(2) Ketone Bodies
1/44
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
45 Terms
Excess — can be used to synthesize ketone bodies via ketogenesis
acetyl coA
Where does ketogenesis occur?
liver mitochondria
Two different sources of acetyl CoA in the body
pyruvate dehydration or beta oxidation
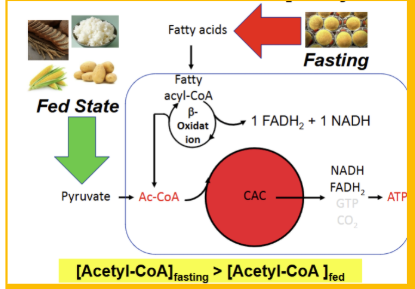
Where does acetyl CoA come from during a fasting state?
beta oxidation
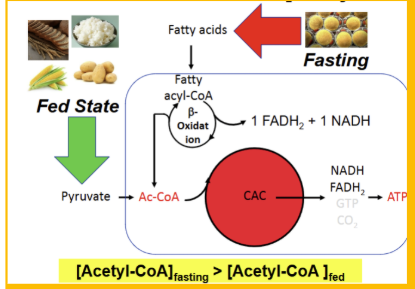
Where does acetyl CoA come from during fed state?
pyruvate dehydrogenase reaction
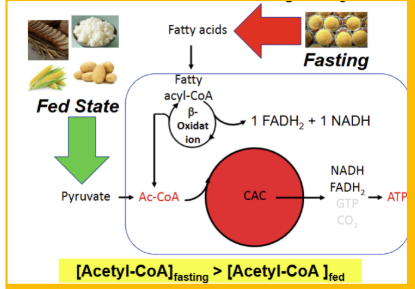
Acetyl CoA has a great concentration in a (fed or fasting ) state
fasting
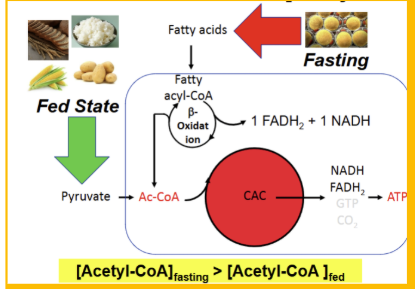
Show the ketone bodies, their names and how they may be converted between one another
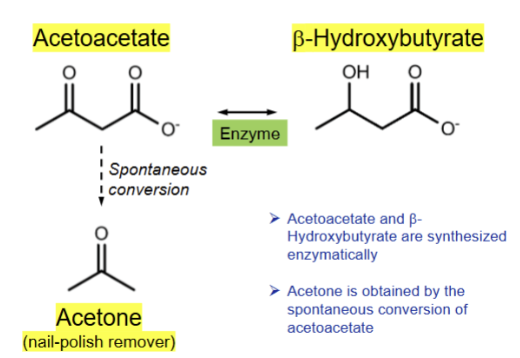
Ketogenesis occurs during (an extended fast or a large meal)
extended fast
What can cause excess lipolysis?
fasting, prolonged exercise and low exercise levels
How does excess lipolysis result in ketogenesis?
it creates and overflow of acetyl coA as beta oxidation degrade fatty acids produced by lipolysis
Excess lipolysis results in what 2 outcomes?
ketogenesis in the liver and slowing of Krebs’ cycle as it is inhibited by high [NADH] and [Acetyl-CoA]
Ketogenesis
the synthesis/ production of ketone bodies. 2 acetyl-CoA are synthesized into acetoacetyl-CoA which is then converted to acetoacetate.
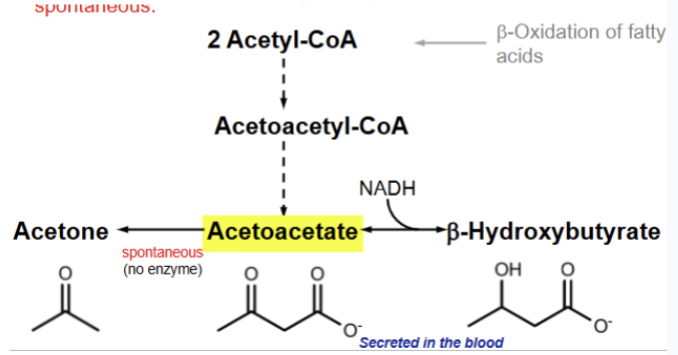
Ketone bodies stimulate — secretion which attenuates lipolysis. How does this hormone inhibit lipolysis?
insulin; it inhibits ATGL and HSL as well as increase malonyl-CoA levels which inhibits FA uptake into mitochondria and thus decreases beta oxidation
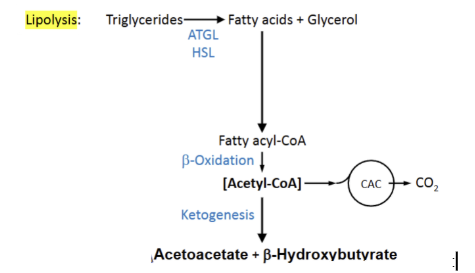
Show the feedback loop that ketone bodies are involved in within the image
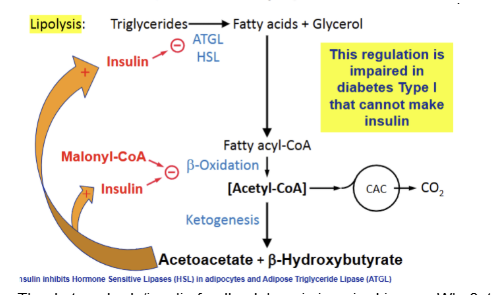
The ketone body/insulin feedback loop is impaired in —--. Why?
type 1 diabetes due to issues with insulin production
Fatty acids and ketone bodies stimulate — secretion after (a few days of fasting or a large meal)
insulin; few days of fasting
What is the purpose of the ketone feedback loop?
prevents ketoacidosis, thus ensuring ketone bodies are only used as a fuel without causing damage to the organism
Ketogenic diets
low CHO diet. The body produces lots of ketone bodies as lipolysis proceeds rapidly. Based on the belief that the body will burn fat in the absence of carbs. Usually happens within 2 to 3 days of stopping carb intake. Limits carb intake to 20 g/day
Ketolysis
ketone body oxidation. Metabolic process of breaking down ketone bodies (beta-hydroxybutyrate and acetoacetate) into acetyl CoA to produce energy (ATP) in extrahepatic tissues
Ketone bodies are used in ketolysis in what cell types
brain, heart, skeletal muscle, and kidneys
Ketone bodies are NOT used in what cell types?
liver and RBCs
The brain (can or cannot) use ketone bodies
can
In a fed state, the brain gets –% of its energy from glucose and –% from ketone bodies. In a fasting state, it gets –% of energy from glucose and –% from ketone bodies
100 and 0; 25 and 75
t/f acetyl-CoA can be used a C-skeleton for glucose in the liver
false
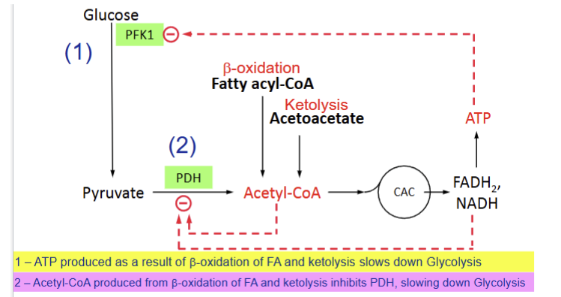
Glucose sparing
phenomenon during which metabolic conditions degrade a large quantity of fatty acids via beta oxidation and high ketolysis inhibit glucose degradation, thereby contributing to glucose-sparing effect essential for brain survival during starvation.
Ketosis
physiological state of increased production of ketone bodies (typically occur 2-3 days after fasting/starving).
Ketosis represses —- by secreting —-, restoring homeostasis. Therefore it is not pathogenic to the body
lipolysis; insulin
Ketosis occurs sooner in people who consume very few —
carbs
Ketosis may be pathogenic under what conditions?
patients who have impaired glucose production from glycogen (e.g. glycogen storage diseases) or who have impaired gluconeogenesis
Ketoacidosis
dangerous, life-threatening pathological state in which ketone-overproductions exceed body’s ketone use. May cause depletion of blood [HCO3-] and blood acidification
Ketoacidosis manifests with very high rate of —- and —- is high
lipolysis and [ketone bodies] is high
Ketoacidosis is common seen with —-
insulin deficiency
Diabetic ketoacidosis
usually occurs in those with type 1 diabetes but is rare in type 2 diabetes. Characterized by extreme hyperglycemia, severe lack of insulin, high ketone level, low pH, low serum bicarbonate and dehydration
Diabetic ketoacidosis is the number — killer of children and adolescents with type 1 diabetes
1
If untreated, people with ketoacidosis can become —- and —-
unconscious and die
Ketostix
self-testing kit for detecting excess ketone bodies in urine
Small vs moderate vs large(high) concentration of ketone bodies in blood
Ketotic hypoglycemia
characterized by low blood glucose and high blood ketones
Possible causes of Ketotic hypoglycemia
prolonged fasting, metabolic disorders (diminished gluconeogenesis, impaired glycogen synthesis or degradation), diabetic over-injecting insulin, and/or ketogenic diet
Symptoms of Ketotic hypoglycemia
shakiness/trembling, confusion or lethargy, seizures, nausea, vomiting, abdominal pain, fruity smelling breath
Remedy for Ketotic hypoglycemia
immediate glucose administration
Non-ketoic (or hypo-ketotic) hypoglycemia
characterized by both low blood glucose and low blood ketones
Possible causes of non-Ketotic hypoglycemia
excess of drugs that stimulate insulin secretion, presence of insulinoma (pancreas tumors that over-secrete insulin), fatty acid oxidation disorder, and glycogen storage disorder type 1 (GSD 1)
Symptoms of non-Ketotic hypoglycemia
shaking, tremors, sweating, hunger, headache, dizziness, fatigue, irritability, vision changes, confusion, and heart palpitations
Remedy for non-Ketotic hypoglycemia
eating small meals every 3 hours to prevent blood sugar levels from dropping too low. Implant pumps that inject glucose constantly