INB 446L Test 4
1/61
Earn XP
Description and Tags
Cardiovascular, Immune + Lymph, GI
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
62 Terms
Cardiovascular System Overview
Transports blood, nutrients, oxygen, and waste throughout the body.
consists of heart, blood vessels (arteries, veins, capillaries), and lymphatic system.
plays a key role in maintaining homeostasis and immune function
Pulmonary Circulation
Right heart → lungs → left heart
carries deoxygenated blood from right ventricle to lungs for oxygenation
Systemic Circulation
Left heart → Body → Right heart
delivers oxygenated blood from left ventricle to body and returns deoxygenated blood to heart
Portal Circulatory Systems
Blood travels through 2 capillary beds before returning to heart
venous portal systems:
Hepatic portal system carries blood from intestines to liver
hypophyseal portal system connects hypothalamus and anterior pituitary gland
Arterial portal system includes efferent arteriole in kidney that carries blood between two capillary networks in nephrons
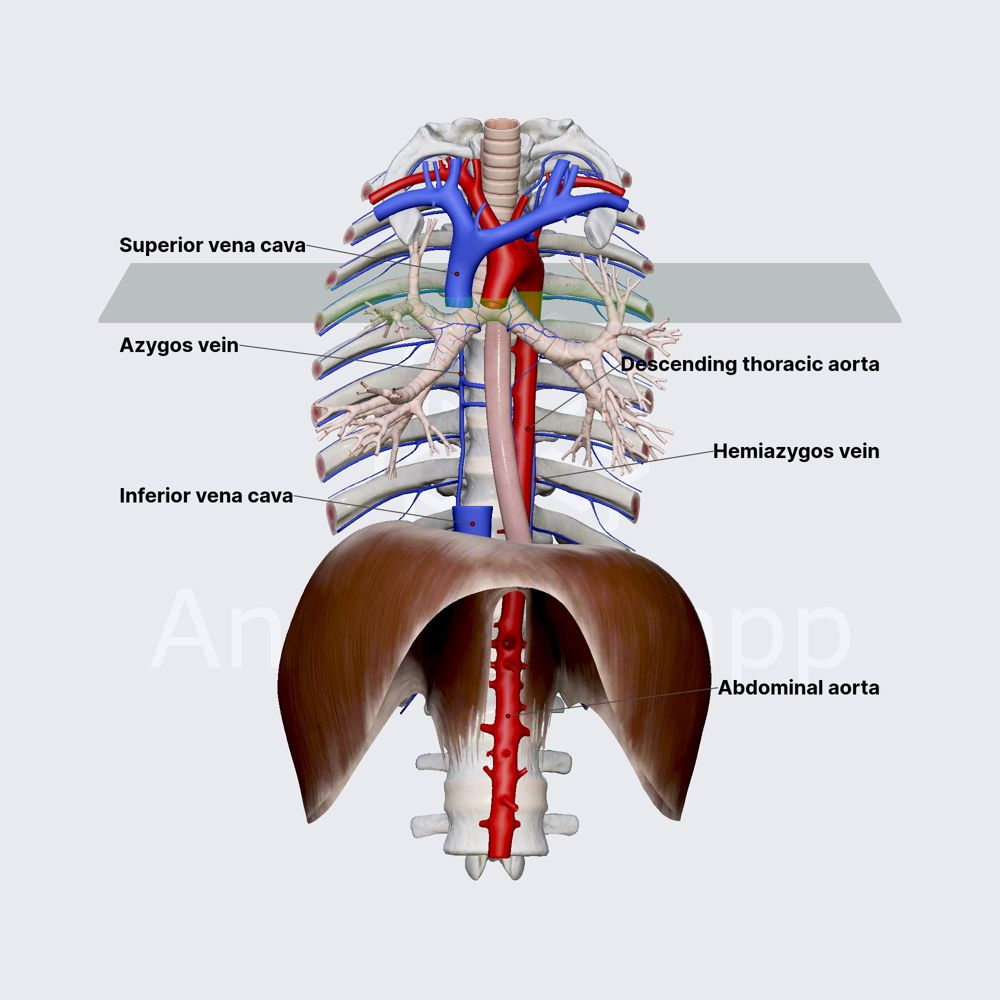
Azygos Vein
Vein that drains the right side of thoracic cavity, receiving venous return from the intercostal spaces and forms a connection between the superior and inferior vena cava, allowing alternative blood return to the heart
empties into the superior vena cava, near the right atrium
provides collateral circulation if there’s obstruction in the superior or inferior vena cava
enlarges in cases of superior vena cava syndrome, causing venous congestion
Cardiac Tamponade
Blood or fluid accumulates in the pericardial sac, restricting heart expansion and the heart cannot fill properly, leading to decreased stroke volume and cardiac output.
Decreased arterial pressure & pulse pressure → due to limited ventricular filling
elevated venous pressure → blood backs up into the venous system
jugular venous distention (JVD swelling) → sign of impaired venous return
shock → reduced cardiac output leads to systemic hypoperfusion (tissues and organs don’t receive enough oxygen and nutrients, leading to metabolic failure)
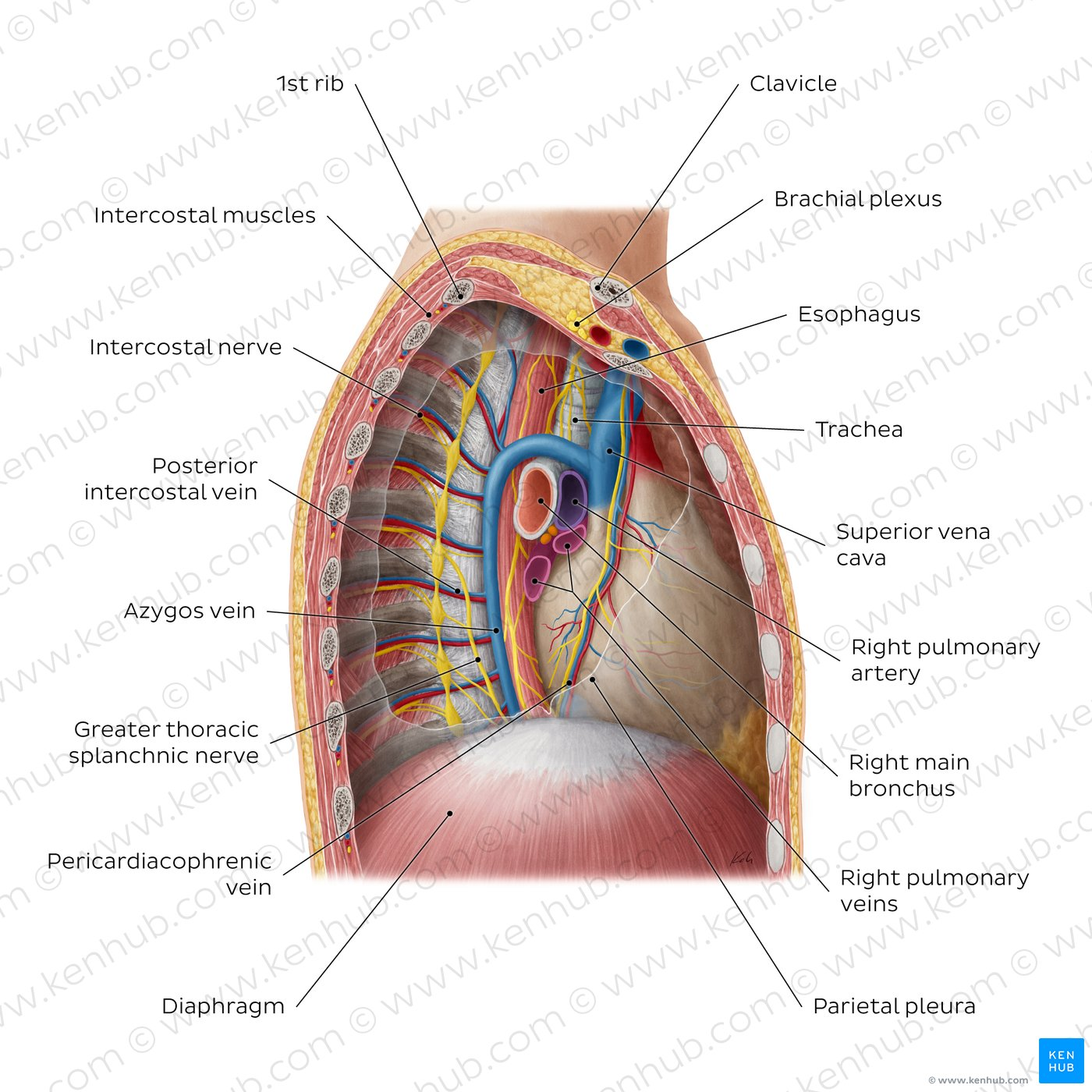
Mediastinum
The central compartment of the thorax
Boundaries:
superior: thoracic inlet
inferior: diaphragm
anterior: sternum
posterior: vertebral column
lateral: lungs (pleural cavities)
Subdivisions:
superior mediastinum: contains the greatest vessels, trachea, esophagus
inferior mediastinum: divided into 3 parts
anterior: thymus, lymph nodes, fat
middle: heart, pericardium, great vessels
posterior: esophagus, descending aorta, thoracic duct, sympathetic chain
Location & orientation of the Heart
Lies between the sternal angle and the 5th intercostal space
positioned anteriorly and slightly to the left within the mediastinum
2/3 of heart sits to left of midline
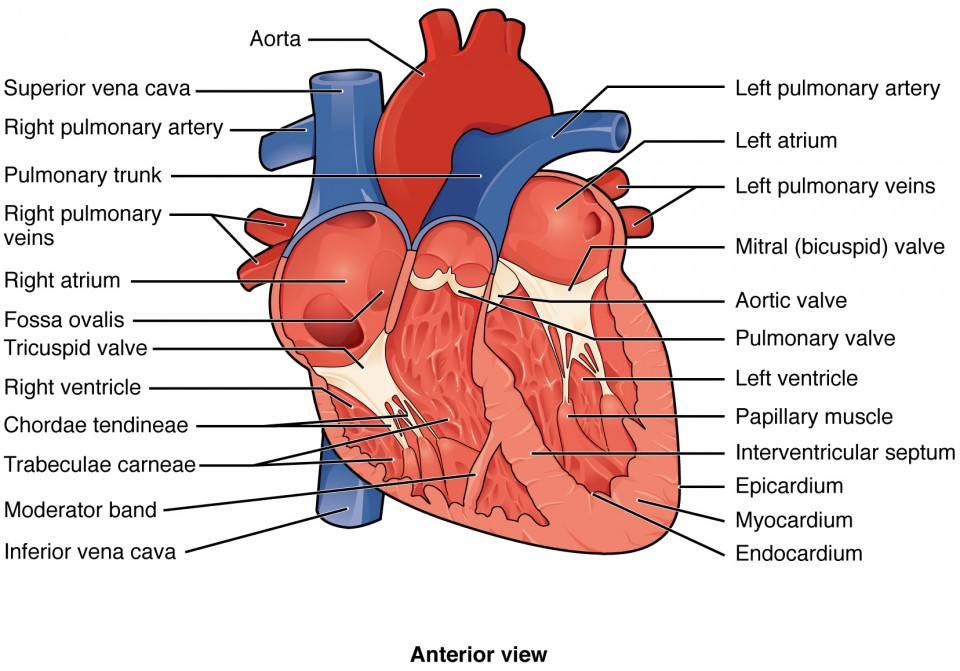
Key anatomical landmarks of the heart
Apex of the heart is located at left 5th intercostal space, near the midclavicular line
Base of heart sits at level of 2nd rib, primarily formed by left atrium
Right border formed by right atrium
left border formed by left ventricle
inferior border formed by right ventricle
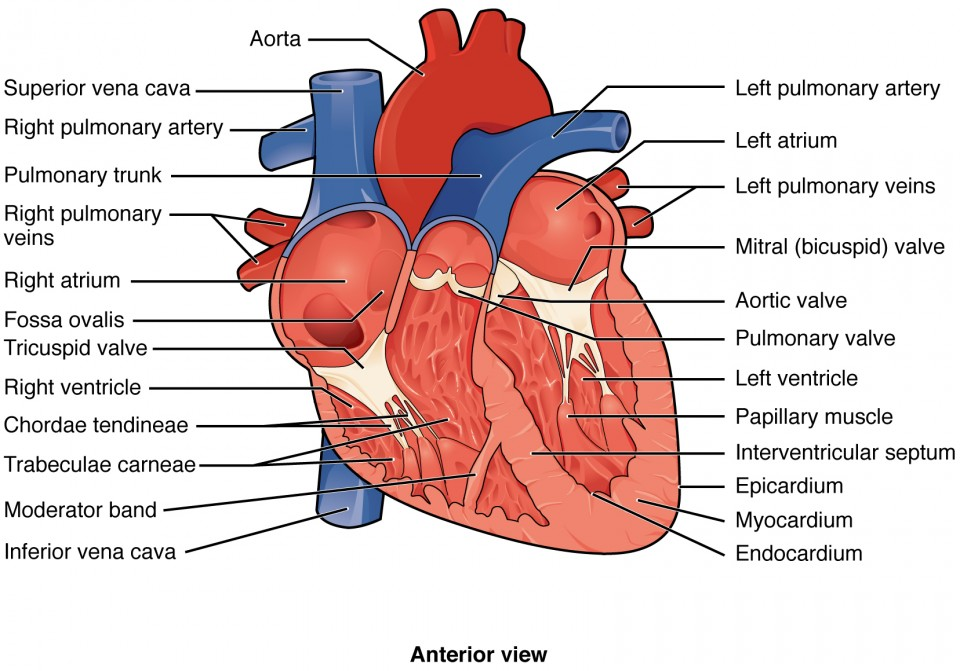
Atrioventricular Valves
control blood filling of ventricles
Tricuspid valves (right AV valve) has 3 cusps to prevent backflow from the right ventricle into the right atrium
chordae tendinae are fibrous cords that anchor cusps to papillary muscles (contract during systole to prevent valve prolapse)
Mitral (bicuspid valve) is between left atrium and ventricle
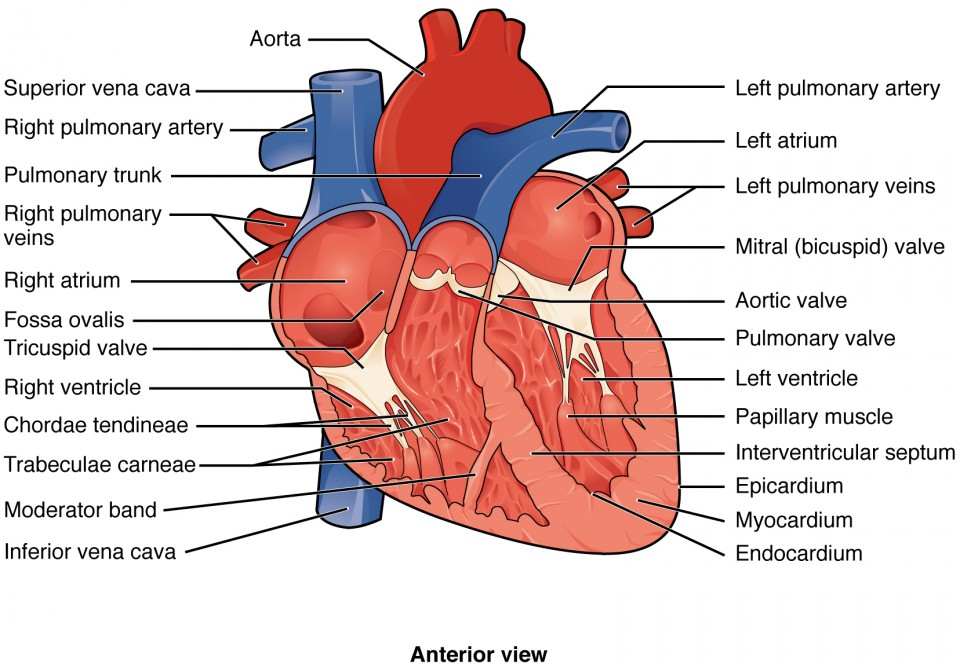
Semilunar valves
control blood ejection from ventricles
pulmonary valve is between right ventricle and pulmonary trunk
opens during systole to allow blood flow into the pulmonary artery, prevents backflow into the right ventricle during diastole
Aortic valve is between left ventricle and ascending aorta
Opens during systole, allowing blood ejection and closes during diastole preventing backflow nad enabling coronary artery perfusion
Valves are operated based on…
a pressure-dependent mechanism
Diastole
relaxation and filling phase
AV valves are open, blood fills the ventricles
atria contract to push remaining blood into ventricles, ventricular pressure decreases
Systole
Contraction and Ejection phase
AV valves close (first heart sound - aligns with QRS complex and AV valve closure)
ventricles contract, pushing blood through aortic and pulmonary valves, ventricular pressure rises
semilunar valves close (second heart sound - follows T wave)
Murmurs
abnormal heart sounds that can indicate valve diseases (stenosis or regurgitation are 2 examples)
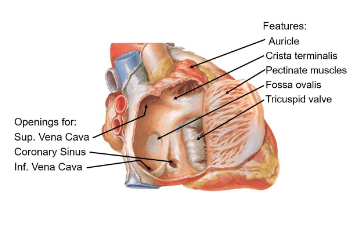
Auricle
Small muscular pouch that increases atrial volume
Cristae Terminalis
ridge separating smooth and rough atrial surfaces (pectinate muscles)
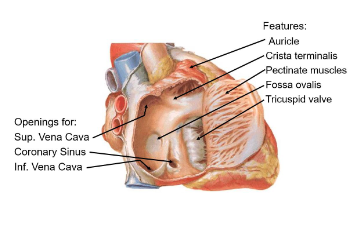
Pectinate muscles
parallel ridges in the atrial wall aiding contraction and strengthens the atrial wall
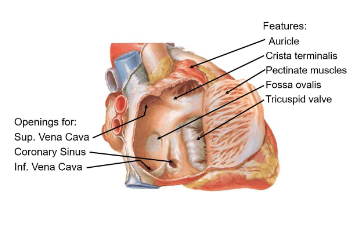
Fossa Ovalis
Remnant of fetal foramen ovale, which allowed blood shunting between atria
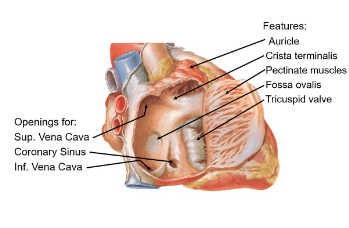
Tricuspid valve
regulates blood flow into the right ventricle
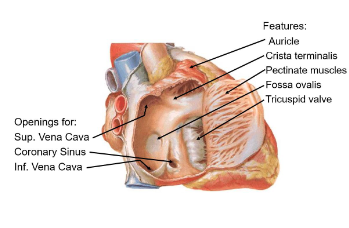
Superior vena cava
Returns deoxygenated blood from upper body
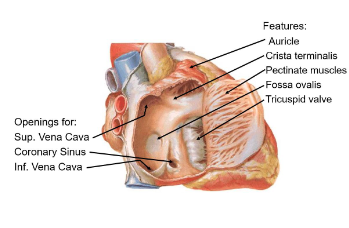
Inferior Vena cava
Returns deoxygenated blood from lower body
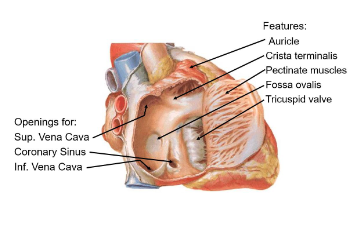
Coronary Sinus
Drains venous blood from the heart’s own circulation
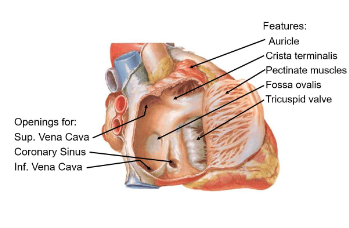
Right Ventricle
pumps deoxygenated blood to lungs via pulmonary valve
Blood flow through heart
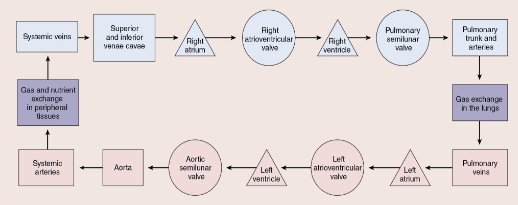
Aortic sinuses
contain openings for right and left coronary arteries.
When the aortic valve closes during diastole, backflow of blood fills the coronary arteries, supplying the heart muscle.
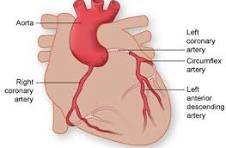
Coronary Circulation
First branches off the aorta are coronary arteries that supply oxygenated blood to the myocardium
travel in the coronary sulcus, encircling the heart
divided into the left and right coronary arteries, each with critical branches
Coronary Artery Disease
narrowing of coronary arteries leads to angina, myocardial infarction, or heart faillure.
Left Anterior Descending Blockage
Causes fatal heart attacks due to its role in supplying the left ventricle and septum
Right Coronary Artery Blockage
Can affect SA & AV node function, leading to bradycardia or heart block
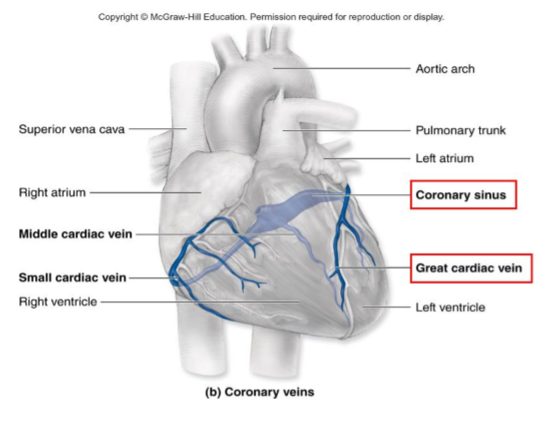
Coronary Venous System
Returns deoxygenated blood from the myocardium to the right atrium
Main veins converge into the coronary sinus (largest cardiac vein)
runs posteriorly in the coronary sulcus between the left atrium and ventricle.
Ascending Aorta
First branches are the right and left coronary arteries → supply oxygenated blood to heart muscle
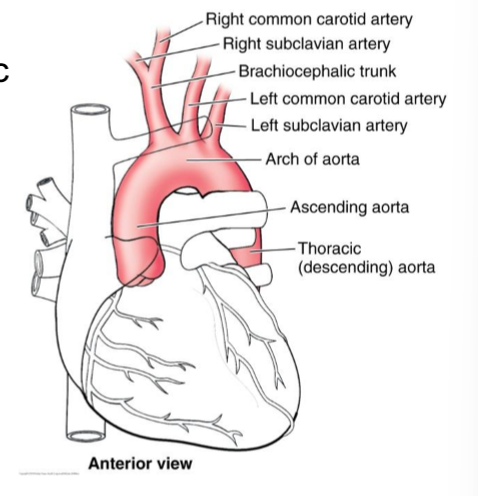
Aortic Arch
3 major branches:
Brachiocephalic trunks supplies right side, divides into:
right common carotid artery → supplies right head and neck
right subclavian artery → supplies right upper limb
Left common carotid artery → supplies left head and neck
left subclavian artery → supplies left upper limb and thoracic structures
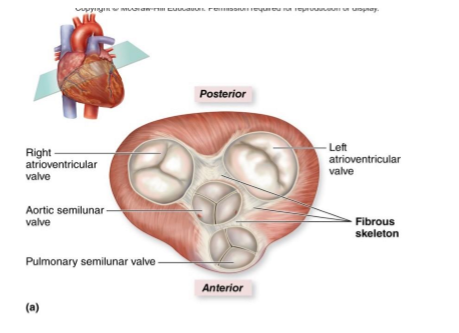
Fibrous Skeleton
provides structural support for heart valves
maintains valve positioning and prevents excessive stretch
serves as an electrical insulator, preventing random electrical impulses from passing between atria and ventricles
forms attachment points for cardiac muscle fibers
Cardiac Muscle’s unique ability
heart muscle contracts rhythmically on its own without direct nervous stimulation (autorhythmicity)
conduction system components are modified cardiac muscle cells that initiate and regulate heartbeat
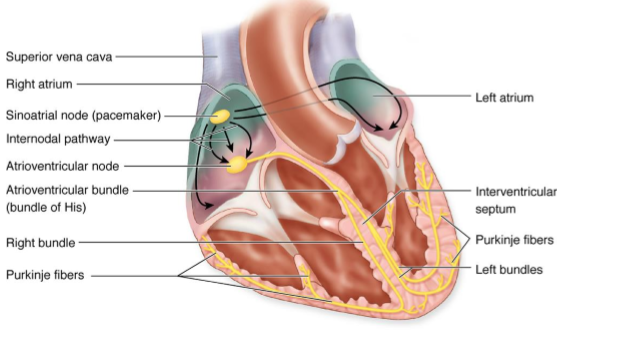
Electrical conduction pathway
SA node: natural pacemaker located at junction of SVC and right atrium, sets heart rate of 60-100 bpm by generating impulses (P wave)
AV node, located in interatrial septum and receives impulses from SA node, delays conduction by 0.1 sec to allow atrial contraction before ventricular contraction (PR interval)
Buncle of His (AV bundle) conducts impulses from AV node to ventricles
Right and left buncle branches carry signals down interventricular septum towards apex
Purkinje Fibers distribute impulses throughout the ventricles, triggering contraction (QRS complex)
Electrical impulses depolarize and repolarize myocardium (T wave is ventricular repolarization)
Baroreceptors
Blood pressure regulation, detect arterial blood pressure changes by sensing vessel wall stretch
high pressure baroreceptors are located in the aortic arch and carotid sinus (detect systemic BP)
low pressure ones are located in the walls of pulmonary vessesl adn atria (detecting venous return)
increased BP activates glossopharyngeal nerve (CN 9) from the carotid sinus and brainstem as well as Vagus nerve (CN 10) to decrease Heart rate (parasympathetic)
decreased BP reduces baroreceptor firing and increases HR and BP via sympathetic activation (T1-T5)
Chemoreceptors
Oxygen, CO2, and pH level changes detected to regulate respiration and circulation
located in aortic and carotid bodies (near baroreceptors)
low O2, high CO2, or acidosis triggers increased sympathetic activity and raises HR and BP to improve oxygenation
Epicardium
visceral pericardium; outer protective layer
mesothelial cells (simple squamous epithelium) and underlying connective tissue
contains blood vessels, lymphatics, and adipose tissue
Myocardium
contractile muscle layer that is composed of cardiac muscle fibers arranged in spirals
intercalated discs (gap junctions & desmosomes) allow coordinated contraction
Endocardium
Inner lining of the heart made from endothelial layer (simple squamous epithelium) and thin subendothelial Connective tissue
subendocardial layer houses purkinje fibers (conducting system)
Purkinje fibers
Specialized cardiac muscle fibers located in the subendocardial layer
pale staining cells due to high glycogen content & fewer myofibrils
found in ventricular walls, conducting impulses rapidly for synchronized contraction
Final component of the conduction system → ensures rapid depolarization of ventricles
transmits impulses from AV bundle of His to ventricular myocardium
allows near-simultaneous contraction of the ventricles for efficient blood ejection
Arteries
carry blood away from the heart
aorta and arteries have highest pressure, large fluctuations between systole and diastole
rounder, thicker wall, prominent tunica media
Veins
carry blood toward the heart
irregular shape, thinner wall, larger lumen, thicker tunica externa relative to wall thickness
contain 65-70% of blood volume at a time
act as blood reservoirs due to high compliance and large lumens
thinner walls and less smooth muscle than arteries
valves in medium and large veins prevent backflow
skeletal muscle pump, muscle contractions compress veins to aid venous return (especially in legs)
arterioles
regulate blood flow into capillary networks, smaller vessels
major drop in pressure due to resistance, they act as pressure regulators
few layers of smooth muscle in tunica media and major role in resistance and blood pressure regulation
capillaries
allow exchange of nutrients, gases, and waste between blood and tissues, smaller vessesl
only composed of endothelium and a basement membrane, allowing efficient exchange of materials
5-10 um diameters (just enough for RBCs to squeeze through)
slow blood flow for maximized exchange time
supported by pericytes - contractile cells that stabilize capillary walls and help with repair
use pinocytotic vesicles for large molecule transport, especially in continuous capillaries
postcapillary venules
return most fluids to blood, excess fluid drains into lymphatic system. Also allow WBCs to migrate into tissues (diapedesis), smaller vessels
decrease in pressure from capillaries, very low in venae cavae
composed of endothelium and pericytes
Muscular venules
Venules that have 1-2 layers of smooth muscle and begin to show a distinct tunica media
pressure is still low and structure is thinner than arterioles
Blood vessel arrangement in series
Elastic arteries → muscular arteries → arterioles → capillaries → venules → small and large veins → venae cavae and pulmonary veins
blood flows in one direction due to pressure gradients generated by the heart and vessel structure
Structure of blood vessels
All have smooth muscle and connective tissue, lined by endothelium (simple squamous epithelium)
tunica intima (inner layer) is made of the endothelium and loose connective tissue with perforated internal elastic lamina
tunica media (middle smooth muscle layer) made of smooth muscle, elastic fibers, Type 3 collagen, proteoglycans, glycoproteins, and external elastic lamina
tunica adventitia (outer connective tissue) is made of type 1 collagen and elastic fibers, contains vasa vasorum (small blood vessels that nourish large vessel walls)
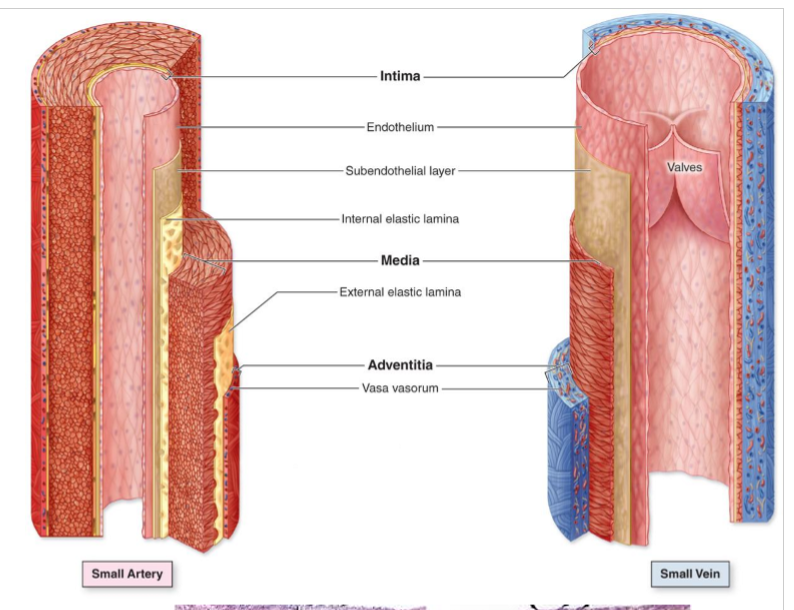
Elastic artery
Type of artery that has a thick tunica media filled with elastic fibers and dampens pressure fluctuations from the heartbeat (aorta)
thick wall accomodates high pressure from the heart
MA: atherosclerotic lesions are common in elastic arteries like the aorta
Muscular artery
Type of artery that has a prominent internal and external elastic lamina and smooth muscle that dominates the tunica media
directs blood to specific organs (femoral artery example)
Continuous capillaries
type of capillary that is the most common and found in muscle, skin, lungs, and brain
has tight junctions, small intercellular clefts, pinocytosis
Fenestrated capillaries
type of capillary that has pores in its endothelium (for rapid exchange) and is found in kidneys, intestines, and endocrine glands
Sinusoidal capillaries
type of capillary that has large gaps and discontinuous basement membrane, found in liver, spleen, bone marrow
Simple pathway flow
type of capillary flow that uses one arteriole, one capillary bed, and one venule and is the most common (skin, muscles)
Arteriovenous shunt (bypass)
Type of capillary flow where blood flows directly from arteriole to venule and is used in thermoregulation (skin in cold temp)
Portal system
type of capillary flow where two capillary beds are connected by a portal vein
enhances exchange between two regions
hepatic portal system and hypophyseal portal system
Immune System
monitors the body’s external and internal environments, responds to potentially harmful substances like pathogens and toxins
composed of cells (lymphocytes, main effector cells), tissues (mucosa associated lymphoid tissues), and organs (lymph nodes, thymus, red bone marrow, spleen)
lymphatic vessles transport lymph and connect with cardiovascular system
Lymph
fluid in immune system that is made up of WBC’s and plasma like fluid (interstitial fluid)
lymph capillaries → lymph vessels → nodes → ducts → veins
valves ensure one-way flow of lymph
right lymphatic duct
drains right upper limb, right side of head/neck and right thorax
Thoracic duct
drains the rest of the body, empties into the left subclavian vein