Innate Defence against Infection
1/17
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced |
|---|
No study sessions yet.
18 Terms
Why Do We Need an Immune System?
-Protection from pathogens and other agents
-Protect against abnormal cells (cancer)
What are the 2 parts of the immune system?
innate immunity and adaptive immunity
-They both have 5 key learning point
What is innate immunity
Innate, or nonspecific, immunity is the defense system with which you were born. It protects you against all antigens. Innate immunity involves barriers that keep harmful materials from entering your body.
What is adaptive immunity?
The adaptive immune system specifically targets the type of microorganism that is causing the infection. But to do that, it first needs to recognise the microorganismas such. This means that it's slower to respond than the innate immune system, but it's more accurate when it does respond. It also has the advantage of being able to "remember" germs. So the next time the adaptive immune system faces a germ it has already met, it can start fighting the germ faster.
What is the first line of defense for innate immunity?
-Epithelial cells - physical barrier
-The skin itself is always shedding which adds to
-Skin secretes things to protect the body e.g. sweat
-Lysozyme in tears, nasal secretion and saliva
-Mucus
-Cilia lining in trachea
-Spermine in semen
Why do microorganisms want to break through epithelial surfaces and connective tissues in the body? How do they do it in one sentence?
-To reproduce in better more nutritious environments
-They produce proteases and lipases (exotoxins) to break down the tissue matrix
How Does The Human Immune System Distinguish Pathogens From Human Tissues?
-Different adaptations due to the different environments they live in (= different proteins= different amino acid sequences - this is what the human immune system detects, regardless if they have the same function!) - self or non-self protein
How does the human immune system Counter Attack Against The Invader microorganism - discuss the alternative complement activation stage here only
Stage 1)
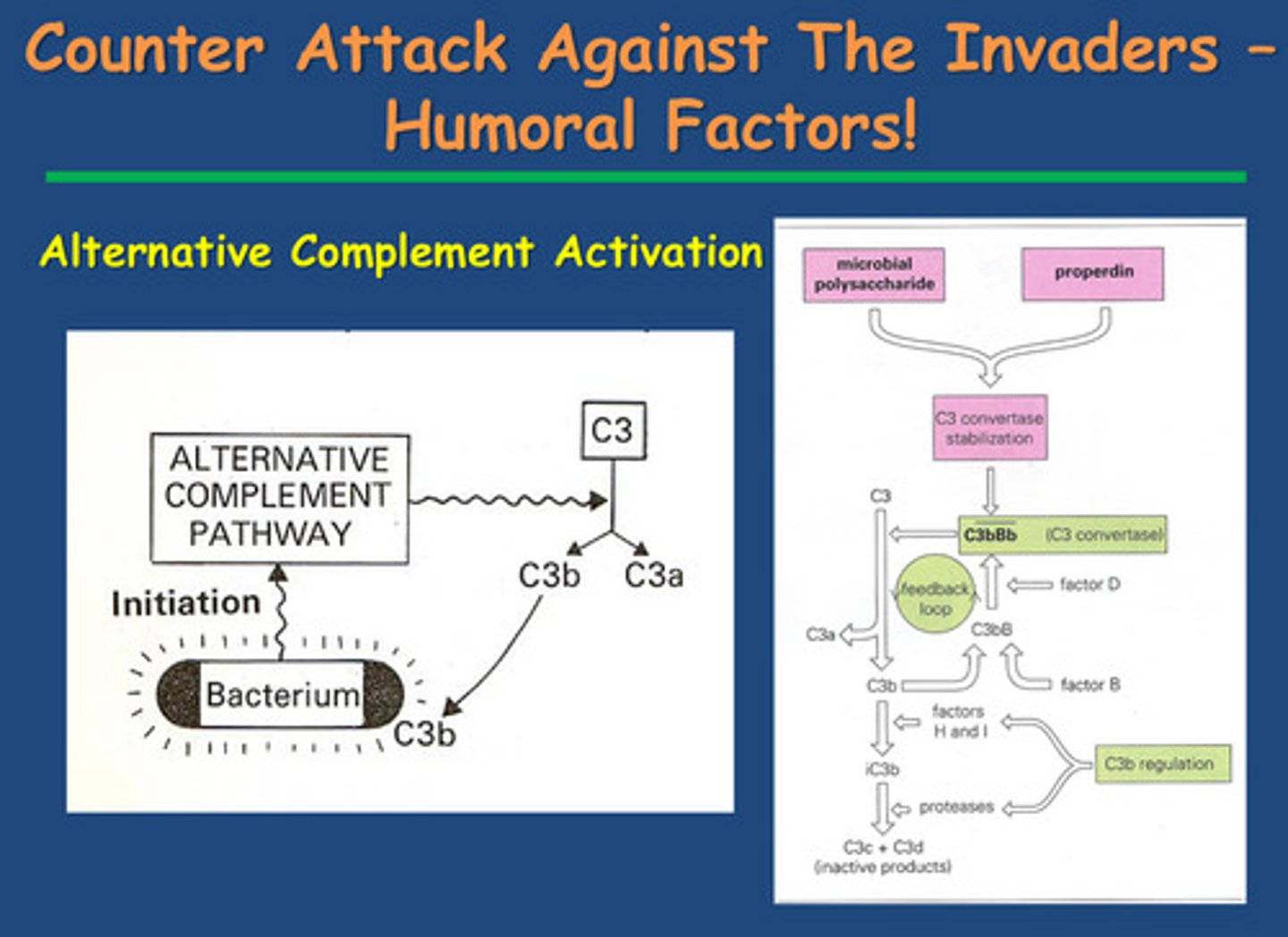
-In the prescence of a microorganism Activation of the complement pathway (a series of soluble proteins that attack bacterial cells) by the alternative complement activation pathway
Note: Factors mentioned below are humoral factors - molecules that act in the defence without direct involvement of cells
How does it work?
1) Protein C3 produced by the liver is constantly floating in circulation
2) It gets turned over into 2 subunits C3a and C3b
3) In the Prescence of a bacterium (microbial polysaccharide in the cell wall) C3b will bind to the cell surface (the polysaccharide) - this is sufficient to start the alternative complement cascade.
4) Properidin and factor D will stabilise C3b on bacterial cell surface.
5) Factor B binds to C3b = Enzyme C3 convertase is produced which converts as much C3 as it encounter into C3a and C3b.
6) Eventually C3b will cover the cell surface of C3b (opsonisation)
How does the human immune system Counter Attack Against The Invader microorganism - discuss the cell mediated response
Stage 2: Cell mediated response
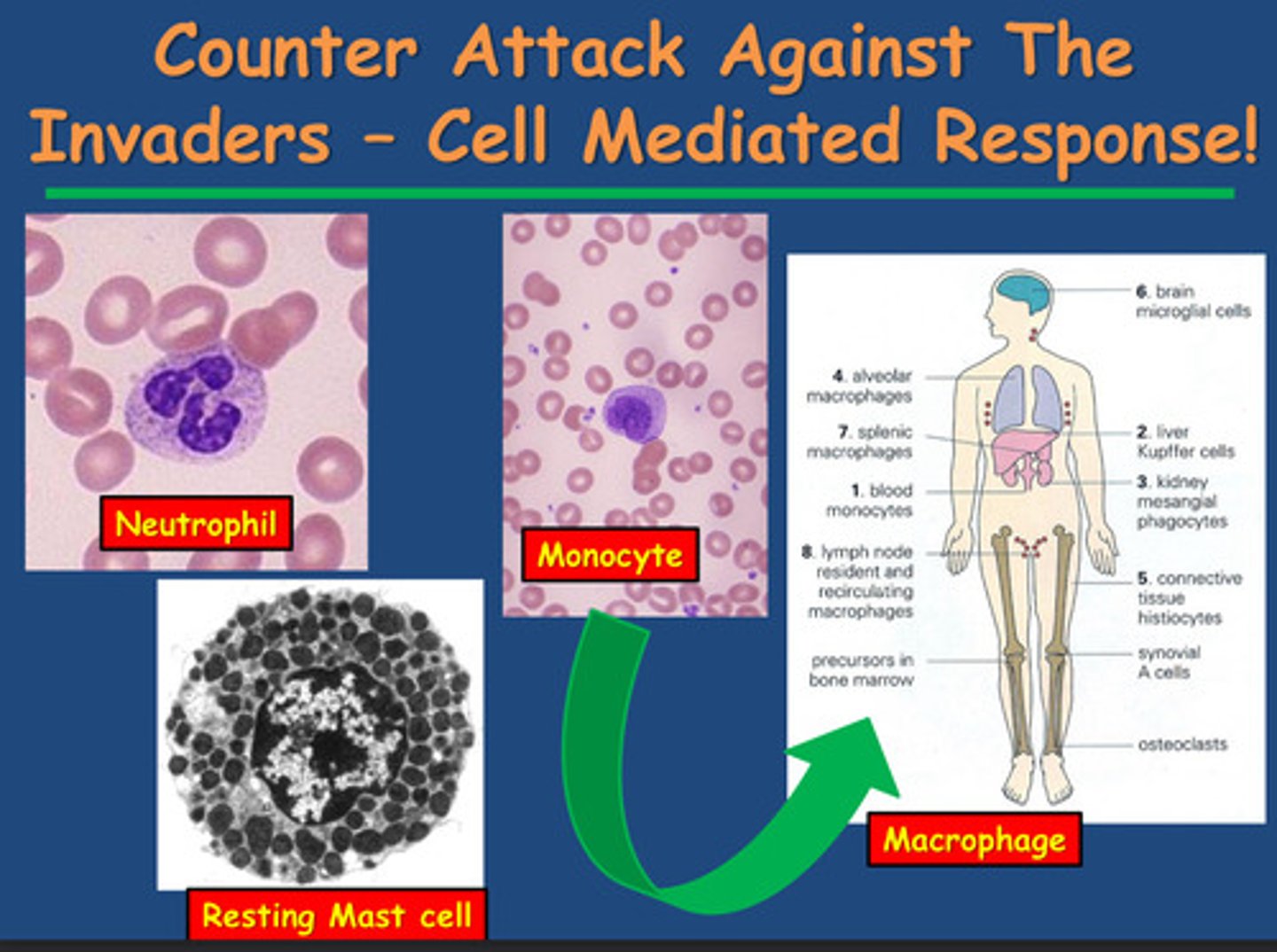
1) Neutrophils and Monocytes have receptors for C3b - these cells will recognise bacteria opsonised by C3b and bind to them and destroy them (phagocytosis)
-Polymorphonuclear leukocytes (PMNs) are a type of white blood cell (WBC) that are part of the body's innate immune system - these are always circulating the blood stream and the lymph looking for a C3b covered bacteria
-Monocytes are very short lived because they differentiate into macrophages that don't circulate within the blood, they become localised at strategic points in the body where theyre most likely to encounter microorganisms
How does the human immune system Counter Attack Against The Invader microorganism - Steps of Phagocytosis
-Microorganisms have evolved to evade this process through a number of different ways
Stage 3:
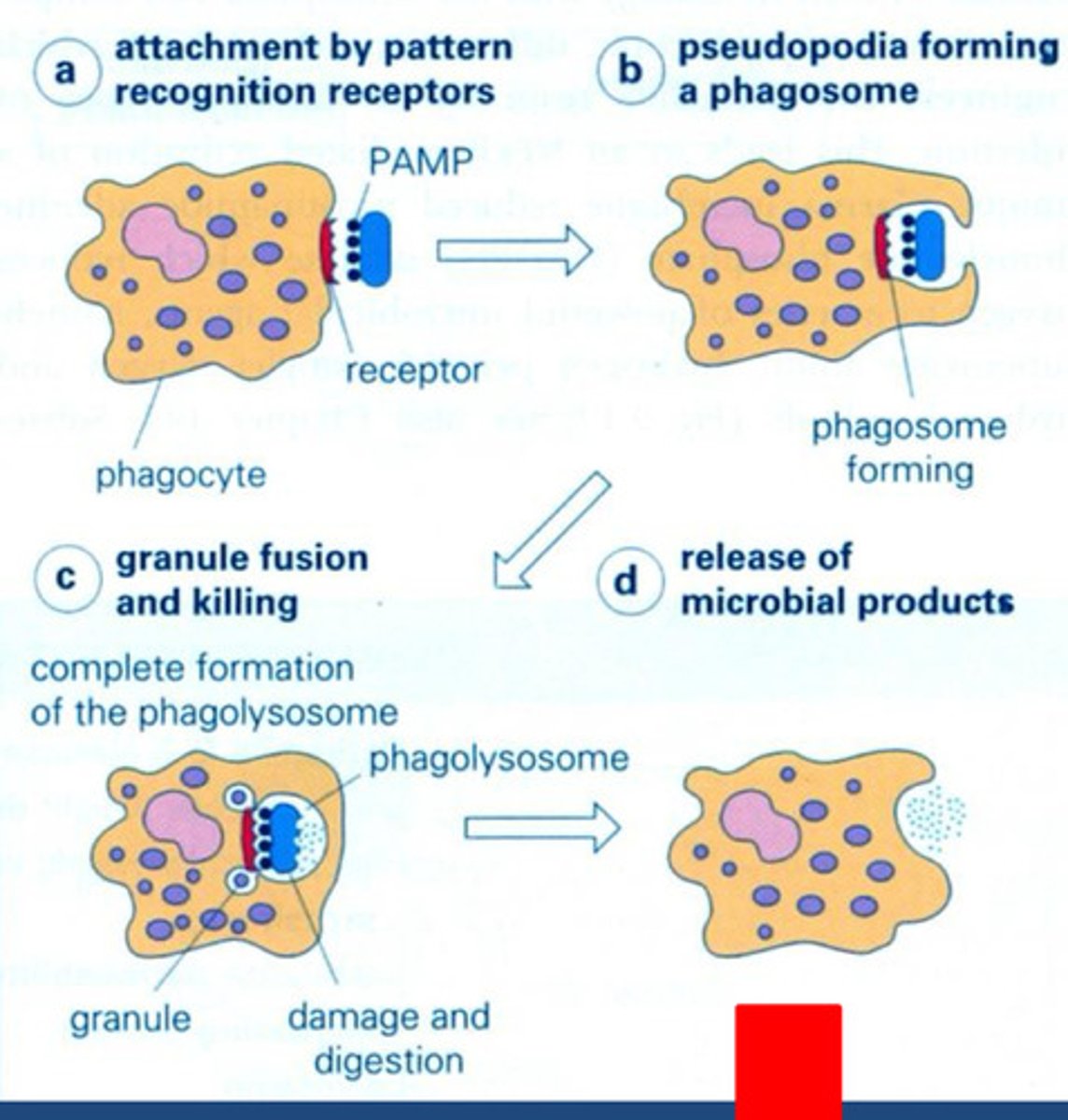
1) Microorganism taken up into a vacuole and granules in the phagocytic cell fuse with the vacuole (forming a phagolysosome) releasing a variety of different enzymes and reactive (redox proteins)
= Digestion of invaded bacteria
How does the human immune system Counter Attack Against The Invader microorganism - What happens to the debris after digestion of bacteria ?
-Neutrophils Are Attracted to Sites of Infection by C3a (a chemo-attractant) & Release Vacuole Contents After Phagocytosis = we can tell from this there are a lot of C3a around the sight where we have C3 degredation (Site of infection) but this will disseminate i.e. spread around the body = there will be a conc. gradient .
-Neutrophils (polymorphs) will be attracted to this and will follow the conc. gradient until they come to the site of infection (These are active moving cells so they will pass through blood vessels for example - Diapedesis)
-The release of C3a stimulates the liver to produce more C3 which transduces into tissues also which Amplifies the Innate Response by Opsonization.
-C3 is an acute phase protein - opsonising and coating bacterial cells so they become targets for phagocytosis
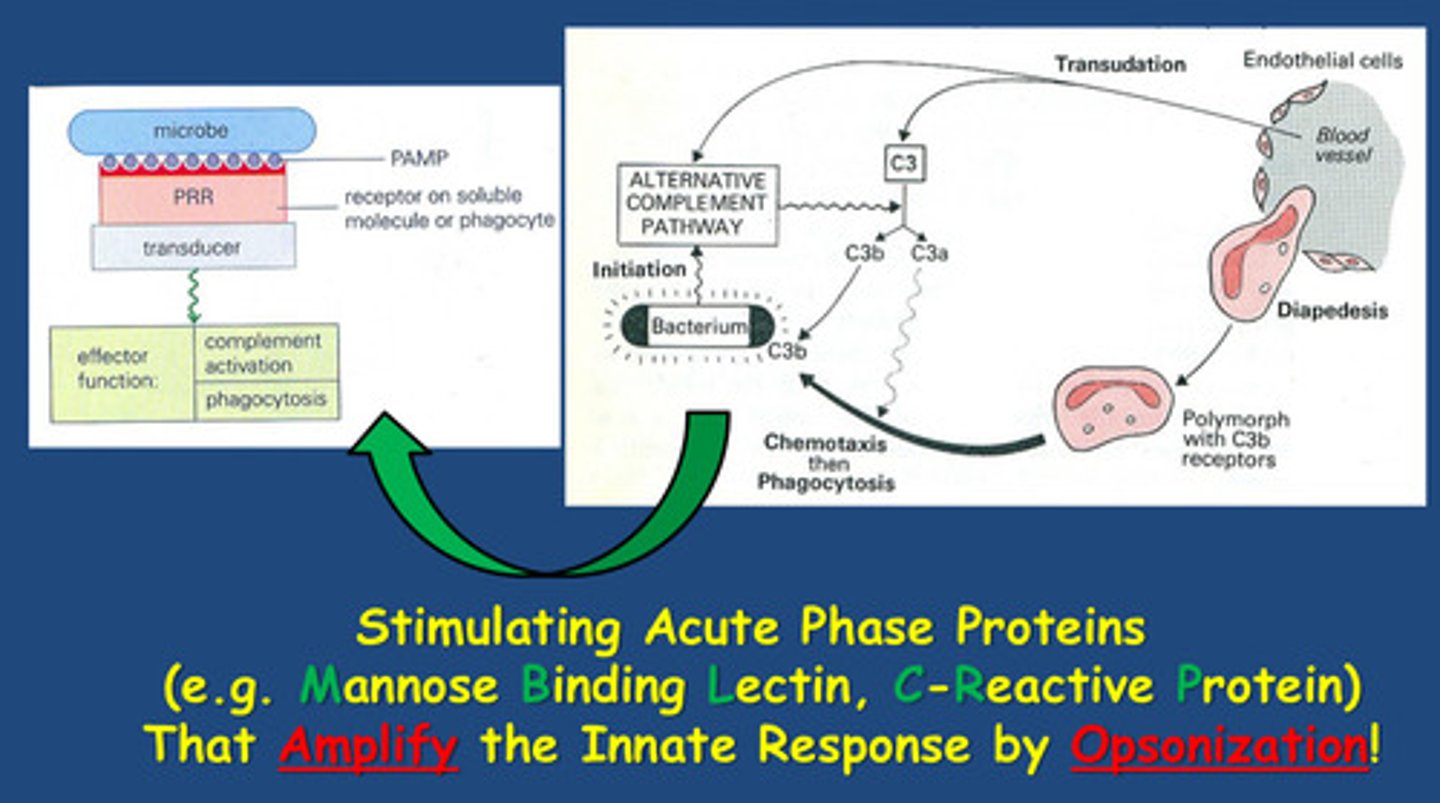
Describe the acute inflammatory response?
-Mast cells will move by chemotaxis through C3a gradient to site of infection where they will degranulate to release their mediators e.g. histamine, heparins, platelet activating factors - increase volume and elasticity of blood vessels allowing polymorphs to pass through more easily and allowing liquid bodily fluid to pass through more easily as it will be carrying C3
-Mast cell degranulation mediate the elasticity of blood cells.
-Mast Granules contain elicitors of cell function which will degranulate.
-C3a will cause mast cell degranulation also !
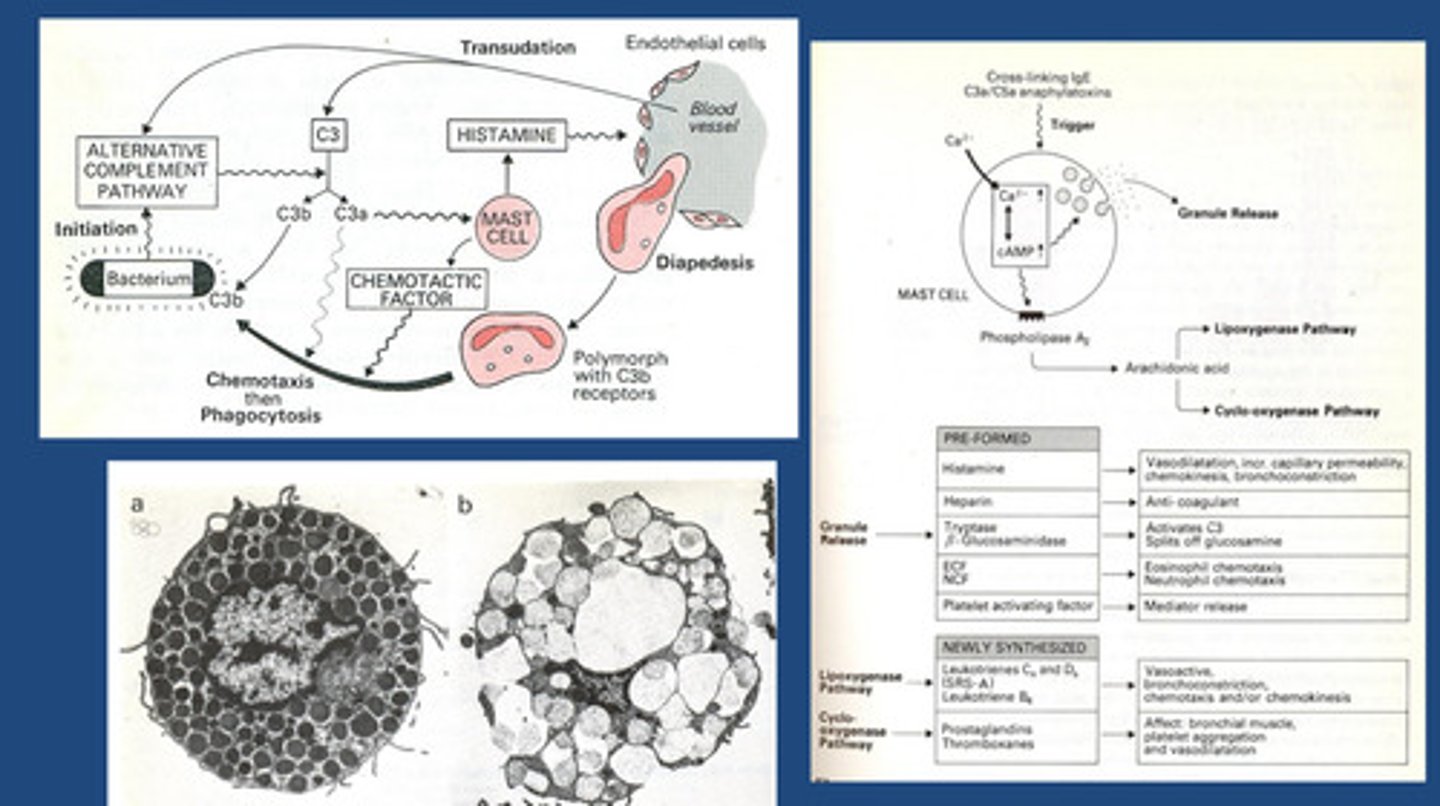
Mock exam question: Briefly summarize the events leading up to and including the process of trans-endothelial migration. (Clue - there are 5 events)
Trans-endothelial migration, also known as diapedesis, is the process by which immune cells move out of the bloodstream and into tissues during inflammation. The key events are:
1) Tethering and Rolling:
Selectins on the endothelial cells bind weakly to carbohydrate ligands on leukocytes, causing them to tether and roll along the vessel wall instead of flowing freely.
2) Activation:
Chemokines released from the site of inflammation bind to receptors on the leukocytes, activating them. This activation triggers conformational changes in integrins on the leukocyte surface.
3) Firm Adhesion:
Activated integrins on the leukocyte surface bind firmly to ICAM-1 and VCAM-1 adhesion molecules on the endothelial cells, leading to firm adhesion of leukocytes to the endothelium.
4) Crawling:
The leukocyte moves along the endothelial surface to find a junction between cells where it can pass through. This step involves actin cytoskeleton rearrangement.
5) Transmigration (Diapedesis):
The leukocyte squeezes between the endothelial cells at cell junctions, migrating through the vessel wall into the surrounding tissue to reach the site of infection or injury. This process may involve the breakdown of the basement membrane.
symptoms of inflammation
- To increase blood flow to site of infection
-Heat - Swelling - Redness - Pain - Loss of Function
What happens when there is a gram negative bacteria invader?
-Another Assault From the Complement pathway
-Recruitment of more soluble proteins
-C3 convertase converting C3 to C3a and C3b
-At the cell membrane we can also recruit C3 to become bound to the cell membrane (so it is not degraded by the enzyme C3 convertase ) forming a new protein called C5 convertase which breaks down C5 into C5a and C5b
-C5b is bound to the cells surface and acts as a magnent to a range of different proteins (C5b678) which form a pore in lipid polysaccharide - big pore = Membrane attack complex.
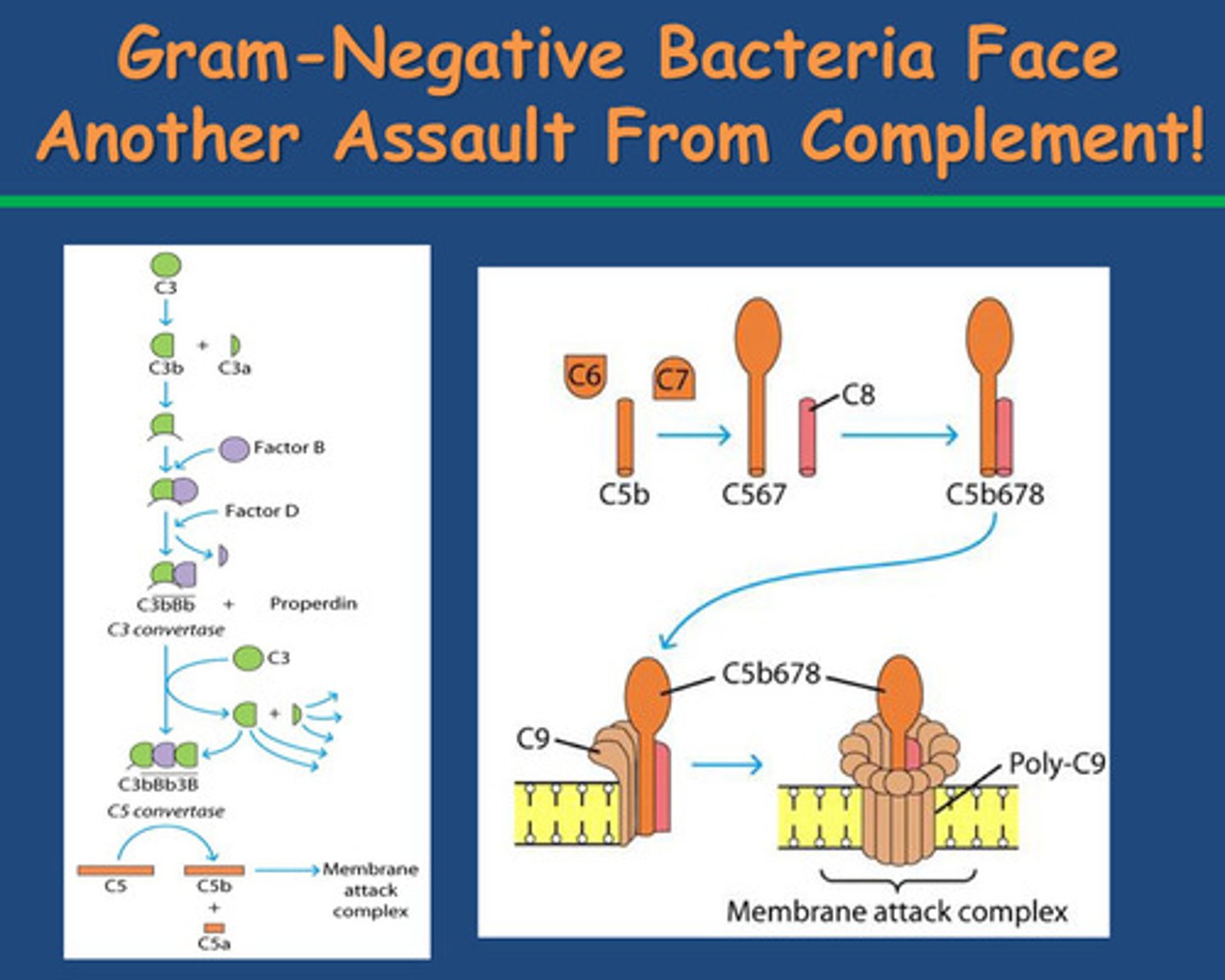
Innate Immunity to Viruses?
-NOT COMPLEMENT PATHWAY - those are mainly for bacteria and some fungi
-Obligate intracellular parasites
-As viruses penetrate through the host cell membrane they may leave part of their capsid behind - these can be identified as non-self
-Usually, all of our cells are covered in the major histocompatibility complex (MHC) - MHC class 1 and MHC class 2.
-MHC class 1 is one of the protein molecules that recognise our cells as self (why we don't attack our own cells)
-Virally infected cells sometimes withdraw that MHC 1 molecule from its surface = now seen as non-self - target for immune respone
-Virally infected cell can also release cytokines to signal other cells there is viral infection occuring
-Natural killer (NK) cells recognise infected cells as being non-self. NK cells fuse with infected host cell and release its granules = cell destruction.
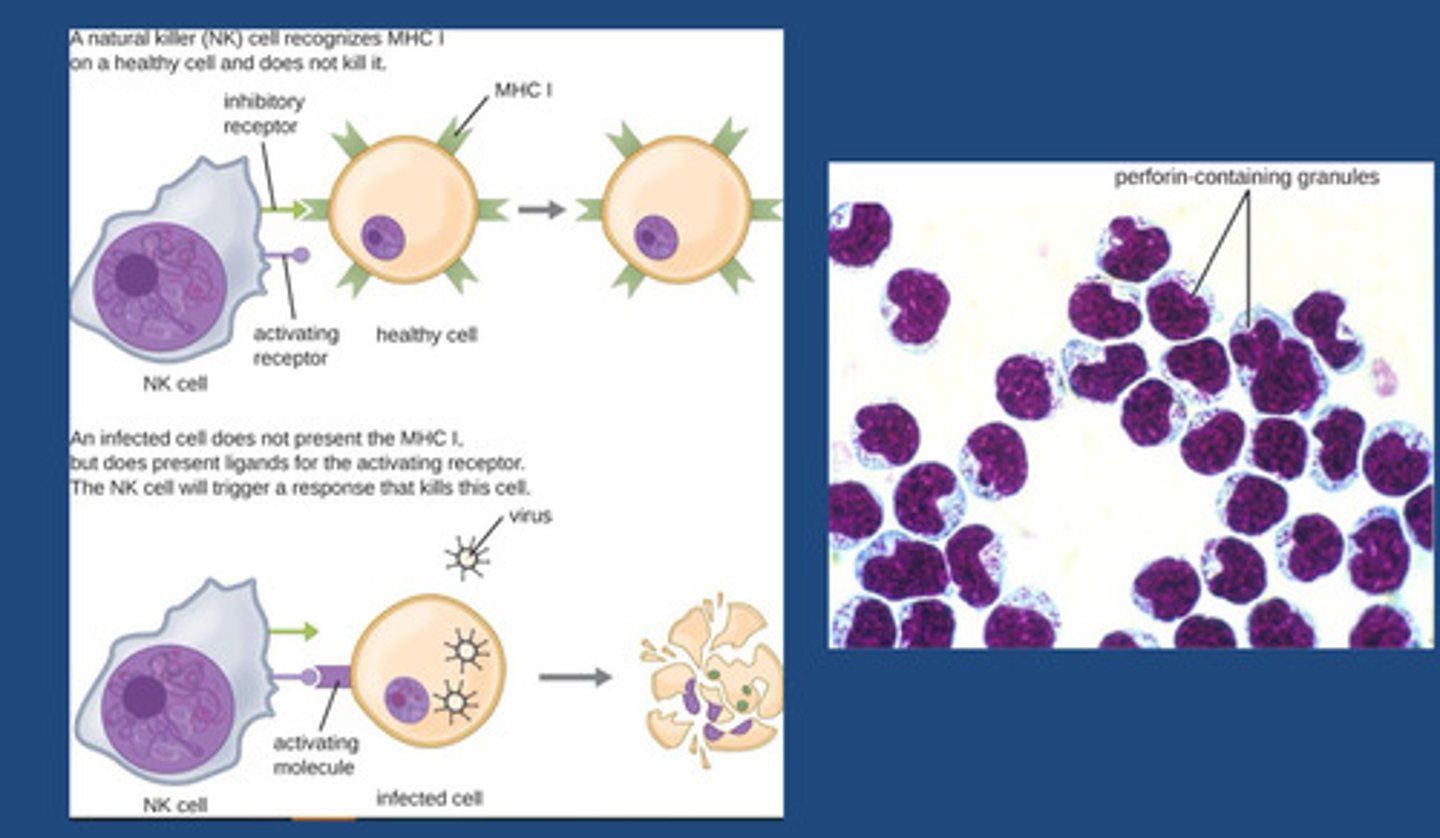
Mock exam question: In Lubeck, Germany, in 1930, a group of 251 infants was accidentally administered a tainted vaccine for tuberculosis that contained live Mycobacterium tuberculosis. This vaccine was administered orally, directly exposing the infants to the deadly bacterium. Many of these infants contracted tuberculosis, and some died. However, 44 of the infants never contracted tuberculosis. Based on your knowledge of the innate immune system, what innate defences might have inhibited M. tuberculosis enough to prevent these infants from contracting the disease?
Mucosal Barriers:
The vaccine was administered orally, so the mucosal lining of the gastrointestinal tract might have helped prevent the bacterium from entering the bloodstream. The mucus acts as a physical barrier that traps pathogens.
Phagocytes (Macrophages and Neutrophils):
Macrophages and neutrophils are key innate immune cells that phagocytose and destroy pathogens. Upon encountering M. tuberculosis, these cells could engulf the bacteria and degrade them using lysosomal enzymes, limiting infection.
Pattern Recognition Receptors (PRRs):
Cells of the innate immune system use PRRs, such as Toll-like receptors (TLRs), to recognize pathogen-associated molecular patterns (PAMPs). These receptors detect bacterial components like lipoproteins, triggering an immune response. For M. tuberculosis, TLR2 is particularly important in recognizing its cell wall components.
Cytokine Release:
Upon activation, innate immune cells release pro-inflammatory cytokines, such as TNF-α and IL-12, which help to control bacterial growth and recruit more immune cells to the site of infection, enhancing defense mechanisms.
Antimicrobial Peptides (AMPs):
The production of antimicrobial peptides (e.g., defensins) by epithelial cells and immune cells creates a hostile environment for pathogens. These peptides can directly kill or inhibit the growth of bacteria, including M. tuberculosis.
Summary 5 key factors of innate immunity
Innate Immunity – No Prior Exposure Required
1/ Physical Barriers 2/ Chemical Barriers 3/ Inflammation
4/ Phagocytosis
5/ NK-Cells