THE PHARMACOLOGY OF LAXATIVES AND EMETICS
1/32
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
33 Terms
What are laxatives used for?
Used to treat proven constipation - excessive water reabsorption and inadequate peristalsis, often in elderly patients with fibre-deficient diets
-often used if an increase in fibre or bran is ineffective
-often used to relieve constipation/evacuate bowel before surgical/medical procedures
What are the different types of laxatives - provide a sentence on how they work
-Water-retaining bulk-forming agents (e.g. unprocessed wheat bran, methylcellulose) that swell and the bulk then stimulates peristalsis, but can be slow onset (days).
• Stimulant laxatives - trigger peristalsis (e.g. senna, bisacodyl). Acts in 6- 12h, but can cause cramps, or atony (decreased tone in the musculature of the GI tract) if used chronically.
• Osmotic laxatives to attract water (magnesium salts, lactulose)
• Lubricants/stool softeners, act in 20-60 min, applied locally.
• Secretagogues – new agents (used in about~50% of constipated subjects are unresponsive to conventional laxatives) approved for chronic constipation
Provide 3 examples of Bulk forming laxatives and how they work?
• Ispaghula husk - indigestible vegetable material, attracts water and swells in colon, increasing peristalsis and promoting a soft stool. Takes several days to start working.
• Methylcellulose, bran, high fibre diets - similar principle. For regular management of constipation caused by poor diet. Take plenty of water with all these. Can cause flatulence & abdominal swelling. • Sterculia - swells in liquid, as for Ispaghula husk.
Provide 4 examples of Osmotic laxatives and how they work?
Osmotic laxatives – generally poorly absorbed ions, carbs or hypertonic products that cause fluid movement into the intestinal lumen by osmosis.
• Lactulose (synthetic non-absorbable disaccharide, fermented by bacteria to SCFAs, H, CO2) acts in 24-48h. Suitable for chronic constipation.
• Macrogols (inert polymers of ethylene glycol e.g. PEG). For chronic constipation also. Superior to lactulose – stool freq, abdominal pain.
• Magnesium salts (Epsom salts); rapid & complete evacuation in 2-4h; attracts water; used in bowel cleansing solutions
-Side effects; abdominal distension, pain, nausea. Usually less effective in more severe forms of constipation.
• Sodium citrate or phosphate enemas – rectal use for proven constipation and bowel clearance prior to endoscopy/surgery.
Provide 4 examples of Stimulant laxatives and how they work?
-(if osmotic laxatives fail to provide relief) Stimulant laxatives induce propagated colonic contractions. Suited for single dose use.
• Bisacodyl (synthetic drug, based on active principle of senna); acts in about 8h, take the night before; stimulates enteric nerves to cause peristalsis. Suppository acts quicker. ‘Abuse’ --> cramps: not suitable for repeated use.
• Senna fruit products, or sodium picosulfate (prodrug like bisacodyl); all have similar laxative properties.
-Bisacodyl or senna are the main OTC therapies, can have limiting side effects e.g. abdominal cramps, diarrhoea, dehydration.
• Glycerol suppositories; act as a rectal stimulant (mild irritant)
• Dantron - for constipation only in terminally ill of all ages (is carcinogenic in rodent models).
Provide 4 examples of Lubricant laxatives (stool softeners/emollients) and how they work?
-those given orally, with care (pneumonia a side effect); useful in management of haemorrhoids and anal fissure
• Docusate sodium - a detergent often used as a stool softener
• Arachis (peanut/ground nut) oil - warmed enema of 130 ml used to soften impacted faeces, promote bowel movement.
• Liquid paraffin - not recommended now as it interferes with fat (and therefore vitamin) absorption and may cause aspiration lipoid pneumonia.
• Glycerol - as a suppository for infants.
Provide 2 examples of Secretagogues laxatives, when would this be used, how do each of them work?
• 5-HT4 agonist, Prucalopride (an agonist of the 5HT4 receptor) (since 2015, EU) for chronic constipation in men/women and elderly who are unresponsive to conventional laxatives of different classes.
• Increases colonic transit by stimulating 5HT4 in colonic mucosa and enteric nerves involved in colonic peristalsis.
• Lubiprostone – is PGE1-like, and a chloride channel (in epithelial cells in the bowel- CFTR) activator, so enhances mucosal Cl- and fluid secretion & increases colonic motility
What 2 mechanisms of action of Secretagogues laxatives?
Mechanism 1 - The Submucosal plexus:
-5HT from enterochromaffin (in the colon i.e. the large intestine) cells acts on enteric sensory nerves and epithelia
-Note: Enterochromaffin cells are the primary source of 5HT in the body
1) 5HT stimulates the activity of 5HT3&4 receptors that are on sensory nerves in the enteric system - which are submucosal enteric neurons that provide a reflex
2) causes secretion via neurotransmission of Substance P and neurokinin A
3) Activates an interneuron at the Submucosal plexus and then cholinergic activation occurs (ACh binds to a nicotinic receptor = depolarisation= release of transmitter)
4) Then activates a secretory motorneuron that releases VIP (Vasoactive Intestinal Peptide)
5) VIP binds to VIP receptors on the intestinal epithelial cells
6)This activates chloride channels (such as CFTR - Cystic Fibrosis Transmembrane Conductance Regulator) in the epithelial cells
7) Chloride ions are then secreted into the intestinal lumen, which draws water into the intestine through osmosis - This increased water content softens stool and promotes intestinal motility, facilitating bowel movements.
Mechanism 2 - The Myenteric plexus:
Steps 1-3 are exactly the same except the interneuron is now at the myenteric plexus - which is sandwiched between the longitudinal muscle and the inner Circular muscle (the other main ganglion in the colon)
4) This causes contraction of the Circular muscle which helps peristalsis. Note : there are 5HT4 receptor's on both longitudinal and circular muscle and when those are bound to 5HT that will stimulate the reflex (or activation of the neurones)
- (the muscle contractions of the intestines), enhancing bowel movement.
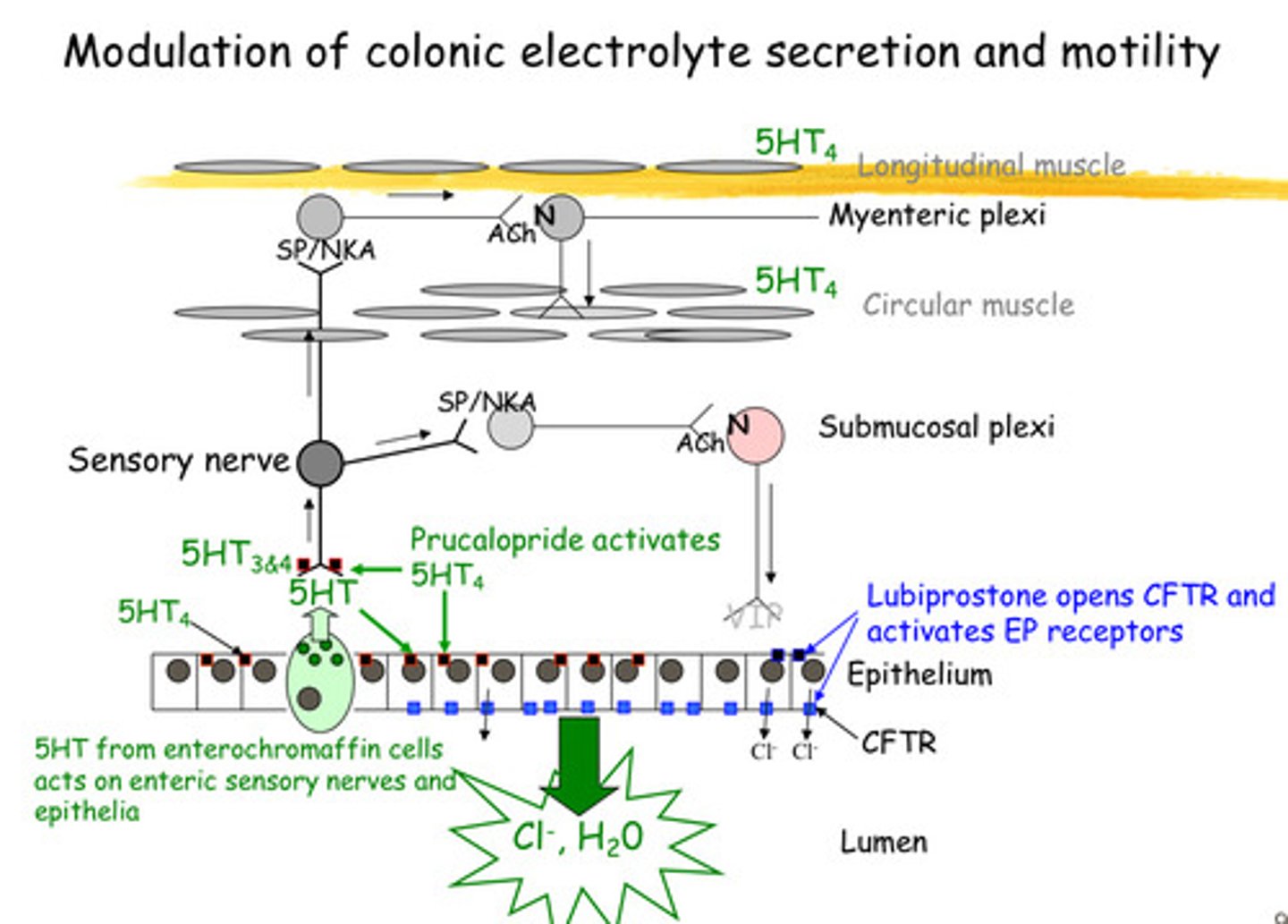
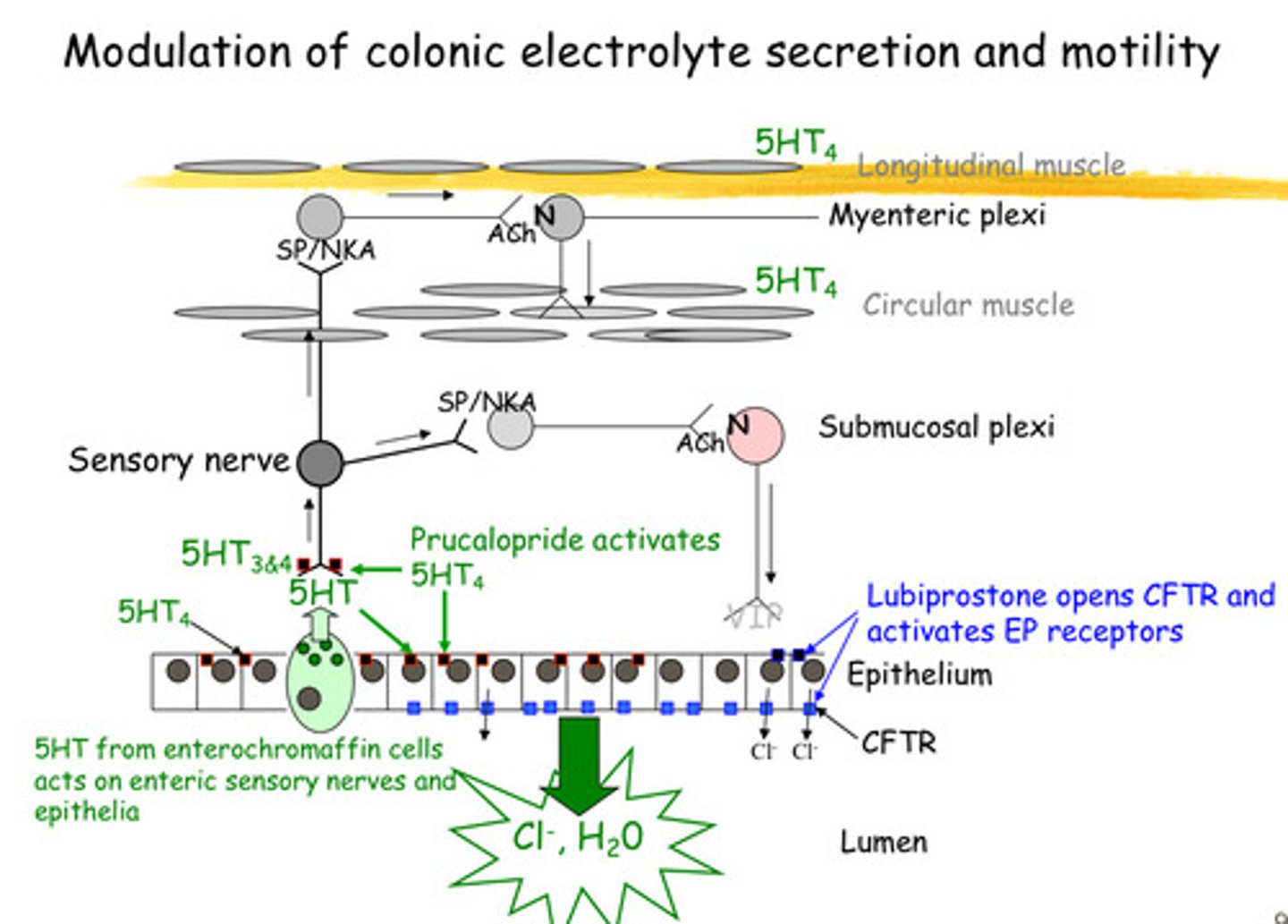
What are the 2 MOA's of Lubiprostone (a type of laxtive) and how does it help Modulation of colonic electrolyte secretion and motility
1) Lubiprostone opens CFTR Chloride ions are then secreted into the intestinal lumen, which draws water into the intestine through osmosis - This increased water content softens stool and promotes intestinal motility, facilitating bowel movements.
2) Activates EP receptors (as its structure is similar to prostaglandin E) - which are linked to g protein coupled receptors and follow the cAMP pathway that causes the opening of CFTR (double action)
What is constipation, suggest some causes of it
• Constipation - less frequent bowel emptying than the patient’s own normal pattern: faeces hard, dry, pain in passing.
• Common in elderly with fibre-deficient diet (reduced peristalsis)
• Can also be caused by drugs (e.g. opioids, calcium antagonists, anti-depressants) - methylnaltrexone is a laxative that blocks opioid-induced constipation
-May be associated with other diseases, or pregnancy, or after surgery
• Laxatives may be needed before surgery or for medical diagnostic procedures.
what is diarrohea, what are the 2 general causes in the body system?
• Increase in frequency (>3/day), fluidity and volume of stools. • General causes : (a) too rapid transit through colon - hypermotility, or (b) failure of colonic water reabsorption; or both
-Can cause infant mortality
• Often transient (protective) - no need for drugs
• Serious and/or chronic diarrhoea needs active intervention especially fluid replacement
-Treatment depends on the cause
List possible causes if Diarrhoea (hint there are 8)
• viral gastro-enteritis (usually self-limiting, rarely needs treatment)
• bacterial (food poisoning, bacillary dysentery and versions of 'travellers' tummy')
• larger parasites including amoebic dysentery and worm infestations
• irritant drugs and poisons
• allergic reactions such as food intolerance
• chronic malabsorption syndromes, need specialised dietary management
• chronic relapsing inflammatory bowel diseases (CD and UC)
• Irritable bowel syndrome (IBS)
What is Irritable bowel syndrome (IBS)
-Abnormal bowel activity, alternating episodes of diarrhoea & constipation assoc. with colic and pain. (added stress of this probably increases these symptoms)
Suggest some treatments for IBS
• Treatment can be symptomatic: + reassurance; anxiolytics; anti-spasmodics; dietary improvement
• Direct acting anti-spasmodics : peppermint oil capsules, mebeverine (both relax the smooth muscle & reduce pain); these are preferred to anti-cholinergics (e.g. dicyclomine - a muscarinic antagonist, side effects, e.g. blurred vision, dry mouth ..)
• Anti-motility drugs like loperamide, reduce diarrhoea (better than codeine - CNS actions)
• Lubiprostone – stimulates colonic fluid secretion (as for laxative mechanism), used to treat chronic idiopathic constipation in adults
What non drug advice can you give to Diarrhoea patients ?
• The best treatment of mild diarrhoea in healthy people is to abstain from food and drink plenty of clear fluids • In infants, children and the elderly check that fluid intake is adequate
• Increasing the amount of dietary fibre may help in the longer term
• Traditional remedies such as charcoal, kaolin (china clay) are helpful for mild infective diarrhoea (BUT - will also help absorb toxins if not a mild infection)
• Do not employ bulk-forming agents with anti-spasmodics as this could lead to intestinal obstruction
What is oral rehydration therapy used for ?
-Aim is to replace electrolytes and water to prevent dehydration & electrolyte imbalance
-Vital to include glucose or other simple carbohydrate (glucose enhances intestinal absorption of salts and water); they also contain NaHCO3 or Na citrate as alkalinising agent to counter acidosis
-Oral or I.V.
Note: Rice water with electrolytes is an effective alternative
What drugs are used to treat diarrhoea
-Narcotic anti-diarrhoeal drugs used to reduce intestinal hypermotility : loperamide, co-phenotrope (diphenoxylate with atropine), codeine phosphate (not available OTC anymore) - They reduce ACh release from enteric nerves which reduces the contractile and pro motile effects that are a consequence of that
-Kaolin (not in acute diarrhoea); or charcoal, to adsorb toxins
-Anti-muscarinic drugs not the best option - because of the complex side effects
-Racecadotril (a pro-drug of thiorphan) – enkephalinase inhibitor (inhibits degradation of endogenous enkephalins, which are the bodys own opiods, that are proabsorptive/procontsipatory) used to treat acute diarrhoea as adjunct to ORT.
-Ciprofloxacin – antibiotic used occasionally, prophylactic against traveller’s diarrhoea.
What are the Benefits of dietary fibre
-Indigestible vegetable fibre (cellulose of plant cell walls = ‘roughage’):
-gives bulk, enhances mechanical efficiency of intestine
-speeds up transit (reduces exposure to toxins ?)
-adsorbs water (keeps stools soft but bulky)
-promotes regular bowel habit
Note:
‘Primitive’ diets of cereals: lower incidence of colon cancer, irritable bowel syndrome (IBS) and other disorders of large intestine (e.g. IBD)
What is Inflammatory bowel disease (IBD = Ulcerative colitis & Crohn's disease)
Acute or chronic relapsing diseases (abdominal pain, bloody diarrhoea with mucus, weight loss, can be life threatening if left untreated)
Describe briefly the mechanism in drugs which treat IBD and the aims of treating Inflammatory bowel disease (IBD)?
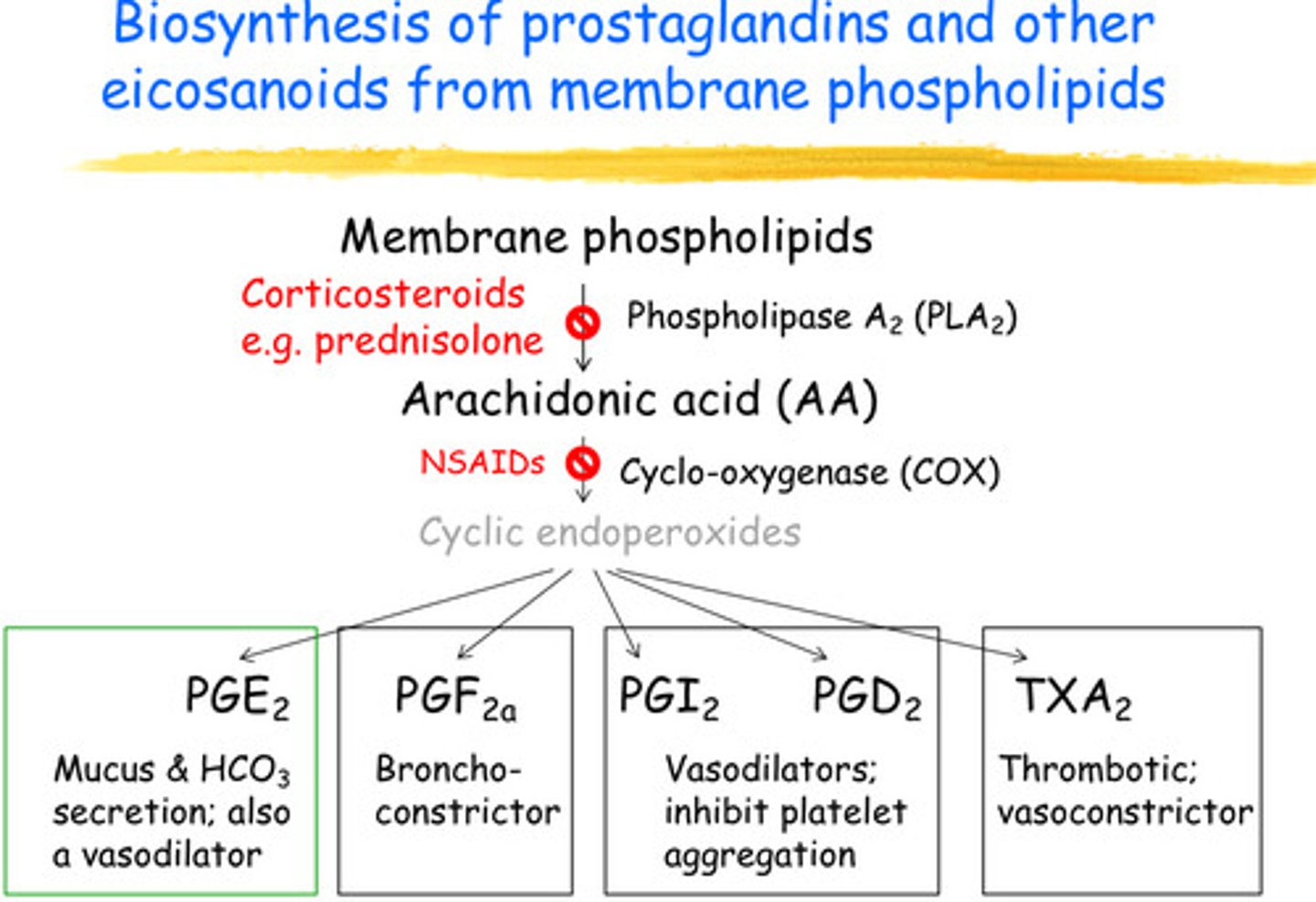
Mechanism: inhibit phospholipase A2 activity (e.g. corticosteroids) and pro inflammatory cytokine (Arachidonic Acid-Prostaglandin-cytokine cascades) cascades
-to restore electrolyte balance in seriously ill patients (i.v. nutrition)
Agents that can be used:
- anti-inflammatory corticosteroids (CS), eg. prednisolone, hydrocortisone (for severe IBD) orally, i.v. or locally. Budesonide – an oral Cprticosteroids for Crohns Disease affecting ileum and asc. colon
-Aminosalicylates (see ulcer and inflammation quizlet) e.g. sulfasalazine for less severe acute-moderate disease affecting rectum or recto-sigmoid colon
-Anti-TNFa monoclonal antibodies, e.g. Infliximab or Adalimumab (severe IBD, not CS-treatable)
Note: some of these drugs can be used to prevent relapse of Ulcerative Colitis (ie. maintain remission)
What is the pathophysiology of Crohns Disease?
Factors that can cause Crohn disease: Genetic predisposition, abnormal intestinal microbiome, environmental factors, disruption of intestinal mucosal barrier, defective innate immune system
1) Penetration of bacterial antigens into the intestinal wall, activation of innate and adaptive immune systems
2) Inflammatory response characterised by ↑Th1/Th17 and ↓T reg cells
3) ↑ interferon γ, TNFα, and interleukins IL17, IL22 & IL23
4) Recruitment of leukocytes from the blood into the intestinal wall
= Inflammatory response
List 3 Newer anti-inflammatories and how are they different
-They are antibodies that have a different MOA - don' need to remember the actual MOA's
e.g. Vedolizumab:
Antibodies against a4 and b7 integrins; membrane proteins on lymphocytes that bind to endothelial adhesion proteins, enabling lymphocyte homing to the gut - by blocking them less of this infiltration occurs
others Ustekinumab and Tofacitinib
What conditions are associated with vomiting (emesis)?
with cancer chemotherapy or migraine, or vertigo
What is the mechanism in which vomiting occur?
activation of chemoreceptor trigger zone (CTZ) in brain stem, via vagus (from the stomach), with influence from vestibular apparatus (VA, e.g. motion sickness).
-The Vomiting Centre receives input from VA (Muscarinic, H1, NK1r in VC).
-5HT-containing enterochromaffin cells sense toxins in the stomach, causing 5HT release/activation of 5HT3 receptors (there are 5HT3 and NeuroKinin-1 receptors on vagal sensory fibres)
List 3 receptors involved in vomiting
D2, 5HT3, NK1 receptors
List antiemetics and their MOA
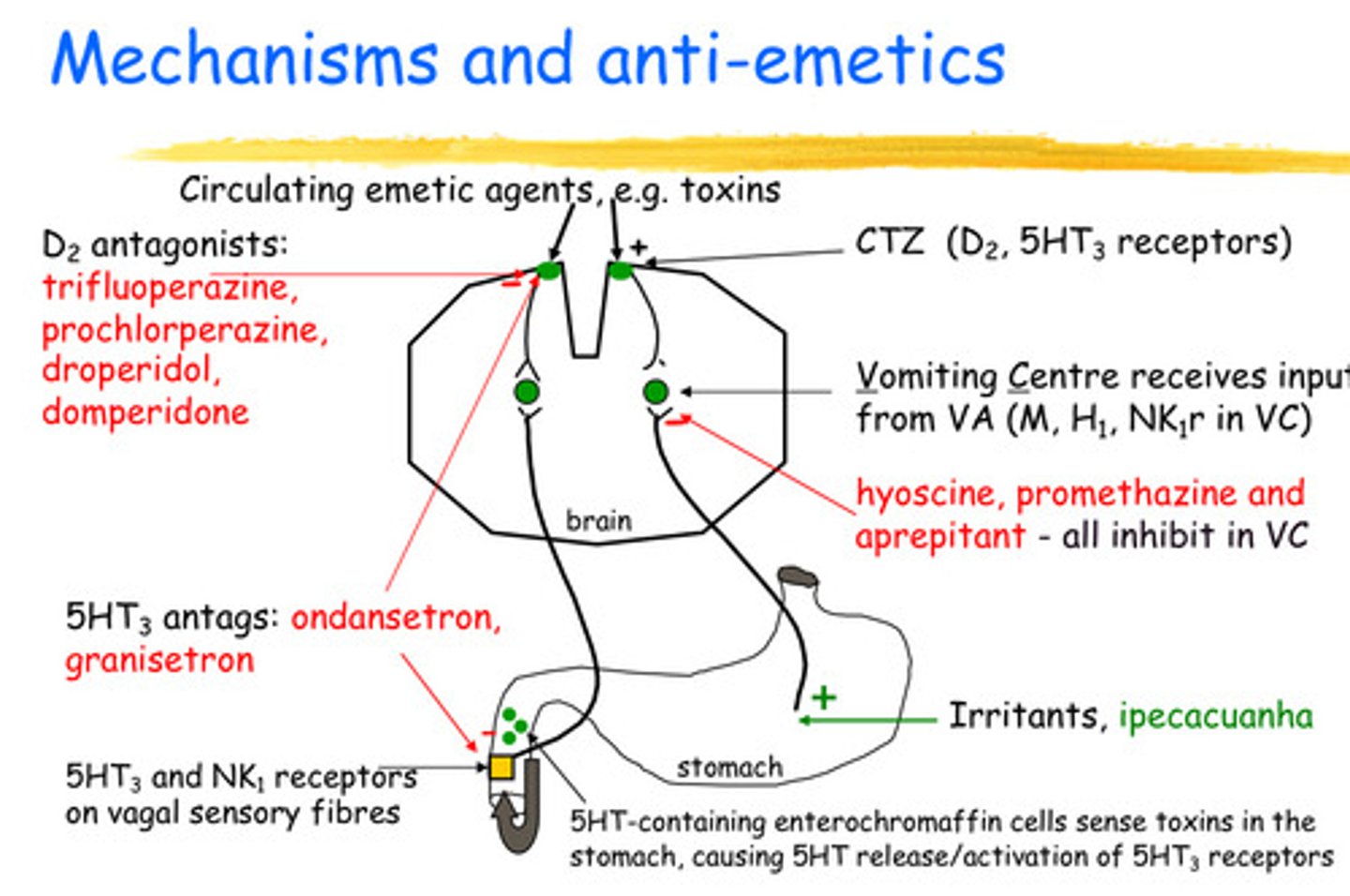
-D2 antagonists block chemoreceptor trigger zone (CTZ) in brain stem- : trifluoperazine, prochlorperazine, droperidol, domperidone
Note: CTZ is made up of (D2, 5HT3 receptors)
-hyoscine (muscarinic antagonist), promethazine (H1 antagonist) and aprepitant (Blocks Substance P and Neurokinin receptors selectively) - all inhibit the Vomiting Centre
-5HT3 antagonists - act at the chemoreceptor trigger zone (CTZ) and the Vagal sensory fibres : ondansetron, granisetron
Others:
Treatments include: -Anti-cholinergic drug (Muscarinic antagonist), e.g. hyoscine
-Sedating anti-histamines (H1 antagonists) e.g. promethazine, cinnarizine – useful against motion sickness etc.
-Phenothiazines (D2 antagonists), e.g. prochlorperazine
-other D2 antagonists, e.g. droperidol, domperidone
-5HT3 antagonists, e.g. granisetron, ondansetron
-Neurokinin (NK)1 antagonists, e.g. aprepitant, fosaprepitant
-Dexamethazone, has anti-emetic effects useful against vomiting assoc. with chemotherapy (mechanism not clear).
How to treat Emesis - < 4 hr post-poisoning with e.g. pesticides?
ipecacuanha (syrup, local irritant, + CTZ) take plus water. Not to be used if strong acids/alkali or petrol based liquid has been ingested.
Vomiting in motion sickness treatment?
: hyoscine (note. other anti-cholinergic effects)
Severe Sickness in pregnancy associated treatment?
promethazine (sedating H1 antagonist, use with caution)
Vertigo & other vestibular disorders treatment?
cinnarizine or cyclizine (H1 antags, less sedating than promethazine)
Post-operative nausea and vomiting
effective drugs are 5HT3 & H1 antags, and dexamethazone, some phenothiazines
Radiation and cytotoxic drug emesis treatment?
• Ondansetron, granisetron, dolasetron (5HT3 antags) very effective against severe nausea/vomiting esp. after anticancer chemotherapy (i.v. plus oral dexamethazone)
• Aprepitant (first of the NK1 antagonists) • Nabilone (synthetic cannabinoid, given if patient is refractory to above drugs, or significant side effects)
• Dexamethasone – anti-emetic corticosteroid
• Domperidone – short term only (D2 antag, less sedating)
When is combination therapy used?
• Combination therapy when the risk of emesis is high e.g. a 5HT3 antag + dex + NK1 antag improves control of cisplatin-related nausea.