Pediatric Dentistry Final Review (ksolman x ryanef123 collab🤩)
1/379
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
380 Terms
0
which Brodsky grade:
Surgically removed tonsils

1
which Brodsky grade:
Tonsils hidden within tonsil pillars
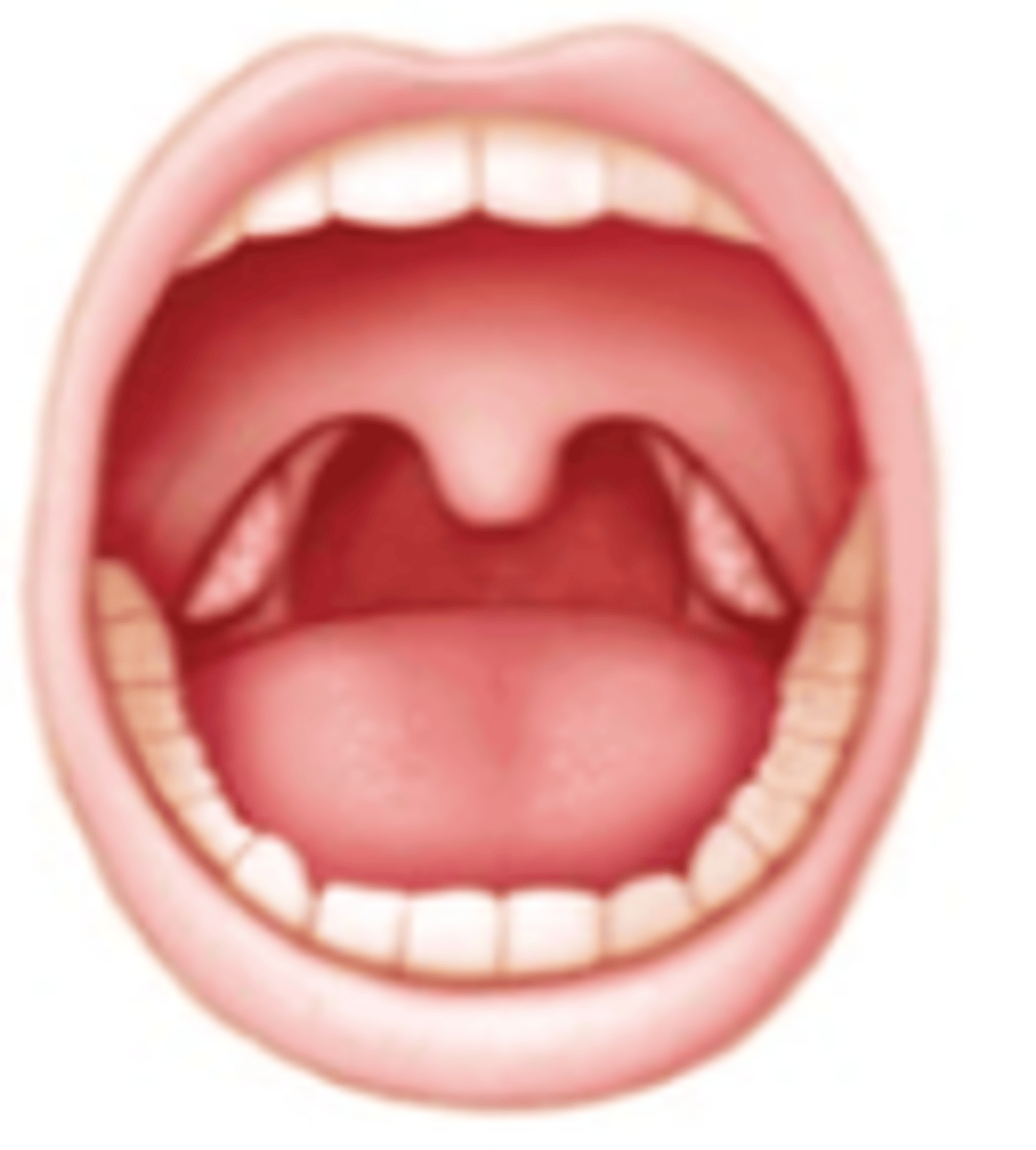
2
which Brodsky grade:
Tonsils extending to the pillars
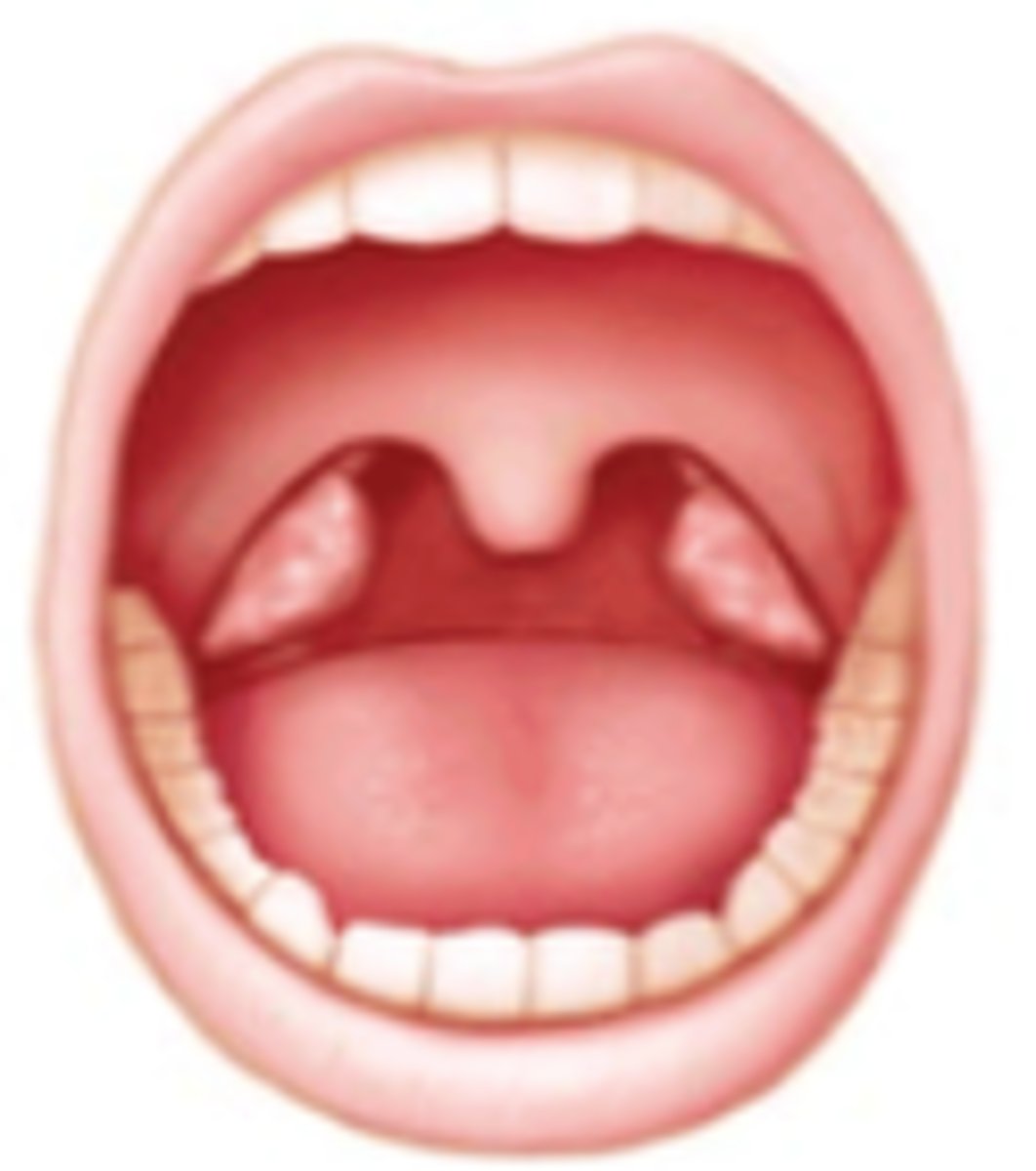
3
which Brodsky grade:
Tonsils beyond the pillars
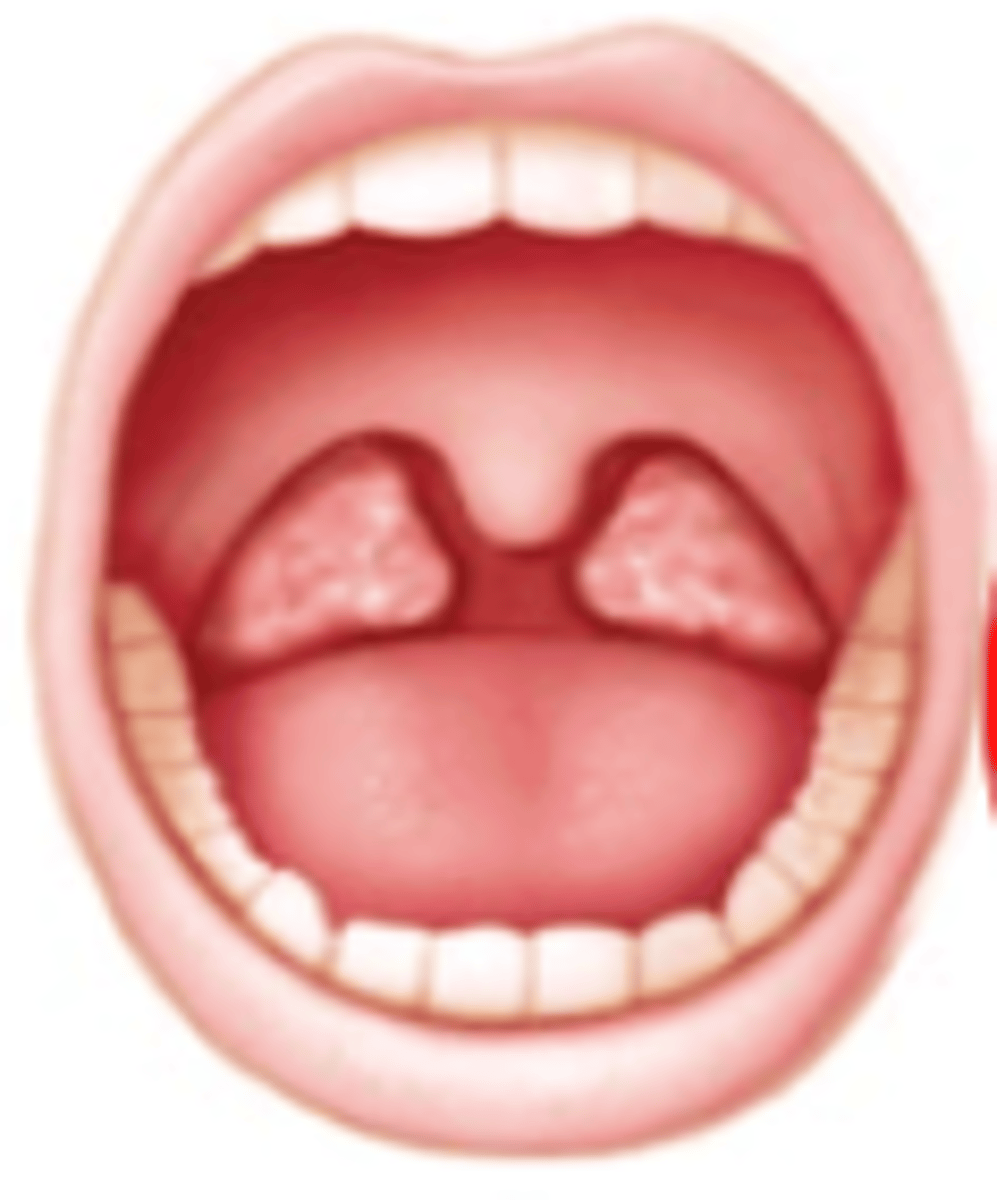
4
which Brodsky grade:
Tonsils extend to midline
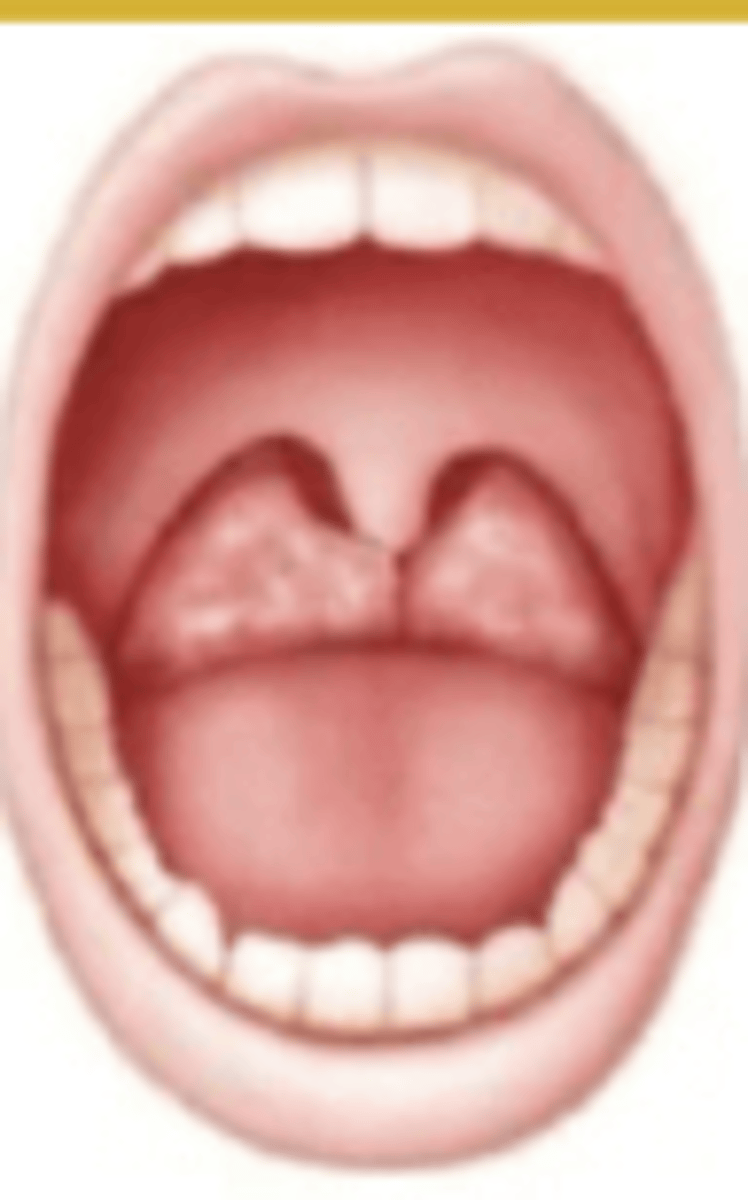
3, 4
Brodsky grades (_ and _) suggest a narrower airway, which increases the risk of airway obstruction during sedation.
minimal
moderate
deep
general anesthesia
4 levels of sedation
Minimal sedation
what type of sedation:
A drug-induced state where pts respond to verbal commands while maintaining stable breathing + heart function
Monitoring
In minimal sedation, children usually only need _________, but if they become moderately sedated, moderate sedation guidelines should be followed.
Moderate sedation
what type of sedation:
A drug-induced state where patients can respond to verbal commands or light tactile stimulation.
cardiovascular
in moderate sedation:
Patients maintain their own airway, and ____ function is typically preserved.
Consciousness
in moderate sedation:
_____ is usually preserved, but precautions are necessary to prevent deeper sedation.
Deep sedation
what type of sedation:
A drug-induced depression of consciousness where patients are difficult to arouse but respond purposefully after repeated verbal or painful stimulation.
ventilatory
in deep sedation:
Patients may have impaired ability to maintain ______ function and might need help with airway maintenance, and spontaneous ventilation can be inadequate.
airway protective reflexes
in deep sedation:
Cardiovascular function is typically preserved, but there may be a partial or complete loss of _________.
General anesthesia
Patients can transition from deep sedation to...
General anesthesia
what type of sedation:
A drug-induced loss of consciousness occurs when patients cannot be awakened, even with painful stimulation.
breathe independently
in general anesthesia:
Their ability to ______ is often impaired, requiring assistance to maintain an open airway + possibly the use of positive-pressure ventilation.
Cardiovascular
in general anesthesia:
______ function may be impaired.
Nitrous oxide
Benzodiazepines: diazepam, midazolam
Opioids (meperidine, morphine)
Antihistamines
Dexmedetomidine
List the 5 common sedation agents.
Depressant
Nitrous oxide is a CNS _________ (minimal CV or respiratory effect).
5, 10
Nitrous oxide has induction time of _ minutes and recovery __ minutes.
true
T/F: Nitrous oxide is an anxiolytic w/ minimal analgesia
20-70
Nitrous oxide: __% concentration w/ an open system + nasal hood
Peripheral neuropathies
Chronic nitrous oxide exposure/abuse can occur in dental professionals and may result in ________ ___________.
lack of potency
dependent on psychological reassurance
interference of nasal hood w/ injection of anterior max
pt must be able to breathe through nose
NO2 pollution + potential occupational exposure hazards
5 disadvantages of nitrous oxide
Midazolam (Versed)
Diazepam (Valium)
CNS depression, minimal CV effects occurs with which 2 sedation agents?
respiratory depression
There is risk of ______ with Midazolam (Versed) and Diazepam (Valium).
Anterograde
_________ amnesia occurs with Midazolam (Versed).
15 min onset; 20-30 min working time
Onset vs. working time for Midazolam (Versed)
0.5-1 mg/kg to 20 mg max dose
Oral dose of Midazolam (Versed)
0.2-0.3 mg/kg to 10 mg max dose
Intranasal dose of Midazolam (Versed)
3-4
Midazolam (Versed) has _x potency of diazepam (valium).
Paradoxical negativism "angry child"
What condition:
2% of patients
Agitated and combative
Screaming and flailing
Midazolam (Versed)
Paradoxical negativism "angry child" is associated with which sedative?
45-50 min onset; peak 60 min with 45-60 min working time
Onset vs. working time for Diazepam (Valium)
0.2-0.3 mg/kg orally with max dose 15 mg as single agent or
10 mg in combo with other agents
Dose of Diazepam (Valium)
Narrow-angle glaucoma
Contraindication for Diazepam (Valium)
20-40 hours but can be extended in some patients because of an active metabolite
Diazepam (Valium) half life = ?
Flumazenil (benzodiazepine)
What pediatric reversal agent do we use?
IV: 0.01 mg/kg to 1 mg max
IN: 0.04 mg/kg to 0.2 mg max
Typical pediatric dose of Flumazenil (reversal agent benzodiazepine)
pulse oximetry
ECG
capnography
noninvasive BP
4 monitoring modalities used for pt safety
Pulse oximetry
Which modality:
Oxygenation (SpO2)
Late indicator of ventilatory problems
ECG
Which modality:
Heart rhythm
Detects arrhythmias
Capnography
Which modality:
Ventilation (EtCO2)
Early indicator of hypoventilation/apnea
Noninvasive BP
Which modality:
Perfusion trend
Cuff size matters
Less
The younger the age, the ____ accepting of sedation.
Less
Sedation is ____ likely to be successful for child with cognitive impairment.
Child's behavior (temperament)
#1 factor influencing sedation outcome
Difficult
Socialization: child with few limits or boundaries can be "_______" = not a good candidate for sedation
Temperament
A powerful indicator of a child's response to dental treatment
Behavioral style of an individual while interacting with the surroundings
definition of temperament
Age, temperament
Both ___ and ___________ seem to act as predictors of child behavior in the dental setting.
4, ++
which Frankl classification:
Definitely positive, good rapport, interest in dental procedures, laughs and enjoys
3, +-
which Frankl classification:
Positive, accepts treatment but may be cautious or reserved, follows directions
2, -+
which Frankl classification:
Negative, reluctant, timid, uncooperative
1, --
which Frankl classification:
Definitely negative, refusal of treatment, defiant, unable to cooperate
Tell-show-do
Most effective for children with communicative/interactive ability, can be used with any child
Hearing impaired
When is tell-show-do contraindicated?
Positive reinforcement
which behavior management technique:
Rewards desired behavior
Best when immediate-concept
Requires consistency and avoid rewarding undesirable behavior
Realization that the desired behavior may be less than totally desired but is still a positive step to be recognized
Distraction
which behavior management technique:
Attention is directed from dental procedure
Affects pain perception
Dental applications: videogames, headphones, storytelling
Voice control
which behavior management technique:
Controlled alteration of voice to direct behavior
Volume
Tone
Pace
Study of Loud Voice control punishment
Highly effective in reducing disruptive behaviors
Unacceptable
Greenbaum et al 1990 - Rated voice control as __________ by parents.
Parental absence/presence
which behavior management technique:
Indicated in any pt who has the potential to be cooperative
Previously cooperative child who becomes uncooperative and practitioner asks parents to leave operatory until child becomes compliant
Most common technique of parental absence/presence involves...
Parents unwilling/unable to extend effective support
Child unable to understand that parent's presence is contingent on cooperation
When is parental absence/presence contraindicated?
Direct observation/modeling
ID the basic behavior guidance technique:
Patient observes another patient exhibiting cooperative behavior during tx
Can be through live model or video
1. Protective stabilization
2. Sedation
3. General anesthesia
What are the 3 advanced behavior guidance techniques?
Risks
Benefits
Alternatives of behavior guidance
Informed consent should be presented in a language easy for parents' understanding and should address: (3)
True
T/F: Advance Behavior Management requires a separate informed consent.
Custom pressure-laminated mouthguards have the best protective qualities (multiple layers)
How do we prevent traumatic dental injuries?
1. Med hx
2. Neurological eval (important to evaluate cranial nerves, nausea, loss of consciousness) they require immediate referral
3. Clinical Exam:
• Radiographs and Photographs
• Indicators of Cranial Fracture (Battle Sign, Racoon Sign)
What are the thorough diagnostic steps for managing traumatic dental injuries? (3)
Battle sign
Raccoon sign
What 2 signs are indicators of cranial fracture?
Uncomplicated
Uncomplicated or complicated trauma to permanent dentition:
Enamel/dentin
Complicated
Uncomplicated or complicated trauma to permanent dentition:
Pulp involvement
Radiograph, resin restoration
Treatment for uncomplicated trauma
Open apex: preserve pulp vitality CaOH2
Matural apical development: RCT
Treatment for complicated trauma
Root fracture
Which trauma:
Coronal segment mobile + displaced
Tender to percussion
Bleeding from gingival sulcus
False negative initially
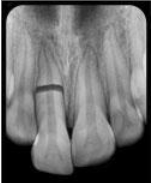
Root fracture
Which trauma:
Crown discoloration (red, gray)
Cervical
For root fracture:
Horizontal plane fracture: ________ third fractures (radiograph PA 90)
Apical
For root fracture:
Oblique plane fracture: _______ third fractures (radiograph occlusal)
Reposition ASAP
Verify position with radiographs
Stabilization flexible splint 4 weeks (apical + middle third)
A patient presents with a root fracture. How do you go about treating them if it's displaced?
Stabilization with flexible splint (up to 4 months) longer period is beneficial
A patient presents with a root fracture. How do you go about treating them if the root fracture is near the cervical area?
RCT
A patient presents with a root fracture. How do you go about treating them if it's necrosed?
1 year
Monitor healing of root fractures for up to ...
Hard tissue healing
On mature teeth with root fracture, repositioning of fragment increases frequency of...
Pulp revascularization, high repair for young cells, healed even sub-optimal repositioning
On immature teeth with root fracture, there is favorable...
Concussion
Which trauma:
Tender to touch or tapping
No displacement or mobility
Sensibility test +
None
Radiographic findings of concussion and subluxation
Monitor pulp condition for a year
A patient presents with concussion. How do you treat them?
Subluxation
Which trauma:
Tender to touch or tapping
No displacement
Increased mobility
Bleeding from gingival crevice
Sensibility test -
No treatment normally
Stabilization for patient comfort if excessive mobility
Monitor normal pulpal response
How do you treat a patient with subluxation?
Subluxation has mobility
Both concussion and subluxation are tender to touch or tapping. How do you tell the difference?
Extrusive luxation
Which trauma:
Tooth appears elongated
Excessively mobile
Sensibility test -
Increased PDL space apically
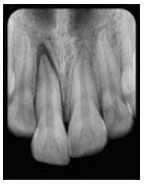
Extrusive luxation
Which trauma:
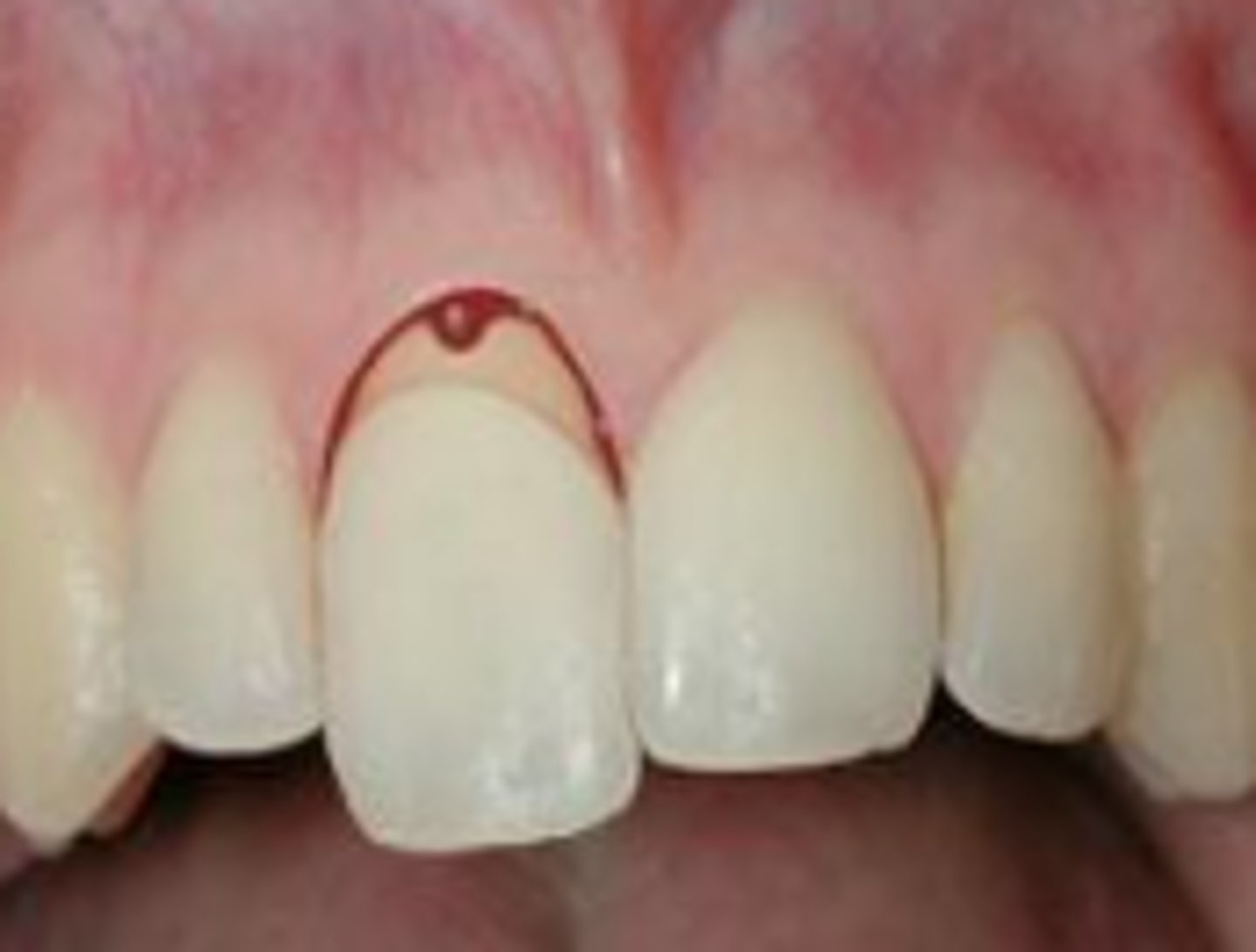
Reposition gently into socket, 2 weeks
A patient has an extrusive luxation and needs treatment. What do you do, and how long does stabilization take?
Lateral luxation
Which trauma:
Tooth displaced in palatal/lingual or labial direction
Nonmobile
Sensibility test -
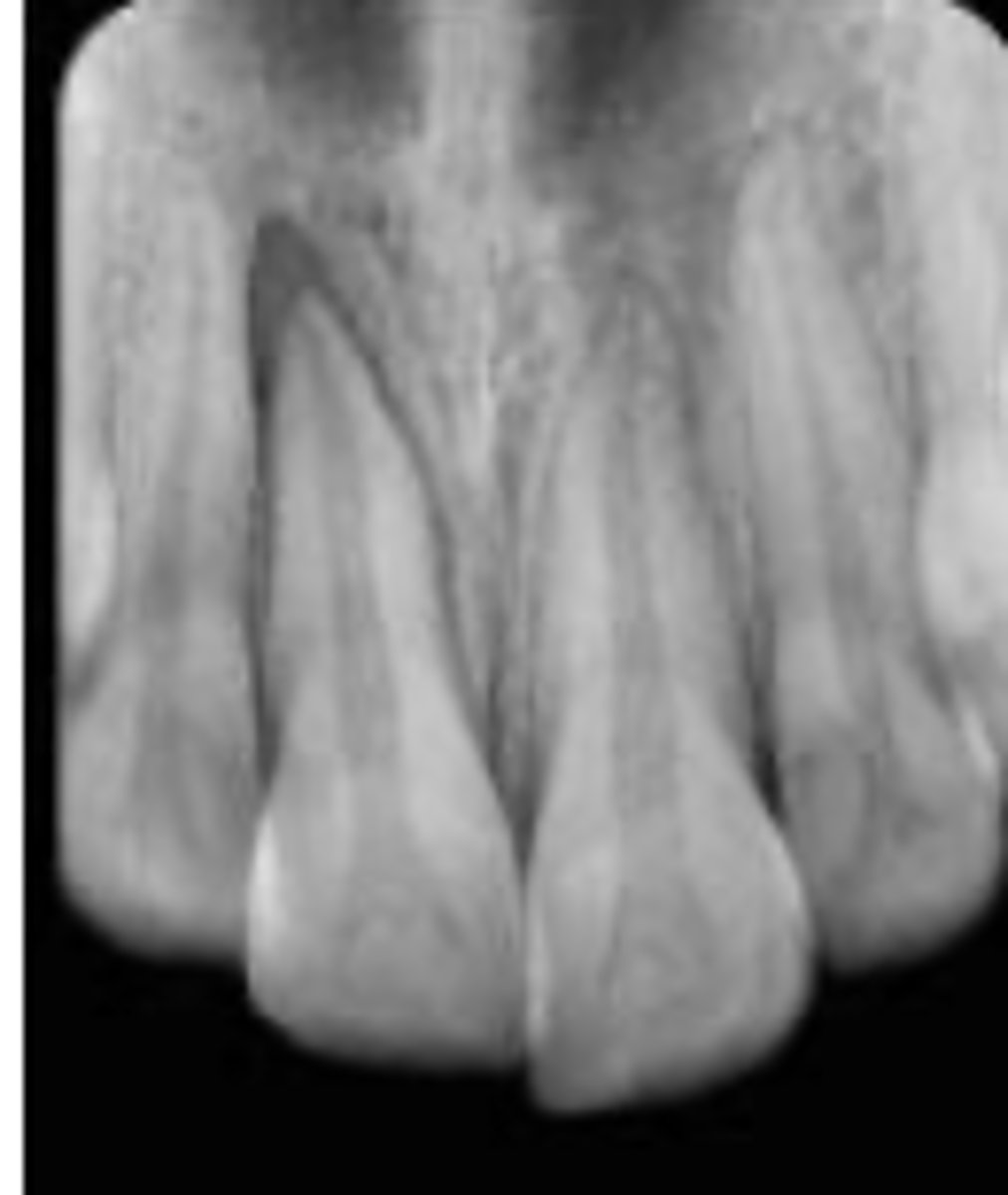
Lateral luxation
A patient presents with a tooth displaced lingually and on percussion, there is a high metallic sound. Which trauma is it?
Widened PDL occlusally
What would you find on the radiographs of a patient who experienced lateral luxation?
Reposition tooth digitally or with forceps to disengage from bony lock
Stabilization 4 weeks
Monitor pulp
How do you treat lateral luxation?