Bone Growth & Maintenance
1/26
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
27 Terms
Surface of bone
There are many active osteocytes (bone cells) upon the surface of bones surrounded by a collagen fibre matrix.
Collagen fibre matrix
Found on the surface of bone.
Function:
allows other molecules to attach onto bone (e.g inorganic salt crystals)
Salt crystals
Found on the surface of bone attached to the collagen fibre matrix.
Formation:
Calcium carbonate + Calcium phosphate → Hydroxyapatite (salt crystal)
Hydroxyapatite
A salt crystal formed within the collagen fibre matrix of bones.
Function:
Incorporates other minerals into bone (e.g Magnesium hydroxide, fluoride, sulphate) as hydroxyapatite calcifies/crystallises on the collagen fibres.
Provides the hardness and strength of bone
What makes bones hard and strong?
Hydroxyapatite
What makes bone flexible?
Collagen fibres (prevents bones from becoming brittle)
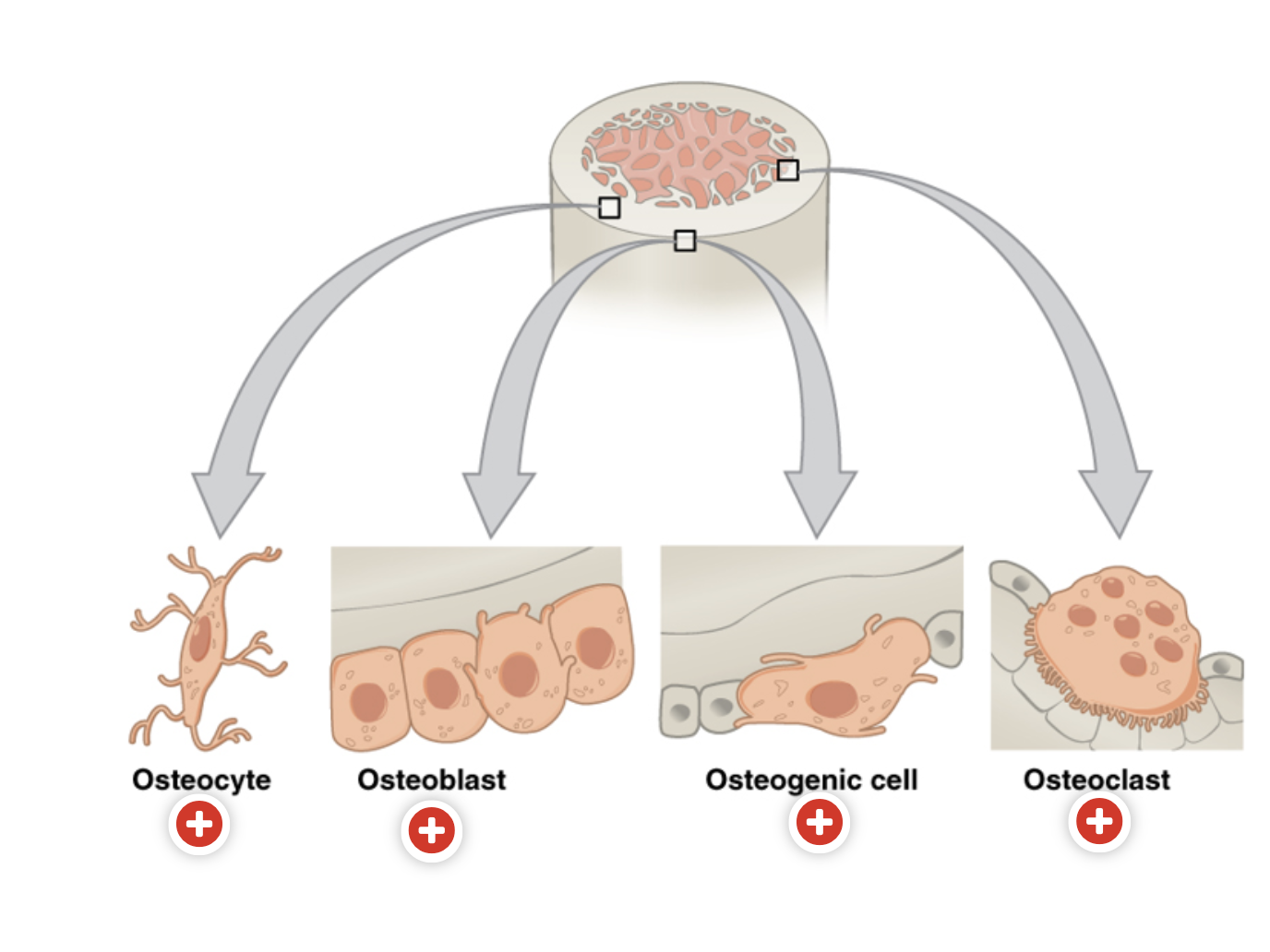
Types of osteocytes
Osteoblasts
Osteogenic cells
Osteogenic cells
Osteoclasts
Osteoblasts
Function:
Forms new bone. By producing and secreting more of the collagen fibre matrix & calcium salts. Osteoblasts themselves do not divide.
When the collagen fibre matrix calcifies around them, osteoblasts become trapped. Cell structure changes to become an osteocyte.
Where is found:
Within the growth plate/epiphyseal plate.
Osteocyte
Primary mature bone cell, most common type.
Function:
Maintains the mineral concentration of the collagen fibre matrix by secreting enzymes.
Communicates with other osteocytes to receive nutrients through long channels.
Do not divide.
Osteogenic cells
Function:
Undifferentiated stem cells.
Can differentiate rapidly into osteoblasts.
Where is found:
Immature osteogenic cells are found in the periosteum and bone marrow.
Osteoclasts
Function:
Breaks down bone through bone resorption.
Where is found:
Bone surfaces
Structure:
Contain many nuclei.
Originate from macrophages & monocytes (two types of white blood cells).
Bone tissue turnover
Where new tissue is constantly being formed and old and injured (or even unnecessary bone) is dissolved either for repair or to release the calcium.
Balance is maintained by osteoblasts (bone former) and osteoclasts (bone remover)
Bone growth in childhood
The growth/epiphyseal plates are continuously growing columns of chondrocytes (cartilage cells that produce collagen).
Chondrocytes
New chondrocytes:
Lay down new cartilage that lengthens the bone.
Old chondrocytes:
Found closer to the diaphysis, where they die. The spaces left where they die allow osteoblasts to enter.
What deactivates the epiphyseal/growth plate causing it to form into the epiphyseal line?
Sex hormones within adolescence. Thus linear bone growth stops after adolescence.
Does bone tissue stop changing after adolescence and the epiphyseal line is formed?
No! bone is a dynamic tissue, and undergoes lifelong remodelling. Most remodelling occurs within spongy bone.
Vertebral bones have the greatest proportion of spongy bone, and thus undergo the most active remodelling.
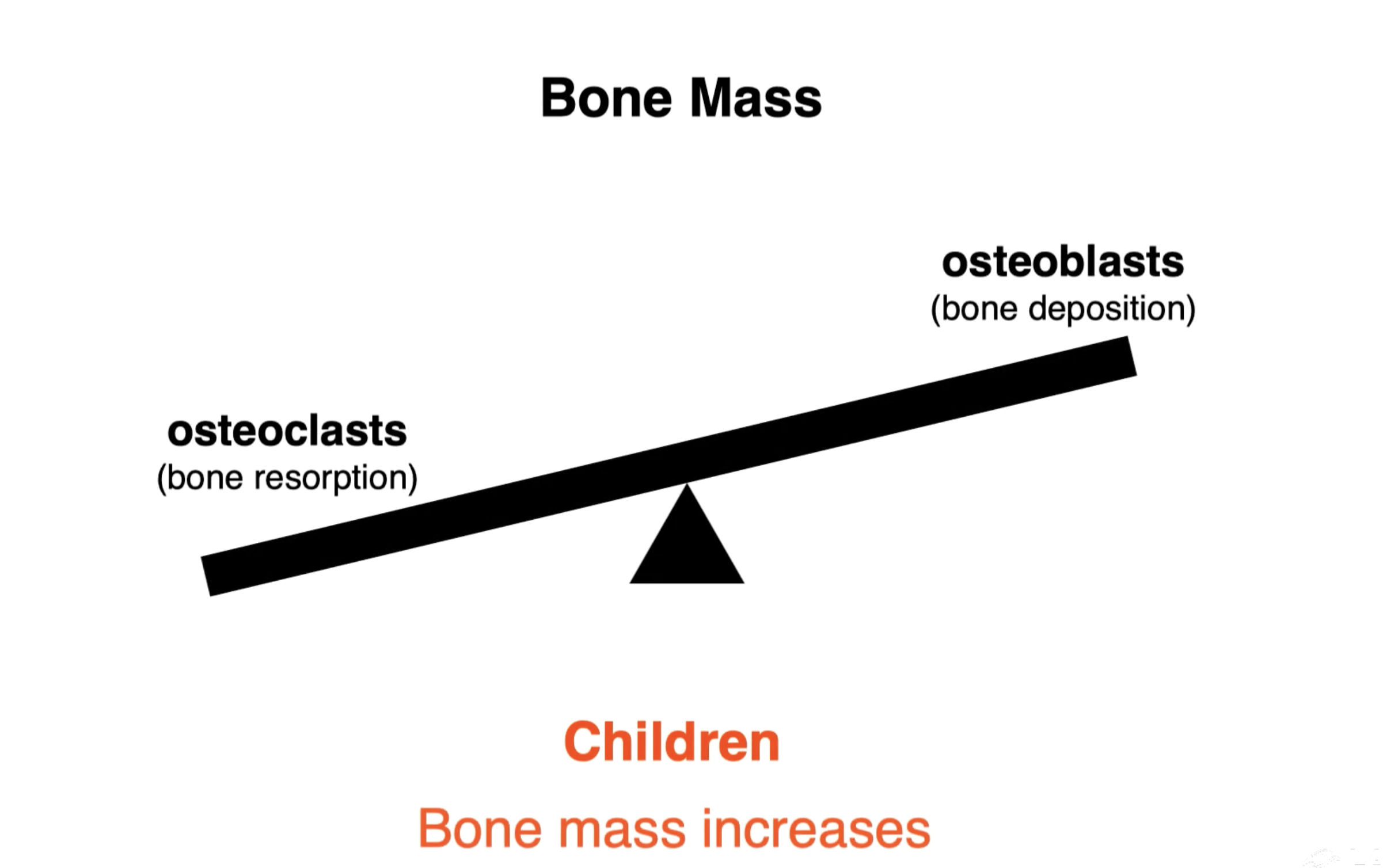
Bone mass in children
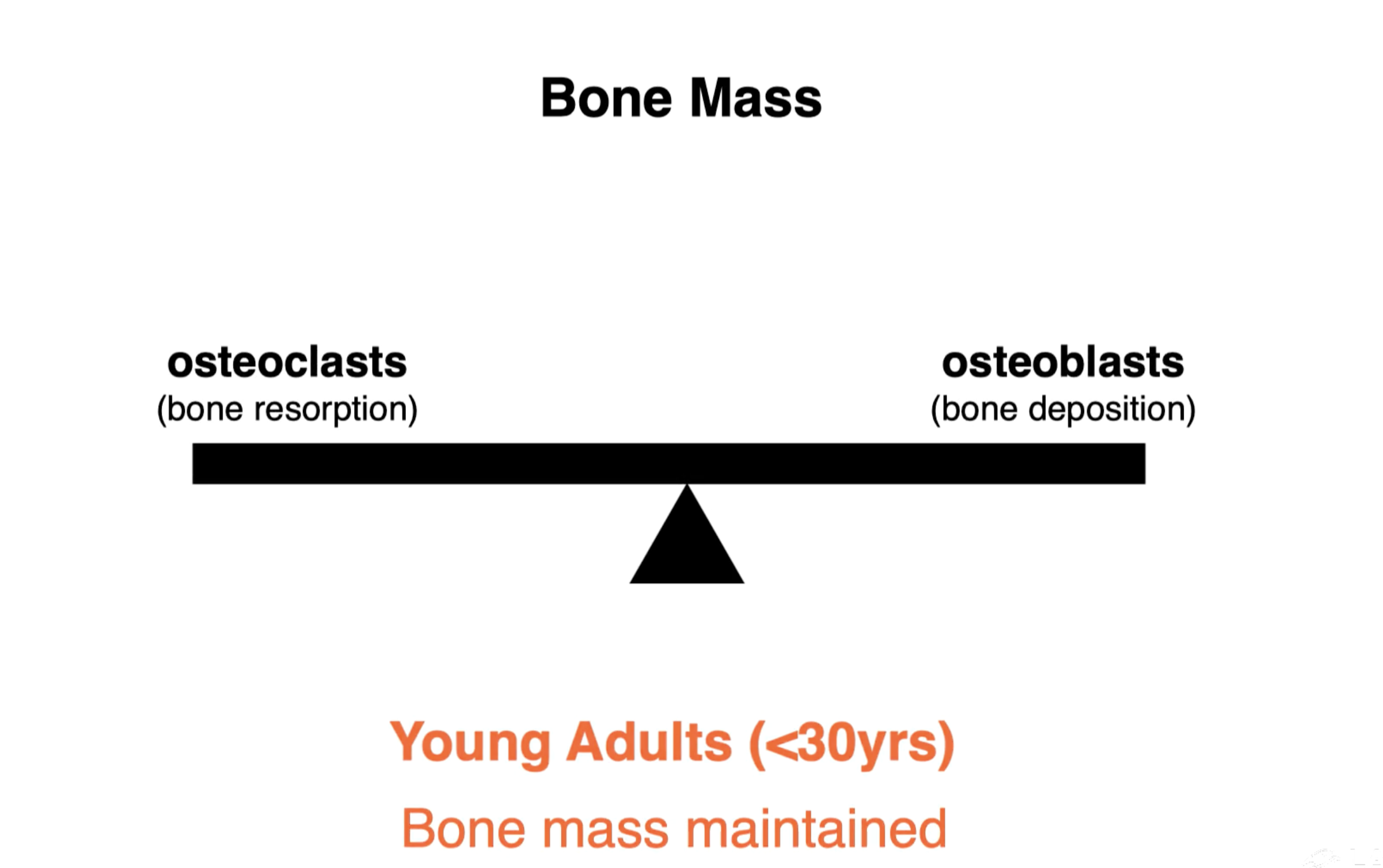
Bone mass in Young adults
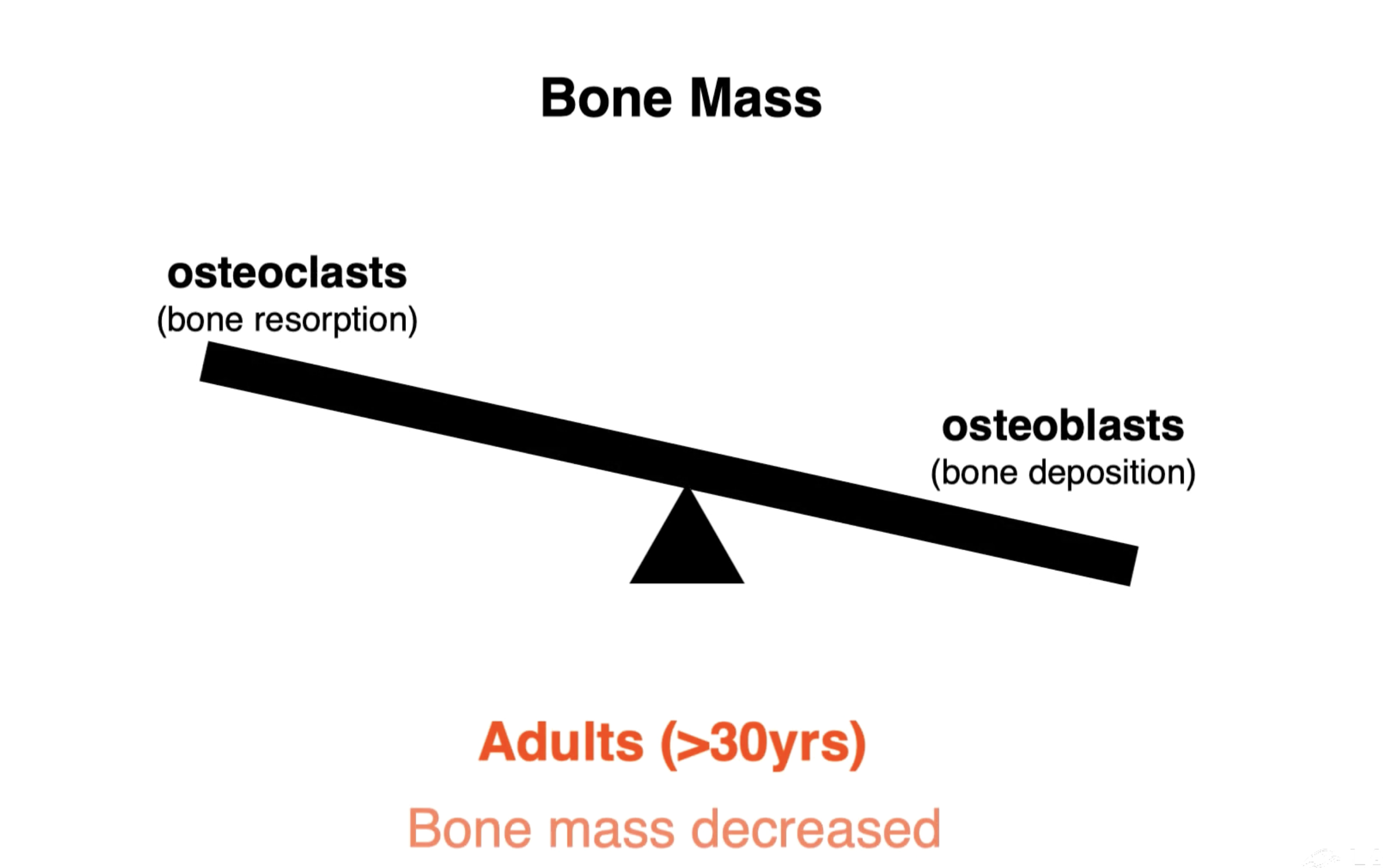
Bone mass in adults
Growth hormone
Influences the growth of long bone & insulin-like growth factors. Without growth hormones, normal bone growth does not occur.
What does exercise do?
Stimulates greater bone deposition, increasing bone density.
Resistance training is more effective than cardiovascular activities
Osteocytes and chondrocytes become mechanosensors
Causes mechanical stimuli to be transduced into intracellular signals to lay down new bone and cartilage.
Why do astronauts lose bone mass in space?
The low gravitational forces in space reduce the mechanical stress on their bodies, resulting in the loss of mineral salts and collagen fibres.
Why do fractured bones regrow smaller?
During the healing of fractured bones, there is a significant lack of forced and mechanical stress placed on the broken bone. This causes the remodelling and final healed bone to be atrophied and smaller.
Why do women lose bone mass when breastfeeding?
Possibly due to baby taking calcium from the mother’s body, or the mother producing less oestrogen (hormone that protects bones).
However, bones loss is fully recovered a few months after breastfeeding ends.
Why is calcium important for bones?
Results in the creation of calcium carbonate and calcium phosphate which both are needed to create hydroxyapatite.
The body cannot produce calcium, must be obtained from diet.
dairy, dark green leafy vegetables, nuts, beans, and even shellfish (which contains some calcium but in much smaller quantities).
Why is Vitamin D important for bones?
Vitamin D is needed for calcium to be absorbed when food passes through the small intestines.
We can get it from fatty fish, such as salmon and tuna. Cereal also contains it, but it's not found naturally in most foods. We do get it from sunlight on the skin, which the body to produce its own vitamin D. Vitamin D supplements are widely available