chapter learning objectives 17.1-17.5
1/24
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
25 Terms
Describe the position of the heart in the thoracic cavity
heart is situated in the chest slightly to the lt side in a subivision of the thoracuc cavity
describe the basic surface anatomy of the chambers of the heart
heart consists of 4 hollow chambers: superior rt and lt atria and inferior rt abd lt ventricles
explain how the hearts functions as a double pump and why this is significant
the heart functions as a duble pump because it is divided into functionally into rt and lt sides.
Rt side pumps deoxygenated blood to the lungs (pulmonary circuit)
lt side pumps oxygenated blood to rest of the body (systemic circuit)
17.2 heart anatomy and blood flow pathway
describe the layers of the pericardium and heart wall
fibrous pericardium- a saw w/ 2 components a tough outer layer that attaches the heart to surrounding structures
serous pericardium-thin inner serous membrane that produces serous fl
parietal pericardium-outer layer is fused to the inner surface of the fibrous pericardium
visceral pericardium- inner layer aka epicardium
Describe the location and function of the coronary circulation and great vessels
great vessels-bring blood to and away from the heart, are the largest ones in the body
coronary circulation-set of arteries, veins, and capillaries that supply blood to and drain blood from the myocardium of the heart
Describe the structure and function of the chambers, septa,valves, and other structural features of the heart
Trace the pathway of blood flow through the heart, and explain how structures of the heart ensure that blood flows in a single direction
figure 17.8
17.3 Cardiac muscle tissue anatomy and elctrophyiology
Describe the histology of cardiac muscle tissue, and differentiate it from that of skeletal muscle
cardiac muscle cells have striations, means that the cells have alternating light and dark bands
skeletal muscle cells results from fusion of multple immature myoblast, causing to form long multinucleated fibers as for cardiac muscle cells they are short, wide cells, that contain a signle nucleus
Describe the phases of the cardiac muscle cell action potential, including the ion movements that occur in each phase, and explain the importance of the plateau phase
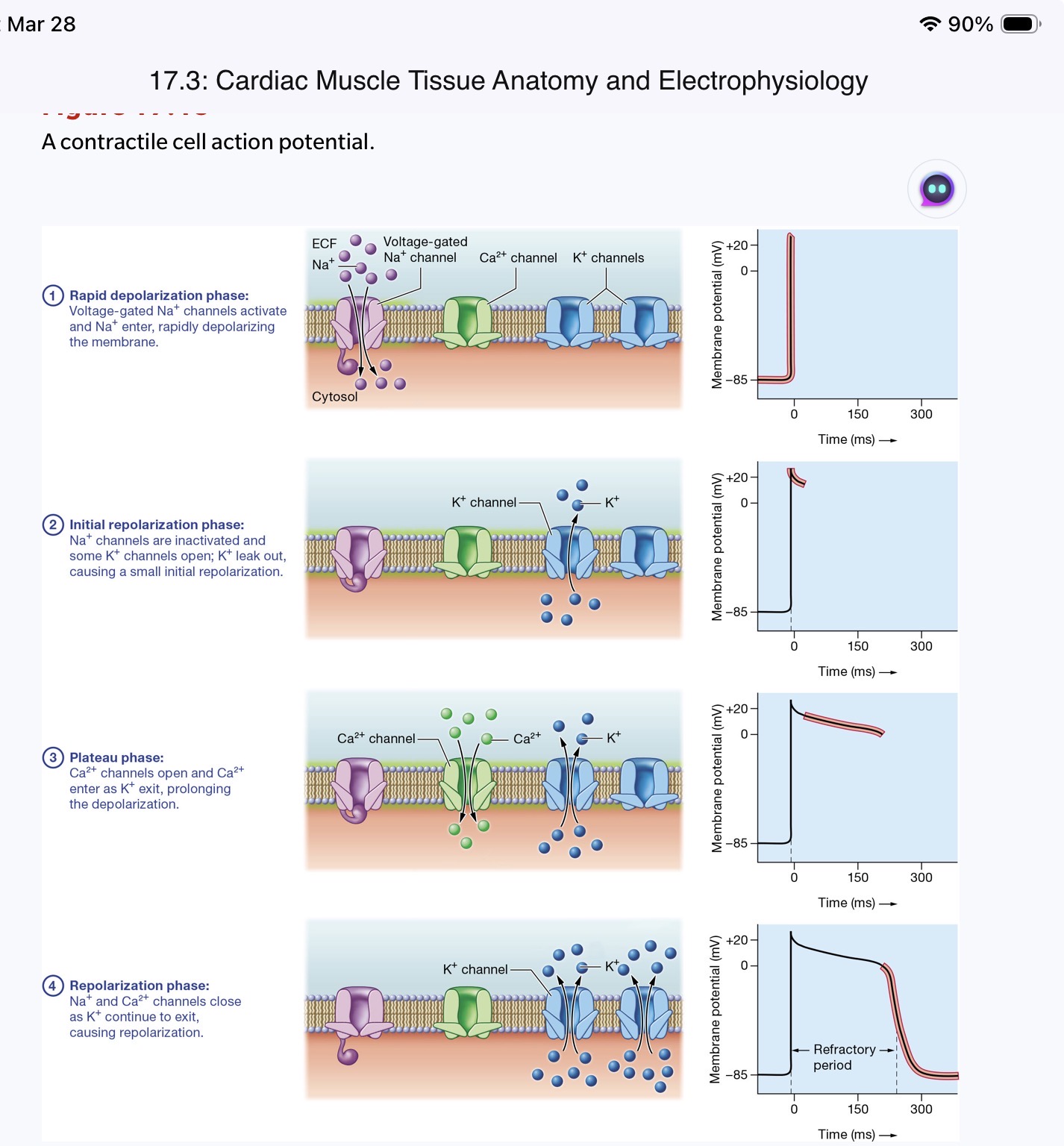
Contrast the way action potentials are generated in cardiac pacemaker cells, cardiac contractile cells, and skeletal muscle cells
Describe the parts of the cardiac conduction system, and explain how the system functions
SA node, AV node, Purkinje fiber system
SA node:cluster of pacemaker cells in the sup RA that normally sets the pace for the heart
AV node: cluster of pacemaker cells in the Inf RA that delays the propagation of the cardiac action potential from the atria to the ventricles
Purkinje fibers: group of atypical pacemaker cells located in the ventricles
Identify the waveforms in a normal electrocardiogram (ECG), and relate the ECG waveforms to electrical activity in the heart
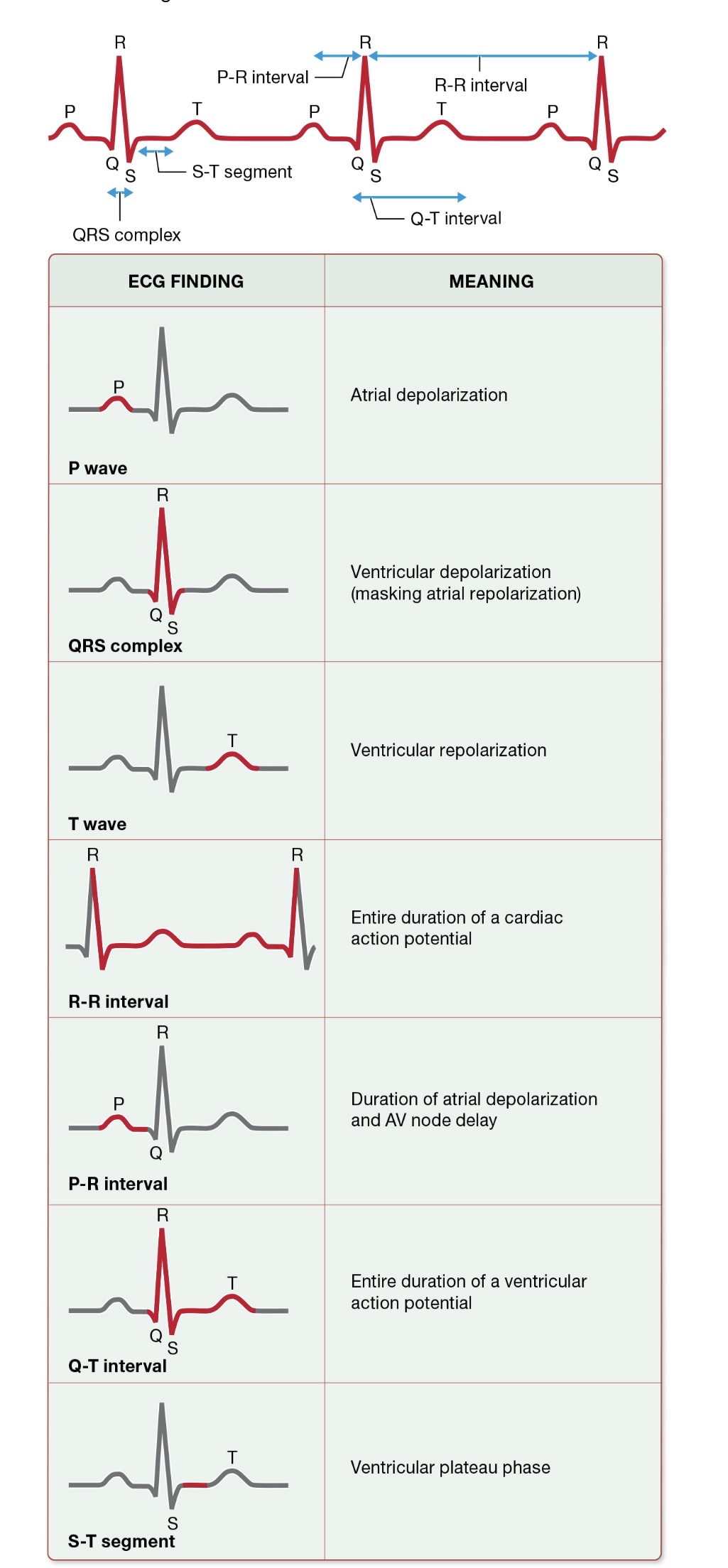
17.4 Mechanical Physiology of the Heart: cardiac cycle
Describe the phases of the cardiac cycle (17.17)
ventricular filling phase
isovolumetric contraction phase
ventricular ejection phase'
isovolumetric relaxation phase
Relate the opening and closing of specific heart valves in each phase of the cardiac cycle to pressure changes in the heart chambers
17.17
Relate the heart sounds and ECG waveforms to the normal mechanical events of the cardiac cycle
17.20
Compare and contrast pressure and volume changes of the left and right ventricles and the aorta during one cardiac cycle
17.18
17.5 Cardiac Output and Regulation
Define and calculate cardiac output, given stroke volume, heart rate, and end-diastolic and end-systolic volumes
CO: the vol. of blood pumped itno the pulmonary and systemic circuits in 1 min
ex: EDV-ESV=SV
120 mL-50mL=70mL
find the CO:
72 bpm*70mL/beat=5040 mL/min or 5 L/min
HR * SV= CO
Describe the factors that influence preload, afterload, and contractility, and explain how they affect cardiac output
preload: imposed on the heart before it contracts
contractility: ability to generate tension
afterload: agaisnt which the heart pumps as it contracts
preload involves EDV whereas contractility ans afterload afftect the ESV
Explain the significance of the Frank-Starling law for the heart
the signigicance of Frank-Starling low of the heart is cardica physiology that describes how the hearts SV is influenced by the degree of stretch of the ventricular muscle cells before contraction
Discuss the influence of positive and negative inotropic and chronotropic agents on stroke volume and heart rate, respectively
Predict how changes in heart rate and/or stroke volume will affect cardiac output
increase in afterload therefore generaaly causes a decrease in SV, which in turn leads to a rise in the ESV of the ventricles.
decrease in afterload generally corresponds to a higher SV and a lower ESV