Exam 4 Pearson
1/83
Earn XP
Description and Tags
chapters 24, 25, & 26
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
84 Terms
Which of the following nutrients is NOT matched with one of its functions in the body?
lipids: major energy source for skeletal muscle and hepatocytes |
vitamins: act as coenzymes |
proteins: structural materials of the body |
carbohydrates: can serve as hormones |
carbohydrates: can serve as hormones |
Which of the following is NOT considered a nutrient?
minerals |
vitamins |
ATP |
carbohydrates |
ATP |
Which of the following statements best describes complete protein?
derived from meat and fish only |
meets all the minimum daily requirements for a healthy diet |
derived only from legumes and other plant material |
must contain all the body's amino acid requirements for tissue maintenance and growth |
must contain all the body's amino acid requirements for tissue maintenance and growth |
The most abundant dietary lipids are ________.
triglycerides |
phospholipids |
fatty acids |
cholesterol |
triglycerides |
Which of the following provides a good source of complex carbohydrates?
vegetable oil |
grain |
chicken breast |
fruit |
grain
Which type of nutrient functions primarily as an energy source for cells?
vitamins |
carbohydrates |
minerals |
oxygen |
carbohydrates |
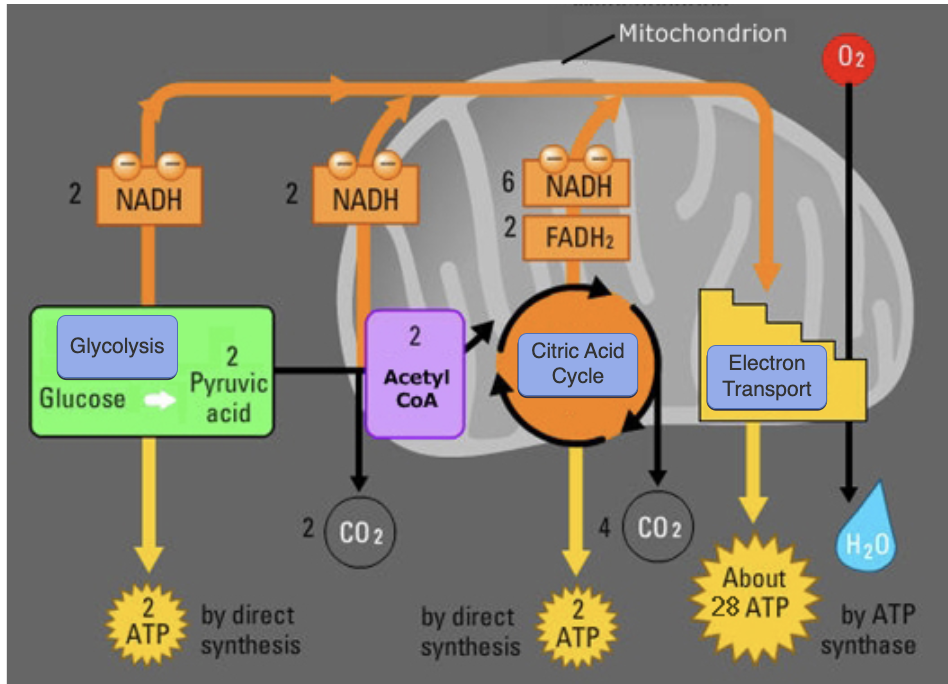
Cellular Respiration; just know
Which of the following is NOT a fat-soluble vitamin?
vitamin A |
vitamin K |
vitamin D |
vitamin B |
vitamin B
__________ refers to reactions in which small molecules are combined to build larger molecules.
Anabolism |
Carboxylation |
Catabolism |
Metabolism |
Anabolism
Redox reactions __________.
are characterized by one substance's gaining an electron while another substance loses an electron |
do not occur under physiological conditions |
rarely involve enzymes |
are characterized by the exchange of water molecules |
are characterized by one substance's gaining an electron while another substance loses an electron
The term metabolism is best defined as ________.
a measure of carbohydrate utilization, typically involving measurement of calories |
the sum of all biochemical reactions in the body |
the length of time it takes to digest and absorb fats |
the number of calories it takes to keep from shivering on a cold day |
the sum of all biochemical reactions in the body
Which of the following mechanisms produces the most ATP during cellular respiration?
oxidation reactions |
substrate-level phosphorylation |
lactic acid production |
oxidative phosphorylation |
oxidative phosphorylation |
What is the primary function of the overall reactions of cellular respiration?
to produce proteins |
to metabolize nutrients |
to regenerate ATP |
to oxidize glucose |
to regenerate ATP |
Which of the following terms is incorrectly matched with a description?
gluconeogenesis: using glucose to build noncarbohydrate structures |
anabolism: building larger molecules from smaller ones |
glycolysis: splitting of glucose molecule |
citric acid cycle: aerobic pathway |
gluconeogenesis: using glucose to build noncarbohydrate structures |
The citric acid cycle occurs in the __________ of cells and is an __________ process.
mitochondria; anaerobic |
mitochondria; aerobic |
cytosol; aerobic |
cytosol; anaerobic |
mitochondria; aerobic
Give word of given definition:
Glucose serves as the initial reactant
Glycolysis
The Citric Acid Cycle involves the removal of ____ electrons and CO2 from the substrate molecule
hydrogen
__ occurs in the cytosol of a cell
Glycolysis
What produces the most ATP?
Electron Transport Chain
The Electron Transport Chain produces the most ATP; It also involves the use of O2/CO2 to pick up excess hydrogen and electrons.
O2
__ is the breakdown of glycogen to release glucose.
Glycogenolysis
__ is the formation of glucose from protein or fats
Gluconeogenesis
__ is the storage of glucose in the form of glycogen
Glycogenesis
__ is the breakdown of glucose to pyruvic acid
Glycolysis
Gluconeogenesis is the process in which ________.
glucose is formed from noncarbohydrate molecules |
glycogen is formed |
glycogen is broken down to release glucose |
glucose is converted into carbon dioxide and water |
glucose is formed from noncarbohydrate molecules |
Glycolysis is best defined as a catabolic reaction based upon the ________.
conversion of glucose into two molecules of pyruvic acid |
formation of sugar |
conversion of glucose into carbon dioxide and water |
conversion of pyruvic acid into carbon dioxide and water |
conversion of glucose into two molecules of pyruvic acid |
Glucose can be obtained from ________.
protein anabolism |
glycogenolysis |
lipogenesis |
triglyceride anabolism |
glycogenolysis |
The process of breaking triglycerides down into glycerol and fatty acids is known as ________.
lipolysis |
lipogenesis |
glycogenesis |
gluconeogenesis |
lipolysis |
When proteins undergo deamination, the waste substance found in the urine is mostly ________.
ketone bodies |
urea |
ammonia |
acetyl CoA |
urea |
__________ is the primary hormonal regulator of the postabsorptive state.
Insulin |
Cortisol |
Parathyroid hormone |
Glucagon |
Glucagon |
Which hormone directs essentially all the events of the absorptive state?
epinephrine |
growth hormone |
insulin |
thyroid hormone |
insulin
Which of the choices below is NOT a mechanism of heat production?
enhanced thyroxine release |
vasoconstriction of cutaneous blood vessels |
shivering |
sweating |
sweating |
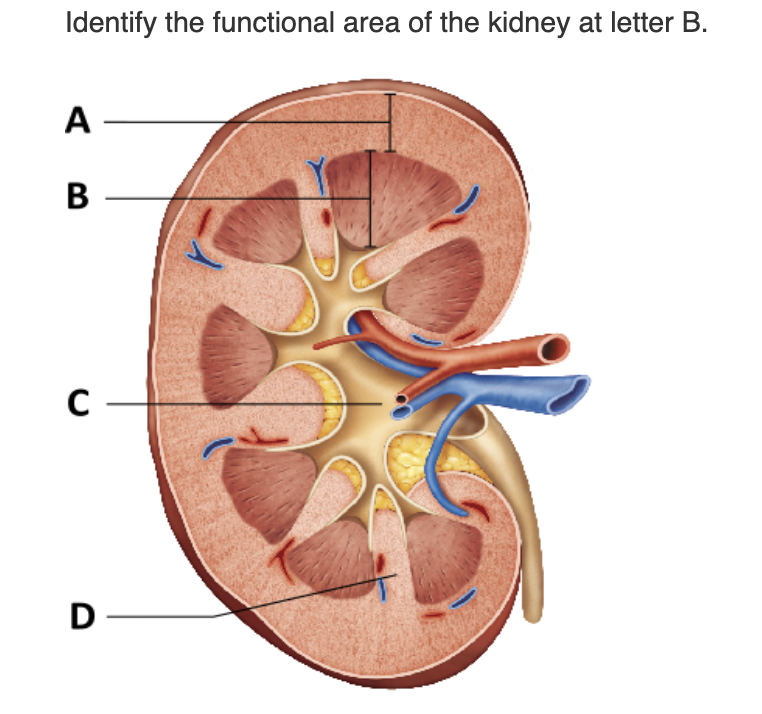
renal pelvis |
renal column |
renal pyramid |
renal cortex |
renal pyramid |
An efferent arteriole supplies blood to a glomerulus.
True |
False |
False |
The fatty tissue surrounding the kidneys is important because it ________.
cushions the kidneys against blows |
produces vitamin D and other chemicals needed by the kidneys |
ensures adequate energy for the adrenal glands to operate efficiently |
is necessary as a barrier between the adrenal glands and kidneys |
cushions the kidneys against blows |
The macula densa cells respond to ________.
changes in pressure in the tubule |
antidiuretic hormone |
aldosterone |
changes in Na+ content of the filtrate |
changes in Na+ content of the filtrate |
Place the following in correct sequence from the formation of a drop of urine to its elimination from the body.
1. major calyx
2. minor calyx
3. nephron
4. urethra
5. ureter
6. collecting duct
3, 1, 2, 6, 5, 4 |
3, 6, 2, 1, 5, 4 |
6, 3, 2, 1, 5, 4 |
2, 1, 3, 6, 5, 4 |
3, 6, 2, 1, 5, 4 |
The position of the kidneys behind the peritoneal lining of the abdominal cavity is described by the term retroperitoneal.
True |
False |
True |
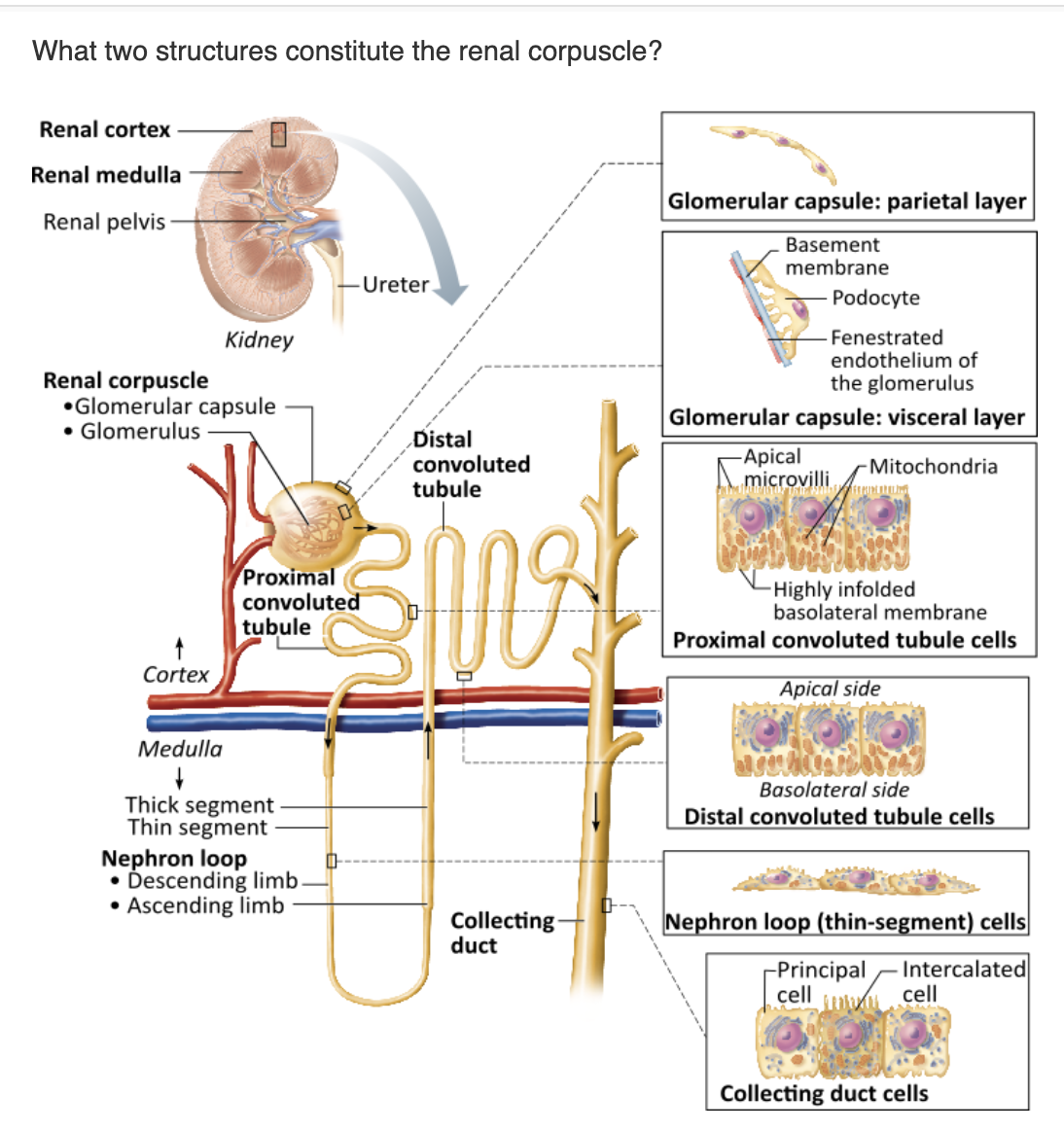
proximal convoluted tubule and nephron loop |
renal tubule and collecting duct |
glomerulus and renal tubule |
glomerulus and glomerular (Bowman's) capsule |
glomerulus and glomerular (Bowman's) capsule |
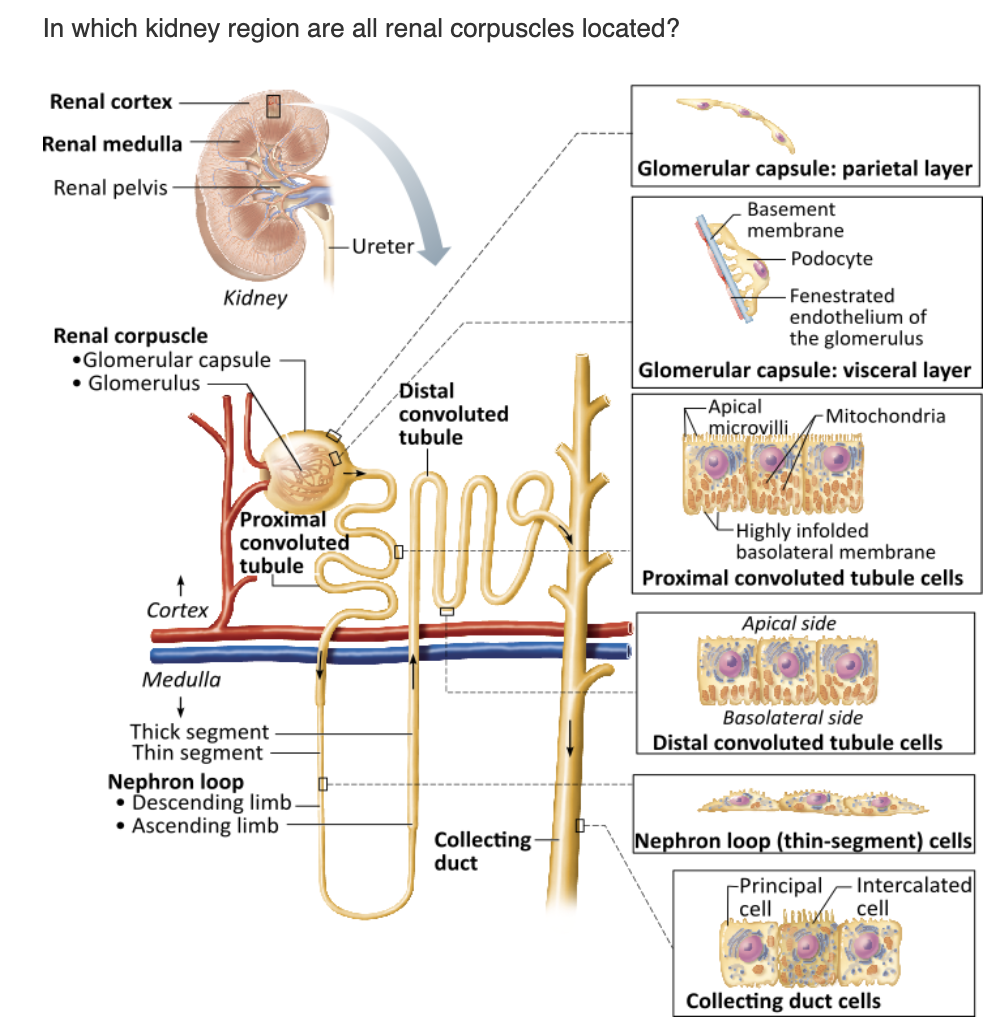
renal pelvis |
renal cortex |
renal columns |
renal medulla |
renal cortex |
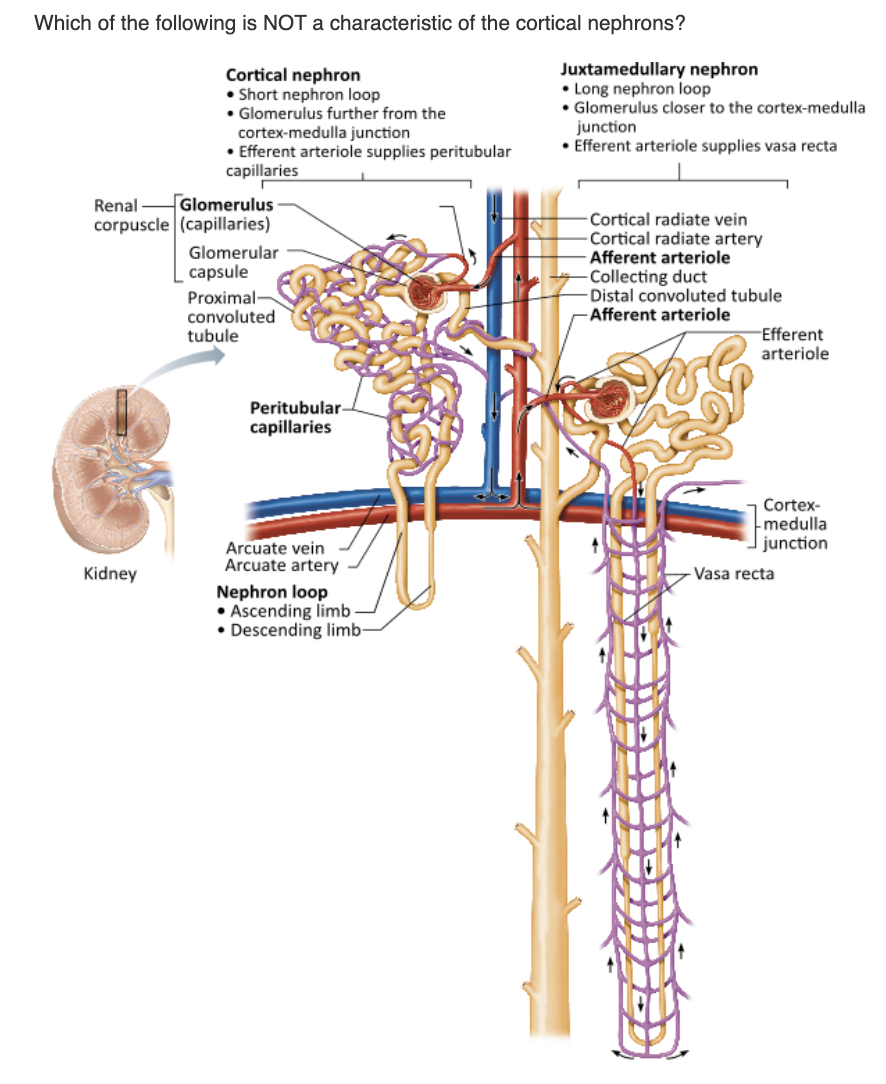
Their nephron loop is closely wrapped with vasa recta. |
The efferent arteriole of the cortical nephrons supplies the peritubular capillaries. |
Cortical nephrons have a short nephron loop. |
Cortical nephrons form the majority of nephrons in the kidney. |
Their nephron loop is closely wrapped with vasa recta. |
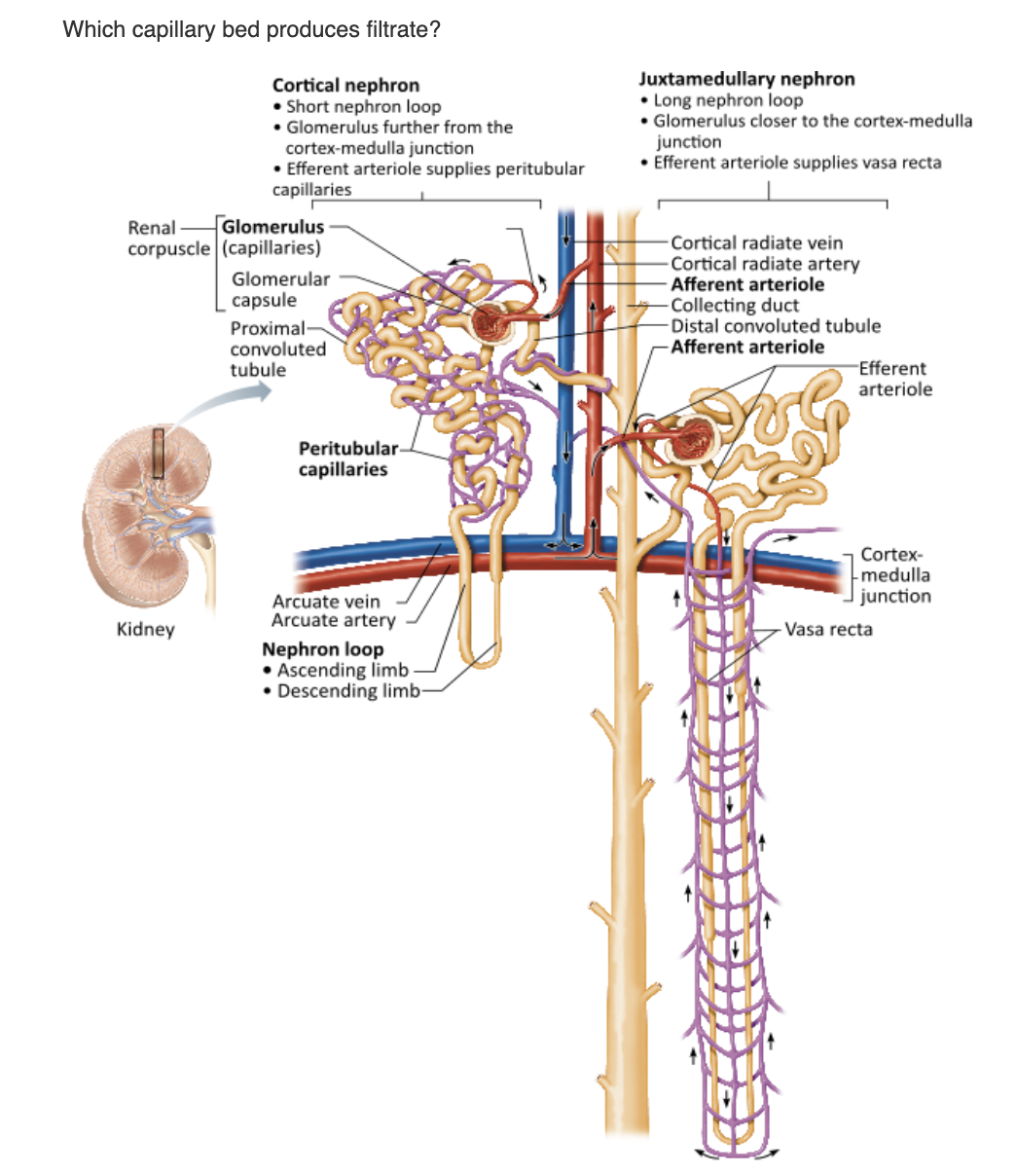
glomerulus |
peritubular capillaries |
juxtaglomerular complex (JGC) |
vasa recta |
glomerulus |
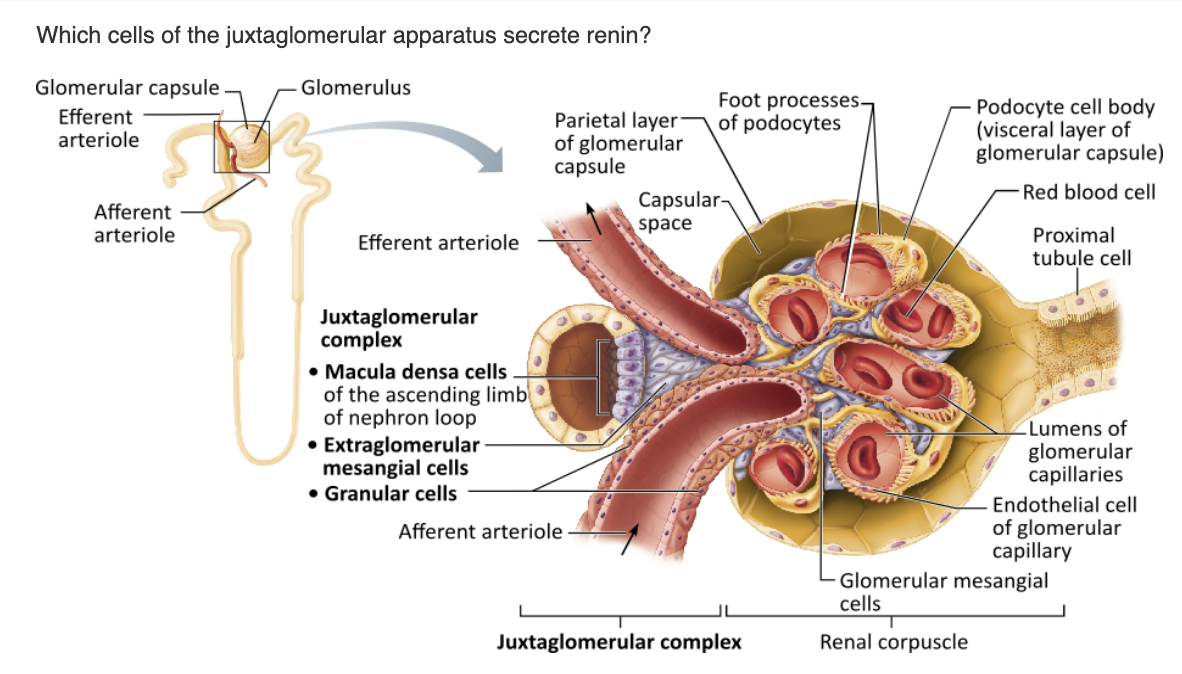
macula densa cells |
granular cells |
extraglomerular mesangial cells |
glomerular mesangial cells |
granular cells |
What is the best explanation for the microvilli on the apical surface of the proximal convoluted tubule (PCT)?
They increase the amount of surface area that comes in contact with the blood's plasma to help actively excrete toxins. |
They hold on to enzymes that cleanse the filtrate before reabsorption. |
Their movements propel the filtrate through the tubules. |
They increase the surface area and allow for a greater volume of filtrate components to be reabsorbed |
They increase the surface area and allow for a greater volume of filtrate components to be reabsorbed |
The functional and structural unit of the kidneys is the ________.
glomerular capsule |
capsular space |
nephron loop |
nephron |
nephron
Which of the following is the primary function of the juxtaglomerular complex?
releases chemical signals that regulate the rate of filtrate formation |
reabsorption of Na+ and other ions |
concentrating urine |
a system that protects the nephron from some chemicals found in blood |
releases chemical signals that regulate the rate of filtrate formation |
Which of the following is NOT a major urine formation process?
glomerular filtration |
tubular secretion |
micturition |
tubular reabsorption |
micturition |
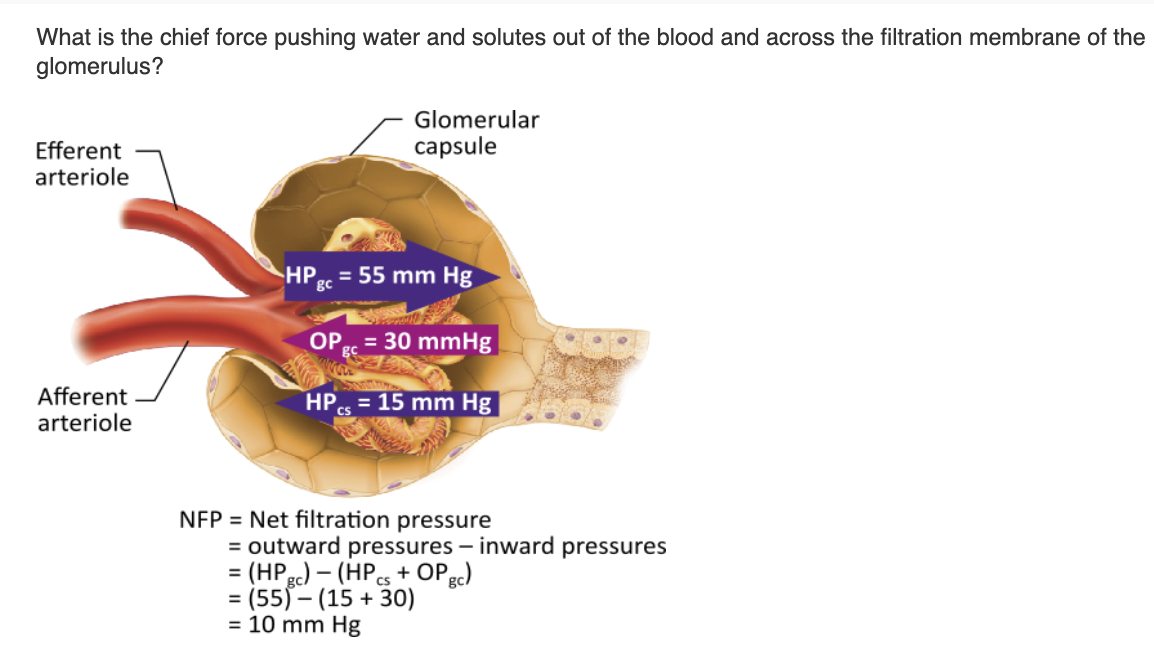
colloid osmotic pressure in glomerular capillaries (OPgc) |
hydrostatic pressure in the capsular space (HPcs) |
colloid osmotic pressure in the capsular space |
hydrostatic pressure in glomerular capillaries (HPgc) |
hydrostatic pressure in glomerular capillaries (HPgc) |
Which of the following statements best describes the difference between the intrinsic and extrinsic controls of the kidney?
Extrinsic and intrinsic controls work in nearly opposite ways. |
Extrinsic controls will reduce blood plasma volume while intrinsic controls will increase blood plasma volumes. |
Extrinsic controls have the greatest effect on systemic blood pressure while intrinsic controls have a greater effect on GFR. |
Intrinsic controls raise blood pressure while extrinsic controls lower blood pressure. |
Extrinsic controls have the greatest effect on systemic blood pressure while intrinsic controls have a greater effect on GFR. |
The glomerulus differs from other capillaries in the body in that it ________.
has a basement membrane |
is impermeable to most substances |
is drained by an efferent arteriole |
has a blood pressure much lower than other organ systems |
is drained by an efferent arteriole |
An excessive urine output is called anuria.
True |
False |
False |
Which of the following substances is not normally found in filtrate?
nitrogenous waste particles, such as urea |
blood cells and large particles |
ions, such as sodium and potassium |
water and small solutes |
blood cells and large particles |
What is the primary driving force (pressure) that produces glomerular filtration?
gravity |
hydrostatic pressure of blood (blood pressure) |
colloid osmotic pressure of blood |
hydrostatic pressure of blood (blood pressure) |
Which substance would be found in higher concentration if the membrane were damaged?
creatinine |
protein |
chloride |
glucose |
protein
If the osmotic pressure in the glomerular capillaries increased from 28 mm Hg to 35 mm Hg, would net filtration increase or decrease?
net filtration would decrease |
net filtration would increase |
net filtration would not be altered |
net filtration would decrease |
Calculate the net filtration pressure if capillary hydrostatic pressure is 60 mm Hg, capillary osmotic pressure is 25 mm Hg, and capsular hydrostatic pressure is 10 mm Hg.
35 mm Hg |
60 mm Hg |
25 mm Hg |
50 mm Hg |
25 mm Hg |
Which of the following best describes glomerular filtration rate (GFR)?
the volume of filtrate created by the kidneys per minute |
the volume of urine leaving the kidneys per minute |
the volume of filtrate created at the glomerulus per liter of blood flowing through the glomerular capillaries |
the volume of blood flowing through the glomerular capillaries per minute |
the volume of filtrate created by the kidneys per minute |
GFR regulation mechanisms primarily affect which of the following?
blood osmotic pressure (OPg) |
glomerular hydrostatic pressure (HPg) |
capsular hydrostatic pressure (HPc) |
capsular osmotic pressure (OPc) |
glomerular hydrostatic pressure (HPg) |
Which of the following are mechanisms of intrinsic control of glomerular filtration (renal autoregulation)?
tubuloglomerular feedback and the renin-angiotensin mechanism |
myogenic mechanism and sympathetic nervous system control |
myogenic mechanism and tubuloglomerular feedback |
sympathetic nervous system control and the renin-angiotensin mechanism |
myogenic mechanism and tubuloglomerular feedback |
Macula densa cells of the juxtaglomerular apparatus (JGA) regulate GFR through which intrinsic mechanism?
renin-angiotensin mechanism |
tubuloglomerular feedback |
myogenic mechanism |
sympathetic nervous system control |
tubuloglomerular feedback |
The myogenic mechanism of renal autoregulation primarily involves smooth muscle in which blood vessels?
glomeruli |
systemic arterioles |
efferent arterioles |
afferent arterioles |
afferent arterioles |
What does a high concentration of NaCl in the renal tubule at the juxtaglomerular apparatus (JGA) most likely indicate?
insufficient NaCl reabsorption due to high GFR |
insufficient NaCl reabsorption due to low GFR |
excessive NaCl reabsorption due to low GFR |
excessive NaCl reabsorption due to high GFR |
insufficient NaCl reabsorption due to high GFR |
Through the tubuloglomerular feedback mechanism, how would an increase in filtrate NaCl concentration affect afferent arteriole diameter?
Afferent arteriole diameter would stay about the same. |
Afferent arteriole diameter would decrease. |
Afferent arteriole diameter would increase. |
Afferent arteriole diameter would decrease. |
Granular cells of the juxtaglomerular apparatus (JGA) regulate GFR indirectly through which mechanism?
tubuloglomerular feedback mechanism |
sympathetic nervous system controls |
myogenic mechanism |
renin-angiotensin mechanism |
renin-angiotensin mechanism |
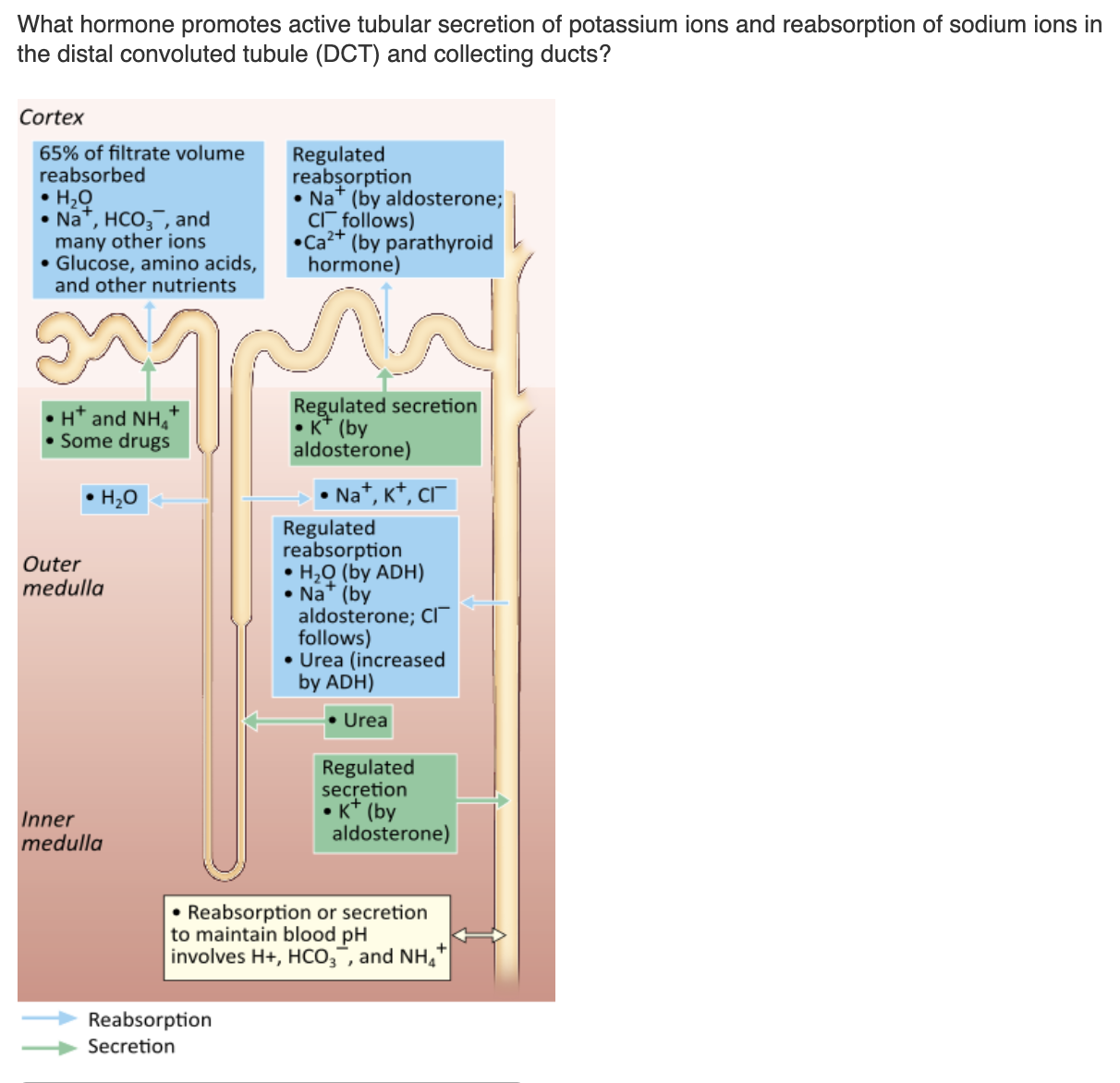
atrial natriuretic peptide (ANP) |
aldosterone |
parathyroid hormone (PTH) |
antidiuretic hormone (ADH) |
aldosterone
Where in the nephron does most solute reabsorption occur?
distal convoluted tubule |
collecting duct |
proximal convoluted tubule |
glomerulus |
proximal convoluted tubule |
CH 25 # 24