Lab Evaluation of Hemostasis Part II
1/37
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
38 Terms
How many platelets/hpf are normal?
8-10
DDx for Thrombocytopenia
1. Rickettsial diseases (Ehrlichia, Anaplasma)(dx by serum titers)
2. Immune mediated thrombocytopenia (IMT)(dx by abs on platelets; exclude other causes)
3. Lack of marrow production(neoplasia, aplasia, fibrosis- BM aspirate!)
4. DIC(Coags, FDPs, blood smear)
Rickettsial dz- Anaplasma/Ehrlichia
Many sp. Ehrlichia (ewingii,canis..) & Anaplasma (phagocytophilum , platys) Others- RMSF
Petechiae or mucosal hemorrhages
Thrombocytopenia may be severe(<10,000 uL)
In the chronic form with E.canis →
pancytopenia
Immune mediated Thrombocytopenia can be caused by…
A) Rickettsial dz
B) History of drugs
C) Mostly idiopathic
D) Neoplasia
Immune Mediated Thrombocytopenia(IMTP/ITP)
Similar to IMHA- but antibodies are directed against platelets
Common cause of thrombocytopenia in dogs ; rare in other sp.
Idiopathic or secondary (drugs, tumors, rickettsial dz)
Dx of exclusion
DISSEMINATED INTRAVASCULAR COAGULATION(DIC)
Like severe inflammation
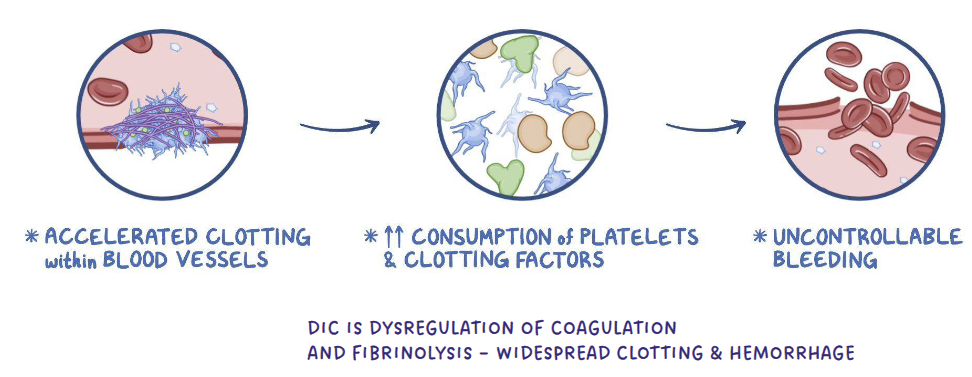
DIC- Thrombocytopenia
DIC- activation of widespread coagulation in the body → consumes coag factors and platelets → hypercoaguable
Widespread thrombosis throughout body at first; then hemorrhage because of depletion of platelets and coag factors (1’,2’)
Expected test results for DIC
Prolonged PT,PTT,ACT
Thrombocytopenia; 50-100k/ul
Increased FDPs/D-dimers(fibrin degradation products) Varies*
Blood smear: Schistocytes/keratocytes: Supports dx, absence does not exclude it
Decreased ATIII-Antithrombin III
Bone Marrow disease
Lack of bone marrow production → thrombocytopenia
Crowding out- Myelopthisis, can also be caused by myelofibrosis
Drugs-estrogen
Ehrlichiosis(damage stem cells in Bone Marrow)
Causes of bone marrow disease
Neoplasia of the bone marrow (leukemia,lymphoma)
Diagnostic test for bone marrow disease
Dx tests: Bone Marrow aspirate
vWd
Reported in many breeds of dogs. Cats & horses- but it’s rare
Doberman are the poster child (other include Shelties, German SHP, Scottish Terriers, mixed breeds)
Most common inherited disorder (diagnosed later in life)
3 forms (types I,II,III)
Expected test results for vWd
Performed if there’s an index of suspicion (breed, bleeding)
vWf assay – measures vWf in plasma
Will only bleed if [vWf]<30%
Platelet count will be normal (if the animal had severe blood loss, mildly decreased)
PT, PTT,D-dimers will be normal (this is a 1’ problem)
vWd
Decreased vWf = trait /carrier state (%)
70% and up = normal
50-69% grey area
x<50% @ risk of clinical dz
Platelet function defects inherited
Basset Hounds, Spitz- defect in IC signaling defect→px plt activation
Otterhounds, Great Pyrenees- defect in GPIIb/IIIa
Persian
Cattle: Simmental- IC signaling defect as above
Platelet function defects acquired
Hepatic/Renal failure, hyperproteinemia (>10mg/dL)
Drugs : Asprin & NSAIDs inhibit plt fn (COX inhibitors)
vwf
increases in pregnancy
Diseases of 2’ hemostasis
Vitamin K antagonism: The most common disease affecting 2’ hemostasis (coag proteins)
Liver failure: Reduced concentration of coagulation factors
DIC: Consumption of coag factors and platelets (both 1’& 2’)
Inherited defects: Hemophilia A (VIII) & B (IX) , C Factor XI
Oxidized Vitamin K needs to be reduced by an enzyme called Vitamin K epoxide reductase to…
become re-activated and act on other factors
Vitamin K epoxide reductase
Normally one vitamin K molecule is recycled many times by this enzyme and activates numerous coagulation factor molecules
Vitamin K antagonism
Vitamin K antagonists do not inhibit the action of reduced Vitamin K
Instead,
They inactivate the Vitamin K epoxide reductase enzyme that regenerates them
the concentration of active Vitamin K dependent factors will begin to decline depending on…
individual ½ life
Bleeding manifests when they drop to critical levels
Poisoning→ deficiencies in II,VII,IX,X
inactive forms continue to be produced →
build up
These inactive forms of II,VII,IX,X are referred to as ‘PIVKAS’(Protein Induced Vitamin K Antagonism)
Expected Results for vitamin K antagonist
Both PT,PTT are markedly prolonged
Factor VII has the shortest half-life so decreases first after poisoning
*If testing within 24-48 hrs PT may be prolonged before PTT
[Plt] usually normal, or mildly decreased if severe hemorrhage
[vWf] usually normal
D-dimers, usually normal; mild increase if cavitary bleeding with clots
clinical signs of vitamin K antagonism
Dyspnea (hemothorax, hemoabdomen)
Large hematomas at site of venipuncture
Causes of vitamin K antagonism
Rat poison (warfarin-like molecules)
Moldy sweet clover (cattle)
Severe cholestatic liver disease (Vit K factors are fat soluble; requires bile absorption from the gut)
Sulfaquinoxaline (coccidiostat)
How long will it take the animal with Vitamin K antagonism to respond to treatment?
Long enough to make new coagulation factors (days)
How do you know if you’ve treated long enough with Vitamin K for the toxin to clear?
Newer rodenticides have longer ½ lives- consider acute tx and re-test PT ~48 & 96 hrs after treatment stops
Liver failure
[Coag factors] by 2 mechanisms
Production or cholestasis(obstructed bile flow)→ fat absorption→ Vitamin K deficiency
Has to be severe liver disease ( Think icteric animals, high liver enzymes)
most animals will not bleed even with liver disease unless…
the procedure is invasive (liver biopsies)
Expected results of liver failure
Both PT,PTT could be prolonged
Platelet usually normal, or decreased depending on dz process
[vWf] usually normal
D-dimers- mild increase due to reduced clearance
Decreased production of urea, glucose, BUN
Increased ALP,ALT
Inherited defects doggie
All factors can be affected, Most commonly:
Factor VIII-Hemophilia A ** German Shepherds
Inherited defects cats
Factor XII- Cats
DIC
affects both primary and secondary
Inactive factors, produced by the liver require:
Vitamin K for carboxylation & activation
Active Vitamin K activates a coagulation factor →
Vit K molecule becomes oxidized and deactivated
The body has limited Vit K molecules all in the oxidized form → no more activation can occur so...
An animal ingesting Vitamin K antagonists initially has normal concentrations of fully activated factors, but no new factors can activate