Final Considerations for EKG
5.0(1)
5.0(1)
Card Sorting
1/41
Study Analytics
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
42 Terms
1
New cards
Protected Health Information
Don’t forget that when dealing in any health care scene, to protect the patient's privacy!
* • PHI - Protected Health Information
* Disclosing health information is a breach of patient confidentiality.
* • PHI - Protected Health Information
* Disclosing health information is a breach of patient confidentiality.
2
New cards
HIPAA
Health insurance portability and Accountability Act
3
New cards
Consent
Don’t forget consent! Implied consent counts if the patient is waiting on the table in a gown but still explain what you are doing!
4
New cards
Medical Asepsis
**The clean technique**
• Make sure you are clean when setting up a EKG
• Follow proper work clothing protocols
• Always wash your hands as well as the location the patient will be laying (protect spread/chain of infection)
• Make sure you are clean when setting up a EKG
• Follow proper work clothing protocols
• Always wash your hands as well as the location the patient will be laying (protect spread/chain of infection)
5
New cards
Patient Communication
When the patient walks into the room,
1. Make sure you make eye contact, face the patient, and repeat and clarify anything the patient may have questions about
2. Ask them to state their name and date of birth, this double check the patient as well as informs you of any disabilities they may have
3. Explain the procedure
1. Make sure you make eye contact, face the patient, and repeat and clarify anything the patient may have questions about
2. Ask them to state their name and date of birth, this double check the patient as well as informs you of any disabilities they may have
3. Explain the procedure
6
New cards
Display Professionalism
Details include physical appearance, eye contact, and displaying an understanding and knowledge of the situation (increase patients’ confidence)
7
New cards
Active Listening Skills
Recognizing messages that are being sent through both verbal and nonverbal methods (body language and facial expressions)
8
New cards
Skilled Interview Techniques
Ask patients a variety of open-ended questions that encourage them to provide detailed information (“What medications do you currently take? & “Describe any chest pain or symptoms are experiencing.”) Open communication & provide a broader picture towards ensuring proper care can be delivered.
9
New cards
Provide Empathy
Avoid jumping to conclusions or passing judgments (be empathetic and provide encouragement).
10
New cards
Practice collaboration
Patients are more likely to respond positively to recommendations and questions in collaborative settings - communication is more effective and overall care improves.
11
New cards
Embrace Technology
Technology provides health care professionals many ways to communicate with patients, but DO NOT OVERWHELM THE PATIENT! Only use no more than three communication channel, and if a patient is only comfortable with one, provide communication via that method.
12
New cards
Communication
* Make sure you are not only communicating with your patient, but also with your team
* Ensure the health care provider is up to speed with the patient
* Make sure to properly document through safe and private means of communication: Electronic Health Records, Verbal Exchange, and Encrypted Work Chats
* Ensure the health care provider is up to speed with the patient
* Make sure to properly document through safe and private means of communication: Electronic Health Records, Verbal Exchange, and Encrypted Work Chats
13
New cards
Vital Signs
* When measuring an adult HR, measure the radial pulse for day to day, carotid for emergencies.
* When measuring a child, use the brachial site.
* Children (3-5) HR are 80-120 normal.
* When measuring a child, use the brachial site.
* Children (3-5) HR are 80-120 normal.
14
New cards
Gather the history of
\
1. Social: Smoking, drinking, stress, exercise
2. Medical: Past history, medical conditions, current symptoms
3. Surgical: Past surgeries
4. Medication: What medications do they take
1. Social: Smoking, drinking, stress, exercise
2. Medical: Past history, medical conditions, current symptoms
3. Surgical: Past surgeries
4. Medication: What medications do they take
15
New cards
Preparing the patient
* Patients disrobed from waist up with access for leg lead placements
* Tights should be removed
* Jewelry should be removed, same with electronic devices, such as watches and cell phones
* Depending on the type of EKG the patient is there for, ensure proper educations on the test
* Tights should be removed
* Jewelry should be removed, same with electronic devices, such as watches and cell phones
* Depending on the type of EKG the patient is there for, ensure proper educations on the test
16
New cards
EKG
* Patient is placed in a supine position
* Uses 10 electrodes
* Takes the LEAST amount of time to complete
* Uses 10 electrodes
* Takes the LEAST amount of time to complete
17
New cards
Stress test
* Requires blood pressure checks throughout the procedure
* Use of a treadmill or stationary bike
* Goal of raising the heart rate
* Use of a treadmill or stationary bike
* Goal of raising the heart rate
18
New cards
Ambulatory Monitoring
* Also known as Holter monitor
* Patient has to document events
* Uses 3 to 5 electrodes
* Monitors over a period of time (NO WATER CONTACT)
* Patient has to document events
* Uses 3 to 5 electrodes
* Monitors over a period of time (NO WATER CONTACT)
19
New cards
Check the patient for
* Tachycardia or bradycardia
* Pallor
* Diaphoresis
* Low blood pressure
* Fast/labored/shallowed/slow respirations
* Anxiety or confusion
* Cyanosis
* Chest pain that radiates to back, arms, or jaw
* Chest tightness (squeezing sensation)
* Shortness of breath
* Nausea and vomiting
* Lightheadedness
* Weakness
* Syncope (EMERGENCY HELP NEEDED)
* Pallor
* Diaphoresis
* Low blood pressure
* Fast/labored/shallowed/slow respirations
* Anxiety or confusion
* Cyanosis
* Chest pain that radiates to back, arms, or jaw
* Chest tightness (squeezing sensation)
* Shortness of breath
* Nausea and vomiting
* Lightheadedness
* Weakness
* Syncope (EMERGENCY HELP NEEDED)
20
New cards
Channels
3 channels records 3 leads aka 3 EKG readings at once (single channel records one lead)
21
New cards
Preparing the EKG
What you need:
1. EKG machine
2. Power Source
3. Electrodes
4. Leads with clips or connectors
5. EKG graph paper (if not digital)
6. Alcohol wipes
7. Gauze pads
8. Scissors and razors
9. Pillows, blankets, and gowns
1. EKG machine
2. Power Source
3. Electrodes
4. Leads with clips or connectors
5. EKG graph paper (if not digital)
6. Alcohol wipes
7. Gauze pads
8. Scissors and razors
9. Pillows, blankets, and gowns
22
New cards
12-lead EKG Positioning
Supine position or semi supine
23
New cards
3-5 lead EKG Positioning
Also known as traveling EKG
Any positioning but ensure patient does not remove the leads and continues with activities
Any positioning but ensure patient does not remove the leads and continues with activities
24
New cards
Stress Testing Positioning
Patient is on the treadmill so they are active during this EKG
25
New cards
Lead I
DIFFERENT FROM V1
Records impulses between left and right arms
Records impulses between left and right arms
26
New cards
Lead II
DIFFERENT FROM V2
Records impulses between right arm and left leg
Records impulses between right arm and left leg
27
New cards
Lead III
DIFFERENT FROM V3
Records impulses between the left arm and left leg
Records impulses between the left arm and left leg
28
New cards
Lead AVL
The left leg and right arm assist with the left arm tracing
29
New cards
Lead AVR
The left arm and left leg assist with the right arm tracing
30
New cards
Lead AVF
The right and left arms assist with the left leg tracing
31
New cards
First 3 Leads
Bipolar and record impulses that travel from a negative to positive pole at specific positions in the heart
32
New cards
Last 3 Leads
Unipolar and due to poor illustration of waveforms, they must be augmented and get assistance from two poles to enhance the tracing
33
New cards
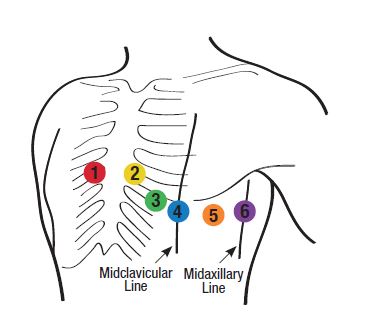
V1
Fourth intercostal space (ICS), right of sternum
34
New cards
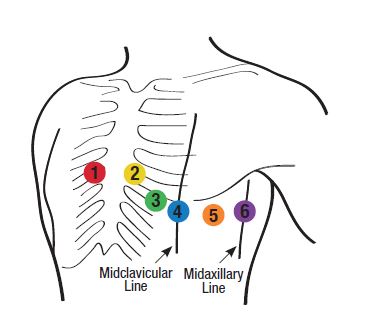
V2
Fourth ICS, left of sternum, directly across from V1
35
New cards
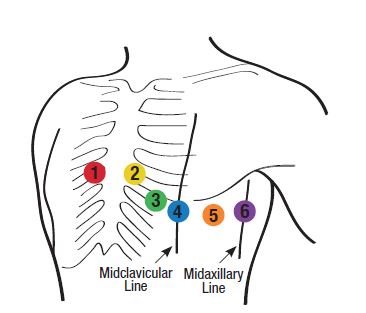
V3
Midway between V2 and V4
36
New cards
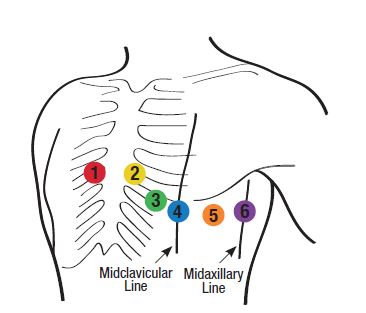
V4
Fifth ICS, midclavicular line
37
New cards
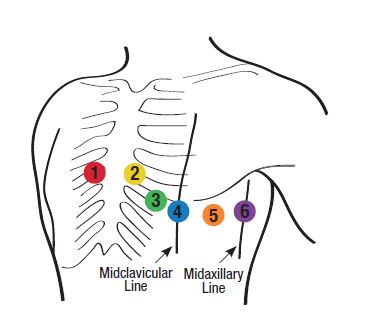
V5
Fifth ICS, midway between V4 and V6, at the anterior axillary line
38
New cards
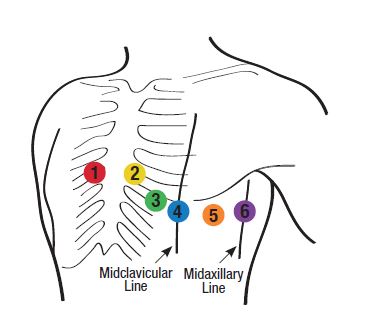
V6
Fifth ICS, at the midaxillary line
39
New cards
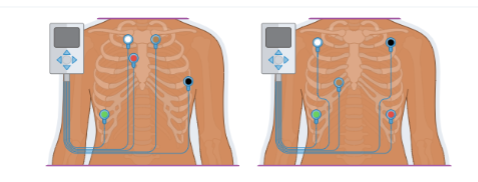
Five-lead EKG
White lead: Right sternal border, first rib
Red lead: Right sternal border, third rib
\
Black lead: Left side, anterior axillary line, fifth rib
Brown lead: Left sternal border, first rib directly opposite the white lead
\
Green lead: Right lower thoracic area anywhere on the rib
Red lead: Right sternal border, third rib
\
Black lead: Left side, anterior axillary line, fifth rib
Brown lead: Left sternal border, first rib directly opposite the white lead
\
Green lead: Right lower thoracic area anywhere on the rib
40
New cards
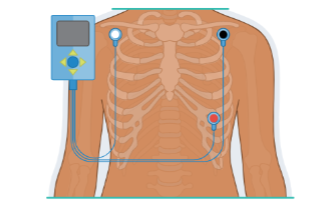
Three-lead EKG
White lead: Right shoulder just below the clavicle
Black lead: Left shoulder just below the clavicle
Red lead: Below the left pectoral muscle at the apex of the heart
Black lead: Left shoulder just below the clavicle
Red lead: Below the left pectoral muscle at the apex of the heart
41
New cards
Specific Considerations
* Some cardiac conditions (ST segment, elevation, myocardial infarction, dextrocardia) and patient younger than 8 years of require right sides 12-lead EKG
* Posterior placement is rare for inferior wall infarcation
* Posterior placement is rare for inferior wall infarcation
42
New cards
Patient Monitoring
• During the EKG, ALWAYS monitor the patient
• Notify the provider if there are any arrhythmias or other hypotensions
• If cardiac arrest occurs, shut off the machine and alert EMS
• Notify the provider if there are any arrhythmias or other hypotensions
• If cardiac arrest occurs, shut off the machine and alert EMS