A&P 3.3 Cardiovascular System (Principles of Physiology)
1/59
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
60 Terms
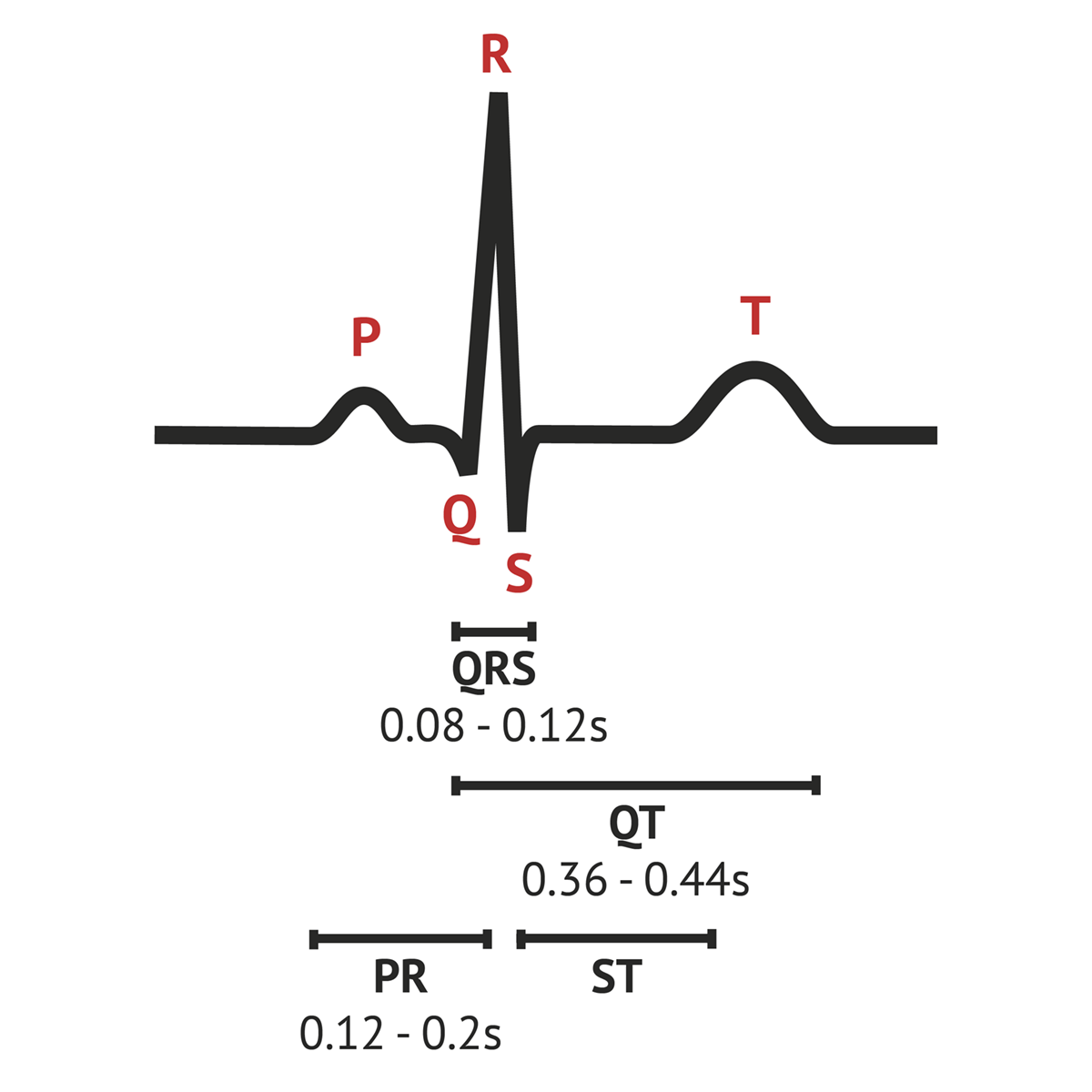
What does the P represent electrically and mechanically?
E: Atrial Depolarization
M: Atrial contraction
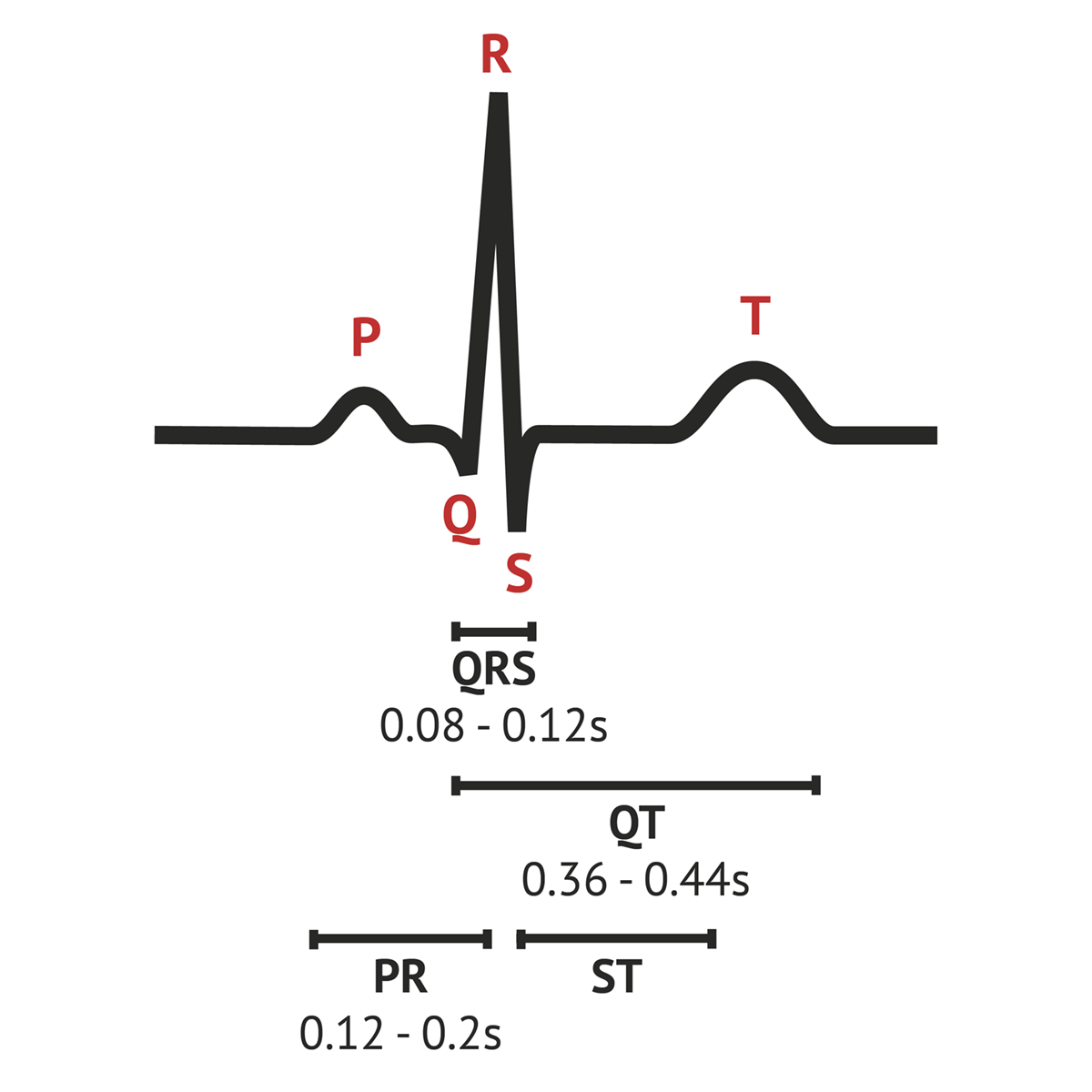
What does the QRS represent electrically and mechanically?
E: Ventricular depolarization
M: Ventricular contraction
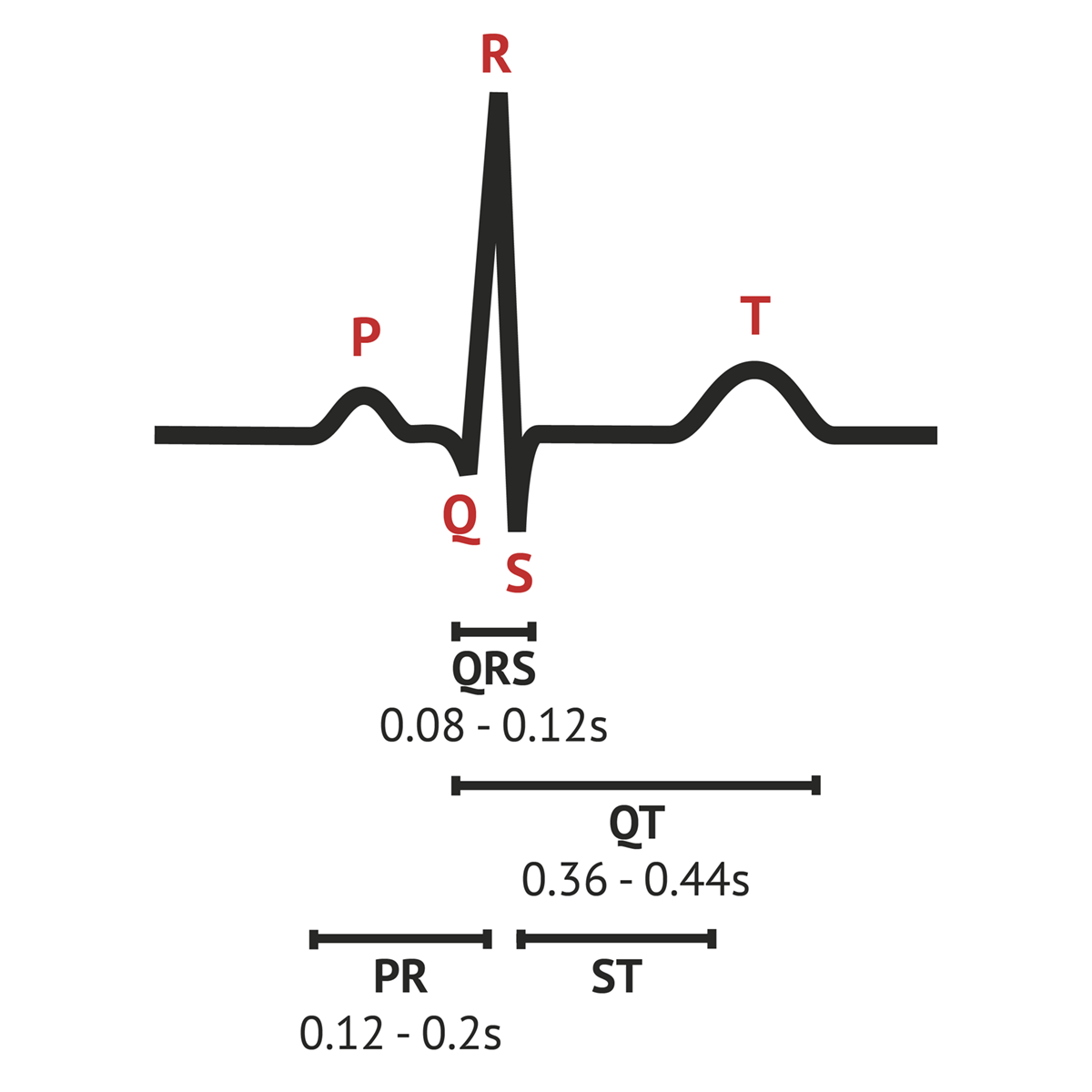
What does the T represent electrically and mechanically?
E: Ventricular repolarization
M: Ventricular relaxation
What is the ejection fraction?
vol of blood pumped from ventricles / vol of blood that fills ventricles
Which lead is placed between the right arm and left arm electrodes, the left arm being positive?
Lead 1
Which lead is places between the right arm and left leg electrodes, the left leg being positive?
Lead 2
Which lead is placed between the left arm and left leg electrodes, left leg being positive?
Lead 3
A diagrammatic representation of lead 1, 2 and 3 is termed
Einthoven’s Triangle
The same three leads that form the standard leads also form the three unipolar leads known as the
Augmented Leads
The 3 Augmented Leads are referred to as
aVR (right arm), aVL (left arm), and aVF (left leg)
SA Nodal Cell:
Phase 4 is the unstable rest or pacemaker potential, it is a
spontaneous depolarization
SA Nodal Cell:
Phase 4 is caused by
influx of Na+, influx of Ca++
SA Nodal Cell:
Phase 0 is the
rapid depolarization
SA Nodal Cell:
Phase 0 is caused by
large influx of Ca++ ions
SA Nodal Cell:
Phase 3 is the
rapid repolarization
SA Nodal Cell:
Phase 3 is caused by
closing of Ca++ channels, efflux of K+
SA Nodal Cell:
The Na+ influx during phase 4 is from what channels?
funny
SA Nodal Cell:
The Ca++ influx during phase 4 is from what channels?
transient
Cardiac Myocyte:
Phase 4 is the influx of
Na+, Ca++
Cardiac Myocyte:
Phase 0 is the influx of
Na+
Cardiac Myocyte:
Phase 1 is the influx of ___ and efflux of ___
Cl-, K+
Cardiac Myocyte:
Phase 2 is the influx of ___ and efflux of ____
Ca++, K+
Cardiac Myocyte:
Phase 3 is the efflux of
K+
Cardiac output is the
volume/minute
Heart rate is the
beats/minute
Stroke Volume is the
volume/beat
CO=
HR x SV
As The Heart Muscle Stretches, Contractile Force Increases Only To A Point.
Starling’s Law
conduction system
functional syncytium
intrinsic factors of heart rate
auto-regulation (Starling)
preload & after load to trigger starlings (but mainly extrinsic)
Intrinsic factors of stroke volume
Which nervous system does the heart rate belong to?
Parasympathetic
Which nervous system does the stroke volume belong to?
Sympathetic
positive chronotrope means the heart rate goes ____
up
negative chronotrope means the heart rate goes _____
down
positive inotrope means the stroke volume goes ____
up
TE=
KE+PE
TPR is
total peripheral resistance
Systolic pressure is measured the moment you are ____ to hear the sound of the pulse.
able
Diastolic pressure is measured the moment you are _____ to hear the sound of the pulse.
unable
Angiotensin II (Ag II) and Arginine-vasopressin (ADH/AVP) are
vasoconstrictors
Which autonomic receptor?
VC @ TPR beds
alpha 1
Which autonomic receptor?
inhibits NE release
alpha 2
Which autonomic receptor?
increased HR and contractility
Beta 1
Which autonomic receptor?
VD @ TPR beds
beta 2
The source of Acetylcholine (ACH)
PNS/CNX
The effect of Acetylcholine (ACH)
decrease HR
The source of Aldosterone (ALD)
adrenal cortex
the effect of aldosterone (ALD)
increase Na+ absorption at kidneys
Increase BV > Increase BP
the source of angiotensin II
kidney/liver/lungs
the effect of angiotensin II
increase VC > increase BP
increase aldosterone & ADH/AVP
the source of atrial naturetic peptide
heart
the effect of atrial naturetic peptide
Na+ loss @ kidney
decrease BV > decrease BP
the source of antidiuretic hormone
hypothalamus/PP
the effect of antidiuretic hormone
increase H2O absorption @ kidney
VC in TPR beds
increase BP
the source of epinephrine
SNS/adrenal medulla
the effect of epinephrine
VC in TPR beds: a1
VD in TPR beds: B2
HR & SV (contractility)
BP increase
the source of renin
kidney
the effect of renin
increase conversion of angiotensinogen
the source of Nitric oxide
vascular endothelium/peripheral nerves
the effect of nitric oxide
increase VD > tissue perfusion