Emerging hallmarks and enabling characteristics of cancer
1/17
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
18 Terms
How does metabolism of normal cells differ from cancer cells?
- Cancer cells obtain energy from alternate sources whilst normal cells don't.
- Allows normal cell to use metabolites for other processes.
What is the Warburg effect?
- Cancer cells will undergo anaerobic glycolysis even in the presence of oxygen.
- This metabolic adaptation causes increased glucose uptake and lactate production.
- This provides cancer cells with the energy required for rapid proliferation.
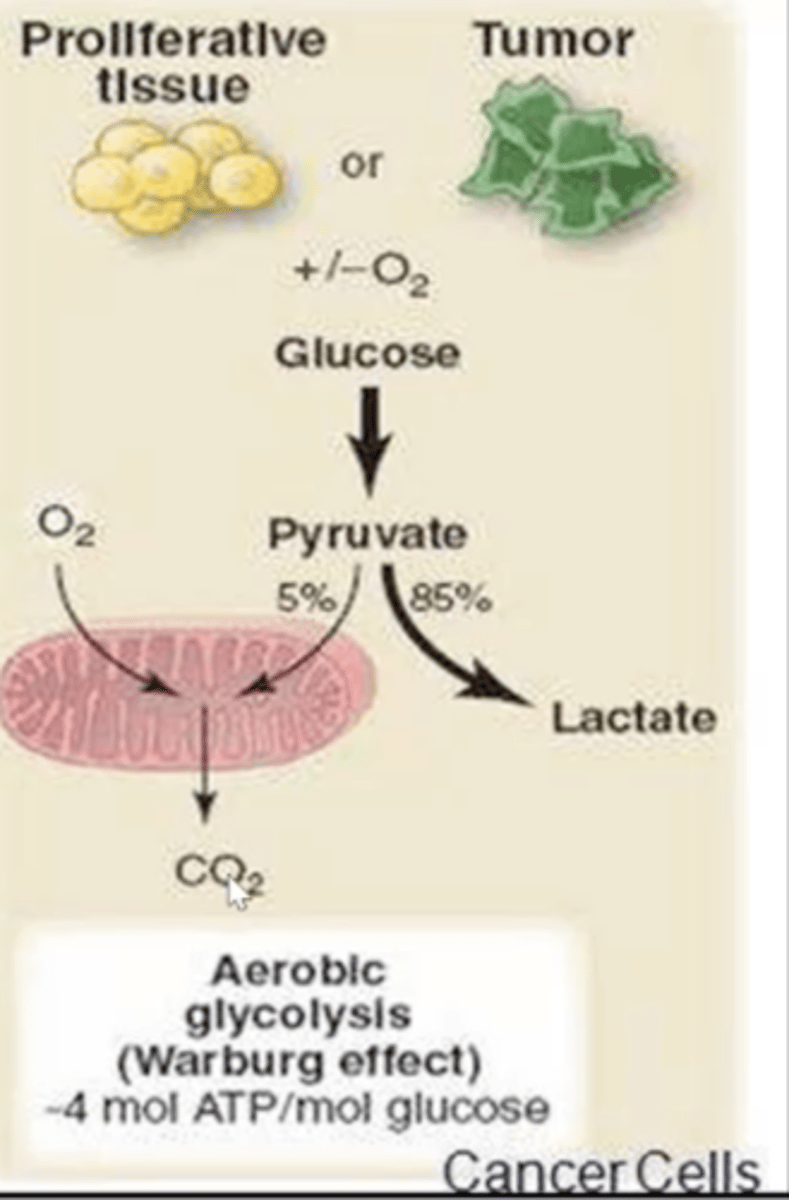
Why do cancer cells use the Warburg effect even though it less efficient than aerobic?
Generates metabolic intermediates for biosynthesis and maintaining a more acidic microenvironment for tumor progression.
How do NK cells kill cancer cells?
- Detect downregulation of MHC-1 in tumour cells.
- Can signal directly to T cells to activate CD8 cells.
- CD8 cells recognise peptides derived from cytoplasmic proteins that are bound to MHC1 to kill cancer cells.
How do CD8 T cells kill tumour cells?
Secretory and non-secretory method
What is the secretory mechanism of CD8+ T-cells to kill tumour cells?
They release perforin and Granzymes which pierce holes into the plasma membrane which kill the pathogens.
What is the non-secretory mechanism of CD8+ T-cells to kill tumour cells?
Once the T-cell Receptor has bound to the MHC-1 receptor the CD8+ cell also has a Fas ligand (FasL) which can bind to the Fas receptor on the pathogen which initiates apoptosis in the target cell.
What are tumour specific antigens?
An antigen that causes the tumour e.g., mutation of TSGs or oncogenes that lead to altered protein production.
What is a tumour antigen?
A protein with an abnormal structure caused by a mutation.
What is a tumour associated antigen?
Present on tumour cells and some normal cells and is a mutation in a gene unrelated to cancer formation but causes synthesis of abnormal proteins.
How do tumour cells stop T-cell killing?
- Cancer cells can stop the MHC antigen-processing complex and prevent loading of antigenic peptides onto MHC molecules, preventing the recognition of tumour antigens.
- Tumour cells can upregulate expression of PDL1 that can bind to PD1 on T-cells and deactivate them.
- Cancer cells can produce cytokines like IL-10 and VEGF that cause immunosuppression by recruiting T-regs and myeloid derived suppressor cells.
How can tumour cells take energy away from immune cells?
They compete for glucose with them.
How can cancer cells induce an immunosuppressive environment?
- Cancer cells have a lower pH environment due to their metabolism which can affect T-cell maturation.
- This also affects recruitment of MDSCs.
- This causes immunosuppression.
What are anti-tumour and pro-tumour cells?
Cells of the immune system can have both tumour antagonising and tumour-promoting effects.
Describe pro-tumour cells.
- Found in hypoxic environments.
- Release pro-angiogenic cytokines and enzymes.
- Produce reactive oxygen and nitrogen species which cause more mutations.
- Secrete a wide range of metalloproteinases which breakdown extracellular matrix which promotes metastasis.
Describe anti-tumour cells.
- Activated by LPS or IFN-γ.
- Produce cytokines and chemokines which stimulate immune system e.g., increase lymphocyte numbers.
- Cause tumour cell lysis.
- Secrete specific metalloproteinases that are required.
How do macrophages contribute to tumourigenesis?
- Release chemotactic factors that attract monocytes.
- Monocytes differentiate in macrophages.
- Tumour associated macrophages (TAMs) then work causing tumourigenesis.
How do tumour associated macrophages (TAMs) cause tumourigenesis?
- They release angiogenic factors e.g., VEGF and IL-8.
- Also release metalloproteases that digest the extracellular matrix.
- Also release mitogenic factors that promote tumour cell proliferation.