Skin Integrity: Burns, Laceration, Pressure Ulcers, and Stasis Dermatitis
1/35
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
36 Terms
Burns
injury to the skin caused by traumatic injuries to the skin or other tissues primarily caused by thermal or other acute exposure
-all or some of the cells in the skin or other tissues are destroyed by heat, electrical discharge, or radiation
depth
Burns are classified by ______
First-Degree (Superficial)
burns that involve only the dermis
-painful, dry, red burn that blanches with pressure WITHOUT blister formation
-typically heal in 1 week
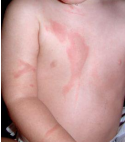
Second-Degree (partial thickness)
burns involving the epidermis / portion of the dermis
-can be superficial or deep
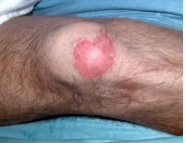
blanches, with, 24, normal
Superficial partial thickness burns can be defined as painful, red, and weeping burns that _________ with pressure _____ blister formation within __ hours
-capillary refill is ________, less than 2 seconds
follicles, nonblanching, blister, absent
Deep partial thickness burns damage hair ________ and glandular tissue. They are painful and _____________ to pressure, almost always ______ (easily unroofed), wet/waxy/dry and variable mottle colorization of cheesy white-red
-Cap refill is _________, limited pain
-3+ weeks to heal
Third Degree (Full thickness)
burns that extend through and destroy all layers of the dermis and often injure subcutaneous tissue
-waxy white/leathery gray/charred-black skin that is dry, inelastic and does NOT blanch with pressure
-Eschar is usually intact
-painless, need surgery
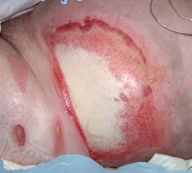
Fourth degree (Extension to deep tissue)
deep and potentially life-threatening burns that extend through skin into soft tissues and can involve muscle or bone
-hemodynamically unstable
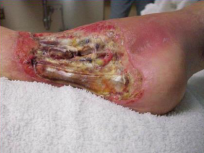
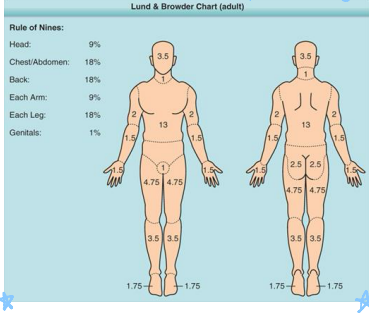
Lund-Browder
most accurate way to estimate burn injury
-uses Lund-Browder chart
-cannot use if the patient has first degree burns
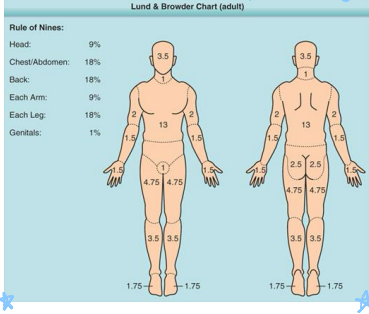
Rules of Nines
another method of estimating burn injury that assigns 9% or 18% to different areas of the body
-head and each arm = 9%
-each leg / anterior trunk / posterior trunk = 18%
severity, PCP, ED, hospital, burn
Treating Burn Injuries
-Estimate _______ of injury: use mechanism of injury, burn depth, extend and anatomic location
-Mild/minor burn injury: treated by ___ or outpatient in __. Partial thickness burns < 10% TBSA in patients 10-50 years or <5% TBSA in patients <10 years or >50 years
-Moderate burn injury: require admission to ________ but not to burn center
-Severe burn injury: referred to and treated at designated ____ center
>, face, genitalia, 3rd, chemical, co-morbid
When to Refer for Burns
-Partial thickness burns _ 10% of TBSA
-Any burn involving the ____, hands, feet, ________, perineum, or major joints
-Any ___ degree burn, size does not matter
-Circumferential burns, which are burns that goes all away around their affected body parts
-Electrical and _______ burns, including lightning
-Burn + trauma
-Burn injury in patient with __-______ conditions or conditions that could complicate management: diabetes, medications, immunosuppressive drugs
remove, cooling, dressing, NSAIDs, management, referral
Treatment for Minor Burns
-________ clothing and debris
-_________, cleansing the area (wound debridement if needed), skin/wound ___________ (dry, nonstick gauze only)
-Pain management using ________. Be sure to avoid aspirin and topical lidocaine
-Tetanus prophylaxis
-Wound ___________, monitor for infection, follow up visits for wound checks/management, _________ to burn center
burn, airway, tetanus, prophylaxis, CBC, fluids
Treatment for Moderate-Severe Burns
-Admission to ED or _______ center
-Trauma management: _________ management, fluid resuscitation, pain management, _______ immunization, topical antibiotics for infection __________
-Obtain ___, electrolytes, urinalysis, and myoglobin
-________ are mainstay: Parkland 4mL/kg per percent of TBSA, give ½ over hours 0-8 and second half over hours 8-16
lacerations, NOT, head, infection, cosmetically
Epidemiology and Etiology of Lacerations
-Minor wounds are considered ___________ that do ___ involve joints, nerves, flexor tendons or underlying structures. Be sure to consult a specialist if the wound is complicated
-Most wounds occur in children on the _____ and most mechanism of action is blunt force
-Goal of treatment is to prevent ________ and achievement of a functional scar that is ___________ acceptable
5, comorbid, 12-18, facial, 24-72, increase, scarring, 24, infected, puncture
Clinical Presentation and Evaluation of Lacerations
-Simple lacerations <_cm, without contamination, not on lower extremities in patient without _______ condition: repaired __-__ hours after injury. Just ask the patient when they hurt themselves.
-______ lacerations without risk factors for infection can be closed __-__ hours after injury. The face is well vascularized, so the risk of infection is quite low.
-Contraindications: if suturing will significantly ________ risk of wound infection, superficial wounds expected to hear without _________, dog/cat/human bites, wounds (other than facial) > __ hours old, lacerations with significant tissue loss, laceration through __________ skin, deep _______ wounds or anything grossly contaminated
FB, delayed, trauma, diabetes, steroids, complex, neurovascular, fracture, eyelid, ear
Evaluation and Referrals for Lacerations
Risks of Poor Outcomes:
-Wound related: retained __, heavy contamination, ________ presentation, deep wounds with tissue ______, wounds caused by glass/ice
-Patient related: __________, obesity, peripheral arterial disease, malnutrition, renal failure, use of _______, tendency to form keloids, connective tissue disorder
When to refer to plastics or a specialist
-Large/________ laceration, severe contamination, _________ compromise, laceration + __________/amputation/joint penetration
-Anatomic location of nasal cartilage/ala/columella, __________ or orbital lacerations that involve eyelid margin or tarsal plate, ___ lacerations
primary, 12-18, secondary, 24, delayed, uncomplicated, human, insufficiently, co-morbid
Type of Closure
________ closure
-Indicated for clean wounds caused by sharp objects within __-__ hours of injury
_________ closure
-Deep stab or puncture wounds that cannot be adequately irrigated, contaminated wounds, abscess cavities, >__ hours after injury or non-cosmetic animal bites
_________ primary closure
-___________ wounds that present after safe period for primary closure
-Animal and _______ bites to soft tissue, wounds > 24 hours that were __________ cleansed/debrided/or decontaminated, wounds > 24 hours in patients with ___-______ conditions
debridement, extent, anesthesia, epinephrine
Laceration Treatment
Prior to closure:
-Hemostasis, wound ___________, hair removal, wound irrigation, tetanus immunization, determine ______ of wound, evaluate for retained foreign body, _________ if indicated, and no ____________ on nose or penis
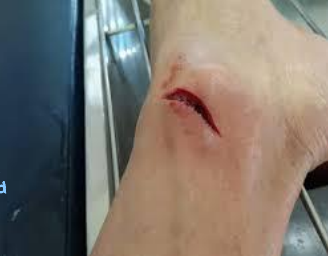
Steri-strips
used to treat linear, low tension lacerations, skin tears, flaps in patients with fragile skin
-avoid in kids because they will rip them off

Dermabond
use to treat linear wounds with low tension, skin tears, facial wounds in children, flaps in patients
Sutures
used to treat any laceration through the dermis that will cause scarring if wound edges not properly opposed
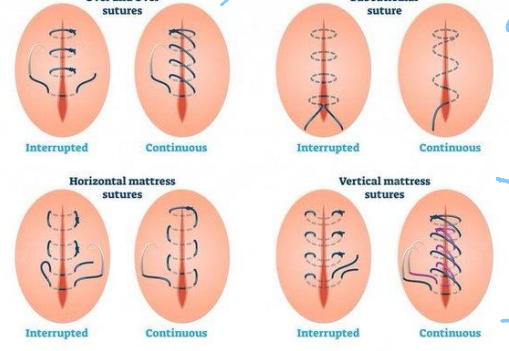
Staples
used to treat scalp wounds, wounds in non-cosmetic areas especially long, linear lacerations

absorbable, face, trunk, tension, larger, analgesia, evaluation, sutures
Treatment of Lacerations
-__________ sutures should be used for subcutaneous tissues and for patients not willing/able to follow up. Non-absorbable sutures can also be used at your discretion.
-Suture size: use 6-0 or 5-0 on the ____, 4-0 or 5-0 on the scalp/_____/extremities/palm/sole/oral mucosa, 3-0 or 4-0 on the trunk/extremities/wounds under _______ near or on a joint/tongue
-The smaller the number, the _______ the suture
-Laceration repair procedure: local ________, wound irrigation and thorough _______, repair with ________, wound dressing
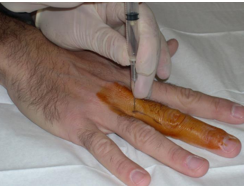
infection, antibiotics, 5, 8-10
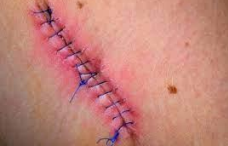
Treatment and Aftercare for Lacerations
-Monitor wound signs of ________ after repair: follow up in 2-3 days for a wound check and follow up after wound check for suture removal and in cases of concerns for infection
-Prophylaxis for oral _________ indicated: animal/human bites, intraoral lacerations, nailbed injuries, and excessive wound contamination
-Suture removal: face/eyelids/neck = _ days, scalp = 7-10 days, trunk/upper extremities = 7 days, lower extremities = _-__ days, digits/palm/sole = 10-14 days
Pressure Ulcer
localized areas of damage to skin and/or underlying tissue due to pressure or pressure in combination with shear
-caused by constant pressure in one area due to lack of movement
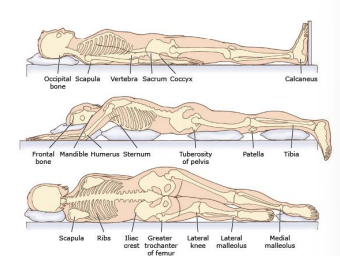
Stage 1
______ _ pressure ulcer involves intact skin with a localized area of non blanchable erythema
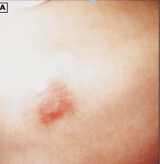
Stage 2
_____ _ pressure ulcers involve partial-thickness loss of skin with exposed dermis. The wound bed is visible, pink or red, moist and may also present as an intact or ruptured serum-filled blister
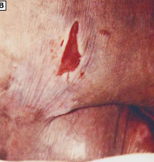
Stage 3
_____ _ pressure ulcers involve a full-thickness loss of skin with visible adipose in the ulcer and granulation tissue and epibole (rolled/curled wound edge) often present. Slough and eschar may be present
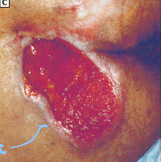
Stage 4
_____ _ pressure ulcers involve full-thickness skin and tissue loss with exposed or directly palpable fascia, muscle, tendon, ligament, cartilage, or bone in the ulcer.
-Slough/eschar may be visible, epibole, undermining, tunneling often occur
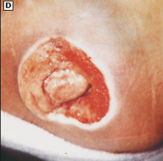
Unstageable
full-thickness skin and tissue loss in which extent of tissue damage within the ulcer cannot be confirmed due to presence of slough/eschar
Redistribution, film, moving, moist, debridement
Treatment of Pressure Ulcers
-Pressure ___________ is the hallmark treatment
-Stage I: cover with transparent _____ for protection, preventative measure to prevent worsening of injury should be implemented like keeping the patient ________ and consulting wound care
-Stage II: dressing that requires a _______ wound environment +/- debridement
-Stage III/IV: ___________ of necrotic tissue and coverage with appropriate dressings and possibly treatment of infection
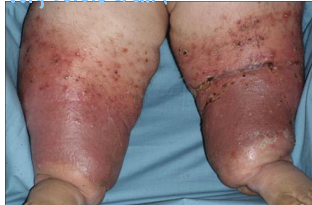
Stasis Dermatitis
common inflammatory dermatosis of the lower extremities associated with chronic venous insufficiency
-RF: age, family hx, female sex, standing occupation, obesity, family hx of DVT
valves, flow, pressure
Pathophysiology of Stasis Dermatitis
-Dysfunction of the venous ______
-Obstruction to the venous ____
-Failure of the venous pump causing a high _________ system and ultimately venous HTN
leg, medial, scaling, edematous, lichenification, bilateral, clinical
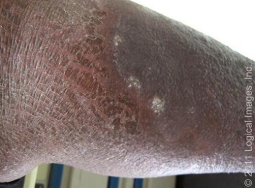
Clinical Presentation and Diagnosis of Stasis Dermatitis
-Physical Exam: find mostly in the lower ___ with an ulcer on the ______ malleolus. You will also see erythematous, _______, and eczematous patches or plaques on chronically ________ legs. There may be hyperpigmentation, ____________, varicosities, secondary lymphedema, atrophie blanche, secondary cellulitis, ulceration, usually _________
-Diagnosis: ________ or biopsy if diagnosis is unclear or to rule out other possible diagnoses
symptomatic, education, elevation, weight, compression, corticosteroids
Treatment of Stasis Dermatitis
-Underlying Chronic Venous Insufficiency: __________ treatment of skin dryness/pruritus/inflammation, prevention of ulceration, and patient ___________
-Treatment of venous HTN: leg _______, daily walking, exercise, ______ reduction, avoid local trauma, _________ therapy, systemic therapy, ablation therapy
-Treatment of acute stasis dermatitis: topical _____________, wet dressing, compression bandages