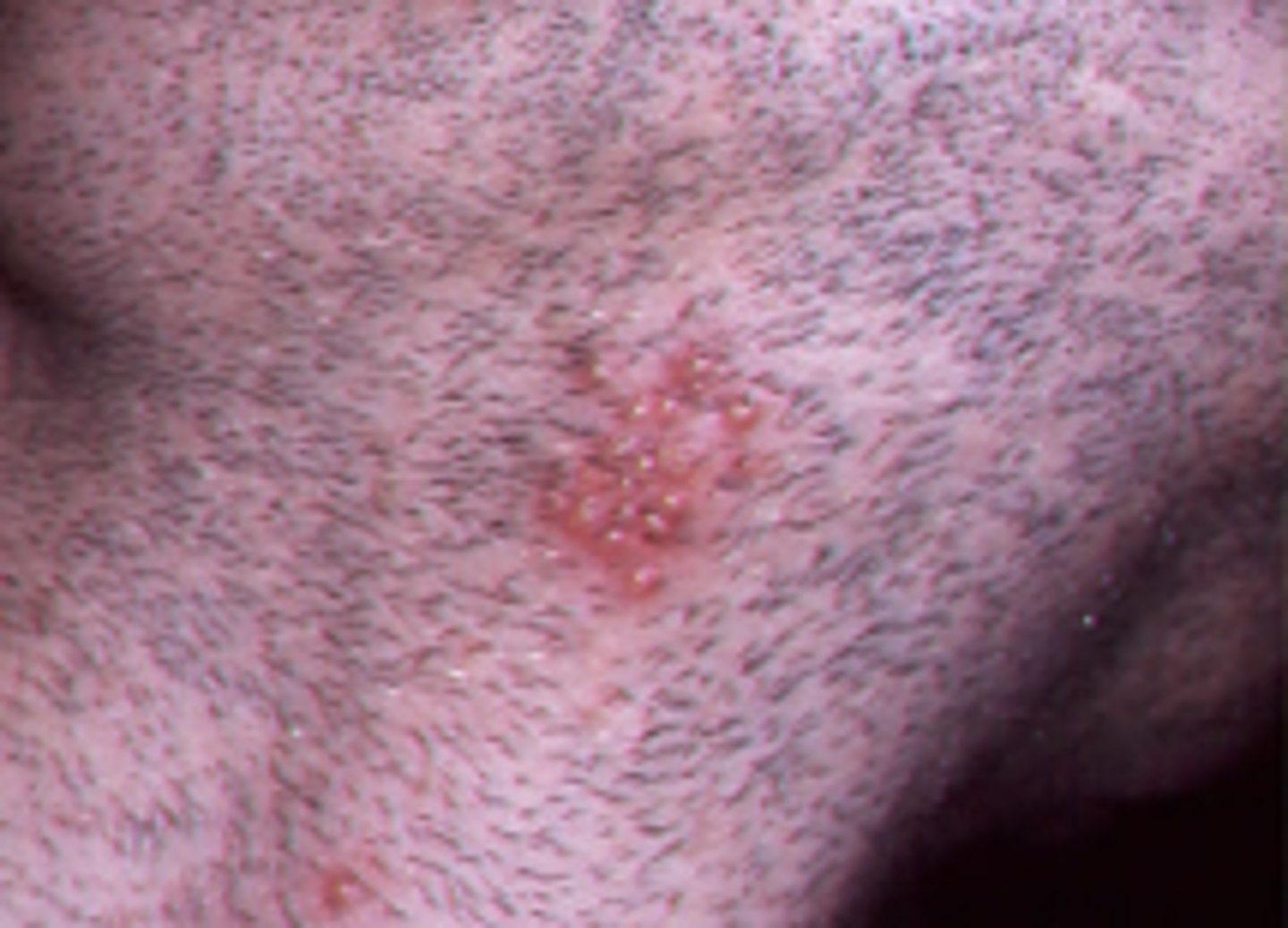
(t/f) recurrent herpes in immunocompromised patients have extensive lesions (not limited to keratinized tissue)
true
what viral vesicular-bullous lesion is also known as chickenpox?
varicella
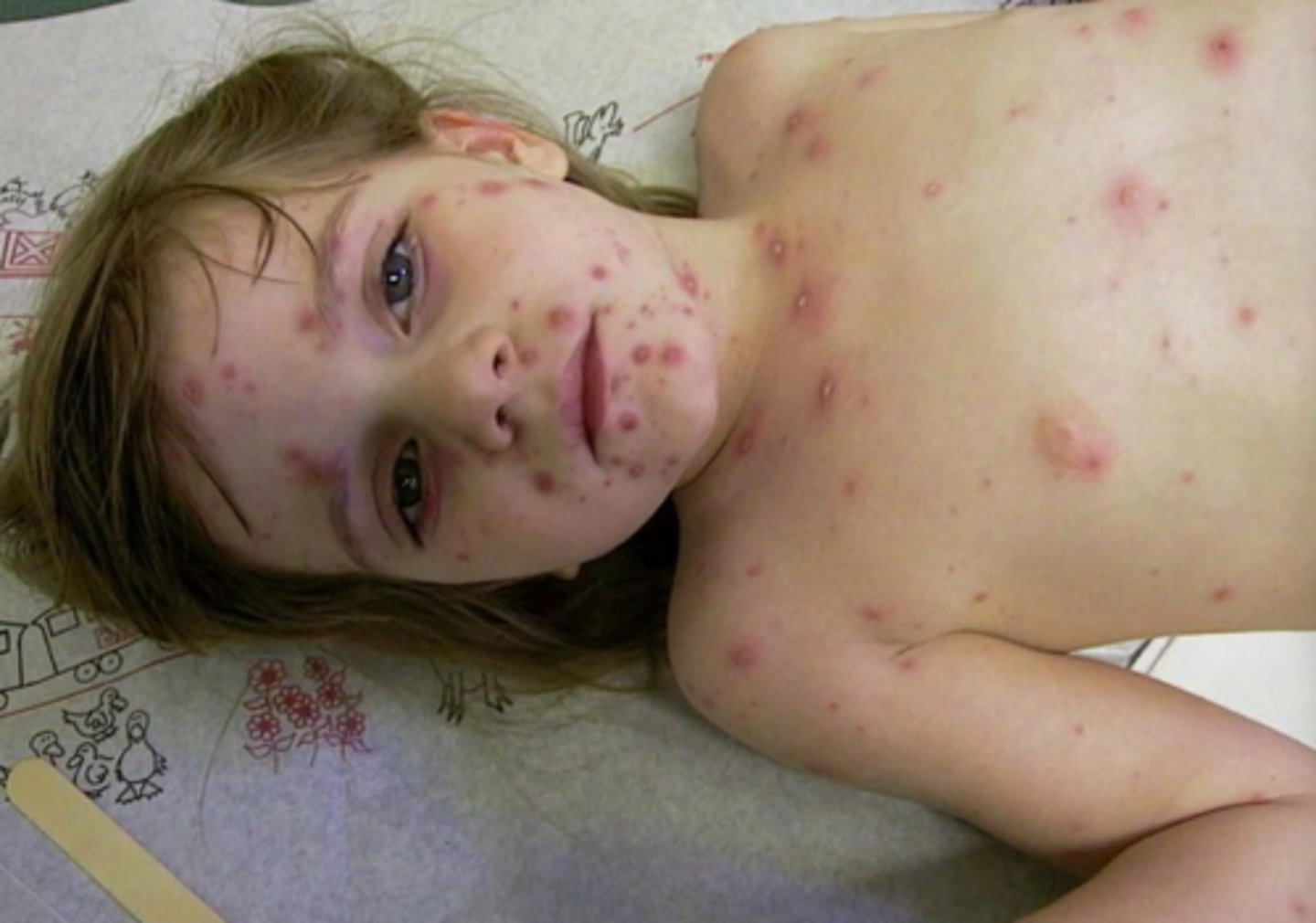
what viral vesicular-bullous lesion has a prodrome of malaise, fever, lymphadenopathy, and successive crops of pruritic papules, vesicles, and ulcers on the skin that begin on the trunk and spread to the extremities and face?
varicella
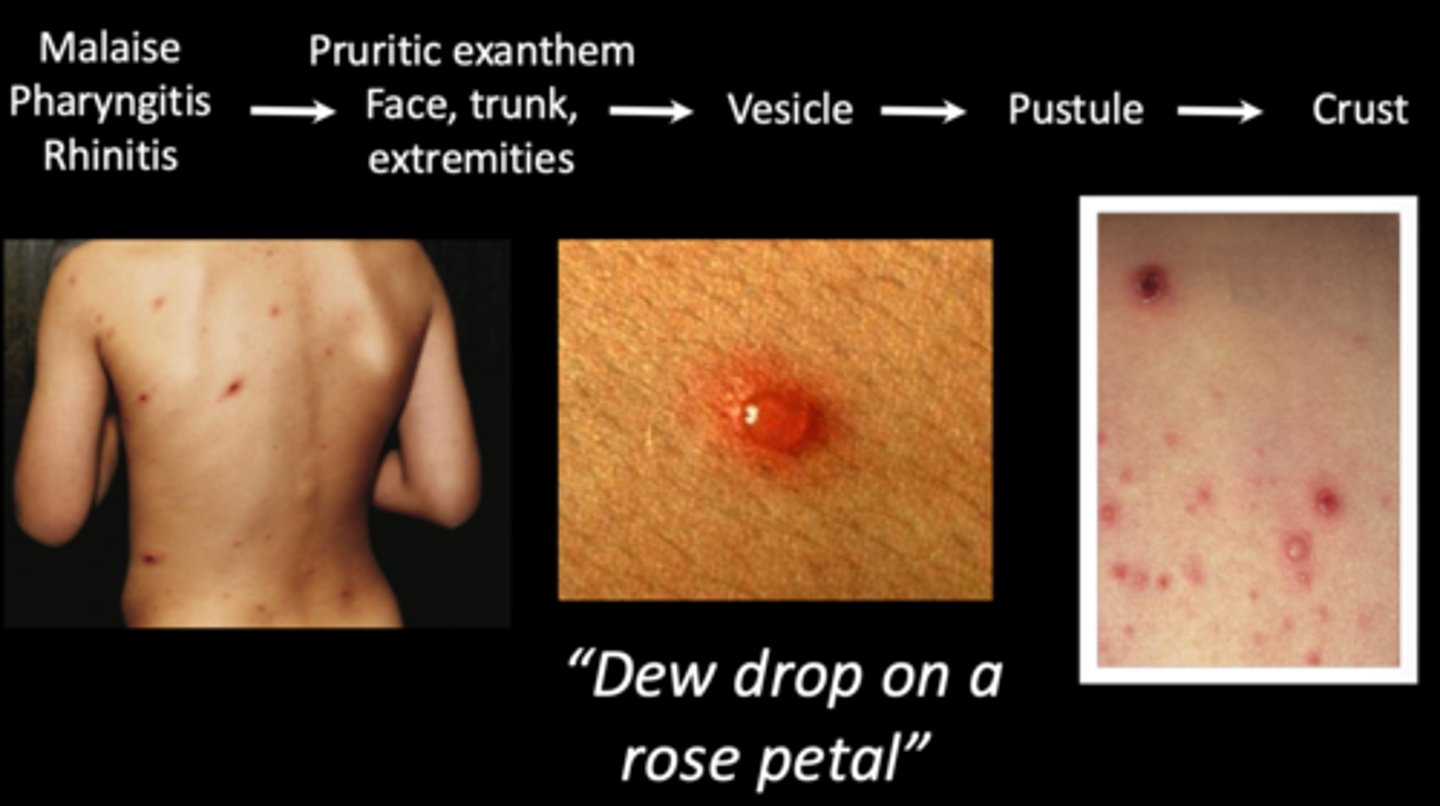
what viral vesicular-bullous lesion is identical to herpes simplex microscopically and may occasionally cause oral vesicles and ulcers?
varicella
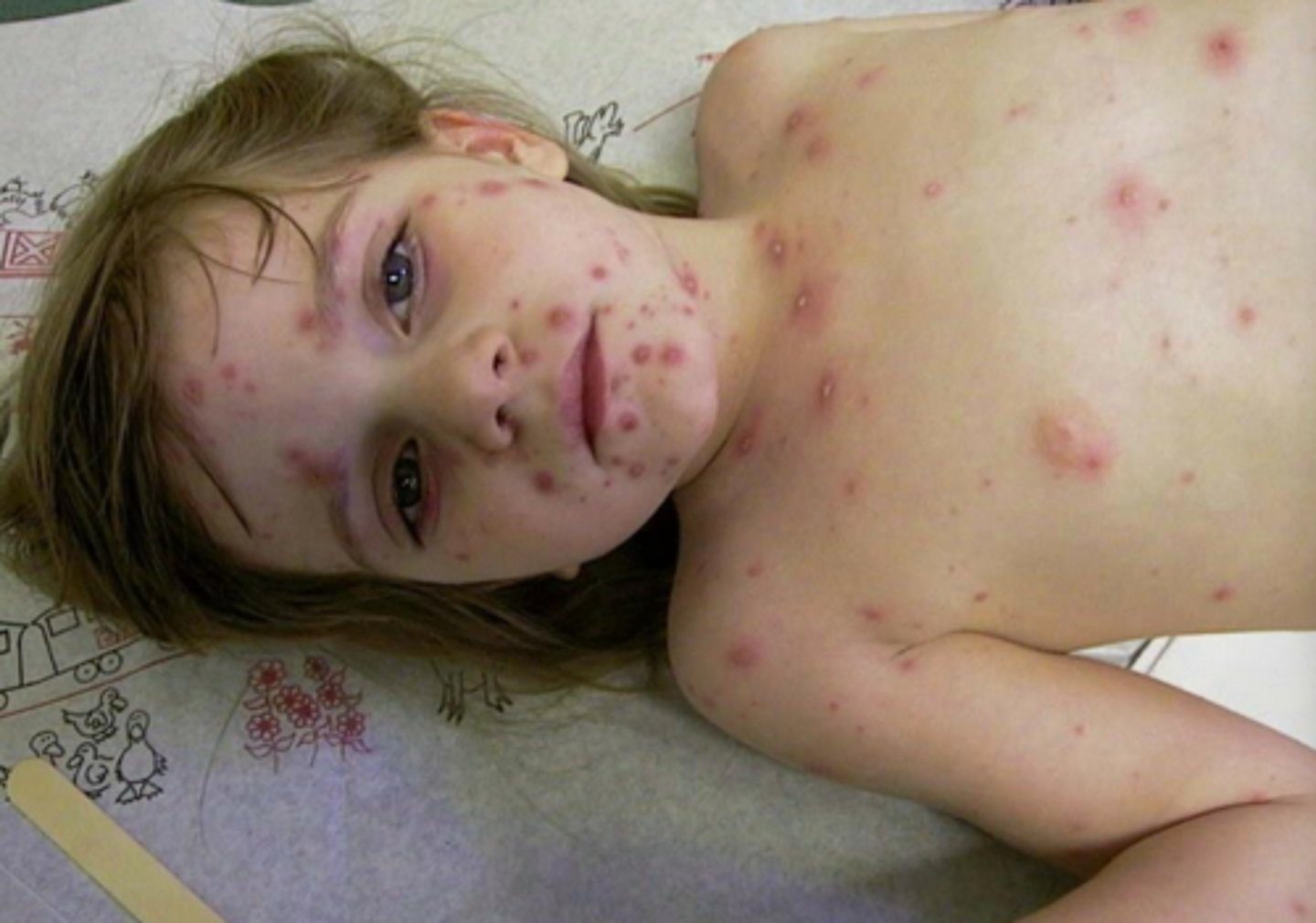
(t/f) symptomatic relief of varicella, a viral infection, is done by antivirals
false; symptomatic relief of varicella is done by antihistamines (topical lotion to relieve pruritis)
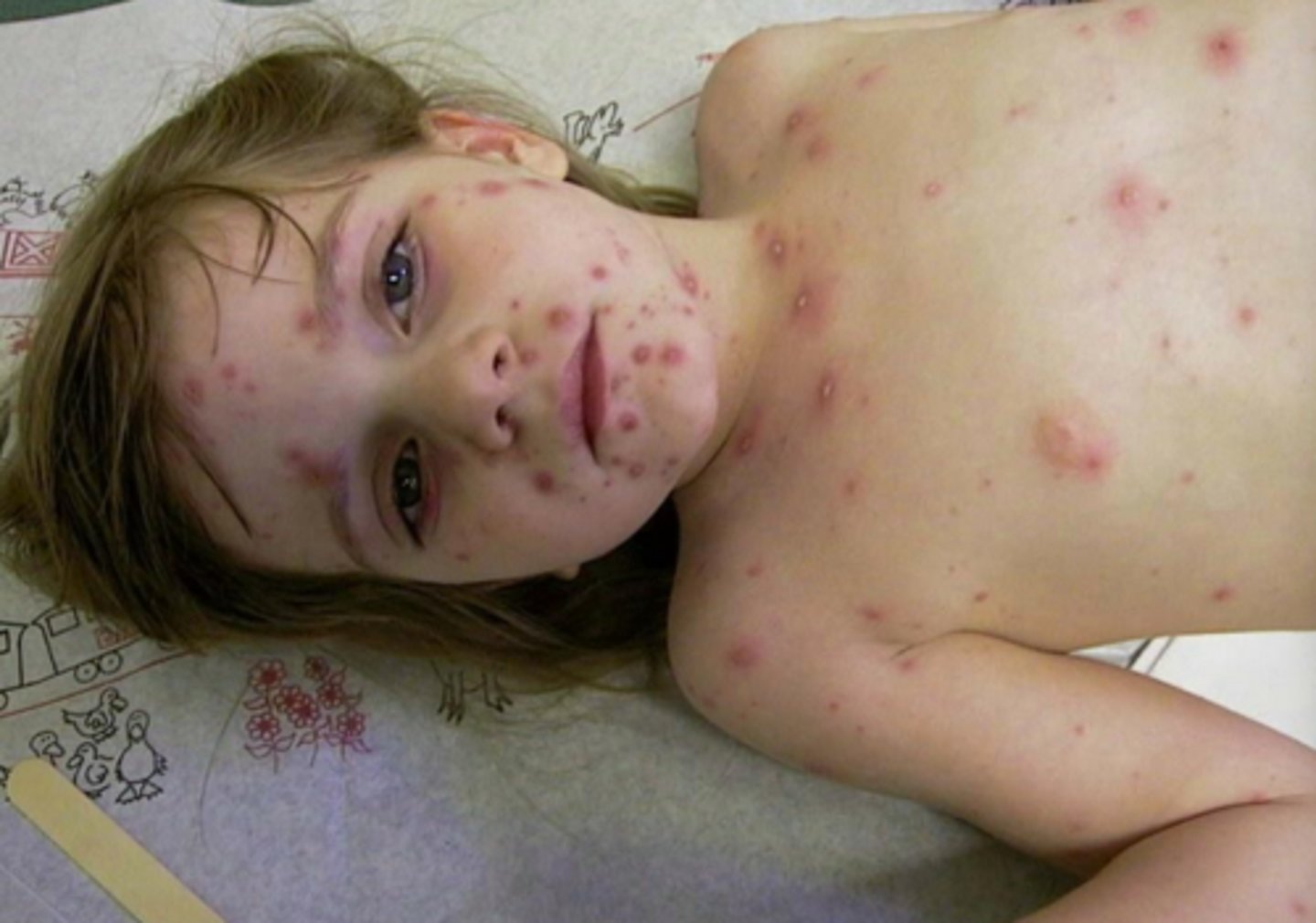
(t/f) varicella is more serious in children which is why vaccinating young is necessary
false; varicella is usually mild in children and more serious in adults
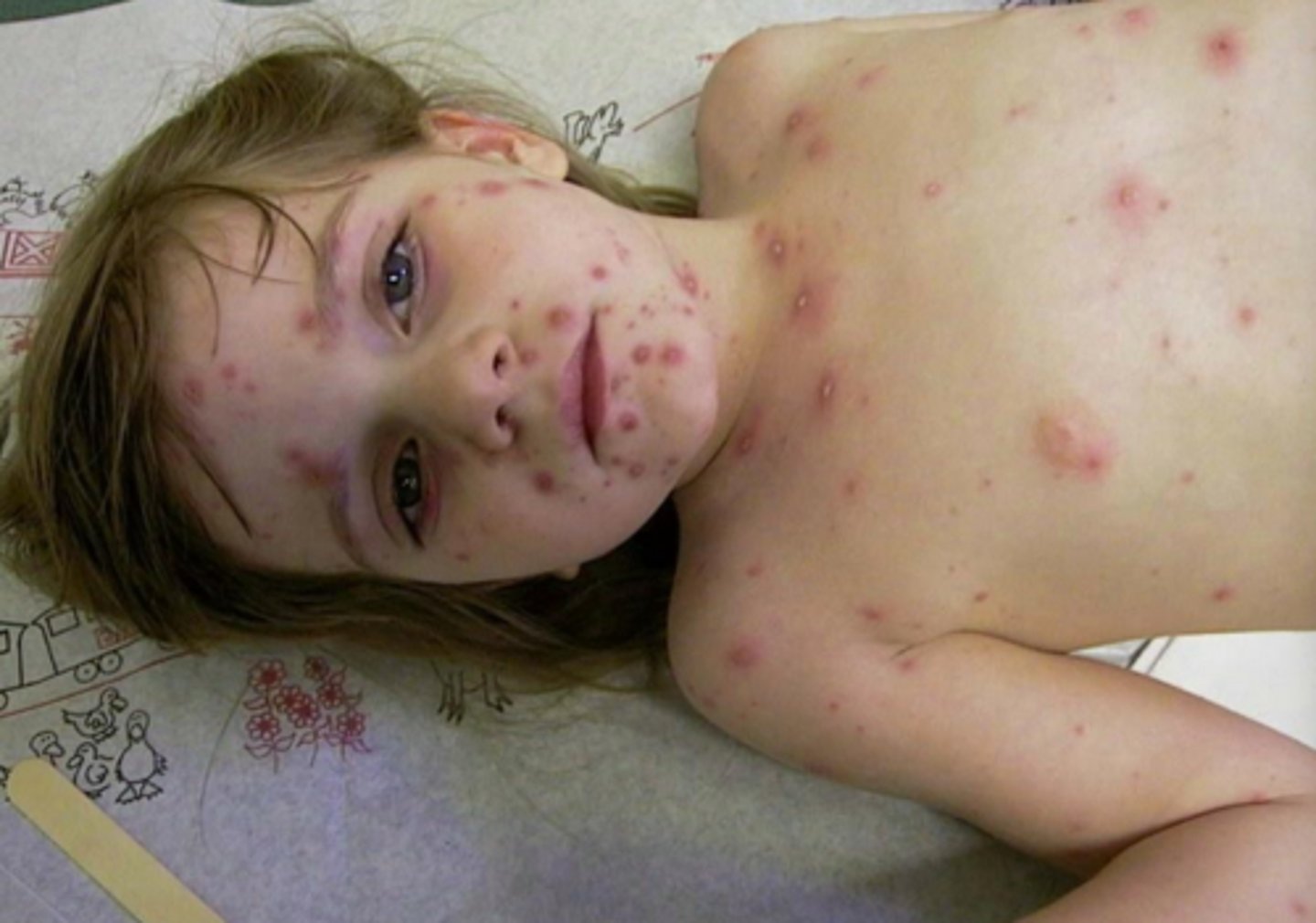
what viral vesicular-bullous lesion is a recurrence of the varicella-zoster virus after it enters its latent state?
herpes zoster
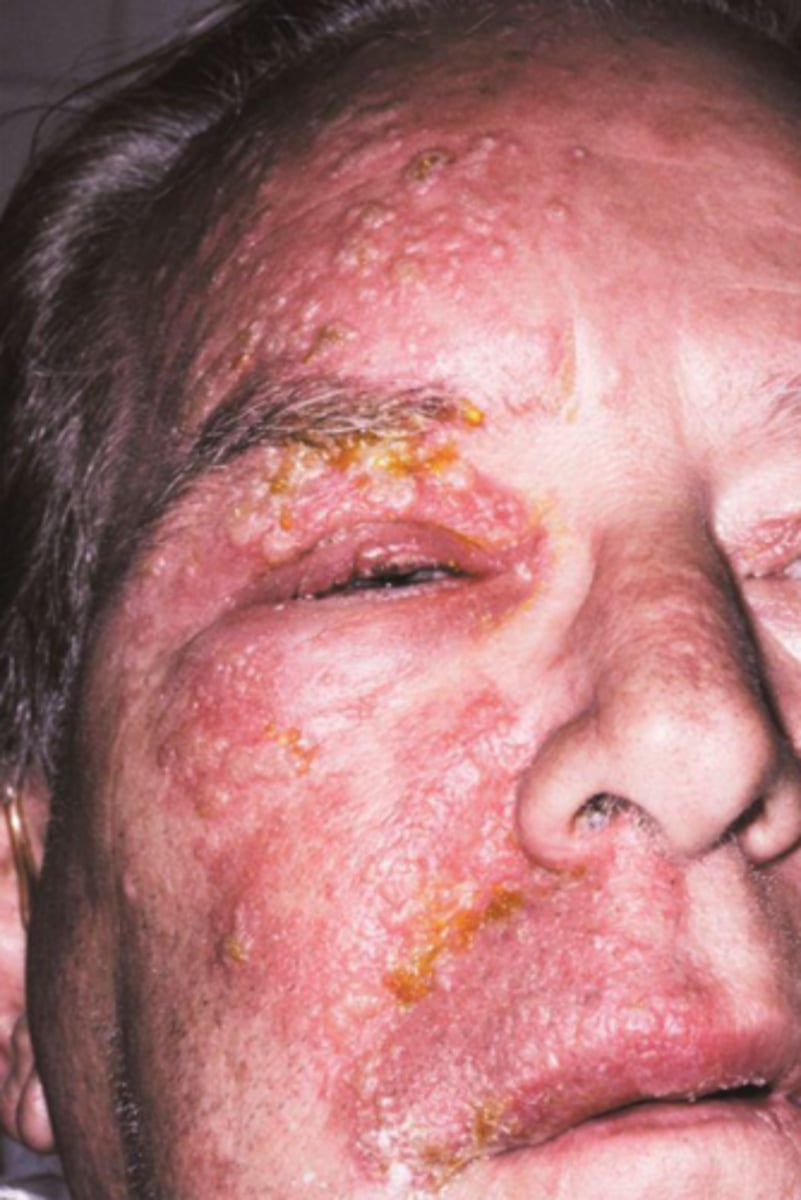
what viral vesicular-bullous lesion may recur from immunosuppression and in elderly patients and has a prodrome of pain, burning, and paresthesia (pain mimicking a toothache)?
herpes zoster
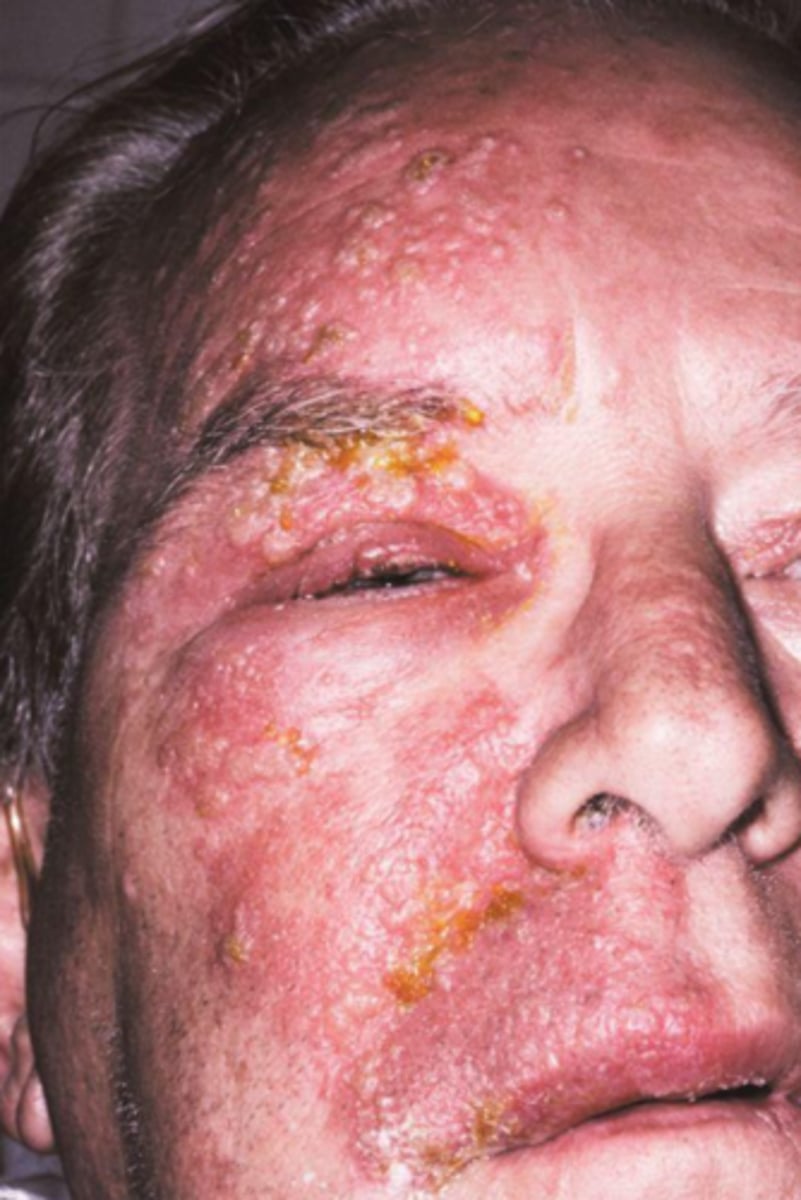
what viral vesicular-bullous lesion is also known as shingles?
herpes zoster
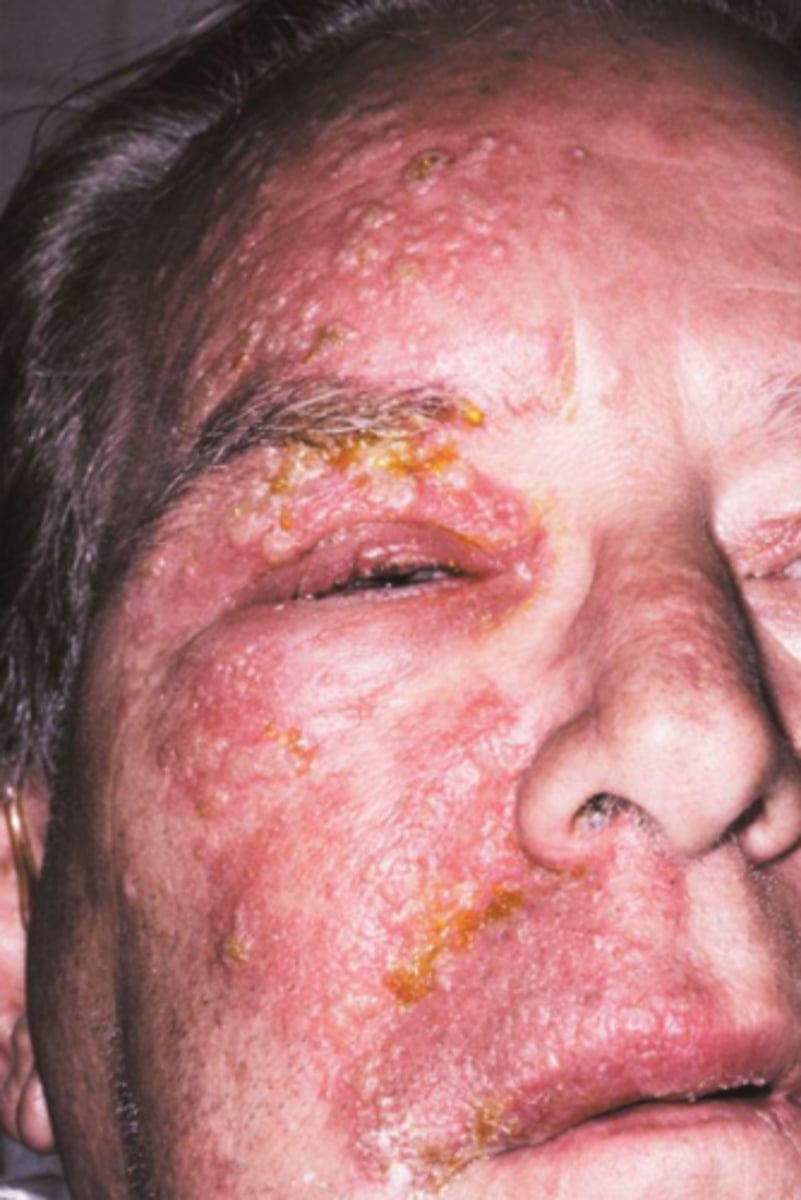
(t/f) shingles follows a bilateral distribution of the peripheral nerve that is infected, most commonly on the trunk and trigeminal area
false; shingles follows a unilateral distribution of the peripheral nerve that is infected, most commonly on the trunk and trigeminal area
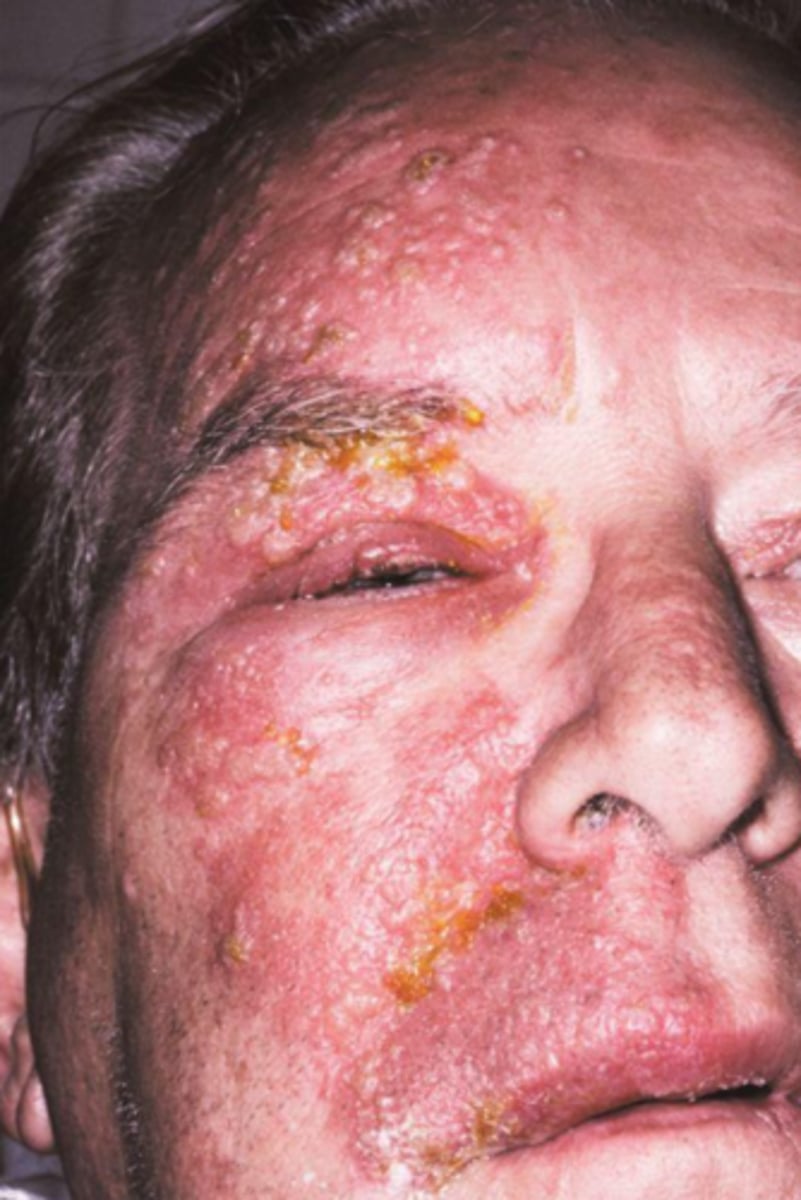
(t/f) shingles, a viral infection, is treated with antivirals
true
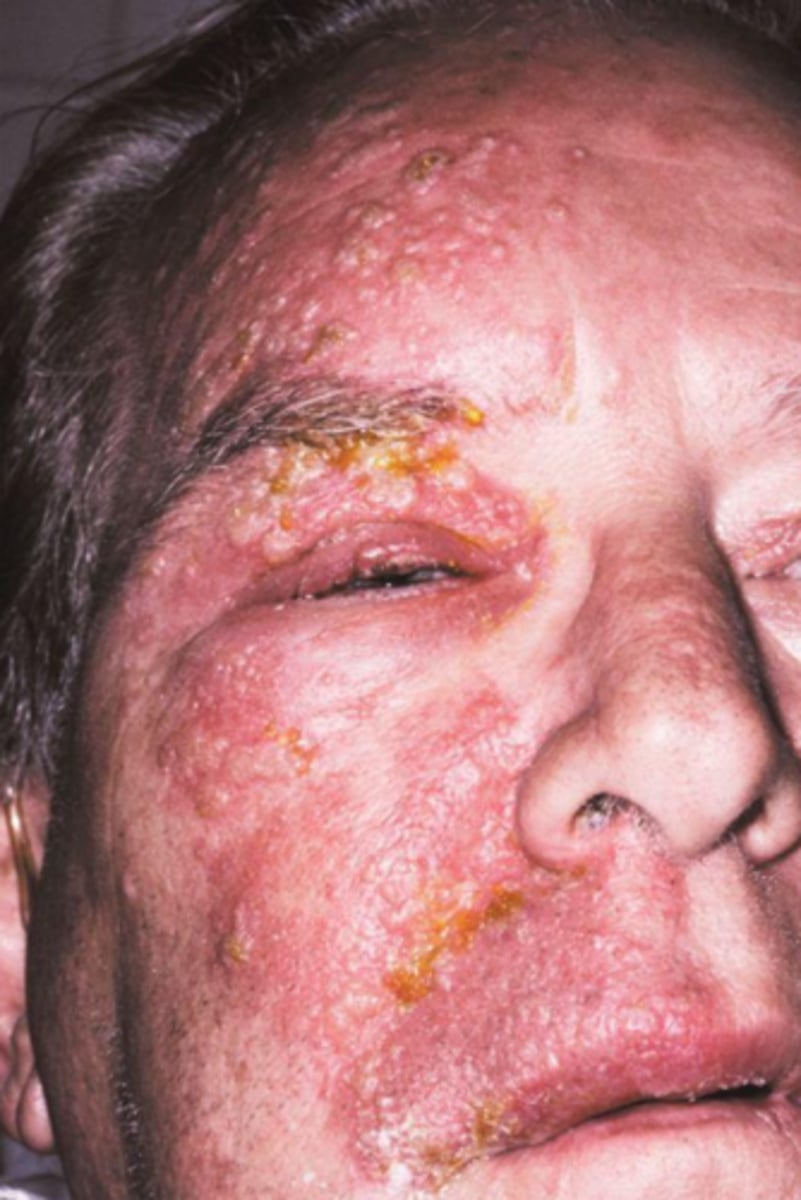
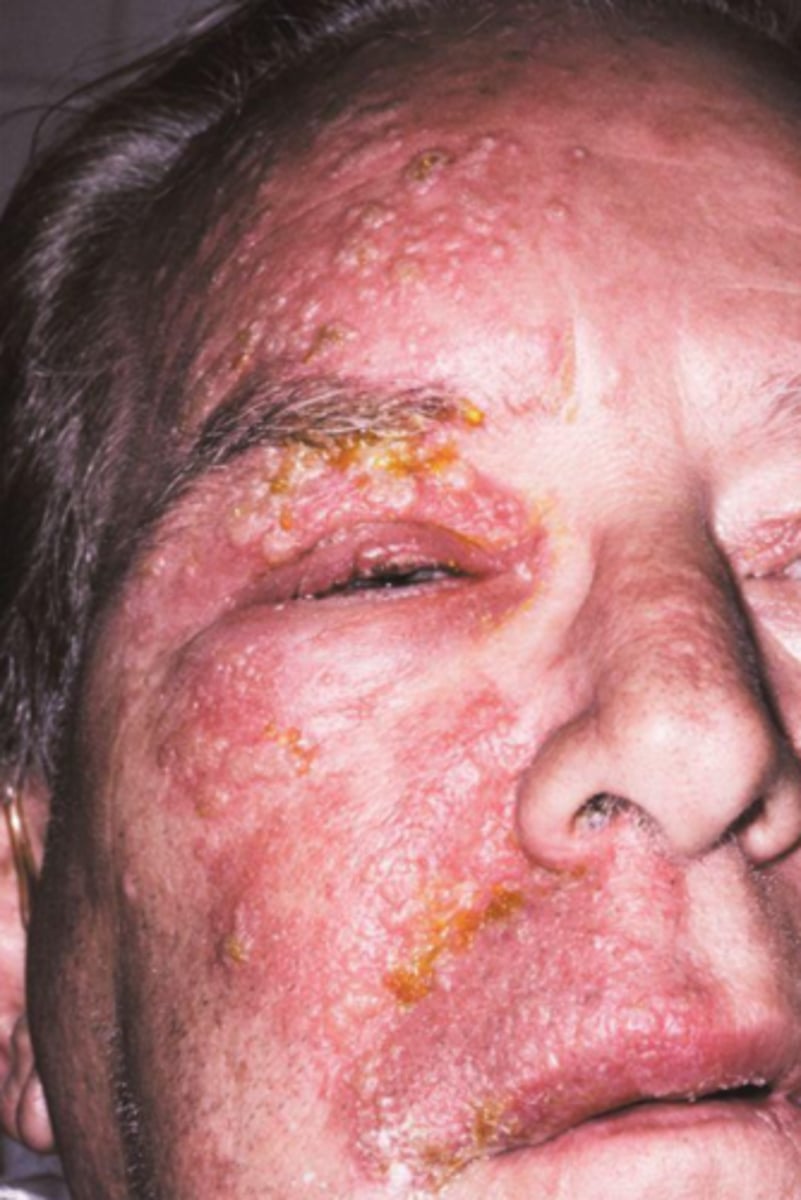
what viral vesicular-bullous lesion can cause post-herpetic neuralgia (chronic severe pain in nerve distribution after the lesion resolves) and Bell's palsy if the facial nerve is involved?
herpes zoster
what viral vesicular-bullous lesion is associated with Burkitt's lymphoma, nasopharyngeal carcinoma, and hairy leukoplakia?
infectious mononucleosis
what viral vesicular-bullous lesion is caused by the epstein-barr virus?
infectious mononucleosis
what viral vesicular-bullous lesion causes fever, malaise, pharyngitis, cervical lymphadenopathy, splenomegaly, hepatomegaly, and hepatitis?
infectious mononucleosis
what viral vesicular-bullous lesion is transmitted via saliva and establishes a lifelong latency (virus is controlled, but not eliminated) resulting a prolonged post-viral fatigue?
infectious mononucleosis; the virus stays latent in B cells and T cells response takes 6-12 months to downregulate
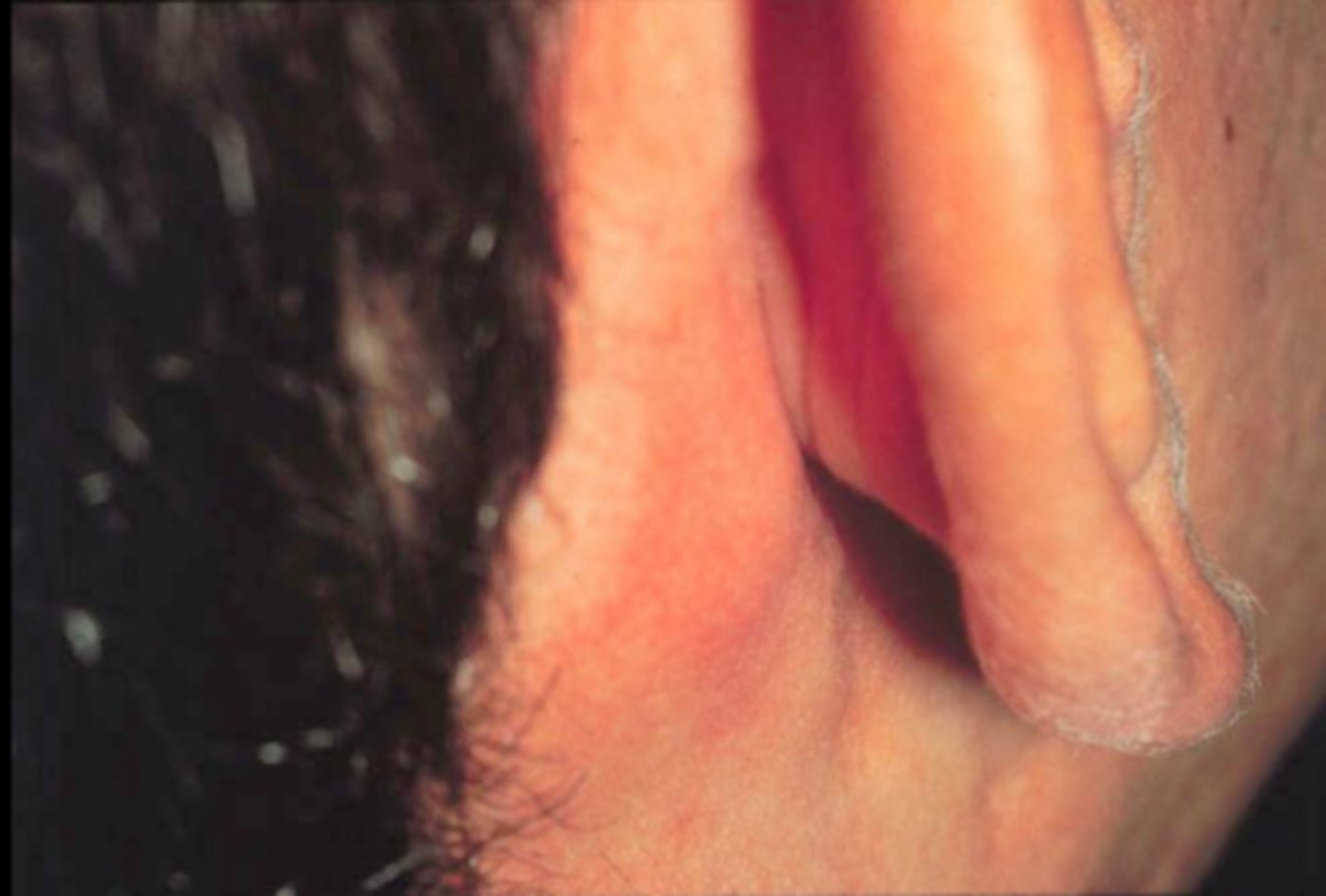
what viral vesicular-bullous lesion infects B lymphocytes that undergo polyclonal activation causing a robust T cell response?
infectious mononucleosis
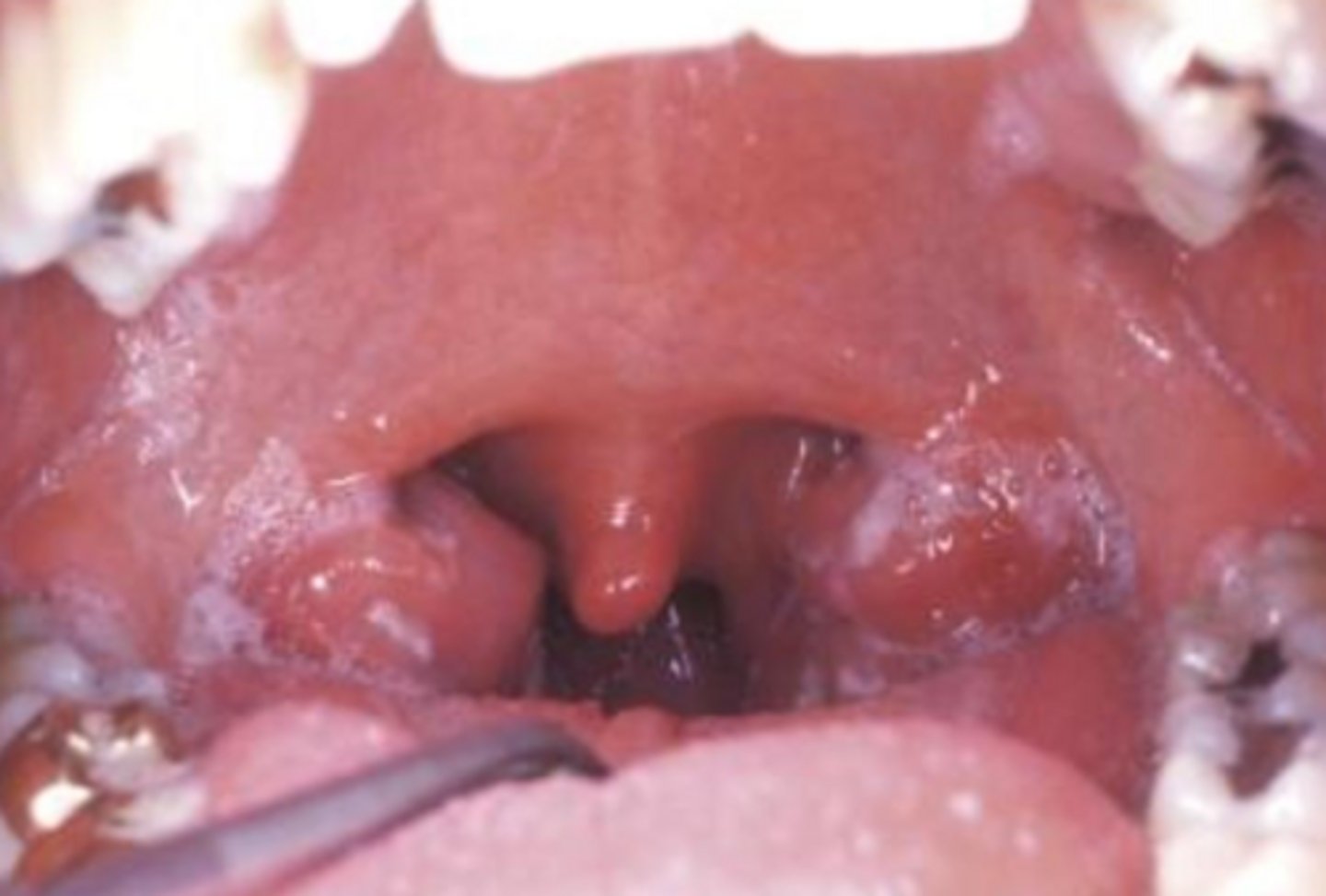
what viral vesicular-bullous lesion causes erythema, petechiae on the palate, and ulcerations WITHOUT vesicles?
infectious mononucleosis
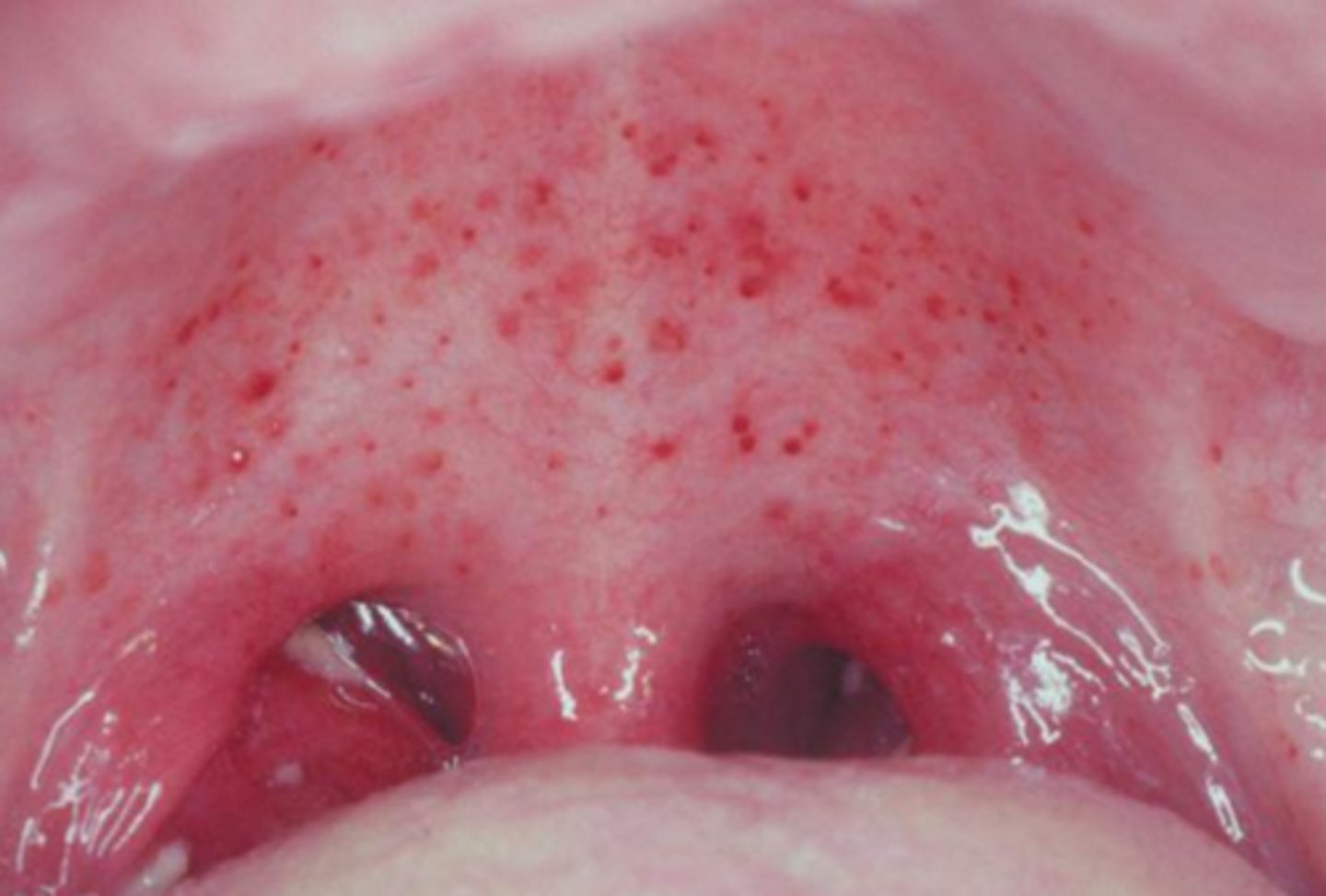
what viral vesicular-bullous lesion results in leukocytosis, lymphocytosis with atypical T lymphocytes, and positive serology?
infectious mononucleosis
(t/f) infectious mononucleosis is treated with antivirals to relieve symptoms
false; infectious mononucleosis is treated with acetaminophen and NSAIDs to relieve symptoms. avoid contact with others as this is highly contagious.
what condition occurs in immunocompromised EBV-infected patients (HIV, transplant, chemotherapy, steroids) who have weakened T cell control and causes hyperkeratosis from viral replication altering keratinocyte differentiation?
hairy leukoplakia
what 2 conditions occur in EBV-infected patients from the latent virus proteins altering cell growth, apoptosis, and immune recognition which increases the risk of malignant transformation?
1. burkitt lymphoma
2. nasopharyngeal carcinoma
what are 2 vesicular-bullous lesions caused by coxsackievirus (group A)?
1. hand, foot, and mouth disease (HFM)
2. herpangina
what viral vesicular-bullous lesion is caused by paramyxovirus?
measles
what viral vesicular-bullous lesion causes mild fever, malaise, diarrhea, and vesicles and ulcers throughout the cavity as well as macules and vesicles on the hands and feet?
hand, foot, and mouth disease (HFM); macules and vesicles on the hands and feet is what helps differentiate it from primary herpes
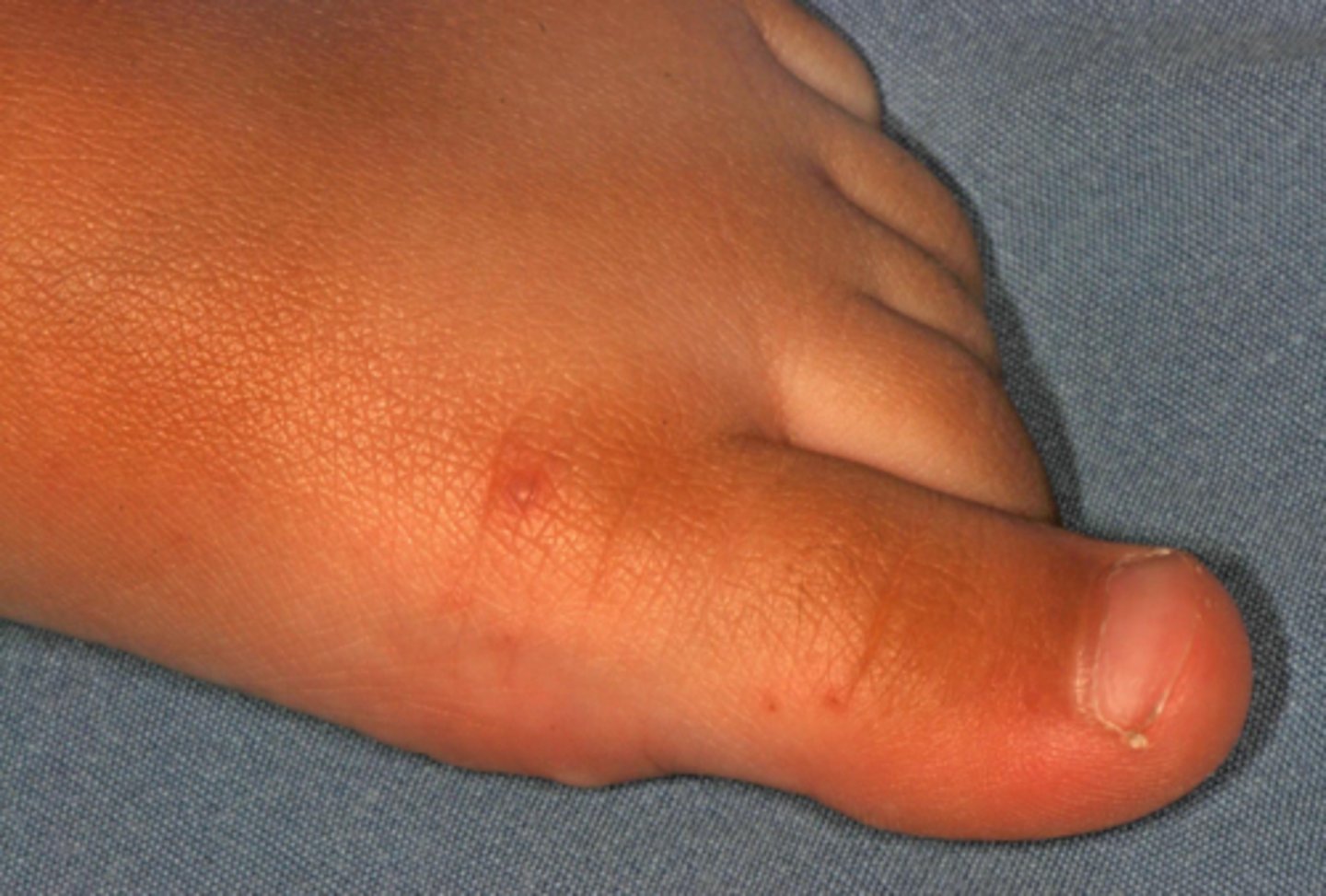
what viral vesicular-bullous lesion is similar to HFM disease (mild fever, malaise, diarrhea, and vesicles and ulcers), but confined to the posterior oral cavity (soft palate, uvula, and tonsillar pillar)?
herpangina; non-keratinized tissue only
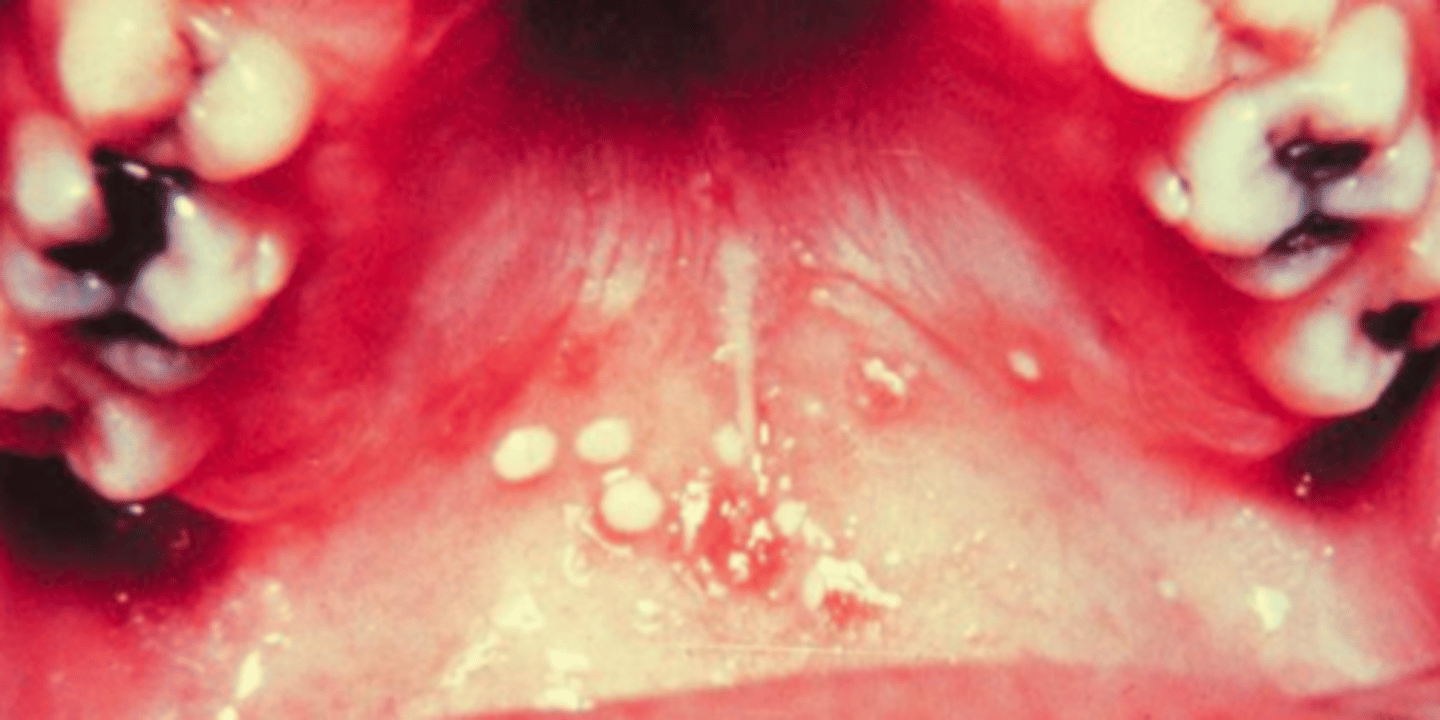
(t/f) herpangina only causes lesions in non-keratinized tissue
true
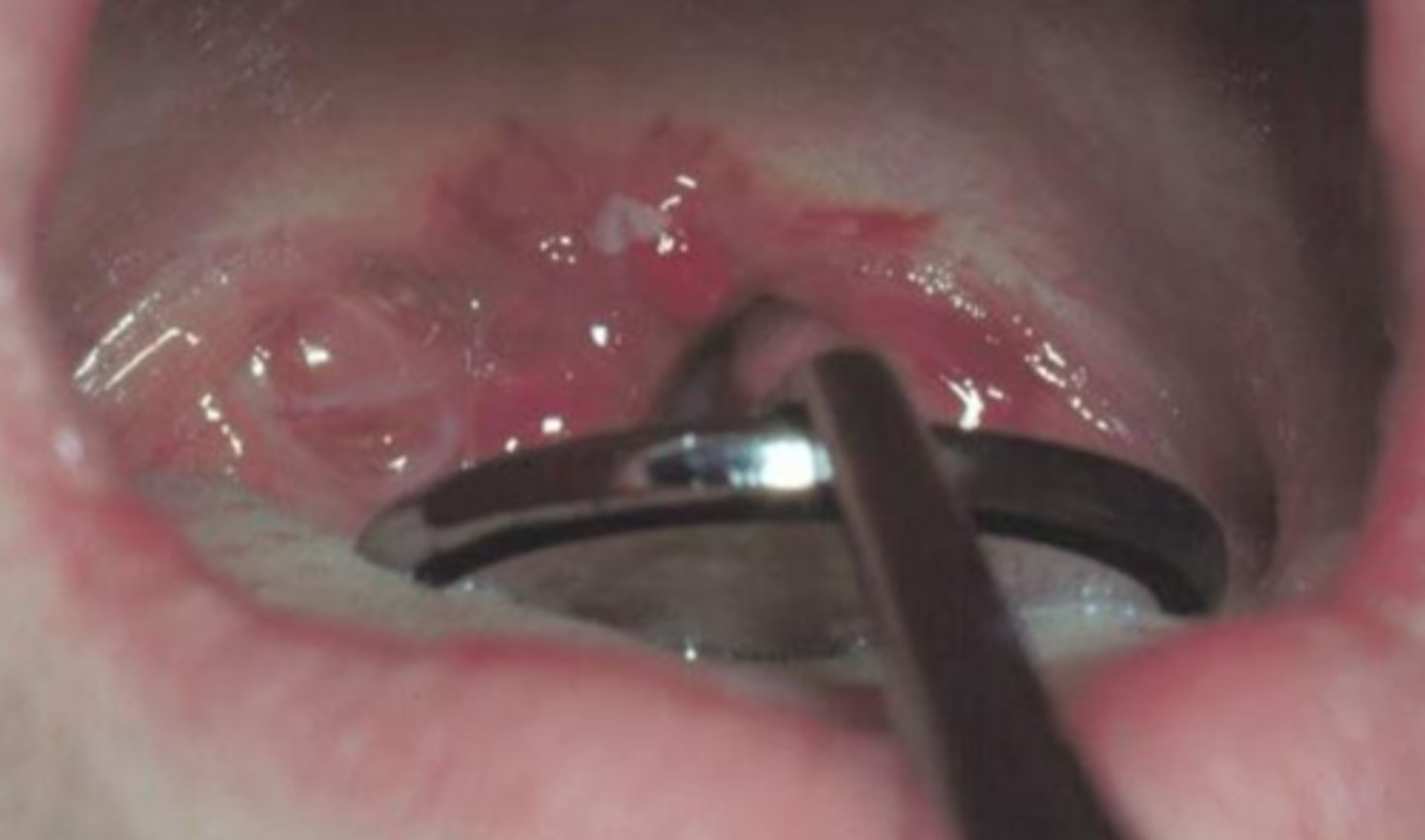
what viral vesicular-bullous lesion is caused by an RNA virus that spreads through respiratory droplets and is uncommon in well-vaccinated populations?
measles
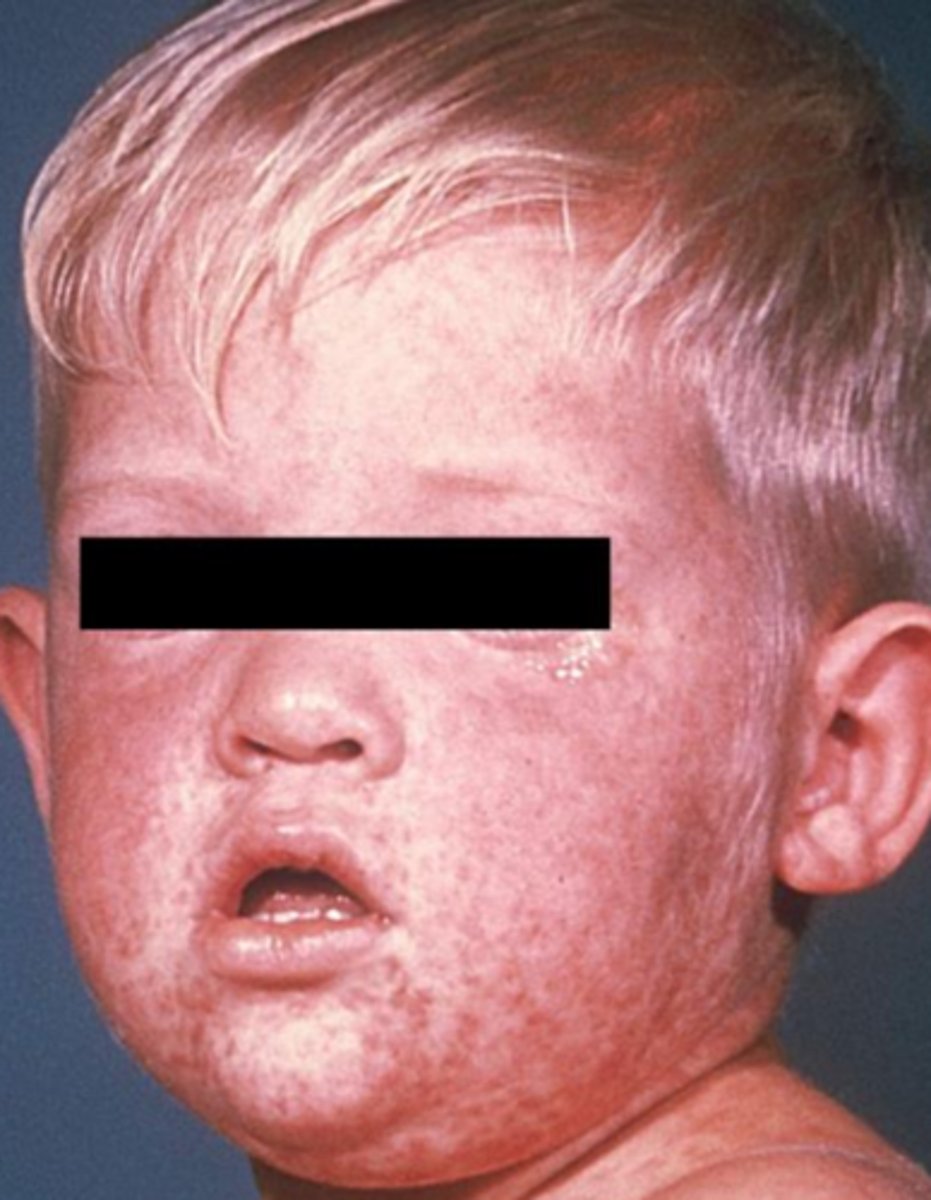
what viral vesicular-bullous lesion is also known as rubeola?
measles
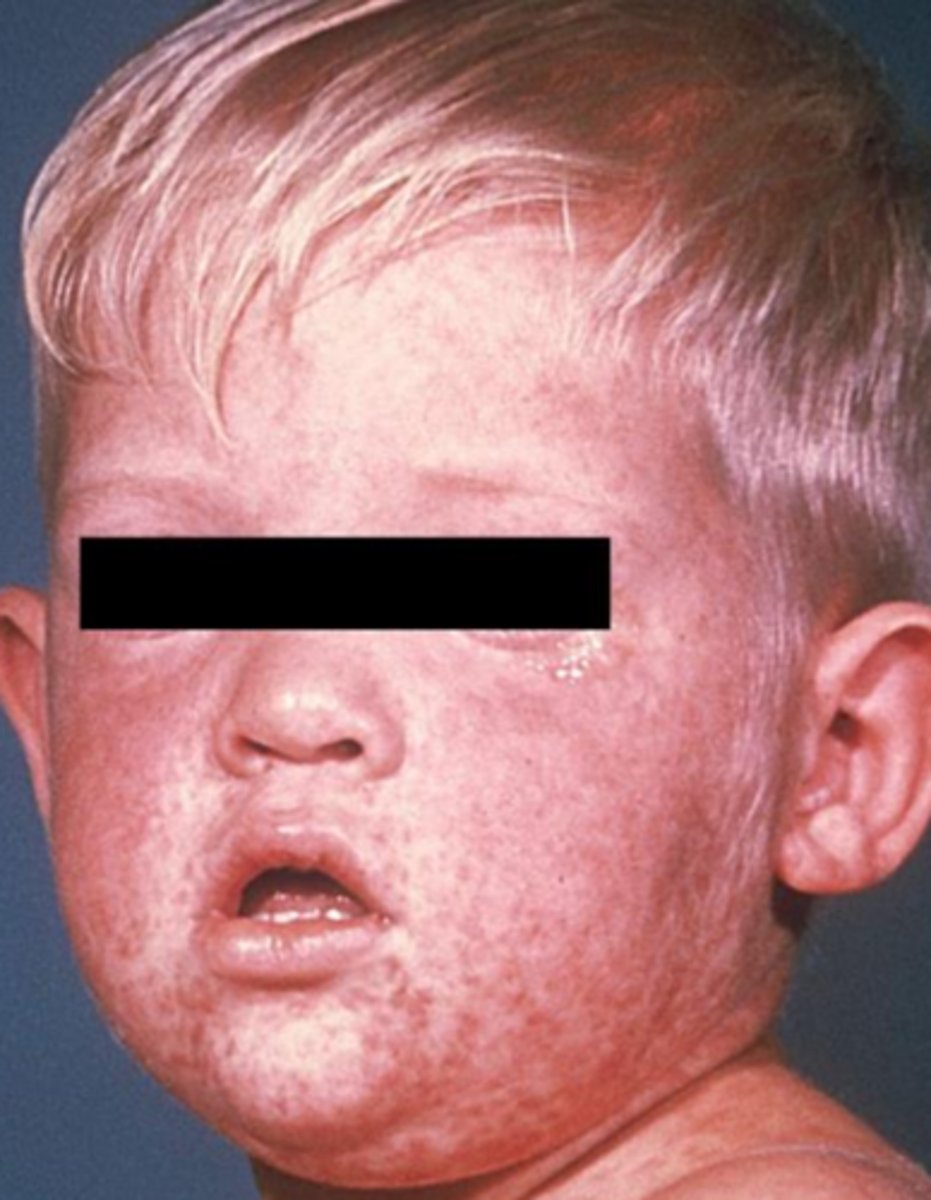
what viral vesicular-bullous lesion infects the respiratory epithelium, causes viremia with immune-mediate tissue injury, and transient immunosuppression (leading to bacterial pneumonia)?
measles
what viral vesicular-bullous lesion causes Koplik spots on the buccal mucosa and small blue-white macules on the erythematous base?
measles
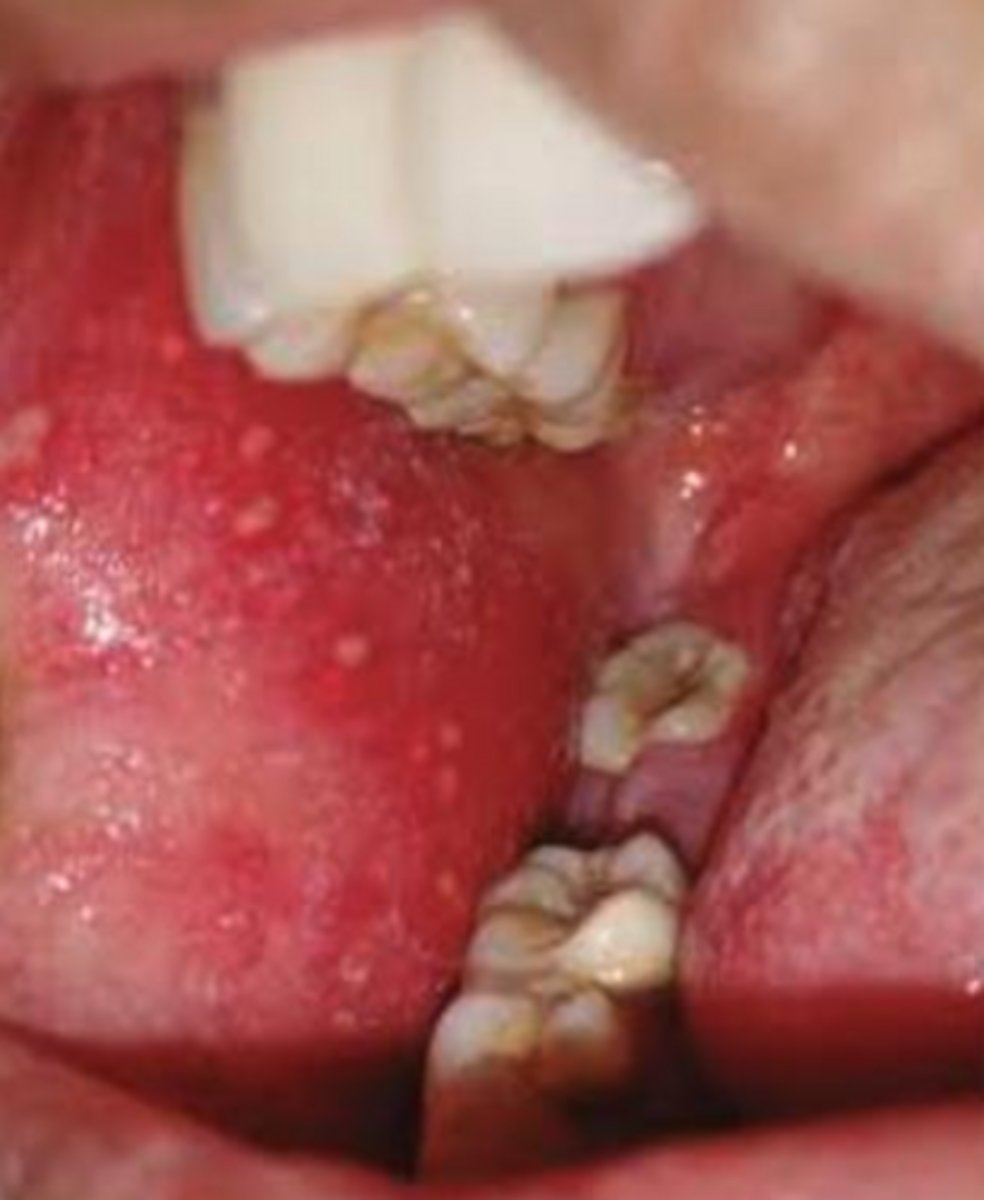
what is the name of the enanthem lesions caused by measles (focal necrosis with inflammatory exudate that look like grains of salt) that fade before a skin rash appears (exanthem)?
Koplik spots; these CANNOT be rubbed off
what viral vesicular-bullous lesion has a complication rate of 21%, has no cure (supportive care only), but is highly prevented with the MMR vaccine?
measles
(t/f) autoimmune diseases have a gradual onset (weeks to months), are progressive, chronic, associated with lymphadenopathy, and cured with corticosteroids
false; autoimmune diseases have a gradual onset (weeks to months), are progressive, chronic, not associated with lymphadenopathy, and controlled (not cured) with corticosteroids
what vesicular-bullous autoimmune disease is caused by an immune abnormality involving T-lymphocytes?
erosive lichen planus
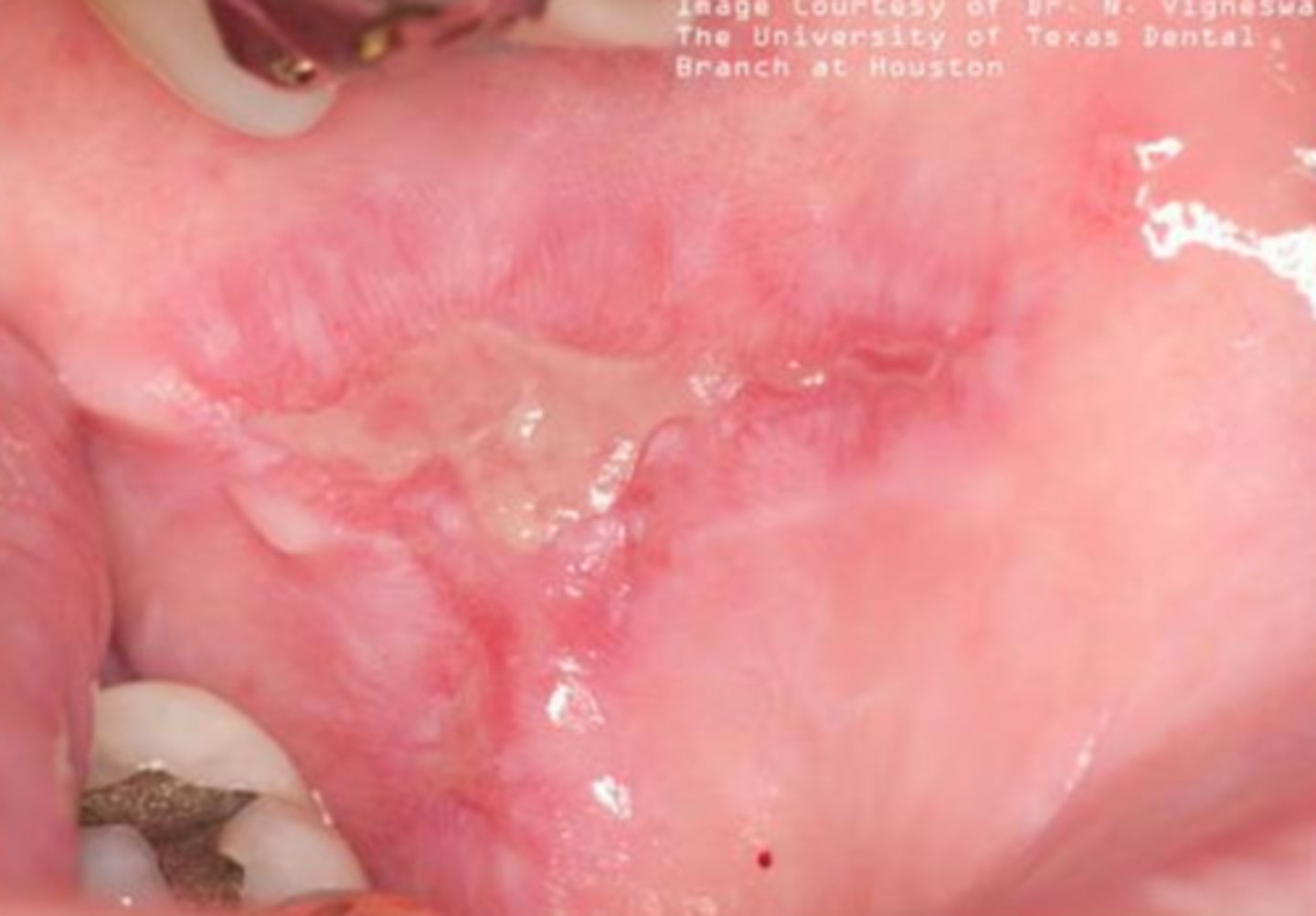
(t/f) lichenoid mucositis can mimic erosive lichen planus
true
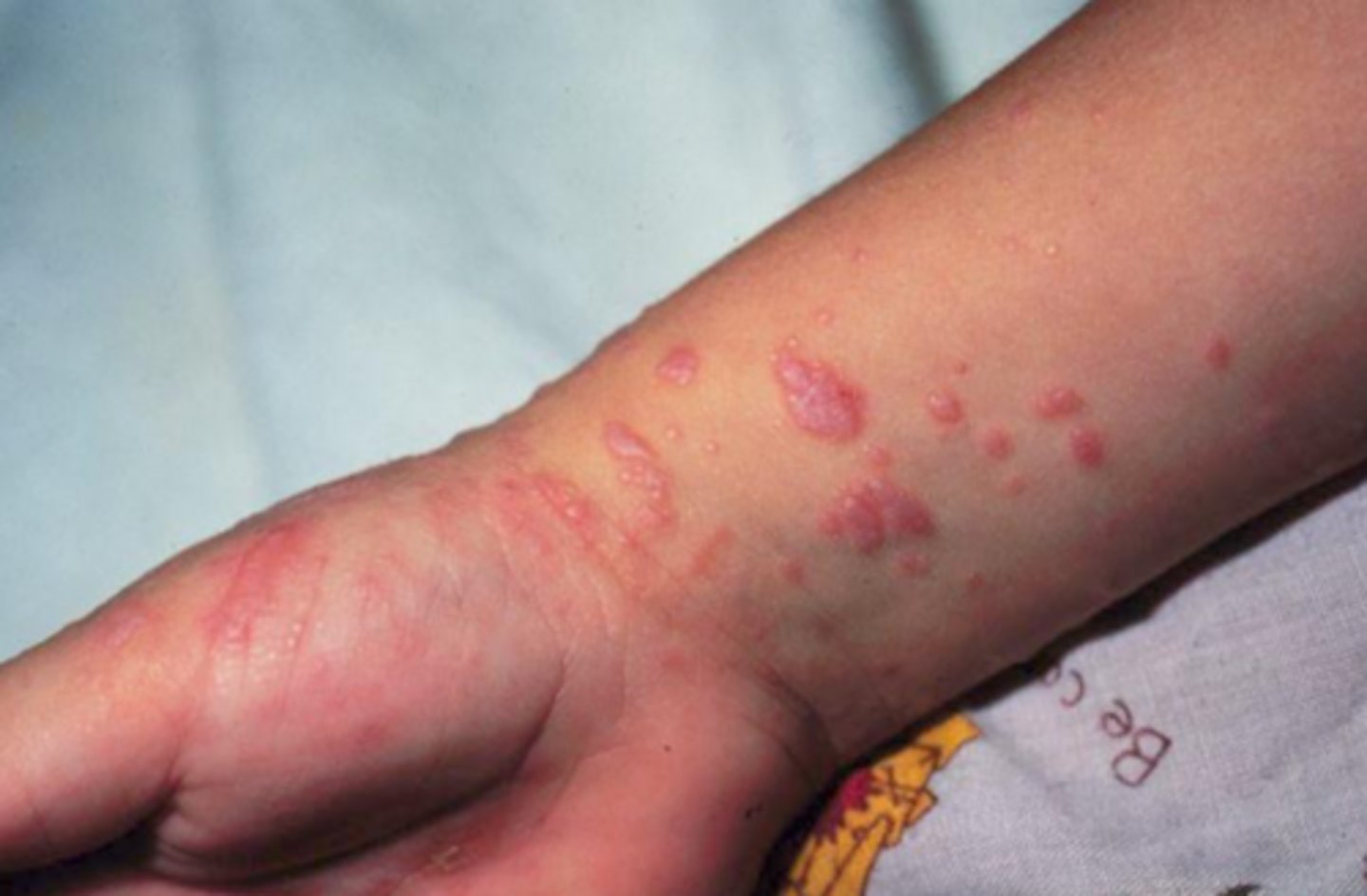
what vesicular-bullous autoimmune disease may occur independent of oral lesions and are pruritic, violet colored plaques with striations?
erosive lichen planus
what vesicular-bullous autoimmune disease causes white striae along the periphery of the oral cavity that are (unilateral/bilateral) and can be focal or generalized?
bilateral; erosive lichen planus
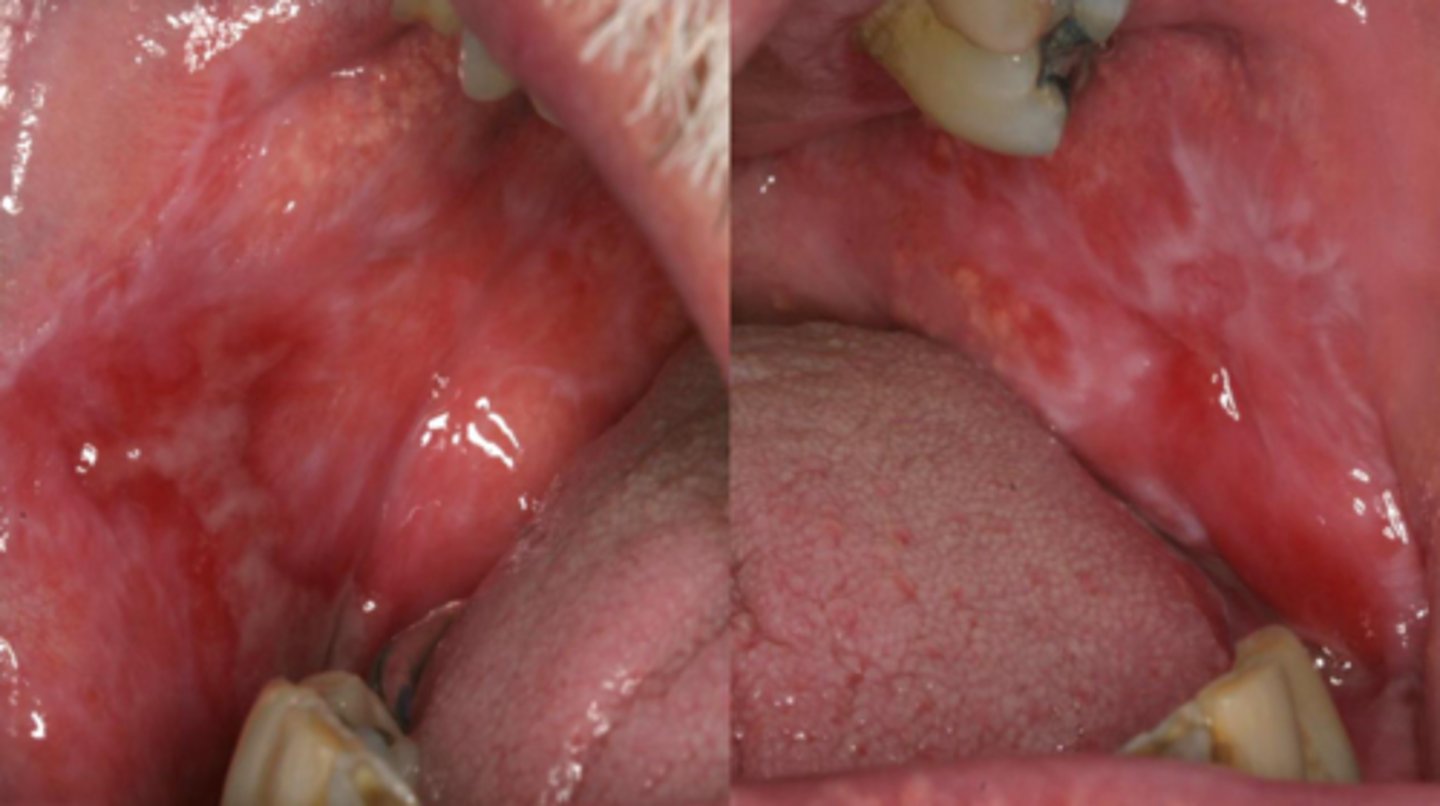
(t/f) vesicle formations before the erosion in erosive lichen planus is very common
false; vesicles in erosive lichen planus are rare
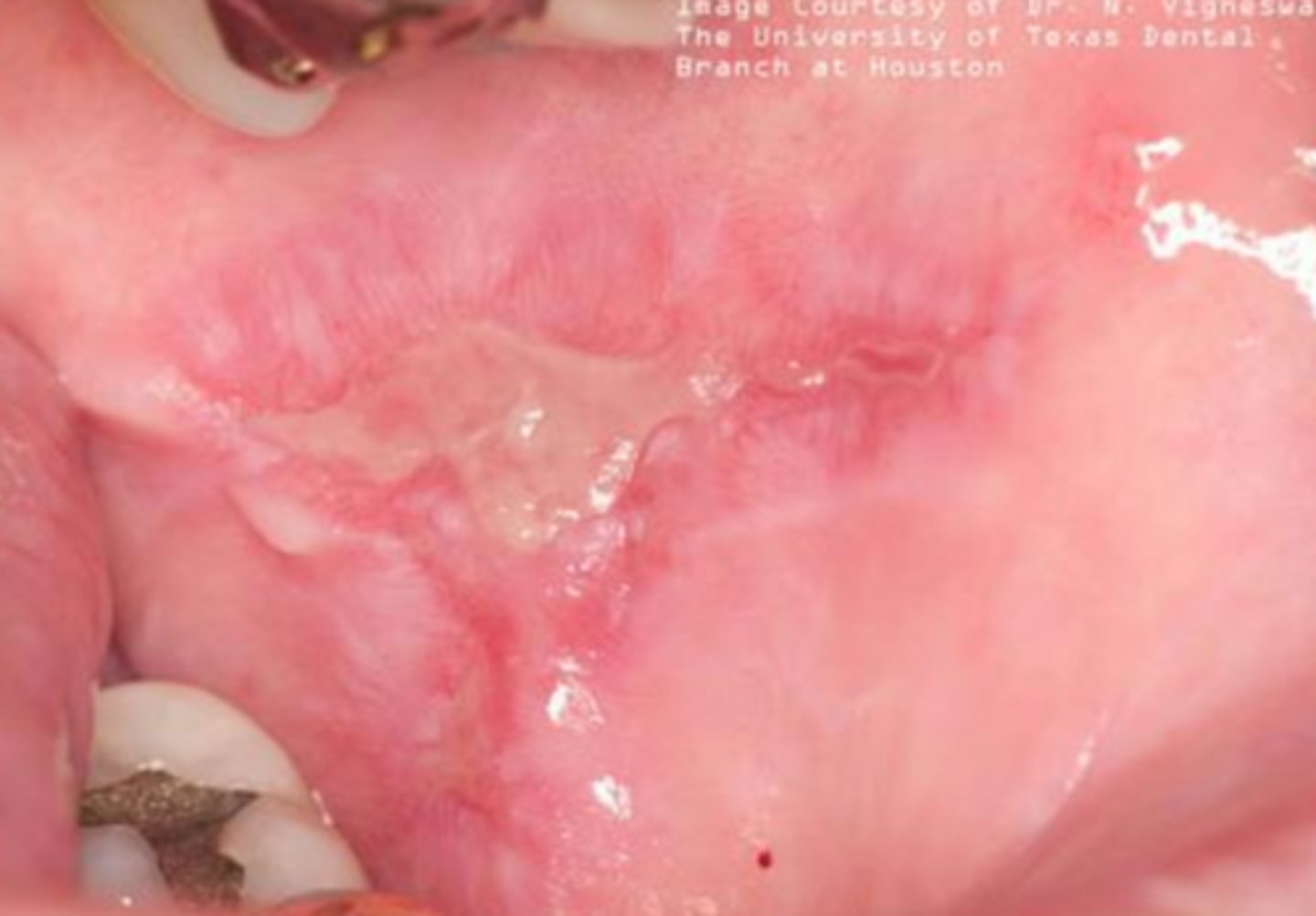
what vesicular-bullous autoimmune disease is caused by autoantibodies to intercellular proteins in desmosome resulting fragile blisters that rupture easily forming painful ulcers?
pemphigus vulgaris
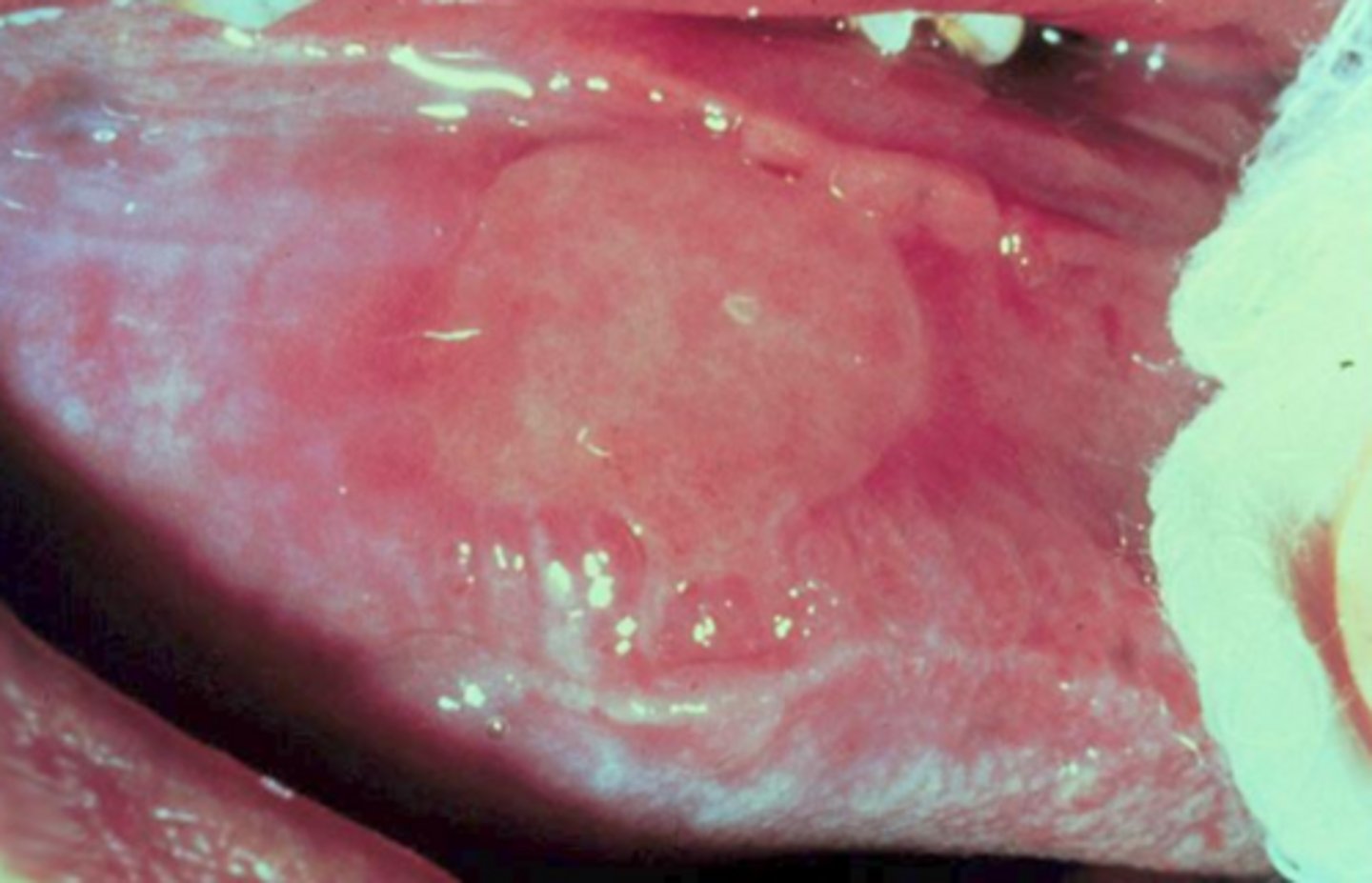
pemphigus vulgaris forms blisters in areas of the skin or mucosa which are usually (multifocal/unifocal)
multifocal; pemphigoid is also multifocal
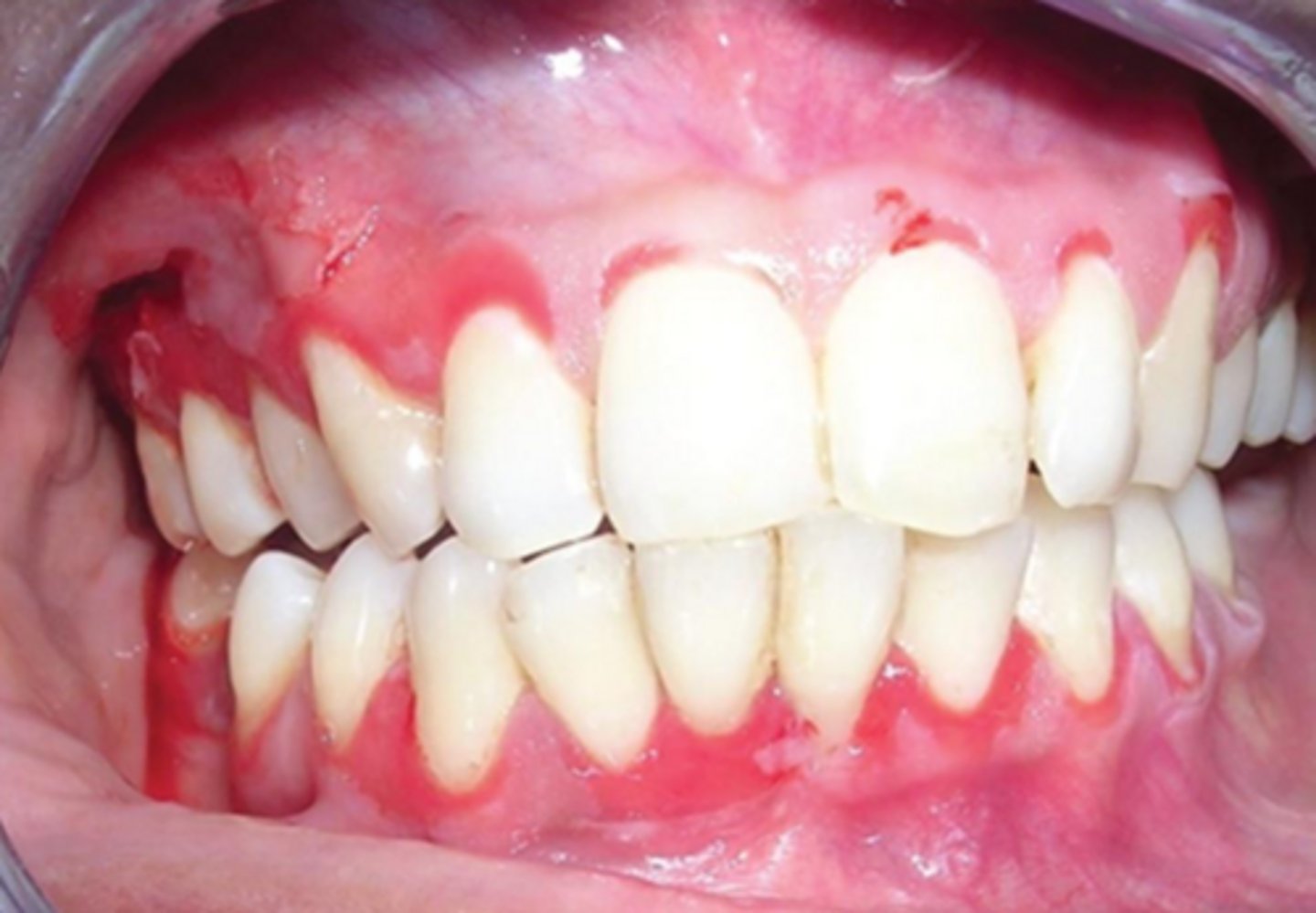
what is the diagnostic skin finding that is sometimes present in pemphigus vulgaris and induced by lateral pressure or application of air?
nikolsky sign
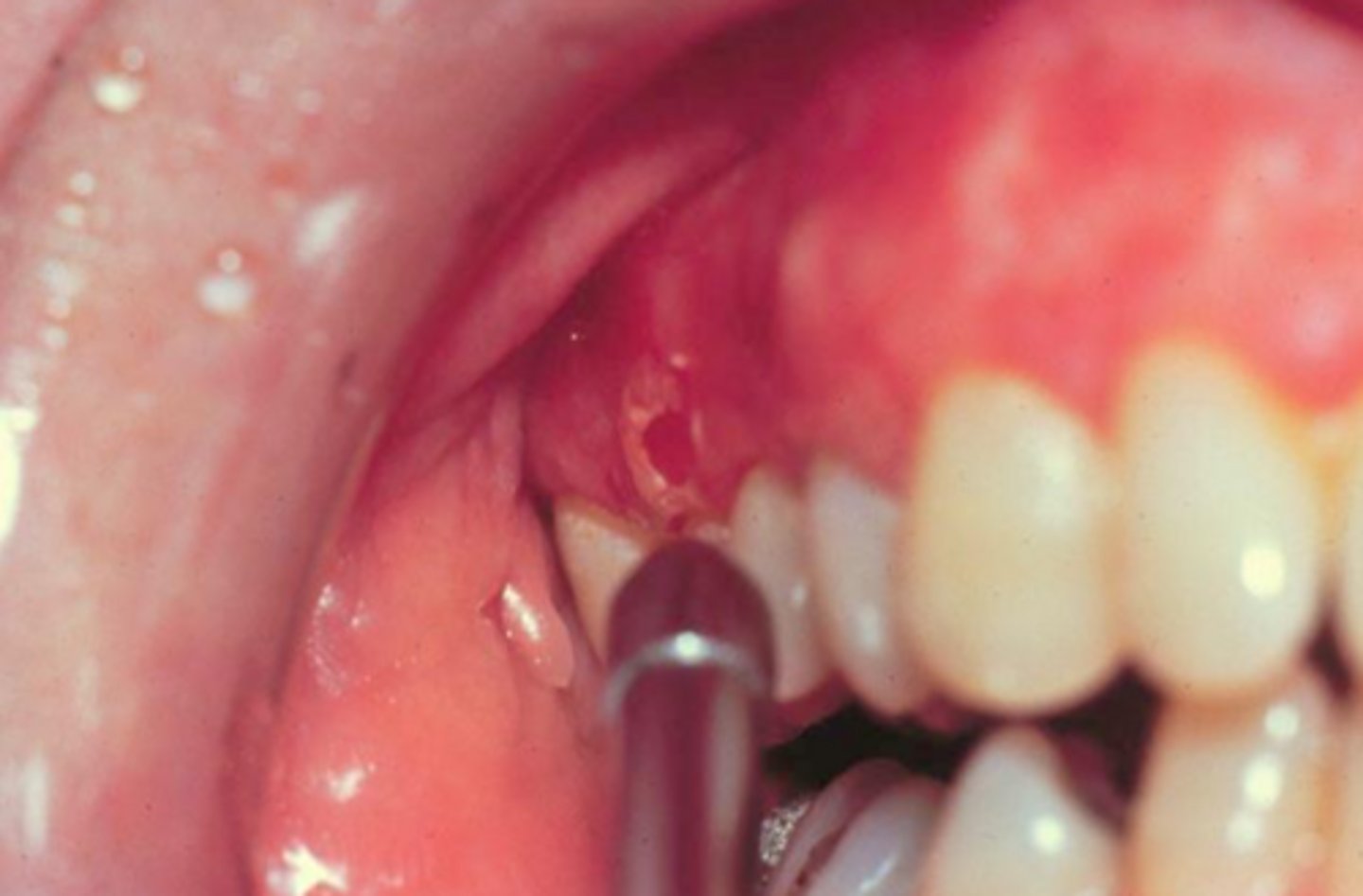
what vesicular-bullous autoimmune disease is associated with Tzanck cells, diagnosed microscopically with direct immunofluorescence on biopsy, and requires 2 specimens (in formalin and Michels solution)?
pemphigus vulgaris
how are oral symptoms of pemphigus vulgaris and mucous membrane (cicatricial) pemphigoid treated?
topical corticosteroids
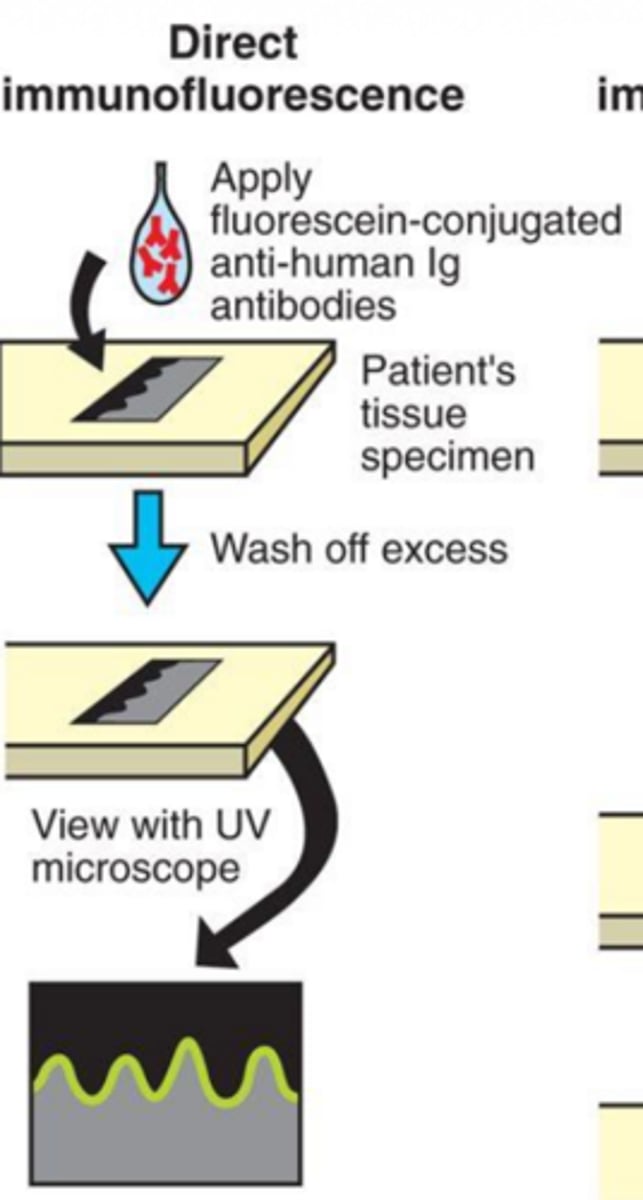
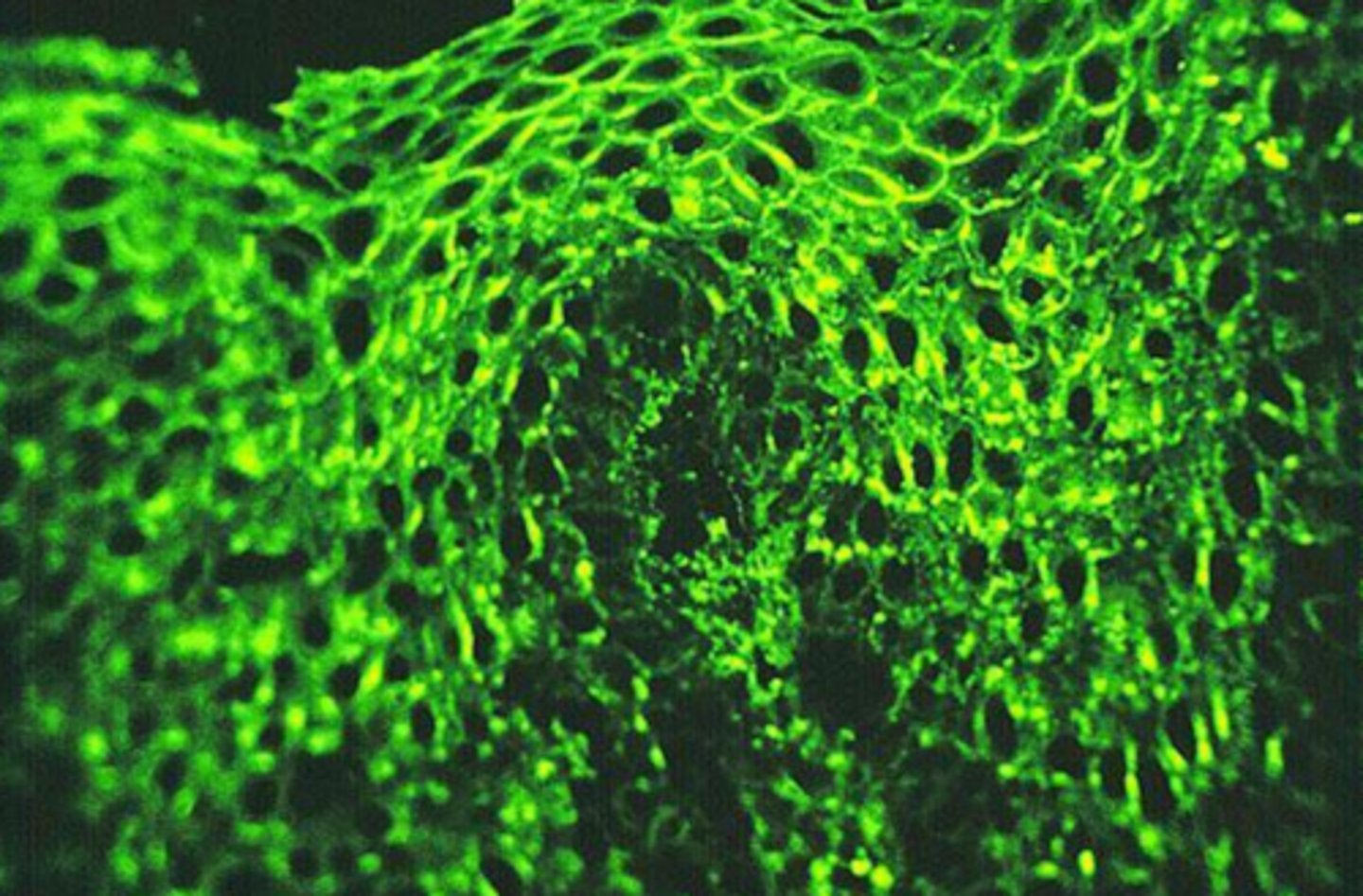
how can immunofluorescence be used to confirm that human auto-antibodies are attacking desmosomes and hemidesmosomes?
using goat antibodies;
1. insert human antibodies into a goat
2. allow goat immune system to form antibodies against the human antibodies
3. remove goat antibodies from the goat and tag with a fluorescent dye
4. apply goat antibodies to a biopsied specimen and view under UV light