Skeletal Muscle: Structure, Function, and Contraction Mechanics
1/567
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
568 Terms
What are the four functional characteristics of skeletal muscle?
Excitability, contractility, extensibility, and elasticity.
What is the hierarchical organization of skeletal muscle from whole muscle to fiber?
Whole muscle is surrounded by epimysium, composed of fascicles wrapped in perimysium, which contain muscle fibers enclosed by endomysium.
What are the primary regulatory proteins found in a sarcomere?
Troponin and tropomyosin.
What is the role of the sarcoplasmic reticulum in muscle contraction?
It stores and releases calcium ions upon stimulation.
What triggers the release of calcium from the sarcoplasmic reticulum?
An action potential traveling along the sarcolemma and down the T-tubules.
What is the sliding filament mechanism?
The process where actin and myosin filaments slide past each other to shorten the sarcomere without the filaments themselves shortening.
What are the components of a myosin molecule?
A long tail and two globular heads containing ATP-binding and actin-binding sites.
What is the function of myosin heads during contraction?
They convert chemical energy (ATP) into mechanical force by pivoting in a power stroke.
What are the components of thin (actin) filaments?
Globular actin (G-actin) subunits, tropomyosin, and troponin.
What is the function of tropomyosin at rest?
It blocks the myosin-binding sites on actin, preventing cross-bridge formation.
What happens when calcium binds to troponin?
Troponin undergoes a conformational change that moves tropomyosin, exposing myosin-binding sites on actin.
What is a cross-bridge?
The physical connection formed when an energized myosin head attaches to an actin filament.
What occurs during the power stroke?
The myosin head releases Pi and ADP, pivoting to pull the actin filament toward the center of the sarcomere.
What causes a myosin head to detach from actin?
The binding of a new ATP molecule.
How is the myosin head re-energized for another cycle?
Through the hydrolysis of ATP into ADP and Pi, which re-***** the head into its high-energy position.
What are T-tubules?
Inward extensions of the sarcolemma that allow electrical signals to reach the interior of the muscle fiber.
What is the role of lateral sacs (terminal cisternae) in muscle contraction?
They store calcium ions and release them into the cytoplasm when triggered by an action potential.
What is a motor unit?
A single motor neuron and all the muscle fibers it innervates.
How does the size of a motor unit relate to muscle function?
Smaller motor units (fewer fibers) allow for fine, precise control, while larger motor units are used for gross movements.
What defines the A band in a sarcomere?
The region containing myosin filaments.
What defines the I band in a sarcomere?
The region containing actin filaments anchored to the Z discs.
What is the primary neurotransmitter at the neuromuscular junction?
Acetylcholine.
What is the definition of a muscle fiber?
A long, multi-nucleated cell containing myofibrils.
What is the functional unit of contraction in a muscle fiber?
The sarcomere.
What happens to the sarcomere length during contraction?
It shortens as actin and myosin filaments slide past each other.
Why is skeletal muscle considered 'striated'?
Because of the ordered arrangement of filaments in the cell cytoplasm.
How does the number of muscle fibers in a motor unit affect muscle function?
The number of fibers is directly related to functional demands; fewer fibers provide precise control, while larger motor units with thousands of fibers generate greater force.
Why is ATP essential for skeletal muscle contraction?
ATP powers the cross-bridge cycle, allows myosin to detach from actin, re-energizes the myosin head, and powers calcium pumps for muscle relaxation.
What happens if ATP is absent in skeletal muscle?
Myosin remains tightly bound to actin, resulting in muscle rigidity, as seen in rigor mortis.
What is the length-tension relationship in skeletal muscle?
It describes how the force a muscle fiber produces depends on the degree of overlap between thick and thin filaments before contraction.
Why is force reduced at very short muscle lengths?
Excessive overlap of actin filaments and myosin pressing against Z-discs interferes with effective cross-bridge formation.
What is the optimal length for skeletal muscle contraction?
The length where there is ideal overlap between actin and myosin, allowing the maximum number of cross-bridges to form.
What happens to muscle force when a muscle is stretched beyond its optimal length?
Overlap between actin and myosin decreases, fewer cross-bridges form, and force production declines.
What is excitation-contraction coupling?
The process by which an action potential along the sarcolemma triggers calcium release from the sarcoplasmic reticulum, leading to muscle contraction.
What is the latency period in skeletal muscle contraction?
The short delay between the action potential and the start of contraction, during which calcium is released and binds to troponin.
How does the load-velocity relationship describe muscle shortening?
It is an inverse relationship: as the load on a muscle increases, the velocity of shortening decreases.
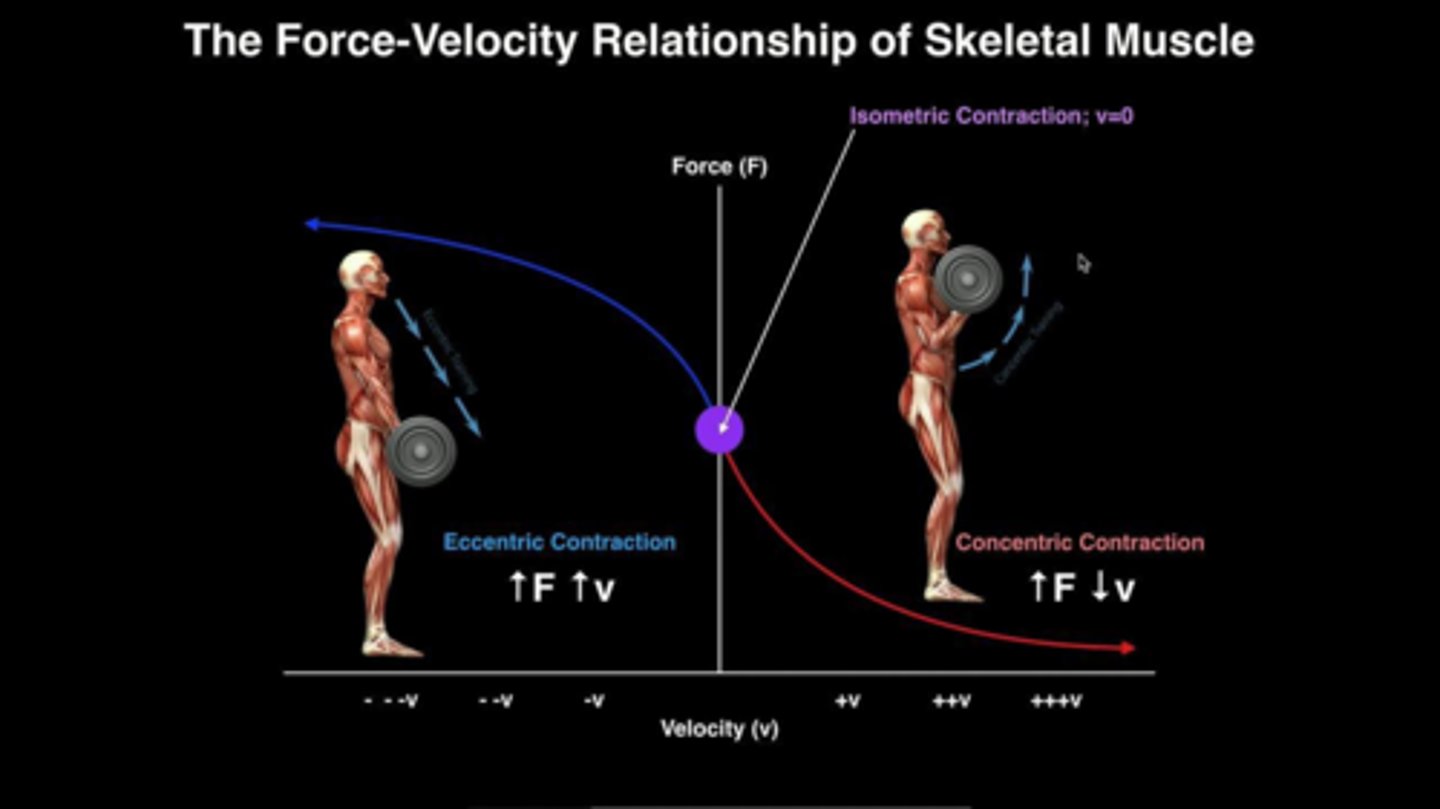
What occurs during an isometric contraction in terms of load and velocity?
The load equals the muscle's maximum force-producing capacity, resulting in zero velocity of shortening.
What is an eccentric contraction?
A contraction where the load exceeds the muscle's maximum force, causing the muscle to lengthen while active.
What is recruitment in skeletal muscle?
The process of increasing contraction strength by activating more motor units.
What is the size principle of motor unit recruitment?
Smaller motor units are recruited first, followed by larger ones as force demands increase.
What are the three metabolic pathways for ATP production in skeletal muscle?
The phosphagen (ATP-PC) system, anaerobic glycolysis, and aerobic respiration.
Which ATP pathway provides immediate energy for high-intensity activity?
The phosphagen (ATP-PC) system, using stored creatine phosphate.
What is the primary byproduct of anaerobic glycolysis?
Lactic acid.
Which metabolic pathway supports long-duration, lower-intensity activities?
Aerobic respiration.
What are the characteristics of Type I (slow oxidative) muscle fibers?
They contract slowly, generate less force, are highly fatigue-resistant, and rely on aerobic respiration.
What are the characteristics of Type IIa (fast oxidative-glycolytic) muscle fibers?
They contract quickly, produce more force than Type I, have moderate fatigue resistance, and use both aerobic and anaerobic pathways.
What are the characteristics of Type IIx (fast glycolytic) muscle fibers?
They contract very rapidly, generate the greatest force, fatigue quickly, and rely mainly on anaerobic glycolysis.
What is temporal (wave) summation?
The process where a single motor unit is stimulated repeatedly in rapid succession, causing twitches to add together and increase tension.
What is tetanus in skeletal muscle?
A sustained and maximal contraction resulting from very rapid temporal summation.
What is motor unit summation?
The process of increasing total muscle force by activating additional motor units.
What role does myoglobin play in Type I fibers?
It stores oxygen and contributes to the red color of the fibers, supporting aerobic metabolism.
How does calcium removal lead to muscle relaxation?
Calcium pumps (Ca²⁺-ATPase) transport calcium back into the sarcoplasmic reticulum, allowing tropomyosin to cover actin binding sites.
What is motor unit recruitment?
The process of activating additional motor units to increase muscle force.
What is the size principle in motor unit recruitment?
Small motor units are recruited first, followed by larger motor units as more force is required.
How do temporal summation and recruitment differ in increasing muscle force?
Temporal summation increases force by increasing stimulation frequency, while recruitment increases force by activating more muscle fibers.
How does exercise stimulate muscle hypertrophy?
Exercise causes mechanical stress and damage, activating satellite cells and increasing protein synthesis, which leads to thicker and stronger muscle fibers.
Does hypertrophy increase the number of muscle fibers in humans?
No, hypertrophy enlarges existing fibers; hyperplasia (increasing the number of fibers) is rare in humans.
What does Ca2+ bind to in skeletal muscle to initiate contraction?
Ca2+ binds to troponin on the actin filament.
What does Ca2+ bind to in smooth muscle to initiate contraction?
Ca2+ binds to calmodulin in the cytoplasm.
What is the role of myosin light-chain kinase (MLCK) in smooth muscle?
It is activated by the Ca2+-calmodulin complex and phosphorylates myosin heads to allow binding to actin.
What is the primary anatomical difference between smooth and skeletal muscle cells?
Smooth muscle cells are small, spindle-shaped, and uninucleated, while skeletal muscle fibers are long, cylindrical, and multinucleated.
Why does smooth muscle lack striations?
Because its actin and myosin filaments are not arranged into organized sarcomeres.
What structures in smooth muscle function similarly to Z-discs in skeletal muscle?
Dense bodies.
What structures do smooth muscle cells use instead of T-tubules to regulate calcium entry?
Caveolae.
What are 'slow waves' in smooth muscle?
Rhythmic fluctuations in membrane potential that oscillate between partial depolarization and repolarization.
What happens when a slow wave reaches the threshold potential?
Voltage-gated calcium channels open, allowing calcium entry, which triggers contraction.
Why is smooth muscle contraction slower than skeletal muscle contraction?
Calcium entry is more gradual, cross-bridge cycling is slower, and contraction depends on the slower process of myosin phosphorylation.
What is the 'latch state' in smooth muscle?
A state where smooth muscle maintains tension for long periods using less ATP.
How does the parasympathetic nervous system generally affect smooth muscle in the digestive tract?
It promotes contraction, increasing motility.
How does the sympathetic nervous system generally affect smooth muscle in the digestive tract?
It promotes relaxation, decreasing motility.
What is smooth muscle tone?
A constant, partial state of contraction maintained even without active stimulation.
What factors contribute to the maintenance of smooth muscle tone?
Spontaneous slow waves, continuous low-level calcium entry, and ongoing autonomic nervous system activity.
What is the functional importance of smooth muscle tone?
It helps maintain the normal function, shape, and pressure of hollow organs and blood vessels.
What is the main structural difference between the left and right ventricles?
The thickness of their walls.
What is the primary contractile protein in the thin filament of skeletal muscle?
Actin.
What is the primary contractile protein in the thick filament?
Myosin.
Where is calcium stored in skeletal muscle?
The sarcoplasmic reticulum.
What is the effect of tropomyosin movement in skeletal muscle contraction?
It moves away from myosin-binding sites on actin, allowing cross-bridge formation.
Why is the left ventricle wall thicker than the right ventricle wall?
The left ventricle must generate higher pressure to pump blood through the high-resistance systemic circulation, whereas the right ventricle pumps into the low-resistance pulmonary circuit.
Why is the sinoatrial (SA) node the heart's primary pacemaker?
It has the fastest rate of spontaneous depolarization, allowing it to reach threshold first and set the rhythm for the entire heart.
What is an ectopic pacemaker?
An area of the heart other than the SA node (such as the AV node or Purkinje fibers) that takes over as the pacemaker if the SA node is damaged or suppressed.
What are the three steps of a nodal cell pacemaker potential?
First, 'funny' sodium channels open causing slow depolarization; second, T-type calcium channels open; third, L-type calcium channels open at threshold to cause the action potential upstroke.
What ion is responsible for the upstroke of the action potential in nodal cells?
Calcium (via L-type calcium channels).
What ion is responsible for the upstroke of the action potential in ventricular myocardial cells?
Sodium (via fast voltage-gated sodium channels).
What is the function of the plateau phase (Phase 2) in a ventricular myocardial action potential?
It maintains a stable membrane potential via calcium influx, allowing for calcium-induced calcium release and sustained contraction.
How does the Purkinje system improve cardiac pumping efficiency?
It rapidly conducts electrical impulses throughout the ventricles, ensuring synchronized contraction from the apex upward.
What does the P wave represent on an ECG?
Atrial depolarization.
What does the QRS complex represent on an ECG?
Ventricular depolarization.
What does the T wave represent on an ECG?
Ventricular repolarization.
Why do AV valves require chordae tendineae and papillary muscles?
To prevent the valve leaflets from inverting or prolapsing into the atria during the high-pressure environment of ventricular contraction.
How do semilunar valves differ structurally from AV valves?
They consist of three cup-shaped cusps and lack chordae tendineae or papillary muscles, relying on blood pressure to fill the cusps and seal the valve.
What causes the first heart sound (S1)?
The closure of the atrioventricular (AV) valves at the beginning of ventricular systole.
What causes the second heart sound (S2)?
The closure of the semilunar valves at the beginning of ventricular diastole.
What are the four primary factors that influence venous return?
Pressure gradients, the skeletal muscle pump, the respiratory pump, and venous tone (sympathetic stimulation).
How does the respiratory pump assist venous return?
During inhalation, the diaphragm descends, decreasing thoracic pressure and increasing abdominal pressure, which draws blood toward the heart.
What is the effect of sympathetic stimulation on venous return?
It causes venoconstriction, which reduces venous capacity and pushes more blood toward the heart.
What is the resting membrane potential of a ventricular myocardial cell?
Approximately -90 mV.
What happens during Phase 1 of the ventricular myocardial action potential?
Sodium channels inactivate and a brief outward movement of potassium causes slight repolarization.
What is the primary role of the skeletal muscle pump in circulation?
Contracting muscles compress nearby veins, pushing blood toward the heart while one-way valves prevent backflow.
What is the significance of the long refractory period in ventricular myocardial cells?
It prevents tetanus and ensures the heart has time to relax and fill with blood between contractions.