Ch 20 Blood Vessels and Circulation
1/82
Earn XP
Description and Tags
EXAM II
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
83 Terms
direction of bloodflow, starting in heart/ending in veins
heart → arteries → arterioles → capillaries → venules → veins → heart
3 layers of blood vessels
tunica externa
tunica media
tunica intima
tunica externa composition and role (arteries)
made up of collagen and elastic fiber
anchors vessels to adjacent tissues in arteries
tunica externa composition (veins)
contains elastic fibers and smooth muscle cells
vasa vasorum
small arteries and veins that supply the tunica media and externa
what types of vessels have vasa vasorum
large arteries and large veins
makeup of the tunica media
smooth muscle
external elastic membrane
separates tunica media and externa
two layers of the tunica media
inner: circular sheets
outer: longitudinal
role of tunica media
vasoconstriction and vasodilation
how is the tunica media regulated
sympathetic fibers via the nervi vasorum
makeup of the tunica intima
connective tissue
endothelium layer
internal elastic membrane
part of tunica intima
only in arteries
what factor allows arteries to absorb pressure
elasticity
contractility (diameter can change)
what regulates the elasticity and contractility of vessels
sympathetic division of the ANS
vasoconstriction
arterial smooth muscle contraction by ANS
vasodilation
relaxation of arterial smooth muscle
lumen is enlarged
conducting arteries
elastic arteries
large size
tunica media is more elastic fibers than muscle fibers
distribution arteries
muscular arteries
medium size
arterioles
very small
thin or incomplete tunica media
little to no tunica externa
aneurysm
bulge in arterial wall
weak spot in elastic fiber
pressure can rupture vessel
structure of capillaries
endothelial tube
similar diameter to red blood cell
no tunica media and no tunica externa
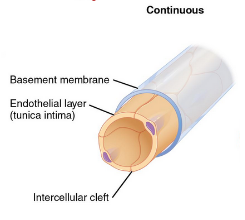
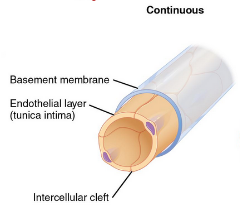
continuous capillaries
complete endothelium
in all tissues except epithelia and cartilage
diffusion of water, small solutes, lipid-soluble materials
block plasma proteins and blood
CNS capillaries
restrict permeability using tight junctions, a thick basement membrane, and astrocyte extensions
makes blood brain barrier
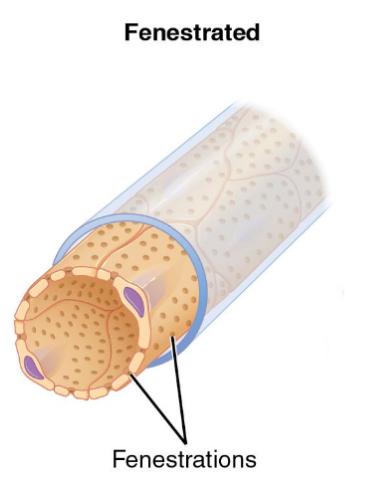
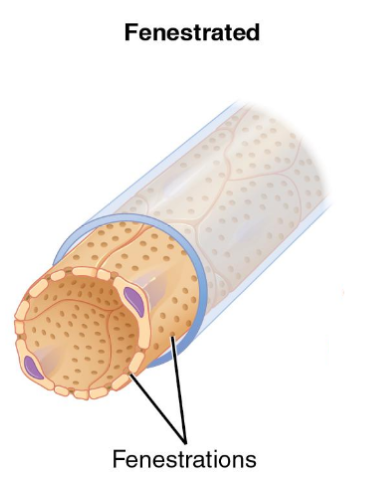
fenestrated capillaries
pores in the endothelial lining
rapid exchange of water and large solutes
where are fenestrated capillaries found
choroid plexus to protect the CSF
endocrine organs for hormone exchange
kidneys to filter blood
intestinal tract for nutrient absorption
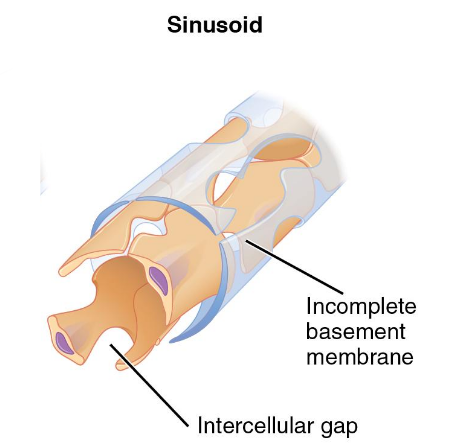
sinusoids
gaps between adjacent endothelial cells
free exchange
phagocytes present to monitor blood
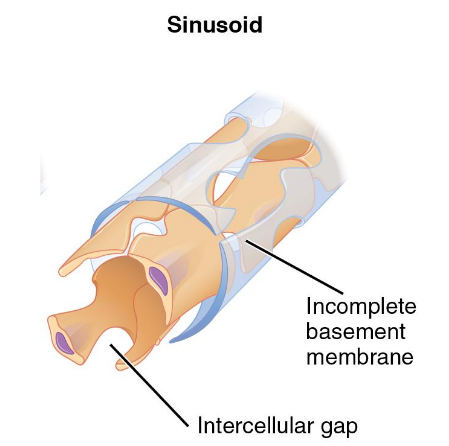
where are sinusoids present
liver to filter blood from hepatic portal and such
spleen to filter systemic blood
bone marrow for new RBCs
endocrine organs to filter lymph
capillary beds
capillary plexus
connects one arteriole and one venule
precapillary sphincter
guard capillary entrance
causes capillary blood to flow in pulses by opening/closing valves
thoroughfare channels
direct connections between arterioles and venules
how are thoroughfare channels controlled
smooth muscle segments called metarterioles
vasomotion
contraction and relaxation of capillaries that causes blood flow to constantly change routes
bulk flow
mass movement of fluids through capillary beds that flows from areas of high to low pressure
filtration
fluid in capillaries pushed out of arterial end
reabsorption
fluid pulled into venous end of capillary
hydrostatic pressure
pressure exerted by blood from the heart pumping against an enclosed space
osmotic pressure
water is drawn into the venous end due to high solute pressure
size comparison between arteries and veins
veins are larger than arteries but have thinner walls
blood pressure comparison between veins and arteries
veins have lower blood pressure
venules
small veins that collect blood from capillaries
describe the tunica media of medium-sized veins
few smooth muscle cells
tunica externa of medium sized veins
longitudinal bundles of elastic fiber
describe each layer of a large vein
all three layers
thick tunica externa
thin tunica media
venous valves composition and function
folds of the tunica intima
prevents backflow and compresses to push blood toward the heart
what percent of blood volume is heart, arteries, and capillaries
30% - 35%
what percent if the body’s blood volume is the venous system
60% - 65%
1/3 in venous networks of liver, bone marrow, and skin
what signal indicates to the body to redistribute blood
vasomotor center in the medulla sends sympathetic stimulation to smooth muscle in veins
resistance
factors that slow blood flow
blood pressure
force exerted on the walls of vessels and the heart chambers
systolic
pressure on the arterial chambers when blood is ejected via ventricular contraction
diastolic
arterial pressure when the ventricles are relaxed
sphygomanometer
instrument that listens to the sound of bloodflow to measure blood pressure
korotkoff sounds
ticking sound created by turbulent blood flow
normal blood pressure
120/80
hypertension
abnormally high blood pressure
>140/90
hypotension
abnormally low blood pressure
pulse
caused by expansion and recoiling of elastic fibers in the arteries
mean arterial pressure
mean arterial pressure
average blood pressure in the arteries
difficult to quantify
70-110 mm Hg
MAP formula
MAP = diastole BP + ((systolic-diastolic BP)/3)
5 examples of things that affect blood flow and blood pressure
cardiac output
compliance (elasticity of vessels)
volume of blood
viscosity of blood
vessel length and diameter
cardiac volume formula
stroke volume x heart rate
stroke volume
amount of blood pumped out by the left ventricle during systole
compliance
blood vessels expanding to accommodate more blood
veins > arteries
healthy vessels > atherosclerotic vessels
Poiseuille’s equation
uses blood viscosity, length of blood vessel, and radius of vessel to descrive the blood flow
pressure (P)
pressure generated to overcome resistance
pressure gradiant (∆P)
difference between pressure at heart and at capillary beds
blood flow (F)
pressure difference (∆P) divided by resistance (R)
blood volume
usually stays roughly constant but can change due to various conditions
hypovolemia
reduction in blood volume
hypervolemia
excessive fluid volume
caused by sodium and water retention
what conditions put one at risk for hypervolemia
heart failure
liver cirrhosis
blood viscosity
also does not change quickly
due to formed elements and plasma proteins
vessel length vs resistance
longer vessels = greater resistance
how many vessels do adults have
60,000 miles
dynamics of the blood vessels diameter
routinely changes throughout the day
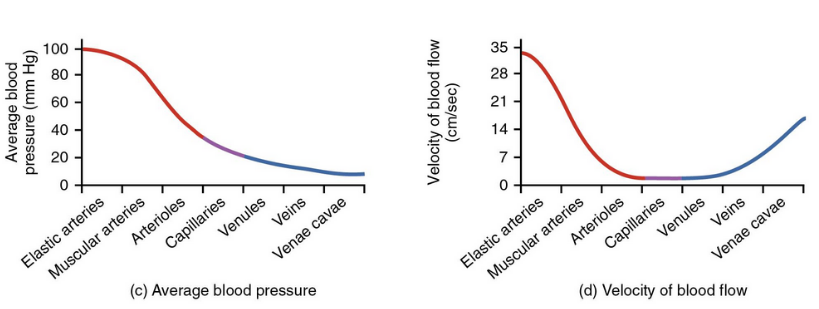
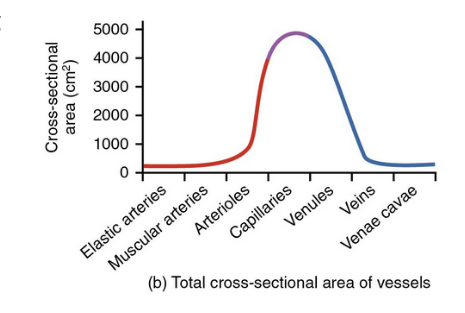
examine these
this one too!
vessel diameter would be a parabola
venous system
blood in the veins are continually moving toward the atria
vascular tone of the venous system creates a pressure gradient
pressure difference between veins and atria
pressure in the veins is higher than the atria
skeletal muscle pump
helps vessels overcome gravity
valve system
respiratory pump
promotes blood flow through veins of abdomen and thorax
respiratory pump during inhalation
thorax volume increases and compresses the abdominal cavity
blood is forced back into the atria