nurs 210: chapter 22 - the respiratory system
1/67
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
68 Terms
respiration is:
the exchange of gases between atmosphere, blood, cells
combo of 3 processes is required for respiration to occur:
ventilation (breathing), external (pulmonary) respiration, internal (tissue) respiration
the cardiovascular system assists:
the respiratory system by transporting gases
structurally, components of respiratory system divided into 2 parts:
upper respiratory system, lower respiratory system
functionally, components of respiratory system divided into 2 zones:
conducting zone, respiratory zone
upper respiratory system consist of:
nose, pharynx, associated structures
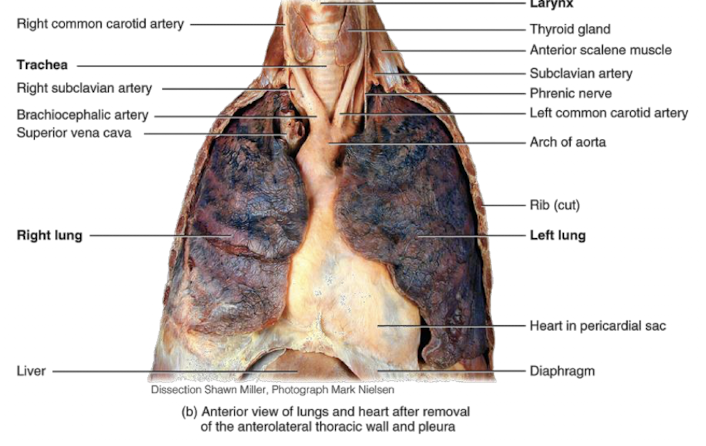
lower respiratory system consist of:
larynx, trachea, bronchi, lungs
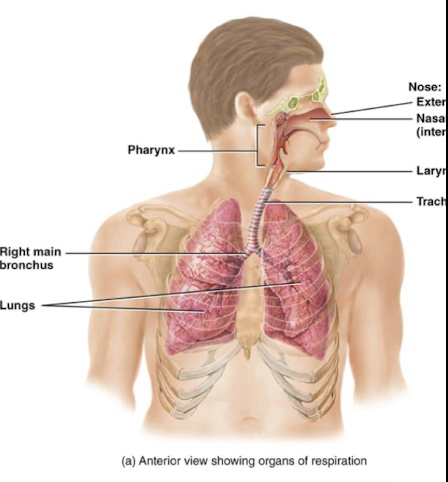
picture of overiew nose, pharynx, larynx, and trachea
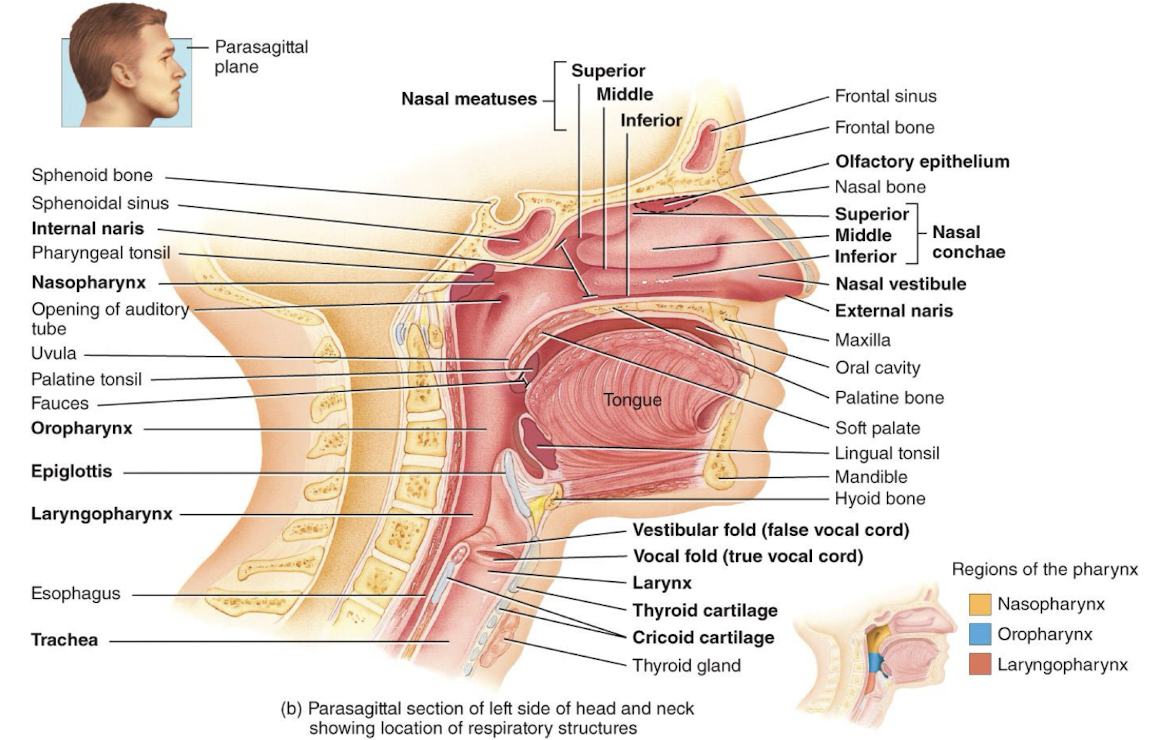
pharynx
functions as a passageway for air and food, houses the tonsils, which participate in immunological reactions against foreign invaders
larynx (voice box)
passageway that connects the pharynx and trachea, contains vocal folds which produce sound when they vibrate
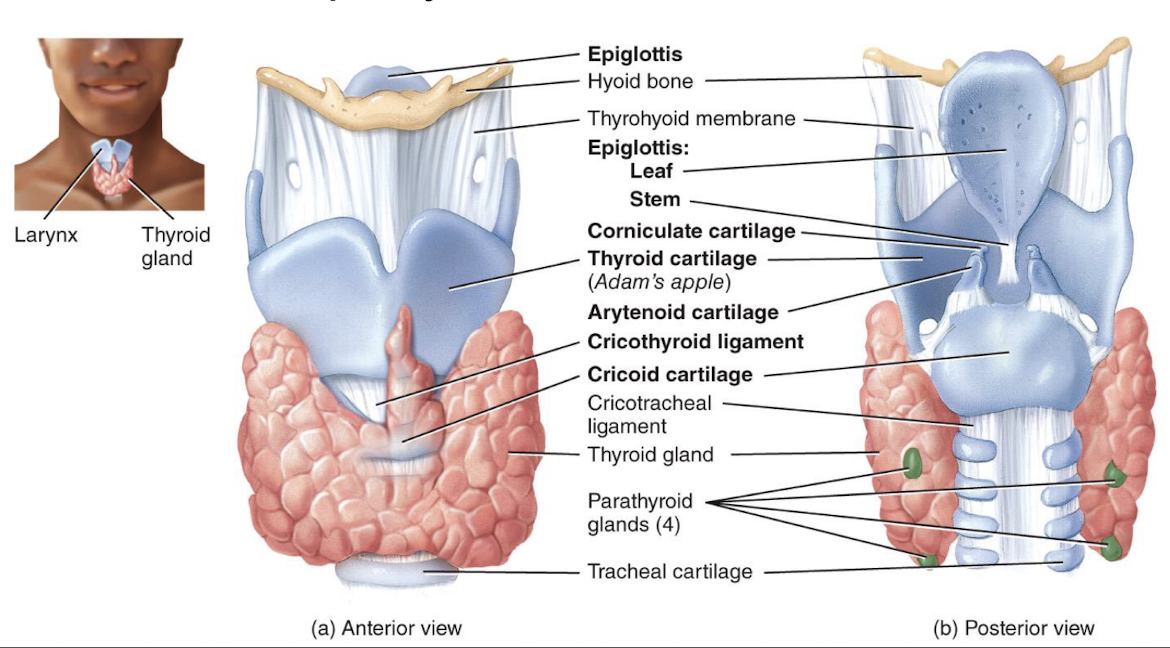
trachea
extends from the larynx to the primary bronchi
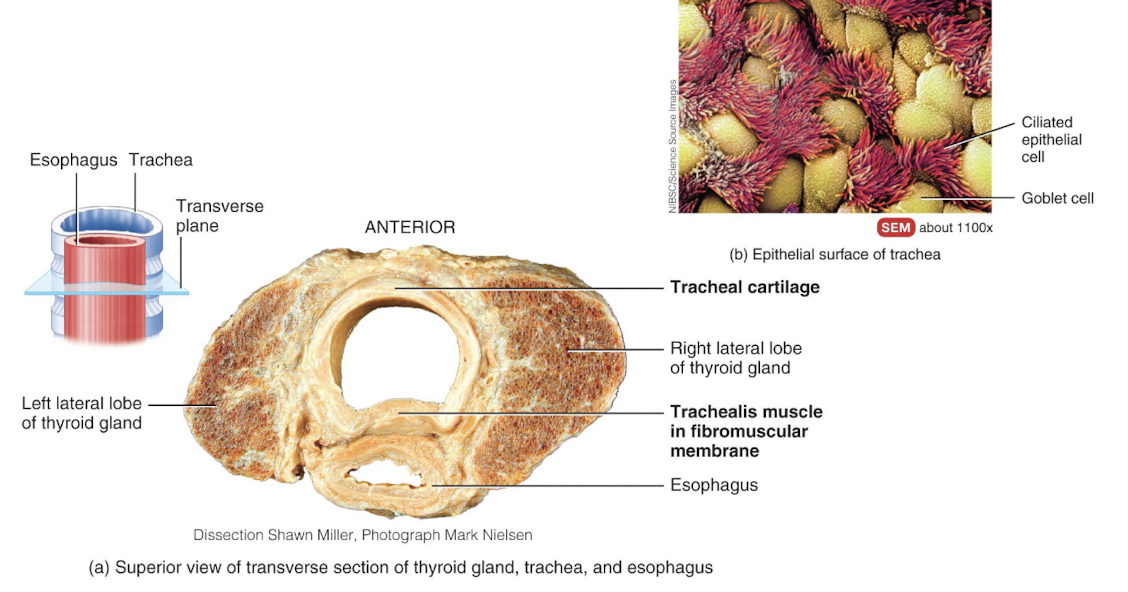
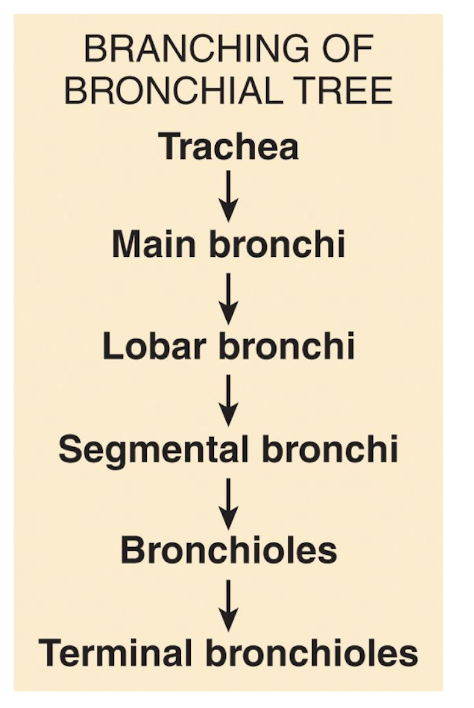
bronchi
trachea branches into right primary bronchus that enters right lung, and left primary bronchus that enters left lung; upon entering the lungs, primary bronchi further divide to form smalelr diameter branches
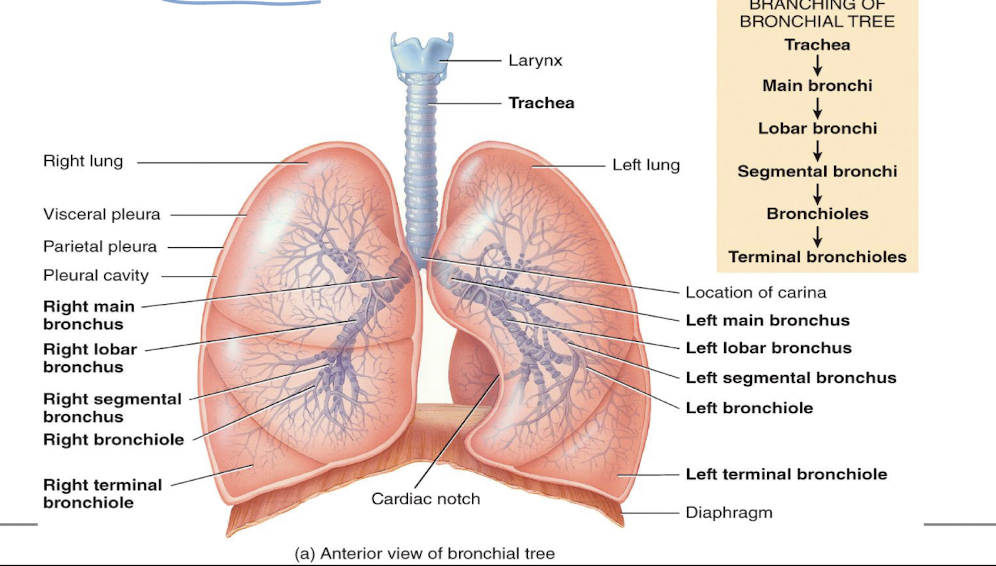
terminal bronchioles
end of conducting zone
picture of table bronchi
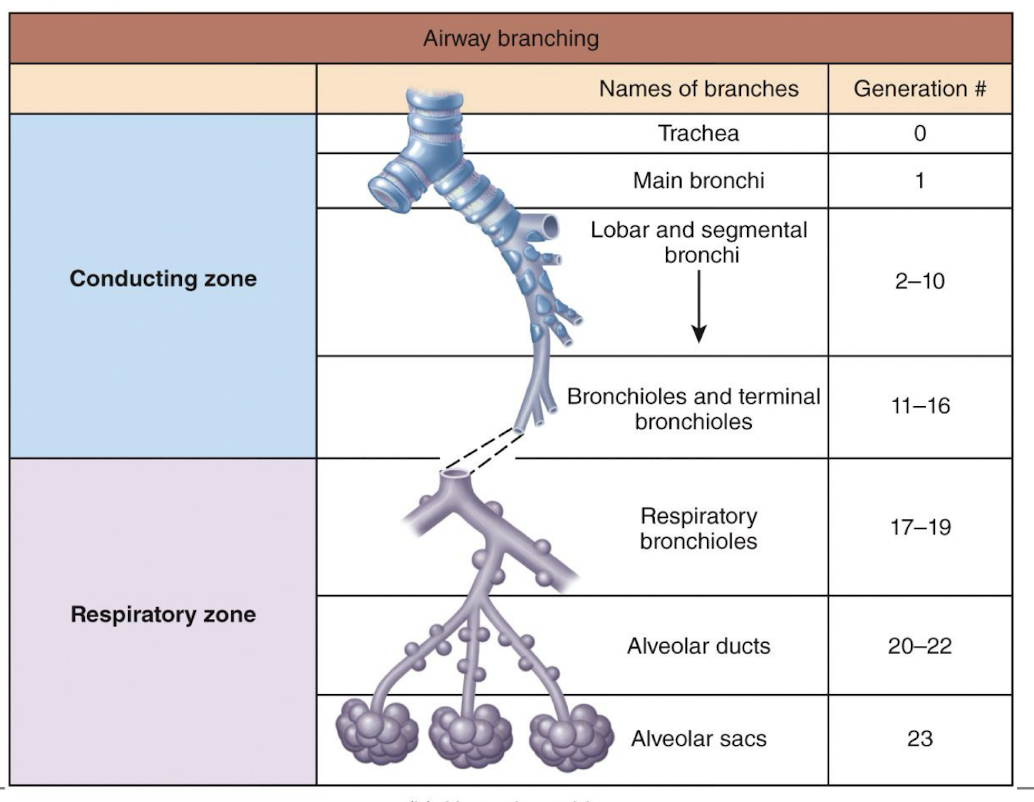
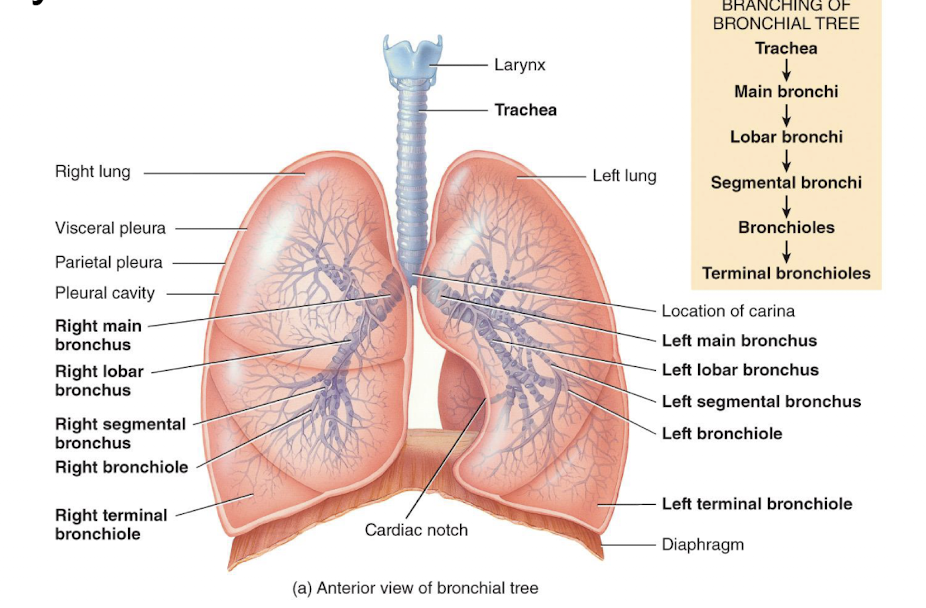
lungs
paired organs in the thoracic cavity; they’re enclosed and protected by the pleural membrane
alveoli
when conducting zone ends at termina branchioles, respiratory zone begins, which then terminates at the alveoli (“air sacs” found within the lungs)
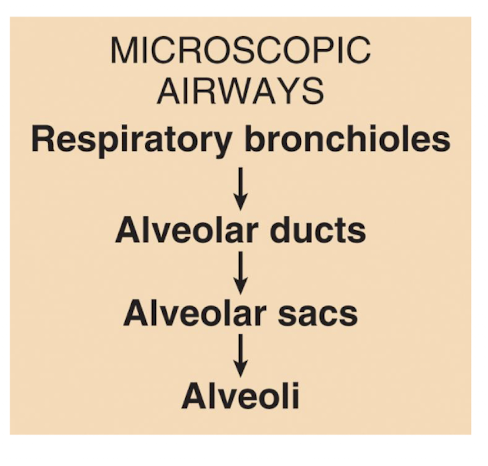
picture of alveoli in a lobule of a lung
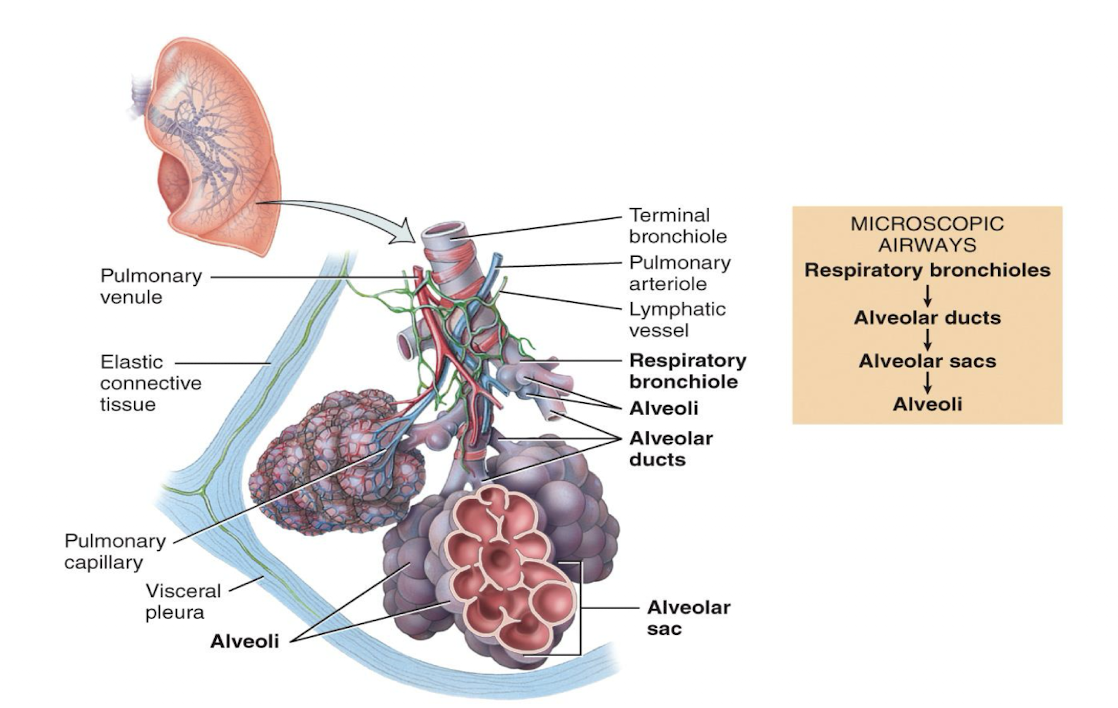
2 kinds of alveoli
type I, type II
type II alveoli secretes:
surfactant, which reduces surface tension in alveoli, which prevents alveoli from collapsing
respiratory membrane is composed of:
layer of type I and type II alveolar cells (and associated alveolar macrophages that constitutes the alveolar wall)
an epithelial basement membrane underlying the alveolar wall
capillary basement membrane that is often fused to epithelial basement membrane
capillary endothelium
pulmonary ventilation
air flows between the atmosphere and the alveoli of lungs between of alternating pressure difference created by contraction and relaxation of respiratory muscles; inhalation (inspiration) air moves out to lungs, exhalation (expiration) air moves into lungs
picture of 3 basic steps involved in respiration
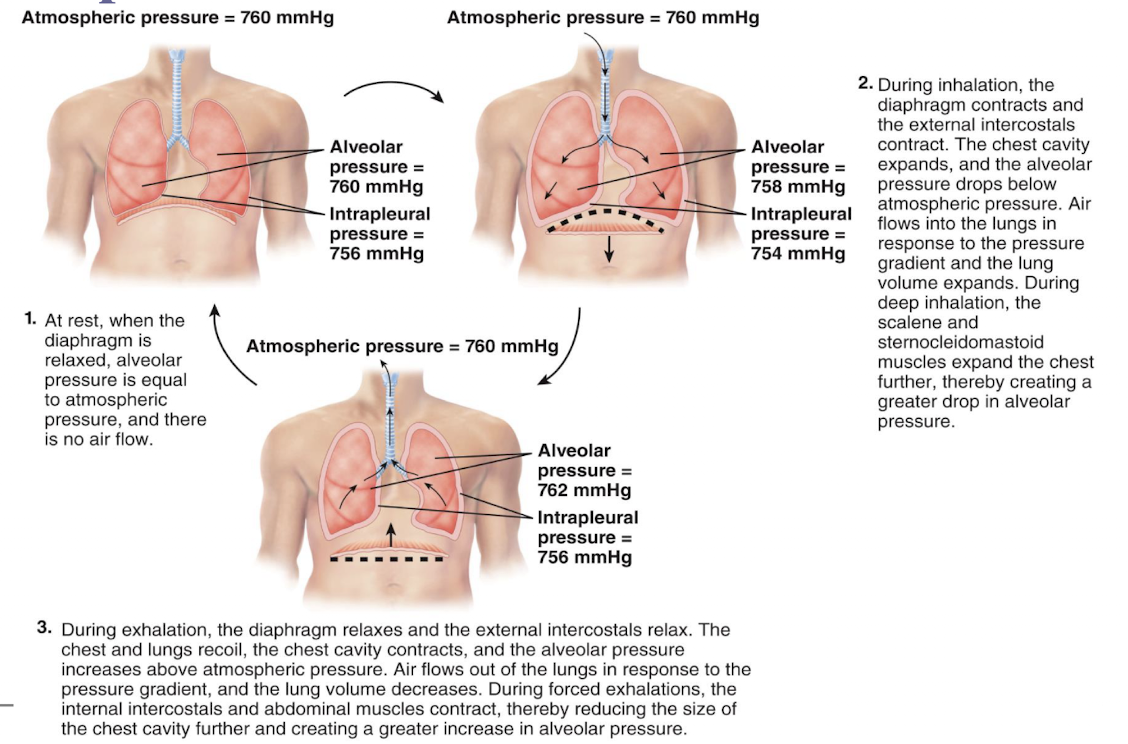
boyle’s law
pressure changes that drive inhalation and exhalation are governed by boyle’s law; volume of gas varies inversely with its pressure
intrapulmonary pressure
aka intra-alveolar pressure; in relaxed breathing, difference between atmosphere pressure and intrapulmonary pressure is small (about -1 mmHg on inhalation or +1 mmHg on exhalation)
intrapleural pressure
pressure in space between parietal and visceral pleura; remains below atmospheric pressure throughout respiratory cycle
picture of muscles of inhalation and exhlation
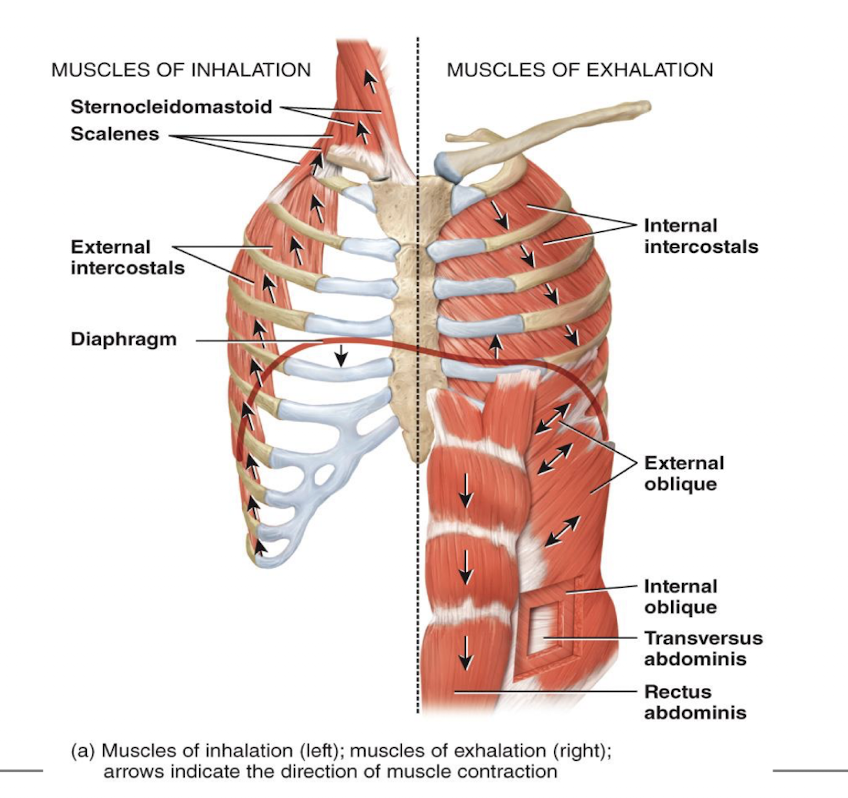
breathing patterns and respiratory movement
eupnea, apnea, dyspnea, tachypnea, bradypnea
eupnea
quiet breathing or resting respiratory rate; adults 12-18 breath/min
apnea
cessation of breathing
dyspnea
labored or difficult breathing
tachypnea
abnormally fast breathing
bradypnea
abnormally slow breathing
picture of spirometry
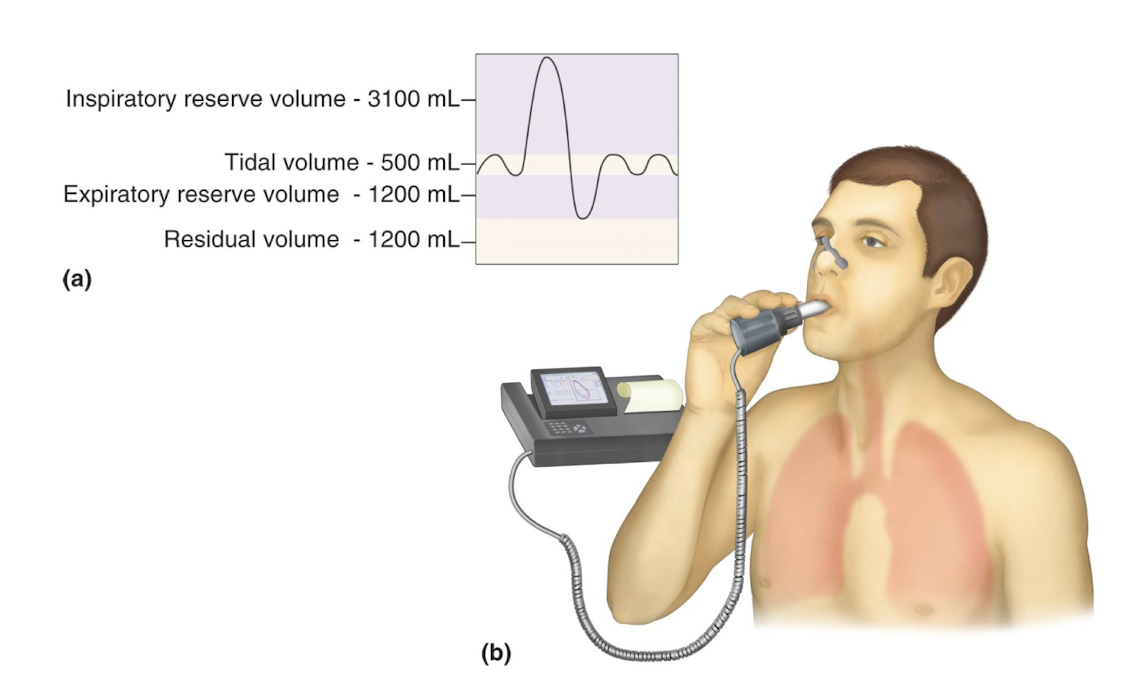
tidal volume (TV)
amount of air moved into and out of lung with each breath (averages ~500 ml)
inspiratory reserve volume (IRV)
amount of air that can be inspired forcibly beyond the tidal volume (2100-3200)
expiratory reserve volume (ERV)
amount of air that can be forcibly expelled from lungs (1000-1200 ml)
residual volume (RV)
amount of air that always remains in lungs; needed to keep alveoli alive
picture of lung volumes and capacities
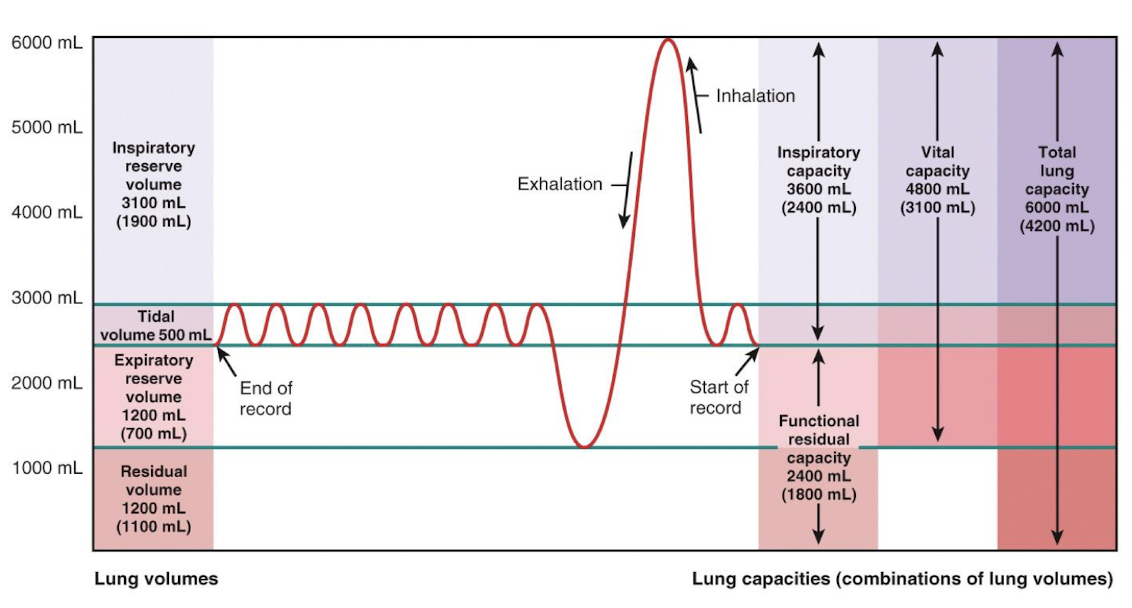
q1
q2
q3
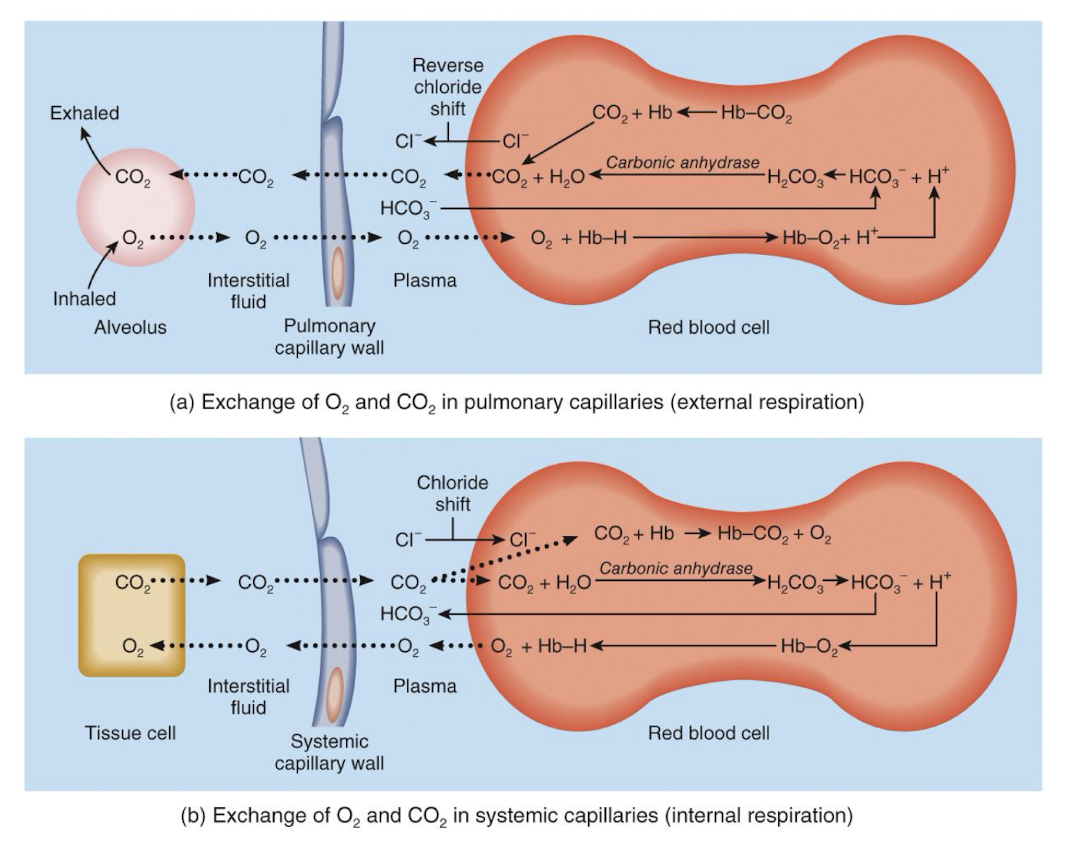
external respiration
oxygen will diffuse from the alveoli into pulmonary capillaries; CO2 moves in opposite direction
internal respiration
oxygen will diffuse from systemic capillaries into tissue; CO2 moves in opposite direction
transport of O2
1.5% of O2 is dissolved in plasma, with 98.5% of O2 being carried by hemoglobin (Hb)
transport of CO2
7% of CO2 is dissolved in plasma, 23% of CO2 is carried by Hb inside red blood cells as carbaminohemoglobin; 70% of the CO2 is transported as bicarbonate ions (HCO3)
formation of bicarbonate involves CO2 combining with:
water to form carbonic acid H2CO3, which quickly associated into bicarbonate and H+, which is part of transport of CO2
transport of CO2 occurs primarily in RBCs, where:
enzyme carbonic anhydrase reversibly and rapidly catalyzes this reaction
for transport of CO2, in systemic capillaries, after HCO3- is created, it:
quickly diffuses from RBC into plasma, which is an outrush of HCO3- from RBCs is balanced as CI- moves into RBCs from plasma, referred to as chloride shift
picture of exchange of O2 and CO2
hypercapnia
a slight increase in P(CO2) and thus H+, stimulates central chemoreceptors
hypoxia
oxygen deficiency at tissue level, caused by low P(O2) in arterial blood due to high altitude, airway obstruction or fluid in lungs
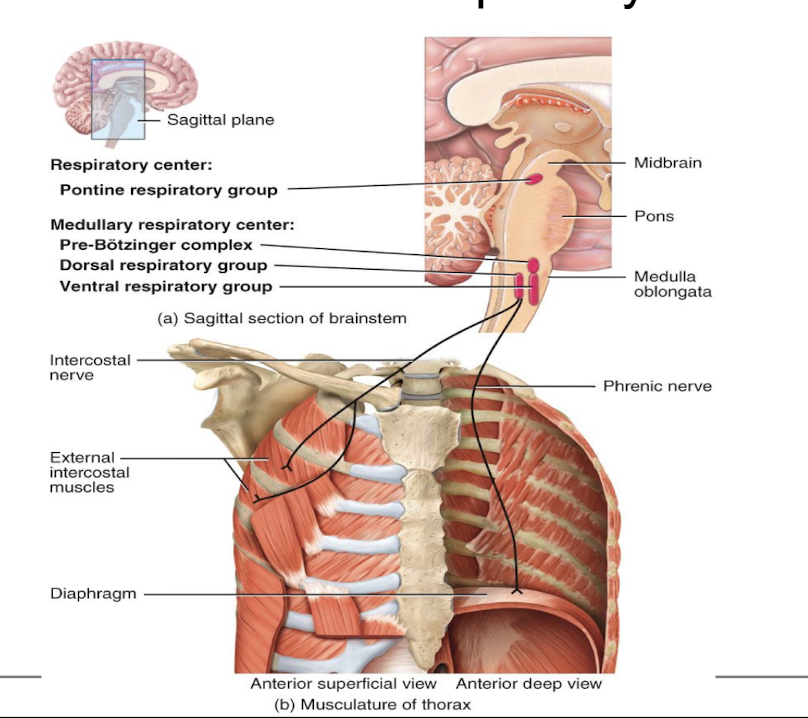
control of respiration
location of areas of respiratory center
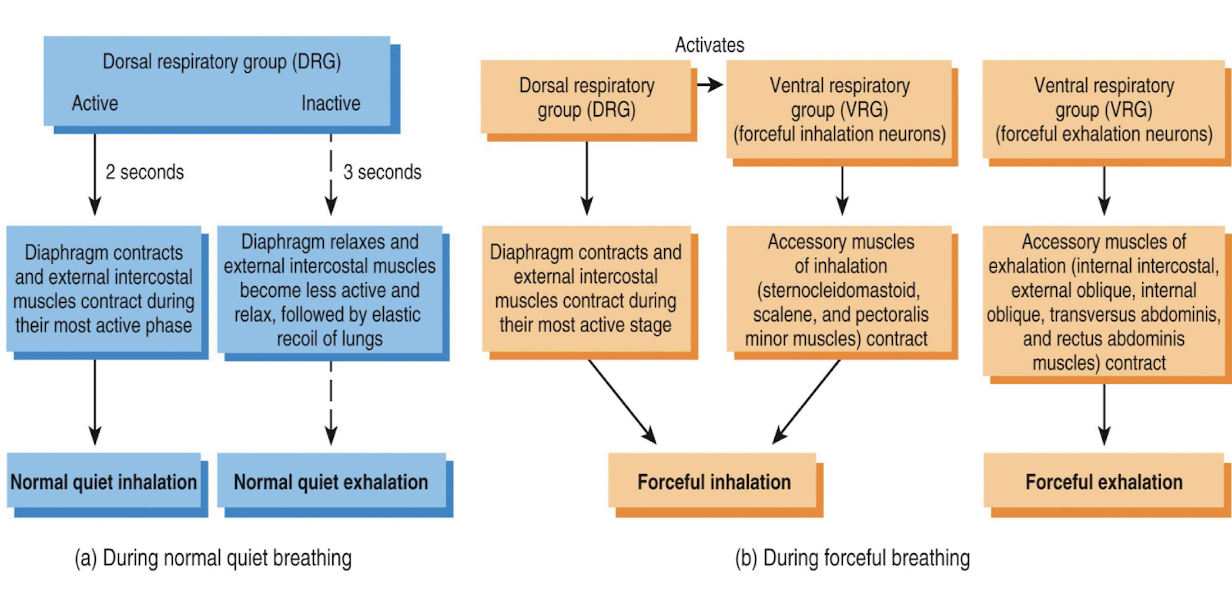
picture of normal and forceful breathing
cortical influences
allow conscious control of respiration that may be needed to avoid inhaling noxious gases or water
chemoreceptor
central and peripheral chemoreceptors monitor levels of O2 and CO2 and provide input to respiratory center
central chemoreceptors
located throughout brain stem
peripheral chemoreceptors
found in aortic arch and carotid arteries
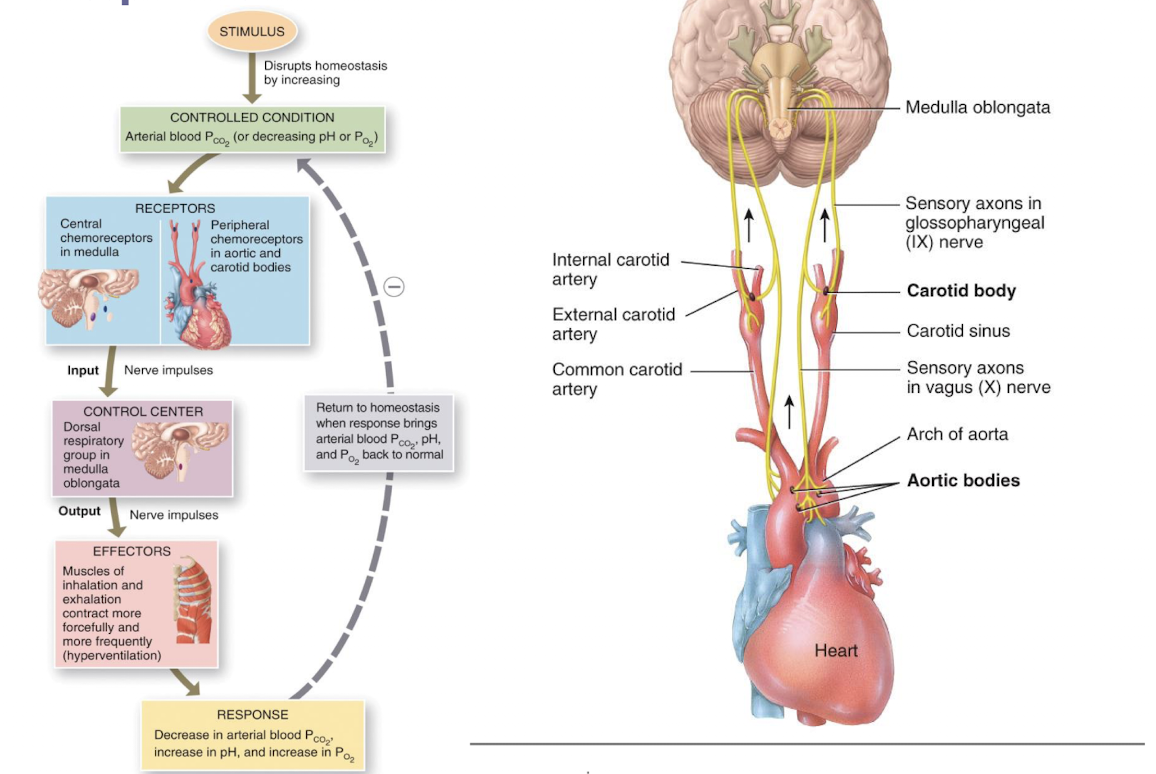
control of respiration
changing levels of PCO2 and pH are most important; levels of these chemicals are sensed by chemoreceptors
if blood P(CO2) levels rise (hypercapnia), which CO2:
accumulates in brain and joins with water to become carbonic acid; carbonic acid dissociates, releasing H+, causing a drop in pH (increase acidity); increases H+ stimulates central chemoreceptors of brain stem, which synapse with respiratory regulatory centers, which even also increases depth and rate of breathing, causing act to lower blood PCO2 and pH to rise to normal levels
picture control of respiration w/ brain
hering-breuer reflex (inflation reflex)
stretch receptors in pleurae and airways are stimulated by lung inflation, send inhibitory signals to medullary respiratory centers to end inhalation and allow expiration; may act as protective response more than as a normal regulatory mechanism
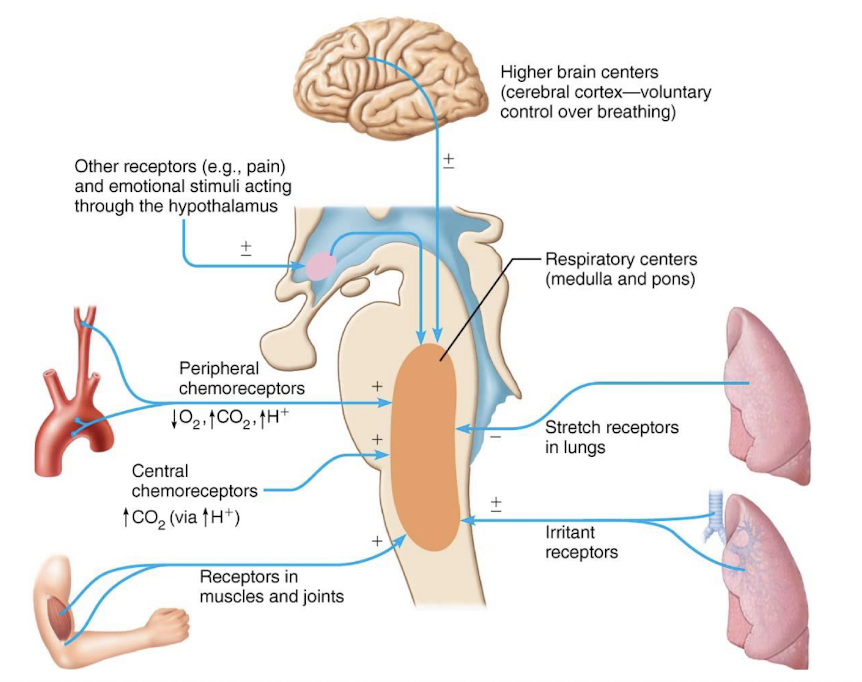
picture of neural and chemical influences on brain
q4
q5
q6
q7
q8
q9