Intro to Pharmacokinetics and Application 29/01
1/51
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
52 Terms
What is a regimens?
To achieve therapeutic conditions
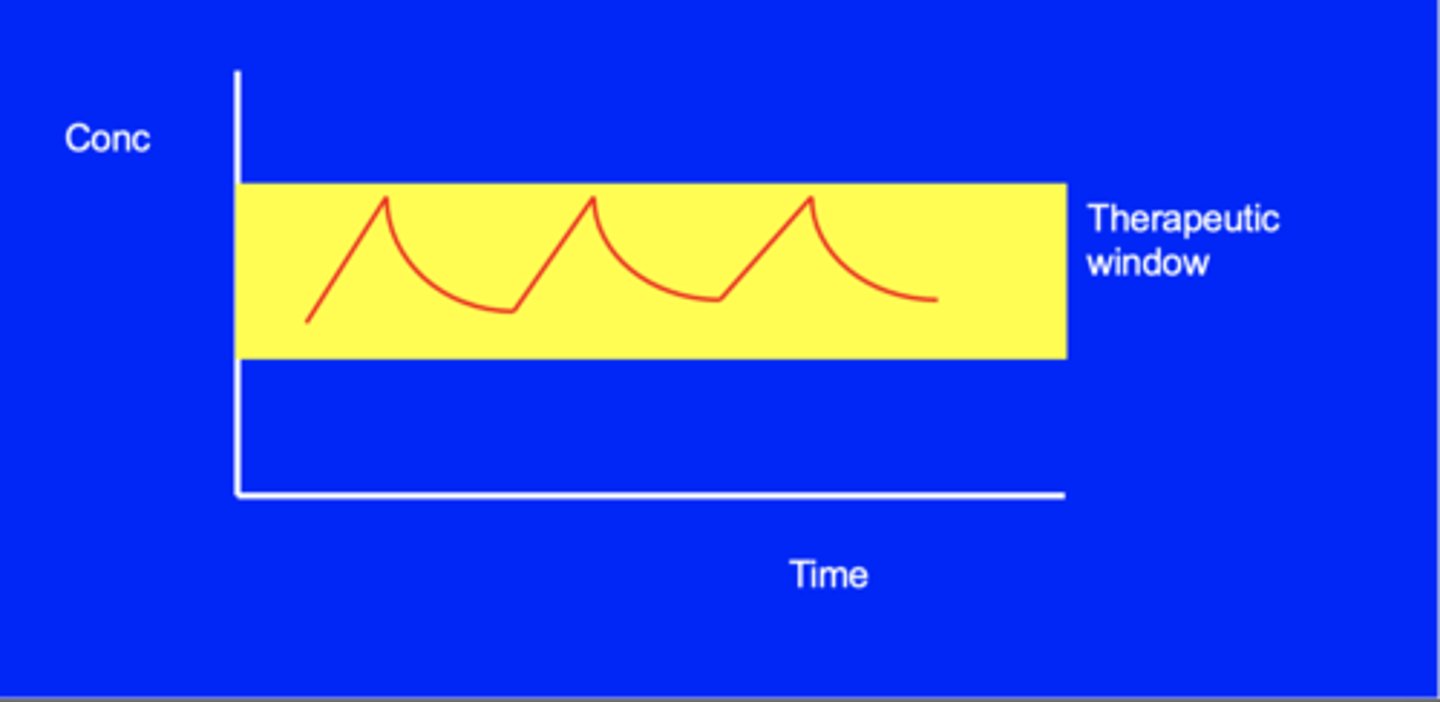
What is the aim of a regimen?
To keep the plasma conc in the therapeutic window. This gives the exponential decay, and then the next dose is timed so you can stay within the window. If you go above the window, you increase the chances of toxicity.
What is volume of distribution?
Apparent volume in which a drug is dissolved in the body.
Amount in body/Conc = Dose/Conc at t=0

What is clearance (CL)?
Volume of plasma cleared of a drug in unit time - i.e. indication of the amount of drug removed from the body in a unit time
What is clearance measured in?
Measured in ml/min or L/h.
How do you calculate total clearance?
Clearance = Renal clearance + hepatic clearance. This varies from drug to drug
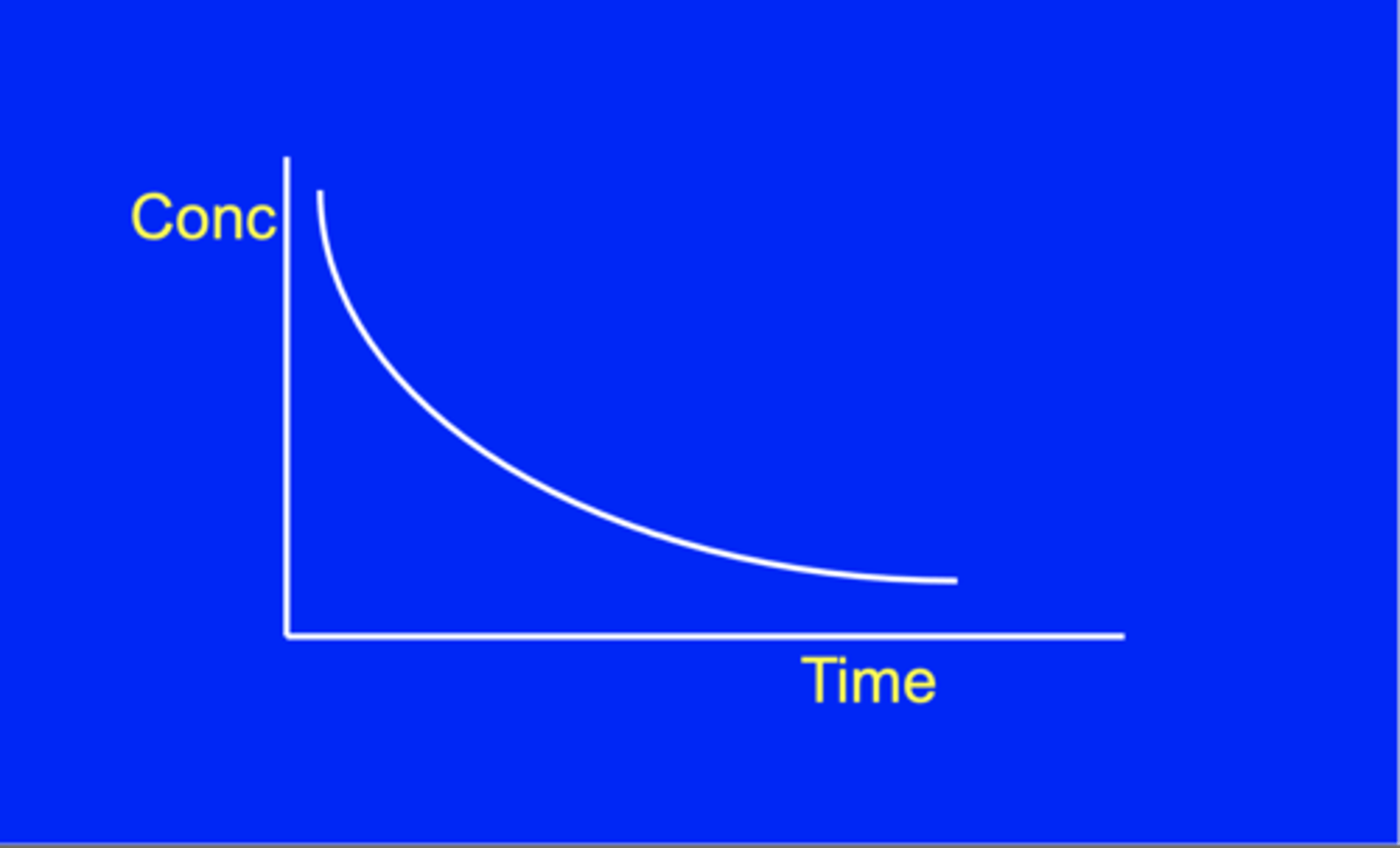
What is exponential decay?
The amount of the drug decreases at a rate proportional to the amount left
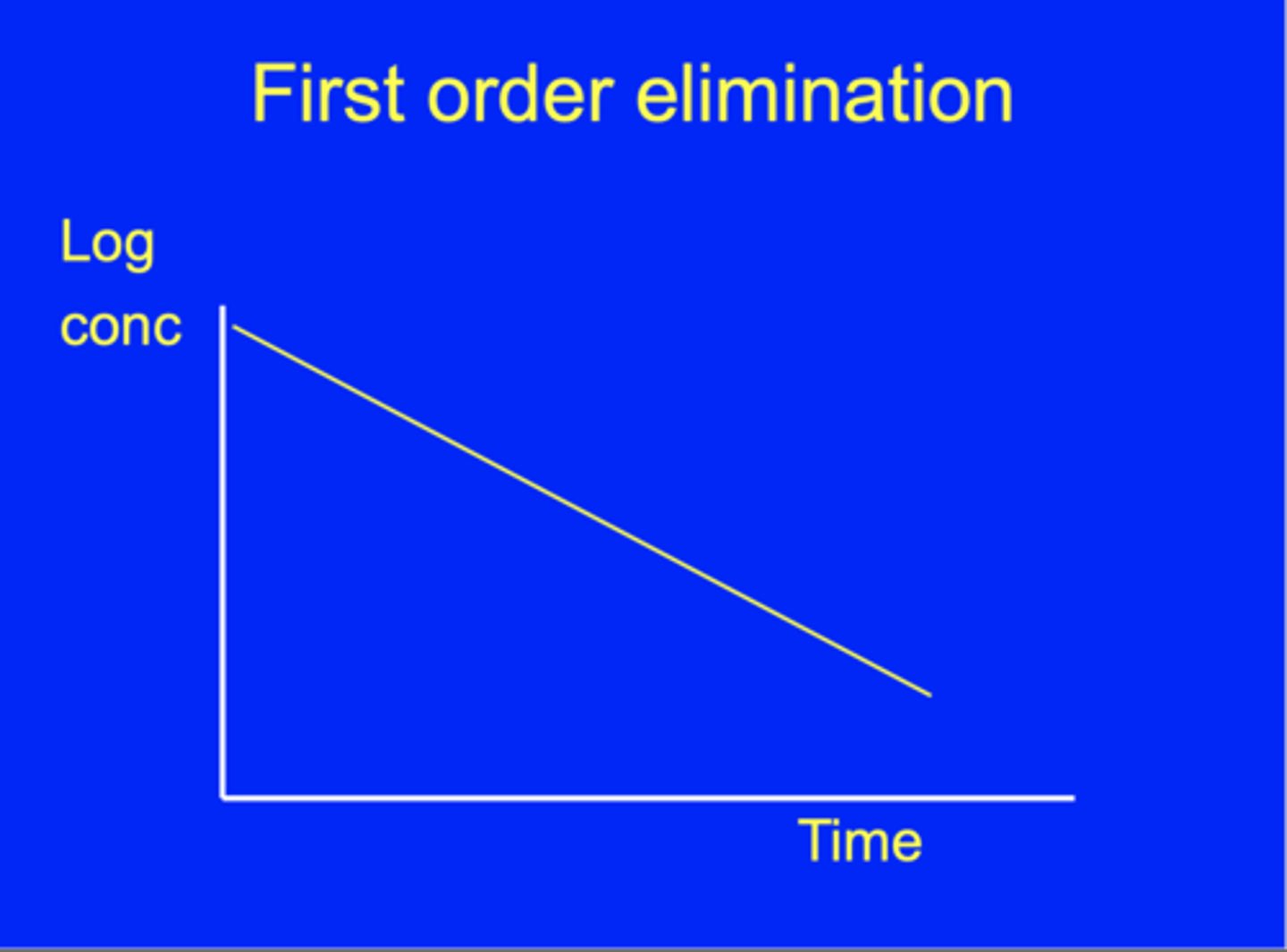
What is first-order elimination?
Rate of elimination is proportional to conc of drug
How do you calculate rate of elimination?

How do you calculate rate constant?
k = Clearance/Vd, or CL = k x Vd.
This is the fraction eliminated per unit time.
What is t-1/2?
Time for conc to decrease by 50%.
t1/2 = 0.693(ln2)/k

What is IV infusion? (type or process, when given)
1. Administration of a drug at a constant rate - zero-order process.
Infused directly into a vein. This is the type of therapy you start with in an emergency.
2. Aim for steady state.
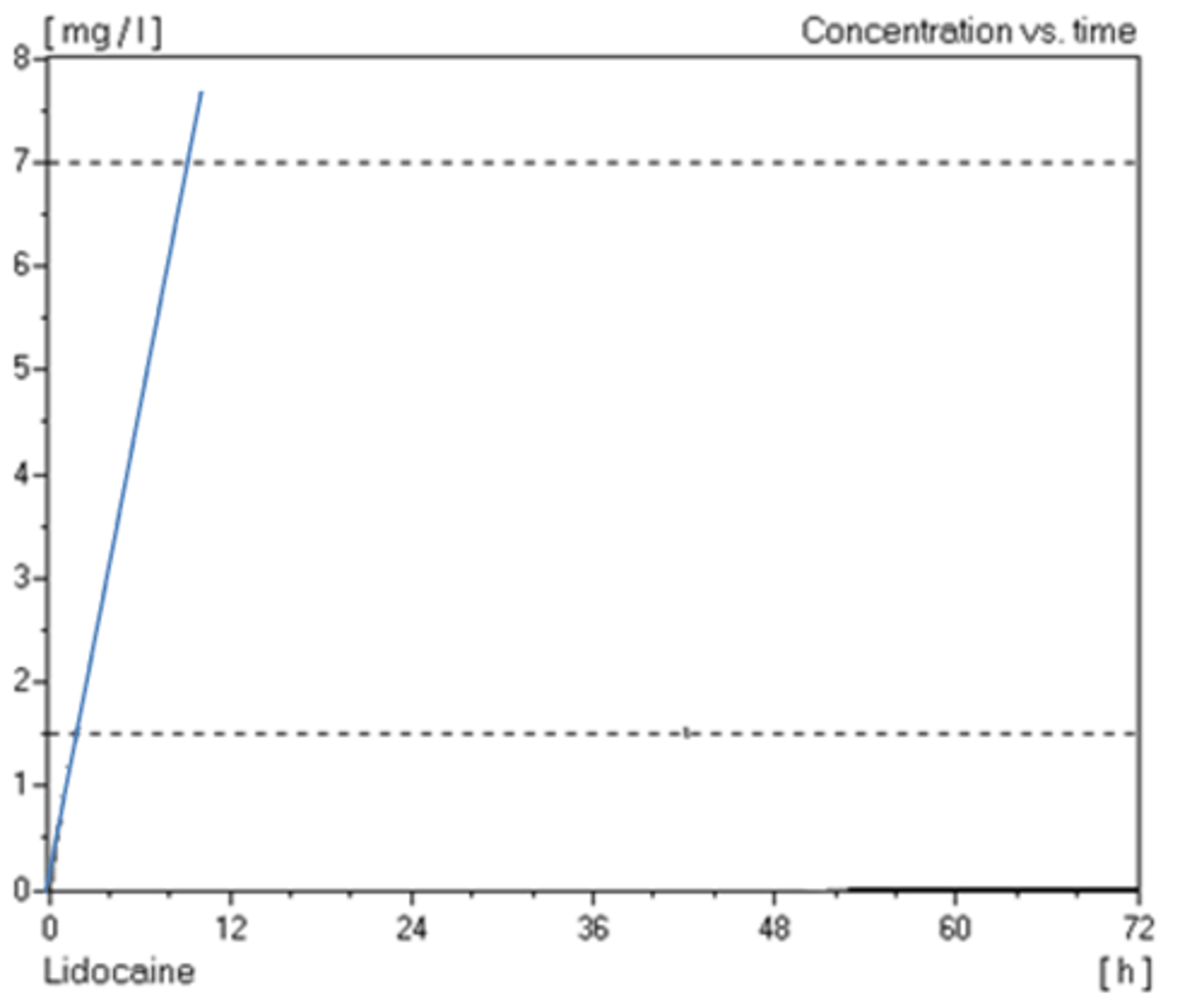
What is the steady state?
For most drugs, elimination shows first order kinetics. this means the body can keep pace with plasma conc.
1. You get a rising phase.
2. Then you get an eqbm - the rate at which drug goes into body = rate at which it is removed. This is the steady state conc (Css). This is what you are aiming for with IV infusion.
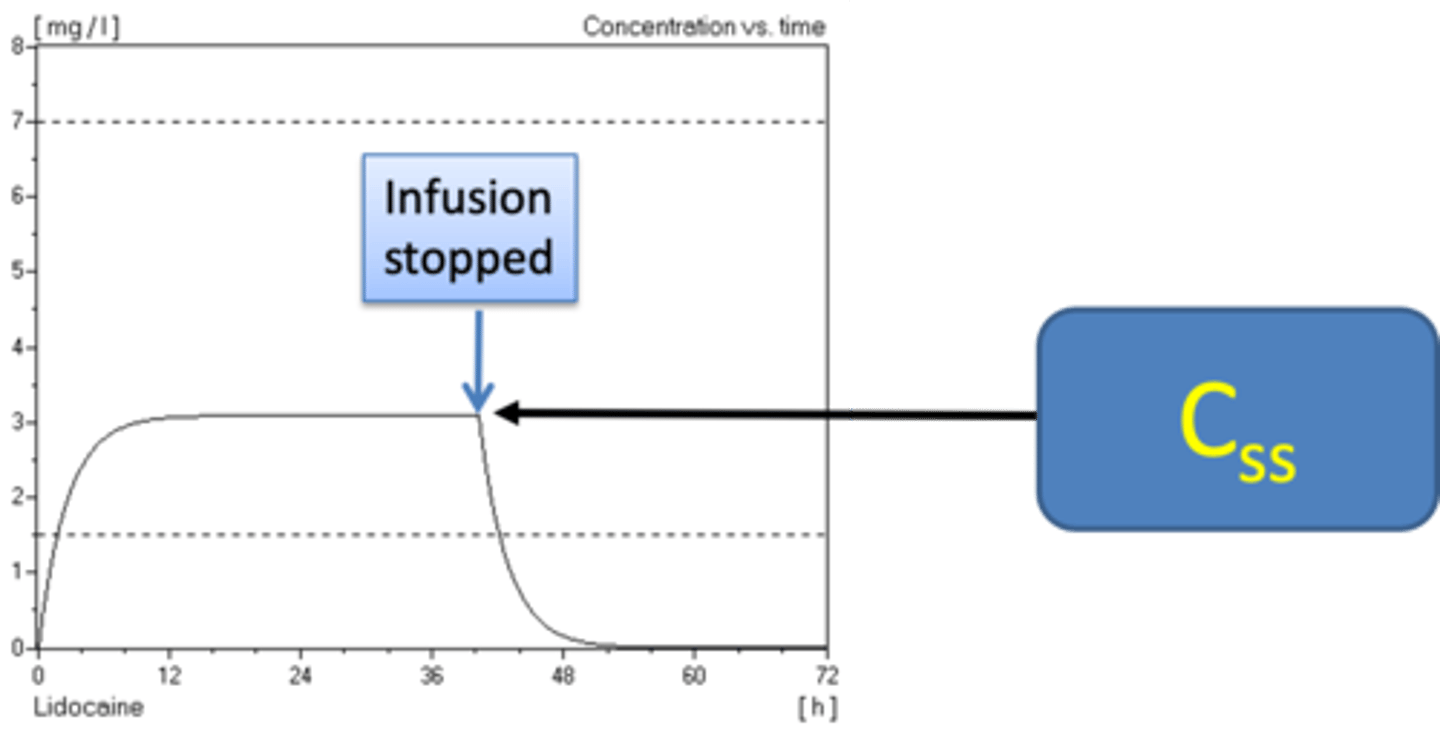
What is zero order process?
A constant amount of a drug is eliminated per unit time. The rate at which a drug is eliminated from the body remains constant regardless of its conc in the bloodstream.
Elimination is a first order process
What is the maintenance dose?
Once you achieve Css, this means the maintenance dose = amount removed. Whatever you put in is being removed.
How do you work out infusion rate?
Infusion rate = Clearance x Css.
Units: dose/time.
What is aminophyline? When is it used?
It's only 80% of the active drug theophylline
It's a bronchodilator
How is aminophylline administered and when?
In severe asthma attacks, given by IV.
Example of aminophylline infusion rate being calculated from theophylline.

What is single oral dosing?
In oral dosing, you can be prescribed drugs orally in different ways - fast oral, oral and slow oral which have effects on how quickly they are absorbed
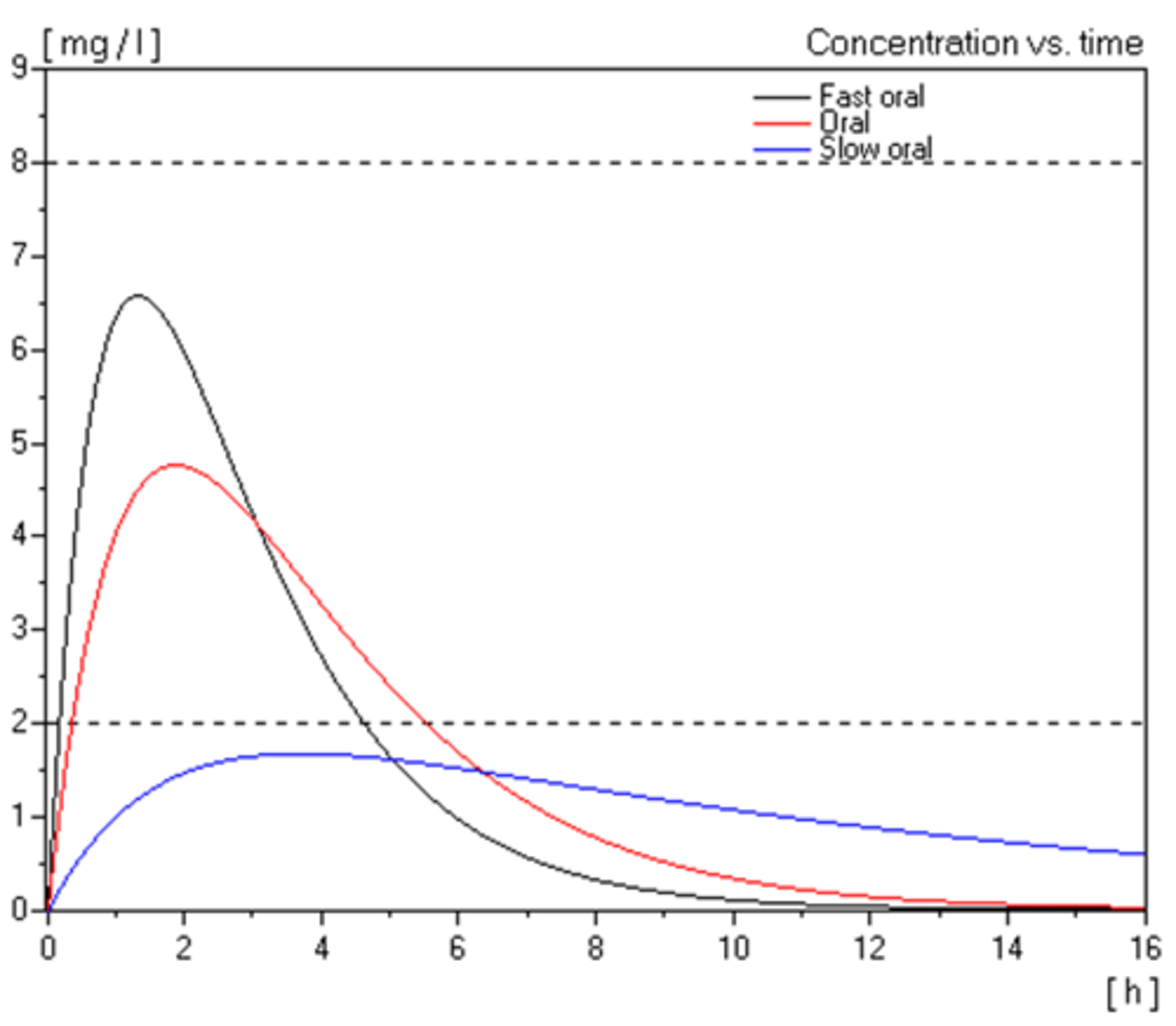
What is the shape of the overall plasma level/time curve influenced by with single oral dosing?
1. Rate of dissolution (if tablet).
2. Rate of absorption.
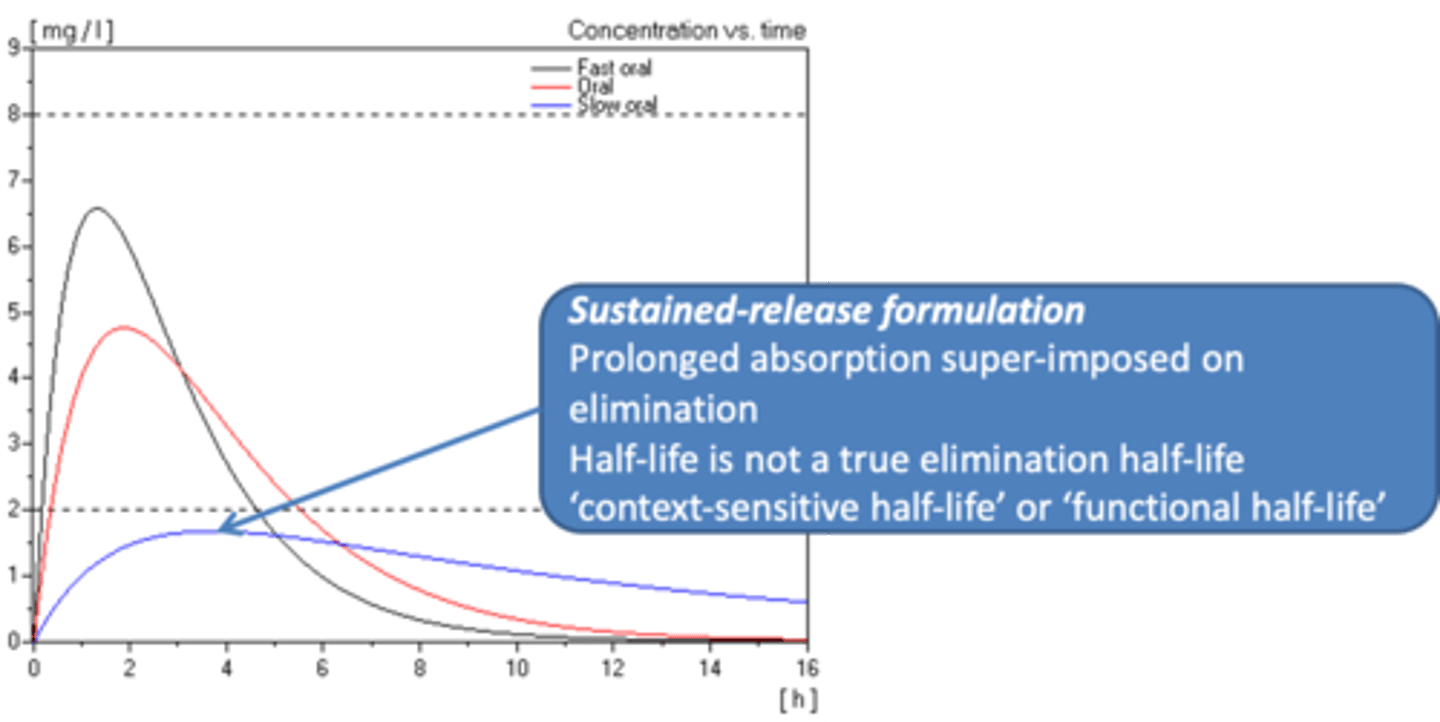
What is rapid-release formulation?
1. The rise to peak is absorption of drug and elimination.
2. After the peak, it is only elimination.
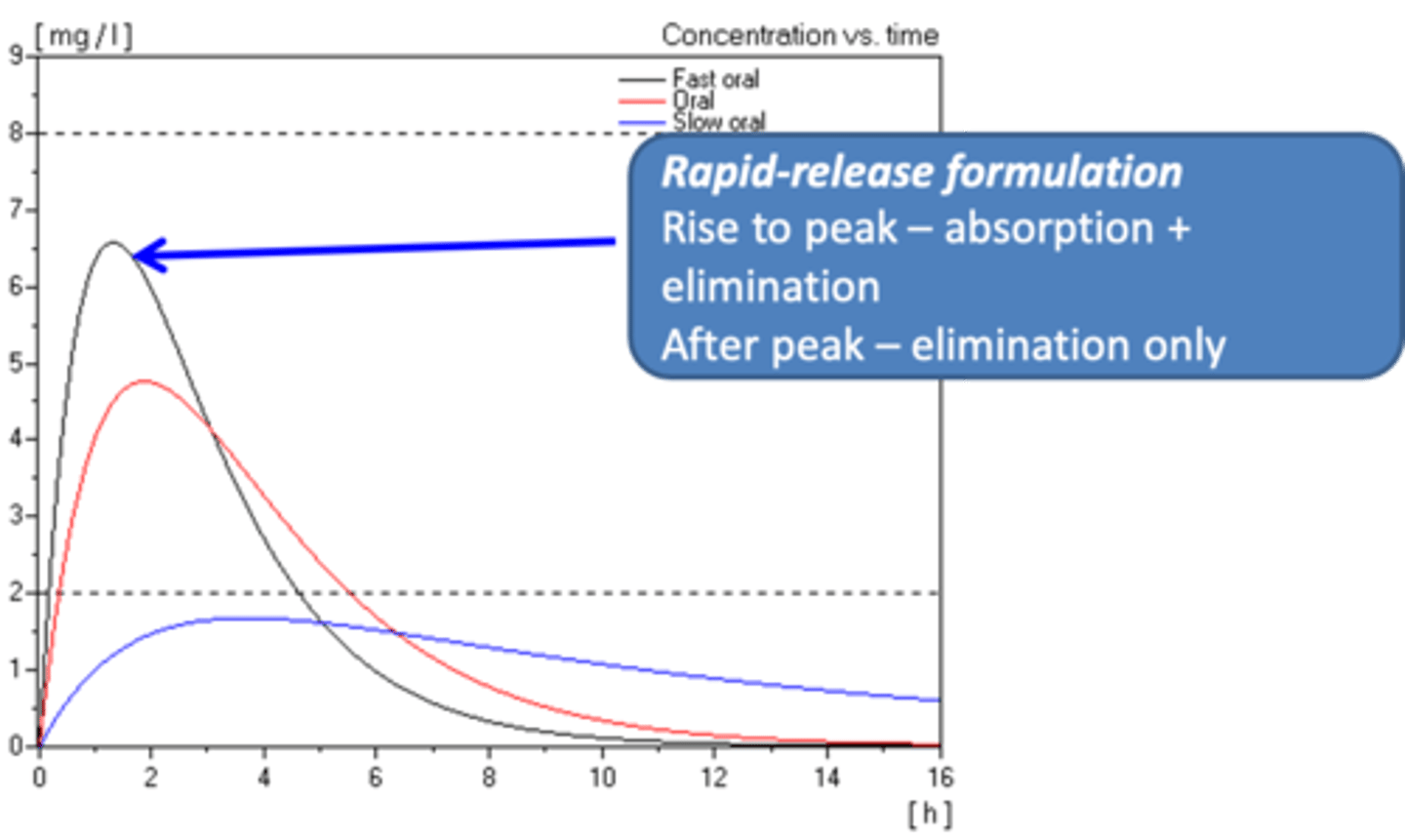
What is sustained-release formulation?
Slow oral.
1. Prolonged absorption is superimposed on elimination.
2. Bottleneck-shape formation.
3. Rate of absorption is slow that the half-life becomes prolonged.
What three things are useful pharmacokinetic data?
1. Absorption rate constant.
2. Time to peak.
3. Bioavailability.
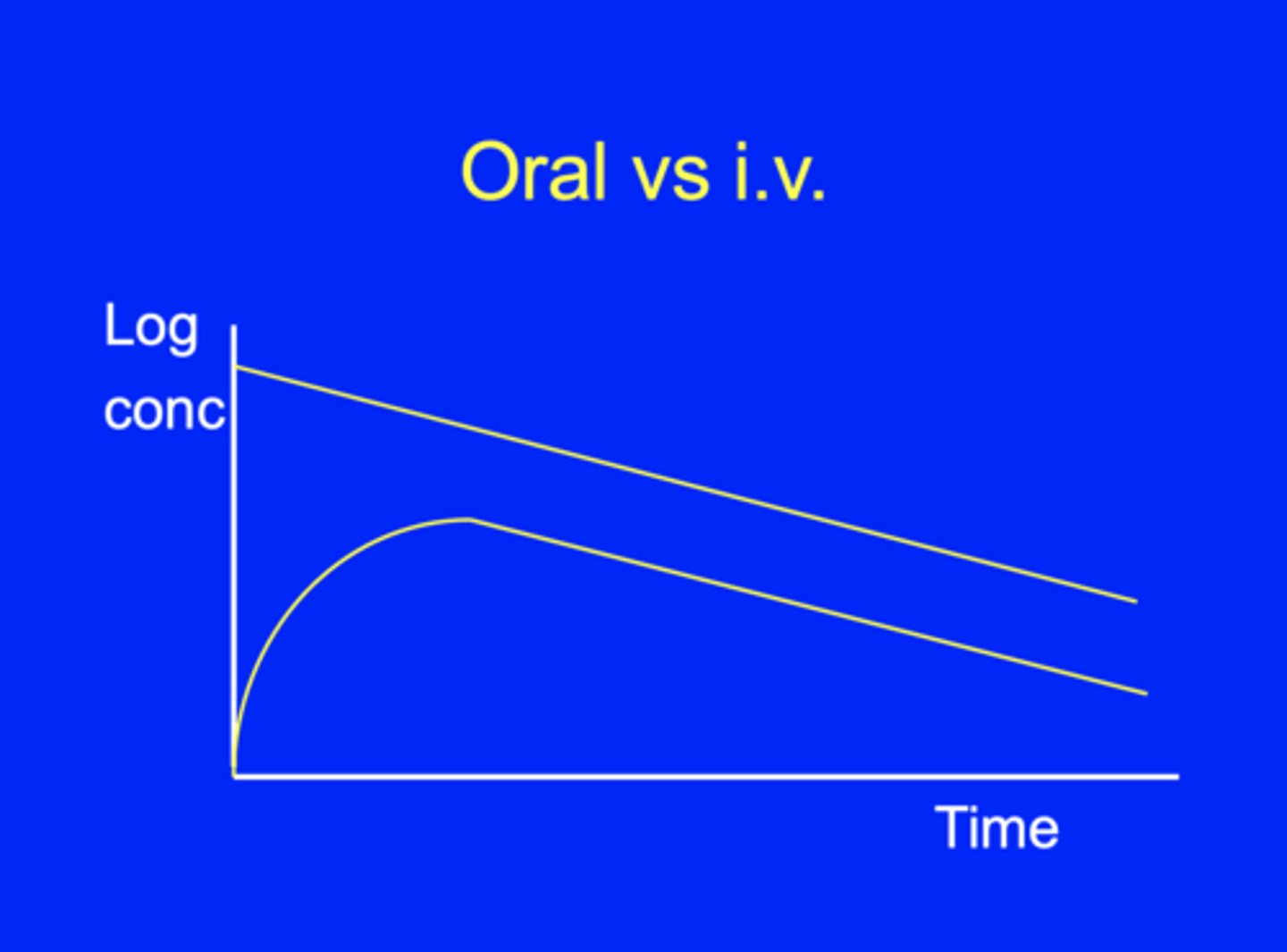
What is bioavailability?
F, fraction absorbed.
F = AUC oral/AUC iv.
(AUC = area under curve).
The same drugs can have different bioavailabilities.
How do you calculate dose given from bioavailability, F?
Dose given = amount needed/F.
What is repeated oral dosing? (3)
1. Applies to most regimens, eg. for maintaining someone's BP, ideally once daily. If given sufficiently far apart in time, each dose behaves independently.
2. The intention is to produce a steady state.
3. You are mimicking IV infusion intermittently.
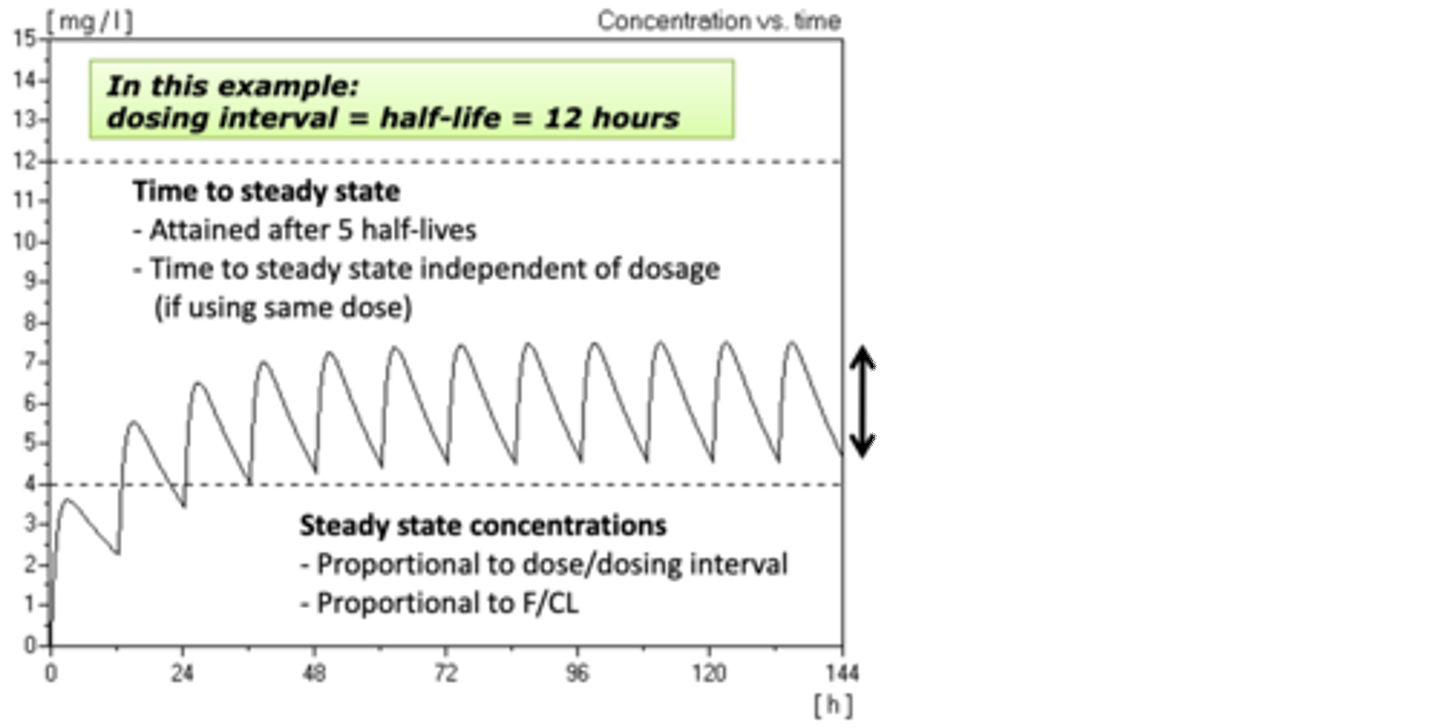
How many half-lives does it take to achieve a steady state?
Approximately 5 half-lives.
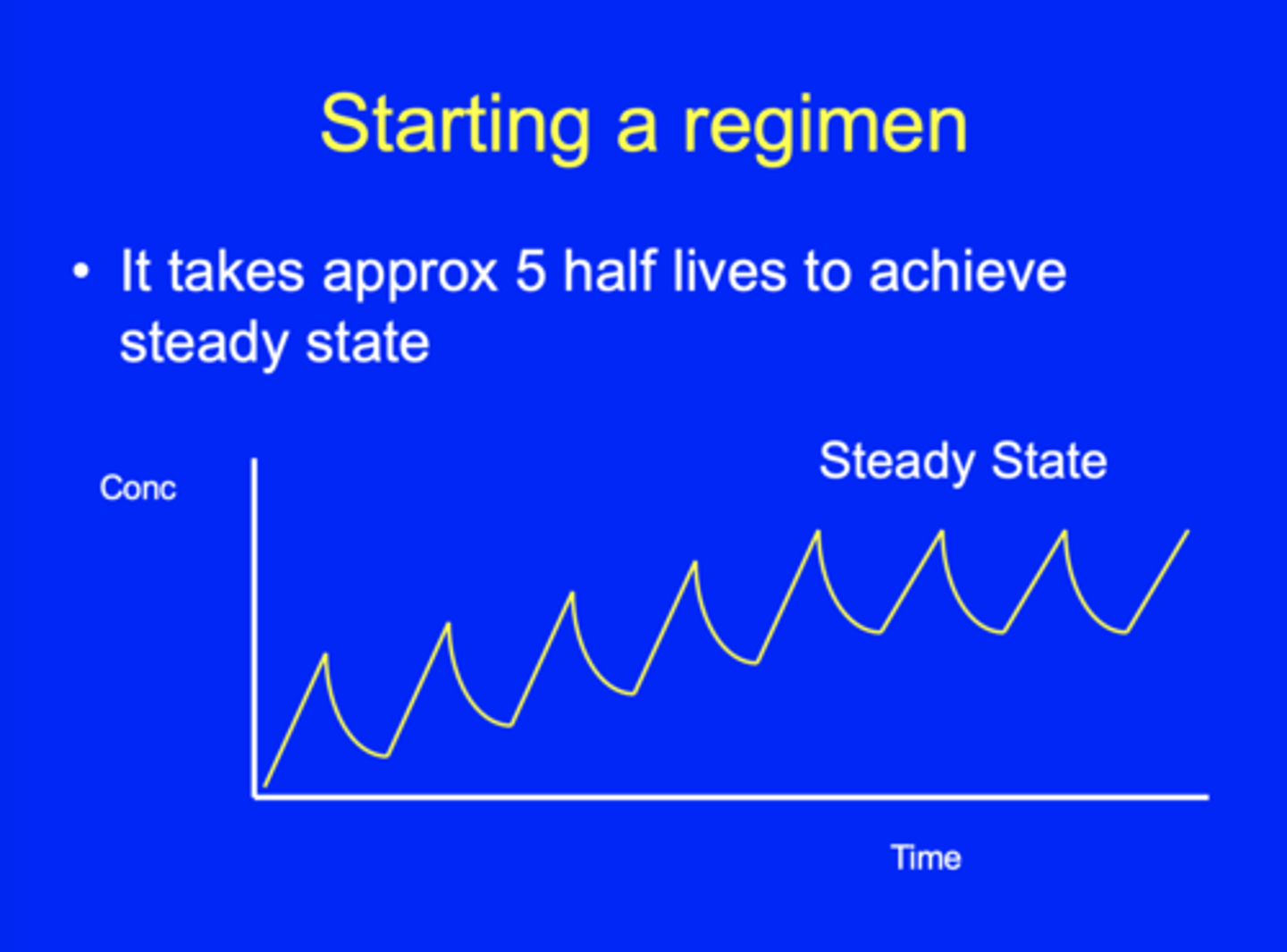
What is the evidence behind why it takes 5 half-lives to achieve a steady state?

What is the formula for an oral regimen dose?
Dose = CL x Css x tau/F.
- tau is the dosage interval.
i.e. if you double the dose, double the conc, due to 1st order kinetics.

How do you prescribe a drug that has a large therapeutic window?
Maximal dose strategy
Less doses are given throughout the day since there are large fluctuations from a large therapeutic window
(E.g. amoxicillin type drugs like penicillin have a large TW)
How do you prescribe a drug that has a narrow therapeutic window?
Better to do an IV in order to control the plasma conc.
(More challenging as they have short half-lives and has to be controlled more)
What is a loading dose?
An initial higher dose of a medication given at the beginning of treatment to rapidly achieve the desired therapeutic conc in the bloodstream or tissues
What is maintenance dose?
A regular ongoing dose of a medication administered after an initial loading dose or as part of a continuous treatment regimen
Difference between maintenance dose and loading dose
Maintenance dose usually lower than loading dose and is intended to maintain the drug conc within the therapeutic range over time
How do you calculate loading dose and thus maintenance dose for urgent medication?
Loading dose = Target Css x Vd/F.
This is for urgent meds.
Maintenance dose = Target Css x CL x tau/F.
Why is a loading dose given at the start and what is used to maintain the dosage after?
A loading dose is given at the start to achieve a rapid rise to achieve the target Css, and then maintenance doses are given to maintain the steady state.
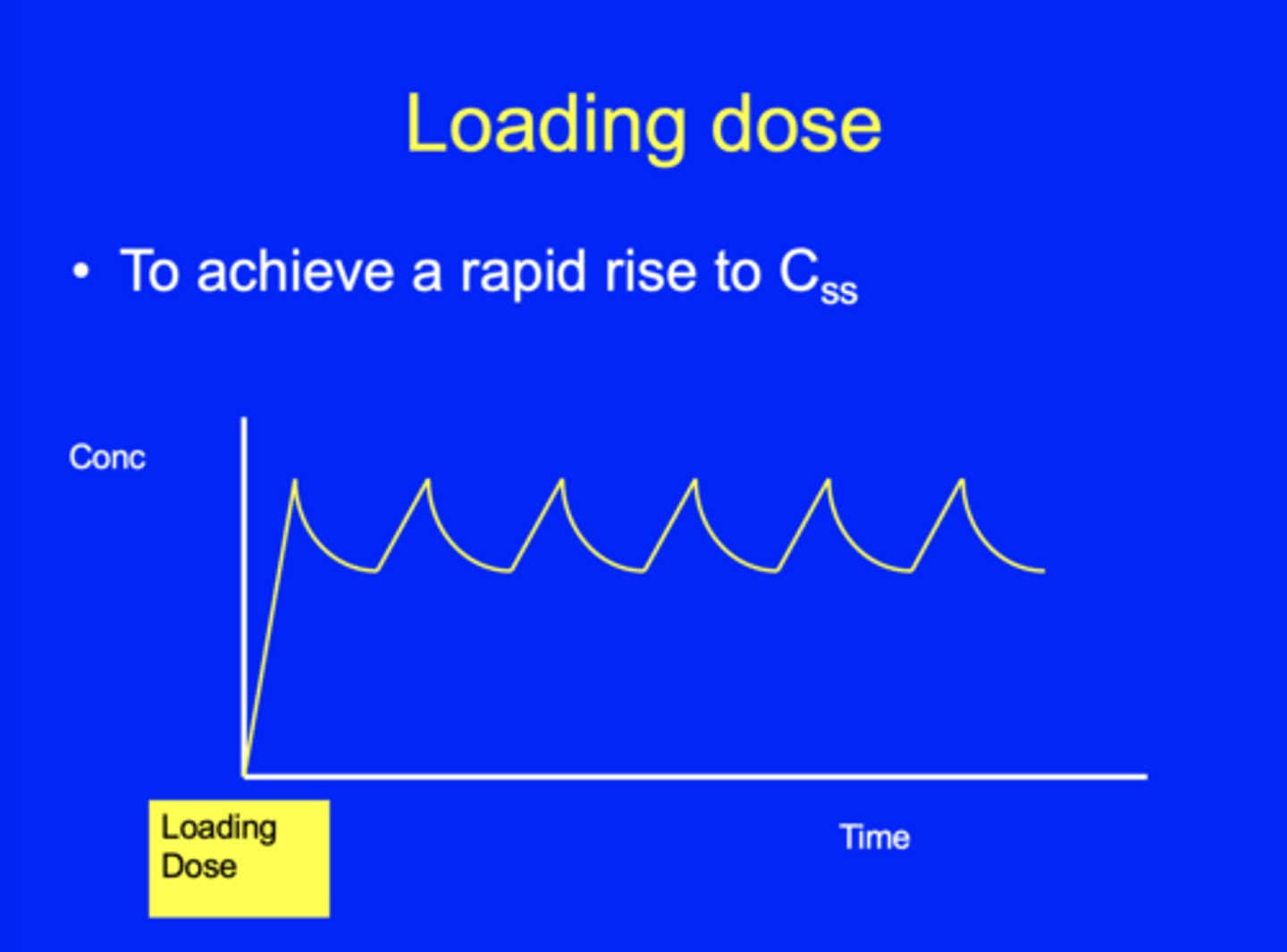
How often are drugs with a short half-life that have a large TW given?
3-4 times a day.
How often are drugs with a short half-live that have a narrow TW given?
Intravenous infusion.
What is the maintenance regimen for drugs with medium half-lives?
Medium half-life is of an intermediate length. By t-1/2 and the therapeutic window.
It is down to logic. Eg, the t-1/2 is 8 hours. You would not want to keep the dosage interval (tau) every 8 hours because that might risk you losing the TW, so you would keep the dosage interval for every 6 hours i.e. choose tau below the half-life value.
What is the maintenance regimen for drugs with long half-lives?
You use daily dosing for better pt. compliance and work out the maintenance dose as the amount eliminated in 24 hours.
tau would be 1 (as in daily).
What is Gentamicin?
Gentamicin is an antibiotic used to treat several types of bacterial infections. This may include bone infections, endocarditis, pelvic inflammatory disease, meningitis, pneumonia, urinary tract infections, and sepsis among others
Which bacterial infections is gentamicin not effective for?
Not effective for gonorrhoea or chlamydia infections
What is the maintenance regimen for Gentamicin and who is it given to?
As a doc, you have to ensure the troughs (plasma conc) is sub-therapeutic so it prevents the damage of the ears and kidney. This is given to vulnerable pts.
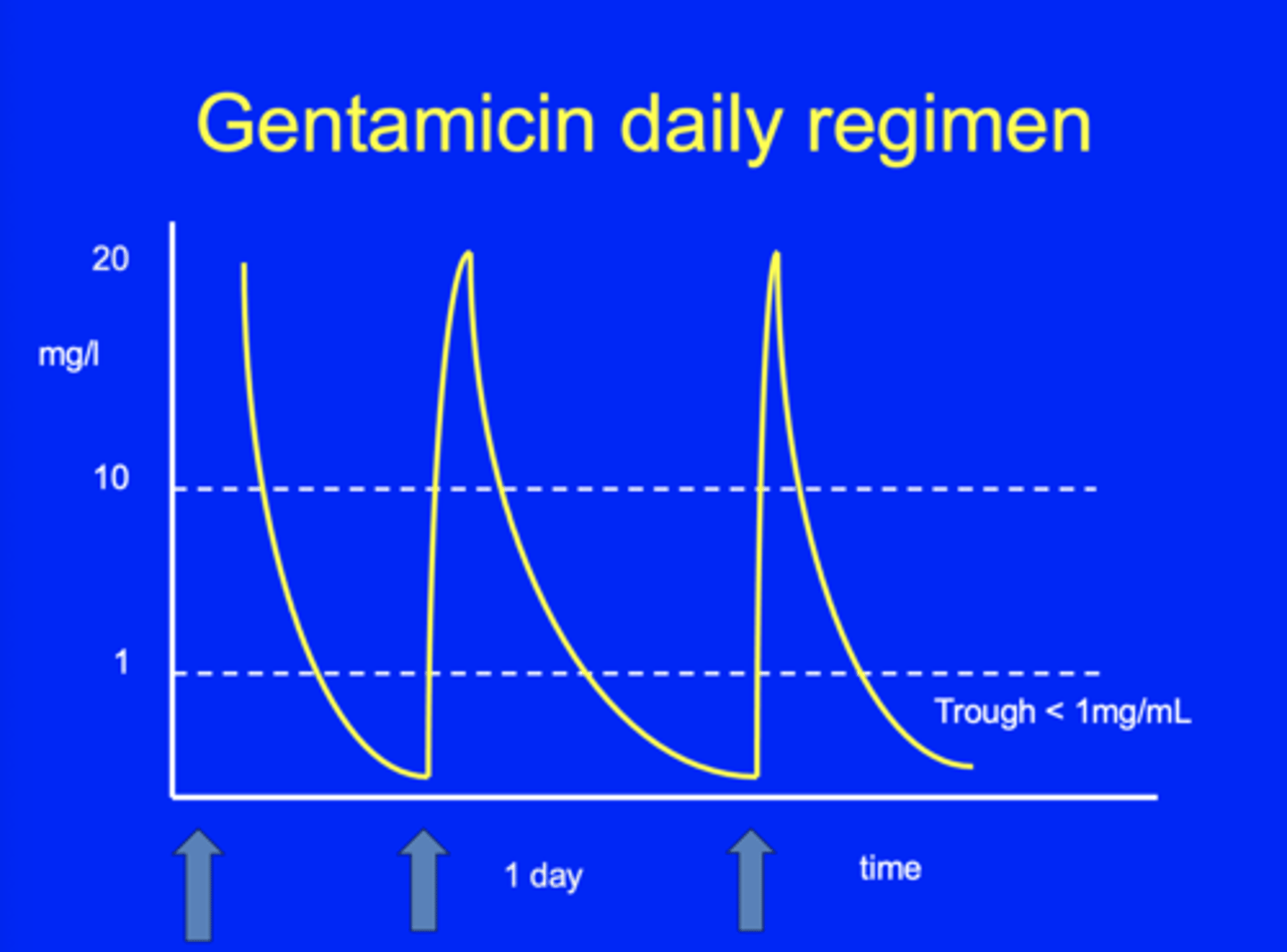
Why are you given a subtherapeutic window for Gentamicin?
1. By using daily dosing, bacteria are killed by the high dose.
2. Dose falls rapidly and kidneys/ears are only exposed to toxic conc for a short time.
What are metered dose inhalers? (2)
1. Rapid effect aerosol.
2. Needs right technique.
What are the advantages of spacers? (3)
1. Improves delivery.
2. Reduces impaction on throat.
3. Improves steroid deposition.
What is the difference between short and long acting bronchodilators? (give examples)
Short: rapid on receptor, rapid offset eg. salbutamol. (rapid onsent of action but quickly cleared from the body so provided short-term relief)
Long: these are preventers, they go on rapidly but stick to receptor and so have a slow offset eg. salmeterol or tiotropium. (offering prolonged bronchodilation for prevention of symptoms)
Example of short acting beta-2 agonist drug
Salbutamol
Example of long acting beta 2 agonist drug
Salmeterol
Short acting antimuscarinic drug
Ipratropium
Long acting antimuscarinic drug
Tiotropium