COMD 4333
1/43
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
44 Terms
Auditory Processing
Auditory System Function & Energy Transformations
transform sound waves → action potentials that code frequency, intensity, and other characteristics of the sound waves
Sound Waves
mechanical energy (movement)
hydraulic energy (fluid)
electrical energy (nerve impulses)
neurochemical
action potentials
brain pathway
Outer Ear - Pinna, EAC, TM
Pinna: focuses sound energy into external auditory meatus
leads to movement of tympanic membrane (ear drum)
Middle Ear
air-filled cavity
Ossicles (malleus, incus, stapes) move in response to movement of tympanic membrane
Eustachian Tube: open into nasopharynx
equalizes pressure on both sides of tympanic membrane
Oval Window: entry into cochlea
covered by Stapes Footplate
vs. round window: other end of cochlea
Inner Ear - semicircular canals, vestibule, cochlea
bony labyrinth: bony cavities within temporal bone
membranous labyrinth housed within the bony labyrinth
Semicircular Canals (vestibular)
Vestibule (vestibular)
Cochlea (auditory)
Cochlea
inner ear part, 3 cavities
scala vestibuli
superior
Resiner membrane
Perilymph
scala media
cochlear duct
Basilar membrane
Endolymph: HIGH K+ concentration HIGH ON K
scala tympani
Perilymph
vestibuli, media, tympani
VMT victory my town
RB
Basilar Membrane
base: narrow and stiff
apex: broad and less stiff
basilar membrane arranged by FREQUENCY
different sound frequencies displace different regions of basilar membrane
base: high frequencies
apex: low frequencies
traveling wave created by movement of stapes in oval window
Organ of Corti
Movement of basilar membrane displaces organ of corti
1 row Inner hair cells - sensory
3 rows Outer hair cells – sensory & motor
Tips of hair cells close to tectorial membrane (tectorial membrane sits on top of organ of corti; organ of corti sits on top of basilar membrane)
4,500 IHC – each synapses with multiple spiral ganglion neurons
INNER HAIR CELLS SYNAPSE WITH MULTIPLE
20,000 OHC – multiple OHC synapse onto each spiral ganglion neuron
OUTER HAIR CELLS SYNAPSE ONE AT A TIME
Hair Cells
Stereocilia
Extend from hair cells
End in proximity to tectorial membrane
Arranged by length
Kinocilium being the tallest
stereocilia Connected by tip links
Action Potentials
Cilia bend toward kinocilium → tip links open → influx of K+ ions
K+ moves INTO hair cell leading to depolarization
Opens calcium channels → lets calcium INTO hair cells
Triggers RELEASE of neurotransmitter (glutamate)
Glutamate bind to receptors on Spiral Ganglion Neurons
cell bodies in spiral ganglion outside of the cochlea, axons create cochlear portion of CN VIII
Cilia bend toward kinocilium, tip links open, K moves in → depolarization, P move in hair cells, neurotransmitter released, it binds to spiral ganglion neuron
Cilia bend AWAY from kinocilium → tip links close → no influx (no further response from hair cell)
Efferent Signals to Outer Hair Cells
stimulation → activate microtubules, lengthen OHC cell bodies
electromotility - conversion of electrical energy into mechanical forces
increase the effect of basilar membrane movement & displacement of cilia
Enhance detection of low intensity sounds
Improves detection of sound in noise
100-fold increase in effect of actual basilar membrane movement
Coding Frequency
Frequency = pitch
Place coding: Hair cell location on basilar membrane
Base = high frequency; apex = low frequency
Characteristic frequencies: hair cells respond best (more action potentials) to specific sound frequencies
Tonotopic organization
Coding Intensity
intensity = loudness
number of action potentials
number of neurons sending action potentials
Coding Location
localization of sound
Interaural time and intensity differences
Sound wave travels around the head; reaches second ear later and a bit softer
Auditory Pathway Summary
Spiral ganglion axons → brainstem, synapse in dorsal & ventral cochlear nuclei
Cochlear nuclei → superior olivary complex (SOC)
SOC extend through lateral lemniscus
Synapse in inferior colliculus
Inferior colliculus → Medial Geniculate Nucleus (MGN in Thalamus)
MGN → Heschl’s gyrus/A1
A1 = posterior superior temporal gyrus
C-SLIMA
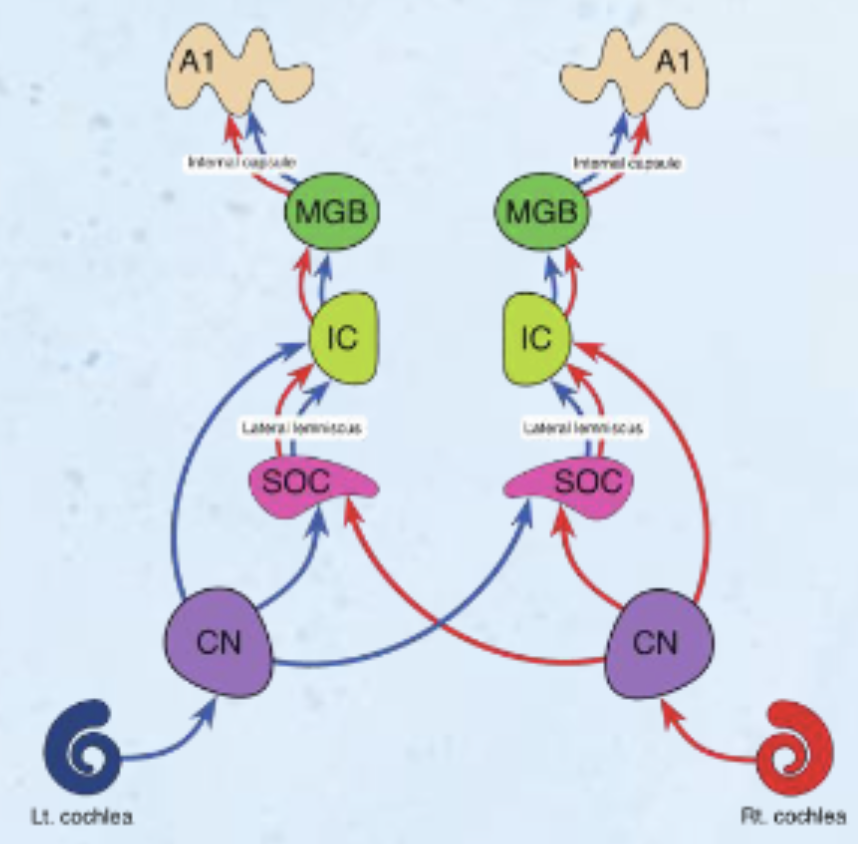
Cochlear Nuclei
Superior Olivary Complex
through Lateral Lemniscus
Inferior Colliculus
Medial Geniculate Body
A1 / Heschl’s Gyrus
cochlear nucleus, superior olivary complex, inferior colliculus, medial geniculate body, A1
Cochlear Nuclei
Ipsilateral, monaural processing in cochlear nuclei
80% cross over to contralateral SOC
All processing is binaural beyond cochlear nuclei
IPSILATERAL PROCESSING
Superior Olivary Complex
Receives information from both ears
Localizes sound based on time delay and intensity difference
SOC = LOCALIZATION
Lateral Lemniscus and Inferior Colliculus
Lateral Lemniscus
Tract between SOC and Inferior colliculus
Not a synapse
connects SOC and inferior colliculus SLIMA
Inferior Colliculus
Some signals sent from inferior colliculus to superior colliculus for auditory-visual integration
Medial geniculate nucleus (MGN) and A1/Heschl’s Gyrus
Medial geniculate nucleus (MGN)
In thalamus
From ipsilateral inferior colliculus
A1 / Heschl’s gyrus
From ipsilateral MGN
only cross over occurs after cochlear nuclei
Thalamic Nuclei called Medial geniculate nucleus (MGN)
Nuclei:
Medial geniculate nucleus
Connections to:
Brainstem auditory areas
Superior temporal gyrus
Heschl’s gyrus
Functions:
Auditory processing
Heschl’s Gyrus
heschl’s gyurs = Primary auditory cortex (A1)
Dorsal surface of superior temporal gyrus
Tonotopic organization
Auditory System Summary
Sound waves → Mechanical energy (movement)
Vibration/pressure from sound waves moves tympanic membrane and ossicles
Mechanical energy → Hydraulic energy (fluid)
Movement of tympanic membrane & ossicles causes movement of fluid in cochlea
Hydraulic energy → Electrical energy (nerve impulses)
Fluid movement causes movement of hair cells in cochlea
Electrical energy → Action potential
Hair cells release glutamate, exciting the auditory nerve (CN VIII)
● Brain Pathway
○ CN VIII → cochlear nucleus → superior olivary complex
→ lateral lemniscus → inferior colliculus → medial
geniculate body → auditory cortex (Heschl’s gyrus)
Hearing Loss
Conductive hearing loss
Problem with conduction of sound waves in outer/middle ear
Typically treatable
Causes: Ear infection, ear wax, damage to ossicles
Sensorineural hearing loss
Damage to sensory mechanism (cochlea – hair cells) or neural pathway
Causes:
Noise exposure
Acoustic neuroma and/or vestibular schwannoma
Tumor in inner ear, leading to hearing loss and/or vestibular dysfunction
Presbycusis: Age related hearing loss
Cortical Damage
fluent aphasia: unilateral LEFT hemisphere damage
Wernicke’s Area
impaired comprehension, jargon, empty speech
receptive aprosodia: unilateral RIGHT hemisphere damage
impairments in interpreting and/or producing prosody
Broca’s = Broken Speech (trouble producing speech, non-fluent, can comprehend fine) and Wernicke’s = Word Salad (fluent but nonsensical, trouble understanding).
Cortical Deafness and Pure Word Deafness
Cortical Deafness
Bilateral damage to Heschl’s gyrus
Inability to hear despite intact peripheral auditory system & pathways to cortex
Unilateral damage to Heschl’s gyrus has limited effects
a rare form of central hearing loss caused by damage to the brain's primary auditory cortex, usually from bilateral strokes or lesions in the temporal lobes. Patients appear profoundly deaf, unable to hear or distinguish sounds, yet have intact peripheral ears. It is characterized by severe auditory processing failures
Pure word deafness
Damage to white matter between primary and association areas
Speech sounds like noise; uninterpretable
Preserved reading, writing, speaking; intact auditory perception of noises/environmental sounds
Vestibular System
Structures in the inner ear
Semicircular canals
Utricle and saccule
Vestibular nuclei in brainstem
Projections to:
○ Superior Colliculus
○ Reticular formation
○ Cerebellum
○ Spinal Cord
○ Cortex
3 Semicircular Canals and Vestibule
3 Semicircular Canals
At right angles (X, Y, Z)
Anterior
posterior
lateral
Ampullae at base of each canal
Responsible for rotation and angular acceleration
SC - RA
Vestibule
otolith organs
Utricle
Saccule
responsible for linear acceleration
V - L
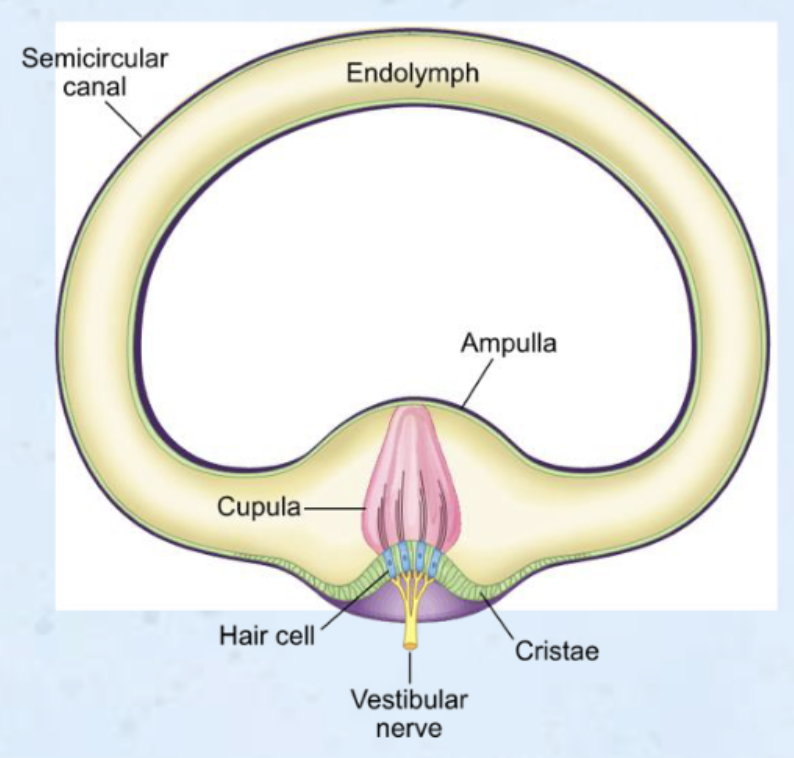
Semicircular Canals
ampulla: enlarged area at base of each semicircular canal
crista: sensory organ within the ampulla
crista contains hair cells
cupula: gelatinous structure encasing cilia
Ampulla Crista
movement of head causes → movement of endolymph in semicircular canals causes → movement of cilia TOWARD kinocilium
movement of cilia toward kinocilium
K+ channels open
depolarization
calcium channels open
triggers release of glutamate
glutamate binds to receptors on scarpa ganglion neurons (aka vestibular portion of CN VIII) creating EPSPs
Movement of cilia AWAY from kinocilium → closing of K+ channels → hyperpolarization & no signal
Vestibule Structures
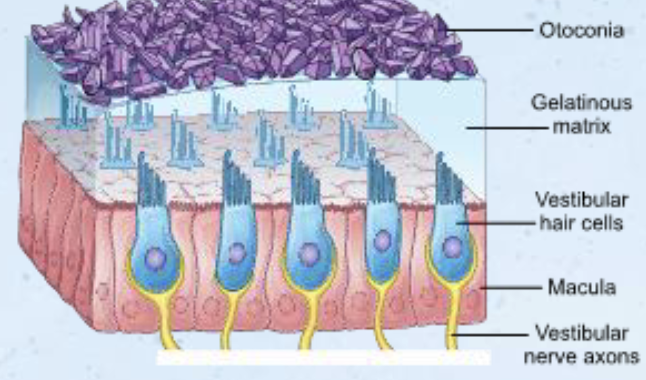
Hair cells embedded in macula (sensory receptor patch found in the vestibular system (utricle and saccule) of the inner ear, crucial for detecting linear acceleration, gravity, and head tilt.)
Cilia embedded in gelatinous structure (otolithic membrane)
Otoconia: calcium carbonate crystals on surface of otolithic membrane
Otolithic organs:
Utricle (horizontal) UH
Saccule (vertical) SV
Movement of head → shifting of otolithic membrane
Enhanced by weight of otoconia
Cilia bend toward kinocilium → open K+ channels → depolarization → open Ca2+ channels → release of neurotransmitter
Utricle positioned horizontally
Saccule positioned vertically
Allows us to detect linear movements in these planes
Vestibular Nerve and Nuclei
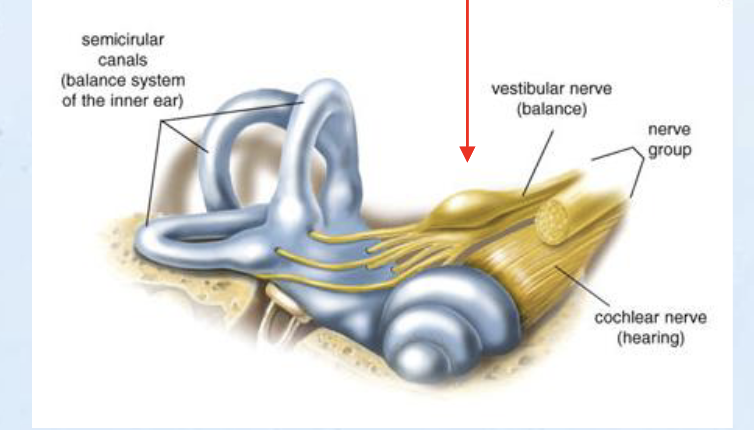
Vestibular nerve
Cell bodies in Scarpa’s ganglion (vestibular potion of CN VIII)
Join with auditory nerve fibers
Synapse in vestibular nuclei in brainstem
Vestibular Projections
from vestibular nuclei (in brainstem) to
superior colliculus in midbrain
eye movement, head/eye position, visual fixation with head movement
cerebellum
vestibulocerebellum
coordinates movement and reflexes, maintains balance
spinal cord
integrated connections for balance, equilibrium, proprioception
reticular formation
visceral-autonomic activities
cause of sea-sickness/motion sickness
Olfaction and Gustation Overview
chemical senses: smell and taste
chemoreceptors
closely related
combine to form our perception of different flavors
Olfactory System
Olfactory Epithelium
Superior surface of nasal cavity
Olfactory Neurons
Continually regenerated
4-8 week lifecycle
Supporting Cells
Secrete mucous
Replaced every 10 minutes
olfactory epithelium, olfactory neurons, supporting cells
Odors
Odorants: chemical compounds
Dissolve in mucous and bind to olfactory neuron cilia
Humans have 350 odorant receptors
Distinct smells identified by population coding
Patterns of action potentials from groups of olfactory neurons
Combine to form over 1 trillion Specific odors
Olfactory Pathway
1st order neurons: in olfactory epithelium
odorants bind to receptors
triggers cascading process to depolarize cell
axons = olfactory nerve (CN I)
synapse onto glomeruli in olfactory bulb
2nd order neurons: in olfactory bulb
travel down olfactory tract
axons extend to olfactory cortex
olfactory epithelium → olfactory bulb down oflactory tract extend to olfactory cortex
Olfaction
action potentials stop when odors diffuse or enzymes destroy odorants
olfactory neurons habituate
stop responding after time
Olfactory Cortex
Olfactory cortex made of 3 parts:
Piriform cortex
perirhinal cortex
entorhinal cortex
Smell is the only sense that does NOT make a stop in the thalamus before reaching the sensory cortex
Though there are branches that connect to mediodorsal nucleus after processing
Olfactory Processing
connections to:
Orbitofrontal cortex
Odor discrimination
Impacts motivation, emotion, memory
Hypothalamus
Appetite, eating/drinking
Limbic system (amygdala, cingulate gyrus)
Emotion & motivation
Hippocampus
Memory
orbitofrontal cortex, hypothalamus, limbic system, hippocampus
Olfactory Impairments
anosmia: loss of sense of smell
conductive anosmia: caused by blockage of transmission
sensorineural anosmia: caused by damage to neurons/pathways involved in smell
TBI, AD, PD, healthy aging
Hyposmia: reduced sensitivity to odors
Dysosmia: alterations in olfactory perception
Parosmia: distorted perception
Phantosmia: olfactory hallucination
Cacosmia: perception of foul smell
Gustation: Sense of Taste
5 basic tastes
Bitter
sweet
sour
salty
umami
Taste perception is a combination of taste, smell, temperature, and texture
Influenced by level of hunger and cognitive expectations
Cortical responses differ based on viscosity, temperature, etc. even if taste is held constant
Taste Receptors
papillae
Each houses hundreds of taste buds, which house 50-150 taste receptors
Most papillae located on on tongue
Some in pharynx, palate, epiglottis
papillae, inside is taste buds, inside is taste receptors
Tastants (chemicals)
chemicals that stimulate taste receptors
Taste cells respond to multiple tastants but are tuned to respond best to specific tastes
Specific flavors created by patterns of action potential
Gustatory Pathway ANTERIOR INSULA
1st order neuron
receptors (dendrites) receive signals from taste receptors
cell bodies in CN ganglia
facial (CN VII): anterior 2/3 of tongue
Glossopharyngeal (CN IX): Posterior 1/3 of tongue
Vagus (CN X): Pharynx
Axons enter medulla and synapse in gustatory nucleus
2nd order neuron:
Cell bodies in gustatory nucleus
Most extend to VPM
Others → brainstem nuclei (swallowing, digestion, salivation, respiration, gagging, etc.)
3rd order neuron:
Cell bodies in VPM go to:
Anterior insula (gustatory cortex/G1)
Inferior/orbitofrontal cortex
Hypothalamus
Limbic system
Gustatory Impairments
Taste cells regenerate every 2 weeks, but cranial nerves do not
Ageusia: Loss of sense of taste
Dysgeusia: reduced/altered sense of taste
Impairments often lead to loss of appetite and weight loss
-usia