Radiology
1/21
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
22 Terms
Define radiograph vs radiography vs radiology vs radiographer vs radiologist
Radiograph = recorded image after xray passes through a patient
Radiography = art and science of taking a radiograph
Radiology = study and interpretation of radiographs and other diagnostic imaging modalities
Radiographer = person with special expertise in taking radiographs
Radiologist = special clinician whose study allows them to accurately interpret radiographs and other diagnostic imaging
Explain Ionising vs Non-ionising radiation
Electromagnetic Radiation = all ionising and non-ionising forms
all travel at 300,000 km/s
various frequency and wavelength determines their ability to travel through objects and heating ability = also effects on people
Ionising Radiation
high energy and frequency + short wavelength
enough energy to cause chemical change / bread bonds = damage living tissue
ionisation = when an electron is given enough energy to break away from an atom
Examples: Gamma Rays, Xrays, UV Light
Gamma Rays = originate from the nucleus of decaying radionuclide
Ex: nuclear medicine or scintigraphy (most energetic photon)
Xrays = produced when electrons interact within an atom
Ex: radiography, fluoroscopy, CT (least energetic photon)
Non-ionising Radiation
low energy and frequency + long wavelengths
enough energy to excite molecules → vibrations = heat
Examples: UV, Visible, Infared, Microwaves, Radio
Explain the components of an Xray Tube and how Xrays are produced
electrons go from cathode (positive charge) → anodes (negative charge)
when electrons his the anode and suddly stop they release energy by either:
Braking = Bremsstrahlung Radiation
electrons slows down and does a U turn around the nucleus, then goes back in the direction it came from
Ejecting = Characteristic Radiation
projectile electron smashes into electron, then darts out of the atom and all the other electrons jump to fill the void
Xray beams diverge from a point source and travel in straight lines
obey the inverse square law
attenuate differently through different tissue due to differences in atomic number, mass density and xray energy
when electrons reach anode, a number of varying intensity xrays are produced in all directions
low energy xrays are filtered out with aluminium filter to reduce absorbed dose
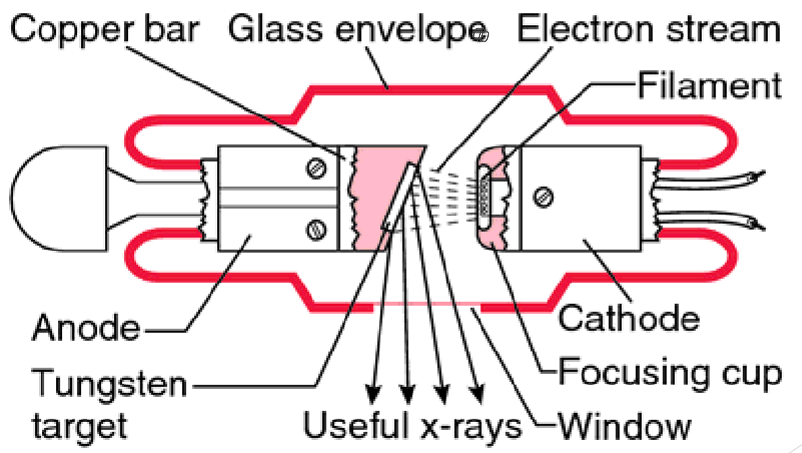
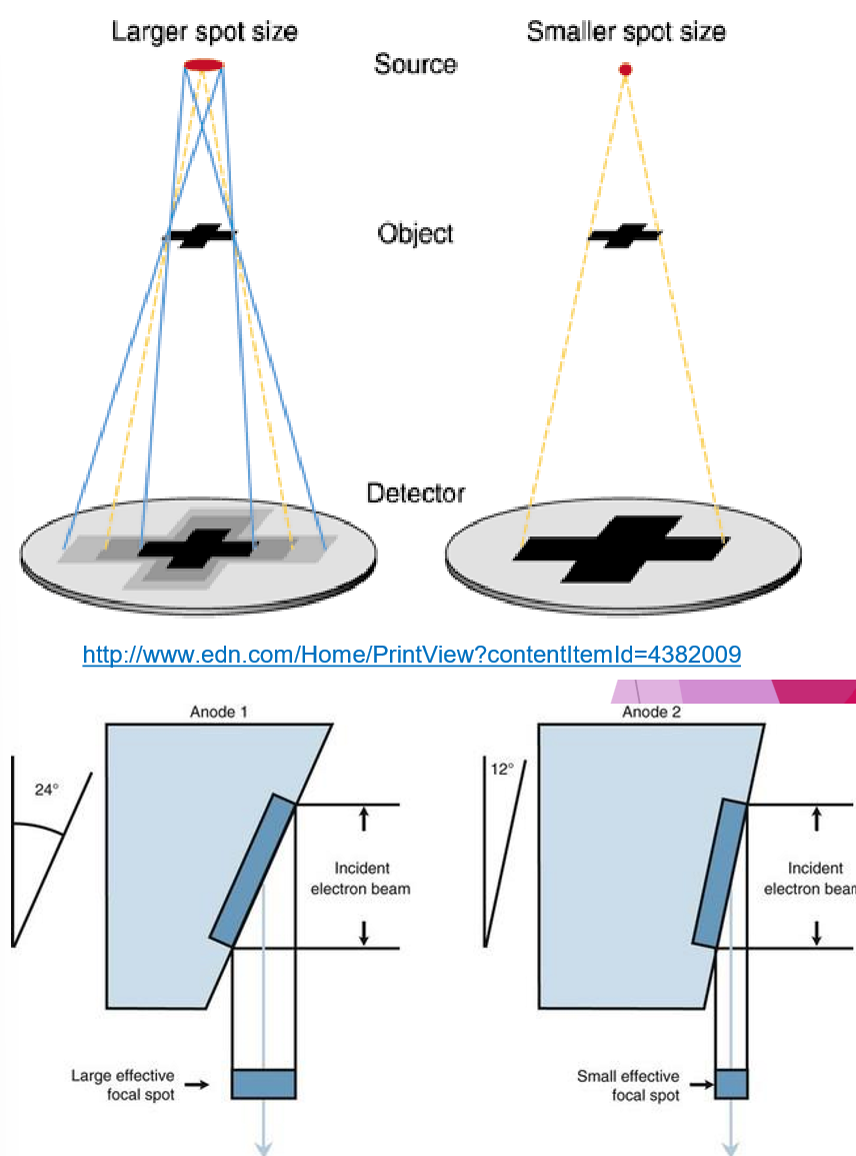
How does energy and anode positions effect Xrays?
low exposure (bright image) → high exposure (dark image)
Xray photons = 1%, vs heat produced = 99% → use oil to dissipate heat
Focal spot is the anode = electrons are focused here (from cathode)
larger focal spot = larger heat dissipation BUT decreases image quality due to Penumbra Effect
Penumbra Effect = ability to increase focal spot size to assist in heat dissipation without effecting the projected size by using the Line Focus Principle
Anode Heel Effect
Xray beam has central rate and many divergent beams (cathode → anode)
cathode side has more intensity than anode side
place thickest part of anatomy on the cathode side, to ensure more even exposure of varying thickness of tissue
increased distance = reduce anode heel effect
reduce field of view + smaller image receptors = uniform/central beam
Stationary vs Rotating Anode
Stationary anode = limited use due to poor heat dissipation
Rotating anode = increased surface area so better heat dissipation, also allows you to use a smaller focal spot for improved image quality
What happens when Xray’s interact with matter?
Penetration
through an object unaffected
limited attenuation
image is black as gas does not absorb xray photons
Absorption
absorbed by an object due to the photoelectric effect
demonstrates attenuation
image is white/radiopaque as photons reach the image receptor
bones = absorb many photons (high attenuation) = white
soft tissue = absorb some photons (varied attenuation) = grey
Scatter
scattered by object due to “Compton scatter”
demonstrated attenuation
photons are deflected from expected course = degrades image quality
can use a grid to reduce the effect of scattered radiation
What are the 3 exposure factors for Xray production?
kVP = Kilovoltage Peak
potential energy difference across the tube
determines the energy of electrons = penetrating power of the photons → contrast
quality of the xray
mA = milliamperage
tube current
number of electrons from filament = number of xray photons produced → density
quantity of xray
Time (seconds)
timing of the tube current
mA x time (s) = mAs
mAs value with a high mA and short time = best
quantity measurement
Effects / damage caused by radiation
Cellular
change nucleus, DNA and organelles
cellular death, scaring or altered cell metabolism
may lead to somatic change (cancer) or genetic depending what cells
Somatic Change = directly harmful → cancer, cateract, radiation burn
Genetic Change = future harm → damage to DNA of germ cells
How (including units) can you measure radiation?
Absorbed Dose = Gy (Gray) = radiation required to deposit energy of 1 Joule in 1kg of tissue
Equivalent Dose = Sv (Sievert) = absorbed dose x radiation weighting factor (Wr)
weight factor accounts that for different types of radiation, there are different abilities to damage biological tissue
Effective Dose = Sv (Sievert) = sum of (equivalent dose x tissue weighting factor) for each organ or body part irradiated
indicates each organs sensitivity to radiation
Maximum Permissible Dose (MPD) = the absolute max - all radiation is damaging
QLD occupational limit = 20 mSv / year
non-occupational limit = 1 mSv / year (comes from space, food, water)
Radiation Badges = all you to measure and record types of radiation
ALARA = as low as reasonably achievable
Radiation Safety Act (1999) and Radiation Safety Regulations (2021) explains that you must have a licence to operate check equipment, safety plan
Explain the 4 Pillars of Radiation Safety
Time = limit time as much as possible
Dose creep allows radiographs to be edited to reduce repeats at varied exposure
Overexposed film = black vs underexposed film = white
Distance = inverse square law (further = safer)
Shielding = PPE such as lead gowns, thyroid collar, lead gloves, hand/arm shields, glasses
Common Sense = rooms are labelled with a warning light visible from outside, certified by gov
Restraining patients for Xrays
Chemical = anaesthetic and sedation
Manual = positioning aids
Physical = staff restraining with PPE (avoid where possible)
Large animals = many people required to be around to restrain or hold machine. Also due to animal side require higher exposures
collimate beam as much as possible
PPE
distance - inverse square law
effective chemical or manual restraint = best radiograph the 1st time
Explain Film radiology
intensifying screens turn xray photons into visible light
visbile light is more efficient at exposing film than xrays
lower exposure = reduce respiratory blur
lower radiation to patient and operator
Advantages = cheap, no technological fauts/risk loosing data, easily portable
Disadvantages = time consuming, physical storage, need a dark room + lots of chemcials
Explain the types of digitised radiography
CR = Computed radiography | DR = Digital radiography |
Use a cassette which is read by a CR reader (big machine) | Directly from plate to computer screen (wired or wireless) |
Advantages
| Advantages
|
Disadvantages
| Disadvantages
|
Both store on CD, DVD, Hard Drives or PACS (Picture Archive Communication System)
Stores as DICOM (Digitial Imaging and Communications in Medicine) files
What are grids?
reduce scattered radiation that reaches the image receptor (film, CR or DR)
grids placed between patient and image receptor - act as a filter
only used when body thickness is >10cm
often made from aluminium and lead (does not absorb photons)
Bucky’s = grids that are fixed to the xray table but can oscillate or vibrate to eliminate grid lines on images
What are the 4 things that effect radiographic quality?
Density
degree of blackness of a film
effected
mAs (increased mAs → more Xrays = black)
double mAs = double film density
time and temperature of film
Contrast
difference in density between the two adjacent areas in film
high contrast = large difference of black vs white → bone
low contrast = small different so mostly grey → soft tissue
primarily affected by kVp → increased kVp = lower contrast
increase kVp by 20% = doubles film density
more Xray photons pass through patient to cassette = more energy and more scatter = less contrast
Definition - sharpness + superimposition
Sharpness = ability to define an edge, dependant on crystal size in screen/film
magnification: increased distance → increases magnification
distortion: unequal magnification of different parts of same object
penumbra effect: blurred edge due to focal spot not aligned
motion: movement whilst taking image
screen: unpreventable light diffusion decreases quality
Superimposition
always take from two views to avoid overlying structures
Scatter
reduces quality of image
increases with = increased patient thickness, kVp and field size (poor collimation)
decreases with = using a grid, decreasing field size (good collimation)
What is a radiographic artifact?
radiographic flaws not normally present on an xray that are produced by artificial means
Examples
motion = blurring, mostly during inspiration/expiration or poor sedation
magnification = object distance from machines which distorts size
distortion = unequal magnification on the same object, poor positioning
foreign object = positioning aids, clips, random objects not relevant
monitoring equipment or legit foreign bodies inside patient don’t count
mal-aligned grid = incorrect position, distance, angling or if upside down
mal-aligned centring/collimation = divergence of beam from anatomy
double exposure / ghosting = only in CR imaging, when not clearing plate between scans which would lead to layered Xray images
Explain Fluoroscopy
uses Xray
“video Xray” = watch images in real time
black and white colours are inverted
often used in theatre using a C-arm = low dose
Advantages | Disadvantages |
|
|
Explain Computed Tomography (CT)
use Xray
cross sectional image of anatomy
CT table goes through gantry (donut), whilst Xrays emitted through
measured in Hounsfield Units (HU)
high HU = white vs low HU = black
tube rotates very quickly at 0.5-1 second/rotation = noisy
allows for continuous data in many planes (axial, sagittal and coronal)
Multi-Planar Reconstructions (MPR)
animals must have GA /very heavy sedation to ensure they are still
can use iodine contrast (IV or oral) due to high xray attenuation (positive contrast) but can cause fatal SE
Advantages | Disadvantages |
|
|
Explain Nuclear Medicine (NM or Scinetigraphy)
use Gamma radiation
high sensitivity but low specificity
used to target an area of interest by injecting a radionuclide bound drug to region → produced gamma photons
patient will continue to emit radiation post procedure, measure half life
keep animals post exam or have limited contact until dose decayed
Advantages | Disadvantages |
|
|
Explain Ultrasound (US)
does not use radiation
uses reflection of soundwaves to form images
piezoelectric crystals in transducer probe produce soundwaves when electric current is applied
transducer identifies echoes to form image
types of images
anechoic (no echo) = fluid filled structure - bladder
hypoechoic (not many echoes) = soft tissue - healthy liver
hyperechoic (many echoes) = solid structure - bone
operator technique and interpretation has a large influence on image quality
ideally need to clip hair and use a gel
often need sedation or GA
Advantages | Disadvantages |
|
|
Explain Magnetic Resonance Imaging (MRI)
does not use radiation
can be open or closed
gold standard for soft tissue imaging
uses very strong magnets - nothing in room!
Hydrogen nuclei exhibits small magnetic properties due to positive proton
hydrogen in water, fat and tissue have different magnetic properties
use large magnetic field and radio frequencies to determine different signals and therefore tissue types
contrast can be used = gadolinium
takes a long time, so need sedation or GA
Advantages | Disadvantages |
|
|