PPN 301 Wk 11: Common childhood illnesses
1/123
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
124 Terms
Nasopharyngitis defined
“Common cold”, Caused by numerous viruses such as , RSV, rhinovirus, adenovirus, influenza, and parainfluenza viruses.
virus not bacteria
4 major defects in tetralogy of fallot
Pulmonary stenosis
Right ventricular Hypertrophy
Overriding aorta
Ventricular septal defect
RSV (respiratory syncytial virus) (Viruses that cause common cold)
virus that causes serious breathing infections, especially in babies.
Most common cause of bronchiolitis in infants and toddlers
If a child is at high risk for serious lung infections, they will need treatment once a month during RSV season – Nov to April
Spread by touching, living on hard objects for more than 6 hours
Treatment is mainly to relieve symptoms
Antibiotics have no effect on viruses, Palivizumab vaccine to prevent RSV from becoming serious
use swab to understand what kind of virus it is
Rhinovirus (Viruses that cause common cold)
the main cause of the common cold
Adenovirus (Viruses that cause common cold)
causes colds, sore throat, bronchitis, or pink eye.
Influenza (Viruses that cause common cold)
Caused by orthomyxoviruses
types A, B, and C
the flu virus, causes fever, body aches, cough, and fatigue.
Clinical manifestations (Influenza)
fever* or feeling feverish/chills.
cough.
sore throat.
runny or stuffy nose.
muscle or body aches.
headaches.
fatigue (tiredness)
Therapeutic management/Nursing care (Influenza)
rest
fluids, like water
medication to reduce any fever or aches
Prevention (influenza)
Yearly vaccination
Parainfluenza (Viruses that cause common cold)
causes croup and other airway infections, especially in young children.
Clinical manifestations (Nasopharyngitis)
Stuffy, runny nose.
Scratchy, tickly throat.
Sneezing.
Watering eyes.
Low-grade fever.
Sore throat.
Mild hacking cough.
Achy muscles and bones.
Therapeutic management and nursing care (Nasopharyngitis)
Treated at home
Promoting comfort
Teach families signs of complications
Types of flu vaccines for children
During the current flu season, CDC recommends annual influenza vaccination during the flu season for everyone 6 months and older with any licensed, age-appropriate flu vaccine.
Injectable influenza vaccines (IIV4)
Live attenuated influenza vaccine (LAIV4)
To create antibodies
Injectable influenza vaccines (IIV4) (types of flu vaccines for children)
are given as an injection (with a needle) and are approved for use in as young people 6 months and older. (Indications vary by vaccine.)
Live attenuated influenza vaccine (LAIV4) (types of flu vaccines for children)
is given as a nasal spray and is approved for use in non-pregnant, healthy people ages 2-49 years old.
Emergency warning signs of the flu (these signs should be reported to medical care immediately)
Fast breathing or trouble breathing (can see grunting as well)
Bluish lips or face
Ribs pulling in with each breath
Chest pain
Severe muscle pain (child refuses to walk)
Dehydration (no urine for 8 hours, dry mouth, no tears when crying)
Not alert or interacting when awake
Seizures (flacid and the child’s eyes would both roll back)
Fever above 104°F
In children less than 12 weeks, any fever
Fever or cough that improve but then return or worsen
Worsening of chronic medical conditions
Acute Otis Media (AOM)
Inflammation or infection located in the middle ear. Otitis media can occur as a result of a cold, sore throat, or respiratory infection.
Etiology/pathophysiology (Acute Otitis Media-AOM)
happen when bacteria or virus infect and trap fluid behind the eardrum, causing pain and swelling/bulging of the eardrum.
Pharmacological Therapeutic management (acute otitis media-AOM)
Antibiotics
Pain-relieving medications
Surgical Therapeutic management (acute otitis media-AOM)
Placement of ear tubes ( Ear tubes are tiny, hollow cylinders that are surgically inserted into the eardrum to enable drainage of the middle ear, allows air to flow into the middle ear and prevents the buildup of fluids behind the eardrum.
Prevention of Acute otitis media-AOM
13-valent conjugate vaccine
Risk factors for acute otitis media
exposure to second hand tobacco smoke
preschool or daycare attendance
bottle feeding
pacifier use
allergies
esophageal reflux
siblings with recurrent ear infections
congenital or acquired autoimmune disease
chromosomal abnormalities
craniofacial abnormalities (i.e cleft palate or down syndrome), which may involve oral-palate and eustachian tube defects that can interfere with normal tube ventilation
lower socioeconomic status. AOM risk may be related to unhealthy diets, poor housing conditions, limited access to medical care
Nursing care (Otitis media)
Relieving pain
Facilitating drainage when possible
Preventing complications or recurrence
Educating the family in care of the child such as:
Positioning. Have the child sit up, raise head on pillows, or lie on unaffected ear.
Heat application. Apply heating pad or a warm hot water bottle.
Healthy diet/fluid intake
Hygiene( hand washing)
Monitoring hearing loss.
Bronchitis
Inflammation of the breathing tubes that causes increased mucus production and narrowing the airway
Bronchitis is caused by:
Viral infection
Bacterial infection
Physical or chemical agents that are breathed in such as dusts, allergens, and strong fumes, including those from chemical cleaning compounds or tobacco smoke.
Acute bronchitis may come after a common cold or other viral infections in the upper respiratory tract.. Pneumonia is a complication that can follow bronchitis.
Bronchitis (Clinical manifestations)
Cough.
Production of mucus (sputum), which can be clear, white, yellowish-gray or green in color — rarely, it may be streaked with blood.
Fatigue.
Shortness of breath.
Slight fever and chills.
Bronchitis nursing care
Avoiding exposure to secondhand smoke
Cough medicine
Humidifying the air
Increased fluid intake
Pain relievers and fever reducers, such as acetaminophen (Tylenol)
Quitting smoking
Avoid antihistamines because they dry up the secretions and can make the cough worse. (NO BENNY)
Asthma
Chronic inflammatory disorder of airways in which the airways narrow and swell and may produce extra mucus(Bronchial hyperresponsiveness) . This can make breathing difficult and trigger coughing, a whistling sound (wheezing) when you breathe out and shortness of breath.
Triggers for asthmatic exacerbations:
Infections like colds and flu.
Allergies – such as to pollen, dust mites, animal fur or feathers.
Exercise and weather.
Smoke, fumes and pollution.
Medicines – particularly anti-inflammatory painkillers like ibuprofen and aspirin.
Emotions, including stress, or laughter.
Asthma (Clinical Manifestations)
Shortness of breath.
Chest tightness or pain.
Wheezing when exhaling, which is a common sign of asthma in children.
Trouble sleeping caused by shortness of breath, coughing or wheezing.
Coughing or wheezing attacks that are worsened by a respiratory virus, such as a cold or the flu.
4 groups of medication (Medication therapy for asthma)
Bronchodilators → opens airway (first line of treatment)
Anti-Inflammatories (Steroidal) → reduce swelling
Leukotriene modifiers → block trigger chemicals
Cromolyn sodium → prevents reactions
Bronchodilators (Medication therapy for asthma)
Opens airway
Anti-inflammatories (steroidal) (Medication therapy for asthma)
Reduce swelling
Leukotriene modifiers (Medication therapy for asthma)
block trigger chemicals
Cromolyn sodium (Medication therapy for asthma)
Prevents reactions
Medication therapy for asthma
Long-term control medications (controllers or preventer medication) such as, Singulair, Flovent, Advair, Pulmicort, Symbicort and QVAR.
Quick-relief medications (reliever medications) such as Albuterol and Ipratropium bromide.
Metered-dose inhaler (MDI)
Corticosteroids (most common)
Cromolyn sodium (is more fast acting)
Albuterol
levalbuterol- commonly inhaled quick relief
terbutaline- can be inhaled injected, sometimes used in emergencies
Long-term bronchodilators
Theophylline: Monitor serum levels
Leukotriene modifiers
Asthma Nursing care
Providing acute asthma care
Long-term asthma care
Avoiding allergens
Relieving bronchospasm
Teaching how to administer medications Supporting the child or adolescent and family
How to use your puffer with a spacer:
Shake the inhaler well before use (3-4 shakes)
Remove the cap from your inhaler, and from your spacer, if it has one
Put the inhaler into the spacer
Breathe out, away from the spacer
Bring the spacer to your mouth, put the mouthpiece between your teeth and close your lips around it
Press the top of your inhaler once
Breathe in very slowly until you have taken a full breath. If you hear a whistle sound, you are breathing in too fast.
Hold your breath for about ten seconds, then breathe out.
If you need to take more than one puff at a time, wait a minimum of 30 seconds between puffs and be sure to shake the puffer (as in step 1) before each puff. Only put one puff of medication into the spacer at a time.
General guidelines for Nursing care/respiratory conditions
Easing respiratory effort
Promoting rest
Promoting comfort
Reducing the spread of infection
Reducing temperature
Promoting hydration
Providing nutrition
Encouraging family support and home care
When parents should be instructed to notify primary healthcare provider if they notice (Emergency warning signs for respiratory complications)
If child is less than 3 months of age:
Is having trouble breathing,
Is not eating or is vomiting, or
Has a fever (temperature of 38.5°C or higher)
In children of all ages (Emergency warning signs for respiratory complications)
Is breathing rapidly or seems to be working hard to breathe
Has blue lips
Is coughing so bad that they are choking or vomiting
Wakes in the morning with one or both eyes stuck shut with dried yellow pus
Is much sleepier than usual, doesn’t want to feed or play, or is very fussy and cannot be comforted
Has thick or coloured (yellow, green) discharge from the nose for more than 10 to 14 days.
Pediatric Gastrointestinal Differences
Mouth is highly vascular
Lower esophageal sphincter muscle tone not fully developed until 1 month of age
Stomach capacity increases with age
Intestinal growth spurts between 1 and 3 years and between 15 and 16 years of age
Children are less able than adults to receive and transform the nutrients given to them as they are born with immature
digestive systems.
Digestive enzymes are not as plentiful and efficient.
Their digestive capacity may be weakened and impaired
due to an early exposure to poor dietary choices and environmental stressors.
The ingestion of incompletely chewed foods places a stress on a child’s digestive and immune systems
Types of dehydration
Isotonic
Hypotonic (diluted)
Hypertonic
Isotonic (types of dehydration)
Water and salt are lost in equal amounts.
Hypotonic (diluted) (dehydration)
Electrolyte deficit exceeds water deficit.
Hypertonic (types of dehydration)
Water loss exceeds electrolyte deficit.
Symptoms of dehydration
dark-colored urine, decreased urination, headaches, fatigue, dry skin, decreased skin turgor.
Therapeutic management of dehydration
Oral fluid therapy , parenteral fluid therapy (oral rehydration solution)
Treat the underlying cause of fluid loss
Diarrhea
loose, watery and possibly more-frequent bowel movements.
Acute diarrhea is a leading cause of illness in children under 5 years of age.
Acute infectious diarrhea (infectious gastroenteritis)
Chronic diarrhea is defined as an increase in stool frequency and increased water content for a duration of more than 14 days
Therapeutic management (Diarrhea)
Assess fluid and electrolytes, rehydrate, maintain fluid therapy, and reintroduction of an adequate diet
Vomiting
Often accompanied by nausea
Therapeutic management of vomiting
Detect and treat cause
Prevent complications(dehydration)
Provide fluids
Antiemetic in some cases
Daily maintenance fluid requirements
1st 10 kg of body weight: 100ml/kg/day
2nd 10kg of bodyweight: 50ml/kg/day
for each kg over 20kg of bodyweight: 20ml/kg/day
maximum: 2000ml for females
maximum: 2500ml for males
Equations (daily maintenance fluid requirements)
Formula method
4/2/1 method
Formula method (Daily maintenance fluid requirements equation)
(100 mL for each of the first 10 kg) + (50 mL for each kg 11–20) + (20 mL for each additional kg)/24 hour
ask for daily use this method
4/2/1 method (Daily maintenance fluid requirements equation)
(4 mL/kg for the first 10 kg) + (2 mL/kg for kg 11–20) + (1 mL/kg for every kg above 20) = hourly rate
Cleft lip or cleft palate
Facial malformations that occur during embryonic development
May appear separately or together
long-term care
Prognosis
Therapeutic management of cleft lip or cleft palate
Surgical correction of cleft lip
Surgical correction of cleft palate
Nursing care of cleft lip or cleft palate
Feeding
Pre-operative care
Post-operative care
Prognosis defined
a prediction of how a disease or condition will progress and the chances of recovery.
Variations in cleft of lip and palate at birth
Notch in vermillion border
Unilateral cleft lip and cleft palate
Bilateral cleft lip and cleft palate
cleft palate
Notch in vermillion border (Variations in cleft of lip and palate at birth)

Unilateral cleft lip and cleft palate (Variations in cleft of lip and palate at birth)
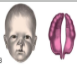
Bilateral cleft lip and cleft palate (Variations in cleft of lip and palate at birth)
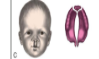
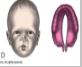
Cleft palate (Variations in cleft of lip and palate at birth)
Breast-feeding (how do I feed my baby with cleft lip?)
During breast-feeding, the soft breast tissue often will fill the opening
in the lip and/or gum line. This seals off the mouth and lets your baby create enough suction.
Sometimes it helps to hold a finger across the cleft while your baby feeds.
Swallowing noises and normal weight gain are signs that breast-feeding is going well.
If your baby is "noisy" with feeding, making clicking or kissing noises, they may not have enough suction.
Bottle-feeding (How do I feed my baby with cleft lip?)
If you bottle-feed your baby, feeding may work better using special bottles or nipples with a wider base.
When starting a feeding, hold your baby in a slightly upright position.
Touch the baby's lower lip with the nipple.
When the baby latches on, direct the nipple slightly downwards.
Try to keep the nipple in the center of the baby's mouth. Do not let it slip up into the cleft.
Juvenile (Type 1 diabetes
Autoimmune condition, pancreas cannot produce any insulin
Exact cause unknown
If untreated/undetected can lead to ketoacidosis
Diagnosis: high blood sugar level symptoms & fasting blood sugar reading of at least 7.0mmol/L or 11mmol/L at any time of day
Early symptoms (Juvenile type 1 diabetes)
Polyuria
polydipsia- increased thirst
Feeling tired or weak
yeast infection
increase in appetite
dry mouth or throat
unexplained weight loss
Advanced symptoms (Juvenile type 1 diabetes)
These symptoms appear if diabetes is not treated, or in some cases when it is undiagnosed
stomach aches
feeling drowsy
nausea and vomiting
kussmaul breathing- heavy, rapid breathing
Management of Juvenile type 1 diabetes
Diet & Exercise
Insulin injections
Monitoring
Hyperglycemia symptoms
fatigue
polyuria
polydipsia- excessive thirst
blurry vison
irritability
Hypoglycemia symptoms
fatigue
paleness
irritability
increased hunger
blurry vision
sweatiness
headache
dizziness
shakiness
Cerebral palsy (CP)
A group of disorders of movement, muscle tone and posture associated with activity limitations and attributed to nonprogressive, permanent injury or malformation of the developing fetal, infant or young child’s brain
Most common permanent physical disability in childhood
A significant number of children with CP will also have epilepsy
Prenatal brain abnormalities (Cerebral palsy-CP)
Gross abnormalities of the brain - Brain is formed incorrectly
Vascular occlusion - blood cannot reach the brain
Laminar(brains layered structure) degeneration - Brain cells die in layers
Effects of low birth weight
Anoxia
Hypoxic infarction or hemorrhage
Six attributes that require investigation (cerebral palsy-cp)
Early handedness- use of one hand over the other in a child under 12 months
Stiffness or tightness in the legs between 6 and 12 months
Persistent fisting of the hands in children over 4 months
Persistent head-lag( weak neck muscles can’t support head) in a child over 4 months
Inability to sit without support in child over 9 months
Any asymmetry in posture or movement
Therapeutic management (Cerebral palsy)
Rehabilitation
Pharmacological
Neurosurgical
Orthopedic
Dental hygiene
Neuromuscular electrical stimulation (NMES)
Rehabilitation (Therapeutic management-cerebral palsy)
Physical, occupational & speech-language therapy
Pharmacological (Therapeutic management-cerebral palsy)
To treat pain related to spasms and seizures
Botulinum toxin A injections (BoNT-A) is effective for reducing over-activity in muscles in children with cerebral palsy. This results in a reduction in muscle strength and muscle tone with small, short-lived gains in aspects of gait and function
Duchenne muscular dystrophy
Also called pseudohypertrophic muscular dystrophy
Most severe and most common of muscular dystrophy in childhood
X-linked inheritance pattern; one third are fresh mutations (i.e not caused by inheritance)
Incidence: 1 in 3600 male births
Early onset, usually between 2 and 5 years of age (Duchenne muscular dystrophy)
Progressive muscular weakness, wasting, and contractures (becomes permanently stiff)
Calf muscle hypertrophy in most patients
Loss of independent ambulation by 12 years of age
Slowly progressive, generalized weakness during teenage years
Relentless progression until death from respiratory or cardiac failure
Symptoms of Duchenne Muscular dystrophy
Waddling gait
Lordosis
Frequent falls
Gower sign (child turning onto side or abdomen, flexing knees to assume a kneeling position, then with knees extended gradually pushing torso to an upright position by “walking” the hands up the legs)
Enlarged muscles (especially thighs and upper arms); feel unusually firm or woody on palpation
Cognitive impairment-Later stages: Profound muscular atrophy (Duchenne Muscular Dystrophy)
Mild (about 20 IQ points below normal)
IQ <70 present in 25 to 30% of patients
Complications -Later stages: Profound muscular atrophy (Duchenne Muscular Dystrophy)
Contracture deformities of hips, knees, and ankles
Scoliosis
Risk of fractures
Respiratory and cardiac compromise
Obesity
Nursing care (Duchenne muscular dystrophy)
Help child and family cope with chronic, progressive, incapacitating disease
Design program to foster independence and activity for as long as possible
Teach child self-help skills
Appropriate health care assistance as child’s needs intensify (e.g., home health, skilled nursing facility, respite care for family)
Often live into adulthood
Congenital heart disease (CHD)
Incidence: 12 per 1000 live births
CHD is a major cause of death in the first year of life (after prematurity).
Critical congenital heart disease (CCHD) is more severe and usually requires intervention early in life
The most common anomaly is ventricular septal defect (VSD).
Atrial septal defect (ASD)
Altered hemodynamics (congenital heart disease)
Two types
Acyanotic
Cyanotic
Acyanotic (Altered hemodynamics- congenital heart disease)
increased pulmonary blood flow
atrial septal defect, ventricular septal defect, patent ductus arteriosus, atrioventricular canal defect
obstruction to blood flow from ventricles
Coarction of aorta, aortic stenosis, pulmonic stenosis
blood has oxygen so baby does not turn blue
Cyanotic (Altered hemodynamics- congenital heart disease)
decreased pulmonary blood flow
tetralogy of fallout
tricuspid atresia
mixed blood flow
Transposition of great arteries, toral anomalous pulmonary venus return, truncus arteriosus, Hypoplastic left heart syndrome
Oxygen in blood is poor so baby turns blue
Defects with increased pulmonary blood flow (common in)
Atrial septal defect (ASD)
Ventricular septal defect (VSD)
Patent ductus arteriosus (PDA)
Defects with increased pulmonary blood flow
Abnormal connection between two sides of heart
Increased blood volume on right side of heart
Increased pulmonary blood flow
Decreased systemic blood flow
In a healthy heart, the wall that separates the right and left chambers (the septum) prevents non-oxygenated blood from mixing with oxygenated blood. A septal defect allows blood to flow back and forth between the right and left sides of the heart.
“When there’s a hole in the heart, either at the atrial or ventricular level, the heart just can’t work efficiently,”. The lungs end up getting too much oxygen-rich blood. This makes both the heart and lungs work harder. The surgical treatment for atrial septal defect (ASDs) and ventricular septal defect (VSDs) is open-heart surgery.
Most common in (Defects with decreased pulmonary blood flow)
tetralogy of Fallot and tricuspid atresa
Tetralogy of fallot (Defects with decreased pulmonary blood flow)
Pressure on right side increases, greater than left-sided pressure which result in desaturated blood in left side of heart and in systemic circulation
Tetralogy of fallout includes four defects (defects with decreased pulmonary blood flow
Narrowing of the lung valve (pulmonary valve stenosis).
A hole between the bottom heart chambers (ventricular septal defect).
Shifting of the body's main artery (aorta).
Thickening of the right lower heart chamber (right ventricular hypertrophy).
Nursing care of family (Congenital heart disease)
Helping the family adjust to the disorder.
Educating the family about the disorder.
Helping the family manage the illness at home.
Preparing the child and family for invasive procedures.
Providing postoperative care:
Observing vital signs
Maintaining respiratory status
monitoring fluids
providing rest and progressive activity
providing comfort and emotional support
Plan for discharge and home care (Congenital heart disease)
Children need at least 3 or 4 more weeks at home and recovery may take 6 to 8 weeks.
child should not do any activity that could result in a fall or a blow to the chest.
keep the child from crying for too long for the first 3 to 4 weeks.
Do not pull or lift the child by the arms or from their armpit area.
Limit feeding time to around 30 minutes, add extra calories to formula if it is necessary.
Check the wound for signs of infection, such as redness, swelling, tenderness, warmth, or drainage.
Call the doctor if the child has fever, nausea, or vomiting, chest pain, redness, swelling, or drainage from the wound, Difficulty breathing or shortness of breath, Puffy eyes or face, bluish or grayish skin, dizziness, fainting, or heart palpitations, and feeding problems or reduced appetite
Preoperative preparation for children
Postoperative preparation for children
Sickle cell disease
Sickle cell disease (SCD) is a group of inherited red blood cell disorders
In SCD, the hemoglobin is abnormal causing the red blood cells to become hard and sticky and appear crescent or sickle-shaped
Sickle or crescent cells die early causing a constant reduction in the number of red blood cells.
Sickle or crescent cells, when they travel through small blood vessels, clump together clogging blood flow and depriving organs of blood and oxygen
Causing severe pain associated with sickle cell crisis
Damage nerves and organs,
Infection, acute chest syndrome, and stroke.
Sickle cell genotypes influence complication risks and potential disease severity
HbA (sickle cell)
Normal adult hemoglobin.