General Patient Care 1
1/56
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
57 Terms
Thermometer
Used to measure body temperature
Stethoscope
Used to amplify sounds in the body, such as the beating of the heart, respirations in the lungs, and bowel sounds in the abdomen
Sphygmomanometer
Used to measure blood pressure
Pulse oximeter
Used to measure oxygen saturation in the blood
Otoscope
Used to examine the ears
Ophthalmoscope
Used to examine the interior of the eye, especially the retina
Dermatology
A medical assistant may assist in minor surgical procedures to help obtain skin biopsies or in the debridement of wounds and collect specimens from wound cultures. Follow sterile procedures when assisting in minor surgical procedures and obtaining wound cultures.
biopsy
Dermal cutter
Scalpel
Gauze
Incision and drainage tray
Specimen collection swabs and containers
Cardiology
A medical assistant may need to perform electrocardiograms (EKGs) and Holter monitoring on patients with cardiac symptoms or diseases. Both tests are used to monitor and record the heart’s electric activity and are often used to diagnose heart disorders, especially regarding its rhythm and rate.
Three-channel electrocardiograph
Electrodes
EKG paper
Holter monitor
Endocrinology
Endocrinology involves hormones. Medical assistants should be familiar with venipuncture and capillary punctures (fingersticks). Medical assistants will perform glucose monitoring and patient education related to proper use of glucose monitoring equipment.
Glucometers
Alcohol pads
Adhesive strips
Test strips
Lancets
Neurology
A neurological examination focuses on the patient’s reflex response, motor response, muscle tone, speech patterns, coordination, sensory response, gait, and mental status and behavior. The MA may assist the provider throughout the exam, as directed.
Obstetrics and Gynecology
This specialty practice may assist in a number of procedures, including minor surgery. A common procedure is a Pap test. A Pap test is a screening procedure that collects and examines cells from the vaginal and cervical mucosa to check for precancerous or abnormal cells.
Vaginal speculums and retractors
Cytology kits
Stitch removal sets
Dressing kits
Exam tables with stirrups
Ultrasound machine
Handheld fetal Doppler machine
Pulmonology
A pulmonology practice may conduct different tests to assess respiratory function, to assist in the diagnosis of patients with suspected obstructive or restrictive pulmonary disease, and to assess the effectiveness of medication and other pulmonary therapies.
One of the most common tests to evaluate lung function that a medical assistant may perform is a pulmonary function test (PFT). The most common tests and procedures performed are spirometry, peak flow meters, and pulse oximetry.
Spirometers are small, handheld devices that provide digital readings, and there are portable meters with integrated printers. Advanced spirometry systems are computerized and can be configured to send results directly to a patient’s electronic health record (EHR). All spirometers consist of a mouthpiece and tubing connected to a recording device.
The peak flow meter is often used for patients who have asthma to monitor their daily respiratory function and condition. The peak flow meter measures the fastest rate at which the patient exhales after taking a maximum breath.
Oxygen saturation is commonly measured by a pulse oximeter, which is a noninvasive device that is clipped on the fingertip, bridge of the nose, forehead, or earlobe.
true
Before a colonoscopy, the patient must prepare by eating a low-fiber diet, consuming clear liquids, and taking a laxative.
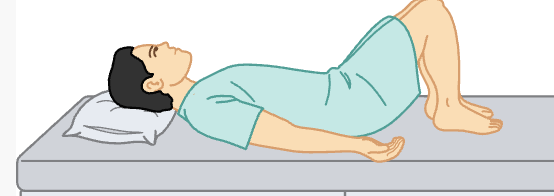
Supine
Horizontal recumbent
patients lie flat on their back with hands at the sides
patient should be draped from the chest down to the feet
Prone
requires the patient to lie face down, flat on the stomach, with the head turned to one side, and arms either alongside the body or crossed under the head
used for back exams and certain types of surgery
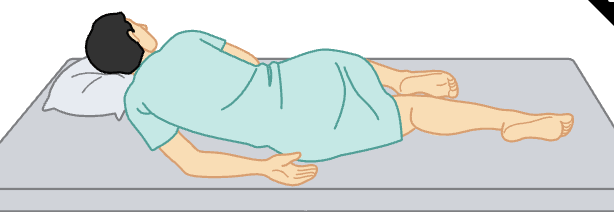
Dorsal Recumbent
the patient is lying flat on the back with knees bent and feet flat on the examination table.
used to inspect the head, neck, chest, vaginal, rectal, and perineal areas
can be used for digital (using the gloved fingers) exams of the vagina and rectum
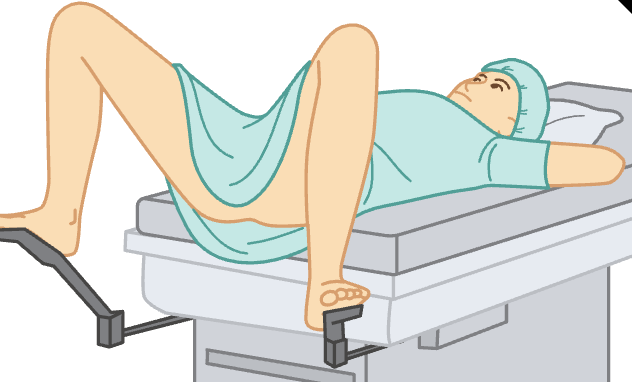
lithotomy
the patient’s feet are placed in stirrups attached to the end and sides of the table
After the feet are in place in the stirrups, the patient is instructed to slide down until the buttocks are positioned at the edge of the table. The patient is draped from under the arms to the ankles. This position is used for vaginal examinations, often requiring the use of a vaginal speculum (an instrument used to hold open the walls of the vagina) and for obtaining cell samples of the cervix
Fowler’s
the patient sits on the examination table with the head of the table raised to a 90-degree angle
If able, the patient may be seated on the edge of the table with feet over the edge in an upright position. This position is useful for examinations of the head, neck, and upper body.
Semi-Fowler’s
modified Fowler’s position with the head of the table at a 45-degree angle instead of a 90-degree angle. This position is used for postsurgical exams and patients with breathing difficulties or lower back injuries
Left Lateral/Sims’ position
requires the patient to be placed on the left side with the right leg sharply bent upward and the left leg slightly bent
right arm is flexed next to the head for support. The patient is draped from under the arm or shoulders to below the knees at an angle. This allows the health care provider to raise a small section of the drape while keeping the rest of the patient covered. This position is used for rectal exams, taking rectal temperatures, enemas, and perineal and pelvic exams.
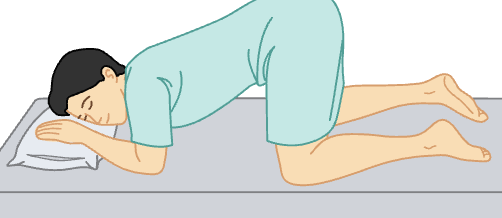
knee chest
the patient is placed in the prone position and then asked to pull the knees up to a kneeling position with thighs at a 90-degree angle to the table and buttocks in the air. The head is turned to one side, and the arms may be placed under the head or on either side of the head for comfort and support. This position is used for proctologic exams, sigmoidoscopy procedures, and rectal and vaginal exams.
parenteral route
Administered or occurring in the body bypassing the gastrointestinal tract.
non-oral
injected directly into the body
nonparenteral route / enteral route
oral medication given by the mouth delivered to the gastrointestinal tract.
otic
relating to the ear
subcutaneous, intravenous, intradermal, intramuscular
parenteral routes
subcutaneous
Injection administered below the skin layer into the adipose (fat) layer
intradermal
Injection administered into the dermis
intramuscular
Injection administered into the muscle
intravenous
Injection administered directly into the vein
sublingual
Placed under the tongue
buccal
Between the cheek and gums resulting in rapid absorption
Inhalation
Inhaled through the mouth, passes through the trachea into the lungs; inhaled through the nose and absorbed through the nasal mucous membrane
Ocular or otic
Drops of medication are instilled directly into the eye (ocular) or ear (otic).
Transdermal
Applied to the skin and designed to release slowly and systemically into circulation. Administered in an adhesive patch in a single layer drug, multi-layer drug, drug in resevoir, or drug matrix.
Topical
Applied to the skin or mucous membrane (faster) and acts locally. Administered as creams, ointments, or emulsions.
ok
Right Patient
Use two patient identifiers, usually full name and date of birth, to verify the right patient. Then verify that data with the information on the medical record or medication administration record (MAR).
Right Medication
Check the label three times to verify the medication, strength, and dose—often referred to as the “three befores.” The first time to check the medication label is when taking the medication container from the storage cabinet or drawer. The second is when taking the medication from its container to prepare to administer it. The third check is when putting the container back in storage or discarding it.
Right Form
Medications can come in several different forms. Some of these include liquid, tablet, capsules, suppositories, drops, and creams. The same medication can be available in several different forms. For example, amoxicillin can come in a capsule, tablet, chewable tablet, and liquid. Each form of medication has benefits in terms of effectiveness, ease of use, and safety. Checking the correct form of medication to be administered is essential when checking all rights of medication administration.
Right Dose
Compare the dosage on the prescription in the patient’s MAR with the dosage on the medication’s label and determine if medication calculations need to be performed to arrive at the prescribed dose.
Right Route
Compare the route on the prescription in the MAR with the administration route they are planning to use. Determine whether the route is appropriate for the patient and that the medication formulation is right for that route.
Right Time
In most office and clinic settings, MAs give medications right after the provider writes the order. Nevertheless, always confirm whether the medication has any timing specifications, such as the patient having an empty stomach or waiting several hours after taking another medication (such as an antacid) that might interact with the new medication.
Right Technique
MAs must know the correct techniques for administering every medication they give by every route, for example, taking an apical pulse prior to administering digoxin to ensure the patient’s pulse is not less than 60.
Right Education
Prior to administration of a medication, explain to the patient the name of the medication, the ordering provider, and the reason and intended effect of the medication; disclose any side effects; and confirm any allergies the patient may have.
Right Documentation
Always document administering a medication after the patient receives it, not before. If you do not administer a medication as prescribed, the documentation must include this and why the patient did not receive it. Proper documentation includes date, time, quantity, medication, strength, lot number, manufacturer, expiration date, consent obtained, and patient outcome.
Critical devices
come in contact with blood or normally sterile tissue
Semi-critical devices
come in contact with mucus membranes
Non-critical devices
come in contact with unbroken skin
Sterilization
The complete destruction of all micro-organisms through specific means.
required for all instruments and equipment that will penetrate a patient’s skin, enter a patient’s body, or come in contact with any other normally sterile areas of the body.
ampule
Sealed glass capsule containing a liquid.
Subcutaneous (SC) injection sites
5/8 inch needle
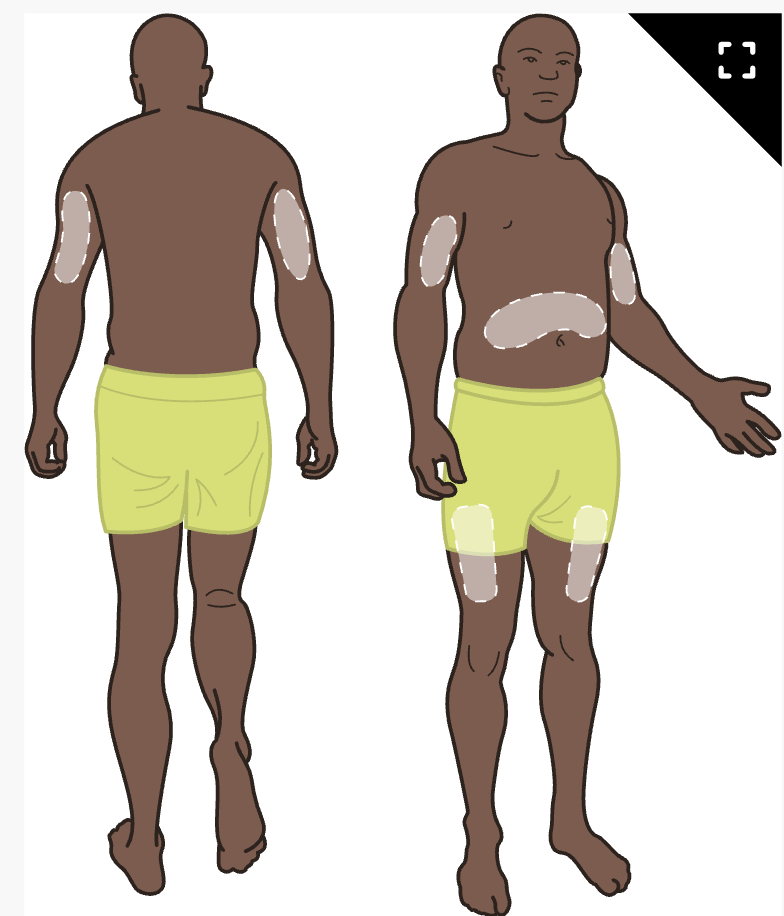
Intradermal (ID) injection sites
¼ to ½ inch needle
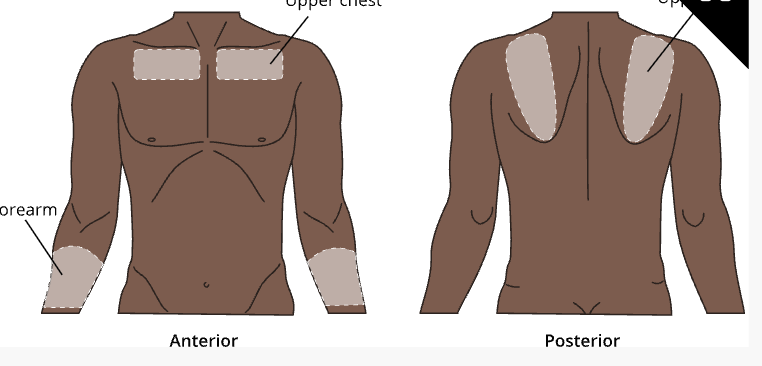
Intramuscular (IM) injection sites
1 to 1 ½ inch needle
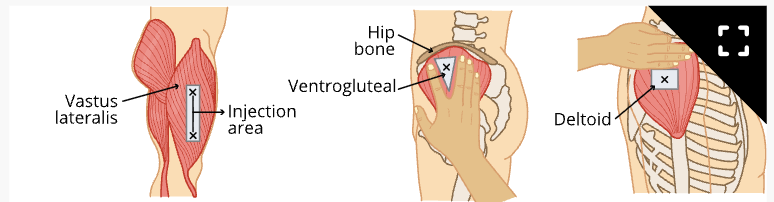
Premeasured Syringes
prefilled syringes that are single dosed and packaged with the needle that is provided by the manufacturer. These syringes are disposable and supplied already loaded with the substance to be injected
Hypodermic Syringe
come in a variety of sizes from 0.5 to 60 mL and even larger. Syringes are calibrated or marked in milliliters but hold varying capacities. Of the small-capacity syringes, the 3 mL syringe is used most often for the administration of medication
tuberculin syringe
a narrow syringe that has a capacity of 0.5 mL or 1 mL. The 1-mL size is used most often. The volume of a tuberculin syringe can be measured on the milliliter scale.
ok
Store refrigerated medications between 2˚ and 8˚ C (35˚ and 46˚ F). Frozen medications must be stored between –50˚ and –15˚ C (–58˚ and 5˚ F).
Food and Drug Administration
Organization responsible for protecting the public health by ensuring safety, efficacy, and security of human medications.
electronic medical record (emr)
Record in a medical practice or clinic to document the patient’s demographic information, care, progress, and treatment.
ok
The following information must be documented in the MAR about the medication.
Any allergies or history of allergies
What medication is being administered
Medication dosage
Administration route
When is it being administered—what time, how often, how long
The name of the health care provider who prescribed the medication
ok
Most medications’ temperature requirements will fall into one of the following categories.
Room temperature is 20˚ to 25˚ C (68˚ to 77˚F).
Refrigeration means 2˚ to 8˚ C (35˚ to 46˚ F). As mentioned previously, these medications must be stored in a refrigerator that is not used for any other purpose. It must have a thermometer so that staff can regularly monitor its storage temperature. Check the temperature daily when storing regular medications and twice daily for stored vaccines
Eye irrigation
Process of using a sterile solution to flush the eyes of any foreign bodies or any toxic chemicals
Sterile technique
A group of strategies used to reduce exposure to micro-organisms and keep the patient as safe as possible.
Eye irrigation procedure
Assemble the equipment and two sets of the supplies and equipment if both eyes are to be irrigated. This may include a sterile basin, a return basin, sterile solution, a sterile irrigating syringe, sterile gauze, tissues, towel, a waterproof drape, and nonsterile gloves. Perform a triple check of the medication and provider’s order and the rights of administration and check for expiration dates on the medication and all supplies.
Warm the irrigation solution to normal body temperature by placing the solution in a basin of warm water. Place the patient in a supine or sitting position and place a waterproof drape on the patient’s shoulder to absorb any solution if any spills. Perform hand hygiene.
Cleanse the eyelid with a gauze pad moistened with the sterile solution, making sure to maintain sterility at all times. Clean from the inner to outer canthus (corner) of the eye, where the upper and lower lids meet. Repeat with a newly moistened gauze pad until the eyelid is free of dirt and other debris. Instruct the patient to tilt the head toward the side that is being irrigated, to hold the return basin below the affected eye, and to look straight ahead on a fixed object while keeping both eyes open.
Using the thumb and index finger of your nondominant hand, pull upward on the patient’s upper lid and downward on the patient’s lower lid—hold the eye open and maintain this position throughout the irrigation. With the dominant hand, hold the irrigating bottle of solution on or near the bridge of the nose and hold the tip of the solution about an inch above the eye. Do not to touch any part of the eye or skin with the tip of the solution applicator. Start squeezing the bottle so that the solution flows from the inner canthus to the outer canthus in a steady stream directed toward the lower conjunctiva.
Take the collection basin from the patient and dry the eyelid with gauze, once again moving from the inner to outer canthus. Provide the patient with a towel to dry any skin that may have gotten wet during the procedure and help the patient to a comfortable position. Examine and take note of any visible debris in the return basin. Discard the solution from the return basin, throw away disposable items, remove gloves, and wash hands.
Ear irrigation procedure
Ear irrigation is necessary to remove impacted cerumen, or earwax, or a foreign matter from the ear. It will be important for you to explain the procedure to the patient and prepare them for possible mild discomfort. Patient preparation will be similar to the eye irrigation procedure. Supplies you will need are an ear syringe, sterile basin, return basin, warmed irrigation solution, a waterproof drape, towel, and gauze or cotton balls.
For ear irrigation, have the patient sitting or lying on the side with the affected ear facing up. Place a waterproof drape over the shoulder on the side that is being irrigated. Using an otoscope, examine the affected ear, taking note of any cerumen or foreign bodies (if allowed by practice policy). Cleanse the outer ear with a gauze pad moistened with the irrigating solution. Instruct the patient to tilt their head toward the side that is being irrigated and to hold the ear wash basin tightly below the affected ear. Gently insert the disposable tip into the ear so that it is positioned toward the top of the ear canal. Start spraying the solution by pushing the trigger on the spray bottle, checking to be sure the tubing remains straight. Continue to spray until you have used up the solution, the maximum time has been reached, or you have obtained the desired results (cleared the ear of cerumen).
Remove the tip from the patient’s ear, allow any residual solution to drain out, and place a loose cotton ball in the canal.
Dry the outside of the ear. If policy allows, examine the ear with an otoscope to see if all cerumen has been removed. (If not, check with provider about proceeding.) Have the provider check the ear and follow any additional orders. Dispose of the supplies in a waste can and clean the area. Remove gloves and wash your hands.
ok
In addition to the elements required on all prescriptions, electronically generated prescriptions must also have the following.
A DEA number of the prescribing health care provider if the prescription is for a controlled substance
The telephone number of the health care provider
The time and date of the transmission
The name of the pharmacy to which the prescription is sent.