colon polyps
1/73
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
74 Terms
discrete mass or lesions that extend into the intestinal lesion that can be either sporadic or familial
colon polyps
4 major pathological groups of colon polyps
mucosal adenomatous; tubular, tubulovillous, villous
mucosal serrated: hyperplastic, sessile, traditional serrated adenoma
mucosal non-neoplastic: juvenille, hamartoma, inflammatory
submucosal: lipomas, lymphoid aggregates, carcinoids, pneumatosis cystoids intestinalis
70% of polyps removed during colonoscopy are ____
adenomatous
(most other 30% are serrated)
adenomatous and serrated colon polyps have a higher chance than submucosal and non-neoplastic polyps for what happening
becoming mallignant
colon polyps present in 30% of adults over 50yo, 95% will develop into carcinoma from dysplastic transition which is why we gotta take em out
nonfamilial adenomatous and serrated colon polyps
what DNA mutation causes adenomatous polyps to turn into cancer
inactivation of normal APC gene → chromosomal instability and inactivation of other tumor suppressor genes → colon cancer (takes roughly 10yrs)
what DNA mutation causes serrated polyps to turn into cancer
Kras mutations or BRAF oncogene activation → inactivation of tumor suppression genes OR mismatch of repair genes → colon cancer
which polyp location has a higher chance of becoming cancerous
polyps in proximal colon (near splenic flexure) esp if over 1cm
polyps under 5mm in rectosigmoid colon dont matter
adenomas that high a higher risk of advancing to carcinomas, over 1cm in size and have villous features and high grade dysplasia
advanced adenomas (pre cancer)
what do serrated polyps arise from (similar chance of developing cancer as adenomatous polpys)
hyperplastic polyps
polyps sx
usually asx (which is why screening is so important!!)
maybe: reported intermittent blood from rectum due to ulcerated polyp, fatigue (from chronic blood loss), pallor, gross blood on rectal exam
polyps labs (±)
fecal occult blood test, fecal immunochemical test, anemia from chronic blood loss
polyps dx of choice to detect and remove polyps (allows for immediate biopsy/removal)
colonoscopy
all pts w pos FOBT, fecal immunochemical test, DNA testing or unexplained anemia should do what
get a colonoscopy
polyps imaging
colonoscopy (allows for immediate biopsy/removal)
CT colonography (requires rectal air insufflation, ok for screening)
barium enema (no longer recommended)
polyps tx
colonoscopic polypectomy (used for most, use forceps or snare cautery), but has risk of perforation and significant bleeding so be careful
when is a malignant polyp considered completely removed and treatment completed and what do we do after
polyp is completely excised and submitted for histologic exam, clean margina, no vascular or lymphatic involvement
(if criteria not met a bowel resection is required)
required follow up in 3 months w repeat colonoscopy
if there are no findings on colonoscopy what is the recommended surveillance for colon polyps and/or cancer
colonoscopy in 10 yrs
if there are 1-2 small (under 1cm) tubular adenomas w/out villous features or high grade dysplasia on colonoscopy what is the recommended surveillance for colon polyps and/or cancer
colonoscopy in 5-10 yrs
if there are 3-10 adenomas, adenomas over 1cm or adenomas w villous features or high grade dysplasia on colonoscopy what is the recommended surveillance for colon polyps and/or cancer
colonoscopy in 3yrs
if there are over 10 adenomas on colonoscopy what is the recommended surveillance for colon polyps and/or cancer
colonoscopy in 1-2 yrs to rule out familial polyposis syndrome w genetic testing
if there are small (under 1cm) serrated polpys without dysplasia on colonoscopy what is the recommended surveillance for colon polyps and/or cancer
colonoscopy in 5yrs
if there are large (over 1cm) serrated polpys and those w cytologic dysplasia on colonoscopy what is the recommended surveillance for colon polyps and/or cancer
colonoscopy in 3yrs
if there are small typical hyperplastic polpys in the distal colon and rectum on colonoscopy what is the recommended surveillance for colon polyps and/or cancer
no surveillance needed until 50yo
germline genetic mutations with high risk for cancer, accounting for 4% of all colorectal cancer cases (family hx huge to determine screening
hereditary polyposis syndromes
if you see any of these conditions in someones family hx genetic counseling is needed
more than 1 family member affected by polyposis syndrome
personal or family hx of colorectal cancer at under 50yo
personal or family hx of 20+ polyps
types of hereditary polyposis syndromes
familial adenomatous polyps, hamartomatous polpyosis syndromes, lych syndrome
type of hereditary polyposis syndrome characterized by development of 100s-1000s of colonic adenomatous polpys and extracolonic manifestations
(15% of these pts have no genetic link and develop this de novo, accounts for 0.5% of colorectal cancer pts)
familial adenomatous polyposis
familial adenomatous polyposis extracolonic manifestations
soft tissue tumors, osteomas, hypertrophy of retinal pigment
DNA mutation associated w familial adenomatous polyposis
autosomal dom inherited mutation of APC (adenomatous polyposis coli) gene in 90% or MUTYH gene in 8%
familial adenomatous polyposis prognosis
colorectal polyps by 15 and cancer by 40
familial adenomatous polyposis tx
prophylactic colectomy to prevent inevitable cancer
complete proctocolectomy w ileoanal anastamosis
colectimy w ileorectal anastamosis before 20yo
upper endoscopy eval every 1-3yrs (lesions over 2cm need excision)
sulindac (NSAID) and COX2 inhibitor (celebrex) to dec number and size of polpys in rectal stump (but not duodenum)
types of hamartomatous polpyosis syndromes (rare, less thatn 0.1% of colorectal cancers)
peutz-jeghers syndrome, familial juvenile polyposis, PTEN multiple hamartoma syndrome (aka cowden disease)
a type of hamartomatous polpyosis syndrome that is autosomal dom and is from a mutation in the serine threanonine kinase 11 gene
peutz-jeghers syndrome
a type of hamartomatous polpyosis syndrome that is autosomal dom and is from a genetic defect in the 18q and 10q gene
familial juvenile polyposis
a type of hamartomatous polpyosis syndrome that is from a mutation in the PTEN gene
cowden disease aka phosphatase & tensin homolog (PTEN) syndrome
clinical presentation/sx of peutz-jeghers syndrome
polyps throughout intestines (mostly small intestines)
pigmented macules on buccal mucosa, lips, skin (not malignant but inc chances of malignancies)
up to 60% develop Gi cancer and 50% develop breast cancer
clinical presentation/sx of familial juvenile polyposis
defined by over 10 polpys, mostly in colon
possible adenomatous polyps
up to 50% risk of adenocarcinoma
affects “juvenile” tissue, not pediatric pts
clinical presentation/sx of cowden disease aka phosphatase & tensin homolog (PTEN) syndrome
polyps and lipomas throught GI tract, trichilemmomas, cerebellar lesions
risk of cancer in thyroid, breast, and GU tract
autosomal dom hereditary nonpolyposis colon CA seen in 3% of all colorectal cancers (pts also have a high risk of other cancers, esp endometrial) that must be ruled out bc high lifetime rate of cancer in all pts
lynch syndrome
we must rule out lynch syndrome in all pts w ____
early onset colorectal cancer, family hx of colorectal cancer or other cancers at young age or in multiple family members
what cells do we see in lynch syndrome
few adenomas, cells are flat w villous features or high grade dysplasia that rapidly transform from benign to cancerous (1-2yrs)
genetic mutation seen in lynch syndrome
defect in either MLH1, MSH2, MSH6, or PMS2 (vital for DNA base-pair matching)
what cell transformation happens in lynch syndrome
normal tissue → HNPCC adenoma → cancer (all in 1-2yrs)
bethesda criteria to select individuals that should get genetic testing for lynch syndrome (all colorectal cancer pts should still receive genetic testing bc this only finds 70% of ppl w lynch syndrome)
colorectal cancer under 50
multiple or reoccuring colorectal or HNPCC associated tumors (regardless of age)
colorectal cancer w 1 or more first degree relatives before age 50
colorectal cancer w 2 or more 2nd degree relatives w either colorectal cancer or HNPCC regardless of age
tumors w infiltrating lymphocytes, mucinous/signet ring differentiation, or medullary growth pattern in pts under 60yo
a protrusion, bulge, or projection of an organ or part of an organ through the abdominal or pelvic wall that form through weak spots within the muscular or facial planes (can be acquired or congenital) and are the 2nd most common cause of bowel wall obstruction
abdominal wall hernias
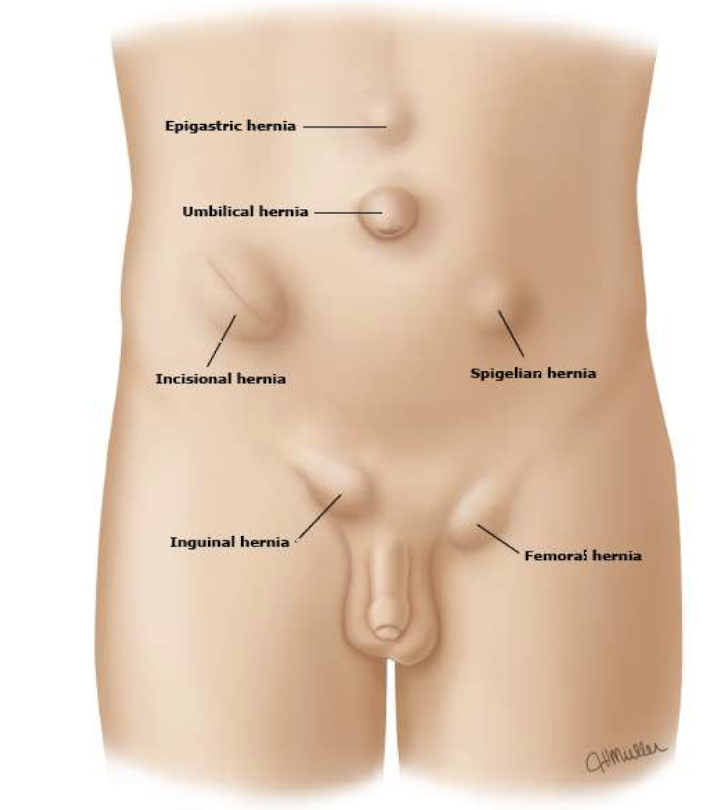
types of abdominal wall hernias
incisional, umbilical, epigastric, spigelian, inguinal, femoral
abdominal wall hernias risk factors
obesity, preg, straining (excessive weightlifting, defecatoin, BPH, exercise), trauma/surgery, smoking, ascites, aging, family hx of hernias, connective tissue disease (EDS, marfan, loeys dietz)
abdominal wall hernias sx
pain/bulge w a palpable mass (reliable means to dx hernia just w this)
how are hernias categorized
by location and reducibility
type of hernia where contents return to the abdomen spontaneously or w light manual pressure, has a full ache w intermittent protrusion
reducible hernia
type of hernia where contents are “stuck” and cant be pushed back into abdomen, if acute will have crampy abdominal pain, localized tenderness, N/V, obstruction, or fever (can become surgical emergency)
incarcerated or irreducible hernias
type of hernia where contents become trapped, and blood supply becomes compromised leading to ischemia and necrosis (can become surgical emergency)
strangulated hernias
technically any hernia of the abdominal wall is a _____
ventral hernia
protrusion through an incision site less than 1yr post surgery (protrusion of contents through a previous incision by a defect in the facial closure, results from 10% of all abdominal surgeries)
incisional hernia
protrusion through the umbilicus
umbilical hernia
protrusion in epigastric region
epigastric hernia
protrusion through lateral wall
spigelian hernia
hernia that is congenital in kids but acquired in adults (from ascites, preg, obesity, cysts or cancer) that usually heals spontaneously in kids under 2yo or can be surgically repaired via primary direct closure w suture/mesh, which is the only cure in adults
umbilical hernia
most common site of all hernias
groin region (indirect inguinal hernia, direct inguinal hernias, femoral hernias)
groin hernia common in men and women, more often on the right side
indirect inguinal hernias
groin hernia thats more commonly incarcerated than other groin hernias
femoral hernias
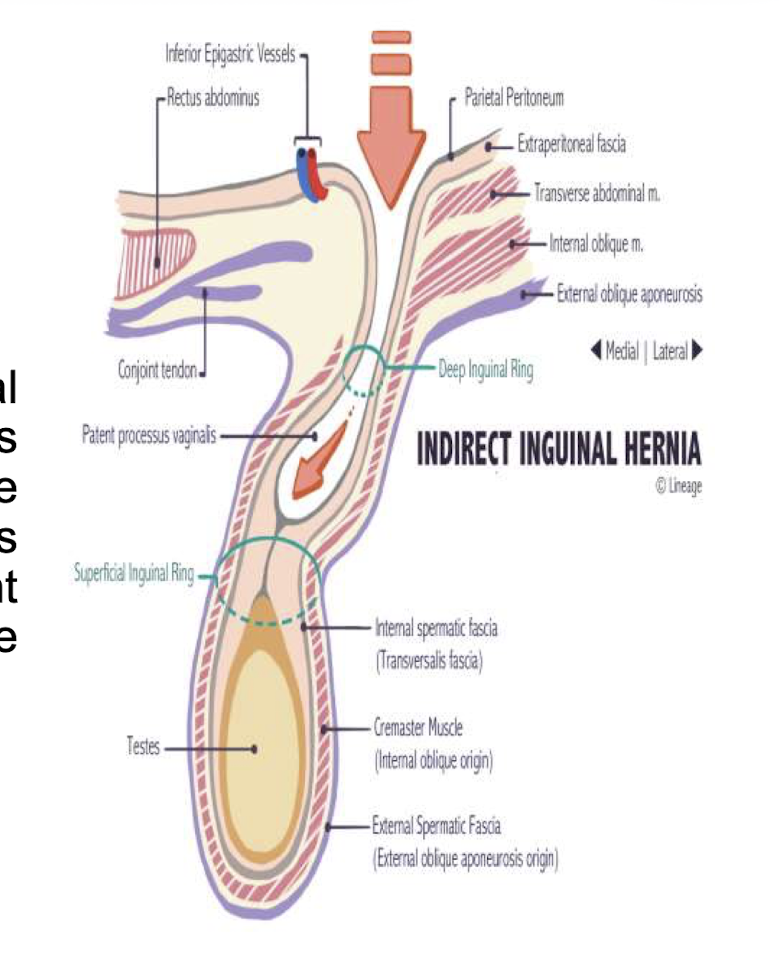
how do indirect inguinal hernias happen
protrusion at internal inguinal ring (where spermatic cord is in men and round ligament in women leaves abdominal cavity) → hernia moves through internal inguinal ring (mesentaric fat, intestines, ovaries, fallopian tubes, or uterus can get herniated)
groin hernia most often found in scrotum, mostly congenital, has a risk for strangulation (cause of narrow defect), often seen in 1yo or younger and 10-30yo and can recurr post op
indirect inguinal hernias
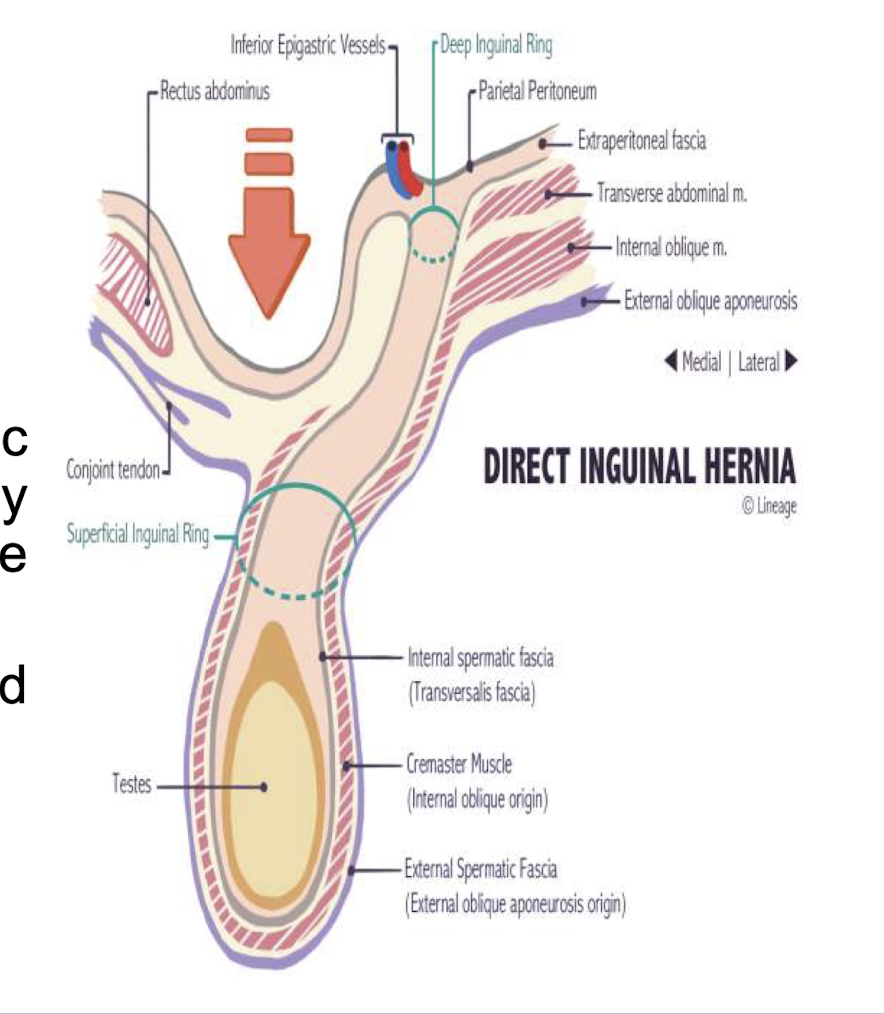
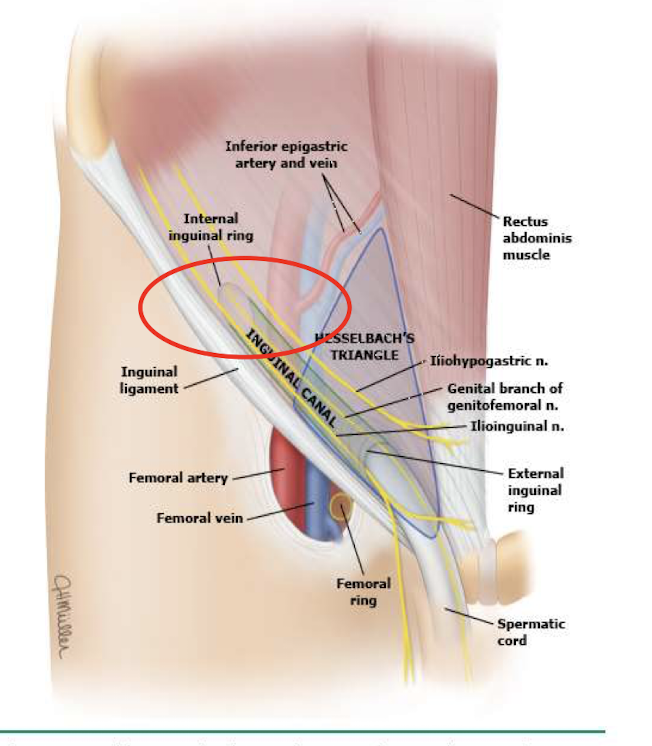
how do direct inguinal hernias happen
herniated sac protrudes through inguinal wall (less likely to end up in scrotum) → protrude medial to inferior epigastric vessels in hesselbach triangle (made of inginal ligament on bottom, inferior epigastric vessels on the side, and rectus abdominus muscle medially)
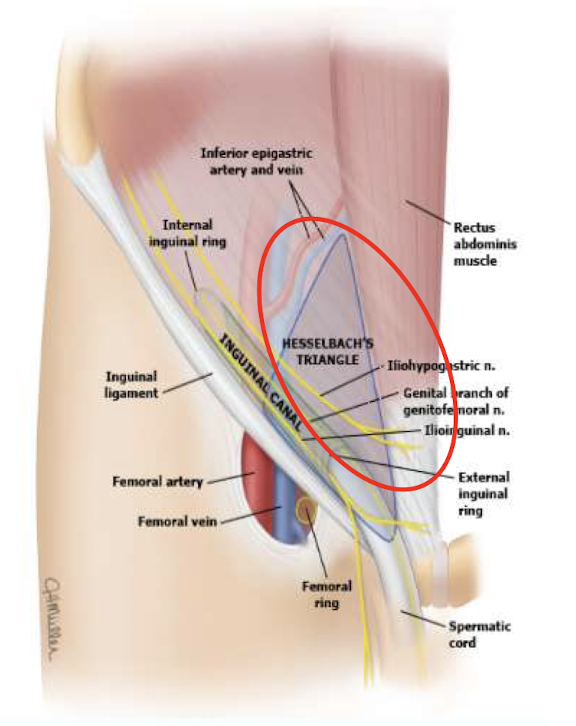
how do femoral hernias happen
located inferior to the inguinal ligaments → protrudes through femoral ring (medial to femoral vein and lateral to lucunar ligament
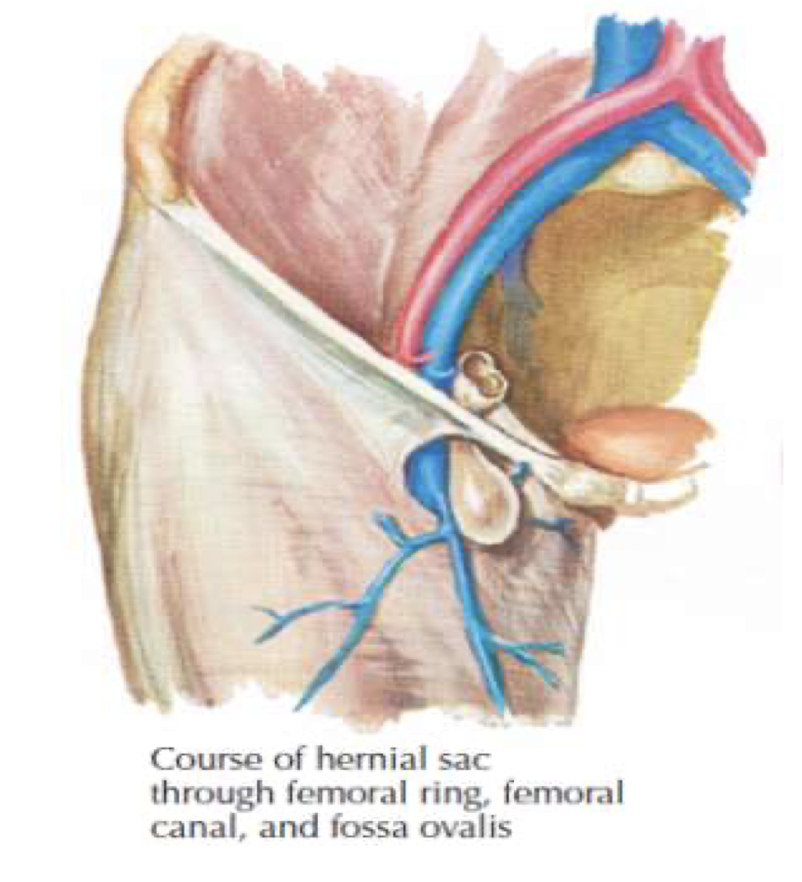
groin hernia more common in women and more on the right side, initially asymptomatic but has high risk for strangulation/incarceration and can reoccur post-op
femoral hernia
inguinal hernia sx
acute= sharp pain and swelling after event
many asx following acute episode or in subacure presentations and found incidentally
gradual onset of discomfort (dull pain radiating into groin)
localized swelling or visible and palpable mass (reducible mass w light pressure or dissappears on its own w supination
infants may have irritability
exacerbated by cough/valsalva/straining
inguinal hernia just superior to pubic tubercle
direct inguinal hernia
inguinal hernia that is a scotal mass or enlargement
indirect inguinal hernia
physical exam preferred maneuvers for inguinal hernias
place gloved finger into external inguinal rung of pt via scrotum. pt asked to cough or strain to inc intraabdominal pressure, done bilaterally w pt standing
mass touching tip of finger = indirect
mass touching side of finger = direct
inguinal hernia dx
abdominal series xrays (rules out perforation and may see bowel in scrotum)
ultrasound (differentiating scrotal masses)
CT w contrast (helps differentiate hernias and identify small hernias causing pain w/o clinical evidence
inguinal hernia tx
daytime truss, avoid straining, manual reduction using supine position, surgical consult (herniorrhaphy or hernioplasty to reduce sac and clsoe defect, only method of tx to prevent incarceration or strangulation)
if you see an inguinal hernia on the left side its not an inguinal hernia its
a varicocele