FUNDAMENTALS OF SPIROMETRY
1/31
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
32 Terms
Pulmonary Function Test
Uses for Spirometry (4)
Screening
Diagnosing Pulmonary Diseases
Monitoring Progression of Disease
Monitor Improvements post-treatment/lifestyle modification
Process of Spirometry
1. Pre-test Questionnaire (medical hx, smoking status, patient
2. Vitals (Ht, Wt, Temp, BP)
- DO NOT PERFORM IF HEMODYNAMICALLY UNSTABLE
3. Explain Procedure
4. Demonstrate Procedure
5. Enter data into spirometer
6. Perform test, Coach patient!
Who should you NOT perform spirometry on?
if they are hemodynamically unstable
How many efforts are required for spirometry?
3 valid efforts
- coach the patient!
How is Spirometry performed?
patient seated, sitting straight with feet flat on the floor
attach disposable mouth piece, APPLY NOSE CLIP
place teeth on mouthpiece and seal lips around mouthpiece
patient breathes normally for a few breaths then instruct patient to breathe in FULLY
BLOW OUT FAST AND STEADY for as long as possible
- encourage the patient!
rest 15-30 seconds
3 acceptable trials needed
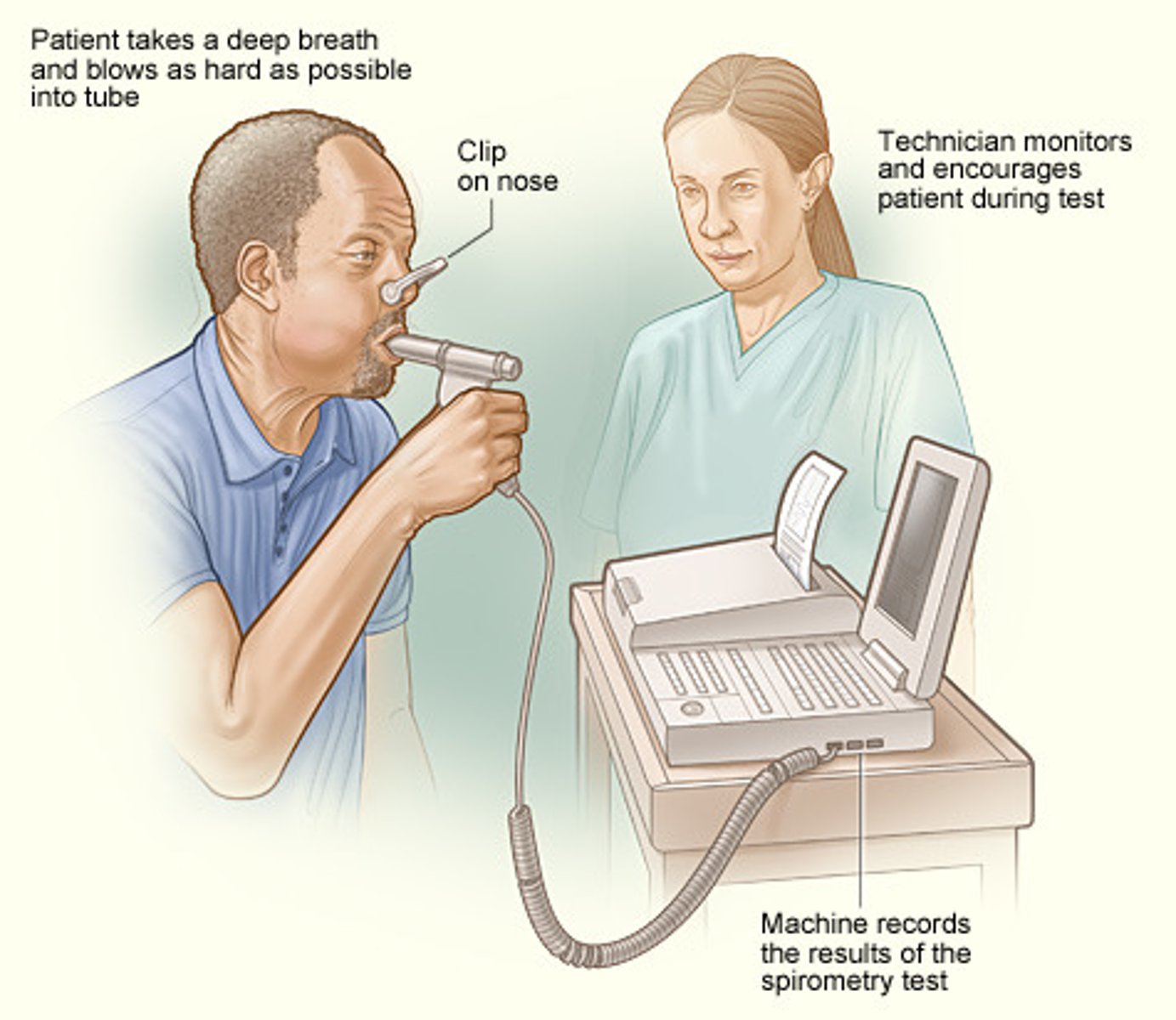
What factors affect lung function?
position
age
ethnic group
weight
height
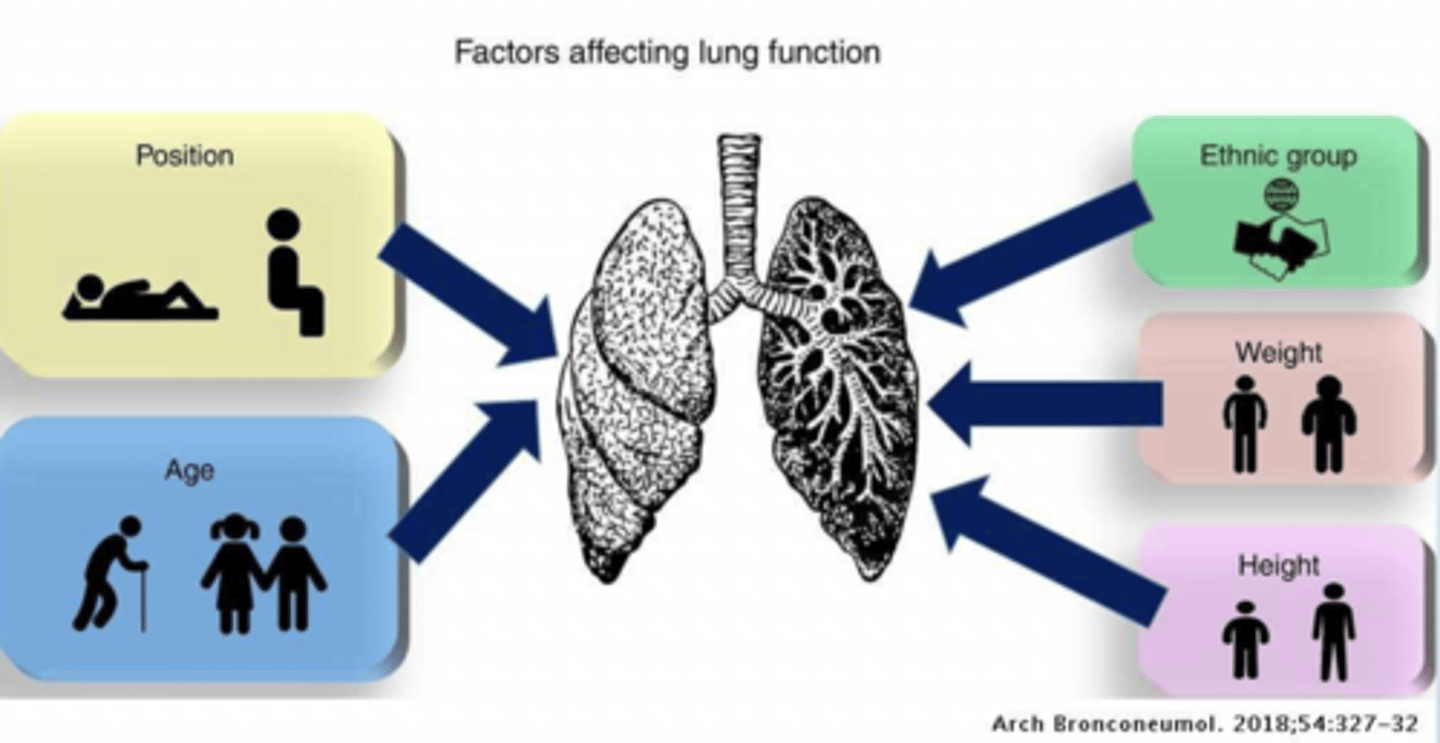
How does ethnicity/race affect lung volume?
Compare highest vs lowest lung volume by Race and Gender.
caucasians have the highest capacity
african americans have the lowest
males have a larger capacity than females
How to educate and perform spirometry on a transgender patient.
explain to the patient the importance of putting their gender assigned at birth
if transitioned gender is used it can lead to misdiagnosis due to improper lung capacity predictions
How is Spirometry measured in PEDIATRICS?
What is the main measurement needed?
children as young as 5-8 YO can perform spirometry with adjustments such as standing instead of sitting
main goal is getting the FEV1 measurement
dependent on child compliance
Measurements of Pulmonary Function Test
- which volume should we never be able to touch?
Residual Volume (keeps lungs inflated, cannot be measured by spirometry)
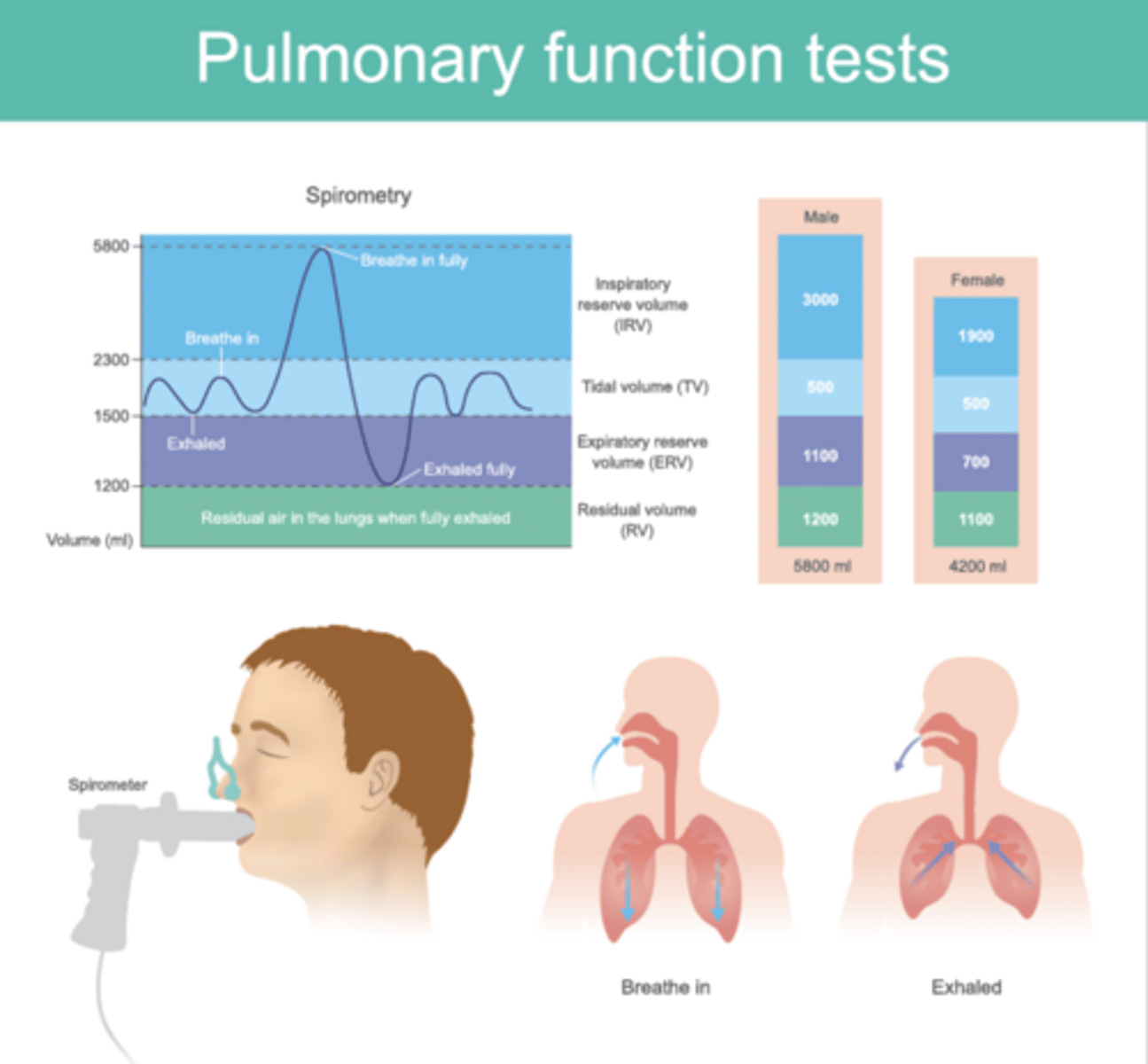
Inspiratory Reserve Volume
The amount of air that can be inhaled after a normal inhalation; the amount of air that can be inhaled in addition to the normal tidal volume.
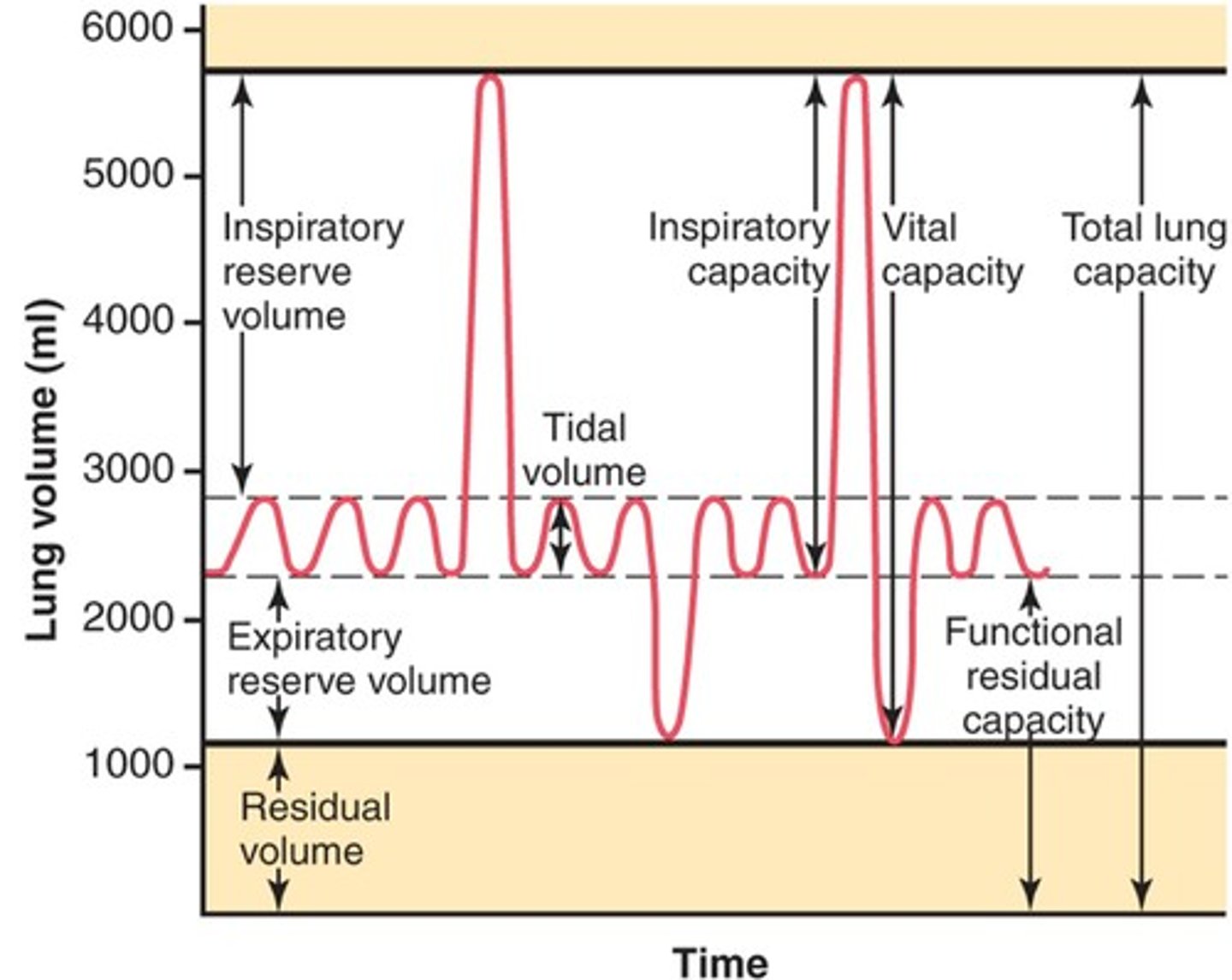
Expiratory Reserve Volume
Amount of air that can be forcefully exhaled after a normal tidal volume exhalation
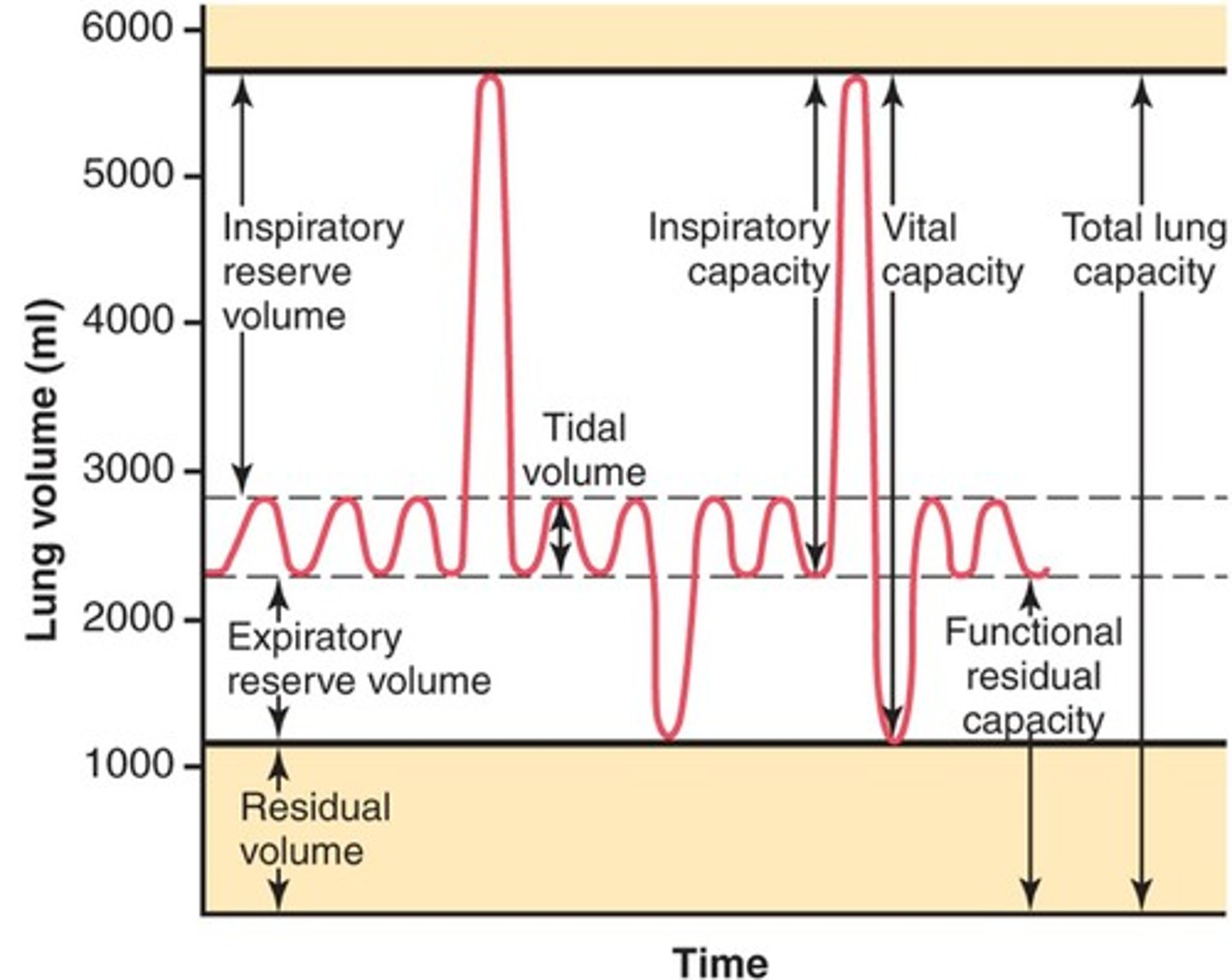
Residual Volume
Amount of air remaining in the lungs after a forced exhalation
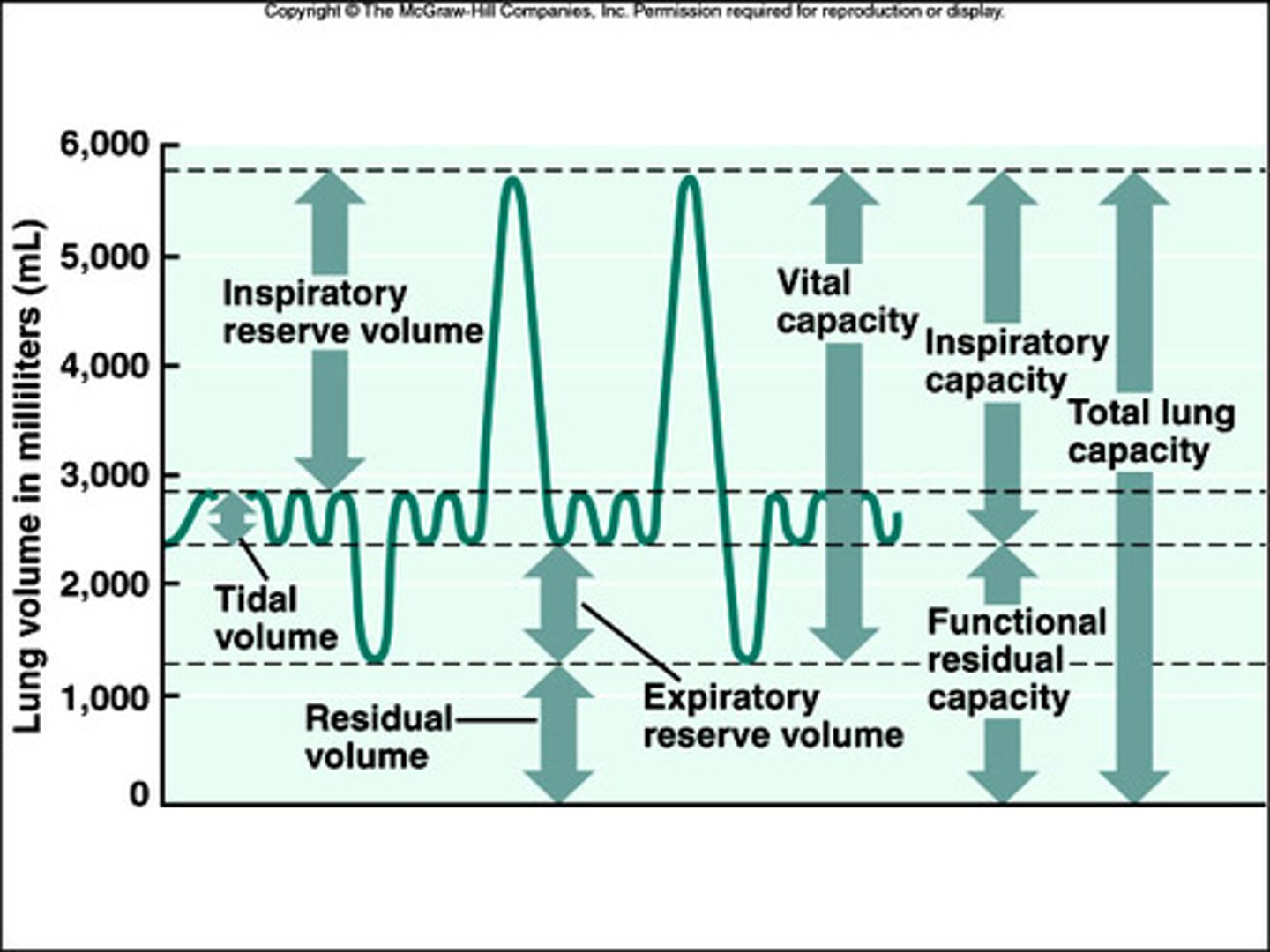
Tidal Volume
Amount of air that moves in and out of the lungs during a normal breath
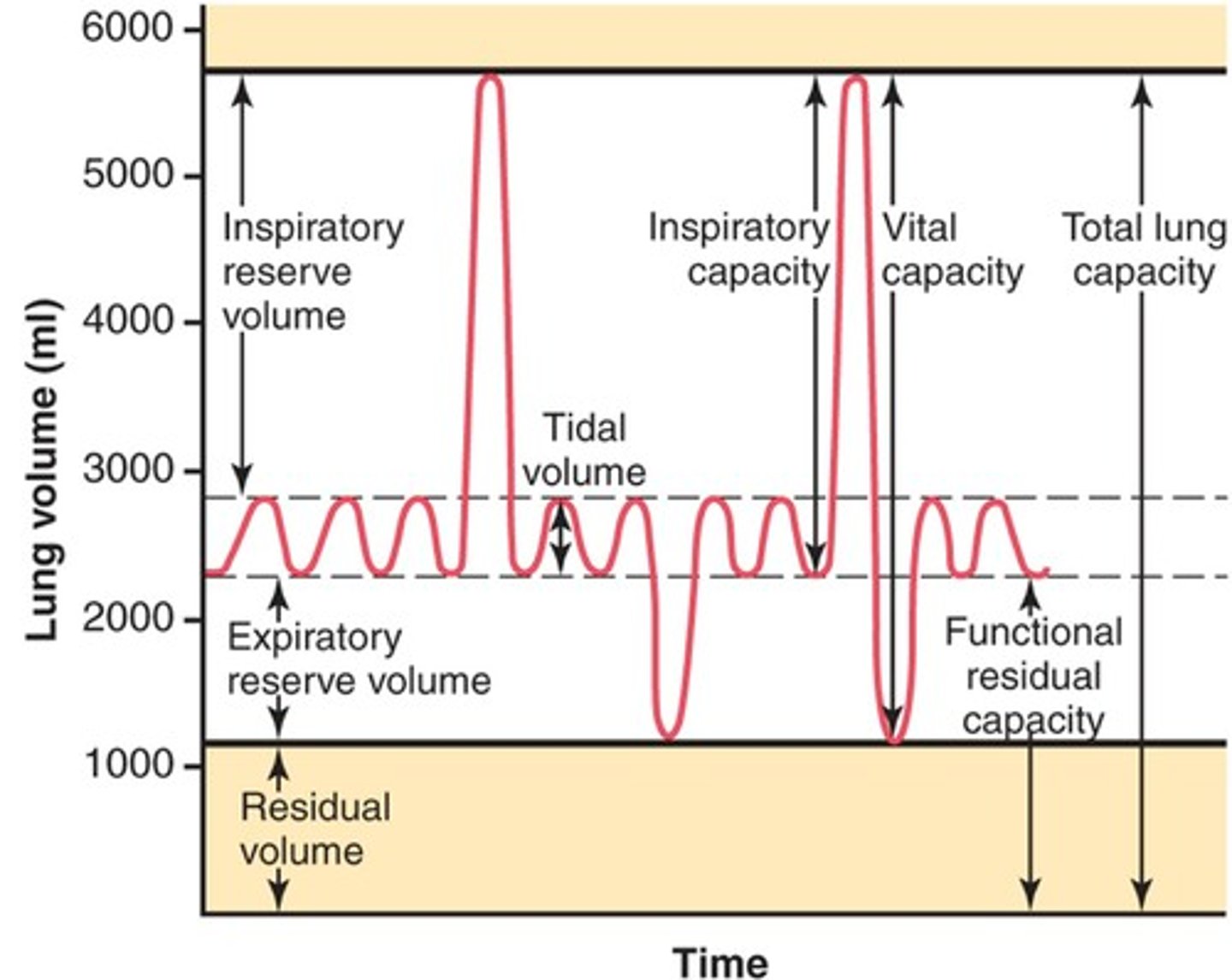
Inspiratory Capacity
tidal volume + inspiratory reserve volume
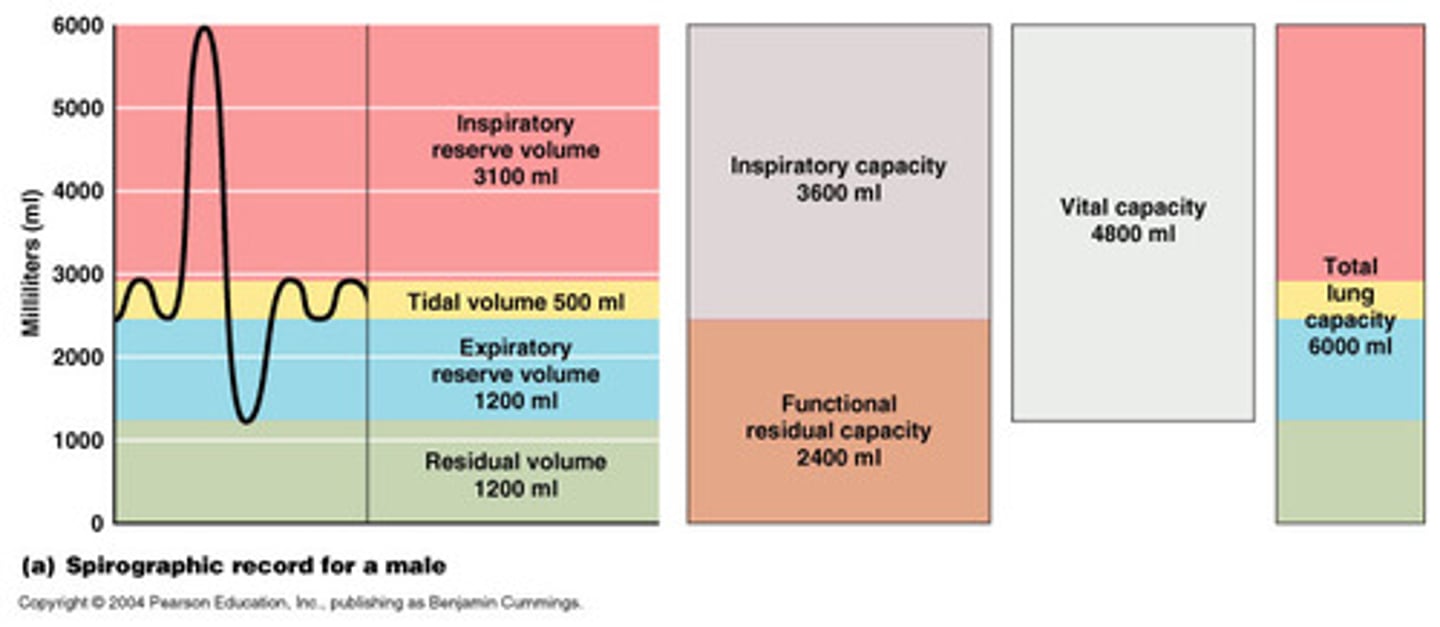
Vital Capacity
The total volume of air that can be exhaled after maximal inhalation.
IRV + TV + ERC
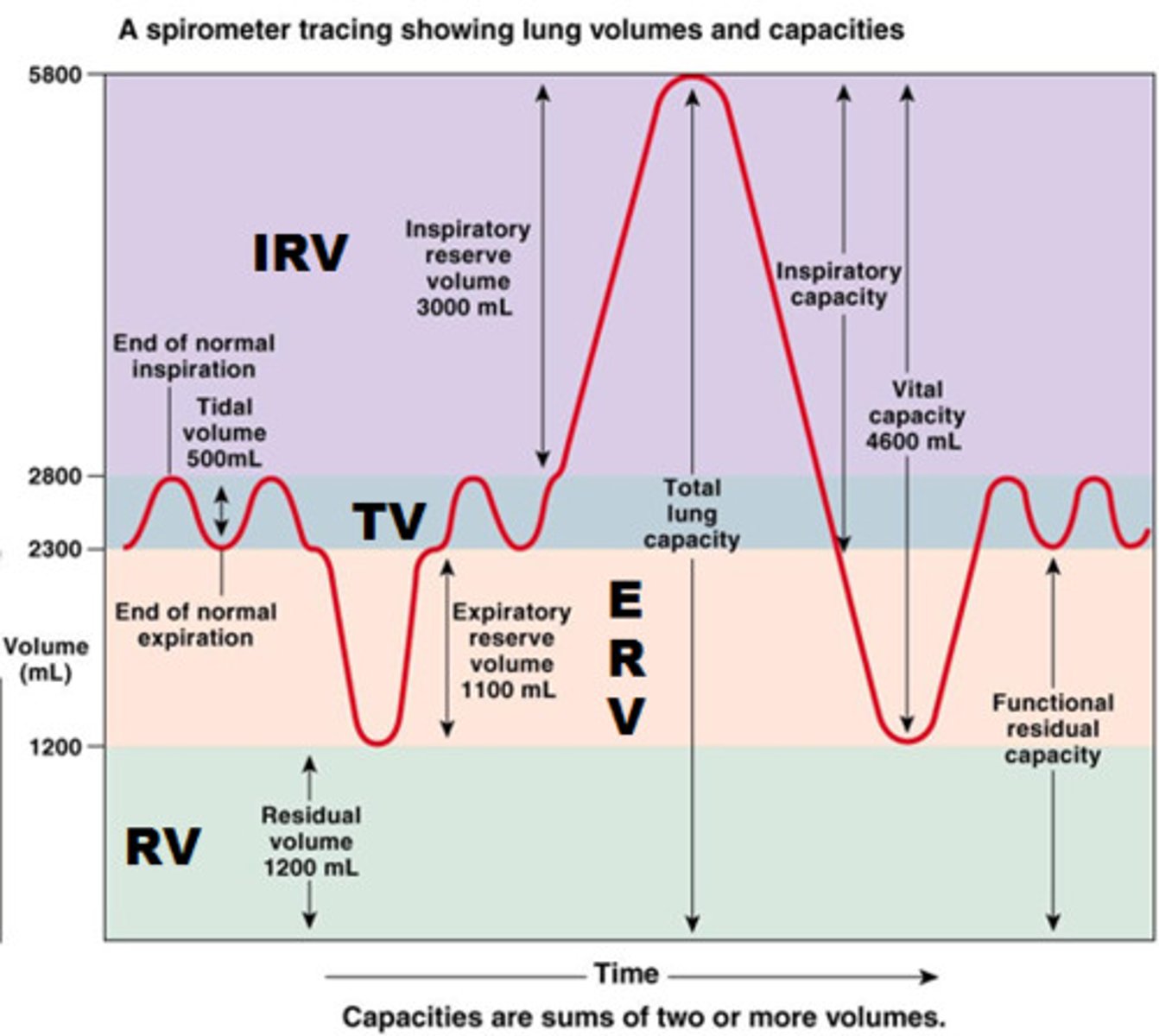
Functional Residual Capacity
expiratory reserve volume + residual volume
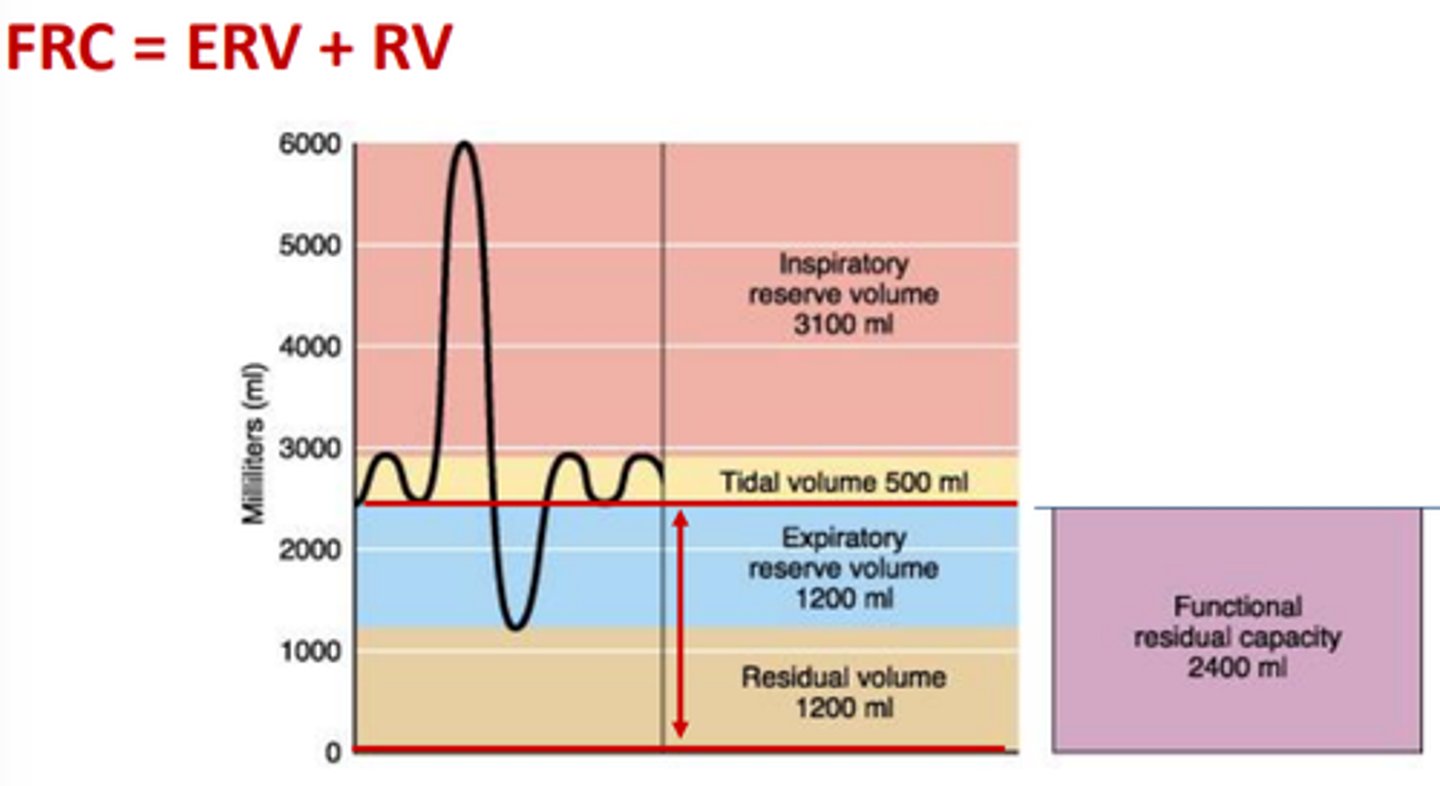
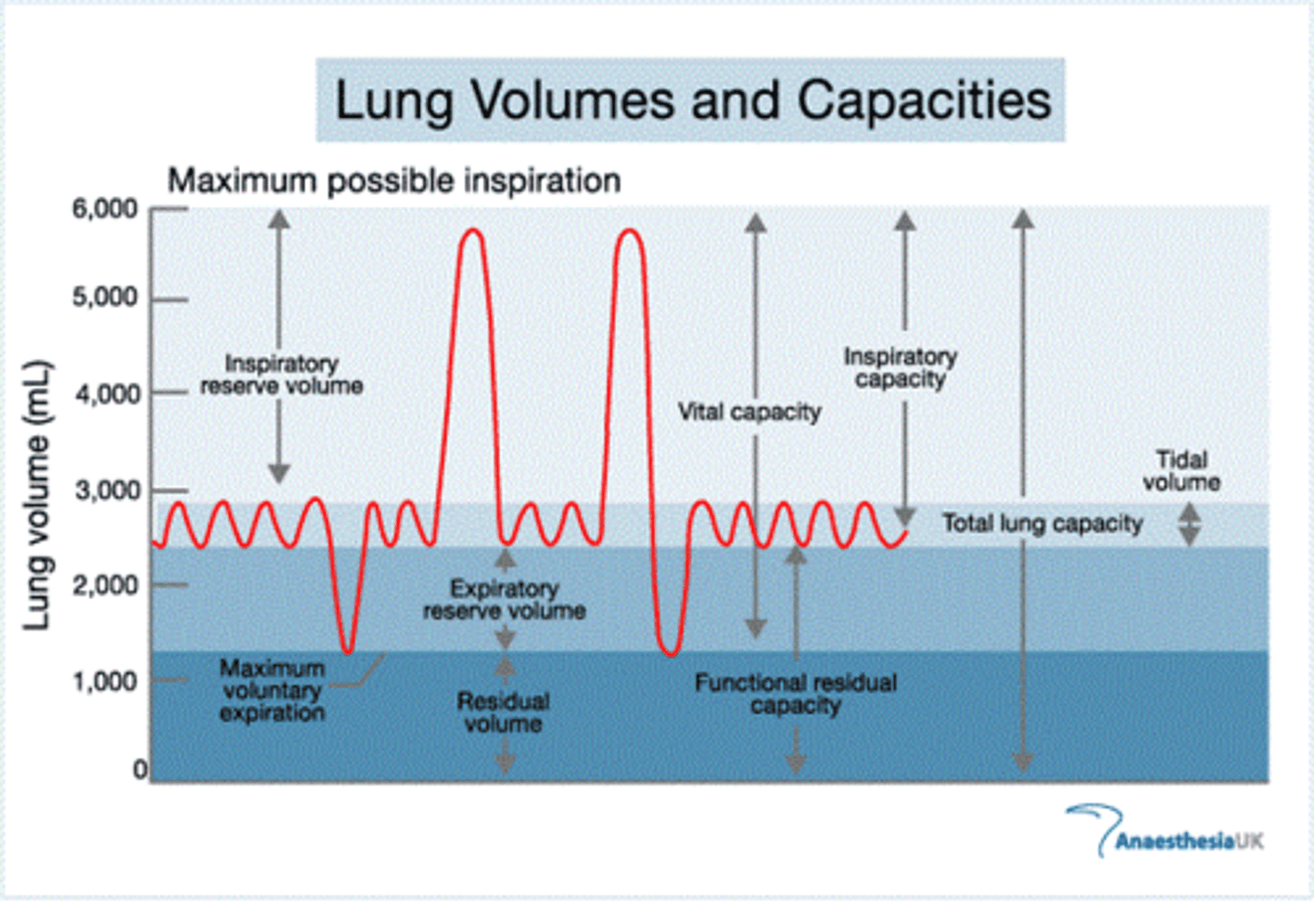
Total Lung Capacity
vital capacity + residual volume
FVC vs FEV1
FVC: forced vital capacity- max amount total air forced out
FVE1: amount of air forced out within the 1st second of expiration
NORMAL VALUE FOR FVE1, FVC, AND FEV1/FVC RATIO
FEV1 = 80% of predicted value
FVC = 80% of predicted value
FEV1/FVC = 80% of predicted value
FVE1/FVC VALUE THAT IS DEFINITIVELY OBSTRUCTIVE
What is the gray area FVE1/FVC value and a possible diagnosis?
DEFINITIVE OBSTRUCTIVE < 70%
if between 70-80% = possibly asthma
What is Obstructive Lung Disease?
What are (4) examples?
limitation of airflow due to partial or complete obstruction
emphysema, chronic bronchitis, bronchiectasis, asthma
Obstructive Lung Disease:
- Total Lung Capacity
- FVC
- FEV1
- FEV1/FVC ratio
TLC: normal
FVC: normal
FEV1: DECREASED
FEV1/FVC < 80%
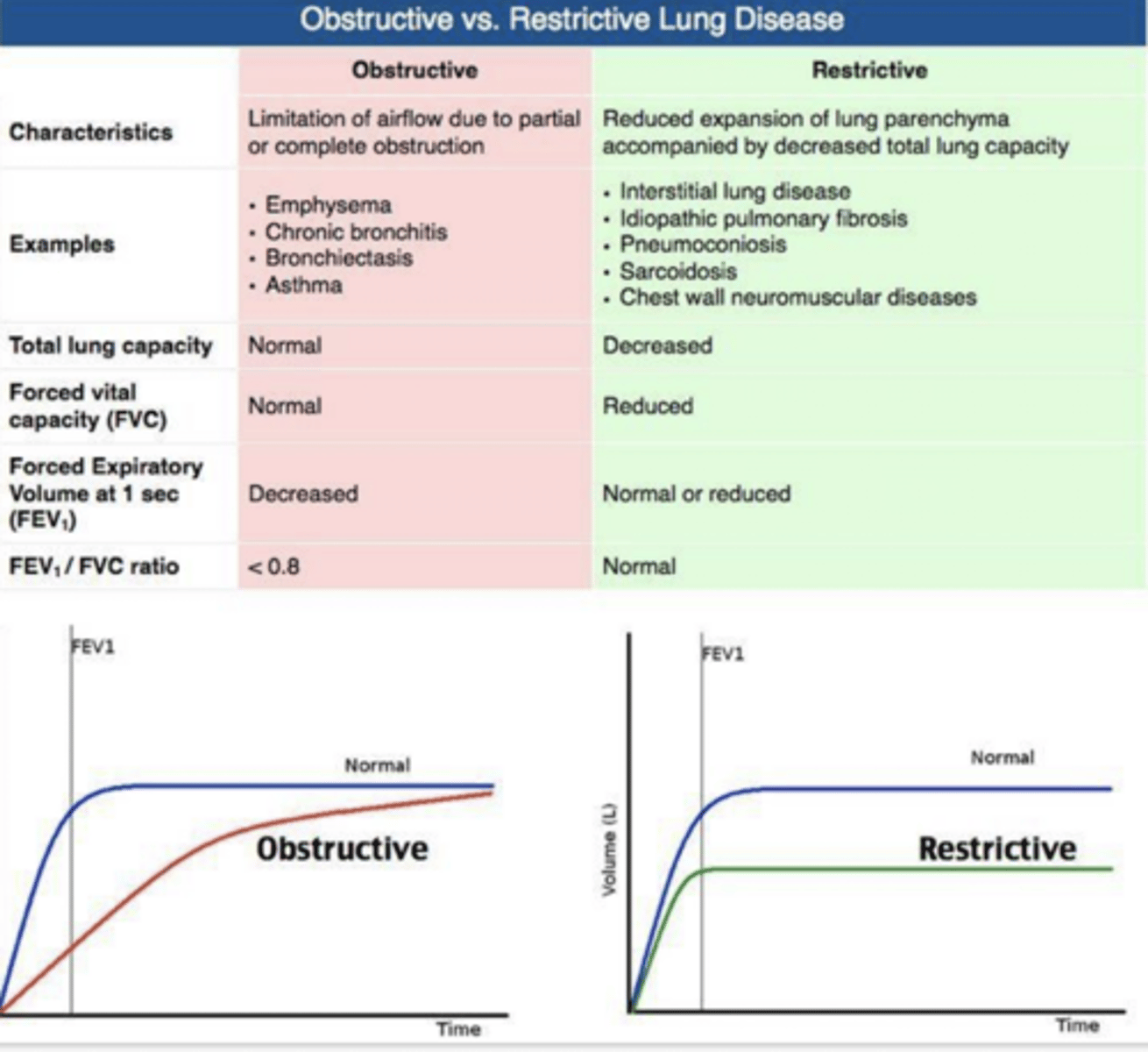
What is Restrictive Lung Disease?
What are some examples?
Reduced expansion of lung parenchyma accompanied by a decreased total lung capacity
ILD, Idiopathic Pulmonary Fibrosis, Pneumoconiosis, Sarcoidosis, Chest wall NM disease
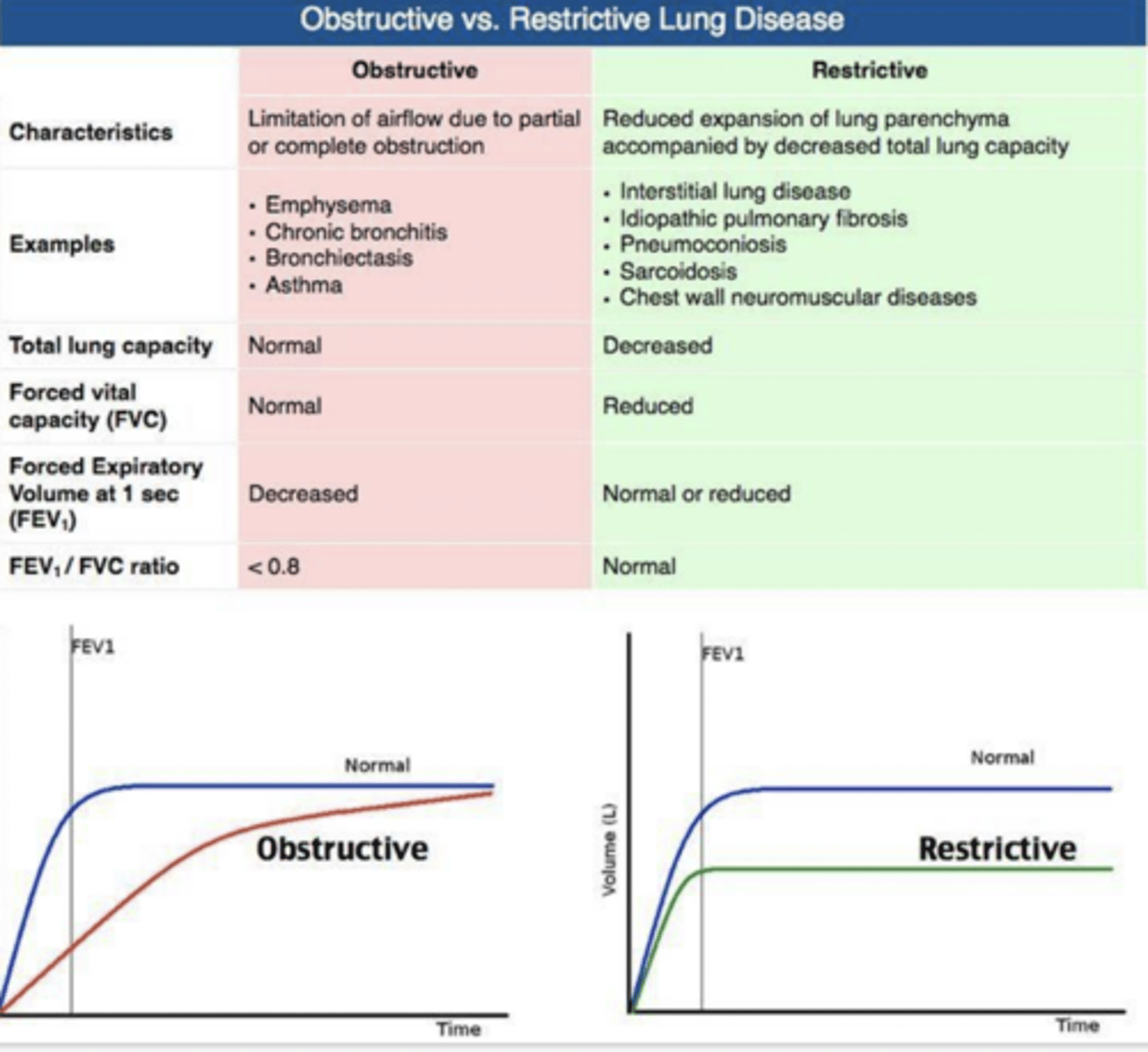
Restrictive Lung Disease
- Total Lung Capacity
- FVC
- FEV1
- FEV1/FVC ratio
TLC: DECREASED
FVC: REDUCED
FEV1: Normal/Reduced
FEV1/FVC: Normal
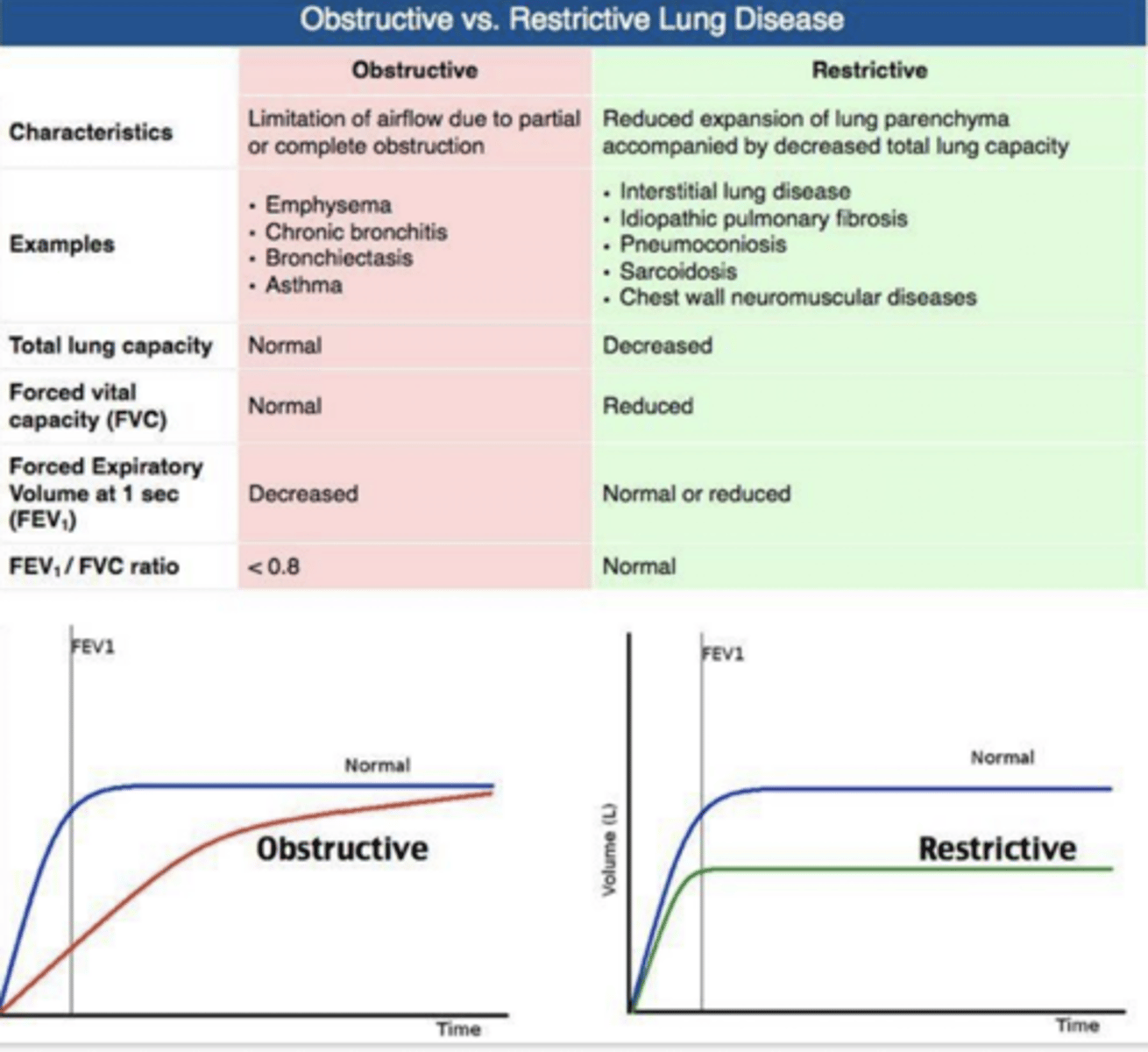
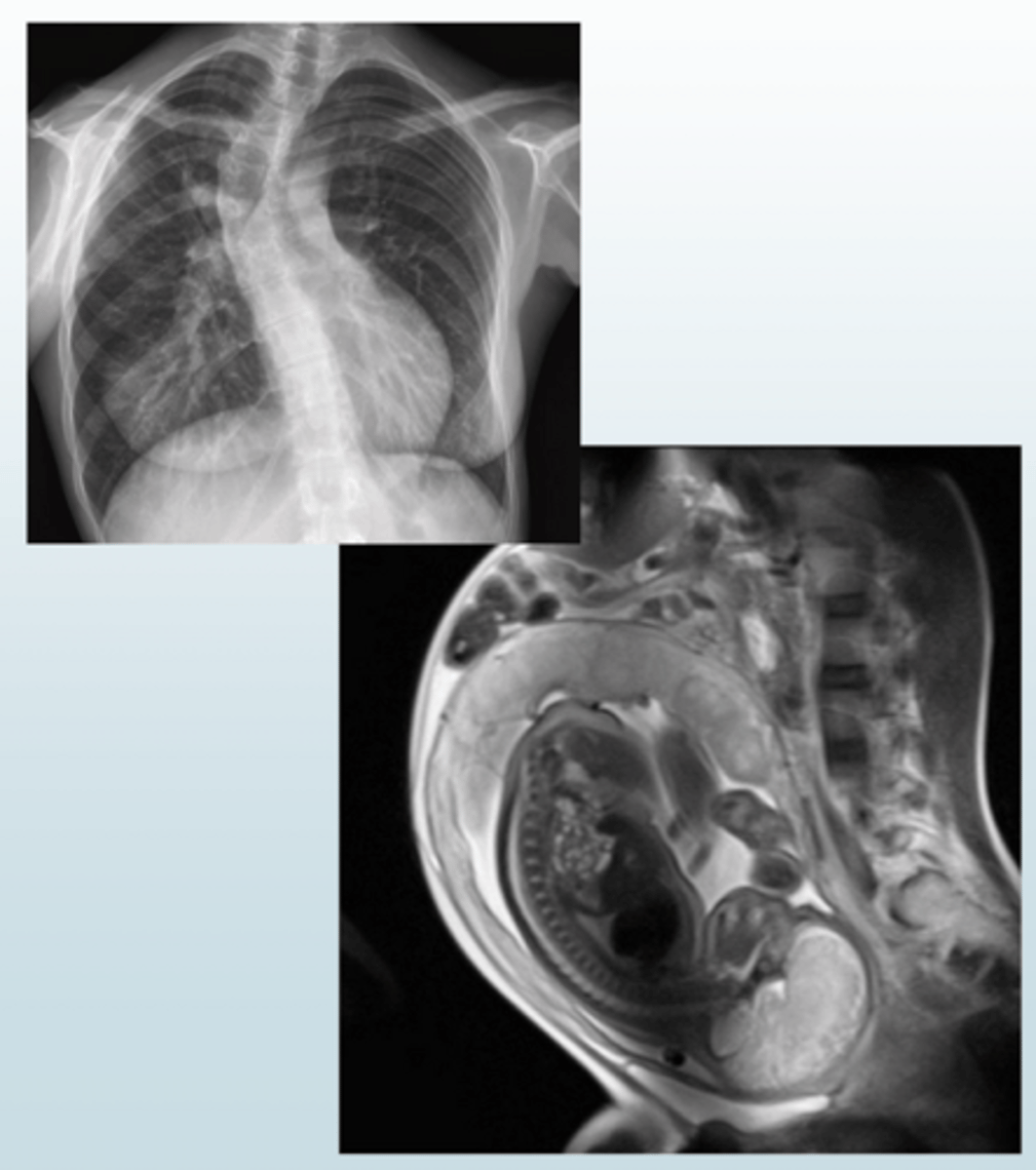
Kyphosis, Scoliosis, Obesity, Rib deformities/fractures, Cardiac enlargement, and Pregnancy are all _________ causes of _______ Lung Disease.
Extrinsic; Restrictive
What is characteristic about the movement of air in OBSTRUCTIVE disease?
air trapping!
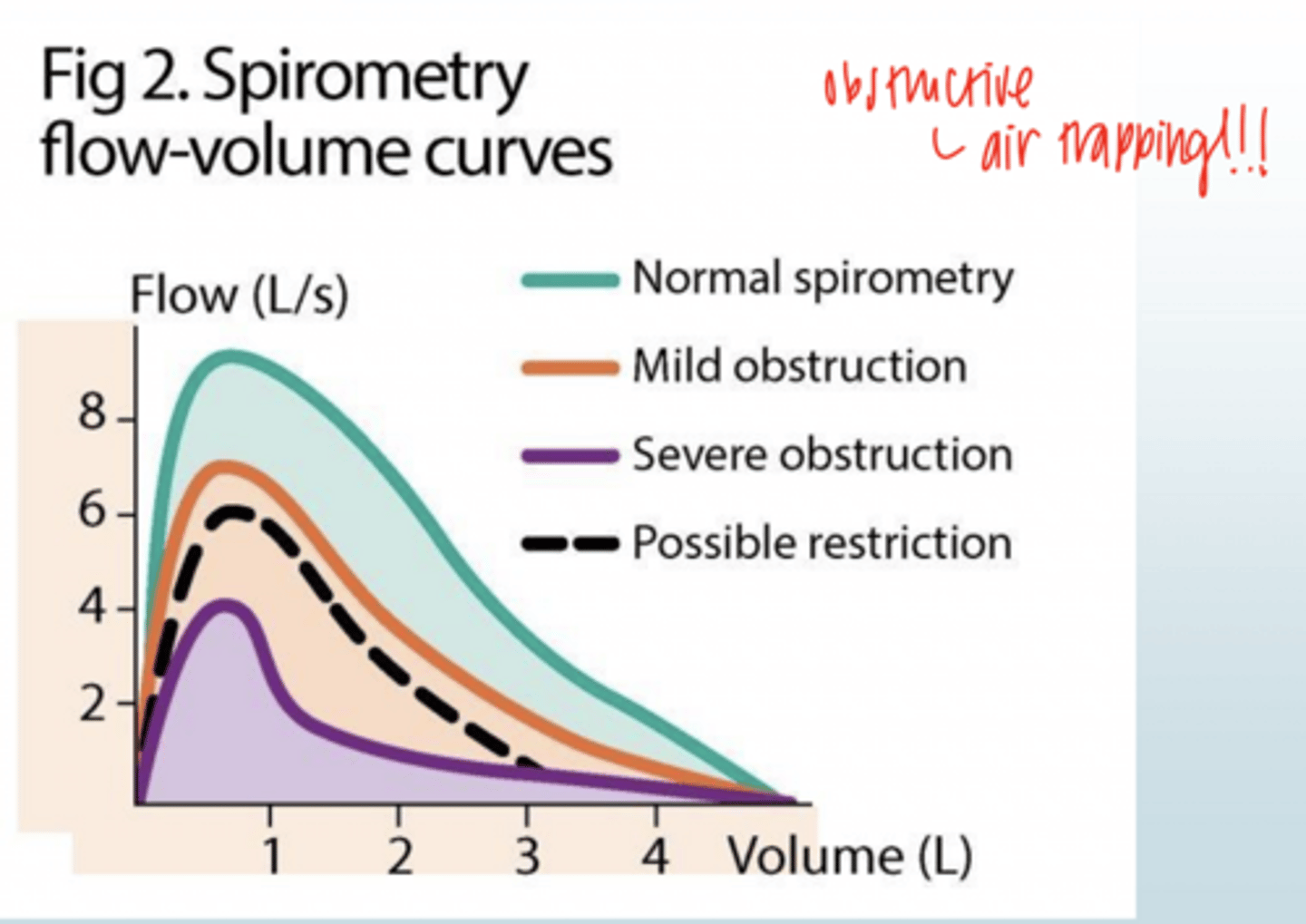
How to Diagnose a Patient that is in the Gray Area (FVE1/FVC).
What result would provide a diagnosis?
How should the patient present to perform this test?
if FEV1/FVC is 70-80% -> possible asthma
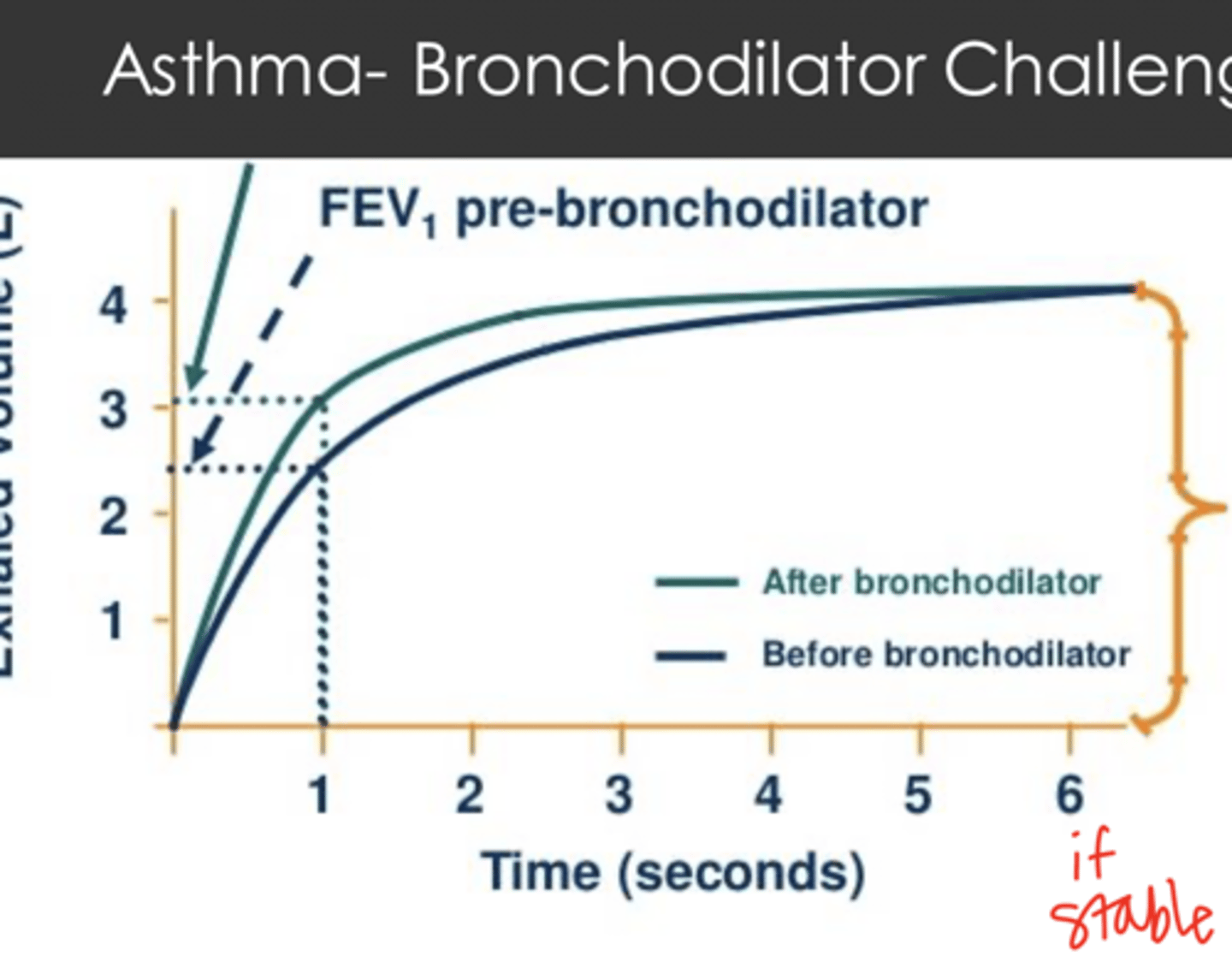
Bronchodilator Challenge:
- test patient before and after introducing a bronchodilator to see if there is improvement
- if > 12% of improvement = Asthma
Patient must be STABLE
FEV1/FVC VALUE INDICATIVE OF RESTRICTIVE AIRWAY DISEASE
What about FEV1 and FVC? Which is always indicative?
FEV1/FVC > 70%
- consider gray area testing
FEV1: mildly reduced or normal
FVC: < 80% (always reduced!)
- never reduced in obstructive lung dz.
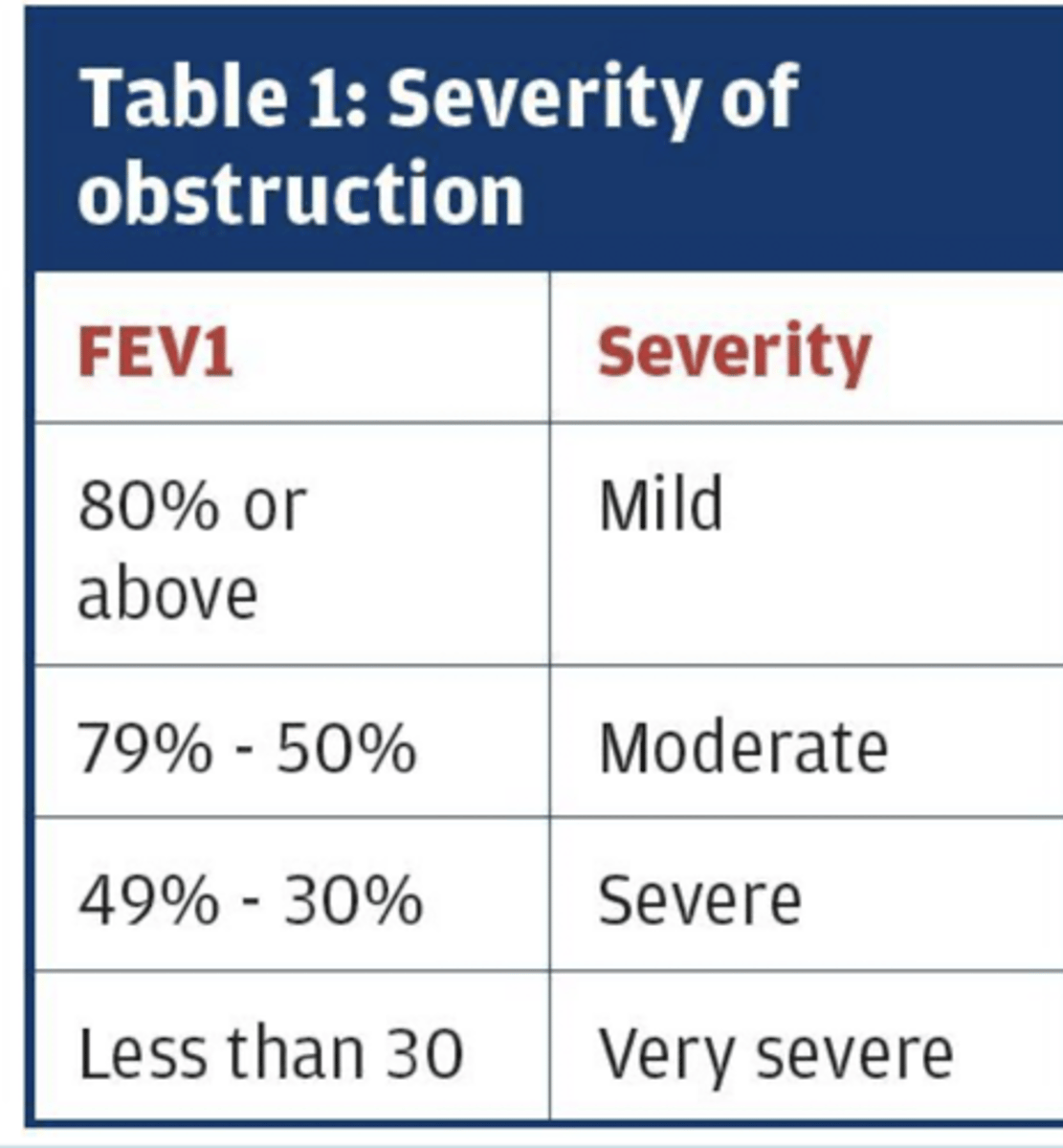
Give FEV1 Values Based on Severity of Obstructive Lung Disease
Mild
Moderate
Severe
Very Severe
mild >/= 80%
moderate: 79-50%
severe: 49-30%
very severe: < 30%
Relative CIs of Pulmonary Function Test
- (5) health conditions
Conditions that may be negatively impacted by increase in pressure:
1. blood pressure conditions/increases in myocardial demand
2. intracranial/intraocular pressures (ex: glaucoma, hydrocephalus shunt)
3. sinus/middle ear pressures (ex: sinus problems, sick, tubes)
4. intra-thoracic and intra-abdominal conditions (ex: surgery)
5. infection control (ex: COVID)