NCLEX: Mark Klimek - Lecture 11 (Fetal Monitoring Patterns, Variations in Newborn, OB Meds, Medication TIPS, Pediatric Teachings, & Psych TIPS)
1/70
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
71 Terms
What is a low fetal heart rate?
<110
What do you do for a low fetal heart rate?
Starts with L. This is BAD! - Perform "LION"
What is a high fetal heart rate?
>160
What do you do for a high fetal heart rate?
Document acceleration of fetal HR
Take the mother's temperature
Not a high priority; baby is WNL.
What is a low baseline variability?
Fetal HR stays the same - it doesn't change
What do you do for a low baseline variability?
Starts with L. This is BAD! - Perform "LION'
What is a high baseline variability?
Fetal heart rate is always changing
What do you do for a high baseline variability?
This is GOOD! Document findings.
What do you do for an acceleration?
VEAL CHOP
High FHR - Okay
No interventions
Shows random upward bumps on FHR monitor
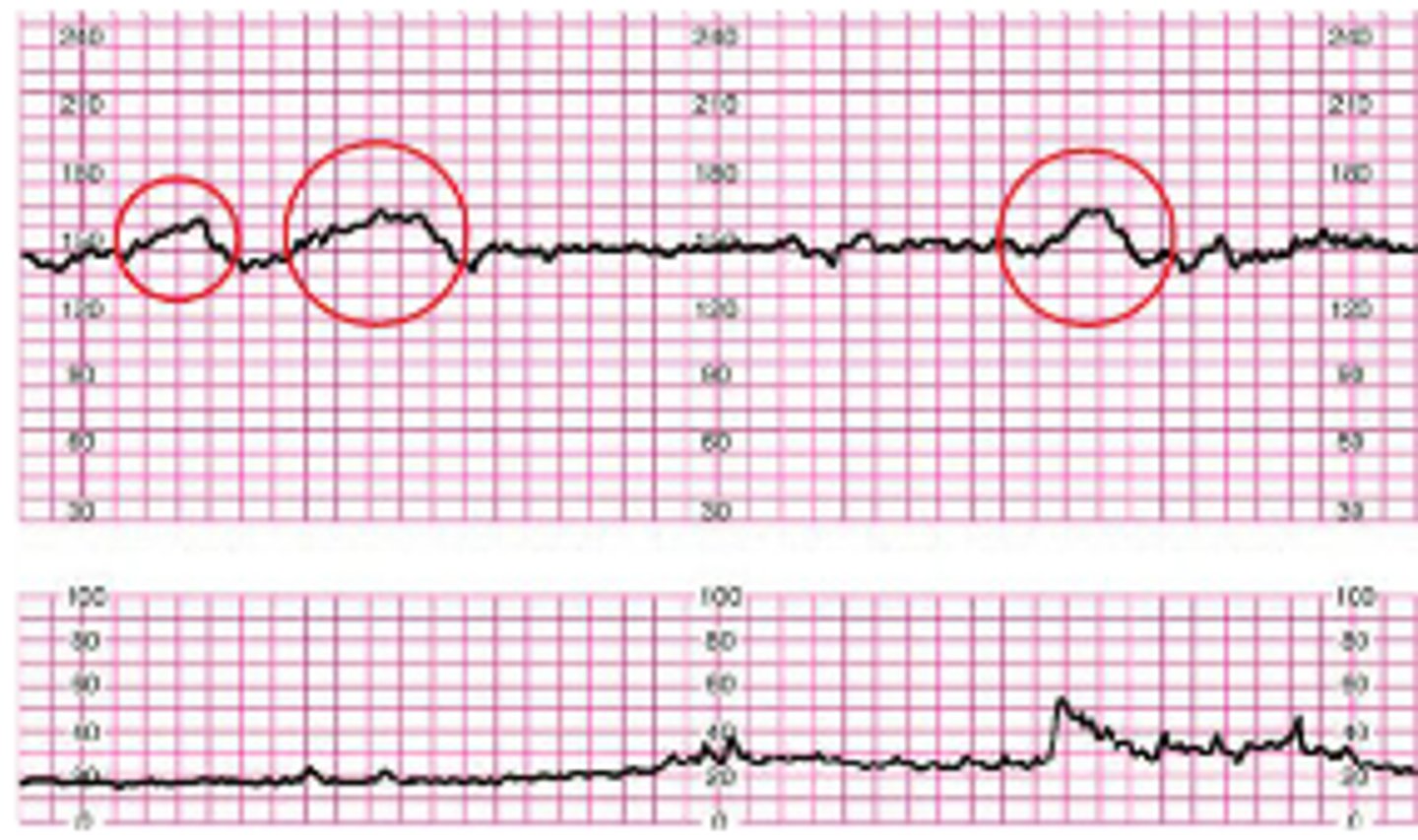
What do you do for a late deceleration?
VEAL CHOP
Placental Insufficiency - "LION"
Stop Pitocin first if running.
What do you do for an early deceleration?
VEAL CHOP
Head compression - Continue to monitor
Document findings
Shows low bumps on FHR monitor that align with contractions
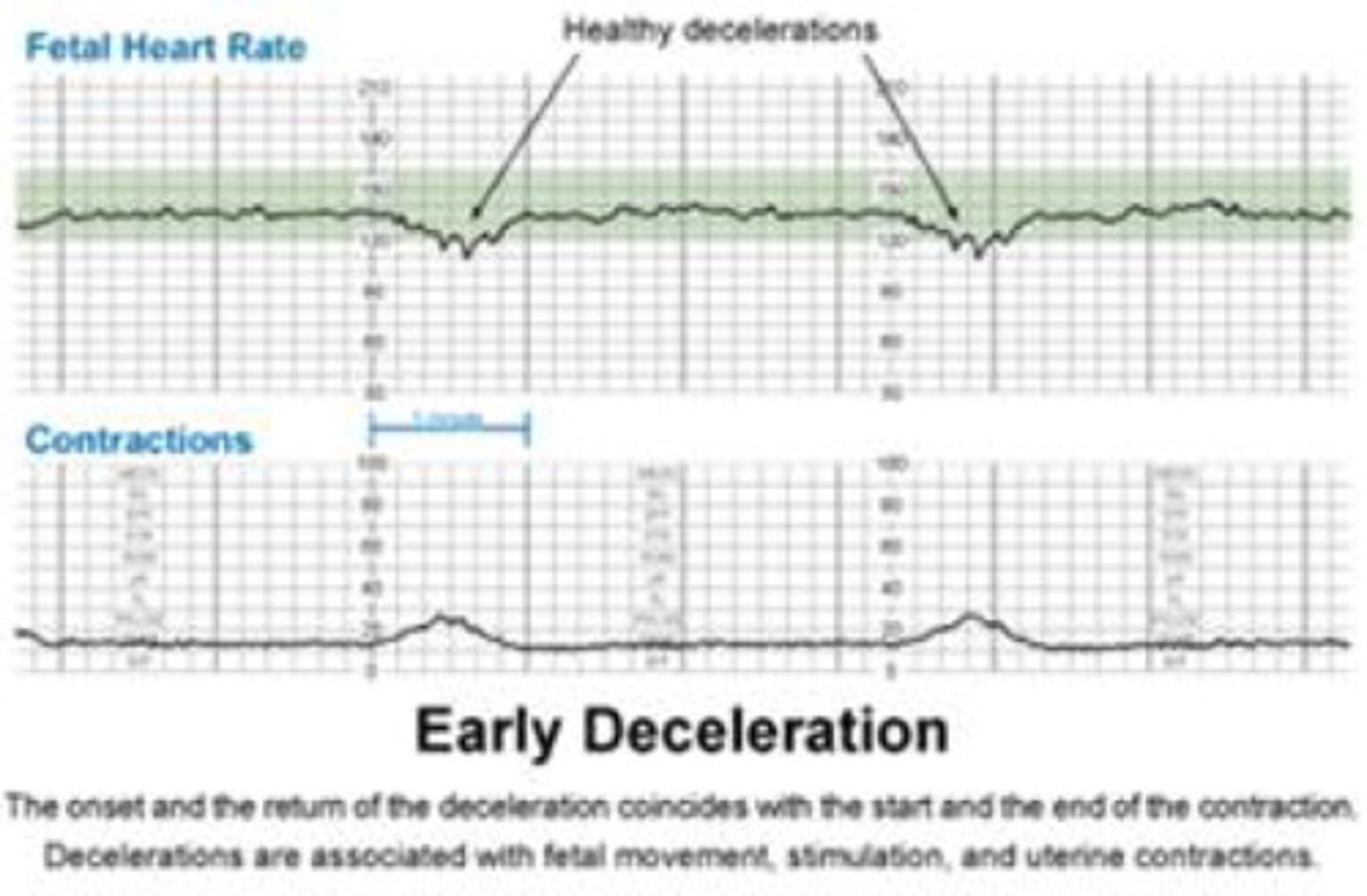
What do you do for a variable deceleration?
VEAL CHOP
Cord compression - "LION"
Shows random low bumps on FHR monitor that don't align with contractions.
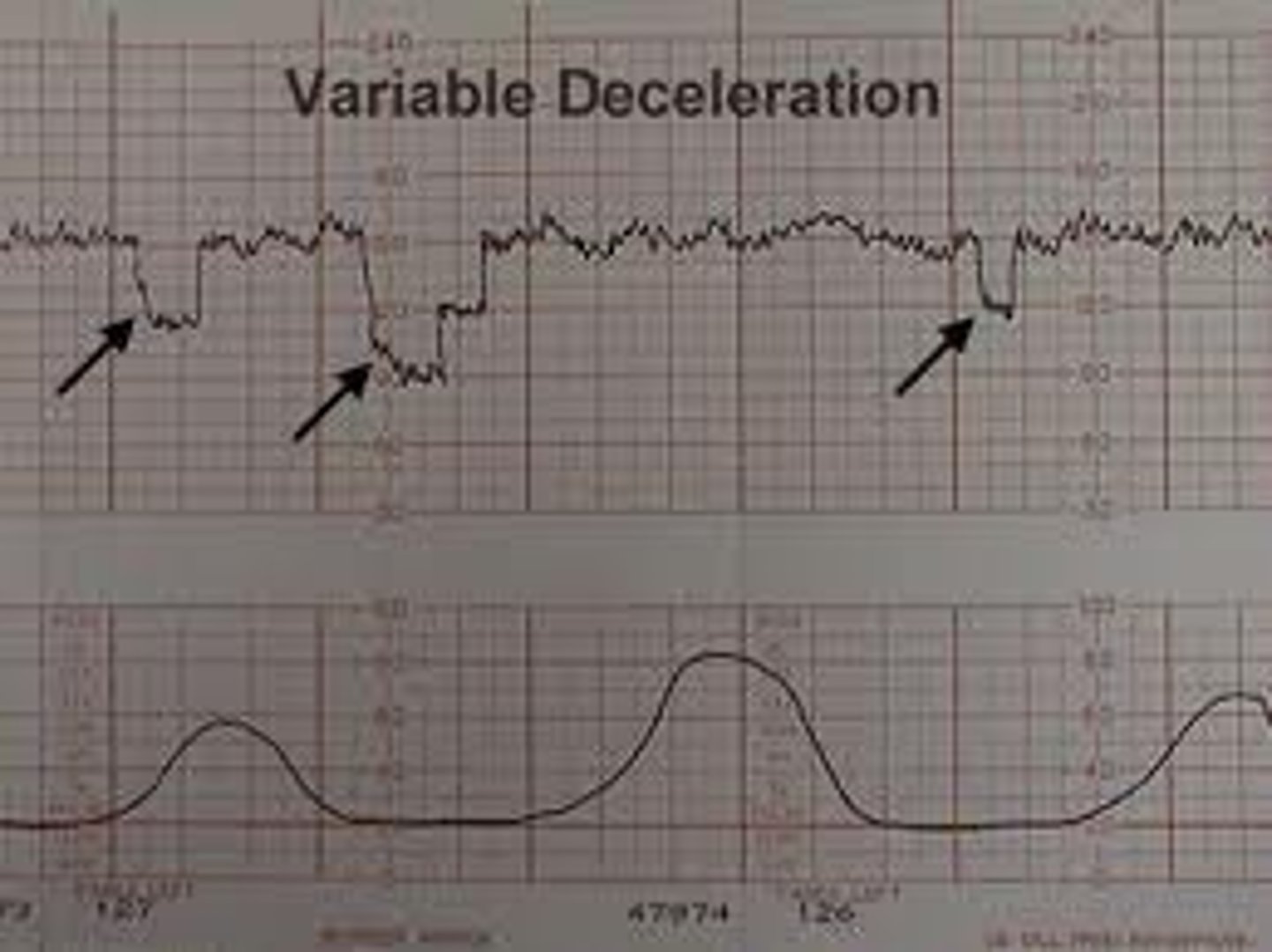
No matter what happens in OB, what would you do?
Check FHR.
What is the intervention order of 2nd stage of L&D?
Delivery of fetus:
- Deliver head - mother should stop pushing!
- Suction the mouth then the nose - ABC order
- Check for nuchal (around the neck) cord
- Deliver the shoulders, next, the body
- Make sure baby has ID band on BEFORE leaving delivery area
What is the intervention order of 3rd stage of L&D?
Delivery of placenta:
- Make sure placenta is complete and intact
- Check for 3-vessel (not 2) cord - 2 arteries, 1 vein (AVA)
What is the intervention order of 4th stage of L&D?
Recovery:
* 4 things to do in 4th stage, 4 times an hour! *
- V/S: Assess for shock... BP down, HR up. Pale, cold, clammy.
- Fundus: Massage if boggy; catheterize if displaced
- Check perineal pads: Excessive bleeding if pad is saturated in <15 min.
- Roll pt over and check for bleeding underneath!!
What assessments would you do postpartum?
- Assess every 4-8 hours
- Assess for "BUBBLE HEAD" :
Breasts
Uterine/fundus - Should be FIRM - IMPORTANT
Bladder
Bowel
Lochia - Rubra (red), Serosa (rosy pink), Alba (White) - IMPORTANT
Episiotomy
Hemoglobin/hematocrit
Extremities - Look for thrombophlebitis - IMPORTANT
Affect
Discomforts
What are the 3 important assessments you should know postpartum?
Uterine fundus - Should be FIRM
Lochia - Rubra (red), Serosa (rosy pink), Alba (White)
Extremities - Look for thrombophlebitis
What should the postpartum uterine tone, height, and
location normally be?
Uterine tone should be FIRM.
Fundal height drops about 2 cm postpartum.
Location should be MIDLINE.
What is the best way to determine if a pt has thrombophlebitis?
Measure bilateral calf circumference
What is milia?
A whitehead trapped under the skin; usually disappear after a few weeks
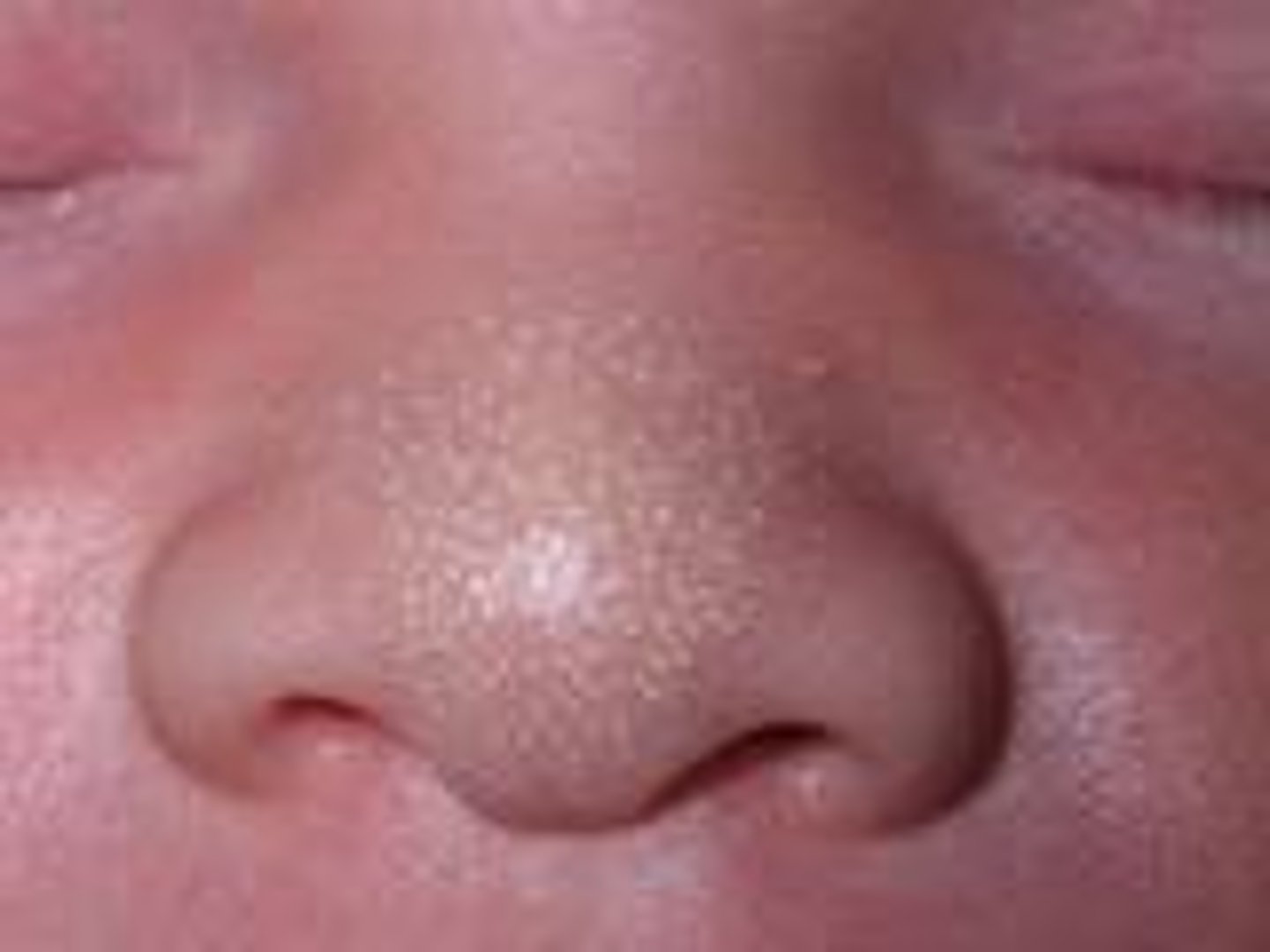
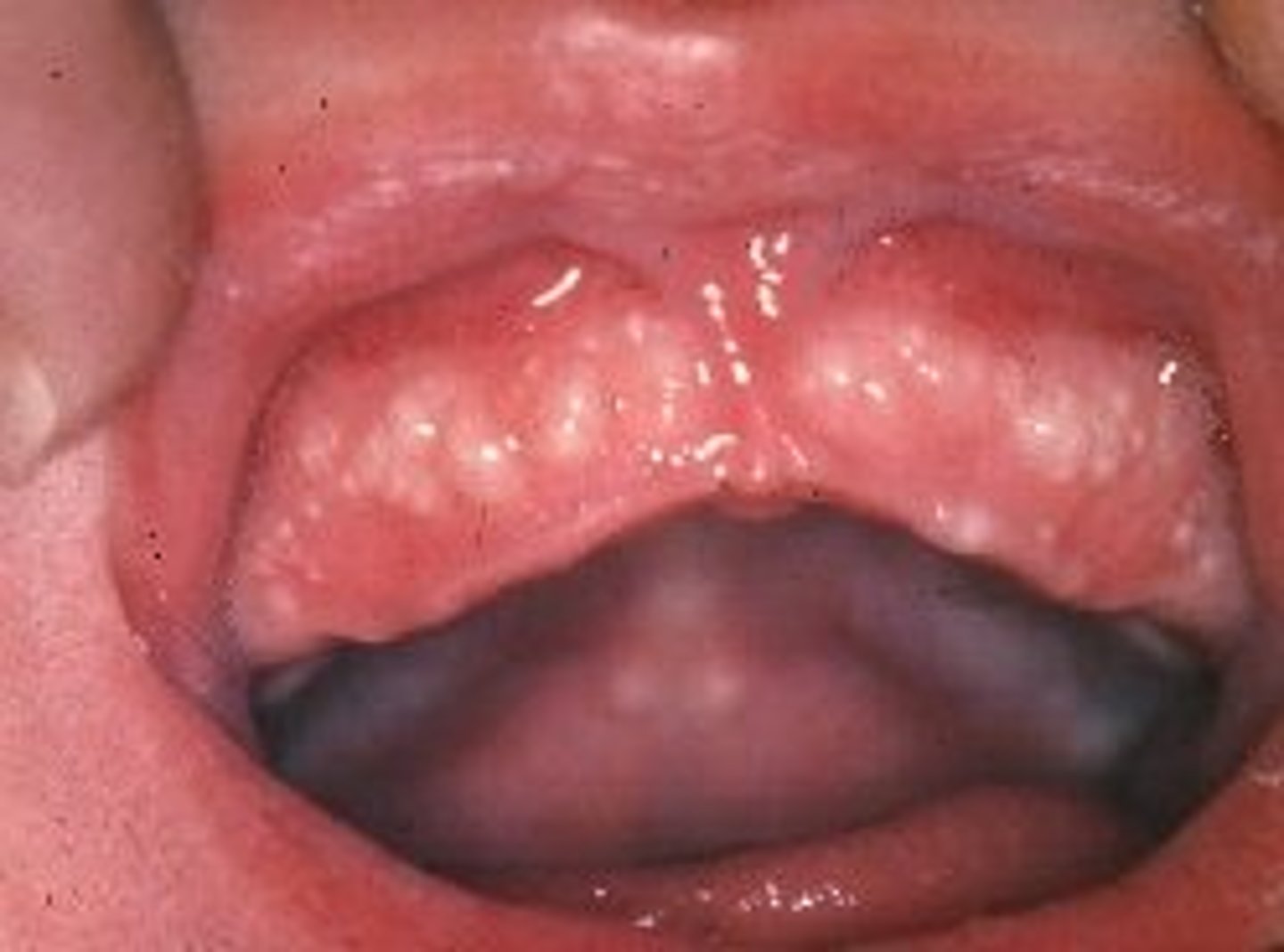
What are Epstein pearls?
Small white cysts found on the hard palate of newborns; disappears within a few weeks
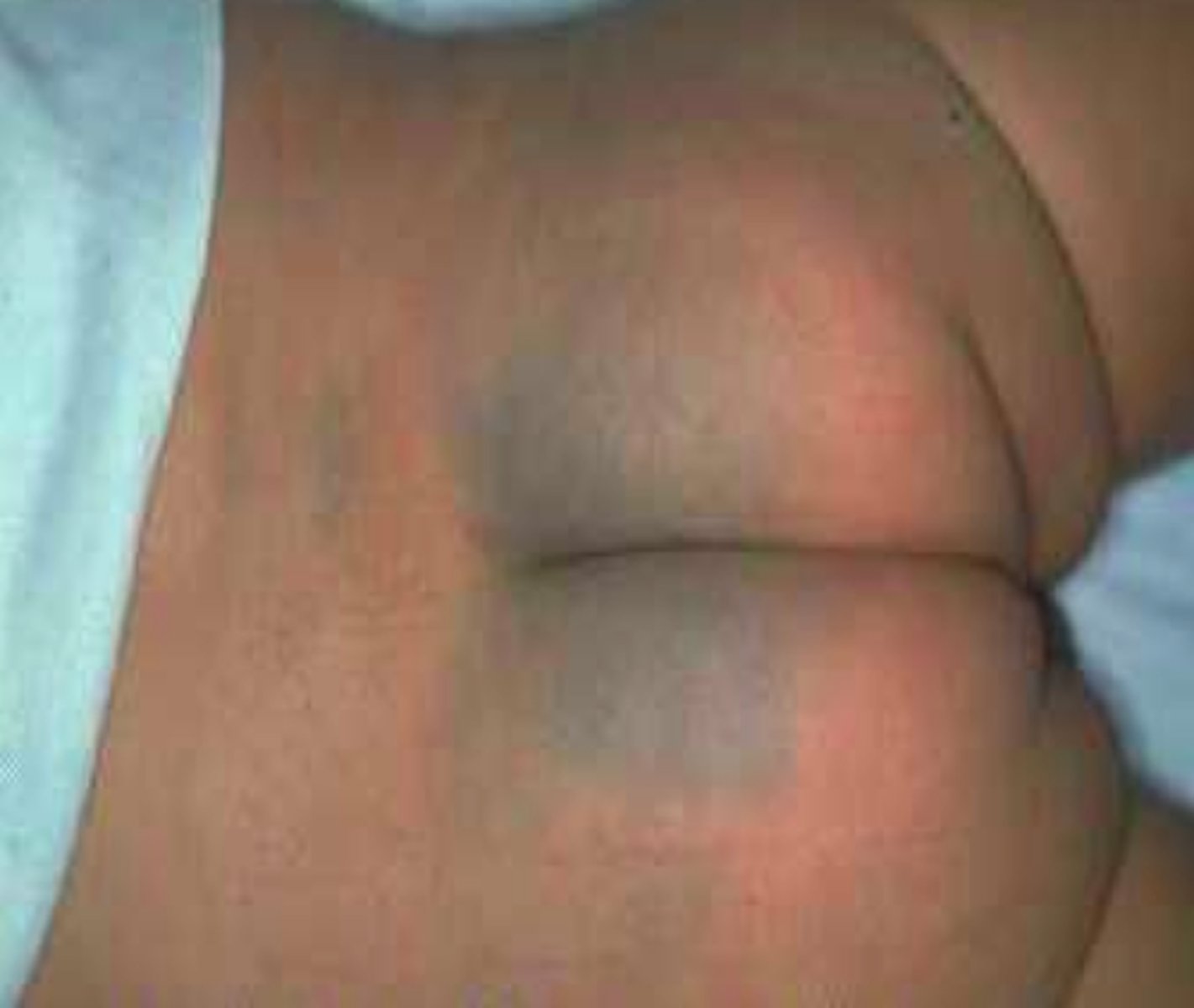
What are mongolian spots?
Benign discoloration of bluish gray on buttocks but usually fades
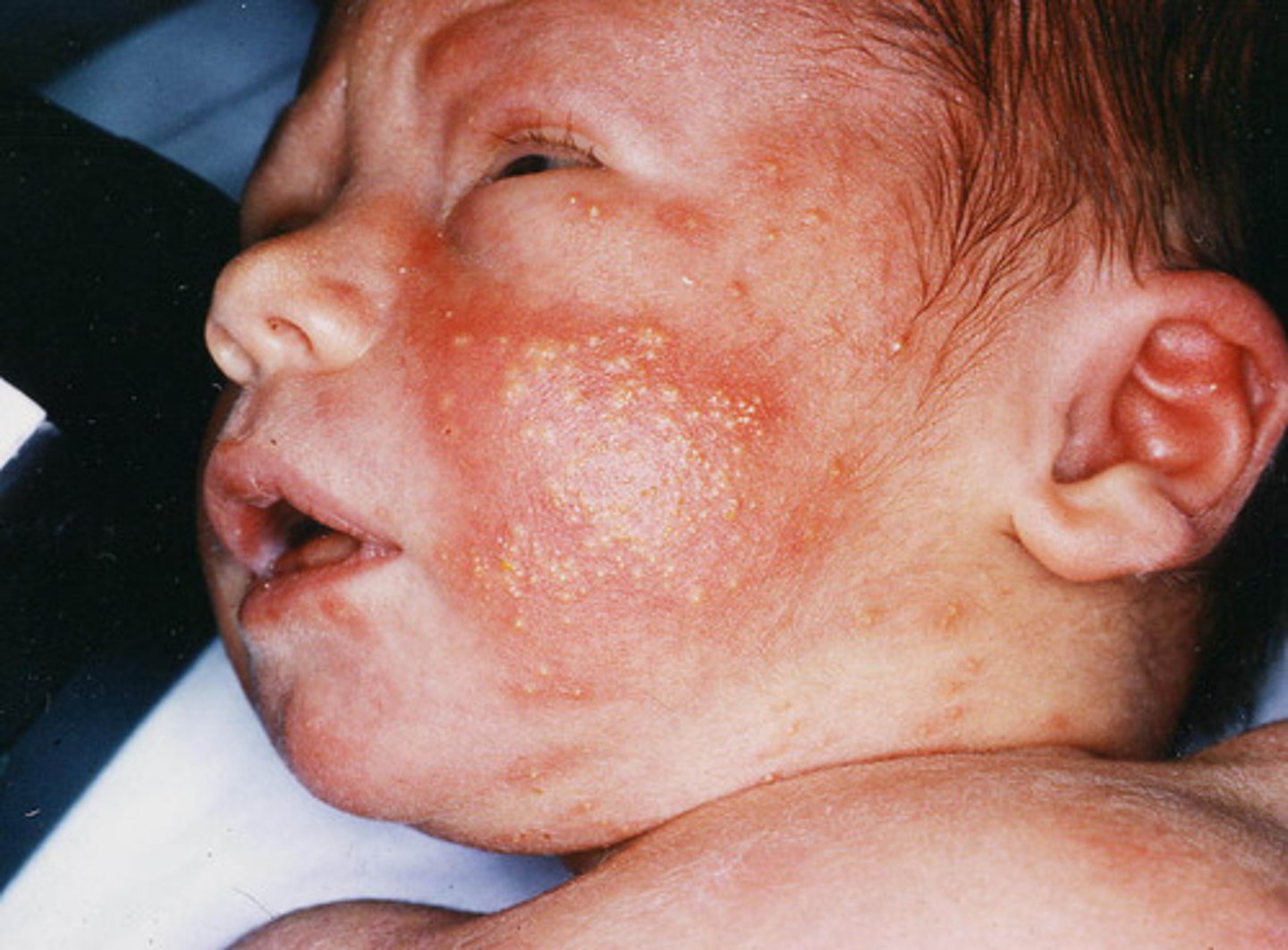
What is erythema toxicum neoratorum?
"Flee-bitten lesion" - Pink rash with firm,
yellow-white papules or pustule; usually appears 24 to 48 hours after birth and disappear in a few days
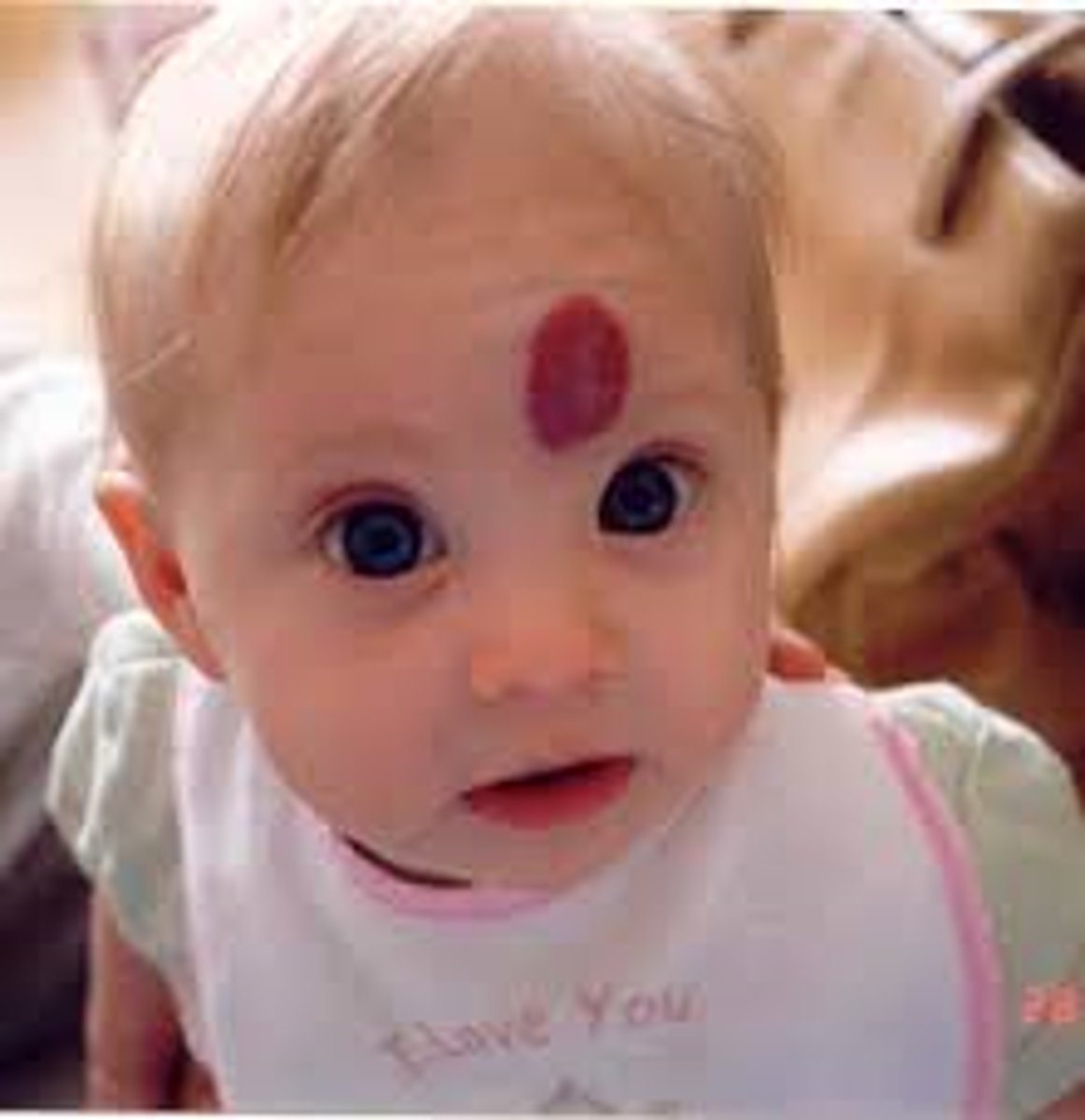
What is a hemangioma?
Abnormal accumulation of blood vessels in the skin; one of the most common birthmarks
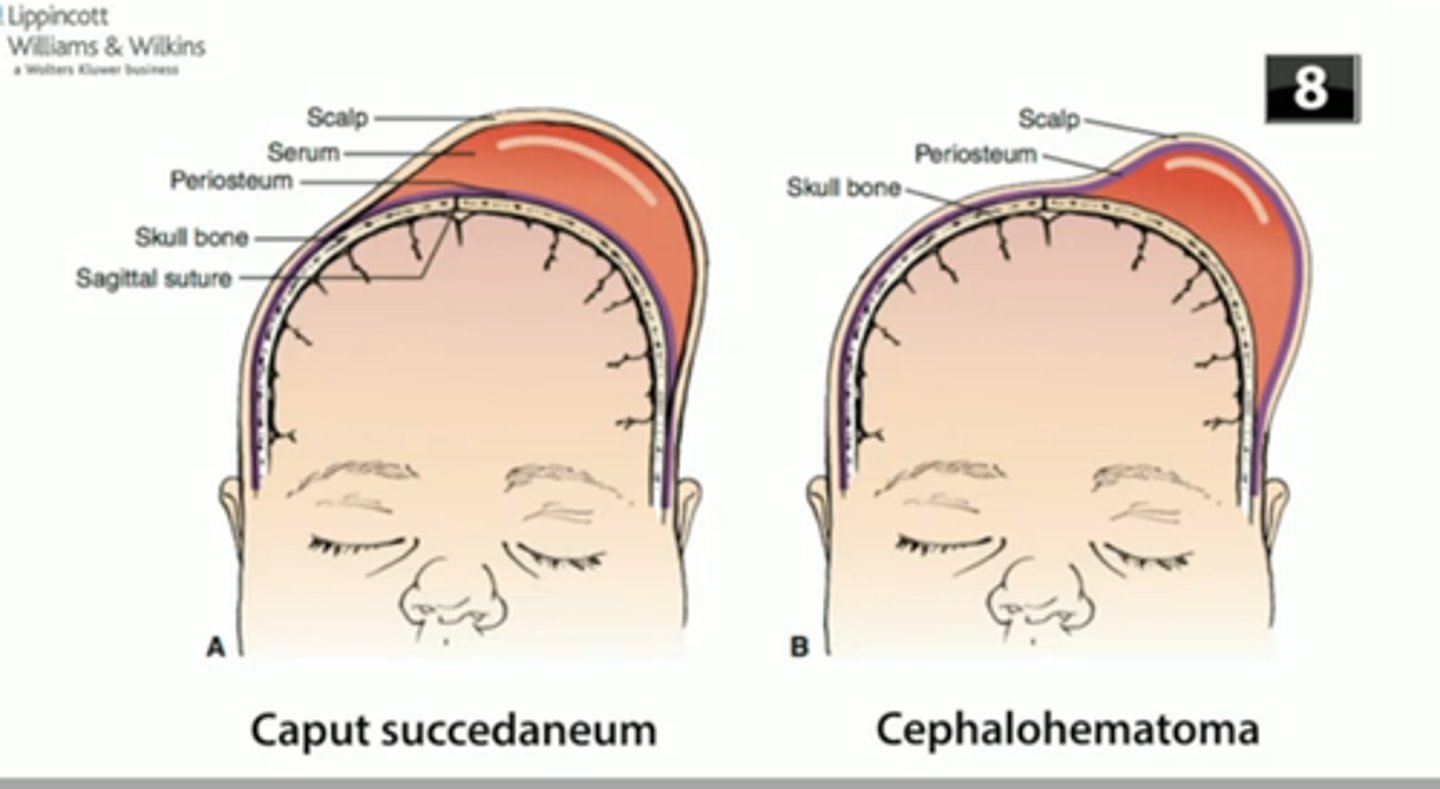
What is a cephalohematoma?
- Collection of blood between periosteum of skull bone and the bone itself; does not cross suture line
- Occurs on one or both sides of head; occasionally over the occipital bone
- Develops within first 24-48 hours after birth
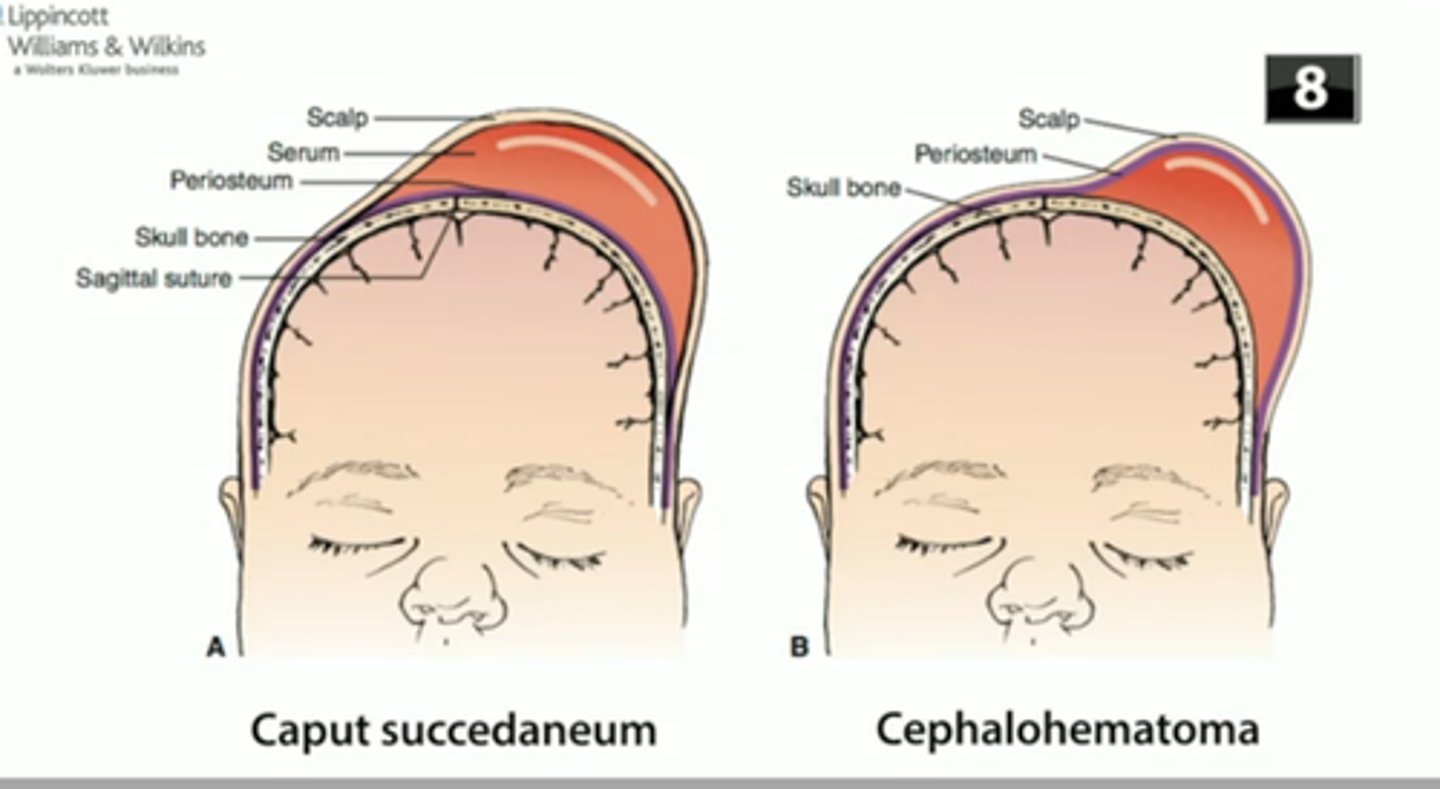
What is caput succedaneum?
- Edema under the scalp from mechanical trauma that crosses suture lines and is usually present at birth.
What do you see in newborns with hyperbilirubinemia?
Physiological jaundice appears after 24 hours of birth - normal, disappears in 1 week
Pathological jaundice appears in the first 24 hours after birth
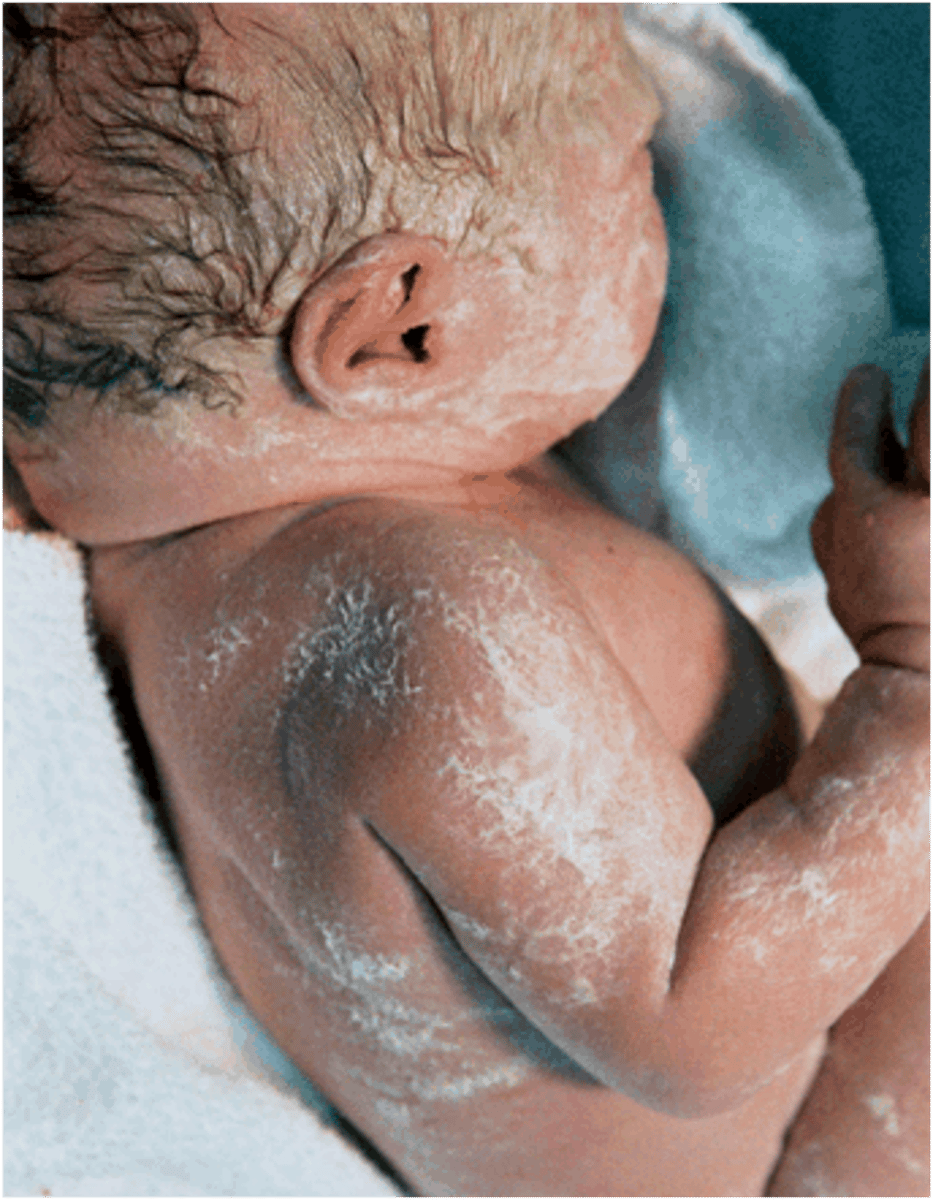
What is vernix caseosa?
A white thick cheesy material that protects the skin, made of epithelial cells and the secretions of glands.
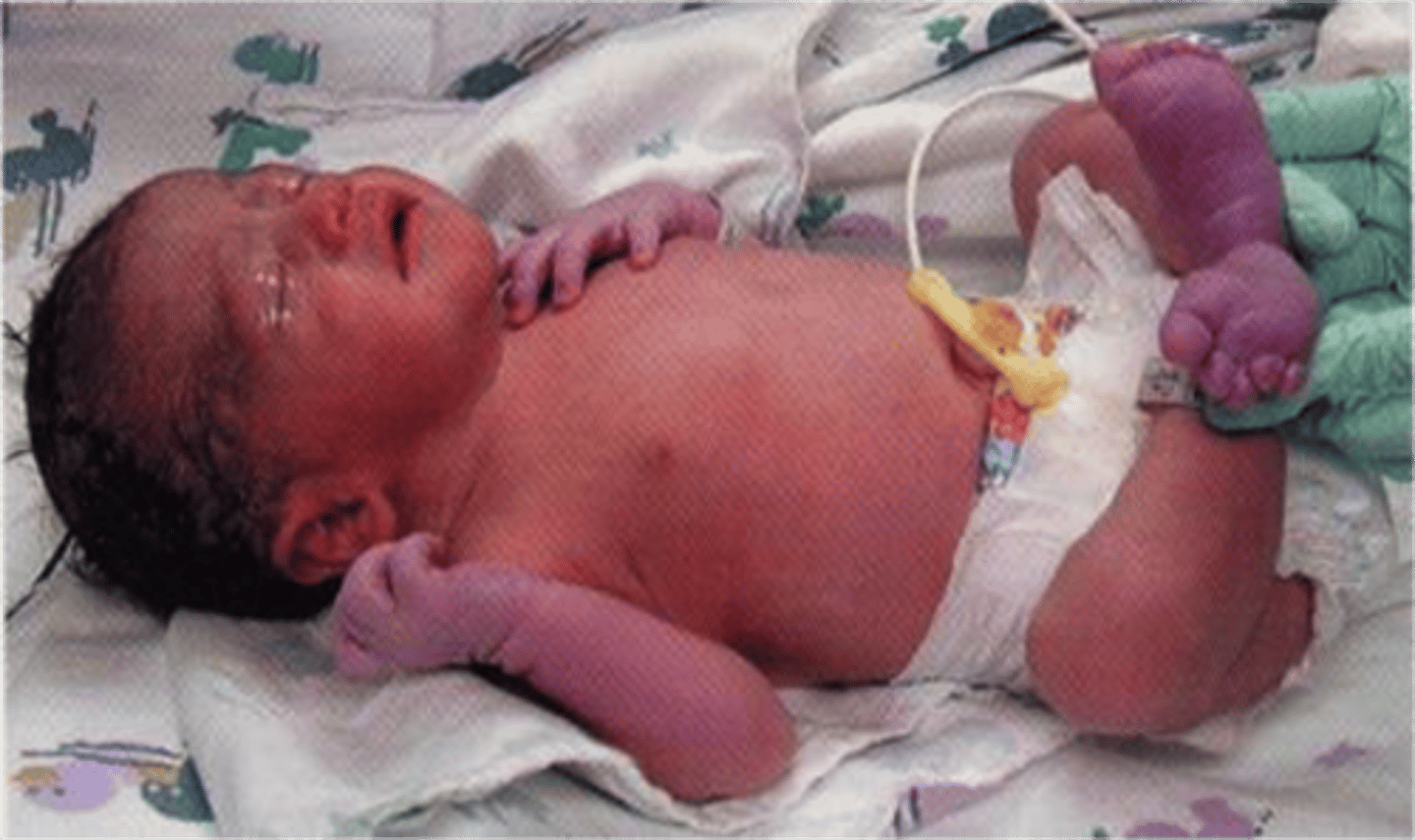
What is acrocyanosis?
Bluish discoloration of the hands and feet
What is telangiectatic nevi?
Flat, deep pink, localized areas usually seen in the back of the neck.
- AKA stork bites or salmon patch.
- They are birth marks; disappears by age 2
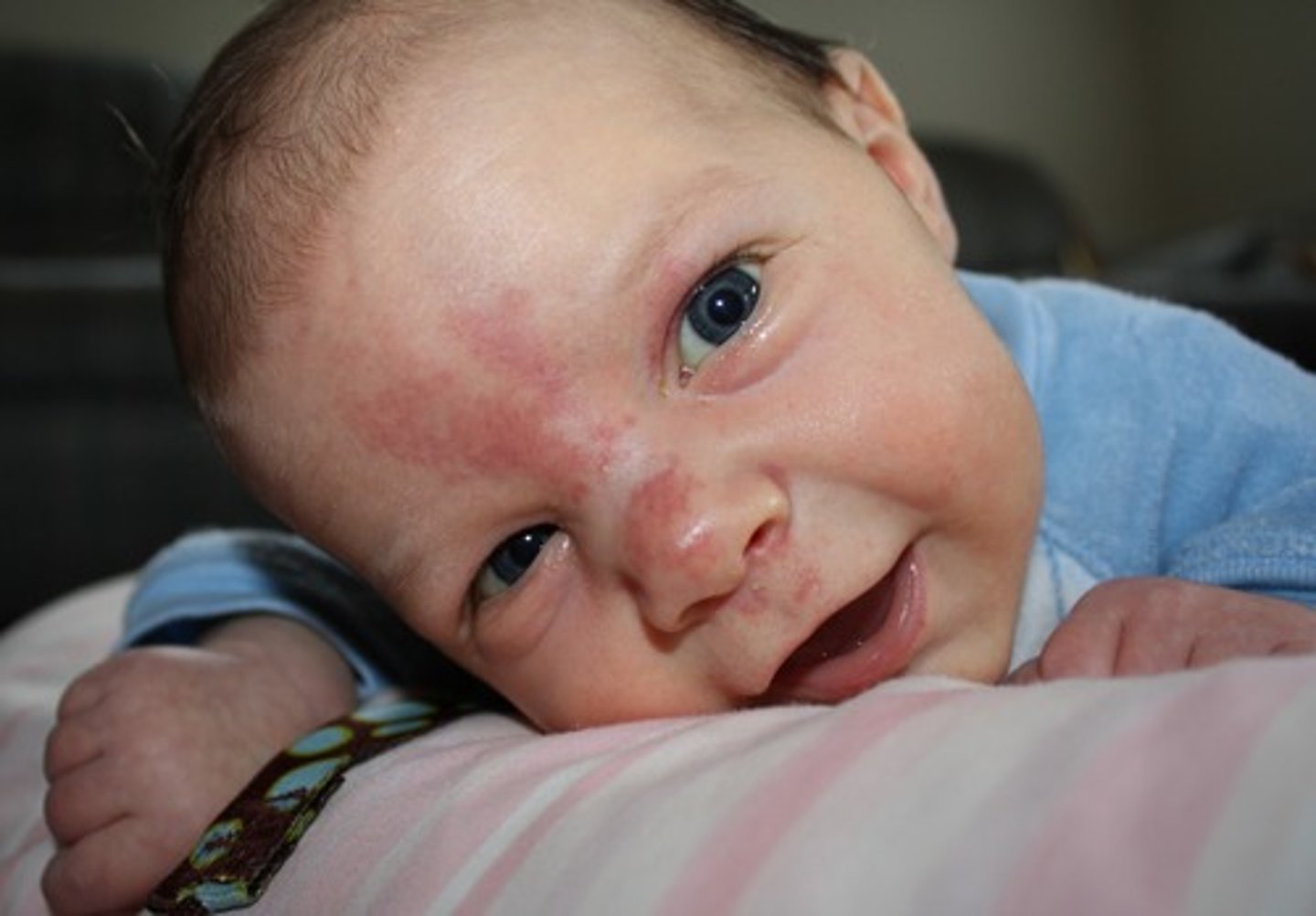
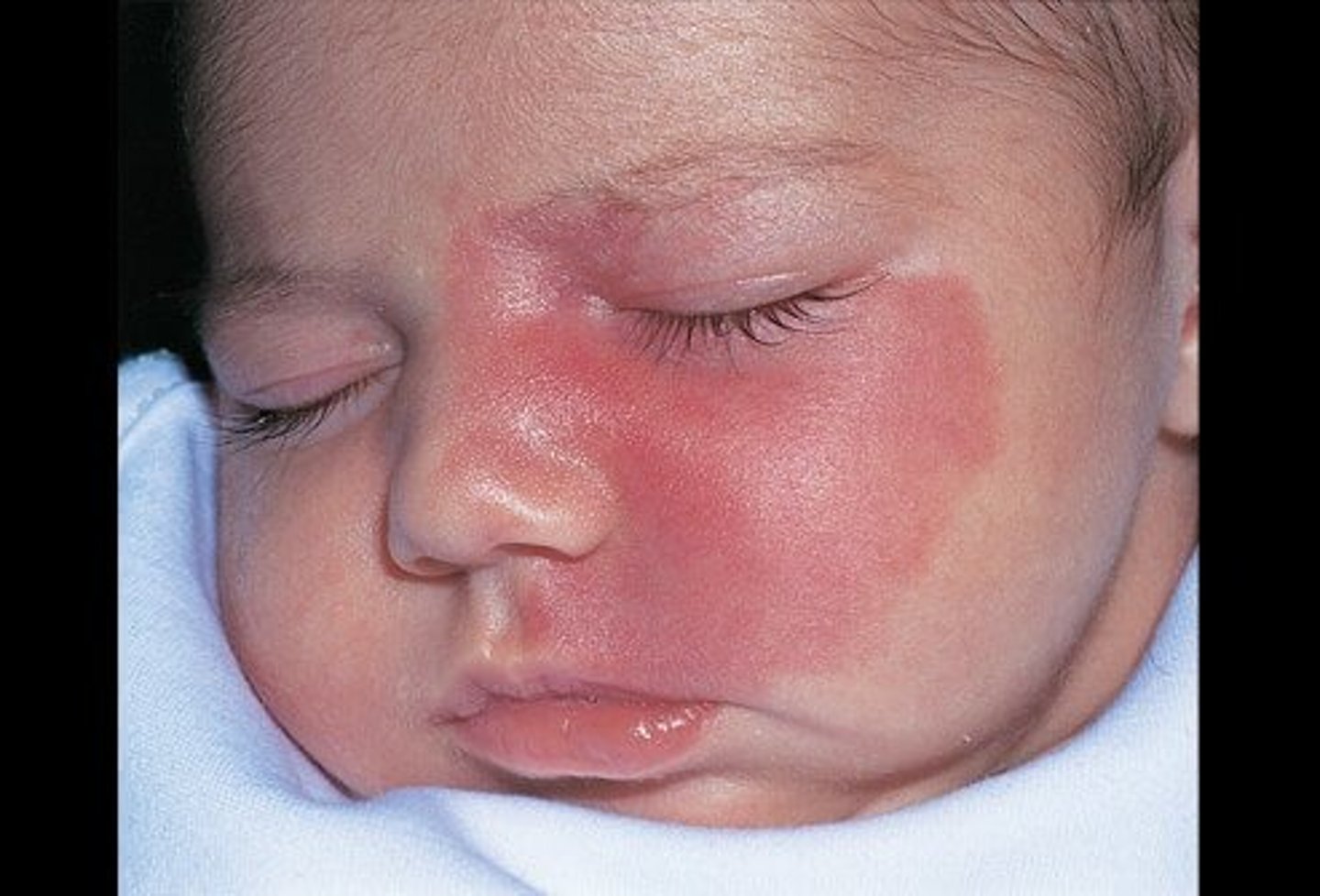
What is a port wine stain (nevus flammeus)?
Newly formed capillaries in the papillary layer of corium
What is a tocolytic agent?
- Stop contractions or relaxes the uterus
- Does not resolve shoulder dystocia
What are 2 tocolytic medications you should be aware of?
Terbutaline (Brethine)
Magnesium sulfate
What are the S/E of terbutaline?
Maternal tachycardia (Do not give with cardiac disease)
What are the S/E of magnesium sulfate?
Induces hypermagnesemia; everything goes opposite = down.
HR, BP, reflexes, RR, LOC all decreases.
What is the nursing intervention for hypermagnesemia due to mag sulfate treatment?
Monitor respirations
Assess for reflexes - Dec. dose if low, inc. dose if high
What are oxytocics?
Stimulates contractions and strengthens labor
What are the 2 oxytocic drugs?
Oxytocin (Pitocin)
Methylergometrine (Methergine)
What are the S/E of Pitocin?
Uterine hyperstimulation (longer than 90secs, closer than 2min) - LOWER dose!
What are the S/E of Methergine?
Causes HTN - Contracts blood vessels
What is Betamethasone used for?
Steroids given to mother (IM) that crosses over the placenta to the baby to help the surfactant in the babies lungs develop; increases glucose
What is surfactant (Survanta)?
- Helps the surfactant in the baby's lungs to develop
- Given to the baby via trans-tracheal route after birth
What is Humalin 70/30?
Mix of insulin N (70%) and R (30%)
Think of fraction; numerator on top is bigger number.
How do you draw up mixed insulin?
Draw up RN:
- Air into NPH
- Air into R
- Draw R
- Draw NPH
What needle is used for insulin injections?
IM: Pick answer in which both answers have "1" for IM (21-gauge; 1 inch).
SubQ: Pick answer that has "5" for "S" in SubQ (25-gauge, 0.5 inch).
What route is heparin given?
IV or SubQ
How long can you give heparin?
NO LONGER than 3 weeks (21 days)
* except for Lovenox (Enoxaparin) *
What is the antidote for heparin?
Protamine sulfate
What lab(s) do you check with heparin?
PTT
Can heparin be used during pregnancy?
Yes, Class C.
What route is coumadin given?
ONLY PO
How long can you give coumadin?
Takes a few days to a week to work (likely 4-5 days), can be on it for their entire life.
What is the antidote for coumadin?
Vitamin K
What lab(s) do you check with coumadin?
PT/INR
Can coumadin be used during pregnancy?
NO, Class X
What is the only antipsychotic drug that can be given during pregnancy?
Haldol
How can you tell the difference between K-wasting and K-sparing diuretic drugs?
Any diuretic drug ending in "x" wastes K PLUS Diuril.
If it does not end in "x," it is a sparer.
o Aldactone / Spinorolactone
o Adactazide / Spinorolacone-Hydrochlorothiazide
o Modurectic / Amiloride-Hydrochlorothiazide
o Lasix / Furosemide
o Bumex / Bumetanide
o Clotrix / Clotrimazole
o Esidrex / Hydrochlorothiazide
o Demadex / Torsemide
o Diuril / Chlorothiazide
What are the 2 muscle relaxants you need to know?
Baclofen (Lioresal)
Cyclobenzaprine (Flexeril)
What are the 2 main S/E of muscle relaxants?
Fatigue/drowsiness
Paresis (muscle weakness)
What are the 3 main things to teach to patients on a muscle relaxant?
Don't drink
Don't drive
Don't operate heavy machinery
"When you are on Baclofen...
you are on your back loafing." - MUSCLE RELAXANT
What are the stages of Piaget's Theory of Cognitive Development?
Sensorimotor: 0-2 years = Tell them what is happening while it's happening. Think present tense.
Pre-operational: 3-6 years = Fantasy-oriented, imaginative, illogical, cannot reason with them.
Concrete operational: 7-11 years = Rule-oriented, live and die by the rules. There is one way to do something... everything else is wrong.
Formal operational: 12+ years = Abstract thinking. They know cause and effect.
A 19-month-old infant is about to have a lumbar puncture (LP) for csf analysis and culture. How would the nurse teach the child?
Tell them what IS BEING done while it is being done. They don't understand play.
Pre-op teaching is ONLY for PARENT/GUARDIAN.
A 3-year-old child is schedule for a lumbar puncture (LP) for csf analysis and culture. What is the nurse's best action to teach the child about the procedure?
Tell them what WILL be done shorty before it happens. They learn by playing.
Answers with "the morning of..." "the day of..." "2 hours before..." etc.
An 8-year-old child is schedule for a lumbar puncture (LP) for csf analysis and culture. What is the nurse's best action to teach the child about the procedure?
Teach them a day or two ahead of time what you're going to do and how to do it. Use age-appropriate reading and demonstration (skill).
When is the first age a child can manage his care?
12 years old
Which of the following 4 children will be able to manage his own care?
a. A 7-year-old with Cystic Fibrosis
b. An 8-year-old with Diabetes Mellitus
c. A 10-year-old with a scraped knee
d. A 13-year-old with Chronic Renal Failure
D. A 13-year-old with Chronic Renal Failure
Manage = 13 year old; Skill = 8 year old.
12+ years old is taught like an adult.
What are the phases of a nurse-client relationship?
Pre-interaction phase: Professional goals
Orientation phase: Purpose, nature, time, trust
Working phase: Active problem-solving
Termination phase: Achieved goals, end relationship
What are the seven principles to obey in psych?
1) KNOW what phase of nurse-patient relationship you're in
2) Do NOT give/receive gifts
3) Do NOT give advice
4) Never give guarantees - "You'll feel better if..."
5) Immediacy - If you are between 2 answer choices, pick the one that keeps them talking.
6) Concreteness - Never use slang or figurative speech.
7) Empathy - Don't say "I know how you feel..."
What are the 4 steps to answering empathy questions?
- Empathy questions will always have a quote
- Roleplay the feelings (Put yourself in their place) and say the words as you really meant them
- Ask yourself if I said these words, how would I be feeling right now?
- Choose the answer that reflects the pt's FEELINGS and ignore what the pt said